Abstract
Contraceptive use in early sexual life is an important health target. Adolescents often display an approach to sexuality and a perception of risk-behavior completely different from adults. For these reasons, contraceptive education and counselling require specific competences. Contextual factors, related to family situations, body dissatisfaction and low self-esteem, peer pressure, internet dependency, experiencing an asymmetric relationship, have a significant impact on protective choice and contraceptive adherence and compliance.
Furthermore, we have to consider that adolescents are still in a growing trajectory, also from a biological point of view. Therefore, we propose also a revision of the impact of various contraceptive methods on cervico-vaginal milieu, on the function of hypothalamus-pituitary- ovarian axis, on bone mineral content increase and on mood disorders.
The clinical history of our young patients should focus, with empathy, both on social and emotional situations and changes, on the need of information, and on physical maturation, together with the well-known biological risk factors, in order to direct a proper protective choice.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Adolescents
- Contraceptive need
- Psychosocial risk-factors
- Sexually transmitted infections
- Peak bone mass
- Steroid and mood
1 Introduction
Protection at sexual debut is a well-known marker of lifelong sexual health and the target of many educational projects for adolescents and of contraceptive counselling. A very young age at the approach of sexuality is often linked to unprotected sex worldwide. The proposal of Palmer [1] and coworkers to focus more on “competence” at first intercourse than on timing is probably more appropriate because it underlines the importance of contextual factors in defining the quality and safety of a sexual relationship. A competent sexual debut means that the choice is consensual, with autonomy in decision and perceived as in the right moment for both the partners, in addition to using contraceptive protection. To promote a responsible choice in approaching sexuality is the challenge for all health care personnel dealing with adolescents, during specific consultations, as well as on other occasions of meeting them (vaccinations, follow-up visits). In many countries, we still need laws and policies to counteract cultural and economic barriers preventing consistent use of contraception by young people.
Contraceptive counselling with young people should take into account both biological and contextual factors in order to develop a shared decision-making approach to help a choice responding to patient characteristics and to promote contraceptive continuation and adherence. From a practical point of view, the medical history and the socio-psychological items are generally collected together, but in our text we will synthetize first the contextual variables known to influence sexual health behaviors and the biological aspects to follow.
2 Contextual Factors Significant for Contraceptive Protection
Information: the availability of health information related to sex education programs at school, to the ability of finding reliable specific websites, and to the possibility of having help and reference in relatives or educators are, of course, preconditions for a contraceptive choice. Very young girls, migrants, and people with intellectual disabilities have fewer opportunities to reach information sources. However, we know well that in all adolescents the gap between knowledge and effective protective behaviors is anyway often deep. Educational interventions and health care consultations must focus on specific difficulties and motivations to disregard what they know about prevention of unwanted pregnancy and of sexually transmitted infections.
Family relationships: In every culture, parents transmit the models of femininity and masculinity, of their relationships and the attention to self-care. The involvement in the daughter’s life and a flexible monitoring together with an open communication about sexual and reproductive health, especially by the mother, are associated in every country with delayed sex and higher contraceptive use [2].
Attitude to risk-taking: various surveys on young people [3,4,5] demonstrated the correlation between risk behaviors and unprotected sex, precocious sexual debut and elevated sexual partner turnover. Therefore, we have to find the words to investigate on alcohol and substance abuse, on the use of the so-called new psychoactive drugs, mixtures of herbs, dusts, crystals, or tablets partially reproducing the effects of cannabis, ecstasy, or other substances. The attitude to risk in young people is mainly related to the need to be similar or considered by peers, sometimes is a component of pleasure or a hidden way to seek help. Longitudinal studies demonstrated that adolescents living in a conflicting or inattentive family milieu, in financial hardship, or with a history of adverse childhood events are more vulnerable to risky behaviors. Most risk-behaviors tend to be associated with depression and correlate with the severity of depressive symptomatology [6]. Poor personal or professional projects, more than school results, can be an indirect measure of self-esteem and of a positive attitude toward life.
A negative body image, related to overweight [7], dermatological diseases, chronic diseases interfering with everyday life, are also linked to low self-esteem, depressive thoughts and can potentially lead to disordered eating and sexual risk behaviors. A strict correlation between having positive feelings about one’s body and oneself and sexual assertiveness, that include the ability to negotiate condom or contraception, has been demonstrated [8].
Problematic internet use is recently considered a risk factor also for sexual behavior [9]. The web is worldwide the place for shopping, meetings, cyberbullying, gambling, but also where it is possible to meet virtual or real sexual partners. Social networks consent a very high number of contacts, reducing a genuine interpersonal communication and spread the idea that everything is public and representable, rarefying the space of privacy and intimacy. Sexting, i.e., the sending of sexually explicit digital images or videos by cell phone, usually in order to seek attention, is related to higher exposure to sexual violence or coercion [10]. It is, therefore, important to rule out a pervasive use of media devices. Considering that about 70% of teenagers use the smartphone during the night, questions about sleep quality are good markers of internet dependence [11].
The characteristics of the couple and the partner: gender norms and attitudes, as Global Early Adolescent Study demonstrated [12], are shaped in early adolescence and impact on first intimate relationships. Currently, peer narratives and experiences and social networks influence generally reinforce traditional gender roles. Partners acting stereotyped masculine role tend to communicate less about sex, to boycott contraception, to act unrealistic pregnancy promoting behaviors and sometimes to impose intercourses [13]. So exploring pregnancy intention and opinions about contraception of the male partner may help to identify girls at risk of unwanted pregnancy, sexually transmitted infections, and intimate partner violence. Sexual coercion, that is quite frequent in adolescent relationships, impact also on future sexual functioning and health protecting behaviors.
In our personal framework of interview for evaluating adolescent contraceptive needs, we have to include the preceding items if we want to identify elements affecting both starting and continuing contraception, as well as biological factors affecting the choice of the method.
3 Critical Biological Issues in Adolescents
The immaturity of cervico-vaginal epithelium and the exposure to Sexually Transmitted Infection (STI) risk.
Reports from various European and non-European countries put in evidence that prevalence of Chlamydia, as well as Gonorrhea infections in young people is still increasing. This increase is probably in part the result of more diagnostic efforts and of the use of more sensitive diagnostic tests, but also of a wide diffusion facilitated by the high rate of asymptomatic infections.
