Abstract
Fungal spondylodiscitis is most commonly encountered in immunocompromised patients. The incidence of fungal infections has increased in the past decade. Candida and Aspergillus are the most common causes of opportunistic fungal infection. The imaging findings are similar to that of pyogenic infection, with T1-hypointense signal at the infected vertebral end plates. However, abnormal T2-weighted signal change is relatively less commonly identified in patients with fungal spondylodiscitis. Even though fungal spondylodiscitis is less common than pyogenic or tuberculous involvement, it is important to consider fungal infection in the differential diagnosis and utilize the clinical history and the patient presentation to enable a more accurate imaging diagnosis.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Candida spondylodiscitis
- Fungal infection
- Fungal spondylodiscitis
- Spinal aspergillosis
- Spinal cryptococcosis
- Spinal osteomyelitis
- Vertebral osteomyelitis
1 Introduction
Fungal spondylodiscitis is uncommon, but the immunocompromised population which is susceptible to fungal infections is ever increasing (Kim et al. 2006). A wide variety of fungal organisms can cause spinal infection. The most common fungal organisms causing spondylodiscitis include Aspergillus spp., Candida spp., and Cryptococcus neoformans (Kim et al. 2006). Whereas Cryptococcus, Candida, and Aspergillus have a worldwide distribution, other fungi such as Coccidioides immitis and Blastomyces dermatitidis are limited to specific geographical areas. Therefore, residence in or travel to endemic areas should be taken into consideration when evaluating patients with chronic spondylodiscitis. The common denominator in many cases appears to be an incompetent host defense mechanism secondary to conditions such as diabetes mellitus, corticosteroid use, chemotherapy, malnutrition, or intravenous drug use.
2 Pathogenesis and Clinical Features
Fungal spondylodiscitis can occur via one of two routes. The first is through hematogeneous spread. As the intervertebral disk does not have a direct blood supply in adults, most hematogeneous infections of the disk space are the result of dissemination from the adjacent bone. The spread from an initial pulmonary source has also been described. The second route of transmission is through contiguous spread or by direct inoculation of the organism during surgery (Kim et al. 2006).
Insidious back pain is the most frequent complaint. Neurological impairment appears to be relatively infrequent (Kim et al. 2006). Kyphosis can also be seen, due to the indolent nature of the infection. Involvement of the vertebral bodies can lead to vertebral compression fractures and deformity of the spine. In addition, the spread of infection along the anterior longitudinal ligament can lead to paravertebral or psoas muscle abscesses (Skaf et al. 2010).
3 Aspergillosis
Aspergillus is an opportunistic mycelial organism which is abundant in the environment. It lives as saprophyte, and its concentration in the air undergoes seasonal variation (higher in summer). Nosocomial aspergillosis is due to infiltration of conidia into ward air from outside. Aspergillus is the most common cause of infection and death in patients with chronic granulomatous disease (Heinrich et al. 1991). Aspergillosis is also the second most common invasive fungal infection in cancer patients, with most of them being or had previously been neutropenic. Bone marrow transplant recipients may be at risk of invasive aspergillosis, especially during profound neutropenia (Govender 2003). Aspergillus is the most common cause of skeletal mycosis, with the vertebrae being the most commonly involved structures in mycotic osteomyelitis. The most common causative species is A. fumigatus. Less frequently, A. flavus, A. niger, A. nidulans, and A. terreus have been isolated (Govender et al. 1991).
The radiological features of Aspergillus spondylodiscitis are nonspecific, and they may involve single or multiple bodies. The lumbar region is the main area (63%) of osseous involvement (Hummel et al. 1993). Spinal aspergillosis is often confused with tuberculous spondylodiscitis. As in tuberculous spondylodiscitis, Aspergillus infection may extend from an anterior lesion of the vertebral body beneath the anterior longitudinal ligament to the anterior parts of neighboring intervertebral disk and vertebral bodies or involve multiple vertebral segments with skip lesions. However, the shape of epidural or paravertebral abscesses may be helpful in differentiating between them. Aspergillus abscesses have a thick irregular wall, whereas tuberculous abscesses typically have a thin smooth wall (Jung et al. 2004) (Fig. 1).
