Abstract
The paraoxonase (PON) gene family consists of three members, PON1, PON2 and PON3. All PON proteins possess antioxidant properties and lipo-lactonase activities, and are implicated in the pathogenesis of several inflammatory diseases including atherosclerosis, Alzheimer’s, Parkinson’s, diabetes and cancer. Despite the role of PON proteins in critical cellular functions and associated pathologies, the physiological substrates and molecular mechanisms by which PON proteins function as anti-inflammatory proteins remain largely unknown. PON1 is found exclusively extracellular and associated solely with high-density lipoprotein (HDL) particles in the circulation, and, in part, confers the anti-oxidant and anti-inflammatory properties associated with HDL. Recent studies demonstrated that the intracellular PON proteins; PON2 and PON3 (i) are associated with mitochondria and mitochondria-associated membranes, (ii) modulate mitochondria-dependent superoxide production, and (iii) prevent apoptosis. Overexpression of PON2 and PON3 genes protected (i) mitochondria from antimycin or oligomycin mediated mitochondrial dysfunction and (ii) ER stress and ER stress mediated mitochondrial dysfunction. These studies illustrate that the anti-inflammatory effects of PON2 and PON3 may, in part, be mediated by their role in mitochondrial and associated organelle function. Since oxidative stress as a result of mitochondrial dysfunction is implicated in the development of inflammatory diseases including atherosclerosis and cancer, these recent studies on PON2 and PON3 proteins may provide a mechanism for the scores of epidemiological studies that show a link between PON genes and numerous inflammatory diseases. Understanding such mechanisms will provide novel routes of intervention in the treatment of diseases associated with pro-inflammatory oxidative stress.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Antioxidants
- Atherosclerosis
- Cancer
- Endoplasmic reticulum stress
- Inflammation
- Paraoxonase 1
- Paraoxonase 2
- Paraoxonase 3
- Quorum sensing
5.1 Introduction
The biology of oxidative stress underlies the molecular mechanisms responsible for the development of a number of inflammatory and infectious diseases, including atherosclerosis, diabetes mellitus, systemic lupus erythematosus, rheumatoid arthritis, cancer, and several ailments associated with age. A number of enzymes have evolved with pro-oxidant or anti-oxidant functions for maintaining oxidative homeostasis in cells and tissues. Understanding the function of such enzymes will pave way for the discovery of novel therapeutic agents in the fight against inflammatory diseases including atherosclerosis.
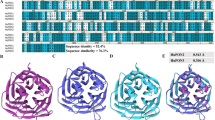
The paraoxonase (PON) gene family consists of three members, PON1, PON2, and PON3. Epidemiological studies suggest that expression of all three PON genes negatively correlates with a number of inflammatory diseases including atherosclerosis [1, 2]. PON genes are located on the long arm of chromosome 7 in human and chromosome 6 in mice [3]. PON2 appears to be the oldest member of the family, followed by PON3 and PON1, which most likely resulted from gene duplication [4]. PON1 was not only the first one of the family to be identified in a screen for plasma hydrolases of paraoxon, the active metabolite of insecticide parathion [5, 6], but also the predominant member of the PON family in the circulation. Most of the early investigations were centered on toxicological research on PON1. Following the discovery that PON1 is associated with high-density lipoproteins (HDL) in the circulation and that PON1 plays an important role in the protective antioxidant and anti-inflammatory effects of HDL [6], a new area of research emerged for PON1 in both its disease association and physiological function. In contrast to PON1, both PON2 and PON3 are predominantly localized to intracellular compartments (although small amounts of hPON3 is also associated with HDL) and modulate cellular oxidative stress generated both by intracellular mechanisms and in response to extracellular stimuli [1] (Fig. 5.1).
Battacharya et al. provided evidence for a mechanistic link between genetic determinants and activity of PON1 with systemic oxidative stress and prospective cardiovascular risk, indicating a potential mechanism for the atheroprotective function of PON1 [7]. Stevens et al. showed that recombinant human PON1 protects against organophosphate poisoning [8]. Stoltz et al. demonstrated that PON proteins can interfere with quorum sensing in vivo and suggested a potential role for PON proteins as regulators of normal bacterial florae, a link between infection/inflammation and cardiovascular disease [9]. Witte et al. [10] demonstrated that PON2 provides apoptosis resistance and stabilizes tumor cells, and Schweikert et al. [11] showed that PON3 is upregulated in cancer tissue and prevents cell death. Each of the studies described above [7–11] make the compelling argument for a role for paraoxonases in inflammation, toxicology, infection, and cancer.
