Abstract
Lymph nodes (LNs) are secondary lymphoid organs that function as the first line of defense against invasive foreign substances. Within the LNs, different types of immune cells are strategically localized to induce immune responses efficiently. Such a sophisticated tissue structure is a complex of functionally specialized niches, constructed by a variety of fibroblastic stromal cells. Elucidating the characteristics and functions of the niches and stromal cells will facilitate comprehension of the immune response induced in the LNs. Three recent studies offered novel insights into specialized stromal cells. In our discussion of these surprisingly diverse stromal cells, we will integrate information from these studies to improve knowledge about the structure and niches of LN.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
1 Introduction
Lymph nodes (LNs) are situated at critical positions in the lymphatic vascular system and widely present throughout the body to filter lymph fluid exudate. They are also secondary lymphoid organs that function as the first line of defense against invasive pathogens or foreign substances. LNs continuously monitor the lymph fluid and, if antigens are detected, rapidly induce adaptive immune responses. The sophisticated tissue structure in LN is suitable for this purpose; it comprises several distinct areas in which different immune cell types are strategically localized (Qi et al. 2014). The “functional segregation” of immune cells is believed to optimize spatiotemporal regulation of motile behaviors, which induce efficient responses.
Individual LN has one or more basic structures called “compartments (or lobules),” which comprise two major parts, the cortex and medulla (Belisle and Sainte-Marie 1981; Gretz et al. 1997; Willard-Mack 2006; Sainte-Marie 2010). The cortex is characterized by a dense lymphocyte accumulation in the hemisphere of afferent lymphatic entry. B cells and T cells are localized in different cortical areas; B cells in the superficial cortex forming multiple follicles, and T cells in the deeper layer called the T cell zone (or paracortex). Upon immune response induction, activated B cells start to construct a specialized structure called the germinal center (GC) in the follicle via the help of follicular helper T (Tfh) cells, which plays a vital role in generating humoral immunity (Victora and Nussenzweig 2012). In a single compartment, individual functional areas occupying a certain spatial expanse with the localization of specific immune cells are classified as “subcompartments” (Takeuchi et al. 2018). Subcompartments are tightly associated with unique non-hematopoietic fibroblastic stromal cells (FSCs) that exhibit specialized roles in organizing niches. Each FSC subset produces specific chemokines and cytokines for immune cells’ localization and function (Cyster 1999; Mueller and Germain 2009; Katakai 2016). Importantly, the construction and maintenance of subcompartments require continuous interaction between immune cells and stromal cells (Roozendaal and Mebius 2011). For instance, follicular dendritic cells (FDCs), which are FSC subsets in the follicular center or GC light zone, organize subcompartments via the production of CXCL13 that attracts B cells and also Tfh cells (Allen and Cyster 2008; McHeyzer-Williams et al. 2011). Conversely, lymphotoxin (LT)-α1β2 and TNFα produced from B cells is required for the maintenance of FDC function and tissue structure (Matsumoto et al. 1997).
As of 2016, four major FSC subsets associated with cortical subcompartments have been identified, including FDC, TRC (T zone reticular cell), MRC (marginal reticular cell), and CRC (CXCL12-expressing reticular cells) (Chen et al. 1978; Link et al. 2007; Katakai et al. 2008; Bannard et al. 2013; Katakai 2016). Several additional subsets that do not correlate with a particular subcompartment were also proposed (Malhotra et al. 2012; Mionnet et al. 2013; Sitnik et al. 2016). Such a growing heterogeneity of LN stromal cells led to slight confusion in the field. Meanwhile, previous reports show a tendency of bias toward the structure and function of cortical areas due to their noticeable anatomy and dedication to lymphocyte-centered responses. Stromal cell studies have also focused on cortical subsets, and information in other regions such as the medullary region of LN has been limited until recently.
In 2018, three independent studies showed extensive evidence that expands our knowledge on the diversity of LN stromal cells with findings of novel subsets (Table 1). Rodda et al. identified nine clusters in a single-cell RNA sequencing (scRNAseq) of CD45–CD31– non-endothelial stromal cells (Rodda et al. 2018). Huang et al. proposed seven different populations of fibroblastic reticular cells (FRCs) with multiparameter flow cytometry-based clustering, primarily focusing on the medulla (Huang et al. 2018). Based on anatomical examinations using multiple gene reporter mice, Takeuchi et al. reported two novel FSC subsets in the cortex-medulla boundary and medullary cords, and proposed at least six FSC subsets existing in LNs (Takeuchi et al. 2018). Since these studies took different approaches in terms of methodologies and experimental conditions, the proposals of stromal subsets could contain conflicting classifications.
Here, we comparatively reviewed these reports with a reevaluation of the scRNAseq dataset, and also histochemical confirmation, to enhance knowledge of the structural and functional significance of LN stromal cells. We defined a “stromal cell subset” as a cell population that constructs a subcompartment, i.e., niche for immune cells. We emphasized anatomical viewpoints to identify the stromal subset. Although single-cell and flow cytometry analyses are powerful approaches, positional information was entirely lost during cell isolation, possibly leading to excess subfractions or inseparable closely related subsets. Therefore, careful confirmation of actual microanatomy and cell/molecular distributions was indispensable.
2 Reevaluating a Single-Cell Analysis of LN Stromal Cells
To resolve discrepancies between the “original” single-cell analysis and other reports, we tried to reanalyze the datasets deposited in a database (Rodda et al. 2018). The results could also be incongruous owing to the use of the latest versions of programs, different from that used for the original analysis (Stuart et al. 2019). From the reanalysis, we successfully identified nine clusters (Fig. 1a); each cluster was assigned to the most probable stromal subset based on marker gene expression. Consequently, we obtained similar results for the majority of clusters as the original report, including FDC, MRC, Ccl19hi TRC, Ccl19lo TRC, Cd34+ stromal cell (SC), and perivascular cell (PvC) (Fig. 1b, c, and data not shown). Of note, the reanalysis improved some crucial points compared to the original report; (1) MRC fraction was enriched for Madcam1 expression, and (2) Ch25h expression was detected in Ccl19lo TRC fraction (Fig. 1c; described later).
