Abstract
Fibrinogen is a large glycoprotein, synthesized primarily in the liver. With a normal plasma concentration of 1.5–3.5 g/L, fibrinogen is the most abundant blood coagulation factor. The final stage of blood clot formation is the conversion of soluble fibrinogen to insoluble fibrin, the polymeric scaffold for blood clots that stop bleeding (a protective reaction called hemostasis) or obstruct blood vessels (pathological thrombosis). Fibrin is a viscoelastic polymer and the structural and mechanical properties of the fibrin scaffold determine its effectiveness in hemostasis and the development and outcome of thrombotic complications. Fibrin polymerization comprises a number of consecutive reactions, each affecting the ultimate 3D porous network structure. The physical properties of fibrin clots are determined by structural features at the individual fibrin molecule, fibrin fiber, network, and whole clot levels and are among the most important functional characteristics, enabling the blood clot to withstand arterial blood flow, platelet-driven clot contraction, and other dynamic forces. This chapter describes the molecular structure of fibrinogen, the conversion of fibrinogen to fibrin, the mechanical properties of fibrin as well as its structural origins and lastly provides evidence for the role of altered fibrin clot properties in both thrombosis and bleeding.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Fibrinogen Structure
Quaternary Structure of Fibrinogen
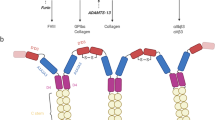
Human fibrinogen is a large 340-kDa oligomeric glycoprotein made up of two symmetrical halves, each containing three polypeptide chains designated Aα, Bβ and γ, with molecular weights of 66,500, 52,000, and 46,500 Da, respectively (Fig. 15.1). The dimeric subunit composition of fibrinogen is presented as (Aα Bβ γ)2 to show that fibrinopeptides A (FpA) and B (FpB) are cleaved by thrombin from the N-termini of each of the Aα and Bβ chains, respectively, to form α and β chains in fibrin. The γ chains remain unaffected by thrombin and the formation of monomeric fibrin from fibrinogen can be described as follows: (Aα Bβ γ)2 → (α β γ)2 + 2FpA + 2FpB. The six subunits are held together by 29 disulfide bonds concentrated in the central nodule of the fibrinogen molecule (Henschen and McDonagh 1986) (Fig. 15.1).

Modified from (Zhmurov et al. 2016)—published with permission from Elsevier
Fibrinogen structure. The atomic resolution structure of about two-thirds of the fibrinogen molecule has been determined by X-ray crystallography (PDB Entry: 3GHG). The folded core of the fibrinogen molecule is shown with addition of portions missing from the crystal structure and reconstructed computationally (in grey), namely: (i) the N-terminal ends of the Aα and Bβ chains with FpA and FpB extending from the central nodule, (ii) the C-terminal portions of the γ-chains containing γ-γ-crosslinking sites, (iii) the αC region composed of the flexible αC connector and compact αC domain (shown on the left halve of the molecule), and (iv) carbohydrate moieties. P, B, and A correspond to the C-terminal A-domain, central B-domain and N-terminal P-domain, respectively, in the γ-nodules. The hinge point is shown in the middle of the α-helical coiled-coil connectors
Tertiary Structure of Fibrinogen
The overall shape of fibrinogen molecules studied using X-ray crystallography, transmission electron microscopy, and atomic force microscopy has been described as a rod-like structure of 45 nm long and 2–5 nm thick (Fig. 15.1) (Hall and Slayter 1959; Fowler and Erickson 1979; Williams 1981; Weisel et al. 1985). Each fibrinogen molecule is composed of two lateral D regions and one central E region, each containing a globular part and a portion of α-helical coiled-coils that connect the lateral globules with the central one (Fig. 15.1) (Medved and Weisel 2009). The X-ray crystallography provided atomic resolution structure of the compact core of fibrinogen (Spraggon et al. 1997; Yee et al. 1997; Brown et al. 2000; Madrazo et al. 2001) while about 30% of the mass of the molecule comprising the unstructured and flexible portions was unresolved. The motifs that could not be crystallized and remained uncharacterized structurally at the atomic level are N-terminal residues Aα1-26, Bβ1-57, and γ1-13 and C-terminal residues Aα201-610, Bβ459-461, and γ395-411 (Kollman et al. 2009).