Biological factors related to the immaturity of the cervical-vaginal epithelium should also be taken into account. The extension of columnar epithelium, that is by nature more immune tolerant, is prevalent in adolescent girls compared to squamous esocervical and vaginal epithelium, more efficient in response to pathogens, especially Chlamydia and Gonorrhea [14]. The junction between squamous and mucous-secreting epithelia (cervical transformation zone) is particularly dynamic in post-menarchal years. An estrogen-dependent metaplastic process occurs with progressive replacement of columnar epithelium by squamous foci, driven by specific reserve junctional cells. The proliferation and differentiation of these reserve cells increase the susceptibility to HPV infection through a deficient expression of innate molecules inhibiting the intracellular steps of virus processing [15]. Few components of cell-mediate immune response (T lymphocytes, and antigen-presenting cells) are also prevalent in the transformation zone and surrounding tissues; therefore, this is also the primary infection site of HIV virus [16].
The production of antimicrobial substances and the acquired immune response are less efficient in adolescents than in adult subjects: IgG and IgA secreting plasma cells are reduced. Bacterial species associated with vaginal microbiota of adolescents resemble those of adults; including lactobacillus crispatus, L. iners, L. gasser, L. Jensenii, and Gardnerella vaginalis, but vaginal pH often remains above what is considered typical in healthy women [17].
Younger sexually inactive girls are at increased risk of infections upon sexual debut [18]. Disruption of the epithelial barrier that may occur in response to seminal plasma cytokines or to micro traumas related to nonconsensual sex is another risk factor. The not rare comorbidity between different infections, increasing inflammatory state, or activating Langherans cells, enhances the risk of extension and complication of the symptomatology. Smoking is an additional risk factor, because nicotine, and its metabolite cotinine, concentrate in cervical mucus more than in blood promoting cell proliferations and suppression of specific cytokines [19]. Cannabis and other psychoactive drugs also reveal immunosuppressive activity.
Finally, the perception of sexuality as a field of curiosity and experimentation promote in adolescents the trend to multiple sexual partners, sequentially or concurrently, often with inconsistent protection.
An evaluation of the risk of STI is part of the contraceptive counseling at any age, but particularly with adolescents. The known risk factors are an early sexual debut, more than three sexual partners in the last year, using dating apps, previous sexually transmitted infection, condom misuse, selling sex, together with poor information on the topic. Probably these appear as hard questions to ask, but if well motivated, are generally accepted by young people. Sometimes the starting of a hormonal contraception after a period of condom use is the circumstance of acquisition from the partner of a silent infection and breakthrough bleeding is the sign of endometrial involvement. The best strategy should be to foster condom use, especially at the beginning of a relationship, before eventual test for STIs, even in association, for subjects using either SARC or LARC. Encouraging condom use means also promoting positive peer norms regarding mechanical protection and improving communications about its correct use.
Evidence on the association between specific contraceptive method and risk of STI is lacking, with few perspective studies. We know that the use of combined hormonal contraceptives generally increases the presence of a healthy vaginal microbiome with H2O2 producing Lactobacilli species and decreases the vaginosis-associated bacterial taxa [20]. The impact of intrauterine contraception is less clear: probably a short-term decrease in lactobacilli colonization is present with a trend to a restoration during time [21]. A highlighting of a possible facilitating effect on endocervical persistence of Chlamydia through a mechanism distinct from vaginal microbial alterations has been reported [22]. In a case-control prospective study, Cu IUD users have higher HPV clearance rates in comparison with non-users [23]. Recent evidence supports an increased risk of Herpes virus two infections among DMPA users [24].
Contrary to diffuse belief, there are no clinical or epidemiological data pointing out that the risk of acquisition or of pelvic complications of sexual infections using intrauterine contraception or systemic hormonal contraception [25, 26]. So in young people, increasing the awareness of the diffusion of sexual pathogens and facilitating diagnostic testing and condom use are the cornerstones of prevention, independently of contraceptive choice.
3.1 Immaturity of Hypothalamic Pituitary Ovarian Axis
During the first postmenarchal years, menstrual disorders are frequent; but a large proportion of healthy adolescent girls with irregular menstrual cycles are still ovulating despite infrequent menses [27]. Young girls with anovulatory cycles or ovulatory cycles with a short luteal phase do not display differences in length from normal ovulatory cycles. Adolescents with ovulatory cycles demonstrate a mature feedback to estradiol, but continue to have lower gonadotropin levels, diminished ovarian responsiveness, and decreased corpus luteum sex steroid synthesis compared with adults, indicating that reproductive axis maturity still requires a complete development of all components of the hypothalamic–pituitary–ovarian axis [28]. A recent study demonstrates the possibility of induction of LH surge using transdermal estradiol (200 ore 300 μg according to body surface for 7 days) even in premenarchal girls [29], indicating an early maturation of hypothalamic sensitivity to ovarian hormones.
Few longitudinal studies pointed out the possibility of a dys-synchrony between central and peripheral maturation: the neuroendocrine mechanisms of GnRH regulation are rapidly established, while the ovarian follicular structures may be still immature [30, 31]. The interaction between oocyte, granulosa, and theca cells may evolve through an increase in thecal androgen production probably related to impaired aromatase activity, with consequent reduced progression of antral follicles and oligomenorrhea. AMH, secreted from granulosa cells, seems to play a critical role, inhibiting FSH action on follicle growth. The ovarian functional pattern of postmenarchal oligomenorrhea generally evolves during time in normal ovulatory cycles, even if a persistence of increased androgen production and menstrual irregularity has been described in the 12% of subjects [32].
Weight modifications are important determinants of menstrual function in this period of life. Low BMI, generally related to reduced energy availability for eating disorders or excess of physical acitivity, has more impact on hypothalamic centers. Weight increase, especially in subjects with genetic or epigenetic predisposition to polycystic ovary syndrome, accentuates ovarian androgen productions and slows down follicular maturation.
Data on adult women demonstrated that there is no impact of hormonal contraception on long-term fecundity [33, 34]. A possible impact of the use of contraceptives inhibiting ovulation on hypothalamic-pituitary axis maturation in very young people is sometimes proposed as a matter of concern. A longitudinal study performed in the past did not find any modifications of hypothalamic-pituitary function before and after the use of combined hormonal contraceptives, in agreement with what we know now about the precocious maturity of neuroendocrine centers [35]. Anyway, before prescribing hormonal contraception to girls with menstrual disorders, it is advisable to understand, with a careful medical history (Table 13.1), the causes of the dysfunction and to identify eating disorders, even if atypical. If we suspect an energy deficiency related to restrictive eating behavior, strenuous physical activity, pathologies causing malabsorption or other chronic diseases that affect menstrual function together with bone structure [36], it is mandatory to elaborate a therapeutic project and share its objectives with the girl, at the same time of contraceptive options.