Identification of 9 clusters by reanalyzing single-cell datasets reported by Rodda et al. 2018. a Clustering reanalysis visualized with tSNE. Each dot indicates a single cell that is colored by each cluster categorized. B: B cell zone, T: T cell zone, and M: Medullary cord, respectively. b Feature plot of indicated genes. Distribution of gene expression levels is projected on to tSNE plots. c Violin plots of Madcam1, Ch25h, and Ccl19 expression in each cluster. Reanalysis of scRNAseq datasets deposited in the GEO database (ID code: GSE112903) was performed using R (version 3.6.2) and Seurat package (version 3.1.0) (Stuart et al. 2019). Default parameters using 10 principle components (PCs) that were determined by the results of JackStrawPlot and ElbowPlot programs set for the analysis. The FindClusters program (resolution = 0.4) finally led to nine clusters, as shown in (a)
Reanalysis provided a few clusters with clearly different features from the original report (Figs. 1 and 2). The Cxcl9+ TRC cluster, proposed as one of the three TRC subsets (Rodda et al. 2018), became part of Ccl19hi TRC fraction, and another Ccl19loCcl21+ TRC-like cluster emerged in addition to the Ccl19loCh25h+ TRCs. As the new Ccl19lo cluster appeared to show the characteristics of a specific stromal cell subset in the cortex-medulla boundary (Takeuchi et al. 2018), we assigned this subset to a new cluster (Fig. 1a; described later). Two clusters differentially expressing Nr4a1 and Inmt were initially designated as stromal cells in the medullary cord (MC) (Rodda et al. 2018). However, in our reanalysis, the expression of these genes was comparable in two candidate medullary clusters (Fig. 1a, b). In particular, Inmt expression corresponded well with these clusters. It was also reported that the leptin receptor (Lepr) is highly expressed in medullary cord reticular cells (MCRCs) (Takeuchi et al. 2018). As the two clusters showed enrichment for Lepr expression, we assigned these as MCRCs (Fig. 1a, b). We also noticed that MCRC clusters could be distinguished by the expression level of Lepr, which was well correlated with the histological examinations of LNs (Fig. 2c). Accordingly, we named these Leprhi MCRC and Leprlo MCRC, respectively (Fig. 1a; described later). We will not provide details about CD34+ SC and PvCs, since these stromal cells are observed in the capsule or surroundings of blood vessels that we do not consider to be subcompartments. Taken together, we propose a current model for subcompartments associated with stromal cell subsets in LN (Fig. 3, Table 1). We will introduce each subset one by one below.
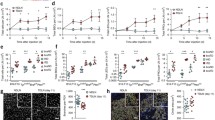
Novel characteristics in TRC and MCRC subsets. a Violin plot of gene expression related to TRC subsets, b DRC is a high producer of IL-7. Section of a brachial LN from IL-7 GFP knock-in mouse (Hara et al. 2012) was stained for B220 and desmin. Arrows indicate the DCP area. c Expression pattern of Lepr in LN. Violin plot of Lepr expression (left) and immunohistochemistry of LN (right). Section of a cervical LN from C57BL/6 wt mouse was stained for Lepr and desmin (upper right) or B220, CD138, and desmin (lower right). Arrows in higher magnification views indicate the MCs with high Lepr staining colocalized with CD138+ plasma cells
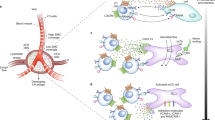
A proposed model of tissue structure and FSC subsets in LN. Various types of stromal cells construct unique subcompartments, which are highly organized and functionally specialized niches for localized immune cells. The representative basic unit of a single “compartment (lobule)” composed of a single B cell follicle with GC, T cell zone, and medulla is shown. B: B cell zone, T: T cell zone, M: medullary cord
3 B Cell Follicle
Follicles are B cell aggregates located in the outer cortex below the capsule. In this area, three stromal subsets, MRCs, FDCs, and CRCs, provide specialized niches in the outer, center, and inner follicle, respectively. After antigen-specific activation, B cells start to proliferate, giving rise to the GC in the follicle (Victora and Nussenzweig 2012). Functionally, GC is subdivided into two areas: the dark zone (DZ) where B cells undergo hyperproliferation and somatic hypermutation (SHM) in the B cell receptor (BCR) gene, and the light zone (LZ) in which B cells expressing high-affinity BCR are selected and differentiated into antibody-producing cells (Allen et al. 2007). GC development leads to the production of FDCs and CRCs to support the LZ and DZ, respectively, for the organization of highly specialized niches.
3.1 Marginal Reticular Cell (MRC)
MRCs are situated in the outermost part of follicles just below the subcapsular sinus (SCS), where afferent lymphatic inflow occurs in LNs (Katakai et al. 2008). MRCs express CXCL13, MAdCAM-1, and RANKL; expressions of these genes are enriched in the corresponding cluster in single-cell reanalysis (Figs. 1b, c, and 2a). This subset is likely to descend directly from lymphoid tissue organizer (LTo) stromal cells (Hoorweg et al. 2015; Katakai 2012) and have the potential to differentiate into FDCs after proliferation (Jarjour et al. 2014). The specific localization of MRCs at the front line of antigen entry suggests a non-redundant role in forming a niche for a defensive barrier.
Several new findings of MRC function were recently reported; RANKL production in MRC is involved in the differentiation of sinusoidal macrophages (SMs) (Camara et al. 2019). Two types of SMs are positioned in the lymphatic sinuses of LNs; SCS macrophages (SSMs) capture lymph-borne antigens in a non-degradative way and transfer them into follicles across the SCS floor (Carrasco and Batista 2007; Phan et al. 2007), while medullary sinus macrophages (MSMs) exhibit robust phagocytosis and release inflammatory cytokines upon immune responses (Chatziandreou et al. 2017). Most SMs, in particular SSMs, disappeared in FRC-specific RANKL deficiency, suggesting the critical role of RANKL signaling in SM differentiation (Camara et al. 2019). Given that antigens, transferred by SSMs into follicular parenchyma, are further transported by migrating B cells up to FDCs (Phan et al. 2009), MRC production of CXCL13 is likely to be important in this process via facilitating B cell motility.
From anatomical viewpoints, Huang et al. classified FRCs into three subpopulations; MRCs (BP3+MAdCAM-1+), TRCs (BP3+MAdCAM-1–), and medullary reticular cells (MedRCs; BP3–MAdCAM-1–). Using multiparameter flow cytometry-based clustering, they further subdivided MRCs into two populations; Ccl21–Cxcl13+ MRC and Ccl21+Cxcl13– MRC (Huang et al. 2018) (Table 1). However, the Ccl21+Cxcl13– subset was undetectable in single-cell reanalysis because almost all the cells in the MRC cluster highly expressed CXCL13. Additionally, MAdCAM-1 expression was detected only in a small fraction of cells (Fig. 1c), even though most MRCs express MAdCAM-1 in immunohistochemistry. As the discrepancies may arise from a difference in the definition of subsets or methodology, it would be essential to confirm the correlation of actual microanatomy and molecular expression.