A 55-year-old man with diabetes mellitus who presented with progressive back pain and fecal and urinary incontinence. (a, b) Sagittal T2-W MR images show multilevel disease with areas of hyperintensity in the T9, T10, T11, and T12 vertebrae and intervertebral disks. Large confluent paraspinal abscess and epidural disease are also present. Subligamentous spread of infection (arrows) is seen along anterior and posterior margins of the vertebral bodies. (c) Axial contrast-enhanced T1-W MR image shows infective arthritis of facet and costovertebral joints and paravertebral abscesses with thin peripheral rim enhancement. CT-guided percutaneous needle biopsy was performed and mycological examination revealed Aspergillus flavus. (d) Histopathological examination showed acute inflammation and necrosis with hyaline, branching septate hyphae (circled)
Additionally, in invasive aspergillosis, the lesion spreads more circumferentially than longitudinally. It destroys the vertebral body and the neural arches and then, extends into the chest wall and the thoracic cavity (Ur-Rahman et al. 2000). Moreover, the nuclear cleft in Aspergillus-induced spondylodiscitis may be preserved, and Aspergillus infection may show band-like signal hypointensity in the subchondral bone marrow on T2-weighted MR images. The subchondral T2-hypointense signal is attributed to the presence of paramagnetic and ferromagnetic elements within the fungi. This finding is similar to the proposed mechanism for T2 hypointensity in fungal sinusitis (Hong et al. 2009; Kwon et al. 2011).
The biological diagnosis is based on the detection of Aspergillus after Sabouraud agar culture of discovertebral biopsy fragments, associated with the observation of mycelial hyphae on the same samples on direct examination. Detection of fungal biomarkers is highly contributory. Serology is based on the detection of anti-Aspergillus fumigatus antibodies by different techniques (ELISA, Western Blot). The search for the galactomannan antigen is particularly recommended for neutropenic patients, while the (1-3)-β-d-glucan antigen has a negative predictive value. Molecular biology by RT-PCR also has a good negative predictive value (Nicolle et al. 2013).
The treatment of Aspergillus spondylodiscitis is multimodal, involving early antifungal therapy and surgical intervention (Korovessis et al. 2014). Various studies have demonstrated the superiority of voriconazole over amphotericin B in the treatment of invasive aspergillosis, with improved survival and lower toxicity (Herbrecht et al. 2002). Despite limited experience with voriconazole for the treatment of Aspergillus spondylodiscitis, it is currently recommended by the Infectious Diseases Society of America (IDSA) guidelines for a minimum of 6–8 weeks in immunocompromised patients (Walsh et al. 2008).
4 Candidosis
Candida spondylodiscitis accounts for approximately 1% of infectious spondylodiscitis (Richaud et al. 2017). It was previously considered a complication of intravenous drug use (Cornely et al. 2012; Pappas et al. 2016) but now is mostly a healthcare-associated infection, such as invasive Candida infection. With the increase in invasive Candida infection, Candida spondylodiscitis cases are increasing, and this trend will likely continue in the future. Although there are nearly ten species of Candida that are pathogenic to humans, 62% of cases of vertebral osteomyelitis are caused by C. albicans, 19% by C. tropicalis, and 14% by C. glabrata (Kim et al. 2006). Infection caused by C. glabrata is becoming more common. The lower thoracic or lumbar spine is most frequently involved, seen in 95% of patients. At presentation, 83% of patients complain of back pain for more than 1 month, and only 32% of patients have fever (Kim et al. 2006).
Radiographs frequently show erosive and destructive vertebral changes, but these may not be visible for weeks to months (Bonakdarpour and Gaines 1983). Candida spondylodiscitis looks like a pyogenic infection with areas of hypointensity on T1-weighted MR images and minimal hyperintensity or isointensity on T2-weighted MR images of the vertebral bodies. The clinical usefulness of minimal signal change on T2-weighted images may however be limited, since a recent review of MRI findings in spinal osteomyelitis showed T2 hyperintensity in the vertebral bodies in only 56% of cases (Dagirmanjian et al. 1996). In Candida spondylodiscitis, there is posterior element involvement, which is unusual in pyogenic spondylodiscitis and is more commonly seen in tuberculosis. In addition, paraspinal inflammation is usually minimal to moderate in extent and commensurate with the amount of bone destruction and disk space involvement. This is in contrast to tuberculosis, which is characteristically associated with a large paraspinal inflammatory component (Whelan et al. 1985) (Fig. 2).