The largest parts of fibrinogen that are missing in the crystal structure are named the αC regions that comprise residues Aα221-610 at the C-terminal parts of the Aα chains. The Aα chain forms a fourth strand at the distal parts of triple α-helical coiled-coils and then extends outward from the bulk of fibrinogen molecule, making the unstructured αC region (Veklich et al. 1993). Each αC region is tethered to the core of the fibrinogen molecule via a flexible connector (residues Aα221-391) linked to the relatively structured but unstable C-terminal domains (residues Aα392-610) that form transitory intramolecular complexes with the central globule (Fig. 15.1) (Weisel and Medved 2001; Litvinov et al. 2007). These 390 residue-long αC regions were visualized in fibrinogen using transmission electron microscopy (Veklich et al. 1993) and atomic force microscopy (Protopopova et al. 2015; Protopopova et al. 2017) as highly flexible appendages. To recover the complete molecular structure of fibrinogen, the crystallographically unresolved parts have been recreated in silico, i.e. computationally (Fig. 15.1) (Zhmurov et al. 2016; Zuev et al. 2017; Zhmurov et al. 2018).
Domain Structure of Fibrinogen
The fibrinogen molecule is organized into structurally and functionally independent units folded into relatively compact domain structures. The nomenclature for fibrinogen and fibrin recommended by the Scientific and Standardization Committee of the International Society on Thrombosis and Haemostasis (Medved and Weisel 2009) implies that each D or E region contains a number of domains with its own designation, which is different from the name of the region. Based on the X-ray crystallographic data, the central E region is segregated into four domains and each distal D region is divided into seven structural domains. A triple α-helical coiled-coil-E domain containing all three chains is formed next to the central nodule in each of two symmetrical halves of the E region. The N-terminal portions of both γ chains connected at the center of the E region form the single asymmetric γN-domain. On the opposite side of the globular portion of the E region, the N-termini of two Aα and two Bβ chains form the funnel-shaped domain. In each of the D regions, a triple α-helical coiled-coil-D domain is formed next to the globular part by the intertwined portions of all three chains. The C-terminal portion of the β chain is folded into the β-nodule (or β-module) and the C-terminal portion of the γ chain forms a compact γ-nodule (or γ-module). Both the β-and γ-nodules each consist of three distinct domains identified in the crystal structure and designated as N-terminal A-domain, central B-domain and C-terminal P-domain roughly shown in Fig. 15.1 (Medved and Weisel 2009). Notably, the structurally distinct domains of a fibrinogen molecule contain functionally important binding sites mediating multiple molecular interactions of fibrinogen.
The Coiled-Coil Connectors
Remarkable and functionally important parts of fibrinogen are the two 17 nm long α-helical coiled-coils that join the central nodule and end globular parts (Fig. 15.1). The α-helical connectors are formed of the intertwined segments of three polypeptide chains, Aα Bβ and γ, each segment containing 111 or 112 amino acid residues. The chains form three right-handed α-helices that wind around each other to form a left-handed supercoil (Cohen and Parry 1990). Importantly, each of the coiled-coils has a fourth helix in the bundle containing 30 residues (Aα166 to Aα195) that begins at the lateral end of the coiled-coil where the Aα chain goes in the reverse direction for about ¼ of the length of the coiled-coil, at which point the rest of the C-terminal part of the Aα chain becomes outstretched (Spraggon et al. 1997). The coiled-coils can bend around a hinge point located in the γ chain near the residue γAsn52 shown in Fig. 15.1 (Marsh et al. 2013). The hinge points of the coiled-coils are highly susceptible to plasmin cleavage, resulting in formation of fibrinogen’s fragments. The hinge also determines the flexibility of fibrinogen molecules observed at interfaces (Köhler et al. 2015) or in solution (Zuev et al. 2017), and has a biomechanical role discussed below.
Carbohydrate Moiety
Each fibrinogen molecule has four N-glycans connected to the symmetrical BβAsn364 residues (located in the β-nodules) and γAsn52 (located in the coiled-coils), the latter carbohydrates not resolved crystallographically (Fig. 15.1). The presence and structural variations of the oligosaccharides affect fibrinogen’s solubility, life span in the blood stream, kinetics of fibrin polymerization, and clot structure.