3.2 Follicular Dendritic Cell (FDC)
FDCs form a dense meshwork in the follicular center or GC-LZ with a unique antigen-presenting property for B cell affinity maturation. They show a distinct transcriptional profile among all FSC subsets in LNs (Rodda et al. 2018). These cells are characterized by the expression of CR1/CD35, CR2/CD21, FcγRIIB/CD32, FcεRII/CD23, MFGE8, MAdCAM-1, and deposition of complement components (Allen and Cyster 2008; Humphrey and Grennan 1982; Tew et al. 1982).
FDCs have been focused on crucial roles in antigen-specific antibody production, presenting immune complexes (IC) to B cells via complement- and Fc- receptors (Papamichail et al. 1975; Tew et al. 2001). Mice deficient in the Cr2 gene show impairment in antigen uptake and reduced responses to low dose or adjuvant-fee antigens, despite retaining GC formation and affinity maturation (Roozendaal and Carroll 2007). They are also deficient in producing serum antibodies and long-lived antibody-forming cells (Barrington et al. 2002). Since internalization via CR1/CR2 keeps antigens intact in FDCs owing to non-degradative recycling and displaying with periodic intervals, this process is assumed to play a crucial role in long-term antigen presentation. However, analysis of FcγRIIB-deficient FDCs demonstrated that this Fc receptor is dispensable for antigen retention (Barrington et al. 2002; Roozendaal and Carroll 2007; Victora and Nussenzweig 2012). Instead, FcγRIIB may be critical in modulating FDC activities associated with trapping IgG-antigen ICs to maintain humoral immunity, recall responses, or both (Barrington et al. 2002; Carroll and Isenman 2012).
Chemokines and cytokines produced by FDCs are necessary to control the GC microenvironment. CXCL13 functions as a chemoattractant for B cells and Tfh cells expressing CXCR5 (Allen and Cyster 2008; McHeyzer-Williams et al. 2011). This chemokine induces the production of LTαβ and TNFα from B cells, which in turn facilitates CXCL13 production by FDCs, driving a positive feedback loop in maintaining follicular structure (Ansel et al. 2000; Cyster et al. 2000). IC-binding onto FDCs enhances IL-6 production, which further promotes B cell SHM and IgG production as well as GC development (Wu et al. 2009). FDCs are also the source of BAFF that is required for the development and survival of B cells (Schneider et al. 1999). Mice deficient in BAFF could not sustain initial GC response due to defects in FDC maturation and lack of the ability to trap and retain ICs (Rahman et al. 2003; Vora et al. 2003). Thus, the engagement of B cells and FDCs induces mutual activation to make a niche for antigen-specific antibody production.
3.3 CXCL12-Expressing Reticular Cells (CRC)
The DZ in GC is a niche for hyperproliferation and SHM of GC-B cells, so-called “centroblasts.” Centroblasts express CXCR4, while the ligand CXCL12 is abundant in the DZ (Allen et al. 2004, 2007). CRC was identified as a stromal subset expressing CXCL12 and forming a network in DZ (Bannard et al. 2013). In the primary follicles, CRCs are positioned in close vicinity to the T cell zone suitable for the early stages of GC polarization (Bannard et al. 2013). Although CRCs and FDCs are morphologically similar, CRCs show undetectable or low expression levels in some FDC markers, including CD35 and distinct profile of chemokine in terms of CXCL12 and CXCL13, suggesting that two subsets could provide distinct niches within GCs. CXCL13 production in LZ controls the positioning of GC-B cells, whereas CXCL12 production in DZ is important for attracting CG-B cells from LZ. CXCR4-deficient B cells are unable to access to the DZ, leading to reduced BCR mutation. Interestingly, the proliferation of centroblasts and differentiation into centrocytes do not require DZ access; however, spatial segregation of two niches provides an optimal environment for effective GC responses (Bannard et al. 2013; Rodda et al. 2015).
In single-cell analyses, CRCs could not be detected as an individual cluster (Rodda et al. 2018) (Fig. 1a). FDCs and CRCs are presumably more similar to each other compared to other stromal subsets, even though some of the gene expressions are different. A large number of cells are required to distinguish these subsets in cluster analysis.
4 T Cell Zone
The T cell zone is situated in the deeper part of the cortex, where T cells and DCs accumulate. Naïve T cells actively migrate in this area for scanning antigens presented by DCs and are activated when they detect cognate antigens (Bajenoff et al. 2006; Miller et al. 2002). Therefore, the T cell zone is the center of immune surveillance mediated by T cells. The hallmark of FSCs in this area is CCL21 (Ccl21a) expression that attracts T cells and DCs via CCR7 (Luther et al. 2000; Link et al. 2007; Woolf et al. 2007). These stromal cells construct an elaborate network of extracellular matrix fiber bundle ensheathed by them, the structure known as the “conduit.” The conduit functions as a highway for transporting small molecules less than 70 kDa into the deep paracortex (Gretz et al. 1997, 2000; Sixt et al. 2005). Historically, stromal cells in the T cell zone have been termed FRCs due to their characteristic morphology. However, since stromal cells with reticular morphology are found in many other places besides the paracortex (Gretz et al. 1997), FRCs in the T cell zone are more specifically called TRCs (Link et al. 2007).
Recent reports independently suggested that TRCs can be further divided into several subpopulations. Based on single-cell analysis, Rodda et al. proposed three TRC subsets, CCL19hi, CCL19lo, and CXCL9+ TRCs (Rodda et al. 2018). Huang et al. also showed three subsets, CCL21–CXCL13–, CCL21–CXCL13+, and CCL21+CXCL13– TRCs (Huang et al. 2018). From histological observations, a unique stromal subset expressing CCL21 and CXCL12 was identified in the cortex-medulla boundary (Takeuchi et al. 2018). Here, we discuss the relevance of these reports, together with the reanalysis of the single-cell dataset.