A 27-year-old man with thalassemia and sickle cell anemia. Coronal (a) T2-W and (b) contrast-enhanced T1-W MR images show extensive signal abnormality involving the entire spine with irregular patchy areas of signal hypointensity due to hemopathy (arrowheads), destruction of L3/L4 disk, and paravertebral abscesses, more prominent on the right (arrows). (c) Axial contrast-enhanced T1-W MR image shows multiple small paraspinal abscesses (arrows) and diffusely enhancing left paraspinal inflammatory mass (arrowheads). CT-guided percutaneous needle biopsy was performed, and mycological examination revealed Candida tropicalis. (d) Histopathological examination showed foci of granulomatous inflammatory tissue and necrosis
Blood cultures are negative in 24–50% of cases (Arias et al. 2004). Antigen and antibody detection assays are useful in fungal infections, where they have a high positive predictive value for the diagnosis of Candida albicans. These tests are based on the detection of circulating cell wall fungal antigens. Molecular techniques have also been used with fungal infections and have enhanced the sensitivity of conventional methods used in diagnostic mycology (Skaf et al. 2010).
There are no treatment guidelines or evidence-based recommendations for Candida spondylodiscitis in immunocompetent or immunocompromised patients. In addition, the optimal medication and treatment duration for fungal spondylodiscitis are unknown. Antifungal drug resistance is considered less problematic in Candida species than in other pathogens. The preferred treatment is fluconazole for 6–12 months or amphotericin B for 6–10 weeks (Kim et al. 2006).
5 Cryptococcosis
Cryptococcosis is a systemic mycosis that often involves the lungs and the central nervous system. It is caused by Cryptococcus neoformans, which is found in fruit, milk, soil, and feces of some birds. The disease has a worldwide distribution. Immunosuppression related to altered T-cell function is the most common predisposing factor. In non-human immunodeficiency virus (HIV)-infected patients, predisposing factors for cryptococcosis include malignancy, solid organ transplantation, connective tissue diseases, and immunosuppressive therapy. Estimates of the annual incidence of cryptococcosis in non-HIV individuals are 1.3–8 per 100,000 (Legarth et al. 2014).
The disease is generally acquired by the respiratory route through inhalation of aerosolized spores. Pulmonary infection with Cryptococcus may be asymptomatic or symptomatic. It may regress, progress, or remain stable for years. Extrapulmonary infection usually results from hematogeneous spread and can involve any organ. There is a predilection for central nervous system involvement, which is the most common extrapulmonary manifestation (Kim et al. 2006). Osseous involvement is a manifestation of disseminated cryptococcosis in 5–10% of cases. The most commonly involved skeletal sites are the spine, pelvis, ribs, skull, tibia, and knee (Chhem et al. 2001).
The thoracic spine is the most frequently affected spinal segment. Radiological findings in spinal cryptococcosis are not specific and are usually similar to those of tuberculosis spondylodiscitis. There is involvement of the vertebral body and extensive involvement of the posterior elements and paraspinous and perivertebral soft tissues, with relative preservation of the disk (Andres et al. 2014). Radiographs may reveal a cystic lesion involving a single body or multiple vertebral bodies, which may mimic metastatic disease or multiple myeloma. In immunocompetent hosts, the lung fields may be normal, but in immunocompromised patients, chest radiographs may reveal pneumonia or a fungal ball in a pre-existing cavity (Hoeprich et al. 1994) (Fig. 3).