Postmenarchal oligomenorrhea may also reveal girls at risk of developing a Polycystic Ovary Syndrome (PCOS) phenotype: exposure to androgens in the intrauterine life [37], as daughters of PCOS mothers, low birth weight, and precocious catch-up growth, subject with premature adrenarche [38], visceral adiposity or elevated insulin levels. In presence of clinical signs or of biochemical evidences of androgen excess, a diagnosis of PCOS is sometimes already possible. In all these subjects, the use of hormonal contraception reduces ovarian androgen production [39], even if a minimal follicular development is still present during treatment, with minimal impact on metabolism. If they are motivated to follow indications about their lifestyle (physical activity, a nutrition program), ovarian functionality will improve under treatment.
So contraceptive consultation becomes also an opportunity to evaluate adolescent menstrual disorders.
3.2 Attainment of Peak Bone Mass
Peak bone mass is the amount of bone acquired when accrual ceases or plateaus after completion of growth. The greatest gain in bone mass in girls occurs approximately 6 months after the pubertal growth spurt, but the increase in bone mineral content continues in the years following the menarche. Timing and determinants of bone acquisition in late adolescence are not completely understood. The exact age when bone mass reaches its peak in various skeletal sites is not clearly defined, but probably for femoral neck, total hip, and spine by 20 years [40] and beyond 30 years for the skull.
Cortical and trabecular components of the bone differ in their responsiveness to disease effects, medications, muscle-loading, and mechanical loading related to physical activity, and hormonal changes. Up to 80% of bone mineral density is genetically determined, while lifestyle (Table 13.2) influences 20–30% of adult peak bone mass [41]. Bone growth, repair, and adaptation to mechanical stimuli are regulated by the structure and the cells of the periosteal membrane. Steroid hormones (androgens and estrogens) have physiologically important effects on periosteal function in adolescence. Estrogens have a biphasic action, with low levels stimulating the periosteal expansion through the increase in the sensitivity for mechanical stimuli and for the effect of IGF-1. On the other hand, high estrogen levels inhibit periosteal bone formation.
At least 14 longitudinal studies investigated the effect of precocious assumption of hormonal contraceptives on bone accrual with different results, but most of them suggested that in young girls the increase of Bone Mineral Density (BMD) could be lower in CHC users than in non-users. WHO Medical Eligibility Criteria (WHO MEC) for Contraceptive Use published in 2015, focusing specifically on the fracture risk, stated that evidence on fracture risk is inconsistent, even if hormonal contraceptives may decrease bone mineral density in adolescents. Considering progestin only contraception, WHO MEC put in evidence that an effect on BMD is also documented for DMPA users and it is unclear whether adolescents can reach peak bone mass after discontinuation. A recent meta-analysis [42] on eight selected studies showed a weighted mean BMD difference at lumbar spine in 1535 adolescents of -0.02 g/cm2 after 12 months (P = 0.04). The 24-month LS meta-analysis with five paired comparisons in 885 adolescents showed a highly significant weighted mean BMD difference of -0.02 g/cm2 in CHC-exposed adolescents (P = 0.0006).
The discussion about these results is also related to the methodology of evaluation: dual-energy X-ray absorptiometry (DXA) evaluates bone density as a ratio between bone mineral content and bone area measurements. Areal BMD is not a volumetric density, it is influenced by vertebral sizes and displays a trend to a continuous increase during growth. Furthermore, bone mineralization is only one determinant of bone health and fragility and does not always reflect the risk of fracture [43].
Even if an impact of precocious hormonal contraception on bone is probable, as a recent document of The Faculty of Sexual and Reproductive Healthcare (FSRH) reminds [44], data present in the literature do not give us information about a “safe” gynecological age for starting contraceptives or about reversibility of their effect. Moreover, we miss clear evidences about the differences between various ethinyl-estradiol dosages, between ethinyl-estradiol and natural estrogens, and between different progestins. Therefore, we currently do not know if specific associations can be considered “neutral” for adolescent bone mass accrual. For this reason, it is important, in the clinical history, to focus on other factors affecting bone mineralization, such as disordered eating, in order to increase the awareness on the central role of adolescent age in building bone for life.
3.3 Mood and Hormonal Contraception
Mood changes in women under treatment with hormonal contraceptives have become an important issue in recent years, and it concerns both CHC and progestin-only methods. The relationship between mood and hormonal contraception treatments is complex. We know that sex steroids and the metabolism of progesterone and progestins in neuroactive steroids can have important neuroendocrine effects. Hormonal contraceptives can interfere in various ways, depending on the combined or progestin-only substances, the characteristics of the progestin, dosage and method of administration (oral, injection, subdermal implant, intrauterine system). Different intrauterine systems release different concentrations of LNG, affecting levels in the endometrium and myometrium and in plasma in the diverse body systems (Table 13.3). The data available for combined hormonal contraception regarding combinations containing ethinylestradiol and various progestins, and the dosages of the two components are not always reported. In addition, the formulation of the combination (monophasic or multiphasic), the regimen of administration (21 + 7, 24 + 4, or extended regimen), and the method (vaginal, cutaneous) all condition the pharmacokinetics, influencing substance concentrations in blood and, probably, mood.
Studies on mood effect show that hormonal contraception may induce interaction of sex steroids with the serotoninergic and noradrenergic pathways (Fig. 13.1). The modifications in allopregnanolone in the central nervous and circulatory systems, induced by hormonal treatments, are related to changes in GABA activity. It is still unclear whether the neuroendocrine effects of progestins are direct or mediated by their metabolism in allopregnanolone [45]. Hormonal contraception affects allopregnanolone brain concentration in an animal model (rats) and the effect of synthetic progestins differs from that of micronized progesterone [46]. One randomized, controlled, double-blind placebo trial that evaluated changes in brain reactivity in regions previously associated with emotion processing showed that OC users had lower emotion induced reactivity in the left insula, left middle frontal gyrus, and bilateral frontal gyri than placebo users [47]. Another study on synthetic estrogen and progestins in oral contraceptive pills reported bilateral decrease of cortical thickness in the lateral orbitofrontal cortex and the posterior cingulate cortex during oral contraceptive use. The functional significance of this cortical thinning remains to be investigated [48]. We note a very recent report on the relationship between hormonal contraceptives and mood that focuses on relevant underlying mechanisms, such as emotion recognition and reactivity, reward processing, and stress response [49]. These are topics that must be given due consideration also in the case of adolescent contraceptive choice.