5.2 Inflammation and Atherosclerosis
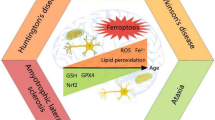
A definitive proof for the antiatherogenic role for PON genes came first from PON1 deficient and transgenic mice, which are susceptible to organophosphate toxicity and atherosclerosis [12–14] and more recently from PON2 deficient [15], which are also susceptible to atherosclerosis. In contrast, overexpression of human PON3 [16] as well as the human paraoxonase gene cluster rendered mice resistant to atherosclerosis [17]. Thus, all three members of the PON gene family are antiatherogenic in mouse models of atherosclerosis (Fig. 5.2).
5.2.1 PON1
PON1 protects LDL against oxidation and preserves function of HDL [18, 19]. PON1 null mice by gene targeting [12, 13] and transgenic mice [14] corroborate the hypothesis that PON1 protects against atherogenesis and is an important contributor to HDL’s antioxidant capacity. The in vivo studies combined with the antioxidant and antiatherogenic nature of PON1 underscore the potential of PON1 as a therapeutic agent to prevent atheroma [20, 21]. The association of PON1 with HDL and its functional consequences support a causal relationship between PON1 and cardiovascular and its associated inflammatory pathologies [22–26].
Multiple in vitro, animal and human studies have demonstrated anti-inflammatory and antioxidative functions of PON1. For example, PON1 deficient mice have been shown to be more susceptible to lipoprotein oxidation, inflammation, atherosclerosis [12, 13, 27], and hepatic steatosis [28], whereas PON1 transgenic mice over-expressing human PON1 are more resistant to inflammation and atherosclerosis [14]. PON1 has been shown to prevent LDL oxidation in vitro [18, 19] and decreased levels of PON1 are associated with increased risk for cardiovascular disease in humans [7, 29–32].
Recent detailed biochemical studies have further elucidated how PON1 exerts its anti-inflammatory and anti-oxidative functions [23, 33]. Besler et al. [33] demonstrated a role of HDL-associated PON1 activity in maintaining the endothelial atheroprotective effects of HDL, namely HDL-mediated stimulation of endothelial NO production. The study showed PON1 prevented the formation of the lipid peroxidation product malondialdehyde (MDA) in HDL. Increased MDA in HDL leads to activation of endothelial lectin-like oxidized LDL receptor 1 (LOX-1), triggering endothelial PKCβII activation, which in turn inhibited eNOS-activating pathways and eNOS-dependent NO production. The authors showed that HDL from PON1 deficient mice failed to stimulate NO production in mouse aortic endothelial cells. Subsequent supplementation of HDL from PON1 deficient mice with purified PON1 partially improved the capacity of HDL to stimulate endothelial NO production. Huang et al. [23] demonstrated that under inflammatory condition, myeloperoxidase (MPO), PON1, and HDL bind to one another, forming a ternary complex, wherein PON1 partially inhibits MPO activity, while MPO inactivates PON1. MPO is a leukocyte-derived heme protein that promotes protein and lipid oxidation [34, 35]. During inflammation, MPO binds to HDL and increases oxidant stress and promotes atherosclerosis. MPO-generated oxidant caused site-specific oxidative modification of certain tyrosine and methionine residues of PON1, leading to reduced PON1 activity [23]. Conversely, PON1 binds and partially inhibits MPO activity. Therefore, recent evidence suggests that PON1 may exert its anti-inflammatory, anti-oxidative functions, in part, by the prevention of MDA formation leading to HDL-mediated eNOS activation in endothelial cells, and inhibition of MPO activity of inflammatory HDL. PON1 has been and continues to be a target/candidate for developing therapeutic interventions for both inflammatory diseases and toxicology applications.
