Abstract
Oral candidiasis is a common opportunistic infection caused by an overgrowth of Candida albicans. The microorganisms take advantage of poor oral hygiene or immunodeficiency to multiply and spread beyond normal levels. In this chapter, we provide a practical approach to assessing, diagnosing, and managing patients with oral candidiasis based on the literature and our clinical experience over the years.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Candida albicans
- Candidiasis
- Pseudomembranous candidiasis
- Erythematous candidiasis
- Acute atrophic candidiasis
- Rhomboid median glossitis
- Angular cheilitis
- Hyperplastic candidiasis
- Mucocutaneous candidiasis
Candidiasis is a disease caused primarily by the fungus Candida albicans and is of particular clinical importance in oral infections. The microorganisms take advantage of poor oral hygiene or immunodeficiency to multiply and spread beyond normal levels (Table 1). Despite relative therapeutic progress in the treatment of opportunistic fungal infectious diseases of the oral mucosa, the prevalence of these lesions has increased, especially in users of total dentures and patients with poor oral hygiene, transient immunodeficiencies, and chronic diseases, polypharmacy, oncology patients, and carriers of other systemic factors. The advent of new medical practices, such as immunosuppressive therapies, the use of broad-spectrum antibiotics, and invasive surgical procedures such as solid organ and bone marrow transplantation, has also contributed to this increase.
1 Clinical Characteristics
1.1 Pseudomembranous Candidiasis
-
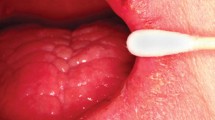
White pseudomembranes that are removed by scraping and exposing an underlying erythematous mucosa (Figs. 1 and 2).
-
On labial and buccal mucosa, gingiva, tongue, hard and soft palates, and oropharynx.
-
Predisposing factors:
-
Age (neonates/infants/elderly).
-
Diabetes mellitus.
-
Patients with HIV/AIDS.
-
Leukemia.
-
Users of steroid aerosol inhalers.
-
Systemic corticosteroids.
-
Broad-spectrum antibiotics and psychotropic drugs.
-
Terminally ill patients.
-
1.2 Erythematous candidiasis
1.2.1 Acute Atrophic Candidiasis
-
After a prolonged course of broad-spectrum antibiotic therapy.
-
It may be seen in xerostomia patients.
-
Often associated with a burning sensation in the oral cavity or on the tongue.
-
The tongue appears bright red and with depapillation.
1.2.2 Chronic Atrophic Candidiasis
-
Additionally, known as “denture stomatitis”.
-
Chronic erythema accompanied by petechial hemorrhage (Fig. 3 and 4).
-
In palatal and gingival tissues.
1.2.3 Rhomboid Median Glossitis
-
A chronic symmetrical area on the tongue (Fig. 3).
-
Anterior to the circumvallate papillae.
-
Consisting of atrophic filiform papillae.
-
Often associated with smoking and the use of inhaled steroids.
1.2.4 Angular Cheilitis
-
Erythematous fissure in one or both labial commissures (Fig. 3).
-
Usually, associated with an intraoral Candida infection.
-
Facial wrinkling, especially in elderly individuals with loss of vertical dimension, can lead to a constantly humid environment that predisposes the lesion to installation.
1.3 Chronic Hyperplastic Candidiasis
-
Known as Candidal leukoplakia.
-
Two types:
-
Homogeneous: smooth white lesions.
-
Heterogeneous: areas of erythema resulting in a speckled nodular appearance.
-
-
Frequent in the lip commissure and dorsum of the tongue.
-
Related to smoking habits.
1.4 Mucocutaneous Candidiasis
-
Rare condition.
-
Immune component present.
-
The degree of infection correlates with the severity of the immune defect.
-
Various clinical forms are seen on mucous membranes, skin, and nails (Fig. 5).
2 Diagnosis
-
Clinical features are the primary means of reaching a diagnosis.
-
Perform cytology or incisional biopsy in cases of nondetachable white plaques.
3 Treatment
3.1 First Line of Treatment
-
In all cases of oral candidiasis, reinforce maintenance of oral hygiene and/or dentures in cases of denture stomatitis.
-
In cases of denture stomatitis, guide patients to sleep without the denture. In cases of old prostheses (4–5 years or more), guide the patient to replace.
-
Correction of underlying conditions (HIV, diabetes, hyposalivation, etc.).
-
Cases of disseminated or nonresponsive candidiasis: investigate anemia, diabetes, or immunosuppression.
3.2 Second Line of Treatment
Before systemic administration, topical treatment should be employed.