4.1 CCL19hi TRC
CCL19hi TRCs are the most distinct subset expressing typical markers of T zone stromal cells (Rodda et al. 2018) (Figs. 1a and 2a). As CCL19hi TRCs are the primary CCL21 producers, they are likely the equivalent of CCL21+CXCL13– TRC (Huang et al. 2018) (Table 1). CCL21 proteins bound on the surface of TRCs and high endothelial venule through glycosaminoglycans (GAGs) play crucial roles in recruitment and interstitial migration of T cells and DCs (Handel et al. 2005; Woolf et al. 2007). DC migration is also regulated by podoplanin (PDPN), in agreement with the enrichment of PDPN expression in CCL19hi TRCs (Rodda et al. 2018) (Figs. 1b and 2a). By using C-type lectin receptor CLEC-2 that binds to PDPN, DCs can spread and migrate along with stromal cells (Acton et al. 2014). Additionally, engagement of PDPN and CLEC-2 is necessary to control the TRC network as an optimal niche (Astarita et al. 2015). Under resting conditions, TRCs have less opportunity to encounter CLEC-2+ mature DCs, thereby PDPN keeps actomyosin contractility in TRCs. When immune response arises, CLEC-2 on DCs causes actomyosin relaxing via PDPN and allows the TRC network to stretch. CLEC-2–PDPN axis also controls ECM production and deposition by TRCs (Martinez et al. 2019).
CXCL9+ TRCs were identified as a cluster in the first single-cell and histological analysis observed in the T cell zone and interfollicular regions (IFRs) (Rodda et al. 2018). They express type 1 IFN, IFN-γ receptors, and some IFN inducible genes. It was also reported that IFN-γ induces CXCL9 production in stromal cells for recruiting memory CD8+ T cells to the periphery of the T cell zone (Sung et al. 2012). Accordingly, CXCL9+ TRCs are suggested to be an activated fraction of CCL19hi TRCs (Rodda et al. 2018). In our reanalysis, CXCL9+ TRCs did not form an independent cluster, but instead, they were mostly included in the Ccl19hi TRC fraction (Fig. 1a, b). Thus, it is still unclear whether CXCL9+ TRCs constitute an individual subset for constructing a specialized niche.
4.2 CCL19lo TRC
CCL19lo TRCs express several genes characteristics of both in the T cell zone and follicles, such as CCL21, IL-7, and CXCL13 (Rodda et al. 2018) (Figs. 1b and 2a). Additionally, CCL19lo TRCs highly express BAFF (Tnfsf13b), a cytokine critical for B cell survival. Therefore, it is reasonable that CCL19lo TRCs possibly reside in the IFR and follicle-T zone interface (FTI), making a niche for engaging B and T cells. Previous reports showed that activated B and T cells express EBI2 (Gpr183), a receptor involved in guiding B cells to the outer follicle (Li et al. 2016; Pereira et al. 2009). An EBI2 ligand, 7α,25-dihydroxycholesterol (7α,25-HC) is synthesized by cholesterol-25-hydroxylase (Ch25h) (Hannedouche et al. 2011; Liu et al. 2011; Yi et al. 2012; Li et al. 2016) that is detected in the surrounding of follicles; IFRs and FTI, as well as the SCS-lining (Rodda et al. 2018). Reanalysis of single-cell datasets successfully detected Ch25h expression in CCL19lo TRCs as well as MRCs (Fig. 1c). These findings suggest the perifollicular distribution of CCL19lo TRCs.
Huang et al. identified CXCL13-producing TRC (CCL21–CXCL13+ TRC) (Huang et al. 2018). Several reports suggest that CXCL13+ FRCs reside in the outer follicle and co-express BAFF, Delta like-4 (DL-4), and Ch25h (Cremasco et al. 2014; Fasnacht et al. 2014; Malhotra et al. 2012; Mionnet et al. 2013; Yi et al. 2012). Huang et al., therefore, proposed to call them “B zone reticular cells (BRCs)” (Huang et al. 2018). However, the anatomical location and gene expression profiles suggest that this population is likely to be CCL19lo TRCs (Table 1). The IFR and FTI correspond to a region named the cortical ridge (CR), where a dense reticular network supports DC–T–B interactions (Bajenoff et al. 2003; Katakai et al. 2004). It will be interesting to determine if the CR has some relevance to CCL19lo TRCs as a functional subcompartment.
4.3 Deep Cortex Periphery Reticular Cell (DRC)
Based on histological examinations, Sainte-Marie et al. reported a tissue layer with dense reticulum at the boundary of the cortex and medulla, named “deep cortex periphery (DCP)” (Belisle et al. 1982; Sainte-Marie 2010). We recently found that B cells accumulate in the DCP in a CCL21- and CXCL12-dependent manner (Takeuchi et al. 2018). Stromal cells in the DCP showed unique properties to form a dense network expressing both CCL21 and CXCL12, allowing us to define them as a new subset named “DCP reticular cells (DRCs).” Interestingly, B and T cells are intermingled in this area, in marked contrast to the follicles. B cells in the DCP migrate at a slower velocity and higher turning angle than that in the follicles, suggesting that DRCs provide a specialized microenvironment. The optimal development of DCP involves B cells, because DCP formation was attenuated in B cell-deficient mice but restored by bone marrow transfer. These results suggest that DRCs require signals from B cells to construct the DCP (Takeuchi et al. 2018).
In the first single-cell analysis, no prominent cluster corresponding to DRCs was detected (Rodda et al. 2018). However, in our reanalysis, another CCL19lo cluster was found in addition to CCL19loCh25h+ TRCs (Fig. 1a, c). We considered that the new cluster represented DRCs because of high CXCL12 and CCL21 expression (Fig. 2a). Meanwhile, this cluster also showed the highest IL-7 expression in all stromal clusters (Figs. 1b and 2a). Immunohistochemical analysis using IL-7 reporter mice demonstrated that IL-7 expression was prominent in the DCP compared with other parts of LN (Fig. 2b), which convinced us that this cluster could be assigned as DRCs. DRC cluster shared some features with CCL19lo TRCs, such as the expression of BAFF (Fig. 2a). These suggest that the DCP area supported by DRCs is a niche suitable for lymphocyte survival. Contrarily, Ch25h expression was weak in DRCs (Fig. 1c), suggesting that DRCs and CCL19lo TRCs are likely to differ in function during immune responses.