5.2.2 PON2
PON2 deficiency impairs respiratory complex activity and mitochondrial oxidative stress in liver, peritoneal macrophages, and aorta. PON2 protects against atherogenesis in vivo by modulating lipoprotein oxidation through the reduction of intracellular oxidative stress [36]. The principal source of cellular free radicals and oxidative stress, ROS generated by mitochondria play a fundamental role for many of the signaling pathways contributing to cardiovascular pathologies [37]. Devarajan et al. [15] hypothesized that PON2 deficiency may be influencing mitochondrial oxidative status. The authors evaluated the activities of mitochondrial ETC complexes from the livers of PON2 deficient and control C57BL/6 J mice administered an atherogenic diet, and results revealed that complex I and complex III activities were more than 50 % lower in PON2 deficient mice than in controls on a corresponding diet [15]. Moreover, the mitochondrial superoxide levels were significantly increased in PON2 deficient mice fed an atherogenic diet, and the ATP levels were reciprocally decreased when compared to control mice [15]. PON2 deficient mice showed a significantly lower level of basal mitochondrial oxygen consumption than the control peritoneal macrophage. Mitochondrial superoxide levels in peritoneal macrophages from PON2 deficient mice were significantly higher (p < 0.05) and ATP levels were significantly lower compared with control mice [15]. Furthermore, superoxide levels (using Mitosox) were significantly higher in the supernatants of whole aorta lysates of PON2 deficient mice relative to controls. PON2 deficient mice backcrossed onto the hyperlipidemic apoE deficient background develop significantly larger atherosclerotic lesions in the aorta and higher levels of macrophage immunoreactivity in the aortic sections compared to their apoE deficient controls [15]. These results demonstrated that the anti-atherogenic activity of PON2 might be linked with mitochondrial function.
5.2.2.1 PON2 Is Associated with Mitochondria, ER, and Plasma Membrane
To determine whether the changes in mitochondrial oxidative stress are due to a direct or indirect effect of PON2 on mitochondrial function, Devarajan et al. [15] isolated and analyzed mitochondria from HeLa cells for the presence of PON2. PON2 protein is present in percoll-purified mitochondria from HeLa cells. To further determine the precise submitochondrial localization of PON2, inner and outer mitochondrial membrane preparations from the livers of C57BL/6 J mice were utilized to demonstrate that PON2 is associated with the inner mitochondrial membrane (IMM). Moreover, individual ETC complex pull-down experiments showed that PON2 is associated with complex III. Western blot analyses for COX IV, an IMM associated protein, and VDAC, an outer mitochondrial membrane-associated protein, showed negligible cross-contamination of the two preparations in these experiments. Similar results were observed with mitochondria isolated from mouse heart tissue (unpublished STR). Altenhöfer et al. [38] demonstrated that PON2 reduced superoxide release from the inner mitochondrial membrane, irrespective whether resulting from complex I or complex III of the electron transport chain by modulating quinones.
5.2.2.2 PON2 Overexpression Protects Against Mitochondrial Dysfunction
HeLa cells overexpressing human PON2 under the control of a tetracycline-inducible promoter [39] were treated with antimycin, a compound known to release ubisemiquinone from the ETC, thereby generating mitochondrial superoxide [40], or with oligomycin, a compound known to inhibit ATP synthesis [41]. HeLa cells overexpressing PON2 had significantly lower superoxide and significantly higher ATP levels than control cells [15].
5.2.2.3 PON2 Protects Against Endoplasmic Reticulum Stress
Horke S et al. [42] were the first to show that PON2 decreases endoplasmic reticulum stress (ER)-induced caspase activation. PON2 was found associated with the nuclear membrane and endoplasmic reticulum and induced at both the promoter and protein levels by endoplasmic reticulum stress pathway unfolded protein response [42]. The authors concluded that PON2 is an endogenous defense mechanism against vascular oxidative stress and unfolded protein response-induced cell death. Horke et al. [43] demonstrated that PON2 protects against ER stress mediated cell death by modulating calcium homeostasis. Devarajan et al. [44] reported that macrophage PON2 regulates calcium homeostasis and cell survival under ER stress conditions and is sufficient to prevent the development of aggravated atherosclerosis in PON2 and apoE double-deficient mice on a Western diet, suggesting that macrophage PON2 modulates mechanisms that link ER stress, mitochondrial dysfunction and the development of atherosclerosis. Taken together, these studies above [10, 15, 36, 38, 39, 41–44] suggest that PON2 plays an important protective anti-oxidant role in the development of inflammatory diseases.
