Abstract
The revolutionary advance of 3D printing technology is currently being tested in many medical applications due to its potential for unique patient-specific treatments. In orthopedics, 3D printing of fracture models can be used to improve the accuracy of fracture identification and classification, as well as for preoperative planning and training. For 3D models to be useful in traumatology, it is necessary that they be available in the limited preoperative time from patient admission to surgery. Our study is based on the proximal ‘hip fractures’ from the Stavanger University Hospital case study. Treatment of this type of fracture occurs within 24 h. Various print parameters in the post-processing software, including layer height, print time, and material consumption, are examined, and evaluated to ensure the optimal balance between 3D print time and print quality. Wrapping and removal of unaffected parts and the reduction of the 3D model size greatly minimize the printing time. Reducing excess information and connecting cylinders decreases print time significantly while still giving enough detail without losing fracture morphology. Other parameters including whether the use of printers with multiple extruders leads to a reduction in printing time, since the distance and size of support structures significantly affect the printing time, needs to be investigated in further studies.
Access provided by Autonomous University of Puebla. Download conference paper PDF
Similar content being viewed by others
Keywords
1 Introduction
The healthcare industry is only one of several industries that are being transformed by the development of 3D printing technology [1]. 3D printing technology has been increasingly used in the medical field in recent years, particularly for preoperative surgical planning [2], prosthetics [3], and organ replacement [4]. One of the main benefits of 3D printing in the medical area is the ability to produce individualized and customized medical devices patient specific implant (PSI) and implants [5, 6]. In orthopedics, 3D Printing of fracture models may improve the accuracy of fracture identification and classification compared to X-ray images for the surgeons, which could further assist in pre-surgical planning and teaching. Furthermore, it may reduce interobserver variability when using a 3D model to classify fractures compared to regular computerized tomography images. For 3D models to be of use in surgical planning in traumatology the time from the patient enters the emergency department to an accurate 3D model printed is limited depending on the fracture location. Here, we use proximal “hip” fractures at Stavanger University Hospital as “case studies”, (REK 2019/470). Thus, among the processes involved from patients entering the emergency department to surgery, (i.e., Digital Imaging and Communications in Medicine (DICOM) and corresponding segmentation processing), 3D Printing time occupies the highest time percentage. Even though there are many parameters to be optimized for general medical treatment when introducing 3D Printing, this work focuses on optimizing the parts to be printed through the removal of the section along with 3D Printer process parameters to reduce the printing time.
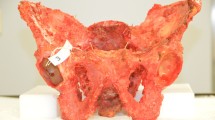
Hip fractures (Fig. 1) are common injuries with exponentially increased incidents in older adults. Hip fractures can cause serious disability, worse quality of life, and increased mortality (25% 1-year mortality) [7]. For effective and proper treatment planning, accurate classification of hip fractures is crucial, and 3D printing technology has become a valuable tool in this process. 3D printing can also help identify any unusual fracture patterns or complex fractures that may be difficult to classify using traditional methods. Based on imaging data, such as computerized tomography (CT) scans, 3D printing can produce precise models of hip fractures [8,9,10]. These models help surgeons understand the fracture pattern better depending on the fracture type, the best and most effective surgical technique can be chosen [10]. Moreover, 3D printed models can be used to inform patients and their families about the fracture and anticipated surgical process, which can reduce anxiety and enhance patient outcomes [11]. Additionally, surgical guides can be produced using 3D printing to help ensure the precise placement of implants and other hardware during surgery [12,13,14]. Being able to produce accurate fracture models using 3D printing, which are made available both within a time constraint and economically feasible, is important. A good model case to test the feasibility of 3D printing as an extra resource for surgical planning in an emergency setting is using hip fractures, as patients ideally should be on the operating table within 24 h of arriving at the emergency room [15, 16]. Thus, the 3D printed model of the patient’s hip fracture needs to be made readily available for the surgeons whilst they are planning the corrective procedure. Therefore, having a fast printing of the fracture while maintaining the anatomical accuracy of the part is necessary.
To do these different ways of optimizing techniques on the parameters of the parts as well as on the printers can be done. Among them, is the optimization of the fracture itself, where the focus will be made only on the fracture area. This can be done during the segmentation process where unnecessary parts which are not involved in the fracture or not necessary for understanding the anatomy such as the femur head will be cut out and removed, segmentation of the bone shaft close to the fracture area as much as possible and wrapping the bone shaft to reduce surface roughness (fracture-free) areas. Removing unnecessary parts of a hip bone model can help reduce printing time in cases of hip fracture by simplifying the 3D model and reducing its overall complexity. This can be done by segmenting the fracture region and isolating it from the surrounding unaffected bone. The segmentation process involves using specialized software to identify and separate the fractured region from the rest of the bone based on information from medical imaging scans such as CT or magnetic resonance imaging (MRI).
