Abstract
Dermatophytes are a group of fungal agents that can invade humans’ keratinized tissues such as skin, nail, and hair, thereby causing dermatophyte infection (dermatophytosis) or ringworm. Some natural products have been reported to possess fungicidal effects. Hence, the present study investigated the effect of curcuminoids (CUR) and difluorinated curcumin (CDF) against clinical isolates of dermatophytes. CUR and CDF powders were evaluated against dermatophyte species including Trichophyton tonsurans (n = 21), T. mentagrophytes (n = 19), T. interdigitale (n = 18), Microsporum canis (n = 4), T. benhamiae (n = 1), and T. verrucosum (n = 1), based on the CLSI M38-A2 guideline. The minimum inhibitory concentration (MIC) ranges of CUR were 4–16, 8–16, 4–16, 8, 8, and 16 μg/ml for T. tonsurans, T. mentagrophytes, T. interdigitale, M. canis, T. benhamiae, and T. verrucosum, respectively. In addition, MIC ranges of CDF were obtained as 2–32, 4–16, 0.125–16, 8–16, 8, and 16 μg/ml, for T. tonsurans, T. mentagrophytes, T. interdigitale, M. canis, T. benhamiae, and T. verrucosum, respectively. CUR and CDF showed an inhibitory effect against dermatophyte isolates. CDF showed a stronger effect than CUR, especially against T. interdigitale. CUR and CDF have the capacity to be developed for use in dermatophytosis to augment existing preventative/therapeutic strategies.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
8.1 Introduction
Dermatophytes as keratinophilic fungi can invade to keratinized tissues of vertebrates. They can cause dermatophytosis (tinea or ringworm), as various disorders in the skin, nails, and hair, and also deep tissue in some cases [1]. More than 50 species of dermatophytes have been introduced as causative agents of dermatophytosis in different parts of the world [2]. The dermatophytosis prevalence and causative agents varies depending on the geographical area and its climate, as well as the lifestyle of the people [3]. However, the dermatophyte species express various susceptibility to antifungal drugs [4]. Some of species may cause chronic and do not respond well to the usual therapeutic procedure [5]. There are reports regarding drug resistance among various dermatophyte species in vitro and in vivo results [6]. Thus, it can lead to fail or requires long-term treatment, and cause anxiety with serious complications for this group of patients [7]. As resistance to antifungal drugs has been increased, natural products and nanoparticles can being widely screened as the potential sources of novel antifungal agents [8, 9]. In many cases and in recent years, herbal extracts and their derivatives have been used to cure infectious diseases, especially fungal infections [10, 11]. These plants can usually produce aromatic chemicals and secondary metabolites against microbial pathogens [12]. Many studies have been conducted to determine antifungal susceptibility by testing the clinical isolates [9]. However, these studies have been limited to some specific types of fungal agents and the antifungal patterns [13]. Nonetheless, there is restricted information regarding the in vitro activity of herbal plants against various species of dermatophytes. Therefore, the determination of antifungal susceptibility of herbal plants on dominant dermatophytes seems necessary. Curcuminoids (CUR) are natural polyphenols extracted from turmeric, which are known to have numerous pharmacological effects [14,15,16,17,18,19,20]. A fluorinated analog of CUR, named difluorinated curcumin (CDF), has been introduced with improved metabolic stability and pharmacological activity [21, 22]. The fungicidal activity of CUR against some fungi has been shown [10]. However, no information has been provided on the antifungal effect of this plant and its synthetic derivatives against different species of dermatophytes. Concerning this, the aim of present study was to investigate the effect of CUR and CDF against clinical isolates of dermatophytes obtained from patients with dermatophytosis.
8.2 Materials and Methods
The clinical isolates of dermatophytes were previously identified based on molecular method (ITS sequencing) [23, 24]. They included six species of Trichophyton tonsurans (n = 21), T. mentagrophytes (n = 19), T. interdigitale (n = 18), Microsporum canis (n = 4), T. benhamiae (n = 1), and T. verrucosum (n = 1).
