Abstract
The lung is a frequent target of autoimmune-mediated injury in patients with connective tissue diseases (CTDs) [1, 2]. Myositis, Systemic Lupus Erythematosus (SLE), Sjögren’s syndrome (SS), and Mixed Connective Tissue Disease (MCTD) can affect different levels of the respiratory tract, with a wide range of symptoms intensity, from asymptomatic to severe or life-threatening forms. Pleural disease is the most common lung manifestation in SLE and MCTD, while SS primarily affects the airways [3]. Myositis mostly affects the parenchyma, and interstitial lung disease (ILD) is the main lung manifestation of this disease [4]. However, ILD can also present in SLE, SS, and MCTD with different clinical presentations, ranging from minimal significant pulmonary restriction to severe progressive pulmonary fibrosis [5, 6].
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Connective tissue disease
- Interstitial lung disease
- Systemic lupus erythematosus (SLE)
- Sjögren’s syndrome (SS)
- Mixed connective tissue disease (MCTD)
- Myositis
- Antisynthetase syndrome
- Dermatomyositis
- Polymyositis
- Interstitial pneumonia with autoimmune features
Introduction
The lung is a frequent target of autoimmune-mediated injury in patients with connective tissue diseases (CTDs) [1, 2]. Myositis, Systemic Lupus Erythematosus (SLE), Sjögren’s syndrome (SS), and Mixed Connective Tissue Disease (MCTD) can affect different levels of the respiratory tract, with a wide range of symptoms intensity, from asymptomatic to severe or life-threatening forms. Pleural disease is the most common lung manifestation in SLE and MCTD, while SS primarily affects the airways [3]. Myositis mostly affects the parenchyma, and interstitial lung disease (ILD) is the main lung manifestation of this disease [4]. However, ILD can also present in SLE, SS, and MCTD with different clinical presentations, ranging from minimal significant pulmonary restriction to severe progressive pulmonary fibrosis [5, 6].
Lung involvement in CTDs is associated with a poor prognosis, leading to increased morbidity and mortality, and an altered quality of life. Early recognition and treatment are imperative issues to limit morbidity and mortality. In addition, clinicians must be aware of non-specific pulmonary complications, such as infection, pulmonary embolism, and left heart failure, which may coexist with specific lung manifestations and contribute to increased morbidity.
Diagnosis of a pulmonary involvement can be easy when occurring in patients with a previously diagnosed CTD or can be helped by the presence of clinical features suggestive of CTD. The close collaboration of pneumologists and rheumatologists is central to the assessment of any patient with a suspicion of CTD, particularly in patients with ILD [7]. Besides clinical expertise, the use of new diagnostic tools, such as ultrasound imaging, where rheumatologists developed specific expertise, may be useful to identify and characterize CTD in patients with respiratory disorders [8] or to screen for lung involvement in patients with CTD [9]. However, respiratory symptoms might occur before any other symptom, and features of CTD can manifest later during follow-up. Homma et al. observed that 19% of the patients with ILD developed CTDs over a period of one to 11 years [10]. These manifestations could be a direct consequence of the inflammatory disease, such as ILD, or an indirect lung involvement such as infections or drug toxicity.
In this review, we aim to provide a short overview of lung involvement of these four CTDs; SLE, SS, MCTD, and myositis. We focus mostly on describing the pulmonary manifestations, the pathophysiology, and the treatment strategies based on current literature.
Clinical Vignette
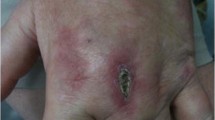
A 56-year-old female with no medical history was evaluated for increasing dyspnea over 3 weeks with hands and ankles inflammatory pain. Physical examination revealed heliotrope facial edema (Fig. 14.1a) with hands and fingers swelling (Fig. 14.1b). Bibasal crackles were heard. Blood tests revealed elevated creatine kinase. A chest computed tomography showed bilateral consolidation with ground glass opacities and a localized pneumothorax (Fig. 14.1c, d). Serology detected anti-nuclear antibodies 1/600, with anti-MDA5 positivity. A diagnosis of dermatomyositis was given. The patient was treated with corticosteroids and intravenous cyclophosphamide.
Systemic Lupus Erythematosus
Epidemiology
Systemic Lupus Erythematosus (SLE) is a chronic, systemic autoimmune disease that mostly affects young women. Classification criteria for SLE are presented in Fig. 14.2 [11]. SLE can present with a large spectrum of clinical manifestations in several organs (skin, joints, kidney, respiratory system), with a relapsing-remitting course [12]. The prevalence of SLE is 24/100,000, with an incidence of 1–8 cases/100,000 persons/year [13]. SLE can affect all lung compartments (Table 14.1); the pleura, the parenchyma, the airways, the pulmonary vasculature, and the respiratory muscles [14] with the prevalence of respiratory involvement throughout the course of the disease ranging from 20 to 90% [15, 16].
2019 European League Against Rheumatism (EULAR)/American College of Rheumatology (ACR) Classification Criteria for Systemic Lupus Erythematosus (SLE). (Modified from [11]). Anti-β2GPI anti–β2-glycoprotein I, anti-dsDNA anti–double-stranded DNA
Pathophysiology
Lupus pathophysiology)involves genetic and environmental factors, which lead to a break of immune tolerance, resulting in an aberrant immune response against endogenous nuclear antigens. Autoreactive B and T cells accumulate in secondary lymphoid organs and produce autoantibodies against multiple nuclear antigens, such as double-stranded DNA (dsDNA), RNP, Smith antigen, Ro, and La. These autoantibodies aggregate with the autoantigens and complement factors to form circulating immune complexes. The complexes deposit in target organs such as joints, skin, central nervous system, and/or kidneys to induce inflammation and tissue injury [17]. Lymphocytic and mononuclear interstitial and peribronchiolar infiltrates can be present in SLE-associated ILD. Pulmonary manifestations are generally associated with disease activity, hypocomplementemia, and increased levels of anti-dsDNA, while interstitial involvement has been associated with anti-Ro and anti-U1RNP antibodies, and with scleroderma traits [15, 18].
Antinuclear antibodies (ANAs) are positive in virtually all patients with SLE (usually 1:160 or higher), but are also often found in other autoimmune diseases, infections, neoplasia, drug exposure, and in healthy individuals, especially the elderly. Anti-dsDNA presents lower sensitivity (66–95%), but higher specificity, ranging from 75 to 100% and are linked to disease activity (Table 14.2). Anti-Smith (anti-Sm) are less sensitive (30%) but highly specific (over 95%). Anti-Ro (SSA), anti-La (SSB),)and anti-RNP antibodies are less specific markers, as they are positive in other autoimmune diseases [19]. Lupus-type circulating anticoagulants, anticardiolipin antibodies, and anti-B2GP1 antibodies are associated with antiphospholipid syndrome.
Pulmonary Manifestations
Pleural Disease
Pleural disease is the most common lung manifestation observed approximately in 60% of patients (50–83% in autopsy series) (Table 14.1) [20, 21].
Treatment choice for pleural disease depends on the severity of symptoms and the amount of liquid. Small asymptomatic effusions may not require specific treatment, while non-steroidal anti-inflammatory drugs and corticosteroids (prednisone dose 0.5 mg/kg) are mostly used when treatment is required [22]. In refractory cases, immunosuppressive and corticosteroid-sparing agents, such as azathioprine, mycophenolate mofetil, or methotrexate should be discussed. Chest tube drainage or pleurodesis are only rarely required for symptomatic relief of resistant disease.
Acute Lupus Pneumonitis and Diffuse Alveolar Hemorrhage
The most life-threatening lung manifestations are acute lupus pneumonitis and diffuse alveolar hemorrhage, which are observed only in a minority of patients (2–4%) [21]. A recent meta-analysis described potent risk factors correlated with increased risk of hemorrhage in SLE patients, such as neuropsychiatric involvement, nephritis, higher Systemic Lupus Erythematosus Disease Activity Index 2000 score, and low levels of C3 and C4 complement fractions, platelets, and hemoglobin [23].
Clinical data about treatment for acute immune-mediated lung injury associated with SLE are limited (no prospective controlled studies), and treatment strategies are based on other autoimmune conditions associated with pulmonary hemorrhage and acute pneumonitis. Corticosteroids are widely accepted as the first line of therapy, and intravenous pulses of corticosteroids are usually given (methylprednisolone 500 mg–1000 mg/day). Cyclophosphamide, rituximab, plasmapheresis, and intravenous immunoglobulins have been also used in critically ill patients [24].
Shrinking Lung Syndrome
The shrinking lung syndrome caused by diaphragmatic dysfunction, although well recognized, is a very rare manifestation [25].
There is no evidence for the optimal management of the shrinking lung syndrome. Corticosteroids and immunosuppressive agents, including azathioprine, mycophenolate mofetil, and rituximab, have been mainly used [26]. Individual cases have been improved with inhaled β-agonists [27], and theophylline [28].
Thrombotic Manifestations
Antiphospholipid syndrome is associated with SLE with a prevalence of 30% [29] and can be associated with thrombotic events, with or without pulmonary embolism in 35–42%, compared to 9% in patients with SLE alone [30]. Pulmonary embolism is an important entity to be considered in patients with SLE, and in that case, the initial management does not differ from the established guidelines. Thrombotic manifestations are mostly observed in patients who have secondary antiphospholipid syndrome [31]. Anticoagulant therapy, mainly with warfarin, is strongly recommended in antiphospholipid syndrome, due to the lack of evidence on novel oral anticoagulants. Pregnant women suffering from antiphospholipid syndrome require treatment with both aspirin and low molecular weight heparin throughout the pregnancy period.