5.2.3 PON3
Of the three members of the PON family, PON3 appears to be the least studied to date. Although these two proteins; PON2 and PON3 appear to be similar in function and their cell-type association [1, 45, 46] recent studies suggest that both intracellular localization and role in inflammatory diseases are likely to be distinct from each other [11, 16].
5.2.3.1 PON3 Protects Against the Development of Diabetes and Atherosclerosis in Mice
Reddy et al. [46]. were the first to demonstrate that PON3 prevents the oxidation of low-density lipoprotein in vitro. To test the role of PON3 in atherosclerosis and related traits, Shih et al. [16] generated two independent lines of human PON3 transgenic (Tg) mice on the C57BL/6 J (B6) and showed that atherosclerotic lesion areas were significantly smaller in both lines of male PON3 Tg mice as compared with the male non-Tg littermates on C57B6 background fed an atherogenic diet. When bred onto the low-density lipoprotein receptor knockout mouse background, the male PON3 Tg mice also exhibited decreased atherosclerotic lesion areas. In addition, decreased adiposity and lower circulating leptin levels were observed in both lines of male PON3 Tg mice as compared with the male non-Tg mice. Shih et al. demonstrated for the first time that elevated PON3 expression significantly decreases atherosclerotic lesion formation and adiposity in male mice.
Interestingly, isolated mitochondria from the PON3 deficient livers exhibited impaired mitochondrial function as compared to the wild type mitochondria [11], suggesting that PON3 deficiency, similar to PON2 deficiency, affects mitochondrial function.
5.3 Infection and Quorum Quenching
All PON proteins possess lipo-lactonase activity [47] and hydrolyze acyl- homoserine lactones (AHLs) [48], which mediate bacterial quorum-sensing (QS) signals. The mechanism of QS has been extensively characterized in several pathogenic bacteria including P. aeruginosa, which causes catastrophic infections in immunocompromised hosts, such as individuals with cystic fibrosis, cancer and severe burns [49]. About a decade ago, Greenberg’s laboratory was the first to show that PON proteins possess AHL-inactivation activity [50] laying the foundation for a role for PON proteins in infection and quorum quenching.
Stoltz et al. [51] investigated the role of PON1, PON2, and PON3 in airway epithelial cell inactivation of N-(3-oxododecanoyl)-l-homoserine lactone (3OC12-HSL), a quorum-sensing molecule produced by gram-negative microbial pathogens such as P. aeruginosa (PAO1). Lysates of tracheal epithelial cells from PON2, but not PON1 or PON3, deficient mice had impaired 3OC12-HSL inactivation compared with wild-type mice. Overexpression of PON2 enhanced 3OC12-HSL degradation by human airway epithelial cell lysates.
Devarajan et al. [53] examined the susceptibility of PON2 deficient mice towards P. aeruginosa and demonstrated that both intact cells and membrane-enriched protein lysates obtained from PON2 deficient macrophages reveal a marked impairment in their ability to hydrolyze 3OC12-HSL. A decrease in bacterial clearance was noted in the spleen, lungs, and liver of PON2 deficient mice by 2.5, 5.7, and 14.8 fold, respectively, following administration of 1.6×107CFU of PAO1. In an ex vivo model, macrophages of PON2 deficient mice had significantly reduced phagocytosis function compared to control macrophages following PAO1 infection. These results suggested that PON2 regulates innate immune defense in PAO1 infection model [52].
Kim JB et al. [53] investigated the common and distinct pro-inflammatory pathways activated by atherogenic lipids and quorum sensing lactones, in PON2 deficient endothelial cells. Using expression profiling and network modeling, identified the unfolded protein response (UPR), cell cycle genes, and the mitogen-activated protein kinase-signaling pathway to be heavily involved in the HAEC response to 3OC12-HSL. The network also showed striking similarities to a network created based on HAEC response to Ox-PAPC, a major component of minimally modified low-density lipoprotein. HAECs in which small interfering RNA silenced PON2 showed increased pro-inflammatory response and UPR when treated with 3OC12-HSL or Ox-PAPC. 3OC12-HSL and Ox-PAPC influence similar inflammatory and UPR pathways. The authors concluded that the antiatherogenic effects of PON2 might include destruction of quorum sensing molecules, such as 3OC12-HSL, which contribute to the proatherogenic effects of chronic infection.