5 Medullary Cord
Lymphocytes are highly concentrated in the cortex, whereas the medulla appears to have relatively low cell density due to the abundance of lymphatic sinus called the medullary sinus (MS). In the medulla, mesenchymal cells are mostly assembled to form the medullary cords (MCs); these are sheath-like parenchymal structures surrounding blood vessels (Ohtani and Ohtani 2008). It was considered that medullary FSCs were distinct from other subsets as this region harbors completely different types of immune cells, such as macrophages, NK cells, and plasma cells (Gray and Cyster 2012; Hargreaves et al. 2001; Kastenmuller et al. 2012; Katakai et al. 2004). However, their precise nature had remained unclear until recently.
5.1 Medullary Cord Reticular Cell (MCRC)
Huang et al. intensively characterized reticular stromal cells in the MCs (MedRCs) as a new subset with the ability to regulate plasma cell homeostasis (Huang et al. 2018). MedRCs differ from TRCs in terms of lower expressions of CCL21, CXCL13, CCL19, and IL-7, but a higher IL-6. MedRCs are the primary source of IL-6, BAFF, and CXCL12, besides also producing APRIL (Cyster 2005; Mohr et al. 2009; Abe et al. 2012). Among these, IL-6 is especially important for the differentiation and survival of plasma cells, since the inhibition of IL-6, but not BAFF, APRIL, and CXCL12, block those events. On the other hand, homing and localization of plasma cells in the MCs depends on the CXCL12-CXCR4 axis (Hargreaves et al. 2001; Cyster 2005). MedRCs express a higher CXCL12 but lower CCL21 and CXCL13 than other subsets (Fig. 2a). Such a profile of chemokine expression is likely to attract plasma cells and macrophages expressing high CXCR4 but low CCR7 and CXCR5.
Huang et al. suggested that MedRCs are composed of two subpopulations, CCL21+CXCL13– and CCX21–CXCL13+ cells (Huang et al. 2018). From a single-cell analysis, Rodda et al. also showed two subsets of medullary stromal cells; Inmt+ and Nr4a1+ SCs. They suggested a possibility that Nr4a1+ SCs are the activated phenotype of other subsets, including Inmt+ SCs (Rodda et al. 2018). Interestingly, in the reanalysis of a single-cell dataset, Inmt and Nr4a1 were broadly expressed in two medullary clusters rather than enriched in either of the clusters (Fig. 1a, b). We have independently identified an FSC subset in the MC; the MCRCs categorized as CXCL12hiCCL21lowLepr+ cells (Takeuchi et al. 2018). Of note, the two medullary clusters corresponded with Leprhi and Leprlo fractions (Figs. 1b and 2c). Histological observations indicated that the MCs could be roughly separated into Leprhi and Leprlo areas, which appeared to correlate with the localization of plasma cells and B cells, respectively (Fig. 2c). Therefore, two types of MCRCs possibly represent different niches within the MCs.
6 Concluding Remarks
Integrating the three core reports and other previous knowledge led to a comprehensive picture of LN architecture founded upon stromal cell diversity. We thereby propose the latest model of the stromal structure, in which at least eight FSC subsets tightly associated with subcompartments construct a functionally organized “niche complex” (Table 1, Fig. 3). Additionally, closely related subsets in major areas of LN can be classified into three upper categories; classes “B (B cell follicle),” “T (T cell zone),” and “M (medulla).”
Within the B cell follicles, the “class B” members MRCs, FDCs, and CRCs support distinct follicular niches. The functions of MRCs are gradually uncovered recently, in particular, the control of niches in the antigenic entry site via RANKL expression. FDCs constitute a prominent structure in the follicular center and GC-LZ, which is reflected by a discrete cluster expressing a variety of specific genes in single-cell analysis. In contrast, even though CRCs are histologically apparent in the inner follicle or GC-DZ, the corresponding cluster is currently undetected in single-cell analysis, probably due to the limited cell number of the datasets.
The “class T” includes FSC subsets in the T cell zone, CCL19hi TRCs, CCL19lo TRCs, and DRCs. The hallmark of these subsets is CCL21 expression. CCL19hi TRCs constitute the center body of the T cell zone by highly producing CCL19 as well as CCL21. In concert with CLEC-2+ DCs, PDPN highly expressed in this subset is suggested to control the scale of the stromal network. CCL19lo TRCs are likely the stromal component of the IFR and FTI (CR), providing a niche for B and T cell engagement. DRCs support the DCP area associated with B cell accumulation at the periphery of the deep T cell zone. Although DRCs highly express various survival factors for lymphocytes, it is still unclear why B cells need to be attracted to the opposite side of the follicles near the medulla.
Stromal cells of the medulla could be categorized as “class M” subsets providing a niche for plasma cells and medullary macrophages. Two types of FSCs possibly constitute distinct areas within the MC; LeprhiCCL19+ MCRCs and Leprlo MCRCs appear to correlate with the accumulations of plasma cells and B cells, respectively. There are some discrepancies between reports; however, the MCs are presumably composed of more than one FSC subset.
The subset composition of LN stromal cells in its entirety is surprisingly complicated and diverse to form functionally different subcompartments. Such a stromal cell diversity is probably indispensable to control elaborate and flexible immune responses. We speculate that the feature of each subset is not uniform nor stable but has overlaps and interchangeable property with neighboring populations. We, therefore, assume that it is possible to discover more FSC types or subsets with intermediate property, especially in the boundary of subcompartments. It is also possible that the condition of stromal cells, subset composition, or both, could be readily changed during immune responses or local stimuli. Overall, further in-depth analysis will be necessary to obtain a universal picture of the diversity and plasticity of LN FSCs.