The second technique will focus on 3D printer settings and parameters optimization, including identification of proper printing layer height for faster printing, selection of nozzle diameter, and material consumption. In this study, fused deposition modeling (FDM) printing technology is used Fig. 2. This technology used is a type of additive manufacturing technology that involves the layering of a three-dimensional object using thermoplastic material extruded through a nozzle [17]. A print bed, a nozzle, and a filament feed mechanism are typical components of an FDM 3D printer. The filament feed mechanism feeds the thermoplastic filament into the printer's nozzle, which melts the filament and extrudes it onto the print bed in the desired shape. The printer's print bed moves up or down to build up the object layer by layer, and the extruded material solidifies as it cools, creating a solid object. FDM based 3D printers are commonly used for quick prototyping, model production, and the fabrication of functional parts. They are also commonly used in the medical field of orthopedics to create patient-specific implants, prostheses, and surgical guides [18]. FDM-based 3D printers are popular because of their versatility, low cost, and ease of use [19].
This article will assess the parameters of the FDM printer affecting the efficiency of the printed part based on the patient’s hip fracture also considering 3 different cases categorized in the segmentation process (part optimization). The highest severe (Complex) case is considered for this work.
2 Materials and Methods
Digital Imaging and Communications in Medicine (DICOM) image of the patient from the CT scan is imported to Materialise Mimics v24 and the fracture is segmented. Thus, imported to 3-Matic software to convert it to a 3D Model. The Severe case (9) based on the Hospital’s AO classification system of fracture is considered. Severe cases are expected to have longer 3D printing time than other fracture conditions as more fragments of the bone require more connecting rods. This condition directly affects the duration of 3D printing time.
In the first part, 3 different segmentation methods were considered on the 3D model to reduce 3D printing time:
-
i.
Normal condition (with head and not wrapped)
-
ii.
Head cut only (not wrapped)
-
iii.
Head cut and wrapping.
In the second part, different printer settings and parameters were assessed.
2.1 Fracture 3D Model Part Optimization
Three different 3D models (.stl files) according to the description of cases were prepared and 3D printed. To keep consistency, all models in the three cases were printed using the same 3D printing parameters. The printing parameter used was the 0.2-layer thickness, 10% infill density, and triangle infill pattern, whereas the printing speed was 70 mm/s with printers using 0.4 mm nozzle diameter. Cases are described below:
Case I - Normal condition (with head)
Figure 3 illustrates the normal segmentation condition considered as case 1. This case implies the full fracture site including the head of the femur where there is no fracture as well as no removal parts. One of the difficulties in orthopedic surgery is dealing with fracture segments that have detached from the bone. When these pieces are not appropriately stabilized and maintained together, they can lead to poor healing and possibly re-fracture. One way to fix this is to use segment cylinders, which are custom-designed devices that are inserted into the bone to hold the split bone segments together. The main location of the fracture, the fracture segments, and the highly porous bone areas found in the femur are shown in the below figure.
Case II - Head cut (Removal)
The second option that was suggested is to cut the head of the femur as seen below in Fig. 4. Typically, the femoral neck or intertrochanteric portion of the femur is the location of the primary fracture in a hip fracture [18]. The femoral neck is the portion of the femur bone that joins the bone's ball-shaped head to the main shaft, while the intertrochanteric region is located right below the femoral neck. These regions are essential for the stability and movement of the hip joint, and a fracture in either of them can have a profound effect on a patient's quality of life.
Case III - Wrapping of no fracture area (shaft and calcar) and femur head removal
The final case, as shown in Fig. 5 is when the wrapping of the bone shaft, was introduced in addition to the head cut. Wrapping the fractured bone involves isolating the fracture region and removing the unaffected parts of the bone from the 3D model. This can help to simplify the 3D model and reduce its complexity, which can potentially reduce the printing time. However, this depends on the specific case and the size and location of the fracture. Wrapping is done in Materialise Mimics segmentation software. The nature of the bone surface is rough which makes 3D printers stay longer to print the edges, it is assumed by smoothing the surface the retraction time of the 3D printer movement will decrease and that makes overall 3D printing timeless.