Interstitial Lung Disease
Interstitial lung involvement has been found in about 15% of patients (Table 14.1). Non-specific interstitial pneumonia (NSIP), organizing pneumonia (OP), lymphocytic interstitial pneumonia (LIP), and less commonly, usual interstitial pneumonia (UIP) have been described [32]. Treatment of SLE-ILD is based on limited data and is mostly extrapolated from studies about other CTD-ILDs. The first-line treatment usually relies on corticosteroids, while mycophenolate mofetil or azathioprine are used as maintenance therapy. Rituximab and cyclophosphamide can be used in more severe cases [33].
Other Pulmonary Manifestations
Airways can be concerned in approximately 16% of the patients, mostly asymptomatic. Infection is the most common parenchymal disease observed in SLE, and it should always be excluded in patients with respiratory symptoms, particularly in patients under immunosuppressive therapy [34, 35]. Clinically significant pulmonary hypertension (PH) is a rare but severe complication of SLE, typically associated with scleroderma clinical features and anti-RNP antibodies [36,37,38].
Prognosis
SLE presents with a highly variable clinical course, while pulmonary infections and thrombotic events govern morbidity and mortality). PH also affects survival with two-year mortality just above 50%, but the most frequent causes of death are thromboses and infections [34, 38]. More rare causes associated with poor prognosis are acute lupus pneumonitis and diffuse alveolar hemorrhage, with mortality ranging from 50% to 90% despite treatment [39] (Table 14.3).
Sjögren’s Syndrome
Epidemiology
Sjӧgren’s Syndrome is a systemic autoimmune disease, the second most common after rheumatoid arthritis. It is characterized by impairment of the exocrine glands (mainly lacrimal and salivary glands) due to lymphocytic infiltration, and also extraglandular, visceral involvement (Table 14.4) [40, 41]. It has a clear female predominance, and it occurs either as a primary disorder or in association with other CTDs as secondary SS. SS has a prevalence of 20–100/100,000 and an incidence of 3.9/100,000. The prevalence of lung involvement is between 10–20%, although up to 65% of asymptomatic patients may have abnormal lung imaging [42, 43].
Pathophysiology
SS pathophysiology involves a combination of environmental, genetic, and hormonal influences, leading to autoimmune epithelitis, deregulated immune responses, and infiltration of B and T lymphocytes into affected tissues [44]. Triggered B-cells favor the secretion of anti-SSA and anti-SSB autoantibodies directed to small cytoplasmic RNP-bound peptides [45]. T-cells are also activated and involved in cytotoxic procedures. Lung involvement is associated with higher levels of circulating immune complexes and autoantibodies [46]. The main serum markers indicative of SS are anti-SSA and anti-SSB (Table 14.2). High levels of these antibodies, and also ANA, rheumatoid factor, hyper-γ-globulinaemia, as well as older age and smoking history, have been considered risk factors for pulmonary involvement [47, 48].
Pulmonary Manifestations
Airway Disorders
Airway disorders are common manifestations of SS (Table 14.1). Apart from upper airway disorders due to mucosal dryness and impaired mucociliary clearance, bronchiolitis and bronchiectasis are also frequently described in patients with SS (more than 20%) (Fig. 14.3a, b) [49, 50]. SS should be included in the differential diagnosis in a patient presenting with airway disorder (chronic cough or small airway disease) or pulmonary lymphoproliferative disorder. However, clinicians should be careful as lymphoma and amyloidosis can present with a LIP pattern on HRCT, and so tissue biopsy should be discussed on a case-by-case base.
Lymphoproliferative Disease
Patients with SS display a high risk for both nonneoplastic (e.g., nodular lymphoid hyperplasia, follicular bronchiolitis, lymphoid interstitial pneumonia), as well as neoplastic monoclonal lymphoproliferative disorders. The prevalence of lymphoma in SS ranges from 5% to 18% [51].
Approximately 6% of Sjögren-associated lymphomas involve the lungs and the most common types are the marginal zone B-cell lymphoma and mucosa-associated lymphoid tissue type [52, 53].
Such a lymphoproliferative involvement of the lungs in patients with SS can present as non-resolving consolidations, solitary or multiple nodules or masses, lymphadenopathy, and cystic lesions (Fig. 14.4). Given the increased risk for lymphoproliferative disorders, active clinical surveillance is recommended, especially for patients who are at high risk for lymphoma due to persistent salivary gland swelling, vasculitis and palpable purpura, lymphadenopathy, low C3 or C4 complement fraction, monoclonal gammopathy, cryoglobulins, anti-SSA and/or anti-SSB, rheumatoid factor, anemia, leukopenia, lymphopenia, neutropenia, thrombocytopenia, and elevated serum beta2-microglobulin [43, 54].
Lymphoma requires specific hematological treatment, and a multidisciplinary approach is suggested for diagnosis and management [43].
Interstitial Lung Disease
ILD is mainly considered to be developed later in the course of Sjögren’s syndrome, with a prevalence of 47% in 15 years; however, in 10–51% of patients, ILD may occur before other SS manifestations [42]. NSIP seems to be the prominent ILD pattern (45%), while UIP (16%), LIP (15%), and OP (7%) are less common, although a combined pattern is frequently described [55, 56]. The UIP pattern is associated with a progressive phenotype (Fig. 14.5a, b) [57].
With regard to the management of pulmonary disease in Sjögren’s syndrome, recent consensus guidelines were published shedding light on the optimal way of evaluation and treatment of these patients [43]. For patients presenting a mild disease with preserved lung function and minimal symptoms, a serial follow-up is recommended. In symptomatic or moderate-severe lung function impairment or/and HRCT findings, the first-line treatment including corticosteroids, followed by azathioprine or mycophenolate mofetil as corticosteroids sparing or as add-on agents is the suggested treatment strategy. In refractory or rapidly progressive cases, high doses of steroids as well as rituximab or cyclophosphamide should be considered [43]. Regarding corticosteroids, which are suggested as a first-line treatment, an initial daily dose of 0.5–1 mg/kg of prednisone has been suggested [58, 59]. The HRCT pattern can help predict the efficacy of treatment, as NSIP, OP, and LIP have been associated with a better response than the UIP pattern [58, 60]. In the case of an established UIP pattern, it is doubtful whether immunosuppressive treatment ameliorates lung fibrosis [61]. The use of tocilizumab in SS-ILD has been reported in a case of steroid-resistant OP [62].
Prognosis
Pulmonary involvement in SS seems to compromise severely the mortality risk, and in particular, the UIP pattern has been associated with worse survival [42] (Table 14.3). A rare complication of SS as PH or lymphoma also worsens prognosis, with an average 5-year survival in case of lymphoma to be 65–90% [38, 63].
Mixed Connective Tissue Disease
Epidemiology
Mixed Connective Tissue Disease (MCTD) is an autoimmune disorder characterized by the detection of serum anti-RNP antibodies associated with features of systemic sclerosis (SSc), SLE, and inflammatory myopathies [64, 65].
The prevalence of MCTD is 3.8/100,000 adults [66] while the annual incidence was 1.9/100,000 in a recent study in the USA [67]. Serositis is common, with an estimated incidence varying from 6% to 50%. ILD occurs in about 36% to 50% of patients and is severe in 19% [68, 69]. PH is a major clinical feature in MCTD, with a prevalence of 10–50% [70,71,72].
Pathophysiology
Autoantibody production may be driven by distinct subsets of HLA-restricted T cells and HLA DRB1*04: 01 was confirmed to be a major risk allele for MCTD [73]. Anti-U1-small nuclear ribonucleoprotein particle autoantibodies (anti-U1-snRNP) may be pathogenic by different mechanisms of action. First, it could bind to endothelial cells, to U1-RNP peptides presented by the MHC class II, or/and recognize fragments of nucleosome RNP in endothelial cell apoptotic blebs. Anti-U1-snRNP may also contribute to immune complexes that may activate the complement. A recent study proposed that the basophil/IgE/IL-4/CCL11 axis could be involved in the pathogenesis of MCTD, as activated basophils and autoreactive IgE to U1-snRNP were found in MCTD patients [74]. However, further studies are needed to better understand the pathophysiology of MCTD.
Anti-U1-snRNP antibodies are a mandatory criteria for diagnosis of MCTD (Table 14.5) [75]. Although highly sensitive (almost 100%), this marker is characterized by its low specificity and can be found in SLE [70]. Two factors are considered highly indicative of MCTD: the positive IgG anti-U1-RNP with negative IgM anti-U1-RNP and the elevated 70 k anti-U1-RNP titers [76]. In MCTD, the anti-DNA positivity could predict drift to SLE, while rheumatoid factor and anti-CCP seem to associate with arthritis. Anti-U1RNP positivity may be a predictor of more aggressive erosive arthritis [70].