References
Abe J, Ueha S, Yoneyama H, Shono Y, Kurachi M, Goto A, Fukayama M, Tomura M, Kakimi K, Matsushima K (2012) B cells regulate antibody responses through the medullary remodeling of inflamed lymph nodes. Int Immunol 24:17–27
Acton SE, Farrugia AJ, Astarita JL, Mourao-Sa D, Jenkins RP, Nye E, Hooper S, van Blijswijk J, Rogers NC, Snelgrove KJ, Rosewell I, Moita LF, Stamp G, Turley SJ, Sahai E, Reis e Sousa C (2014) Dendritic cells control fibroblastic reticular network tension and lymph node expansion. Nature 514:498–502
Allen CD, Ansel KM, Low C, Lesley R, Tamamura H, Fujii N, Cyster JG (2004) Germinal center dark and light zone organization is mediated by CXCR4 and CXCR5. Nat Immunol 5:943–952
Allen CD, Cyster JG (2008) Follicular dendritic cell networks of primary follicles and germinal centers: phenotype and function. Semin Immunol 20:14–25
Allen CD, Okada T, Cyster JG (2007) Germinal-center organization and cellular dynamics. Immunity 27:190–202
Ansel KM, Ngo VN, Hyman PL, Luther SA, Forster R, Sedgwick JD, Browning JL, Lipp M, Cyster JG (2000) A chemokine-driven positive feedback loop organizes lymphoid follicles. Nature 406:309–314
Astarita JL, Cremasco V, Fu J, Darnell MC, Peck JR, Nieves-Bonilla JM, Song K, Kondo Y, Woodruff MC, Gogineni A, Onder L, Ludewig B, Weimer RM, Carroll MC, Mooney DJ, Xia L, Turley SJ (2015) The CLEC-2-podoplanin axis controls the contractility of fibroblastic reticular cells and lymph node microarchitecture. Nat Immunol 16:75–84
Bajenoff M, Egen JG, Koo LY, Laugier JP, Brau F, Glaichenhaus N, Germain RN (2006) Stromal cell networks regulate lymphocyte entry, migration, and territoriality in lymph nodes. Immunity 25:989–1001
Bajenoff M, Granjeaud S, Guerder S (2003) The strategy of T cell antigen-presenting cell encounter in antigen-draining lymph nodes revealed by imaging of initial T cell activation. J Exp Med 198:715–724
Bannard O, Horton RM, Allen CD, An J, Nagasawa T, Cyster JG (2013) Germinal center centroblasts transition to a centrocyte phenotype according to a timed program and depend on the dark zone for effective selection. Immunity 39:912–924
Barrington RA, Pozdnyakova O, Zafari MR, Benjamin CD, Carroll MC (2002) B lymphocyte memory: role of stromal cell complement and FcgammaRIIB receptors. J Exp Med 196:1189–1199
Belisle C, Sainte-Marie G (1981) Topography of the deep cortex of the lymph nodes of various mammalian species. Anat Rec 201:553–561
Belisle C, Sainte-Marie G, Peng FS (1982) Tridimensional study of the deep cortex of the rat lymph node. VI. The deep cortex units of the germ-free rat. Am J Pathol 107:70–78
Camara A, Cordeiro OG, Alloush F, Sponsel J, Chypre M, Onder L, Asano K, Tanaka M, Yagita H, Ludewig B, Flacher V, Mueller CG (2019) Lymph node mesenchymal and endothelial stromal cells cooperate via the RANK-RANKL cytokine axis to shape the sinusoidal macrophage niche. Immunity 50:1467–1481 e1466
Carrasco YR, Batista FD (2007) B cells acquire particulate antigen in a macrophage-rich area at the boundary between the follicle and the subcapsular sinus of the lymph node. Immunity 27:160–171
Carroll MC, Isenman DE (2012) Regulation of humoral immunity by complement. Immunity 37:199–207
Chatziandreou N, Farsakoglu Y, Palomino-Segura M, D’Antuono R, Pizzagalli DU, Sallusto F, Lukacs-Kornek V, Uguccioni M, Corti D, Turley SJ, Lanzavecchia A, Carroll MC, Gonzalez SF (2017) Macrophage death following influenza vaccination initiates the inflammatory response that promotes dendritic cell function in the draining lymph node. Cell Rep 18:2427–2440
Chen LL, Frank AM, Adams JC, Steinman RM (1978) Distribution of horseradish peroxidase (HRP)-anti-HRP immune complexes in mouse spleen with special reference to follicular dendritic cells. J Cell Biol 79:184–199
Cremasco V, Woodruff MC, Onder L, Cupovic J, Nieves-Bonilla JM, Schildberg FA, Chang J, Cremasco F, Harvey CJ, Wucherpfennig K, Ludewig B, Carroll MC, Turley SJ (2014) B cell homeostasis and follicle confines are governed by fibroblastic reticular cells. Nat Immunol 15:973–981
Cyster JG (1999) Chemokines and cell migration in secondary lymphoid organs. Science 286:2098–2102
Cyster JG (2005) Chemokines, sphingosine-1-phosphate, and cell migration in secondary lymphoid organs. Annu Rev Immunol 23:127–159
Cyster JG, Ansel KM, Reif K, Ekland EH, Hyman PL, Tang HL, Luther SA, Ngo VN (2000) Follicular stromal cells and lymphocyte homing to follicles. Immunol Rev 176:181–193
Fasnacht N, Huang HY, Koch U, Favre S, Auderset F, Chai Q, Onder L, Kallert S, Pinschewer DD, MacDonald HR, Tacchini-Cottier F, Ludewig B, Luther SA, Radtke F (2014) Specific fibroblastic niches in secondary lymphoid organs orchestrate distinct Notch-regulated immune responses. J Exp Med 211:2265–2279
Gray EE, Cyster JG (2012) Lymph node macrophages. J Innate Immun 4:424–436
Gretz JE, Anderson AO, Shaw S (1997) Cords, channels, corridors and conduits: critical architectural elements facilitating cell interactions in the lymph node cortex. Immunol Rev 156:11–24
Gretz JE, Norbury CC, Anderson AO, Proudfoot AE, Shaw S (2000) Lymph-borne chemokines and other low molecular weight molecules reach high endothelial venules via specialized conduits while a functional barrier limits access to the lymphocyte microenvironments in lymph node cortex. J Exp Med 192:1425–1440
Handel TM, Johnson Z, Crown SE, Lau EK, Proudfoot AE (2005) Regulation of protein function by glycosaminoglycans–as exemplified by chemokines. Annu Rev Biochem 74:385–410