from Pluchino et al. 2006 [86]
The hypothalamic-pituitary-adrenal axis may also be involved in the effects of female hormones on mood and depression, moderated by mineralocorticoid receptors and glucocorticoid receptors [50]. Another mechanism has also been correlated with depression risk in women using progestin only contraception: in one pilot study investigators found reduced beta-arrestin 1 (β-AR 1) protein levels in peripheral blood mononuclear leukocytes (PBMC). Previous studies [51] demonstrated apparent correlations between β-AR 1 and depressive symptoms in reproductive women. The study involved 29 young women, 12 of whom were using progestin only contraception (4—LNG IUS 20; 1—LNG IUS 12; 4—Nexplanon subdermal implant; 1—DMPA; 2—mini-pill). The authors concluded that since β-AR 1 has been shown to facilitate estrogen-mediated neuroprotection, the estrogen in COC may attenuate the effect of progestin on β-AR 1 levels. We need to discover the specific significance of these two findings, increased cortisol and reduced β-AR 1, in adolescents [52].
The main discussion is centered around LNG IUS 20 in relation to recent studies on the possible causes of mood changes. One study on a wide age range of women, 18–45 years old, suggests that panic attacks, anxiety, mood changes, sleep disturbances, and restlessness may be related to elevated cortisol levels during treatment [53]. The authors found an exaggerated salivary cortisol response to the Trier Social Stress Test -TSST (24.95 ± 13.45 nmol/L, 95% CI 17.49–32.40), compared to EE30/LNG (3.27 ± 2.83 nmol/L, 95% CI 1.71–4.84) and natural cycling women (10.85 ± 11.03 nmol/L, 95% CI 6.30–15.40) (P < 0.0001). The conclusion is that LNG-IUD contraception induces a centrally-mediated sensitization of both autonomic and hypothalamic-pituitary-adrenal (HPA) axis responsivity. The European Society of Contraception (ESC) expert statement considers it “unlikely that slightly higher cortisol levels in LNG IUS users, as found in this one study, are associated with evidence of an increased risk of an adverse event” and calls for further studies, larger and clinically appropriate [54].
Another important point to consider is the effect of hormonal contraceptives on mood in specific gynecologic and psychiatric populations, such as those with polycystic ovarian syndrome and premenstrual dysphoric disorder who may need treatment, during the postpartum period or even in early adolescence [55]. In any case, we emphasize the importance of family history as a risk factor. It is necessary to evaluate mood and risk factors for depression and its very first symptoms in girls who have early menarche [56]. Below, we present the most relevant findings regarding adverse effects of contraceptives on mood with particular reference to adolescence.
Progestin only contraception. One systematic review [57] of 26 studies (5 randomized controlled trials, 11 cohort studies and 10 cross-sectional studies) on the relationship between progestin hormonal contraception and depression concluded that despite perceptions in the community of increased depression following the initiation of progestin contraceptives, the preponderance of evidence does not support an association based on validated measures. The substances evaluated were injectable medroxyprogesterone acetate (DMPA), subdermal progestin, levonorgestrel intrauterine device, and progestin only contraceptive pills. The association between contraception and depression in adolescents was evaluated in trials using DMPA.
DMPA. Three previous studies [58,59,60] had also concluded that depression symptoms were no more likely in adolescents taking DMPA than other hormonal contraceptives. A fourth study [61] found little evidence of increasing depression in young girls with long-term use of DMPA and no evidence of a short-term effect of dose (within the contraceptive range) on mood. Then, 13 years later, a study published in 2008 found no negative mood changes with either DMPA or oral contraceptive pill in 805 patients divided into two age groups, 16–24 years and 25–55 years. DMPA was considered to be protective against mood swings (OR 0.7) and the contraceptive pill against nervousness (OR 0.5) as well as mood swings (OR 0.7) [62]. Another study published the same year [63] involving 328 girls, 14–17 years old (mean age 16.7 years), had different findings. The participants were followed longitudinally for up to 41 months at primary care clinics to evaluate the effects of hormonal contraceptives on mood and sexual interest. The girls kept daily diaries where they recorded positive mood, negative mood, and sexual interest. A total of 938 diary periods were analyzed: participants reported significantly higher mean weekly negative mood in the periods of DMPA use than in periods of non-use. A recent study related to use of hormonal contraception by 800,000 Swedish women [64] states that hormonal contraception increases the risk of psychotropic drug use in adolescent girls but not in adults; the OR for DMPA is 2.37; 95% (CI: 1.46–3.84).
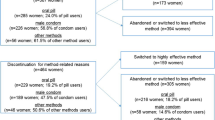
Etonogestrel implants. In a large multicenter study [65], designed to assess the safety and efficacy of the etonogestrel (ENG) implant in 474 American women (18–48 years) who used the implant for up to 2 years (6186 cycles of exposure), common adverse experiences that led to discontinuation, besides bleeding irregularities, were emotional lability (6.1%), weight increase (3.3%), depression (2.4%), and acne (1.5%). Another American study [66] involving 160 adolescents and young women (12–24 years) with ENG subdermal implant or levonorgestrel IUS, found that the reasons for discontinuation of the contraceptive treatment included bleeding problems (59%), weight gain (22%), pelvic pain/cramps (15%), desire for pregnancy (15%), and mood changes (11%).
LNG intrauterine systems. The LNG IUS 20 [67, 68] system in adolescents is used for contraception with certain therapeutic indications, such as idiopathic heavy menstrual bleeding, other causes of heavy bleeding (adenomyosis), pain treatment from endometriosis or adenomyosis, and endometrial hyperplasia. The device is prescribed also for adolescents and young women with hemostasis defects and bleeding disorders [69,70,71]. In general, studies on mood changes during contraceptive treatment with LNG IUS 20 have involved prevalently adult populations or a wide range of ages, and the results are contradictory [72,73,74]. A systematic review [75] regarding hormonal contraception in women (15–45 years old) clinically diagnosed with depressive or bipolar disorders evidenced no significant differences between four treatment groups in the number of hospitalizations for bipolar disorder (Cu-IUD 3.6%; LNG-IUS 5.3%; sterilization 5.7%; and DMPA 6.0%) or depression (LNG-IUS 0.7%, Cu-IUD 0.9%; DMPA 2.2%; and sterilization 3.2%). In particular, no significant associations between hormonal contraception and increased risk of depressive symptoms were found in two of the studies: one regarding 9688 young women (18–23 years old) in Australia [76], the other 103 adolescents under 18 years old in the USA [77]. To the contrary, recent studies on Swedish adolescents show that LNG IUS had the strongest association with use of psychotropic drugs (adjusted OR 2.90; 95% CI: 2.22–3.79) [64]. Furthemore, the above-mentioned study done in the USA [66] reported mood changes in 11% of 160 young women (12–24 years old) using LNG IUS 20 or subdermal implant the majority of treatment discontinuations was due to other factors.