Recent work by Schweikert et al. [54] demonstrated that the anti-oxidative and anti-inflammatory functions of PON2 and PON3 are an important part of innate defense system against P. aeruginosa infections. Taking the work described above on PON2 and PON3 [50–54] together with the demonstration by Stoltz et al. [9] that Drosophila are protected from P. aeruginosa lethality by transgenic expression of PON1, it is very clear that PON proteins are natural quorum quenchers. Similar to PON2, PON3 not only hydrolyzes 3OC12-HSL, but also diminishes the oxidative stress and NF-κb activation induced by pyocyanin [54], a virulent factor produced by P. aeruginosa. These studies suggest involvement of PON gene family in innate immunity.
5.4 Cancer
Witte et al. [10] hypothesized that since ER stress is also relevant to cancer and associated with anti-cancer treatment resistance, PON2 may play a role in tumorigenesis. Human tumors had upregulated PON2, and PON2 knockdown caused apoptosis of tumor cells [10]. Schweikert et al. [11] demonstrated that PON3 is overexpressed in human tumors and diminishes mitochondrial superoxide formation by sequestering ubisemiquinone in cancer cells, leading to enhanced cell death resistance. The authors suggest that PON3, similar to PON2, may aid in tumor cell development. In a review of functions and mechanisms of PON2 and PON3 proteins, Witte et al. [55] suggest that although PON2 and PON3 proteins are protective from a cardiovascular standpoint, they may not be protective but may actually promote cancer cells by preventing cell death [55].
Currently, in vivo proof for a pro-tumorigenic role of PON2 and PON3 proteins is lacking and future studies in animal models will determine whether PON protein family indeed aids in cancer development.
5.5 Conclusions
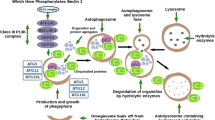
Expression of all three PON genes negatively correlates with a number of inflammatory diseases including atherosclerosis and cancer. Based on published studies, it is evident that all three PON proteins play important roles in inflammation, infection, toxicology, and cancer (Fig. 5.3). However, there is a gap in our knowledge on the mechanisms of action and function of PON proteins. Future studies aimed at understanding the molecular targets of PON proteins will unravel novel markers and therapeutic targets for the treatment of inflammatory diseases associated with ER and mitochondrial dysfunction mediated oxidative stress including atherosclerosis, bacterial infections, and cancer.
References
Reddy ST, Devarajan A, Bourquard N, Shih D, Fogelman AM. Is it just paraoxonase 1 or are other members of the paraoxonase gene family implicated in atherosclerosis? Curr Opin Lipidol. 2008;19:405–8.
She ZG, Chen HZ, Yan Y, Li H, Liu DP. The human paraoxonase gene cluster as a target in the treatment of atherosclerosis. Antioxid Redox Signal. 2012;16:597–632.
Primo-Parmo SL, Sorenson RC, Teiber J, La Du BN. The human serum paraoxonase/arylesterase gene (PON1) is one member of a multigene family. Genomics. 1996;33:498–507.
Draganov DI, La Du BN. Pharmacogenetics of paraoxonases: a brief review. Naunyn Schmiedebergs Arch Pharmacol. 2004;369:78–88.
Aldridge WN. Serum esterases I. Two types of esterase (A and B) hydrolysing p-nitrophenyl acetate, propionate and butyrate and a method for their determination. Biochem J. 1953;53:110–7.
Aldridge WN. Serum esterases II. An enzyme hydrolyzing diethyl p-nitrophenyl acetate (E600) and its identity with the A-esterase of mammalian sera. Biochem J. 1953;53:117–24.
Bhattacharyya T, Nicholls SJ, Topol EJ, Zhang R, Yang X, Schmitt D, et al. Relationship of paraoxonase 1 (PON1) gene polymorphisms and functional activity with systemic oxidative stress and cardiovascular risk. JAMA. 2008;299:1265–76.
Stevens RC, Suzuki SM, Cole TB, Park SS, Richter RJ, Furlong CE. Engineered recombinant human paraoxonase 1 purified from Escherichia coli protects against organophosphate poisoning. Proc Natl Acad Sci U S A. 2008;105:12780–4.