Pulmonary Manifestations
Pulmonary Hypertension
PH is frequently observed during the course of MCTD (Table 14.1) and can be classified into group 1, pulmonary arterial hypertension, or group 3, as a consequence of ILD according to the World Health Organization classification. Among CTDs, MCTD was found to be the most commonly associated with pulmonary arterial hypertension in a Japanese study [77]. In the national UK registry study, 8% of the pulmonary arterial hypertension-CTD patients presented MCTD compared to 74% presenting systemic scleroderma [78].
There are no specific guidelines for the treatment of PH associated with MCTD, and the treatment options are derived from studies of pulmonary arterial hypertension-specific therapies in idiopathic pulmonary arterial hypertension. In group 1 PH, endothelin receptor antagonists (bosentan, ambrisentan), phosphodiesterase 5 inhibitors (sildenafil, tadalafil), and prostanoids (intravenous epoprostenol, subcutaneous treprostinil, nebulized iloprost) could be discussed according to the prognostic risk calculation. Compared to idiopathic/heritable pulmonary arterial hypertension, patients with CTD respond poorly to treatment [79] and have a worse prognosis. Aggressive up-front combination therapy with ambrisentan and tadalafil has been shown to reduce the risk of clinical failure compared to monotherapy [80] and could be the ideal option in CTD-PH patients.
Interstitial Lung Disease
MCTD-associated ILD affects up to 60% of patients, is usually slowly progressive, and is associated with increased mortality (Figs. 14.6 and 14.7). No controlled data are available, but immunosuppressive treatments are commonly suggested, including corticosteroids and immunosuppressive therapies, such as azathioprine, mycophenolate mofetil, cyclosporine, and methotrexate. Intravenous cyclophosphamide should be considered in severe ILD [69, 81, 82].
Prognosis
The most common cause of death is PH followed by severe infections due to immunosuppressive therapies [83]. Data on the course and outcome of ILD in MCTD are limited. A study has calculated the 5-year survival rates for <5% ILD extent to be 94%, compared to 82% for >5%. Common risk factors for ILD progression in MCTD is male gender, high anti-RNP antibody titer, presence of anti-Ro-52 antibodies, and no prior arthritis (Table 14.3) [68, 84].
Myositis
Epidemiology
Myositis, also known as idiopathic inflammatory myopathies, is a group of rare autoimmune diseases characterized by skeletal muscle inflammation, associated with frequent extramuscular signs such as arthritis, Raynaud’s phenomenon, mechanic’s hands, and interstitial lung disease (ILD) (Table 14.6) [85]. Myositis is a heterogenous group of CTDs composed of polymyositis (PM), dermatomyositis (DM), clinically amyopathic dermatomyositis and anti-synthetase syndrome [6, 86].
Due to this highly heterogeneous nature of myositis, along with the lack of clear diagnostic criteria, epidemiological data are scarce. Based on current data, myositis are rare, with a prevalence ranging from 2.4 to 33.8 per 100,000 inhabitants, and an annual incidence ranging from 1.16 to 19 per million worldwide [87].
Pathophysiology
Pathophysiology of anti-histidyl-tRNA synthetase, also known as an anti-Jo1 positive anti-synthetase syndrome, is best described. It can be favored by environmental exposure, such as tobacco, airborne contaminants and mineral particles, or by respiratory tract infections. These factors lead to aggression of lung tissue, and to a break of immune tolerance [88]. Innate immune cells such as NK lymphocytes are unspecifically activated and release proteolytic enzymes. The release of histidyl-tRNA-synthetase, an antigen that has immune properties, then leads to the recruitment of immune cells, with CD8-T cell priming and CD4-T cell-B cell crosstalk, with the production of anti-histidyl-tRNA synthetase autoantibody. Genetic factors can also be involved, such as HLA-B*08.01. The propagation of the disease to other organs remains poorly explained [89].
Measurement of myositis-associated antibodies and myositis-specific antibodies levels is required in the initial evaluation of ILD, especially in the presence of skin or muscle clinical features (Table 14.2). The negativity of antinuclear autoantibodies does not rule out the presence of myositis-associated antibodies or myositis-specific antibodies [90].
Patients with the anti-synthetase syndrome are clinically characterized by arthritis, Raynaud’s phenomenon, mechanics hands, and fever, but can also present with isolated ILD [91, 92].
The anti-synthetase antibodies (anti-Jo1, anti-PL7, anti-PL12, anti-KS, anti-OJ, anti-EJ, anti-SC, anti-JS, anti-YRS, anti-Zo) targeting the aminoacyl-tRNA synthetase enzyme are the most frequently found myositis-specific antibodies, occurring on average in 20% of PM patients and 29% of DM patients (Table 14.2). Anti-PL-7 appears to be associated with ILD preceding the diagnosis of myositis, and anti-PL12 patients have a higher rate of isolated ILD [92]. Anti-MDA5 antibody (previously known as anti-CADM-140) is a myositis-specific antibody associated with pulmonary involvement and is a risk factor for severe and rapidly progressive ILD, with increased mortality [93, 94]. Moreover, it is associated with a higher likelihood of having clinically amyopathic dermatomyositis [95]. Anti-MDA5 antibody detection identifies a subgroup of patients characterized by dermatomyositis skin rash, skin ulcers, calcinosis, mechanic’s hands, ILD, arthralgia/arthritis, and a high mortality rate [96].
Anti-PM-Scl and anti-Ku are two myositis-associated antibodies associated with a high prevalence of ILD, ranging from 38 to 78% for anti-PM-Scl and 27% for anti-Ku [93].
Pulmonary Manifestations and Treatments
Interstitial Lung Disease
ILD is the most frequent and severe extramuscular involvement of myositis, leading to a significant increase in mortality [4, 97]. A prevalence varying between 19.9 and 86% was reported, representing one of the highest prevalence among CTDs (Table 14.1) [98,99,100]. ILD is particularly frequent in patients with anti-tRNA synthetase [101, 102], anti-MDA5 [49], and anti-PM-Scl antibodies [103,104,105].
ILD is responsible for estimated excess mortality of 50% in some series [4, 97] and may precede muscular manifestations in up to 20% of cases [106]. Muscular involvement can be subtle or even absent. Rapidly progressive ILD is associated with a poorer prognosis, with a 68% mortality at 3 months (Table 14.3) [107,108,109,110].
The most frequent pattern observed on HRCT is an association of consolidations, corresponding to areas of OP, and NSIP features, with bilateral ground-glass opacities, reticulation, and peribronchovascular thickening mostly affecting lower lobes (Fig. 14.8) [111,112,113]. These features correspond histologically to an overlap pattern of OP and NSIP patterns [114, 115]. HRCT features of ILD are usually unspecific to a subset of myositis.
Organizing pneumonia pattern with consolidation with a peribronchovascular predominance in both lower lobes (Panel a) in a patient with anti-glycyl-tRNA synthetase antibody (anti-EJ). With corticosteroids, there was a resolution of consolidation with residual ground glass opacities and bronchial distortions (panel b)
Due to the low prevalence of the disease and the high variability in clinical presentation, there is no guideline regarding the treatment of ILD associated with myositis. The choice of immunosuppressive therapy should distinguish between rapidly progressive forms or acute forms associated with respiratory failure, and slowly progressive forms. In rapidly progressive forms or in acute respiratory failure an aggressive treatment should be considered as a first-line treatment, associating high-dose corticosteroids with cyclophosphamide, rituximab, or a calcineurin inhibitor. In patients with mild disease or chronic presentation, corticosteroids alone or in association with mycophenolate mofetil or azathioprine could be proposed [99, 116].
Corticosteroids represent the cornerstone of the initial treatment of myositis-ILD and are generally used as a first-line strategy [4, 117]. An oral administration of 0.5–1 mg/kg of prednisone for 4–8 weeks is usually admitted, followed by progressive tapering with a duration of treatment that generally exceeds 24 months. In chronic presentations or slowly progressive forms of ILD, a recent meta-analysis reported an improvement rate of 89.2% (95%CI 89.2–93.6) with corticosteroids alone [107]. However, prednisone-resistance is frequent. Corticosteroids alone show a response rate of 50%, suggesting that combined use of immunosuppressive therapies should be preferred in rapidly progressive cases [118,119,120]. In a retrospective study, two treatment approaches were compared: an association of immunosuppressive treatment (cyclosporine, cyclophosphamide, azathioprine, or tacrolimus) and prednisone at the treatment initiation (intensive approach), or the adjunction of immunosuppressive therapy when prednisone alone had no favorable response (step-up approach). The intensive approach was associated with better survival [121]. In patients showing initially elevated serum levels of muscle enzymes (creatine phosphokinase), it has been suggested that tapering of corticosteroids should be initiated once enzymes return to normal levels.
Immunosuppressive therapies should be considered in relapsing diseases, or as corticosteroid-sparing agents. Data supporting the effectiveness of azathioprine and mycophenolate mofetil, as maintenance therapy after induction or for patients with mild ILD, are limited to small case series and case reports. Mira-Avendano et al., reported the same efficacy on clinical and functional stabilization and corticosteroids daily dose tapering, for oral cyclophosphamide, azathioprine, and mycophenolate mofetil in PM/DM-ILD and anti-synthetase syndrome-ILD [60]. In a recent retrospective study on 66 patients with myositis-associated ILD treated with azathioprine and 44 with mycophenolate mofetil, a significant improvement was observed in FVC (%) with both drugs, and DLCO (%) with azathioprine, allowing a tapering of corticosteroids daily dose [122].