Hannedouche S, Zhang J, Yi T, Shen W, Nguyen D, Pereira JP, Guerini D, Baumgarten BU, Roggo S, Wen B, Knochenmuss R, Noel S, Gessier F, Kelly LM, Vanek M, Laurent S, Preuss I, Miault C, Christen I, Karuna R, Li W, Koo DI, Suply T, Schmedt C, Peters EC, Falchetto R, Katopodis A, Spanka C, Roy MO, Detheux M, Chen YA, Schultz PG, Cho CY, Seuwen K, Cyster JG, Sailer AW (2011) Oxysterols direct immune cell migration via EBI2. Nature 475:524–527
Hara T, Shitara S, Imai K, Miyachi H, Kitano S, Yao H, Tani-ichi S, Ikuta K (2012) Identification of IL-7-producing cells in primary and secondary lymphoid organs using IL-7-GFP knock-in mice. J Immunol 189:1577–1584
Hargreaves DC, Hyman PL, Lu TT, Ngo VN, Bidgol A, Suzuki G, Zou YR, Littman DR, Cyster JG (2001) A coordinated change in chemokine responsiveness guides plasma cell movements. J Exp Med 194:45–56
Hoorweg K, Narang P, Li Z, Thuery A, Papazian N, Withers DR, Coles MC, Cupedo T (2015) A stromal cell niche for human and mouse type 3 innate lymphoid cells. J Immunol 195:4257–4263
Huang HY, Rivas-Caicedo A, Renevey F, Cannelle H, Peranzoni E, Scarpellino L, Hardie DL, Pommier A, Schaeuble K, Favre S, Vogt TK, Arenzana-Seisdedos F, Schneider P, Buckley CD, Donnadieu E, Luther SA (2018) Identification of a new subset of lymph node stromal cells involved in regulating plasma cell homeostasis. Proc Natl Acad Sci U S A 115:E6826–E6835
Humphrey JH, Grennan D (1982) Isolation and properties of spleen follicular dendritic cells. Adv Exp Med Biol 149:823–827
Jarjour M, Jorquera A, Mondor I, Wienert S, Narang P, Coles MC, Klauschen F, Bajenoff M (2014) Fate mapping reveals origin and dynamics of lymph node follicular dendritic cells. J Exp Med 211:1109–1122
Kastenmuller W, Torabi-Parizi P, Subramanian N, Lammermann T, Germain RN (2012) A spatially-organized multicellular innate immune response in lymph nodes limits systemic pathogen spread. Cell 150:1235–1248
Katakai T (2016) Stromal cells in secondary lymphoid organs. Encyclopedia of Immunobiology 3:473
Katakai T (2012) Marginal reticular cells: a stromal subset directly descended from the lymphoid tissue organizer. Front Immunol 3:200
Katakai T, Hara T, Lee JH, Gonda H, Sugai M, Shimizu A (2004) A novel reticular stromal structure in lymph node cortex: an immuno-platform for interactions among dendritic cells, T cells and B cells. Int Immunol 16:1133–1142
Katakai T, Suto H, Sugai M, Gonda H, Togawa A, Suematsu S, Ebisuno Y, Katagiri K, Kinashi T, Shimizu A (2008) Organizer-like reticular stromal cell layer common to adult secondary lymphoid organs. J Immunol 181:6189–6200
Li J, Lu E, Yi T, Cyster JG (2016) EBI2 augments Tfh cell fate by promoting interaction with IL-2-quenching dendritic cells. Nature 533:110–114
Link A, Vogt TK, Favre S, Britschgi MR, Acha-Orbea H, Hinz B, Cyster JG, Luther SA (2007) Fibroblastic reticular cells in lymph nodes regulate the homeostasis of naive T cells. Nat Immunol 8:1255–1265
Liu C, Yang XV, Wu J, Kuei C, Mani NS, Zhang L, Yu J, Sutton SW, Qin N, Banie H, Karlsson L, Sun S, Lovenberg TW (2011) Oxysterols direct B-cell migration through EBI2. Nature 475:519–523
Luther SA, Tang HL, Hyman PL, Farr AG, Cyster JG (2000) Coexpression of the chemokines ELC and SLC by T zone stromal cells and deletion of the ELC gene in the plt/plt mouse. Proc Natl Acad Sci U S A 97:12694–12699
Malhotra D, Fletcher AL, Astarita J, Lukacs-Kornek V, Tayalia P, Gonzalez SF, Elpek KG, Chang SK, Knoblich K, Hemler ME, Brenner MB, Carroll MC, Mooney DJ, Turley SJ, Immunological Genome Project C (2012) Transcriptional profiling of stroma from inflamed and resting lymph nodes defines immunological hallmarks. Nat Immunol 13:499–510
Martinez VG, Pankova V, Krasny L, Singh T, Makris S, White IJ, Benjamin AC, Dertschnig S, Horsnell HL, Kriston-Vizi J, Burden JJ, Huang PH, Tape CJ, Acton SE (2019) Fibroblastic reticular cells control conduit matrix deposition during lymph node expansion. Cell Rep 29:2810–2822 e2815
Matsumoto M, Fu YX, Molina H, Huang G, Kim J, Thomas DA, Nahm MH, Chaplin DD (1997) Distinct roles of lymphotoxin alpha and the type I tumor necrosis factor (TNF) receptor in the establishment of follicular dendritic cells from non-bone marrow-derived cells. J Exp Med 186:1997–2004
McHeyzer-Williams M, Okitsu S, Wang N, McHeyzer-Williams L (2011) Molecular programming of B cell memory. Nat Rev Immunol 12:24–34
Miller MJ, Wei SH, Parker I, Cahalan MD (2002) Two-photon imaging of lymphocyte motility and antigen response in intact lymph node. Science 296:1869–1873
Mionnet C, Mondor I, Jorquera A, Loosveld M, Maurizio J, Arcangeli ML, Ruddle NH, Nowak J, Aurrand-Lions M, Luche H, Bajenoff M (2013) Identification of a new stromal cell type involved in the regulation of inflamed B cell follicles. PLoS Biol 11:e1001672
Mohr E, Serre K, Manz RA, Cunningham AF, Khan M, Hardie DL, Bird R, MacLennan IC (2009) Dendritic cells and monocyte/macrophages that create the IL-6/APRIL-rich lymph node microenvironments where plasmablasts mature. J Immunol 182:2113–2123
Mueller SN, Germain RN (2009) Stromal cell contributions to the homeostasis and functionality of the immune system. Nat Rev Immunol 9:618–629
Ohtani O, Ohtani Y (2008) Structure and function of rat lymph nodes. Arch Histol Cytol 71:69–76
Papamichail M, Gutierrez C, Embling P, Johnson P, Holborow EJ, Pepys MB (1975) Complement dependence of localisation of aggregated IgG in germinal centres. Scand J Immunol 4:343–347
Pereira JP, Kelly LM, Xu Y, Cyster JG (2009) EBI2 mediates B cell segregation between the outer and centre follicle. Nature 460:1122–1126