-
Nystatin: Oral suspension (100,000 IU), 4 times a day for 7–14 days. Nystatin is presented in vials of 50 mL. Calculate how many vials the patient will need for the desired time of treatment. Usually, it is recommended to rinse the oral cavity with 10 mL four times a day, which results in 40 mL per day.
-
Miconazole: Oral gel (20 mg/mL), used from 5 (1 teaspoon) to 10 mL at a time, 4 times a day for a period of 7–14 days. In case of chronic atrophic candidiasis on the palate, apply at the base of the prosthesis (when a patient uses prosthesis). This way, we guarantee prolonged contact of the drug with the oral mucosa.
Directions for nystatin swabbing | |
|---|---|
Note 1: Instruct dentures to be removed before rinsing. Note 2: Remind the patient who, more important than “rinsing” the solution, is to leave it in contact with the lesion area for a long time because this potentiates the medication effect. Considering that the treatment is topical, the patient should not eat or drink for 30 minutes after using the medication. Note 3: If candidiasis extends to the oropharynx, the patient should swallow the nystatin. It is not absorbed. However, because its composition contains sugar, it should be used with caution or avoided in diabetic patients. |
3.2.1 Third Line of Treatment
Systemic administration should be used for cases that do not respond to topical treatment. In some cases, laboratory tests should be performed for systemic evaluation of the patient (complete blood count, fasting glycemia, platelet count, serum iron, folic acid, vitamin B2, and anti-HIV):
-
Ketoconazole: 200–400 mg daily for 7–14 days. Ketoconazole should be administered during one of the daily meals for maximum absorption. Presentation – Ketoconazole 200 mg tablet in a pack containing 10 and 30 tablets. Contraindications—It should not be administered to patients with acute or chronic liver pathology or to patients with known hypersensitivity to the drug.
-
Fluconazole: For oropharyngeal candidiasis, the usual dose is 50 mg–100 mg as a single dose daily for 7–14 days. When necessary, treatment can be continued for longer periods in patients with severely compromised immune function.
Disinfection of total or partial removable prostheses | |
|---|---|
Prosthesis without metal component: Place the prosthesis immersed in a glass of water with a tablespoon of sodium hypochlorite overnight. In the morning, wash the prosthesis with plenty of tap water before use. Prosthesis with metal component: Place the prosthesis immersed in a glass with 0.2% chlorhexidine digluconate solution overnight. In the morning, wash the prosthesis with plenty of tap water before use. Note: The solution of chlorhexidine digluconate is more concentrated than that used for chemical biofilm control because Candida penetrates the acrylic. Because of this, this solution must be manipulated. |
Sources
Akpan A. Oral candidiasis. Postgraduate Medical Journal. 2002;78(922):455–9.
Bensadoun RJ, Patton LL, Lalla RV, Epstein JB. Oropharyngeal candidiasis in head and neck cancer patients treated with radiation: update. Support Care Cancer. 2011;19:737–44.
Campisi G, Panzarella V, Matranga D, Calvino F, Lo Muzio L, Porter S. Risk factors for oral candidiasis: a twofold approach of study by fuzzy logic and traditional statistics. Arch Oral Biol. 2008;53:388–97.
Sitheeque MA, Samaranayake P. Chronic hyperplastic candidiasis/candidiasis (Candidal leukoplakia). Crit Rev Oral Biol Med. 2003;14(4):253–67.
Wiseman M. The treatment of oral problems in the palliative patient. J Can Dent Assoc. 2006;72:453–8.
Williams DK, Kuriyama T, Silva S, Malic S, Lewis MA. Candida biofilms and oral candidiasis: treatment and prevention. Periodontol 2000. 2011;55:250–65.
Williams David W, et al. Candida biofilms and oral candidiasis: treatment and prevention. Periodontol 2000. 2011;55(1):250–65.
Acknowledgments
The São Paulo State Research Foundation (FAPESP, São Paulo, Brazil, grant number JFS 19/09419-0) and the Coordination of Training of Higher Education Graduate Foundation (CAPES, Brasilia, Brazil, finance code 001). MDM and FPF are research fellow funded by the Brazilian National Council for Scientific and Technological Development (CNPq).
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Martins, M.D., Fonseca, F.P., Scarini, J.F., Innocentini, L.M.A.R. (2023). Oral Candidiasis. In: Santos-Silva, A.R., Lopes, M.A., Scarini, J.F., Vargas, P.A., Almeida, O.P.d. (eds) Clinical Decision-Making in Oral Medicine. Springer, Cham. https://doi.org/10.1007/978-3-031-14945-0_11
Download citation
DOI: https://doi.org/10.1007/978-3-031-14945-0_11
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-14944-3
Online ISBN: 978-3-031-14945-0
eBook Packages: MedicineMedicine (R0)