Methotrexate is mostly used in case of rheumatic manifestations of myositis. It has been used for the treatment of myositis-associated ILD despite the absence of pulmonary-specific evidence, with a good safety profile.
Many retrospective studies, regarding both cyclosporine and tacrolimus, suggested that calcineurin-inhibitors may be useful in treating myositis-ILD. Tacrolimus might have an effect on functional and clinical improvement, as well as muscle strength improvement, especially in patients who did not respond to first-line corticosteroid treatment, with a decrease of prednisone daily dose [123, 124]. Cyclosporine could be suggested in chronic ILD associated with myositis, with a favorable outcome observed when associated with corticosteroids. In acute forms, cyclosporine is associated with a favorable outcome in polymyositis-ILD and in half of ILD associated with dermatomyositis patients, with a better survival rate when cyclosporine and prednisone were associated [125].
The use of cyclophosphamide is currently limited to the aggressive, rapidly progressive, or refractory forms of myositis-associated ILD with an improvement in survival. A systematic review of 12 studies published in 2015 supported the use of cyclophosphamide in myositis- ILD, with 58% (34 of 59) of patients showing an improvement in survival rate. In a recent meta-analysis, the global 3-month survival rate was 72.4% (95%CI 6.4–99.0) in rapidly progressive cases [107].
In myositis-ILD, rituximab was shown to have a role as a second-line treatment for refractory ILD in several retrospective studies, with a functional, imaging, and/or clinical improvement [126,127,128,129]. Overall, rituximab appears as a drug of choice in the management of refractory myositis-ILD and rapidly progressive ILD. Prospective randomized trials are ongoing to assess the efficacy and tolerability of rituximab in CTD-ILD [130, 131].
Intravenous immunoglobulin combined with steroids is effective in improving muscle strength and decreasing creatine kinase levels in patients with active muscle disease. Data suggesting a benefit in ILD are scarce [132, 133]. However, intravenous immunoglobulin could be discussed in patients with refractory disease associated with muscular involvement or with marked contraindications to immunosuppressive agents.
Respiratory Muscle Weakness
Respiratory muscle weakness is a rare but potentially life-threatening complication that can develop independently from skeletal muscle weakness. The management of respiratory muscle involvement is similar to that of peripheral muscle or extramuscular involvement and mostly relies on immunosuppressive therapies [134, 135]. In a retrospective series of 18 patients with respiratory muscle involvement leading to a restriction, an 83% remission rate was observed after treatment with corticosteroids or immunosuppressive therapies (azathioprine, cyclosporine) [136]. Intravenous immunoglobulin can also be rapidly effective in muscular involvement. In severe patients, close monitoring in the intensive care unit for possible noninvasive mechanical ventilation can be necessary.
Other Pulmonary Manifestations
Other pulmonary conditions can be observed during myositis, although with a lower frequency. PH can be observed with a low prevalence, as a consequence of ILD in most cases (group 3), although anecdotal cases of myositis-associated pulmonary arterial hypertension in the absence of ILD (group 1) were also reported [137]. Pleural effusion is also a rare complication of myositis, mostly observed in dermatomyositis.
Prognosis
Myositis-ILD is associated with significant morbidity and mortality. Mean overall mortality related to ILD is 14%, and retrospective studies have shown 10-year survival rates between 71 and 89%. Mortality is greatly increased in rapidly progressive ILD compared to chronic forms, with mortality at 3 months of 68% [138, 139].
The type of myositis and myositis-specific autoantibody is correlated with outcome (Table 14.3). Thus, patients with anti-PM/Scl autoantibodies tend to have less severe lung involvement than those with anti-synthetase antibodies and present relatively low mortality related to ILD (0–11%) [104].
A recent study identified acute/subacute presentations of ILD, older age, lower FVC, and clinically amyopathic dermatomyositis as predictors associated with higher mortality in myositis-ILD. In that study, more than 25% of patients died in the follow-up period [140]. HRCT pattern also seems to be related to outcome, with OP associated with a better prognosis than NSIP or UIP [141].
Moreover, treatment response and prognosis are variable among patients. Polymyositis-ILD is associated with a better response than dermatomyositis-ILD [123, 140]. An anti-MDA5 antibody is associated with corticosteroid resistance and poor prognosis (Fig. 14.9). Anti-aminoacyl tRNA synthetase antibodies are characterized by a greater response to corticosteroids, although associated with a greater risk of relapse (Table 14.3) [124, 142]. The use of JAK inhibitors for the treatment of myositis-ILD is of growing interest because of the potential anti-inflammatory and anti-fibrotic properties of these molecules [143], with small series and case reports suggesting that these molecules might be of interest in refractory cases and in rapidly progressive ILD [144], particularly when associated with an anti-MDA5 antibody [145].
Rapidly progressive pneumonitis in a 22 years-old patient with anti-MDA5 antibody. Very subtle ground glass opacities were observed at diagnosis (Panel a) which progressed to diffuse opacities and acute respiratory failure within 6 weeks, despite high dose corticosteroids and cyclophosphamide (panel b). The patient’s condition required an emergency lung transplantation
Other Therapeutic Options in CTD-ILD
Antifibrotic Therapy
The currently available antifibrotic drugs are under investigation as promising candidates for the management of CTD-ILD patients, mainly focusing on progressive fibrotic phenotypes. Recently, the INBUILD trial assessed the efficacy and safety of nintedanib in non-IPF progressive fibrosing ILDs despite conventional therapies [146]. The use of nintedanib was associated with a slower decline of lung function in patients with progressive fibrotic ILDs, compared to placebo, with non-significant differences in the efficacy of nintedanib across ILD subgroups [146]. Additionally, patients with unclassifiable ILD, including IPAF, were randomized to pirfenidone or placebo in a recent trial. The analysis of secondary endpoints suggested that pirfenidone may reduce lung function decline in unclassifiable progressive fibrotic ILD [147]. Similarly, pirfenidone was associated with a reduced decline of FVC in patients with progressive pulmonary fibrosis in the RELIEF trial which included some patients with CTD-ILD [148]. More data are needed to clarify the benefit of antifibrotic drugs and to investigate the optimal combination with immunosuppressive therapy.
Lung Transplantation
It remains controversial whether patients with CTD-ILD are eligible for lung transplantation [79]. It is generally believed that due to extrapulmonary disease and a higher risk for allograft rejection, these patients have increased mortality after transplantation [80, 81]. However, recently, several studies have shed light on the role of lung transplantation in scleroderma and non-scleroderma-associated ILD [149]. Selected patients should be considered eligible for transplantation when there is progressive pulmonary disease despite the appropriate immunosuppressive therapy when the systemic component of the disease is well controlled [150, 151]. A recent study suggested that adjusted survival was not significantly different among subgroups of myositis-associated ILD patients compared with IPF patients after lung transplantation [149]. There is emergent evidence to support emergency lung transplantation in patients with rapidly progressive ILD associated with anti-MDA5 antibody [152].
Conclusion
Myositis, SLE, SS, and MCTD can affect almost the entire respiratory tract. However, several differences exist mainly regarding the reversibility of lung disease and the prognosis. Pleural effusion in SLE, ILD in myositis, and airway disease in SS represent frequent lung-associated manifestations. ILD and pulmonary hypertension in all these diseases are mainly associated with morbidity and mortality. Diagnosis relies on pulmonary function tests, HRCT, and serological testing. Immunosuppressive agents and steroids are the main treatments to date although randomized trials are lacking. Data regarding long-term follow-up are lacking but it is of great importance to identify patients having a high risk for disease progression and initiate early treatment. Several factors and biomarkers have been proposed to be related to the severity and prognosis of ILD in CTDs, but further research should validate these data in order to evaluate possible pathogenetic associations [153, 154].
References
Papiris SA, Manali ED, Kolilekas L, Kagouridis K, Maniati M, Borie R, et al. Investigation of lung involvement in connective tissue disorders. Respiration. 2015;90(1):2–24.
Duchemann B, Annesi-Maesano I, Jacobe de Naurois C, Sanyal S, Brillet P-Y, Brauner M, et al. Prevalence and incidence of interstitial lung diseases in a multi-ethnic county of greater Paris. Eur Respir J. 2017;50(2):1602419.
Antoniou KM, Vasarmidi E, Trachalaki A, Bibaki E, Crestani B. Pulmonary involvement in systemic lupus erythematosus, Sjögren syndrome and mixed connective tissue disease. In: Wuyts WA, Cottin V, Spagnolo P, Wells AU, editors. Pulmonary manifestations of systemic diseases [internet]. Sheffield: European Respiratory Society; 2019. p. 106–23. https://doi.org/10.1183/2312508X.10014319.
Cottin V, Thivolet-Béjui F, Reynaud-Gaubert M, Cadranel J, Delaval P, Ternamian PJ, et al. Interstitial lung disease in amyopathic dermatomyositis, dermatomyositis and polymyositis. Eur Respir J. 2003;22(2):245–50.
Barba T, Mainbourg S, Nasser M, Lega J-C, Cottin V. Lung diseases in inflammatory myopathies. Semin Respir Crit Care Med. 2019;40(2):255–70.
Cottin V, Barba T, Mainbourg S, Nasser M, Valenzuela C, Lega J-C. Pulmonary involvement in inflammatory myopathies. In: Wuyts WA, Cottin V, Spagnolo P, Wells AU, editors. Pulmonary manifestations of systemic diseases [internet]. Sheffield: European Respiratory Society; 2019. p. 68–89. https://doi.org/10.1183/2312508X.10014119.