Concerning possible mood change risk, one group of investigators has proposed precise pre-insertion counseling regarding potential effects on mood, as part of good informed choice, with additional counseling 6–12 weeks and 12 months after insertion [78]. To date, there have been no reports of a causal relationship of adverse effects regarding mood in LNG 12 and LNG 8 users [79]. We do note that both these devices release low concentrations of LNG (Table 13.4) and that more of the users ovulate compared to LNG IUS 20 users.
Progestin-only pill. The recent findings on adolescents 15–19 years of age include a report of increased depressive symptoms with RR 2.2 (95% CI, 1.99–2.52) with first use of an antidepressant in subjects taking progestin-only pills, compared to RR 1.4 (95% CI, 1.31–1.42) for LNG IUS and RR 1.8 (95% CI, 1.75–1.84) for combined hormonal contraception. The absolute increase in depression diagnoses for girls was 3 per 1000 for depression diagnosis and 8 per 1000 for first use of antidepressants, compared to boys who had an increase of 1.1 and 3 per 1000, respectively [80]. In another study, the same authors found that use of hormonal contraception was positively associated with subsequent suicide or suicide attempts, with an estimated risk for attempted suicide of 2.29 (95% CI = 1.77–2.95) for oral progestin-only products and 1.91 (95% CI = 1.79–2.03) for combined oral contraceptive preparations [81].
Combined hormonal contraception (CHC). A 2002 review of the literature found that CHC users presented more stable affectivity than non-users throughout the entire menstrual cycle [82]. Subjects taking combined hormonal contraceptives who have negative mood changes generally report a history of depression, psychiatric problems, dysmenorrhea with premenstrual syndrome, family history of mood disturbances related to hormonal contraceptive treatment, or particular life events (post-partum, age). A Swedish double-blind, placebo-controlled randomized trial on a combined oral contraceptive containing levonorgestrel (EE 30/LNG 150 μg) evidenced higher scores of depressed mood, mood swings, and fatigue in the CHC than placebo users. All the 34 women (18–45 years old) randomized for the trial, had had previous episodes of mood problems during CHC use [47]. Another Swedish study was done using telephone screening of 347 young women, 18–35 years old. The investigators evidenced a statistically significant reduction in general well-being in the women who took CHC (first-choice: EE30/LNG 150 μg) compared to those on placebo; the findings were based on the first 3 months of treatment. There was no information regarding any statistically significant effects on depression [83]. Recent data, again in Sweden, on the use of psychotropic drugs show an association with CHC treatment (adjusted OR 1.34, 95% CI 1.30–1.37). Age-stratified analysis evidenced that this association was strongest in adolescent girls (adjusted OR 3.46, 95% CI 3.04–4.94 for age 12–14 years), and non-existent in adult women. The 12–14 year olds were found to present the strongest relationship between psychotropic drugs and CHCs, specifically non-oral methods (skin patch or intravaginal ring) with OR 4.47 (95% CI: 2.08–8.78). This was a pharmaco-epidemiological study with a total population of 815,662 women aged 12–30 years who had no history of psychiatric disease [64]. A prospective cohort study (Tracking Adolescents’ Individual Lives Survey TRAILS) of a total 1010 girls analyzed at the first assessment of oral contraceptive use (mean age 16.3) done in the Netherlands showed no association between CHC and depressive symptoms for the total of all age groups. However, the 16-year-old girls were found to have higher scores for depressive symptoms with oral contraceptives than older age groups [84]. To the contrary, data specifically related to 4765 adolescents (13–16 years old) in the USA who took CHC did not evidence any increase in depressive disorders. The type of oral contraceptive was not specified [85].
The European Society for Contraception [54] recommends the following steps for balanced and individualized counseling:
-
“Take a thorough medical history, considering especially any conditions that could cause a complication with use of a contraceptive method.
-
Identify women predisposed to depressed mood by taking a past and current psychiatric history; ask specifically about ever-use of antidepressants. Include a family history to identify women at increased cardiovascular risk.
-
Take time to cover in a personal history the woman’s life situation, partnership, and sexual life.
-
After starting a new method, offer a follow-up visit to discuss options in situations of severe or troublesome adverse events. Adverse events should include affective symptoms and sexual function.”
This is particularly true dealing with very young subjects, because issues such as changing body, parents and academic expectations, peer pressure can induce significant distress and sometimes overwhelming emotional and mood disorders.
References
Palmer M, Clarke L, Ploubidis G, Mercer C, Gibson L, Johnson A, Copas A, Weillings K. Is “sexual competence” at first heterosexual intercourse associated with subsequent sexual health status? J Sex Res. 2017;54(1):91–104.
Widman L, Noar SM, Choukas-Bradely S, Francis D. Adolescent sexual health communication and condom use: a meta-analysis. Health Psychol. 2014;33(10):1113–24.
Gambadauro P, Carli V, Wasserman C, Hadlaczky G, Sarchiapone M, Apter A, et al. Psychopathology is associated with reproductive health risk in European adolescents. Reprod Health. 2018;15(1):186–95.
London S, Quinn K, Scheidell JD, Frueh BC, Khan MR. Adverse experiences in childhood and sexually transmitted infection risk from adolescence into adulthood. Sex Transm Dis. 2017;44(9):524–32.
Scheidell JD, Quinn K, McGorray SP, Frueh BC, Beharie NN, Cottler LB, Khan MR. Childhood traumatic experiences and the association with marijuana and cocaine use in adolescence through adulthood. Addiction. 2018;113(1):44–56.
Chang T, Davis MM, Kusunoki Y, Ela EJ, Hall KS, Barber JS. Sexual behavior and contraceptive use among 18 to 19 year old adolescent women by weight status: a longitudinal analysis. J Pediatr. 2015;167(3):586–92.