(a, b) Sagittal T2-W and (c) right parasagittal contrast-enhanced fat-suppressed T1-W MR images show areas of T2 hyperintensity in the collapsed T8 and T9 vertebral bodies and spinous processes. Epidural abscess with compression of spinal cord and a large prevertebral abscess are also seen at the T8-T9 levels. There is also extension to the right pedicle and lamina of the T8 and T9 vertebrae. The vertebral bodies and right posterior elements show peripheral enhancement. Note normal height and signal intensity of the adjacent disks. (d) Axial and (e) coned right parasagittal contrast-enhanced fat-suppressed T1-W MR images show a large paravertebral abscess which protrudes into the pleural cavity and involves the adjacent posterior ribs. CT-guided percutaneous needle biopsy revealed cryptococcosis
The serum cryptococcal antigen test has been reported to have an accuracy of 66% in immunocompetent patients with cryptococcosis (Kiertiburanakul et al. 2006). The detection of fungal nucleic acid by PCR has promise as a diagnostic tool. Biopsy and histopathological assessments are critical in the diagnosis of fungal infection. Further identification can be aided by the phenol oxidase reaction for cryptococcus. It is crucial that microscopical appearances are correlated with microbiological findings and other tests for specific host antibodies, fungal antigens, and fungal nucleic acids (O’Shaughnessy et al. 2003). Amphotericin B in combination with oral flucytosine is the recommended medical therapy (Casadevall and Perfect 1998). Surgery helps in establishing the diagnosis, in reducing the burden of infection, and in the stabilization of the spine (Gupta et al. 2003).
6 Coccidioidomycosis
Coccidioidomycosis is endemic in South Africa, South America, and the United States (Dalinka et al. 1971). Coccidioidomycosis results from inhalation of spores of the fungus, which causes a variable pulmonary response in affected individuals. Extrapulmonary dissemination develops in approximately 0.5% of affected patients. Spinal involvement develops in approximately 25% of patients with disseminated disease (Huntington et al. 1967; Galgiani 1993).
In patients with coccidioidomycotic spondylodiscitis, radiographs usually show single or multiple osteolytic lesions with poorly defined borders. A rim of sclerosis may be present in patients under amphotericin treatment (Herron 2003). The MRI features of spinal coccidioidomycotic spondylodiscitis are nonspecific. An abnormal but minimally narrowed disk, extensive soft tissue involvement, heterogeneous marrow signal intensity, and a lack of bony deformity are features that suggest coccidioidomycosis (Olson et al. 1998). The posterior elements alone may rarely be affected but are not uncommonly involved with advanced disease. One-third of patients have contiguous or noncontiguous multiple levels of disease (Olson et al. 1998). Extraosseous soft tissue involvement is typical and is usually extensive, with spread beneath the longitudinal ligaments and epidural disease (Fig. 4).
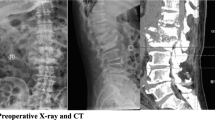
A 59-year-old man with T10-11 coccidioidomycotic spondylodiscitis. (a) Lateral radiograph shows destruction and collapse of the T10 and T11 vertebral bodies and T10/11 disk (arrows), producing a kyphotic deformity. (b) Sagittal CT image shows the extent of discovertebral destruction in greater detail, including several small bony fragments. Sagittal (c) T1-W, (d) T2-W and (e) contrast-enhanced fat-suppressed T1-W MR images show T1-hypointense and heterogeneous T2-hyperintense signal alteration of the infected vertebral bodies with moderate enhancement, including rim enhancement around the T10/11 discovertebral fluid collection. Anterior subligamentous (small arrows) and epidural (arrowhead) extensions are present. (f) Axial contrast-enhanced fat-suppressed T1-W MR image shows involvement of the posterior elements bilaterally, as well as anterior and paravertebral soft tissue extension (arrows). [Courtesy of Prof. Mihra Taljanovic, University of New Mexico, Albuquerque, USA]
Serological testing and biopsy are the mainstays of diagnosis. Mature spherules with endospores on pathology indicate Coccidioides immitis infection (Herron 2003). The preferred medical treatment is amphotericin B and flucytosine for 2 weeks and then fluconazole for a minimum of 10 weeks (Kim et al. 2006). The indications for surgical treatment in coccidioidal spondylodiscitis are those of spinal surgery in general, namely, instability, neurological deficit, and/or deformity (Herron 2003).
7 Blastomycosis
Blastomyces dermatitidis is a dimorphic fungus endemic in the southeastern and south central states of the United States. It is considered to be an inhabitant of soil, and infection occurs by inhalation of conidia. Hematogeneous dissemination of infection to almost any organ can occur months to years after the initial pulmonary involvement (Kuzo and Goodman 1996). The skin is the most common extrapulmonary site, with a 40–80% incidence (Hadjipavlou et al. 1998). Skeletal blastomycosis is seen in 14–60% of disseminated cases (Riegler et al. 1974; Hadjipavlou et al. 1998). The spine is the most common site of skeletal involvement, followed by the skull, ribs, tibia, and the bones of the foot and wrist.