Ottaviani S, Khaleche S, Borie R, Debray M-P, Dieudé P, Crestani B. Rheumatological evaluation of patients with interstitial lung disease. Scand J Rheumatol. 2022;51(1):34–41.
Lesturgie-Talarek M, Goossens J, Berkani S, Forien M, Juge P-A, Ebstein E, et al. Salivary gland ultrasonography in patients with connective tissue diseases: a multi-center observational study. Rheumatology (Oxford). 2021;61:keab907.
Antoniou KM, Tzilas V, Vasarmidi E, Symvoulakis EK, Tzouvelekis A, Bouros D. Interstitial lung abnormalities: ignotum per ignotius. Lancet Respir Med. 2019;7(5):376–8.
Homma Y, Ohtsuka Y, Tanimura K, Kusaka H, Munakata M, Kawakami Y, et al. Can interstitial pneumonia as the sole presentation of collagen vascular diseases be differentiated from idiopathic interstitial pneumonia? Respiration. 1995;62(5):248–51.
Aringer M, Costenbader K, Daikh D, Brinks R, Mosca M, Ramsey-Goldman R, et al. 2019 European league against Rheumatism/American college of rheumatology classification criteria for systemic lupus erythematosus. Arthritis Rheumatol. 2019;71(9):1400–12.
Amarnani R, Yeoh S-A, Denneny EK, Wincup C. Lupus and the lungs: the assessment and management of pulmonary manifestations of systemic lupus erythematosus. Front Med (Lausanne). 2020;7:610257.
Abu-Shakra M, Urowitz MB, Gladman DD, Gough J. Mortality studies in systemic lupus erythematosus. Results from a single center. I. Causes of death. J Rheumatol. 1995;22(7):1259–64.
Toyoda Y, Koyama K, Kawano H, Nishimura H, Kagawa K, Morizumi S, et al. Clinical features of interstitial pneumonia associated with systemic lupus erythematosus. Respir Investig. 2019;57(5):435–43.
Alamoudi OSB, Attar SM. Pulmonary manifestations in systemic lupus erythematosus: association with disease activity. Respirology. 2015;20(3):474–80.
Kim JS, Lee KS, Koh EM, Kim SY, Chung MP, Han J. Thoracic involvement of systemic lupus erythematosus: clinical, pathologic, and radiologic findings. J Comput Assist Tomogr. 2000;24(1):9–18.
Kaul A, Gordon C, Crow MK, Touma Z, Urowitz MB, van Vollenhoven R, et al. Systemic lupus erythematosus. Nat Rev Dis Primers. 2016;2:16039.
Alharbi S, Ahmad Z, Bookman AA, Touma Z, Sanchez-Guerrero J, Mitsakakis N, et al. Epidemiology and survival of systemic sclerosis-systemic lupus erythematosus overlap syndrome. J Rheumatol. 2018;45(10):1406–10.
Goldblatt F, O’Neill SG. Clinical aspects of autoimmune rheumatic diseases. Lancet. 2013;382(9894):797–808.
Jawad H, McWilliams SR, Bhalla S. Cardiopulmonary manifestations of collagen vascular diseases. Curr Rheumatol Rep. 2017;19(11):71.
Keane MP, Lynch JP. Pleuropulmonary manifestations of systemic lupus erythematosus. Thorax. 2000;55(2):159–66.
Wang D-Y. Diagnosis and management of lupus pleuritis. Curr Opin Pulm Med. 2002;8(4):312–6.
Xu T, Zhang G, Lin H, Xie Y, Feng Y, Zhang X, et al. Clinical characteristics and risk factors of diffuse alveolar hemorrhage in systemic lupus erythematosus: a systematic review and meta-analysis based on observational studies. Clin Rev Allergy Immunol. 2020;59(3):295–303.
Martínez-Martínez MU, Oostdam DAH, Abud-Mendoza C. Diffuse alveolar hemorrhage in autoimmune diseases. Curr Rheumatol Rep. 2017;19(5):27.
Smyth H, Flood R, Kane D, Donnelly S, Mullan RH. Shrinking lung syndrome and systemic lupus erythematosus: a case series and literature review. QJM. 2018;111(12):839–43.
Duron L, Cohen-Aubart F, Diot E, Borie R, Abad S, Richez C, et al. Shrinking lung syndrome associated with systemic lupus erythematosus: a multicenter collaborative study of 15 new cases and a review of the 155 cases in the literature focusing on treatment response and long-term outcomes. Autoimmun Rev. 2016;15(10):994–1000.
Warrington KJ, Moder KG, Brutinel WM. The shrinking lungs syndrome in systemic lupus erythematosus. Mayo Clin Proc. 2000;75(5):467–72.
Van Veen S, Peeters AJ, Sterk PJ, Breedveld FC. The « shrinking lung syndrome » in SLE, treatment with theophylline. Clin Rheumatol. 1993;12(4):462–5.
Levine JS, Branch DW, Rauch J. The antiphospholipid syndrome. N Engl J Med. 2002;346(10):752–63.
Somers E, Magder LS, Petri M. Antiphospholipid antibodies and incidence of venous thrombosis in a cohort of patients with systemic lupus erythematosus. J Rheumatol. 2002;29(12):2531–6.
Wahl DG, Guillemin F, de Maistre E, Perret C, Lecompte T, Thibaut G. Risk for venous thrombosis related to antiphospholipid antibodies in systemic lupus erythematosus–a meta-analysis. Lupus. 1997;6(5):467–73.
Cheema GS, Quismorio FP. Interstitial lung disease in systemic lupus erythematosus. Curr Opin Pulm Med. 2000;6(5):424–9.
Lim SW, Gillis D, Smith W, Hissaria P, Greville H, Peh CA. Rituximab use in systemic lupus erythematosus pneumonitis and a review of current reports. Intern Med J. 2006;36(4):260–2.
Cervera R, Khamashta MA, Font J, Sebastiani GD, Gil A, Lavilla P, et al. Morbidity and mortality in systemic lupus erythematosus during a 10-year period: a comparison of early and late manifestations in a cohort of 1,000 patients. Medicine (Baltimore). 2003;82(5):299–308.
Noël V, Lortholary O, Casassus P, Cohen P, Généreau T, André MH, et al. Risk factors and prognostic influence of infection in a single cohort of 87 adults with systemic lupus erythematosus. Ann Rheum Dis. 2001;60(12):1141–4.
Swigris JJ, Fischer A, Gillis J, Gilles J, Meehan RT, Brown KK. Pulmonary and thrombotic manifestations of systemic lupus erythematosus. Chest. 2008;133(1):271–80.
Li M, Wang Q, Zhao J, Li Z, Ye Z, Li C, et al. Chinese SLE treatment and research group (CSTAR) registry: II. Prevalence and risk factors of pulmonary arterial hypertension in Chinese patients with systemic lupus erythematosus. Lupus. 2014;23(10):1085–91.
Zhao J, Wang Q, Liu Y, Tian Z, Guo X, Wang H, et al. Clinical characteristics and survival of pulmonary arterial hypertension associated with three major connective tissue diseases: a cohort study in China. Int J Cardiol. 2017;236:432–7.
Schwab EP, Schumacher HR, Freundlich B, Callegari PE. Pulmonary alveolar hemorrhage in systemic lupus erythematosus. Semin Arthritis Rheum. 1993;23(1):8–15.
Shiboski CH, Shiboski SC, Seror R, Criswell LA, Labetoulle M, Lietman TM, et al. 2016 American College of Rheumatology/European league against Rheumatism classification criteria for primary Sjögren’s syndrome: a consensus and data-driven methodology involving three international patient cohorts. Ann Rheum Dis. 2017;76(1):9–16.
Ferro F, Marcucci E, Orlandi M, Baldini C, Bartoloni-Bocci E. One year in review 2017: primary Sjögren’s syndrome. Clin Exp Rheumatol. 2017;35(2):179–91.
Sambataro G, Ferro F, Orlandi M, Sambataro D, Torrisi SE, Quartuccio L, et al. Clinical, morphological features and prognostic factors associated with interstitial lung disease in primary Sjӧgren’s syndrome: a systematic review from the Italian Society of Rheumatology. Autoimmun Rev. 2020;19(2):102447.
Lee AS, Scofield RH, Hammitt KM, Gupta N, Thomas DE, Moua T, et al. Consensus guidelines for evaluation and management of pulmonary disease in Sjögren’s. Chest. 2021;159(2):683–98.
Lessard CJ, Li H, Adrianto I, Ice JA, Rasmussen A, Grundahl KM, et al. Variants at multiple loci implicated in both innate and adaptive immune responses are associated with Sjögren’s syndrome. Nat Genet. 2013;45(11):1284–92.
Cornec D, Devauchelle-Pensec V, Tobón GJ, Pers J-O, Jousse-Joulin S, Saraux A. B cells in Sjögren’s syndrome: from pathophysiology to diagnosis and treatment. J Autoimmun. 2012;39(3):161–7.
Mira-Avendano IC, Abril A. Pulmonary manifestations of Sjögren syndrome, systemic lupus erythematosus, and mixed connective tissue disease. Rheum Dis Clin North Am. 2015;41(2):263–77.