Heger JP, Brunner R, Parzer P, Fischer G, Resch F, Kaess M. Depression and risk behavior in adolescence. Prax Kinderpsychol Kinderpsychiatr. 2014;63(3):177–99.
Auslander BA, Baker J, Short MB. The connection between young women’s body esteem and sexual assertiveness. J Pediatr Adolesc Gynecol. 2012;25(2):127–30.
European Society of Contraception and Reproductive Health Position Paper on Sexual and Reproductive Health and Rights 2019 (The Madrid Declaration). https://eschr.eu.
Titchen KE, Maslyanskaya S, Silver EJ, Coupey SM. Sexting and young adolescents: associations with sexual abuse and intimate partner violence. J Pediatr Adolesc Gynecol. 2019;32(5):481–6.
Kawabe K, Horiuchi F, Oka Y, Ueno SI. Association between sleep habits and problems and internet addiction in adolescents. Psichiatry Investig. 2019;16(8):581–7.
Chandra-Mouli V, Plesons M, Adebayo E, Amin A, Kraft JM, Lane C, et al. Implications of the global early adolescent study’s formative research findings for action and for research. J Adolesc Health. 2017;61:55–9.
Miller E, Decker MR, Reed E, Raj A, Hathaway JE, Silverman JG. Male partner pregnancy-promoting behaviors and adolescent partner violence: findings from a qualitative study with adolescent females. Ambul Pediatr. 2007;7(5):360–6.
Barrios De Tomasi A, Opata MM, Mowa CN. Immunity in the cervix: interphase between immune and cervical epithelial cells. J Immunol Res. 2019;2019:7693183.
Herfs M, Soong TR, Delvenne P, Crum CP. Deciphering the multifactorial susceptibility of mucosal junction cells to HPV infection and related carcinogenesis. Viruses. 2017;9:85–98.
Pudney J, Quayle AJ, Andrson DJ. Immunological microenvironments in the human vagina and cervix: mediators of cellular immunity are concentrated in the cervical transformation zone. Biol Reprod. 2005;73:1253–63.
Hickey RJ, Zhou X, Settles ML, Erb J, Malone K, Hansmann MA, Shew ML, Van Der Pol B, Fortenberry JD, Forney LJ. Vaginal microbiota of adolescent girls prior to the onset of menarche resemble those of reproductive-age women. MBio. 2015;6(2):e00097-15.
Ghosh M, Jais M, Biswas R, Jarin J, Daniels J, Joy C, Juzumaite M, Emmanuel BS, Gomes LV. Immune biomarkers and anti-HIV activity in the reproductive tract of sexually inactive adolescent girls. Am J Reprod Immunol. 2018;79(6):e12846.
Scott ME, Ma Y, Farhat S, Shiboski S, Moscicki AB. Covariates of cervical cytokine mRNA expression by real-time PCR in adolescents and young women: effects of Chlamydia trachomatis infection, hormonal contraception, and smoking. J Clin Immunol. 2006;26(3):222–32.
Brooks JP, Edwards DJ, Blithe DL, Fettweis JM, Serrano MG, Sheth NU, Strauss JF, Buck GA, Jefferson KK. Effects of combined oral contraceptives, depot medroxyprogesterone acetate, and the levonorgestrel-releasing intrauterine system on the vaginal microbiome. Contraception. 2017;95(4):405–14.
Donders GGG, Bellen G, Ruban K, Van Bulck B. Short-and long-term influence of the levonorgestrel-releasing intrauterine system (Myrena) on vaginal microbiota and Candida. J Med Microbiol. 2018;67:308–13.
Eastman AJ, Bergin IL, Chai D, Bassis CM, LeBar W, Oluoch GO, Liechty ER, Nyachieo A, Young VB, Aronoff DM, Patton DL, Bell JD. Impact of the levonorgestrel-releasing intrauterine system on the progression of chlamydia trachomatis infection to pelvic inflammatory disease in a baboon model. J Infect Dis. 2018;217(4):656–66.
Deese J, Pradhan S, Goetz H, Morrison C. Contraceptive use and the risk of sexually transmitted infection: systematic review and current perspectives. Open Access J Contracept. 2018;9:91–112.
Agenjo González M, Lampaya Nasarre B, Salazar F, Varillas D, Cristobal I. Influence of intrauterine dispositive in human papillomavirus clearance. Eur J Obstet Gynecol Reprod Biol. 2019;232:65–9.
Stoddard AM, Xu H, Madden T, Alisworth JE, Peipert JF. Fertility after intrauterine device removal: a pilot study. Eur J Contracept Reprod Health Care. 2015;20(3):223–30.
Mendoza RM, Garbers S, Lin S, Stockwell MS, Warren M, Gold MA. Chlamydia infection among adolescent long-acting reversible contraceptive (LARC) and shorter acting hormonal contraceptive users receiving services at New York City school-based health centers. J Pediatr Adolesc Gynecol. 2020;33:53–7.
Peña AS, Doherty DA, Atkinson HC, Hickey M, Norman RJ, Hart R. The majority of irregular menstrual cycles in adolescence are ovulatory: results of a prospective study. Arch Dis Child. 2018;103(3):235–9.
Sun BZ, Kangarloo T, Adams JM, Sluss PM, Welt CK, Chandler DW, Zava DT, McGrath JA, Umbach DM, Hall JE, Shaw ND. Healthy post-menarchal adolescent girls demonstrate multi-level reproductive axis immaturity. J Clin Endocrinol Metab. 2019;104(2):613–23.
Rovner P, Keltz J, Allshouse A, Isaac B, Hickmon C, Lesh J, Chosich J, Santoro N. Induction of the LH surge in premenarchal girls confirms early maturation of the hypothalamic- pituitary-ovarian axis. Reprod Sci. 2018;25(1):33–8.
Legro RS, Lin HM, Demers LM, Lloyd T. Rapid maturation of the reproductive axis during perimenarche independent of body composition. J Clin Endocrinol Metab. 2000;85(3):1021–5.
Zhang K, Pollack S, Ghods A, Dicken C, Isaac B, Adel G, Zeitlian G, Santoro N. Onset of ovulation after menarche in girls: a longitudinal study. J Clin Endocrinol Metab. 2008;93(4):1186–94.