The lower thoracic and lumbar spines are most affected. The anterior aspect of the vertebral body is usually affected initially. Further bone destruction can lead to vertebral compression fractures, and spread to adjacent vertebral bodies is through the disk (Kim et al. 2006). Nonadjacent vertebral bodies also can be affected by spread of infection along the anterior longitudinal ligament. Infection can lead to psoas or paravertebral abscesses. With Blastomyces, collapse and gibbus deformity tends to be seen more commonly. As in tuberculosis, blastomycosis can form large paraspinal abscesses that occasionally extend into the groin and upper thigh with fistula formation.
The diagnosis can be made only by visualization of the yeast in pus, sputum, and secretions and on the basis of the histological examination (Hadjipavlou et al. 1998). The most sensitive test, and therefore the gold standard for diagnosis, remains fungal culture which may take several days or weeks. Antigen testing for blastomycosis antigens can be performed with urine and serum, using enzyme immunoassay (EIA). PCR testing of culture material and formalin-fixed paraffin-embedded tissue is also available (Emamian et al. 2019). The preferred treatment for blastomycosis is amphotericin B for life-threatening disease and itraconazole for 6–12 months for mild to moderate disease. Local debridement with abscess drainage may be necessary for spinal or skin involvement (Detrisac et al. 1980).
8 Mycetoma
Mycetoma is a neglected tropical disease that is endemic in many tropical and subtropical areas. Mycetoma is a chronic mutilating disease of the skin and the underlying tissues which is caused by fungi (eumycetoma) or bacteria (actinomycetoma). The most common pathogens reported in eumycetoma are Madurella mycetomatis, Madurella grisea, Pseudallescheria boydii, and Leptosphaeria senegalensis. It follows implantation of infectious organisms into subcutaneous tissue, from where infection spreads to the skin and bone. The organisms form small microcolonies that are discharged onto the skin surface via sinus tracts or can burrow into other adjacent tissues including the bone (Zijlstra et al. 2016).
Mycetoma occurs in all age groups but is rarely seen in children. It commonly occurs in field laborers and cultivators whose occupation involves direct contact with the soil (Lichon and Khachemoune 2006). The foot is the commonest site affected by mycetoma (70%), followed by the hand (12%) (Fahal 2004). Spinal cord involvement is rare, and only a few cases have been reported (Cascio et al. 2011; Fahal 2011). In mycetoma, spread occurs locally and through the lymphatics. Hematological spread has also been described.
In early disease, radiographs are essentially normal. Eventually a soft tissue mass may be seen as a dense shadow or as multiple scattered soft tissue shadows. Later on, there may be bone scalloping, periosteal reaction, and multiple punched-out cavities. MRI is useful for determining the extent of the lesions and invasion of structures. It usually shows multiple small lesions (2–5 mm) of hyperintense signal, interspersed within a hypointense matrix. The “dot in circle” sign, which indicates the presence of grains, highly characteristic (Fahal 2017).
Different laboratory-based diagnostic techniques are available to determine and identify the causative agents. These include direct microscopy and cytological, histopathological, and immunohistochemical techniques in addition to the classical grain culture and molecular-based techniques (Fahal 2017). Treatment of mycetoma is still based on expert opinion, in the absence of WHO treatment guidelines. Varying antimicrobial treatment options for actinomycetoma exist. Eumycetoma treatment usually poses a challenge. Antifungals are used, and in many cases, a combination of surgery and antifungals is preferred (Emmanuel et al. 2018).
9 Conclusion
Fungal spondylodiscitis remains a rare pathology, although an increased incidence has been reported. Fungal infection should be considered in an immunodeficient patient with lumbar pain, progressive onset with atypical changes on the spine imaging, negative cultures, and persistent symptoms despite antibiotic treatment.