Stoltz DA, Ozer EA, Taft PJ, Barry M, Liu L, Kiss PJ, et al. Drosophila are protected from Pseudomonas aeruginosa lethality by transgenic expression of paraoxonase-1. J Clin Invest. 2008;118:3123–31.
Witte I, Altenhöfer S, Wilgenbus P, Amort J, Clement AM, Pautz A, et al. Beyond reduction of atherosclerosis: PON2 provides apoptosis resistance and stabilizes tumor cells. Cell Death Dis. 2011;13(2):e112.
Schweikert EM, Devarajan A, Witte I, Wilgenbus P, Amort J, Förstermann U, et al. PON3 is upregulated in cancer tissues and protects against mitochondrial superoxide-mediated cell death. Cell Death Differ. 2012;19:1549–60.
Shih DM, Gu L, Xia YR, Navab M, Li WF, Hama S, et al. Mice lacking serum paraoxonase are susceptible to organophosphate toxicity and atherosclerosis. Nature. 1998;394:284–7.
Shih DM, Xia YR, Wang XP, Miller E, Castellani LW, Subbanagounder G, et al. Combined serum paraoxonase knockout/apolipoprotein E knockout mice exhibit increased lipoprotein oxidation and atherosclerosis. J Biol Chem. 2000;275:17527–35.
Tward A, Xia YR, Wang XP, Shi YS, Park C, Castellani LW, et al. Decreased atherosclerotic lesion formation in human serum paraoxonase transgenic mice. Circulation. 2002;106:484–90.
Devarajan A, Bourquard N, Hama S, Navab M, Grijalva VR, Morvardi S, et al. Paraoxonase 2 deficiency alters mitochondrial function and exacerbates the development of atherosclerosis. Antioxid Redox Signal. 2011;14:341–51.
Shih DM, Xia YR, Wang XP, Wang SS, Bourquard N, Fogelman AM, et al. Decreased obesity and atherosclerosis in human paraoxonase 3 transgenic mice. Circ Res. 2007;100:1200–7.
She ZG, Zheng W, Wei YS, Chen HZ, Wang AB, Li HL, et al. Human paraoxonase gene cluster transgenic overexpression represses atherogenesis and promotes atherosclerotic plaque stability in ApoE-null mice. Circ Res. 2009;104:1160–8.
Aviram M, Rosenblat M, Bisgaier CL, Newton RS, Primo-Parmo SL, La Du BN. Paraoxonase inhibits high-density lipoprotein oxidation and preserves its functions. A possible peroxidative role for paraoxonase. J Clin Invest. 1998;101:1581–90.
Watson AD, Berliner JA, Hama SY, La Du BN, Faull KF, Fogelman AM, et al. Protective effect of high density lipoprotein associated paraoxonase. Inhibition of the biological activity of minimally oxidized low density lipoprotein. J Clin Invest. 1995;96:2882–91.
Deakin SP, Bioletto S, Bochaton-Piallat ML, James RW. HDL-associated PON1 can redistribute to cell membranes and influence sensitivity to oxidative stress. Free Radic Biol Med. 2011;50:102–9.
Aviram M. Atherosclerosis: cell biology and lipoproteins – paraoxonases protect against atherosclerosis and diabetes development. Curr Opin Lipidol. 2012;23:169–71.
Kim DS, Marsillach J, Furlong CE, Jarvik GP. Pharmacogenetics of paraoxonase activity: elucidating the role of high-density lipoprotein in disease. Pharmacogenomics. 2013;14:1495–515.
Huang Y, Wu Z, Riwanto M, Gao S, Levison BS, Gu X, et al. Myeloperoxidase, paraoxonase-1, and HDL form a functional ternary complex. J Clin Invest. 2013;123:3815–28.
Mackness M, Mackness B. Targeting paraoxonase-1 in atherosclerosis. Expert Opin Ther Targets. 2013;17:829–37.
Tang WH, Hartiala J, Fan Y, Wu Y, Stewart AF, Erdmann J, et al. Clinical and genetic association of serum paraoxonase and arylesterase activities with cardiovascular risk. Arterioscler Thromb Vasc Biol. 2012;32:2803–12.