Van Hoof MHA, Voorhorst FJ, Kaptein MBH, Hirasing RA, Koppenaal C, Schoemaker J. Predictive value of menstrual cycle pattern, body mass index, hormone levels and plycystic ovaries at age 15 years for oligo-amenorrhea at age 18 years. Hum Reprod. 2004;19(2):383–92.
Berglund Scherwitzl E, Lundberg O, Kopp Kallner H, Rowland SP, Holte J, Trussell J, Gemzell Danielsson K, Scherwitzl R. Short- and long-term effect of contraceptive methods on fecundity. Eur J Contracept Reprod Health Care. 2019;24(4):260–5.
Girum T, Wasle A. Return of fertility after discontinuation of contraception: a systematic review and meta-analysis. Contracept Reproduct Med. 2018;3:1–9.
Rey-Stocker I, Zufferey MM, Lemarchand MT, Rais M. Sensitivity of the hypophysis, the gonads and the thyroid gland in young girls before and after the use of combined oral contraception. Gynakol Rundsch. 1980;20(3):135–61.
Papageorgiou M, Dolan E, Elliott-Sale KJ, Sale C. Reduced energy availability: implications for bone health in physically active populations. Eur J Nutr. 2018;57(3):847–59.
Filippou P, Homburg R. Is foetal hyperexposure to androgens a cause of PCOS? Hum Reprod Update. 2017;23(4):421–32.
Efthymiadou A, Bogiatzidou M, Kritikou D, Chrysis D. Anti-Müllerian hormone in girls with premature adrenarche: the impact of polycystic ovary syndrome history in their mothers. J Pediatr. 2019;205:190–4.
Teede HJ, Misso ML, Costello MF, Dokras A, Laven J, Mora L, Piltonen T, Norman RJ. On behalf of the International PCOS Network Recommendations from the international evidence-based guideline for the assessment and management of polycystic ovary syndrome. Hum Reprod. 2018;33(9):1602–18.
Xue S, Kemal O, Lu M, Lix LM, Leslie WD, Yang S. Age at attainment of peak bone mineral density and its associated factors: The National Health and Nutrition Examination Survey 2005–2014. Bone. 2019;131:115–23.
Weaver CM, Gordon CM, Janz KF, Kalkwarf HJ, Lappe JM, Lewis R, O’Karma M, Wallace TC, Zemel BS. The National Osteoporosis Foundations ’s position statement on peak bone mass development and lifestyle factors: a systematic review and implementation recommendations. Osteporos Int. 2016;27:1281–386.
Goshtasebi A, Subotic Brajic T, Scholes D, Beres Lederer Goldberg T, Berenson A, Prior JC. Adolescent use of combined hormonal contraception and peak bone mineral density accrual: a meta-analysis of international prospective controlled studies. Clin Endocrinol. 2019;90(4):517–24.
Di Iorgi N, Maruca K, Patti G, Mora S. Update on bone density measurements and their interpretation in children and adolescents. Best Pract Res Clin Endocrinol Metab. 2018;32(4):477–98.
FSRH Guidelines “Hormonal contraception” January 2019 (amended July 2019) p.25. www.fsrh.org.
Pluchino N, Santoro A, Casarosa E, Wenger JM, Genazzani AD, Petignat P, et al. Advances in neurosteroids: role in clinical practice. Climacteric. 2013;16:8–17.
Pluchino N, Ansaldi Y, Genazzani AR. Brain intracrinology of allopregnanolone during pregnancy and hormonal contraception. Horm Mol Biol Clin Invest. 2019;37:1.
Gingnell M, Engman J, Frick A, Moby L, Wikström J, Fredrikson M, Sundström-Poromaa I. Oral contraceptive use changes brain activity and mood in women with previous negative affect on the pill—a double-blinded, placebo-controlled randomized trial of a levonorgestrel-containing combined oral contraceptive. Psychoneuroendocrinology. 2013;38(7):1133–44.
Petersen N, Touroutoglou A, Andreano JM, Cahill L. Oral contraceptive pill use is associated with localized decreases in cortical thickness. Hum Brain Mapp. 2015;36(7):2644–54.
Lewis CA, Kimmig AS, Zsido RG, Jank A, Derntl B, Sacher J. Effects of hormonal contraceptives on mood: a focus on emotion recognition and reactivity, reward processing, and stress response. Curr Psychiatry Rep. 2019;21(11):115.
Hamstraa DA, de Kloetc ER, de Rovera M, Van der Doesa W. Oral contraceptives positively affect mood in healthy PMS-free women: a longitudinal study. J Psychosom Res. 2017;103:119–26.
Schreiber G, Golan M, Avissar S. Beta-arrestin signaling complex as a target for antidepressants and as a depression marker. Drug News Perspect. 2009;22:467–80.
Smith K, Nayyar S, Rana T, Archibong AE, Looney KR, Nayyar T. Do progestin-only contraceptives contribute to the risk of developing depression as implied by beta-arrestin 1 levels in leukocytes? A pilot study. Int J Environ Res Public Health. 2018;15(9):1–21.
Aleknaviciute J, Tulen JHM, De Rijke YB, Bouwkamp CG, van der Kroeg M, Timmermans M, Kushner SA. The levonorgestrel-releasing intrauterine device potentiates stress reactivity. Psychoneuroendocrinology. 2017;80:39–45.
Merki-Feld GS, Apter D, Bartfai G, Grandi G, Haldre K, Lech M, et al. ESC expert statement on the effects on mood of the natural cycle and progestin-only contraceptives. Eur J Contracept Reprod Health Care. 2017;22(4):247–9.
Robakis T, Williams KE, Nutkiewicz L, Rasgon NL. Hormonal contraceptives and mood: review of the literature and implications for future research. Curr Psychiatry Rep. 2019;21(7):57.
Shen Y, Varma DS, Zheng Y, Boc J, Hu H. Age at menarche and depression: results from the NHANES 2005–2016. PeerJ. 2019;7:e7150.
Worly BL, Gur TL, Schaffir J. The relationship between progestin hormonal contraception and depression: a systematic review. Contraception. 2018;97(6):478–89.
Cromer BA, Smith RD, Blair JM, Dwyer J, Brown RT. A prospective study of adolescents who choose among levonorgestrel implant (Norplant), medroxyprogesterone acetate (Depo-Provera), or the combined oral contraceptive pill as contraception. Pediatrics. 1994;94(5):687–94.
Harel Z, Biro FM, Kollar LM. Depo-Provera in adolescents: effects of early second injection or prior oral contraception. J Adolesc Health. 1995;16(5):379–84.