Abbreviations
- CT:
-
Computed tomography
- MRI:
-
Magnetic resonance imaging
- PCR:
-
Polymerase chain reaction
References
Andres A, Feliza R, Mauricio C (2014) Spinal infections: clinical and imaging features. Top Magn Reson Imaging 23:303–314
Arias F, Mata-Essayag S, Landaeta ME et al (2004) Candida albicans osteomyelitis: case report and literature review. Int J Infect Dis 8:307–314
Bonakdarpour A, Gaines VD (1983) The radiology of osteomyelitis. Orthop Clin North Am 14:21–33
Casadevall A, Perfect JR (1998) Cryptococcus neoformans. ASM Press, Washington, DC, pp 407–456
Cascio A, Mandraffino G, Cinquegrani M et al (2011) Actinomadura pelletieri mycetoma—an atypical case with spine and abdominal wall involvement. J Med Microbiol 60:673–676
Chhem RK, Wang S, Jaovisidha S et al (2001) Imaging of fungal, viral, and parasitic musculoskeletal and spinal diseases. Radiol Clin North Am 39:357–378
Cornely OA, Bassetti M, Calandra T et al (2012) ESCMID guideline for the diagnosis and management of Candida diseases 2012: non-neutropenic adult patients. Clin Microbiol Infect 18(Suppl 7):19–37
Dagirmanjian A, Schils J, McHenry M et al (1996) MR imaging of vertebral osteomyelitis revisited. AJR Am J Roentgenol 167:1539–1543
Dalinka MK, Dinnenberg S, Greendyk WH et al (1971) Roentgenographic features of osseous coccidioidomycosis and differential diagnosis. J Bone Joint Surg Am 53:1157–1164
Detrisac DA, Harding WG, Greiner AL et al (1980) Vertebral North American blastomycosis. Surg Neurol 13:311–312
Emamian S, Fox MG, Boatman D et al (2019) Spinal blastomycosis: unusual musculoskeletal presentation with literature review. Skeletal Radiol 48:2021–2027
Emmanuel P, Dumre SP, John S et al (2018) Mycetoma: a clinical dilemma in resource limited settings. Ann Clin Microbiol Antimicrob 17:35. https://doi.org/10.1186/s12941-018-0287-4
Fahal AH (2004) Mycetoma: a thorn in the flesh (2006). Trans R Soc Trop Med Hyg 98:3–11
Fahal AH (2011) Mycetoma. Review article. Khartoum Med J 4:514–523
Fahal AH (2017) Mycetoma. In: Current progress in medical mycology. Springer Nature, pp 355–380
Galgiani JN (1993) Coccidioidomycosis. West J Med 159:154–171
Govender S (2003) Aspergillosis of the spine. In: Govender S, Leong JCY (eds) Inflammatory diseases of the spine. TTG Asia, Singapore, pp 13.1–13.8
Govender S, Rajoo R, Goga IE et al (1991) Aspergillus osteomyelitis of the spine. Spine 16:746–749
Gupta SK, Chhabra R, Sharma BS et al (2003) Vertebral cryptococcosis simulating tuberculosis. Br J Neurosurg 17:556–559
Hadjipavlou AG, Mader JT, Nauta HJ et al (1998) Blastomycosis of the lumbar spine: case report and review of the literature, with emphasis on diagnostic laboratory tools and management. Eur Spine J 7:416–421
Heinrich SD, Finney T, Craver R et al (1991) Aspergillus osteomyelitis in patients who have chronic granulomatous disease. J Bone Joint Surg Am 73:456–460
Herbrecht R, Denning DW, Patterson TF et al (2002) Invasive Fungal Infections Group of the European Organisation for Research and Treatment of Cancer and the Global Aspergillus Study Group. Voriconazole versus amphotericin B for primary therapy of invasive aspergillosis. N Engl J Med 347:408–415
Herron L (2003) Coccidioidal spondylitis. In: Govender S, Leong JCY (eds) Inflammatory diseases of the spine. TTG Asia, Singapore, pp 14.1–14.9
Hoeprich PD, Hoeprich PD, Jordan C et al (1994) Cryptococcosis. In: Infectious diseases. Lippincott-Raven, Philadelphia, pp 1132–1140
Hong SH, Choi JY, Lee JW et al (2009) MR imaging assessment of the spine: infection or an imitation? Radiographics 29:599–612