Difluorinated curcumin was prepared using the synthesis method previously described [25]. Briefly, a solution comprising curcumin (1 mmol) and piperidine (0.05 mmol) was added to difluorobenzaldehyde (1 mmol) in methanol. At room temperature under a nitrogen stream, the reaction mixture was stirred for 48 h. The chemical structure of difluorinated curcumin was confirmed with the use of nuclear magnetic resonance (NMR).
The CLSI M38A2 guideline was used to antifungal susceptibility testing procedure [4]. Briefly, the dermatophytes were cultured on potato dextrose agar (Sigma, Germany) and incubated at 30 °C for 2 weeks. Fungal suspensions containing harvested conidia and hyphal fragments were prepared using sterile saline solution along with Tween 20. They were evaluated using a spectrophotometer at a wavelength of 530 nm to reach a 65–70% transmittance. The suspension was diluted 1:50 in RPMI 1640 medium to achieve the final concentrations (1–3 × 103 CFU/ml). The inocula along with the indicated concentrations of CUR and CDF were added to 96-well plates, and incubated at 35 °C for 3–5 days. The final concentrations of CUR and CDF were 0.0625–16 (0.0625, 0.125, 0.25, 0.5, 1, 2, 4, 8 and 16) μg/ml, Finally, the minimum inhibitory concentration (MIC) ranges were determined visually as the lowest concentration of CUR/ CDF that resulted in at least 80% growth inhibition, compared to the growth of the control well. The definition of MIC50 and MIC90 was as inhibition the minimum concentration at which 50% and 90% of the isolates, respectively. The average geometric mean (GM) of the MICs of the antifungal compounds, and differences between the mean values were determined using the SPSS software (version 16).
8.3 Results
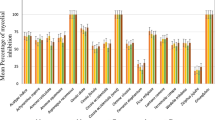
The detailed information on the results of antifungal effects of CUR and CDF against the dermatophyte clinical isolates is shown in Table 8.1.
According to the results, generally, CDF had a more effect than CUR, and T. interdigitale showed the lowest MIC with 0.125 μg/ml than other species. Followed by T. tonsurans at concentration of 2 μg/ml. However, CUR had a more effect on T. interdigitale and T. tonsurans than other species with 4–16 μg/ml. Accordingly , CDF had also the lowest MIC50 for T. interdigitale at concentration of 4 μg/ml. However, T. mentagrophytes showed the highest MIC50 and MIC90 at concentration of 16 μg/ml.
The GM of CUR for T. tonsurans, T. mentagrophytes, T. interdigitale, and M. canis were estimated at 9.75, 11.52, 9.33, and 8, respectively. Moreover, CDF of GM for T. tonsurans, T. mentagrophytes, T. interdigitale, and M. canis were estimated at 6.56, 8.92, 2.61, and 9.51, respectively. Due to small number, GM MIC values of T. benhamiae and T. verrucosum species could not be achieved. Generally, the dermatophyte isolates showed GM MIC values of 5.78 and 10.04 for CUR and CDF, respectively. Furthermore, according to the GM MIC, CDF was the most effective agent against species of T. interdigitale, T. tonsurans, and T. mentagrophytes, respectively.
8.4 Discussion
Although few reports of resistance to antifungal agents have been presented on dermatophytes as causative agents of dermatophytosis; the development of resistance to the current clinically used antifungal drugs, has emerged as a growing problem [26, 27]. Several dermatophyte species, in particular, T. interdigitale and T. rubrum described are resistant or less susceptible to several classes of antifungals [28]. It appears the developed acquisition of resistance mechanisms to antifungal agents be following a prior exposure [28]. The present study was aimed at evaluating the activity of CUR and CDF against the clinical isolates of dermatophytes obtained from patients affected by dermatophytosis. In general, both tested compounds exhibited good activity against all tested isolates. Collectively, these data demonstrated that CUR/CDF have the therapeutic potential to be used in dermatophytosis. Natural products can be used as the potential sources of novel antifungal agents, particularly in the case of acquired or high antifungal resistance [8, 11]. Traditionally, medicinal plants have been investigated to prevent and cure infectious diseases [29]. They can produce aromatic chemicals and secondary metabolites as defense mechanisms and antimicrobial effects [12]. Polyphenols, found in various edible plants, may serve as an alternative source of antimicrobials [10]. CUR is a bioactive polyphenol that is extracted from the rhizomes of the Curcuma longa plant [30]. Curcumin constitutes typically about less than 5% of turmeric composition [31, 32]. Interestingly, it displays broad-spectrum antimicrobial activity, particularly antibacterial and antifungal properties [33,34,35]. Also, it is able to influence the adhesion ability of bacteria, whereby less fimbriae leads to reduced adhesion ability against planktonic and biofilm cells [36, 37]. Possibly, CUR can directly impact cell wall permeability through signaling of the MAP kinase and calcineurin-mediated signaling, pathways which play significant role in cell wall integrity [38]. Interestingly, some studies showed that CUR can reduce the production of aflatoxin B1 by Aspergillus flavus too [39].