Gupta N, O’Brien R, Jacobsen LJ, Davis A, Zuckerman A, Supran S, Kulig J. Mood changes in adolescents using depot-medroxyprogesterone acetate for contraception: a prospective study. J Pediatr Adolesc Gynecol. 2001;14(2):71–6.
Westhoff C, Wieland D, Tiezzi L. Depression in users of depo-medroxyprogesterone acetate. Contraception. 1995;51(6):351–4.
Berenson AB, Tan A, Hirth JM. Complications and continuation rates associated with 2 types of long-acting contraception. Am J Obstet Gynecol. 2015;212(6):761–6.
Ott MA, Shew ML, Ofner S, Tu W, Fortenberry JD. The influence of hormonal contraception on mood and sexual interest among adolescents. Arch Sex Behav. 2008;37(4):605–13.
Zettermark S, Perez Vicente R, Merlo J. Hormonal contraception increases the risk of psychotropic drug use in adolescent girls but not in adults: a pharmaco-epidemiological study on 800,000 Swedish women. PLoS One. 2018;3(3):e0194773.
Funk S, Miller MM, Mishell DR, Archer DF, Poindexter A, Schmidt J, Zampaglione E. Safety and efficacy of Implanon™, a single-rod implantable contraceptive containing etonogestrel. Contraception. 2005;71(5):319–26.
Sznajder KK, Tomaszewski KS, Burke AE, Trent M. Incidence of discontinuation of long-acting reversible contraception among adolescent and young adult women served by an urban, primary care clinic katharine. J Pediatr Adolesc Gynecol. 2017;30(1):53–7.
Nelson AL, et al. Exp Opin Drug Deliv. 2017;14(9):1131–40.
Paterson H, Ashton J, Harrison-Woolrych M. A nationwide cohort study of the use of the levonorgestrel intrauterine device in New Zealand adolescents. Contraception. 2009;79(6):433–8.
Chi C, Pollard D, Tuddenham EG, Kadir RA. Menorrhagia in adolescents with inherited bleeding disorders. J Pediatr Adolesc Gynecol. 2010;23(4):215–22.
Pillai M, O’Brien K, Hill E. The levonorgestrel intrauterine system (Mirena) for the treatment of menstrual problems in adolescents with medical disorders, or physical or learning disabilities. BJOG. 2010;117(2):216–21.
Lu M, Yang X. Levonorgestrel-releasing intrauterine system for treatment of heavy menstrual bleeding in adolescents with Glanzmann’s Thrombasthenia: illustrated case series. BMC Womens Health. 2018;18(1):45.
Elovainio M, Teperi J, Aalto AM, Grenman S, Kivelä A, et al. Depressive symptoms as predictors of discontinuation of treatment of menorrhagia by levonorgestrel-releasing intrauterine system. Int J Behav Med. 2007;14(2):70–5.
Tazegül Pekin A, Seçilmiş Kerimoğlu Ö, Kebapcılar AG, Yılmaz SA, Benzer N, Çelik Ç. Depressive symptomatology and quality of life assessment among women using the levonorgestrel-releasing intrauterine system: an observational study. Arch Gynecol Obstet. 2014;290(3):507–11.
Slattery J, Morales D, Pinheiro L, Kurz X. Cohort study of psychiatric adverse events following exposure to levonorgestrel-containing intrauterine devices in UK general practice. Drug Saf. 2018;41(10):951–8.
Pagano HP, Zapata LB, Berry-Bibee EN, Nanda K, Curtis KM. Safety of hormonal contraception and intrauterine devices among women with depressive and bipolar disorders: a systematic review. Contraception. 2016;94(6):641–9.
Duke JM, Sibbritt DW, Young AF. Is there an association between the use of oral contraception and depressive symptoms in young Australian women? Contraception. 2007;75(1):27–31.
O’Connell K, Davis AR, Kerns J. Oral contraceptives: side effects and depression in adolescent girls. Contraception. 2007;75(4):299–304.
Bitzer J, Rapkin A, Soares CN. Managing the risks of mood symptoms with LNG-IUS: a clinical perspective. Eur J Contracept Reprod Health Care. 2018;23(5):321–5.
Gemzell-Danielsson K, Apter D, Dermout S, Faustmann T, Rosen K, Schmelter T, et al. Evaluation of a new, low-dose levonorgestrel intrauterine contraceptive system over 5 years of use. Eur J Obstet Gynecol Reprod Biol. 2017;210:22–8.
Skovlund CW, Kessing LV, Mørch LS, Lidegaard Ø. Increase in depression diagnoses and prescribed antidepressants among young girls. A national cohort study 2000–2013. Nord J Psychiatry. 2017;71(5):378–85.
Skovlund CW, Mørch LS, Kessing LV, Lange T, Lidegaard Ø. Association of hormonal contraception with suicide attempts and suicides. Am J Psychiatry. 2018;175(4):336–42.
Oinonen KA, Mazmanian D. To what extent do oral contraceptives influence mood and affect? J Affect Disord. 2002;70(3):229–40.
Zethraeus N, Dreber A, Ranehill E, Blomberg L, Labrie F, von Schoultz B. A first-choice combined oral contraceptive influences general well-being in healthy women: a double-blind, randomized, placebo-controlled trial. Fertil Steril. 2017;107(5):1238–45.
de Wit AE, Booij SH, Giltay EJ, Joffe H, Schoevers RA, Oldehinkel AJ. Association of use of oral contraceptives with depressive symptoms among adolescents and young women. JAMA Psychiatr. 2019;77:52–9.
McKetta S, Keyes KM. Oral contraceptive use and depression among adolescents. Ann Epidemiol. 2019;29:46–51.
Pluchino N, Luisi M, Lenzi E, Centofanti M, Begliuomini S, Freschi R, Ninni F, Genazzani AR. Progesterone and progestins: effect on brain, allopregnanolone and betaendorphin. J Steroid Biochem Mol Biol. 2006;102(1–5):205–13.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Bruni, V., Dei, M. (2021). Critical Issues in Adolescent Contraception. In: Meriggiola, M.C., Gemzell-Danielsson, K. (eds) Female and Male Contraception. Trends in Andrology and Sexual Medicine. Springer, Cham. https://doi.org/10.1007/978-3-030-70932-7_13
Download citation
DOI: https://doi.org/10.1007/978-3-030-70932-7_13
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-70931-0
Online ISBN: 978-3-030-70932-7
eBook Packages: MedicineMedicine (R0)