Charles-Schoeman C, Lee YY, Shahbazian A, Gorn AH, Fitzgerald J, Ranganath VK, et al. Association of paraoxonase 1 gene polymorphisms and enzyme activity with carotid plaque in rheumatoid arthritis. Arthritis Rheum. 2013;65:2765–72.
Garcia-Heredia A, Marsillach J, Rull A, Triguero I, Fort I, Mackness B, et al. Paraoxonase-1 inhibits oxidized low-density lipoprotein-induced metabolic alterations and apoptosis in endothelial cells: a non directed metabolomic study. Mediat Inflamm. 2013;2013:156053.
Garcia-Heredia A, Kensicki E, Mohney RP, Rull A, Triguero I, Marsillach J, et al. Paraoxonase-1 deficiency is associated with severe liver steatosis in mice fed a high-fat high-cholesterol diet: a metabolomic approach. J Proteome Res. 2013;12:1946–55.
Jarvik GP, Rozek LS, Brophy VH, Hatsukami TS, Richter RJ, Schellenberg GD, et al. Paraoxonase (PON1) phenotype is a better predictor of vascular disease than is PON1(192) or PON1(55) genotype. Arterioscler Thromb Vasc Biol. 2000;120:2441–7.
Mackness B, Durrington P, McElduff P, Yarnell J, Azam N, Watt M, et al. Low paraoxonase activity predicts coronary events in the Caerphilly Prospective Study. Circulation. 2003;107:2775–9.
Tang WH, Wu Y, Mann S, Pepoy M, Shrestha K, Borowski AG, et al. Diminished antioxidant activity of high-density lipoprotein-associated proteins in systolic heart failure. Circ Heart Fail. 2011;4:59–64.
Aviram M, Vaya J. Paraoxonase 1 activities, regulation, and interactions with atherosclerotic lesion. Curr Opin Lipidol. 2013;24:339–44.
Besler C, Heinrich K, Rohrer L, Doerries C, Riwanto M, Shih DM, et al. Mechanisms underlying adverse effects of HDL on eNOS-activating pathways in patients with coronary artery disease. J Clin Invest. 2011;121:2693–708.
Hazen SL, Heinecke JW. 3-Chlorotyrosine, a specific marker of myeloperoxidase-catalyzed oxidation, is markedly elevated in low density lipoprotein isolated from human atherosclerotic intima. J Clin Invest. 1997;99:2075–81.
Zhang R, Brennan ML, Shen Z, MacPherson JC, Schmitt D, Molenda CE, et al. Myeloperoxidase functions as a major enzymatic catalyst for initiation of lipid peroxidation at sites of inflammation. J Biol Chem. 2002;277:46116–22.
Ng CJ, Bourquard N, Grijalva V, Hama S, Shih DM, Navab M, et al. Paraoxonase-2 deficiency aggravates atherosclerosis in mice despite lower apolipoprotein-B-containing lipoproteins: anti-atherogenic role for paraoxonase-2. J Biol Chem. 2006;281:29491–500.
Mabile L, Meilhac O, Escargueil-Blanc I, Troly M, Pieraggi MT, Salvayre R, et al. Mitochondrial function is involved in LDL oxidation mediated by human cultured endothelial cells. Arterioscler Thromb Vasc Biol. 1997;17:1575–82.
Altenhöfer S, Witte I, Teiber JF, Wilgenbus P, Pautz A, Li H, et al. One enzyme, two functions: PON2 prevents mitochondrial superoxide formation and apoptosis independent from its lactonase activity. J Biol Chem. 2010;6(285):24398–403.
Ng CJ, Wadleigh DJ, Gangopadhyay A, Hama S, Grijalva VR, Navab M, et al. Paraoxonase-2 is a ubiquitously expressed protein with antioxidant properties and is capable of preventing cell-mediated oxidative modification of low density lipoprotein. J Biol Chem. 2001;276:44444–9.
Ohnishi T, Trumpower BL. Differential effects of antimycin on ubisemiquinone bound in different environments in isolated succinate. Cytochrome c reductase complex. J Biol Chem. 1980;255:3278–84.
Kim SB, Berdanier CD. Oligomycin sensitivity of mitochondrial F(1)F(0)-ATPase in diabetes-prone BHE/Cdb rats. Am J Physiol. 1999;277:E702–7.