There is little information about the use of CUR as a natural antifungal compound for fungal pathogens so far. Unfortunately, up until now, there is no significant report about CDF antifungal effect, as a CUR analogue, against fungal pathogens too. However, most of studies investigated CUR effect again Candida and Aspergillus species [10, 35]. To our knowledge, there have been no studies that report on pathogenic dermatophytes. In a study, Martins et al. (2009) investigated the antifungal effects of CUR and fluconazole against Candida spp., Cryptococcus neoformans, Sporothrix schenckii, Paracoccidioides brasiliensis and Aspergillus species [35]. They reported P. brasiliensis isolates were the most susceptible to CUR while the growth of Aspergillus isolates was not affected. Moreover, CUR was much more efficient than fluconazole in inhibiting the adhesion of Candida species to human buccal epithelial cells. They obtained that a MIC range of 0.5–32 μg/ml against P. brasiliensis isolates, but in our study the MIC range were 4–16, 0.125–32 μg/ml for CUR and CDF, respectively. Our results indicate that CDF may be a promising compound for the design of new antifungal agents capable of inhibiting of P. brasiliensis with more impact. To the best of our knowledge, this study reports for the first time the effect of CUR and CDF on the growth of dermatophytes of clinical interest. Our in vitro results highlight the potential of CUR and CDF as the effective antifungals against various dermatophytes strains including T. tonsurans, T. mentagrophytes, T. interdigitale, M. canis, T. benhamiae, and T. verrucosum. Among the dermatophyte isolates examined in the present study, the widest MIC range of CDF was observed for T. interdigitale (0.125–16 μg/ml) that is higher than those obtained for CUR. This concentration show that CDF could act against dermatophyte species more effectively, particularly on T. interdigitale. This is important since the T. interdigitale species is one of the most common species among patients with dermatophytosis in the world. Therefore, it can play an effective role in the prevention and treatment of dermatophytosis. The widest MIC range of CUR was observed for T. tonsurans T. tonsurans with 4–16 μg/ml. However, CUR showed more effect against them than other species. The MIC50 of CDF against T. interdigitale (with 4 μg/ml concentration) was lower than CUR, thus showing a stronger effect against this species. However, the MIC50 (8 μg/ml) of CDF was equal to CUR for the 64 dermatophyte isolates in general. Nevertheless, several studies have shown that the different types of fungal agents have different sensitivities to CUR [35, 40]. In a study performed by Alalwan et al. (2017) investigating the antifungal effects of CUR, was reported to be efficient in 50 μg/ml concentration to inhibit and kill C. albicans [10]. This concentration is different from the results obtained against dermatophyte isolates in the present study. It appears that different fungal pathogens could show various susceptibility to CUR. In the case of clinical pathogenic fungi, this difference can be even due to different geographical locations. In this regard, general and specific relevance of environmental conditions can affect specific secretion of enzymes and the expression of certain genes in pathogenic fungi [41]. Furthermore, the number of fungi examined and their diversity can fundamentally influence the results. Thus, one of the limitations of the present study was the low number of clinical isolates of dermatophytes.