Flament T, Bigot A, Chaigne B, Henique H, Diot E, Marchand-Adam S. Pulmonary manifestations of Sjögren’s syndrome. Eur Respir Rev. 2016;25(140):110–23.
Wang Y, Hou Z, Qiu M, Ye Q. Risk factors for primary Sjögren syndrome-associated interstitial lung disease. J Thorac Dis. 2018;10(4):2108–17.
Sato S, Hirakata M, Kuwana M, Suwa A, Inada S, Mimori T, et al. Autoantibodies to a 140-kd polypeptide, CADM-140, in Japanese patients with clinically amyopathic dermatomyositis. Arthritis Rheum. 2005;52(5):1571–6.
Lohrmann C, Uhl M, Warnatz K, Ghanem N, Kotter E, Schaefer O, et al. High-resolution CT imaging of the lung for patients with primary Sjogren’s syndrome. Eur J Radiol. 2004;52(2):137–43.
Vasaitis L, Nordmark G, Theander E, Backlin C, Smedby KE, Askling J, et al. Comparison of patients with and without pre-existing lymphoma at diagnosis of primary Sjögren’s syndrome. Scand J Rheumatol. 2019;48(3):207–12.
Ito I, Nagai S, Kitaichi M, Nicholson AG, Johkoh T, Noma S, et al. Pulmonary manifestations of primary Sjogren’s syndrome: a clinical, radiologic, and pathologic study. Am J Respir Crit Care Med. 2005;171(6):632–8.
Voulgarelis M, Ziakas PD, Papageorgiou A, Baimpa E, Tzioufas AG, Moutsopoulos HM. Prognosis and outcome of non-Hodgkin lymphoma in primary Sjögren syndrome. Medicine (Baltimore). 2012;91(1):1–9.
Brito-Zerón P, Kostov B, Fraile G, Caravia-Durán D, Maure B, Rascón F-J, et al. Characterization and risk estimate of cancer in patients with primary Sjögren syndrome. J Hematol Oncol. 2017;10(1):90.
Ramos-Casals M, Brito-Zerón P, Seror R, Bootsma H, Bowman SJ, Dörner T, et al. Characterization of systemic disease in primary Sjögren’s syndrome: EULAR-SS task force recommendations for articular, cutaneous, pulmonary and renal involvements. Rheumatology (Oxford). 2015;54(12):2230–8.
Dong X, Zhou J, Guo X, Li Y, Xu Y, Fu Q, et al. A retrospective analysis of distinguishing features of chest HRCT and clinical manifestation in primary Sjögren’s syndrome-related interstitial lung disease in a Chinese population. Clin Rheumatol. 2018;37(11):2981–8.
Zhang T, Yuan F, Xu L, Sun W, Liu L, Xue J. Characteristics of patients with primary Sjögren’s syndrome associated interstitial lung disease and relevant features of disease progression. Clin Rheumatol. 2020;39(5):1561–8.
Roca F, Dominique S, Schmidt J, Smail A, Duhaut P, Lévesque H, et al. Interstitial lung disease in primary Sjögren’s syndrome. Autoimmun Rev. 2017;16(1):48–54.
Robles-Perez A, Molina-Molina M. Treatment considerations of lung involvement in rheumatologic disease. Respiration. 2015;90(4):265–74.
Mira-Avendano IC, Parambil JG, Yadav R, Arrossi V, Xu M, Chapman JT, et al. A retrospective review of clinical features and treatment outcomes in steroid-resistant interstitial lung disease from polymyositis/dermatomyositis. Respir Med. 2013;107(6):890–6.
Parambil JG, Myers JL, Lindell RM, Matteson EL, Ryu JH. Interstitial lung disease in primary Sjögren syndrome. Chest. 2006;130(5):1489–95.
Justet A, Ottaviani S, Dieudé P, Taillé C. Tocilizumab for refractory organising pneumonia associated with Sjögren’s disease. BMJ Case Rep. 2015;2015:bcr2014209076.
Wang J, Li M, Wang Q, Zhang X, Qian J, Zhao J, et al. Pulmonary arterial hypertension associated with primary Sjögren’s syndrome: a multicentre cohort study from China. Eur Respir J. 2020;56(5):1902157.
Sharp GC, Irvin WS, Tan EM, Gould RG, Holman HR. Mixed connective tissue disease—an apparently distinct rheumatic disease syndrome associated with a specific antibody to an extractable nuclear antigen (ENA). Am J Med. 1972;52(2):148–59.
Amigues JM, Cantagrel A, Abbal M, Mazieres B. Comparative study of 4 diagnosis criteria sets for mixed connective tissue disease in patients with anti-RNP antibodies. Autoimmunity group of the Hospitals of Toulouse. J Rheumatol. 1996;23(12):2055–62.
Gunnarsson R, Hetlevik SO, Lilleby V, Molberg Ø. Mixed connective tissue disease. Best Pract Res Clin Rheumatol. 2016;30(1):95–111.
Ungprasert P, Crowson CS, Chowdhary VR, Ernste FC, Moder KG, Matteson EL. Epidemiology of mixed connective tissue disease, 1985-2014: a population-based study. Arthritis Care Res (Hoboken). 2016;68(12):1843–8.
Gunnarsson R, Aaløkken TM, Molberg Ø, Lund MB, Mynarek GK, Lexberg AS, et al. Prevalence and severity of interstitial lung disease in mixed connective tissue disease: a nationwide, cross-sectional study. Ann Rheum Dis. 2012;71(12):1966–72.
Bodolay E, Szekanecz Z, Dévényi K, Galuska L, Csípo I, Vègh J, et al. Evaluation of interstitial lung disease in mixed connective tissue disease (MCTD). Rheumatology (Oxford). 2005;44(5):656–61.
Ciang NCO, Pereira N, Isenberg DA. Mixed connective tissue disease-enigma variations? Rheumatology (Oxford). 2017;56(3):326–33.
Gunnarsson R, Andreassen AK, Molberg Ø, Lexberg ÅS, Time K, Dhainaut ASS, et al. Prevalence of pulmonary hypertension in an unselected, mixed connective tissue disease cohort: results of a nationwide, Norwegian cross-sectional multicentre study and review of current literature. Rheumatology (Oxford). 2013;52(7):1208–13.
Vegh J, Szodoray P, Kappelmayer J, Csipo I, Udvardy M, Lakos G, et al. Clinical and immunoserological characteristics of mixed connective tissue disease associated with pulmonary arterial hypertension. Scand J Immunol. 2006;64(1):69–76.
Flåm ST, Gunnarsson R, Garen T, Norwegian MCTD Study Group, Lie BA, Molberg Ø. The HLA profiles of mixed connective tissue disease differ distinctly from the profiles of clinically related connective tissue diseases. Rheumatology (Oxford). 2015;54(3):528–35.
Lamri Y, Vibhushan S, Pacreau E, Boedec E, Saidoune F, Mailleux A, et al. Basophils and IgE contribute to mixed connective tissue disease development. J Allergy Clin Immunol. 2021;147(4):1478–1489.e11.
Kasukawa R. Mixed connective tissue disease. Intern Med. 1999;38(5):386–93.
Dima A, Jurcut C, Baicus C. The impact of anti-U1-RNP positivity: systemic lupus erythematosus versus mixed connective tissue disease. Rheumatol Int. 2018;38(7):1169–78.
Shirai Y, Yasuoka H, Okano Y, Takeuchi T, Satoh T, Kuwana M. Clinical characteristics and survival of Japanese patients with connective tissue disease and pulmonary arterial hypertension: a single-Centre cohort. Rheumatology (Oxford). 2012;51(10):1846–54.
Condliffe R, Kiely DG, Peacock AJ, Corris PA, Gibbs JSR, Vrapi F, et al. Connective tissue disease-associated pulmonary arterial hypertension in the modern treatment era. Am J Respir Crit Care Med. 2009;179(2):151–7.
Galiè N, Denton CP, Dardi F, Manes A, Mazzanti G, Li B, et al. Tadalafil in idiopathic or heritable pulmonary arterial hypertension (PAH) compared to PAH associated with connective tissue disease. Int J Cardiol. 2017;235:67–72.
Coghlan JG, Galiè N, Barberà JA, Frost AE, Ghofrani H-A, Hoeper MM, et al. Initial combination therapy with ambrisentan and tadalafil in connective tissue disease-associated pulmonary arterial hypertension (CTD-PAH): subgroup analysis from the AMBITION trial. Ann Rheum Dis. 2017;76(7):1219–27.
Graney BA, Fischer A. Advocating for early interstitial lung disease detection in mixed connective tissue disease. Rheumatology (Oxford). 2018;57(2):204–5.
Reiseter S, Gunnarsson R, Corander J, Haydon J, Lund MB, Aaløkken TM, et al. Disease evolution in mixed connective tissue disease: results from a long-term nationwide prospective cohort study. Arthritis Res Ther. 2017;19(1):284.
Burdt MA, Hoffman RW, Deutscher SL, Wang GS, Johnson JC, Sharp GC. Long-term outcome in mixed connective tissue disease: longitudinal clinical and serologic findings. Arthritis Rheum. 1999;42(5):899–909.