2.2 Study of the FDM 3D Printer Parameters
The experimental 3D printer used in this article is the Ultimaker S5. This is considered for the efficiency of the printer as well as the low cost of the 3D printer in general. The material selected for model printing is PLA, which is affordable and eco-friendly, and PVA for the support structure. Ultimaker’s Cura v5 slicer was used to check the parameters. Tested parameters are:
-
i.
Print time
-
ii.
Layer height
-
iii.
Material consumption
-
iv.
Nozzle diameter (0.4 mm and 0.8 mm).
The fixed printing parameters are given in Table 1.
3 Results and Discussion
3.1 Fracture 3D Model Part Optimization
By using the same printing parameters for a 0.4 mm nozzle and 0.2 mm layer height, the printing time for the 3D model after part optimization for the 3 cases is recorded from slicer software. Among the 3 cases, it is found that removing the head as well as wrapping reduces the time. This is directly related to the reduction of the file size (Table 2).
Removal of unaffected parts of the bone during fracture like cutting the femur head in this case, can greatly help to reduce the printing time. This is because the printing process will go more quickly because there will be less material to build and fewer details to print. The 3D model created when a fractured bone is segmented from a medical image has rough edges or surface imperfections due to the nature of the bone that needs to be smoothed out before printing. Also, this involves additional steps in the 3D modeling preparation for models’ geometry refinement. Wrapping helps simplify the 3D model and reduce complexity, which reduces the printing time. However, this depends on the specific case and the size and exact location of the fracture.
3.2 Study of the FDM 3D Printer Parameters
The layer height can be configured to be no more than 75% of the nozzle diameter for any specific print core or nozzle combination. Considering this, different layer height is given and the printing time for each case is recorded. The parameters are discussed below.
-
i.
Layer height vs print time (0.4 mm nozzle diameter).
Recorded data of the relation between layer height and print time for 0.4 mm is shown in Table 3.
The above experimental data (Fig. 6) result shows that there exists an increment in the height of the layer corresponding to a decrement in the printing time. Although the printing time and speed decrease with increasing layer thickness, the resulting model is rougher. This is because when the layer height drops, the printer head must make more passes to complete each layer. This indicates that printing the same thing takes longer than printing it with a thicker layer height. Furthermore, printing with thinner layers necessitates a higher level of precision and accuracy, which can extend printing time. The rate of change is increasing gradually.
-
ii.
Layer height vs material consumption.
The relation between the layer height and the material is shown in Fig. 7. Table 4 also illustrates the relation between the print time and layer height recorded.
Figure 8 shows the experimental data of print layer height, printing time, and consumables, and the relationship between layer height and print time, and consumables. The figure illustrates the evolution of the relationship between layer height, printing time, consumables, and precision over time. According to the figure presented, the results of the experiments indicate that the printing time is reduced to its minimum while still maintaining a high level of print quality when the layer height is set between 0.1 and 0.15 mm. The 3D Printing time between 0.1 mm and 0.15 mm for the complex (severe) case selected is between 13 h and 9.8 h, whereas the consumable material is almost similar for the cases.
3.3 Connecting Cylinders
Fracture fragments connecting cylinders (Fig. 9) can lengthen the printing process for a hip fracture model. The addition of these connecting cylinders to the fracture fragments in the 3D model ensures that the fracture fragments are kept in the proper places and simulate the true bone structure. However, including these connecting cylinders may complicate the 3D model, lengthening the print process. This is because a model with connected cylinders can require a longer print time than a simpler model because connecting cylinders require the printer to print more precise details, such as the shape and location of the cylinders. The number and size of fracture fragments in the model can also have an impact on print time. The model will demand more material to print and take longer to manufacture the larger the fracture fragments. Similarly, to this, the model will be more complex and take longer to print more fracture fragments it has.
Using fracture fragments to connect cylinders can make the printed model stronger and more stable, but it's important to consider how this will affect the 3D print time and cost. Depending on the needs of the hip fracture treatment, it may be better to make a simpler model without the cylinders in some situations.
4 Conclusion
It is seen that optimizing part itself plays an important role in a better 3D printing time, especially in a condition where there is a complex geometry like a hip fracture. It's important to note that reducing print time may also affect the quality and accuracy of the final print. Thus, finding the right balance between the print time and print quality to ensure the best possible outcomes for patients.
Wrapping and removal of unaffected parts greatly reduced the printing time. Reducing the size of the 3D model by removing the unaffected areas of the bone can help to speed up the printing process. This is because there will be less overall information to print and less specific information to print. Wrapping the fractured bone helps to reduce the complexity of the 3D model and makes it easier to print. However, wrapping the bone can also reduce the accuracy of the model and may not be suitable in cases where the unaffected parts of the bone are crucial for treatment planning.