In another study by Garcia-Gomes et al., the synergistic effect of curcumin and fluconazole was evaluated on the C. albicans isolate resistant to fluconazole [42]. They showed that CUR has a great capability to inhibit fluconazole resistance of the isolate of C. albicans, and it could restore its sensitivity to this azole. Therefore, interestingly, azole-resistant isolates can be further investigated by azole-CUR whether such combinations can be beneficial. Oglah et al. in their review article stated that analogues of CUR had antifungal activities against the genera of Aspergillus, Penicillium and Alternaria [43]. Therefore, the use of these analogues can be evaluated among the clinical isolates too. However, there are no reports of possible effects of CUR and its analogues on dermatophytes.
The present study was the first attempt investigating the antifungal effect of CUR and its analogue (CDF) against clinical dermatophyte isolates obtained from dermatophytosis. Based on the results of the present study, and according to GM definition, CUR and CDF, particularly CDF had an effective impact against the dermatophyte isolates. Furthermore, among dermatophyte species, T. interdigitale showed a greater sensitivity to CDF and CUR, respectively.
8.5 Conclusion
As the results of the present study indicated, CUR and CDF had respectively the antifungal effect against clinical isolates of dermatophyte . Furthermore, none of the dermatophyte isolates showed too high MIC to these compounds. Additionally, T. interdigitale, as a common agent of dermatophytosis in the world, showed the lowest GM (the highest sensitivity) to CDF and CUR, respectively.
References
Weitzman I, Summerbell RC (1995) The dermatophytes. Clin Microbiol Rev 8(2):240–259
de Hoog GS, Dukik K, Monod M, Packeu A, Stubbe D, Hendrickx M et al (2017) Toward a novel multilocus phylogenetic taxonomy for the dermatophytes. Mycopathologia 182(1–2):5–31
White TC, Oliver BG, Gräser Y, Henn MR (2008) Generating and testing molecular hypotheses in the dermatophytes. Eukaryot Cell 7(8):1238–1245
Behnam M, Zarrinfar H, Najafzadeh MJ, Naseri A, Jarahi L, Novak Babič M (2020) Low in vitro activity of sertaconazole against clinical isolates of dermatophyte. Curr Med Mycol 6(1):36–41
Ghannoum M (2016) Azole resistance in dermatophytes: prevalence and mechanism of action. J Am Podiatr Med Assoc 106(1):79–86
Mukherjee PK, Leidich SD, Isham N, Leitner I, Ryder NS, Ghannoum MA (2003) Clinical Trichophyton rubrum strain exhibiting primary resistance to terbinafine. Antimicrob Agents Chemother 47(1):82–86
Coelho LM, Aquino-Ferreira R, Maffei CML, Martinez-Rossi NM (2008) In vitro antifungal drug susceptibilities of dermatophytes microconidia and arthroconidia. J Antimicrob Chemother 62(4):758–761
Gupta AK, Foley KA, Versteeg SG (2017) New antifungal agents and new formulations against dermatophytes. Mycopathologia 182(1):127–141
Kazemi M, Akbari A, Zarrinfar H, Soleimanpour S, Sabouri Z, Khatami M et al (2020) Evaluation of antifungal and photocatalytic activities of gelatin-stabilized selenium oxide nanoparticles. J Inorg Organomet Polym Mater
Alalwan H, Rajendran R, Lappin DF, Combet E, Shahzad M, Robertson D et al. (2017) The anti-adhesive effect of curcumin on Candida albicans biofilms on denture materials. Front Microbiol 8659
Katiraee F, Eidi S, Bahonar A, Zarrinfar H, Khosravi A (2008) Comparision of MICs of some Iranian herbal essences against azole resistance and azole susceptible of Candida Albicans. J Med Plants 3(27):37–44
Gupta SC, Patchva S, Koh W, Aggarwal BB (2012) Discovery of curcumin, a component of golden spice, and its miraculous biological activities. Clin Exp Pharmacol Physiol 39(3):283–299
Pakshir K, BAHA AL, Rezaei Z, Sodaifi M, Zomorodian K (2009) In vitro activity of six antifungal drugs against clinically important dermatophytes
Soleimani V, Sahebkar A, Hosseinzadeh H (2018) Turmeric (Curcuma longa) and its major constituent (curcumin) as nontoxic and safe substances: Review. Phytother Res 32(6):985–995
Panahi Y, Khalili N, Sahebi E, Namazi S, Simental-Mendía LE, Majeed M, Sahebkar A. Effects of Curcuminoids Plus Piperine on Glycemic, Hepatic and Inflammatory Biomarkers in Patients with Type 2 Diabetes Mellitus: A Randomized Double-Blind Placebo-Controlled Trial. Drug Res (Stuttg). 2018 Jul;68(7):403-409. doi: 10.1055/s-0044-101752.