Reiseter S, Gunnarsson R, Mogens Aaløkken T, Lund MB, Mynarek G, Corander J, et al. Progression and mortality of interstitial lung disease in mixed connective tissue disease: a long-term observational nationwide cohort study. Rheumatology (Oxford). 2018;57(2):255–62.
Lundberg IE, Tjärnlund A, Bottai M, Werth VP, Pilkington C, de Visser M, et al. 2017 European league against Rheumatism/American College of Rheumatology classification criteria for adult and juvenile idiopathic inflammatory myopathies and their major subgroups. Arthritis Rheumatol. 2017;69(12):2271–82.
Lundberg IE, de Visser M, Werth VP. Classification of myositis. Nat Rev Rheumatol. 2018;14(5):269–78.
Meyer A, Meyer N, Schaeffer M, Gottenberg J-E, Geny B, Sibilia J. Incidence and prevalence of inflammatory myopathies: a systematic review. Rheumatology (Oxford). 2015;54(1):50–63.
Gallay L, Gayed C, Hervier B. Antisynthetase syndrome pathogenesis: knowledge and uncertainties. Curr Opin Rheumatol. 2018;30(6):664–73.
Hervier B, Uzunhan Y. Inflammatory myopathy-related interstitial lung disease: from pathophysiology to treatment. Front Med (Lausanne). 2019;6:326.
McHugh NJ, Tansley SL. Autoantibodies in myositis. Nat Rev Rheumatol. 2018;14(5):290–302.
Liu Y, Liu X, Xie M, Chen Z, He J, Wang Z, et al. Clinical characteristics of patients with anti-EJ antisynthetase syndrome associated interstitial lung disease and literature review. Respir Med. 2020;165:105920.
Hamaguchi Y, Fujimoto M, Matsushita T, Kaji K, Komura K, Hasegawa M, et al. Common and distinct clinical features in adult patients with anti-aminoacyl-tRNA synthetase antibodies: heterogeneity within the syndrome. PLoS One. 2013;8(4):e60442.
Koga T, Fujikawa K, Horai Y, Okada A, Kawashiri S-Y, Iwamoto N, et al. The diagnostic utility of anti-melanoma differentiation-associated gene 5 antibody testing for predicting the prognosis of Japanese patients with DM. Rheumatology (Oxford). 2012;51(7):1278–84.
Moghadam-Kia S, Oddis CV, Sato S, Kuwana M, Aggarwal R. Antimelanoma differentiation-associated gene 5 antibody: expanding the clinical spectrum in north American patients with dermatomyositis. J Rheumatol. 2017;44(3):319–25.
Cao H, Pan M, Kang Y, Xia Q, Li X, Zhao X, et al. Clinical manifestations of dermatomyositis and clinically amyopathic dermatomyositis patients with positive expression of anti-melanoma differentiation-associated gene 5 antibody. Arthritis Care Res (Hoboken). 2012;64(10):1602–10.
Allenbach Y, Uzunhan Y, Toquet S, Leroux G, Gallay L, Marquet A, et al. Different phenotypes in dermatomyositis associated with anti-MDA5 antibody: study of 121 cases. Neurology. 2020;95(1):e70–8.
Saketkoo LA, Ascherman DP, Cottin V, Christopher-Stine L, Danoff SK, Oddis CV. Interstitial lung disease in idiopathic inflammatory myopathy. Curr Rheumatol Rev. 2010;6(2):108–19.
Sun K-Y, Fan Y, Wang Y-X, Zhong Y-J, Wang G-F. Prevalence of interstitial lung disease in polymyositis and dermatomyositis: a meta-analysis from 2000 to 2020. Semin Arthritis Rheum. 2021;51(1):175–91.
Morisset J, Johnson C, Rich E, Collard HR, Lee JS. Management of myositis-related interstitial lung disease. Chest. 2016;150(5):1118–28.
Mimori T, Nakashima R, Hosono Y. Interstitial lung disease in myositis: clinical subsets, biomarkers, and treatment. Curr Rheumatol Rep. 2012;14(3):264–74.
Lega J-C, Fabien N, Reynaud Q, Durieu I, Durupt S, Dutertre M, et al. The clinical phenotype associated with myositis-specific and associated autoantibodies: a meta-analysis revisiting the so-called antisynthetase syndrome. Autoimmun Rev. 2014;13(9):883–91.
Mahler M, Miller FW, Fritzler MJ. Idiopathic inflammatory myopathies and the anti-synthetase syndrome: a comprehensive review. Autoimmun Rev. 2014;13(4–5):367–71.
Wolfe JF, Adelstein E, Sharp GC. Antinuclear antibody with distinct specificity for polymyositis. J Clin Invest. 1977;59(1):176–8.
Lega J-C, Cottin V, Fabien N, Thivolet-Béjui F, Cordier J-F. Interstitial lung disease associated with anti-PM/Scl or anti-aminoacyl-tRNA synthetase autoantibodies: a similar condition? J Rheumatol. 2010;37(5):1000–9.
Troyanov Y, Targoff IN, Payette M-P, Raynauld J-P, Chartier S, Goulet J-R, et al. Redefining dermatomyositis: a description of new diagnostic criteria that differentiate pure dermatomyositis from overlap myositis with dermatomyositis features. Medicine (Baltimore). 2014;93(24):318–32.
Hervier B, Devilliers H, Stanciu R, Meyer A, Uzunhan Y, Masseau A, et al. Hierarchical cluster and survival analyses of antisynthetase syndrome: phenotype and outcome are correlated with anti-tRNA synthetase antibody specificity. Autoimmun Rev. 2012;12(2):210–7.
Barba T, Fort R, Cottin V, Provencher S, Durieu I, Jardel S, et al. Treatment of idiopathic inflammatory myositis associated interstitial lung disease: a systematic review and meta-analysis. Autoimmun Rev. 2019;18(2):113–22.
Kobayashi N, Takezaki S, Kobayashi I, Iwata N, Mori M, Nagai K, et al. Clinical and laboratory features of fatal rapidly progressive interstitial lung disease associated with juvenile dermatomyositis. Rheumatology (Oxford). 2015;54(5):784–91.
Xu Y, Yang CS, Li YJ, Liu XD, Wang JN, Zhao Q, et al. Predictive factors of rapidly progressive-interstitial lung disease in patients with clinically amyopathic dermatomyositis. Clin Rheumatol. 2016;35(1):113–6.
Lega J-C, Reynaud Q, Belot A, Fabien N, Durieu I, Cottin V. Idiopathic inflammatory myopathies and the lung. Eur Respir Rev. 2015;24(136):216–38.
Boitiaux J-F, Debray M-P, Nicaise-Roland P, Adle-Biassette H, Danel C, Clérici C, et al. Idiopathic interstitial lung disease with anti-SSA antibody. Rheumatology (Oxford). 2011;50(12):2245–50.
Douglas WW, Tazelaar HD, Hartman TE, Hartman RP, Decker PA, Schroeder DR, et al. Polymyositis-dermatomyositis-associated interstitial lung disease. Am J Respir Crit Care Med. 2001;164(7):1182–5.
Zare Mehrjardi M, Kahkouee S, Pourabdollah M. Radio-pathological correlation of organizing pneumonia (OP): a pictorial review. Br J Radiol. 2017;90(1071):20160723.
Todd NW, Marciniak ET, Sachdeva A, Kligerman SJ, Galvin JR, Luzina IG, et al. Organizing pneumonia/non-specific interstitial pneumonia overlap is associated with unfavorable lung disease progression. Respir Med. 2015;109(11):1460–8.
Mejía M, Herrera-Bringas D, Pérez-Román DI, Rivero H, Mateos-Toledo H, Castorena-García P, et al. Interstitial lung disease and myositis-specific and associated autoantibodies: clinical manifestations, survival and the performance of the new ATS/ERS criteria for interstitial pneumonia with autoimmune features (IPAF). Respir Med. 2017;123:79–86.
Solomon J, Swigris JJ, Brown KK. Myositis-related interstitial lung disease and antisynthetase syndrome. J Bras Pneumol. 2011;37(1):100–9.
Frazier AR, Miller RD. Interstitial pneumonitis in association with polymyositis and dermatomyositis. Chest. 1974;65(4):403–7.
Mukae H, Ishimoto H, Sakamoto N, Hara S, Kakugawa T, Nakayama S, et al. Clinical differences between interstitial lung disease associated with clinically amyopathic dermatomyositis and classic dermatomyositis. Chest. 2009;136(5):1341–7.
Tillie-Leblond I, Wislez M, Valeyre D, Crestani B, Rabbat A, Israel-Biet D, et al. Interstitial lung disease and anti-Jo-1 antibodies: difference between acute and gradual onset. Thorax. 2008;63(1):53–9.
Takada T, Suzuki E, Nakano M, Kagamu H, Tsukada H, Hasegawa T, et al. Clinical features of polymyositis/dermatomyositis with steroid-resistant interstitial lung disease. Intern Med. 1998;37(8):669–73.
Takada K, Kishi J, Miyasaka N. Step-up versus primary intensive approach to the treatment of interstitial pneumonia associated with dermatomyositis/polymyositis: a retrospective study. Mod Rheumatol. 2007;17(2):123–30.
Huapaya JA, Silhan L, Pinal-Fernandez I, Casal-Dominguez M, Johnson C, Albayda J, et al. Long-term treatment with azathioprine and Mycophenolate Mofetil for myositis-related interstitial lung disease. Chest. 2019;156(5):896–906.