Phan TG, Green JA, Gray EE, Xu Y, Cyster JG (2009) Immune complex relay by subcapsular sinus macrophages and noncognate B cells drives antibody affinity maturation. Nat Immunol 10:786–793
Phan TG, Grigorova I, Okada T, Cyster JG (2007) Subcapsular encounter and complement-dependent transport of immune complexes by lymph node B cells. Nat Immunol 8:992–1000
Qi H, Kastenmuller W, Germain RN (2014) Spatiotemporal basis of innate and adaptive immunity in secondary lymphoid tissue. Annu Rev Cell Dev Biol 30:141–167
Rahman ZS, Rao SP, Kalled SL, Manser T (2003) Normal induction but attenuated progression of germinal center responses in BAFF and BAFF-R signaling-deficient mice. J Exp Med 198:1157–1169
Rodda LB, Bannard O, Ludewig B, Nagasawa T, Cyster JG (2015) Phenotypic and morphological properties of germinal center dark zone Cxcl12-expressing reticular cells. J Immunol 195:4781–4791
Rodda LB, Lu E, Bennett ML, Sokol CL, Wang X, Luther SA, Barres BA, Luster AD, Ye CJ, Cyster JG (2018) Single-cell RNA sequencing of lymph node stromal cells reveals niche-associated heterogeneity. Immunity 48:1014–1028 e1016
Roozendaal R, Carroll MC (2007) Complement receptors CD21 and CD35 in humoral immunity. Immunol Rev 219:157–166
Roozendaal R, Mebius RE (2011) Stromal cell-immune cell interactions. Annu Rev Immunol 29:23–43
Sainte-Marie G (2010) The lymph node revisited: development, morphology, functioning, and role in triggering primary immune responses. Anat Rec (hoboken) 293:320–337
Schneider P, MacKay F, Steiner V, Hofmann K, Bodmer JL, Holler N, Ambrose C, Lawton P, Bixler S, Acha-Orbea H, Valmori D, Romero P, Werner-Favre C, Zubler RH, Browning JL, Tschopp J (1999) BAFF, a novel ligand of the tumor necrosis factor family, stimulates B cell growth. J Exp Med 189:1747–1756
Sitnik KM, Wendland K, Weishaupt H, Uronen-Hansson H, White AJ, Anderson G, Kotarsky K, Agace WW (2016) Context-dependent development of lymphoid stroma from adult CD34(+) adventitial progenitors. Cell Rep 14:2375–2388
Sixt M, Kanazawa N, Selg M, Samson T, Roos G, Reinhardt DP, Pabst R, Lutz MB, Sorokin L (2005) The conduit system transports soluble antigens from the afferent lymph to resident dendritic cells in the T cell area of the lymph node. Immunity 22:19–29
Stuart T, Butler A, Hoffman P, Hafemeister C, Papalexi E, Mauck WM, Hao Y, Stoeckius M, Smibert P, Satija R (2019) Comprehensive integration of single-cell data. Cell 177:1888–1902 e1821
Sung JH, Zhang H, Moseman EA, Alvarez D, Iannacone M, Henrickson SE, de la Torre JC, Groom JR, Luster AD, von Andrian UH (2012) Chemokine guidance of central memory T cells is critical for antiviral recall responses in lymph nodes. Cell 150:1249–1263
Takeuchi A, Ozawa M, Kanda Y, Kozai M, Ohigashi I, Kurosawa Y, Rahman MA, Kawamura T, Shichida Y, Umemoto E, Miyasaka M, Ludewig B, Takahama Y, Nagasawa T, Katakai T (2018) A distinct subset of fibroblastic stromal cells constitutes the cortex-medulla boundary subcompartment of the lymph node. Front Immunol 9:2196
Tew JG, Thorbecke GJ, Steinman RM (1982) Dendritic cells in the immune response: characteristics and recommended nomenclature (A report from the reticuloendothelial society committee on nomenclature). J Reticuloendothel Soc 31:371–380
Tew JG, Wu J, Fakher M, Szakal AK, Qin D (2001) Follicular dendritic cells: beyond the necessity of T-cell help. Trends Immunol 22:361–367
Victora GD, Nussenzweig MC (2012) Germinal centers. Annu Rev Immunol 30:429–457
Vora KA, Wang LC, Rao SP, Liu ZY, Majeau GR, Cutler AH, Hochman PS, Scott ML, Kalled SL (2003) Cutting edge: germinal centers formed in the absence of B cell-activating factor belonging to the TNF family exhibit impaired maturation and function. J Immunol 171:547–551
Willard-Mack CL (2006) Normal structure, function, and histology of lymph nodes. Toxicol Pathol 34:409–424
Woolf E, Grigorova I, Sagiv A, Grabovsky V, Feigelson SW, Shulman Z, Hartmann T, Sixt M, Cyster JG, Alon R (2007) Lymph node chemokines promote sustained T lymphocyte motility without triggering stable integrin adhesiveness in the absence of shear forces. Nat Immunol 8:1076–1085
Wu Y, El Shikh ME, El Sayed RM, Best AM, Szakal AK, Tew JG (2009) IL-6 produced by immune complex-activated follicular dendritic cells promotes germinal center reactions, IgG responses and somatic hypermutation. Int Immunol 21:745–756
Yi T, Wang X, Kelly LM, An J, Xu Y, Sailer AW, Gustafsson JA, Russell DW, Cyster JG (2012) Oxysterol gradient generation by lymphoid stromal cells guides activated B cell movement during humoral responses. Immunity 37:535–548
Acknowledgements
This work was funded by a Grant-in-Aid for Scientific Research (C) (A. Takeuchi, 19K07603) and a Grant-in-Aid for Challenging Exploratory Research (T. Katakai, 16K15287) from The Ministry of Education, Culture, Sports, Science and Technology of Japan.
Author’s note: Due to a significant delay in the publication process caused by the COVID-19 pandemic, the content of this paper is as of April 2020.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Takeuchi, A., Ozawa, M., Cui, G., Ikuta, K., Katakai, T. (2021). Lymph Node Stromal Cells: Diverse Meshwork Structures Weave Functionally Subdivided Niches. In: Nagasawa, T. (eds) Bone Marrow Niche. Current Topics in Microbiology and Immunology, vol 434. Springer, Cham. https://doi.org/10.1007/978-3-030-86016-5_5
Download citation
DOI: https://doi.org/10.1007/978-3-030-86016-5_5
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-86015-8
Online ISBN: 978-3-030-86016-5
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)