Mollazadeh H, Cicero AFG, Blesso CN, Pirro M, Majeed M, Sahebkar A (2019) Immune modulation by curcumin: the role of interleukin-10. Crit Rev Food Sci Nutr 59(1):89–101
Momtazi AA, Derosa G, Maffioli P, Banach M, Sahebkar A (2016) Role of micro RNAs in the therapeutic effects of curcumin in non-Cancer diseases. Mol Diagn Ther 20(4):335–345
Saberi-Karimian M, Keshvari M, Ghayour-Mobarhan M, Salehizadeh L, Rahmani S, Behnam B, Jamialahmadi T, Asgary S, Sahebkar A (2020) Effects of curcuminoids on inflammatory status in patients with non-alcoholic fatty liver disease: A randomized controlled trial. Complement Therap Med. 49, art. no. 102322. https://doi.org/10.1016/j.ctim.2020.102322
Ghandadi M, Sahebkar A (2017) Curcumin: An effective inhibitor of interleukin-6. Curr Pharm Des 23(6):921–931
Teymouri M, Pirro M, Johnston TP, Sahebkar A (2017) Curcumin as a multifaceted compound against human papilloma virus infection and cervical cancers: a review of chemistry, cellular, molecular, and preclinical features. Biofactors 43(3):331–346
Momtazi AA, Sahebkar A (2016) Difluorinated curcumin: a promising curcumin analogue with improved anti-tumor activity and pharmacokinetic profile. Curr Pharm Des 22(28):4386–4397
Padhye S, Banerjee S, Chavan D, Pandye S, Swamy KV, Ali S et al (2009) Fluorocurcumins as cyclooxygenase-2 inhibitor: molecular docking, pharmacokinetics and tissue distribution in mice. Pharm Res 26(11):2438–2445
Ebrahimi M, Zarrinfar H, Naseri A, Najafzadeh MJ, Fata A, Parian M et al (2019) Epidemiology of dermatophytosis in northeastern Iran; a subtropical region. Curr Med Mycol 5(2):16
Nejati-Hoseini R, Zarrinfar H, Parian Noghani M, Parham S, Fata A, Rezaei-Matehkolaei A (2019) Identification of dermatophytosis agents in Mashhad, Iran, by using polymerase chain reaction sequencing (PCR sequencing) method. J Isfahan Med Sch 37:256–262
Qiu X, Du Y, Lou B, Zuo Y, Shao W, Huo Y et al (2010) Synthesis and identification of new 4-arylidene curcumin analogues as potential anticancer agents targeting nuclear factor-kappaB signaling pathway. J Med Chem 53(23):8260–8273
Shivamurthy RPM, Reddy SGH, Kallappa R, Somashekar SA, Patil D, Patil UN (2014) Comparison of topical anti-fungal agents sertaconazole and clotrimazole in the treatment of tinea corporis-an observational study. J Clin Diagn Res 8(9):HC09
Carrillo-Muñoz A, Fernández-Torres B, Cárdenes D, Guarro J (2003) In vitro activity of sertaconazole against dermatophyte isolates with reduced fluconazole susceptibility. Chemotherapy 49(5):248–251
Martinez-Rossi NM, Bitencourt TA, Peres NTA, Lang EAS, Gomes EV, Quaresemin NR et al (2018) Dermatophyte resistance to antifungal drugs: mechanisms and prospectus. Front Microbiol:91108–91108
Prasad CS, Shukla R, Kumar A, Dubey N (2010) In vitro and in vivo antifungal activity of essential oils of Cymbopogon martini and Chenopodium ambrosioides and their synergism against dermatophytes. Mycoses 53(2):123–129
Mahmood K, Zia KM, Zuber M, Salman M, Anjum MN (2015) Recent developments in curcumin and curcumin based polymeric materials for biomedical applications: a review. Int J Biol Macromol:81877–81890
Esatbeyoglu T, Huebbe P, Ernst IM, Chin D, Wagner AE, Rimbach G (2012) Curcumin—from molecule to biological function. Angew Chem Int Ed 51(22):5308–5332