Sharma N, Putman MS, Vij R, Strek ME, Dua A. Myositis-associated interstitial lung disease: predictors of failure of conventional treatment and response to tacrolimus in a US cohort. J Rheumatol. 2017;44(11):1612–8.
Gono T, Kawaguchi Y, Satoh T, Kuwana M, Katsumata Y, Takagi K, et al. Clinical manifestation and prognostic factor in anti-melanoma differentiation-associated gene 5 antibody-associated interstitial lung disease as a complication of dermatomyositis. Rheumatology (Oxford). 2010;49(9):1713–9.
Nagasaka K, Harigai M, Tateishi M, Hara M, Yoshizawa Y, Koike T, et al. Efficacy of combination treatment with cyclosporin a and corticosteroids for acute interstitial pneumonitis associated with dermatomyositis. Mod Rheumatol. 2003;13(3):231–8.
Keir GJ, Maher TM, Ming D, Abdullah R, de Lauretis A, Wickremasinghe M, et al. Rituximab in severe, treatment-refractory interstitial lung disease. Respirology. 2014;19(3):353–9.
Andersson H, Sem M, Lund MB, Aaløkken TM, Günther A, Walle-Hansen R, et al. Long-term experience with rituximab in anti-synthetase syndrome-related interstitial lung disease. Rheumatology (Oxford). 2015;54(8):1420–8.
Sharp C, McCabe M, Dodds N, Edey A, Mayers L, Adamali H, et al. Rituximab in autoimmune connective tissue disease-associated interstitial lung disease. Rheumatology (Oxford). 2016;55(7):1318–24.
Doyle TJ, Dhillon N, Madan R, Cabral F, Fletcher EA, Koontz DC, et al. Rituximab in the treatment of interstitial lung disease associated with Antisynthetase syndrome: a multicenter retrospective case review. J Rheumatol. 2018;45(6):841–50.
Saunders P, Tsipouri V, Keir GJ, Ashby D, Flather MD, Parfrey H, et al. Rituximab versus cyclophosphamide for the treatment of connective tissue disease-associated interstitial lung disease (RECITAL): study protocol for a randomised controlled trial. Trials. 2017;18(1):275.
Bejan-Angoulvant T, Naccache J-M, Caille A, Borie R, Nunes H, Ferreira M, et al. Evaluation of efficacy and safety of rituximab in combination with mycophenolate mofetil in patients with nonspecific interstitial pneumonia non-responding to a first-line immunosuppressive treatment (EVER-ILD): a double-blind placebo-controlled randomized trial. Respir Med Res. 2020;78:100770.
Suzuki Y, Hayakawa H, Miwa S, Shirai M, Fujii M, Gemma H, et al. Intravenous immunoglobulin therapy for refractory interstitial lung disease associated with polymyositis/dermatomyositis. Lung. 2009;187(3):201–6.
Bakewell CJ, Raghu G. Polymyositis associated with severe interstitial lung disease: remission after three doses of IV immunoglobulin. Chest. 2011;139(2):441–3.
Suresh E, Wimalaratna S. Proximal myopathy: diagnostic approach and initial management. Postgrad Med J. 2013;89(1054):470–7.
Kalluri M, Oddis CV. Pulmonary manifestations of the idiopathic inflammatory myopathies. Clin Chest Med. 2010;31(3):501–12.
Selva-O’Callaghan A, Labrador-Horrillo M, Muñoz-Gall X, Martínez-Gomez X, Majó-Masferrer J, Solans-Laque R, et al. Polymyositis/dermatomyositis-associated lung disease: analysis of a series of 81 patients. Lupus. 2005;14(7):534–42.
Sanges S, Yelnik CM, Sitbon O, Benveniste O, Mariampillai K, Phillips-Houlbracq M, et al. Pulmonary arterial hypertension in idiopathic inflammatory myopathies: data from the French pulmonary hypertension registry and review of the literature. Medicine (Baltimore). 2016;95:e4911.
Marie I, Hatron PY, Dominique S, Cherin P, Mouthon L, Menard J-F. Short-term and long-term outcomes of interstitial lung disease in polymyositis and dermatomyositis: a series of 107 patients. Arthritis Rheum. 2011;63(11):3439–47.
Dankó K, Ponyi A, Constantin T, Borgulya G, Szegedi G. Long-term survival of patients with idiopathic inflammatory myopathies according to clinical features: a longitudinal study of 162 cases. Medicine (Baltimore). 2004;83(1):35–42.
Fujisawa T, Hozumi H, Kono M, Enomoto N, Hashimoto D, Nakamura Y, et al. Prognostic factors for myositis-associated interstitial lung disease. PLoS One. 2014;9(6):e98824.
Aggarwal R, McBurney C, Schneider F, Yousem SA, Gibson KF, Lindell K, et al. Myositis-associated usual interstitial pneumonia has a better survival than idiopathic pulmonary fibrosis. Rheumatology (Oxford). 2017;56(3):384–9.
Hozumi H, Fujisawa T, Nakashima R, Johkoh T, Sumikawa H, Murakami A, et al. Comprehensive assessment of myositis-specific autoantibodies in polymyositis/dermatomyositis-associated interstitial lung disease. Respir Med. 2016;121:91–9.
Lescoat A, Lelong M, Jeljeli M, Piquet-Pellorce C, Morzadec C, Ballerie A, et al. Combined anti-fibrotic and anti-inflammatory properties of JAK-inhibitors on macrophages in vitro and in vivo: perspectives for scleroderma-associated interstitial lung disease. Biochem Pharmacol. 2020;178:114103.
Wendel S, Venhoff N, Frye BC, May AM, Agarwal P, Rizzi M, et al. Successful treatment of extensive calcifications and acute pulmonary involvement in dermatomyositis with the Janus-kinase inhibitor tofacitinib–a report of two cases. J Autoimmun. 2019;100:131–6.
Selva-O’ Callaghan A, Romero-Bueno F, Trallero-Araguás E, Gil-Vila A, Ruiz-Rodríguez JC, Sánchez-Pernaute O, et al. Pharmacologic treatment of anti-MDA5 rapidly progressive interstitial lung disease. Curr Treatm Opt Rheumatol. 2021;28:1–15.
Wells AU, Flaherty KR, Brown KK, Inoue Y, Devaraj A, Richeldi L, et al. Nintedanib in patients with progressive fibrosing interstitial lung diseases—subgroup analyses by interstitial lung disease diagnosis in the INBUILD trial: a randomised, double-blind, placebo-controlled, parallel-group trial. Lancet Respir Med. 2020;8(5):453–60.
Maher TM, Corte TJ, Fischer A, Kreuter M, Lederer DJ, Molina-Molina M, et al. Pirfenidone in patients with unclassifiable progressive fibrosing interstitial lung disease: a double-blind, randomised, placebo-controlled, phase 2 trial. Lancet Respir Med. 2020;8(2):147–57.
Behr J, Prasse A, Kreuter M, Johow J, Rabe KF, Bonella F, et al. Pirfenidone in patients with progressive fibrotic interstitial lung diseases other than idiopathic pulmonary fibrosis (RELIEF): a double-blind, randomised, placebo-controlled, phase 2b trial. Lancet Respir Med. 2021;9(5):476–86.
Courtwright AM, El-Chemaly S, Dellaripa PF, Goldberg HJ. Survival and outcomes after lung transplantation for non-scleroderma connective tissue-related interstitial lung disease. J Heart Lung Transplant. 2017;36(7):763–9.
Lee JC, Ahya VN. Lung transplantation in autoimmune diseases. Clin Chest Med. 2010;31(3):589–603.
Yusen RD, Christie JD, Edwards LB, Kucheryavaya AY, Benden C, Dipchand AI, et al. The registry of the International Society for Heart and Lung Transplantation: thirtieth adult lung and heart-lung transplant report—2013; focus theme: age. J Heart Lung Transplant. 2013;32(10):965–78.
Marchiset A, Neuville M, Voiriot G, De Wolf J, Glorion M, Parquin F, et al. High-emergency lung transplantation for interstitial lung disease associated with anti-MDA5 Dermatomyositis: a case report. Transplant Proc. 2021;53(8):2613–5.
Chan C, Ryerson CJ, Dunne JV, Wilcox PG. Demographic and clinical predictors of progression and mortality in connective tissue disease-associated interstitial lung disease: a retrospective cohort study. BMC Pulm Med. 2019;19(1):192.
Elhai M, Avouac J, Allanore Y. Circulating lung biomarkers in idiopathic lung fibrosis and interstitial lung diseases associated with connective tissue diseases: where do we stand? Semin Arthritis Rheum. 2020;50(3):480–91.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Ghanem, M., Vasarmidi, E., Morer, L., Le Guen, P., Crestani, B. (2023). Lung Disease in Systemic Lupus Erythematosus, Myositis, Sjögren’s Disease, and Mixed Connective Tissue Disease. In: Cottin, V., Richeldi, L., Brown, K., McCormack, F.X. (eds) Orphan Lung Diseases. Springer, Cham. https://doi.org/10.1007/978-3-031-12950-6_14
Download citation
DOI: https://doi.org/10.1007/978-3-031-12950-6_14
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-12949-0
Online ISBN: 978-3-031-12950-6
eBook Packages: MedicineMedicine (R0)