Horke S, Witte I, Wilgenbus P, Krüger M, Strand D, Förstermann U. Paraoxonase-2 reduces oxidative stress in vascular cells and decreases endoplasmic reticulum stress-induced caspase activation. Circulation. 2007;17(115):2055–64.
Horke S, Witte I, Wilgenbus P, Altenhöfer S, Krüger M, Li H, et al. Protective effect of paraoxonase-2 against endoplasmic reticulum stress-induced apoptosis is lost upon disturbance of calcium homoeostasis. Biochem J. 2008;416:395–405.
Devarajan A, Grijalva VR, Bourquard N, Meriwether 3rd D, Imaizumi S, Shin BC, et al. Macrophage paraoxonase 2 regulates calcium homeostasis and cell survival under endoplasmic reticulum stress conditions and is sufficient to prevent the development of aggravated atherosclerosis in paraoxonase 2 deficiency/apoE(−/−) mice on a western diet. Mol Genet Metab. 2012;107:416–27.
Shih DM, Xia YR, Yu JM, Lusis AJ. Temporal and tissue-specific patterns of PON3 expression in mouse: in situ hybridization analysis. Adv Exp Med Biol. 2009;660:73–87.
Reddy ST, Wadleigh DJ, Grijalva V, Ng C, Hama S, Gangopadhyay A, et al. Human paraoxonase-3 is an HDL-associated enzyme with biological activity similar to paraoxonase-1 protein but is not regulated by oxidized lipids. Arterioscler Thromb Vasc Biol. 2001;21:542–7.
Draganov DI. Lactonases with organophosphatase activity: structural and evolutionary perspectives. Chem Biol Interact. 2010;187:370–2.
Draganov DI, Teiber JF, Speelman A, Osawa Y, Sunahara R, La Du BN. Human paraoxonases (PON1, PON2, and PON3) are lactonases with overlapping and distinct substrate specificities. J Lipid Res. 2005;46:1239–47.
Shiner EK, Rumbaugh KP, Williams SC. Interkingdom signaling: deciphering the language of acyl homoserine lactones. FEMS Microbiol Rev. 2005;29:935–47.
Chun CK, Ozer EA, Welsh MJ, Zabner M, Greenberg EP. Inactivation of a Pseudomonas aeruginosa quorum-sensing signal by human airway epithelia. Proc Natl Acad Sci U S A. 2004;101:3587–90.
Stoltz DA, Ozer EA, Ng CJ, Yu JM, Reddy ST, Lusis A, et al. Paraoxonase-2 deficiency enhances Pseudomonas aeruginosa quorum sensing in murine tracheal epithelia. Am J Physiol Lung Cell Mol Physiol. 2007;292:L852–60.
Devarajan A, Bourquard N, Grijalva VR, Gao F, Ganapathy E, Verma J, et al. Role of PON2 in innate immune response in an acute infection model. Mol Genet Metab. 2013;110:362–70.
Kim JB, Xia YR, Romanoski CE, Lee S, Meng Y, Shi YS, et al. Paraoxonase-2 modulates stress response of endothelial cells to oxidized phospholipids and a bacterial quorum-sensing molecule. Arterioscler Thromb Vasc Biol. 2011;31:2624–33.
Schweikert EM, Amort J, Wilgenbus P, Förstermann U, Teiber JF, Horke S. Paraoxonases-2 and -3 are important defense enzymes against Pseudomonas aeruginosa virulence factors due to their anti-oxidative and anti-inflammatory properties. J Lipids. 2012;2012:352857.
Witte I, Foerstermann U, Devarajan A, Reddy ST, Horke S. Protectors or traitors: the roles of PON2 and PON3 in atherosclerosis and cancer. J Lipids. 2012;2012:342806.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Devarajan, A., Shih, D., Reddy, S.T. (2014). Inflammation, Infection, Cancer and All That…The Role of Paraoxonases. In: Camps, J. (eds) Oxidative Stress and Inflammation in Non-communicable Diseases - Molecular Mechanisms and Perspectives in Therapeutics. Advances in Experimental Medicine and Biology, vol 824. Springer, Cham. https://doi.org/10.1007/978-3-319-07320-0_5
Download citation
DOI: https://doi.org/10.1007/978-3-319-07320-0_5
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-07319-4
Online ISBN: 978-3-319-07320-0
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)