Kwon Y (2014) Estimation of curcumin intake in Korea based on the Korea National Health and nutrition examination survey (2008-2012). Nutr Res Pract 8(5):589–594
Zorofchian Moghadamtousi S, Abdul Kadir H, Hassandarvish P, Tajik H, Abubakar S, Zandi K (2014) A review on antibacterial, antiviral, and antifungal activity of curcumin. Biomed Res Int 2014
Tyagi P, Singh M, Kumari H, Kumari A, Mukhopadhyay K (2015) Bactericidal activity of curcumin I is associated with damaging of bacterial membrane. PLoS One 10(3)
Martins C, Da Silva D, Neres A, Magalhaes T, Watanabe G, Modolo L et al (2009) Curcumin as a promising antifungal of clinical interest. J Antimicrob Chemother 63(2):337–339
Shahzad M, Millhouse E, Culshaw S, Edwards CA, Ramage G, Combet E (2015) Selected dietary (poly) phenols inhibit periodontal pathogen growth and biofilm formation. Food Funct 6(3):719–729
Shahzad M, Sherry L, Rajendran R, Edwards CA, Combet E, Ramage G (2014) Utilising polyphenols for the clinical management of Candida albicans biofilms. Int J Antimicrob Agents 44(3):269–273
Kumar A, Dhamgaye S, Maurya IK, Singh A, Sharma M, Prasad R (2014) Curcumin targets cell wall integrity via Calcineurin-mediated signaling in <span class="named-content genus-species" id="named-content-1">Candida albicans</span>. Antimicrob Agents Chemother 58(1):167–175
Temba BA, Fletcher MT, Fox GP, Harvey J, Okoth SA, Sultanbawa Y (2019) Curcumin-based photosensitization inactivates Aspergillus flavus and reduces aflatoxin B1 in maize kernels. Food Microbiol:8282–8288
Murugesh J, Annigeri RG, Mangala GK, Mythily PH, Chandrakala J (2019) Evaluation of the antifungal efficacy of different concentrations of Curcuma longa on Candida albicans: an in vitro study. J Oral Maxillofac Pathol: JOMFP 23(2):305–305
Khedmati E, Hashemi Hazaveh SJ, Bayat M, Amini K (2020) Identification of subtilisin virulence genes (SUB1-7) in Epidermophyton floccosum isolated from patients with dermatophytosis in Iran. Gene Rep 20100748
Garcia-Gomes A, Curvelo J, Soares RA, Ferreira-Pereira A (2012) Curcumin acts synergistically with fluconazole to sensitize a clinical isolate of Candida albicans showing a MDR phenotype. Med Mycol 50(1):26–32
Oglah MK, Mustafa YF, Bashir MK, Jasim MH, Mustafa YF (2020) Curcumin and its derivatives: a review of their biological activities. Syst Rev Pharm 11(3):472–481
Acknowledgments
We appreciate the staff of Medical Mycology and Parasitology Laboratory in Ghaem Teaching hospitals affiliated to Mashhad University of Medical Sciences. This work was financially supported by the Deputy of Research of Mashhad University of Medical Sciences (grant No. 951808).
Conflicts of Interest
The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Zarrinfar, H., Behnam, M., Hatamipour, M., Sahebkar, A. (2021). Antifungal Activities of Curcuminoids and Difluorinated Curcumin Against Clinical Dermatophyte Isolates. In: Barreto, G.E., Sahebkar, A. (eds) Pharmacological Properties of Plant-Derived Natural Products and Implications for Human Health. Advances in Experimental Medicine and Biology, vol 1308. Springer, Cham. https://doi.org/10.1007/978-3-030-64872-5_8
Download citation
DOI: https://doi.org/10.1007/978-3-030-64872-5_8
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-64871-8
Online ISBN: 978-3-030-64872-5
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)