Hummel M, Schuler S, Weber U et al (1993) Aspergillosis with Aspergillus osteomyelitis and diskitis after heart transplantation: surgical and medical management. J Heart Lung Transplant 12:599–603
Huntington RW, Waldmann WJ, Sargent JA et al (1967) Pathologic and clinical observations on 142 cases of fatal coccidioidomycosis. In: Ajello L (ed) Coccidioidomycosis. University of Arizona Press, Tucson, pp 221–222
Jung NY, Jee WH, Ha KY et al (2004) Discrimination of tuberculous spondylitis from pyogenic spondylitis on MRI. AJR Am J Roentgenol 182:1405–1410
Kiertiburanakul S, Wirojtananugoon S, Pracharktam R et al (2006) Cryptococcosis in human immunodeficiency virus-negative patients. Int J Infect Dis 10:72–78
Kim CW, Perry A, Currier B et al (2006) Fungal infections of the spine. Clin Orthop Relat Res 444:92–99
Korovessis P, Repanti M, Katsardis T et al (2014) Anterior decompression and fusion for aspergillus osteomyelitis of the lumbar spine associated with paraparesis. Spine 19:2715–2718
Kuzo RS, Goodman LR (1996) Blastomycosis. Semin Roentgenol 31:45–51
Kwon JW, Hong SH, Choi SH et al (2011) MRI findings of Aspergillus spondylitis. AJR Am J Roentgenol 197:W919–W923
Legarth RA, Christensen M, Calum H et al (2014) Cryptococcal rib osteomyelitis as primary and only symptom of idiopathic CD4 penia. Med Mycol Case Rep 4:16–18
Lichon V, Khachemoune A (2006) Mycetoma: a review. Am J Clin Dermatol 7:315–321
Nicolle A, De la Blanchardière A, Bonhomme J et al (2013) Aspergillus vertebral osteomyelitis in immunocompetent subjects: case report and review of the literature. Infection 41:833–840
O’Shaughnessy EM, Shea YM, Witebsky FG (2003) Laboratory diagnosis of invasive mycoses. Infect Dis Clin North Am 17:135–158
Olson EM, Duberg AC, Herron LD et al (1998) Coccidioidal spondylitis: MR findings in 15 patients. AJR Am J Roentgenol 171:785–789
Pappas PG, Kauffman CA, Andes DR et al (2016) Clinical Practice Guideline for the Management of Candidiasis: 2016 update by the Infectious Diseases Society of America. Clin Infect Dis 62:e1–e50
Richaud C, De Lastours V, Panhard X et al (2017) Candida vertebral osteomyelitis (CVO) 28 cases from a 10-year retrospective study in France. Medicine (Baltimore) 96:e7525
Riegler HF, Goldstein LA, Betts RF (1974) Blastomycosis osteomyelitis. Clin Orthop Relat Res 100:225–231
Skaf GS, Kanafani ZA, Araj GF et al (2010) Non-pyogenic infections of the spine. Int J Antimicrob Agents 36:99–105
Ur-Rahman N, Jamjoom ZA, Jamjoom A (2000) Spinal aspergillosis in non-immunocompromised host mimicking Pott’s paraplegia. Neurosurg Rev 23:107–111
Walsh TJ, Anaissie EJ, Denning DW et al (2008) Infectious Diseases Society of America. Treatment of aspergillosis: clinical practice guidelines of the Infectious Diseases Society of America. Clin Infect Dis 46:327–360
Whelan MA, Schonfeld S, Post JD et al (1985) Computed tomography of nontuberculous spinal infection. J Comput Assist Tomogr 9:280–287
Zijlstra EE, Van de Sande WW, Welsh O et al (2016) Mycetoma: a unique neglected tropical disease. Lancet Infect Dis 16:100–112
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Riahi, H., Ladeb, M.F., Chelli Bouaziz, M., Ammari, L., Rammeh, S. (2021). Imaging of Fungal Spondylodiscitis. In: Ladeb, M.F., Peh, W.C. (eds) Imaging of Spinal Infection. Medical Radiology(). Springer, Cham. https://doi.org/10.1007/978-3-030-70459-9_14
Download citation
DOI: https://doi.org/10.1007/978-3-030-70459-9_14
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-70458-2
Online ISBN: 978-3-030-70459-9
eBook Packages: MedicineMedicine (R0)