One method for reducing the 3D print time for models of hip fractures is to simplify the model by lowering the number and size of fracture fragments as well as the quantity of connecting cylinders. To accomplish this, it demands only adding connecting cylinders to the most important fracture fragments and leaving the less important fragments without connecting cylinders.
References
Schubert, C., M.C. Van Langeveld, and L.A. Donoso, Innovations in 3D printing: a 3D overview from optics to organs. British Journal of Ophthalmology 98(2), 159–161 (2014).
Tejo-Otero, A., I. Buj-Corral, and F. Fenollosa-Artés, 3D printing in medicine for preoperative surgical planning: a review. Annals of biomedical engineering 48(2), 536–555 (2020).
Ventola, C.L., Medical applications for 3D printing: current and projected uses. Pharmacy and Therapeutics 39(10), 704 (2014).
Arslan-Yildiz, A., et al., Towards artificial tissue models: past, present, and future of 3D bioprinting. Biofabrication 8(1), 014103 (2016).
Wixted, C.M., et al., Three-dimensional printing in orthopaedic surgery: current applications and future developments. JAAOS Global Research & Reviews 5(4), (2021).
Han, Q., et al., Novel exploration of 3D printed wrist arthroplasty to solve the severe and complicated bone defect of wrist. Rapid Prototyping Journal, (2017).
Zanker, J. and G. Duque, Osteoporosis in older persons: old and new players. Journal of the American Geriatrics Society 67(4), 831–840 (2019).
Maryada, V.R., et al., pre-operative planning and templating with 3-D printed models for complex primary and revision total hip arthroplasty. Journal of Orthopaedics 34, 240–245 (2022).
Sallent, A., et al., Feasibility of 3D-printed models of the proximal femur to real bone: a cadaveric study. HIP International 29(4), 452–455 (2019).
Lim, P.K., et al., Use of 3D printed models in resident education for the classification of acetabulum fractures. Journal of surgical education 75(6), 1679–1684 (2018).
Bizzotto, N., et al., Three-dimensional printing of bone fractures: a new tangible realistic way for preoperative planning and education. Surgical Innovation 22(5), 548–551 (2015).
Kim, T., et al., Accuracy of a simplified 3D-printed implant surgical guide. The Journal of prosthetic dentistry 124(2), 195–201 (2020).
Henckel, J., et al., 3D-printed patient-specific guides for hip arthroplasty. JAAOS-Journal of the American Academy of Orthopaedic Surgeons 26(16), 342–348 (2018).
Bizzotto, N., et al., 3D printed models of distal radius fractures. Injury 47(4): 976–978 (2016).
Kjaervik, C., et al., Waiting time for hip fracture surgery: hospital variation, causes, and effects on postoperative mortality: data on 37,708 operations reported to the Norwegian Hip fracture Register from 2014 to 2018. Bone & joint open 2(9), 710–720 (2021).
Pincus, D., et al., Association between wait time and 30-day mortality in adults undergoing hip fracture surgery. Jama, 2017. 318(20): p. 1994–2003 (2017).
Wu, J. Study on optimization of 3D printing parameters. in IOP conference series: materials science and engineering. IOP Publishing (2018).
Sontakke, U. and S. Jaju, The Role of 3D Printing in the Biomedical Application: A Review. Smart Technologies for Energy, Environment and Sustainable Development, Vol 2: Select Proceedings of ICSTEESD: 371–381 (2020).
Hoy, M.B., 3D printing: making things at the library. Medical reference services quarterly 32(1), 93–99 (2013).
Woo, S.-H., et al., Three-dimensional-printing technology in hip and pelvic surgery: current landscape. Hip & pelvis 32(1),1–10 (2020).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2024 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this paper
Cite this paper
Adugna, Y.W. et al. (2024). Study on How 3D Printer Process Parameters Can Be Optimized for Use in Orthopedics Fracture Classification and Surgical Planning. In: Pavlou, D., et al. Advances in Computational Mechanics and Applications. OES 2023. Structural Integrity, vol 29. Springer, Cham. https://doi.org/10.1007/978-3-031-49791-9_10
Download citation
DOI: https://doi.org/10.1007/978-3-031-49791-9_10
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-49790-2
Online ISBN: 978-3-031-49791-9
eBook Packages: EngineeringEngineering (R0)