Conversion of Fibrinogen to Fibrin
Formation of Monomeric Fibrin and A:a Knob-Hole Interactions
Fibrin formation is initiated by the thrombin-catalyzed release of two 16-residue-long peptides (FpA) from the N-termini of the Aα chains of fibrinogen to produce desA-fibrin monomer. The release of two 14-residue-long peptides (FpB) from the N-termini of the Bβ chains occurs at a much slower rate and is not necessary for fibrin polymerization. The critical importance of FpA release is supported by dysfibrinogenemias or genetic fibrinogen variants with impaired cleavage of FpA that precludes the enzymatic conversion of fibrinogen to fibrin (Galanakis et al. 1989).
The enzymatic cleavage of FpA in fibrinogen results in exposure of a new glycine(Gly)-proline(Pro)-arginine(Arg) motif. This tripeptide at the N-terminus of fibrin’s α chain is called knob ‘A’ to highlight that it fits into a complementary hole ‘a’ located in another monomeric fibrin, hence their binding is named the A:a knob-hole interaction (Fig. 15.2). The first evidence for the high affinity and structural compliance of knobs ‘A’ and holes ‘a’ was provided by X-ray crystallography of fibrinogen fragment D co-crystallized with the free peptide Gly-Pro-Arg-Pro that mimics the sequence of knob ‘A’. Because fragment D corresponds to the lateral D region, the binding pocket for the synthetic knob ‘A’ was identified as the hole ‘a’ located in the γ-nodule (Everse et al. 1998b; Kostelansky et al. 2002). If holes ‘a’ are blocked by synthetic Gly-Pro-Arg-Pro (Everse et al. 1998b) or compromised by a point mutation of the key residue γAsp364 (Okumura et al. 1997), fibrin polymerization is impossible. Overall, these and other data indicate that A:a knob-hole interactions, mainly electrostatic by nature, are the driving force of fibrin polymerization and blood clot formation.
Schematic diagram of fibrin polymerization. Fibrinopeptides in the central nodule cover knobs that are complementary to holes that are always exposed at the ends of the protein. When the fibrinopeptides are removed by thrombin, knob-hole interactions occur, giving rise to oligomers (a trimer is shown), which elongate to produce the two-stranded protofibrils made up of half-staggered molecules. The protofibrils aggregate laterally to make fibers, a process enhanced by interactions of the αC regions and formation of the αC-polymers. The fiber has a 22.5 nm periodicity as a result of half-staggering of 45 nm molecules. At the bottom of the diagram, branch points have been initiated by the divergence of two protofibrils (right) and splitting of each strand of a single protofibril (left) (Weisel and Litvinov 2017)—with permission from Springer Nature
The natural A:a knob-hole interactions between full-length fibrin(ogen) molecules have been reproduced and measured at the single-molecule level and these A:a complexes turned out to be strong and mechanically stable (Litvinov et al. 2005). Surprisingly, in response to increasing pulling force an unusual strengthening of A:a knob-hole bonds followed by their weakening was revealed, suggesting the existence of A:a complex in two distinct conformational states (Litvinov et al. 2018). The amino acid residues in holes ‘a’ binding to Gly-Pro-Arg-Pro are located within a segment γ290-379 and include γAsp364, γArg375, γHis340, γGln329, and γLys338 (Everse et al. 1998b). However, the interaction between fibrin monomers involves residues other than those comprising the “hot spots” in holes ‘a’ and knobs ‘A’. In particular, at the D:E:D interface residues αVal20-Lys29 (adjacent to the knob ‘A’ sequence αGly17-Arg19) interact with residues γAsp298-Phe304, γAsn319-Asn325, and γGln329 in the γ-nodule area next to hole ‘a’. There are also binary contacts between residues αLeu54, αGlu57, αPhe62, αArg65, γGln33, γAsp37, and γGln49 in the coiled coil and γGln329-Asp330 in the γ-nodule (Zhmurov et al. 2016). In other words, in the real monomer-monomer interactions there is an intermolecular interface beyond knobs ‘A’ and holes ‘a’ that can be considered more generally as binding sites ‘A’ and ‘a’.
Formation of Fibrin Protofibrils
As the first non-enzymatic step of fibrin polymerization, highly reactive desA-fibrin monomers (i.e. molecules with both FpA cleaved off) self-assemble in a half-staggered manner so that two knobs ‘A’ located in the central E region of one elongated molecule fit into two holes ‘a’ located in the D regions of two rod-like monomers connected end-to-end (Erickson and Fowler 1983). This primary polymerization step leads to formation of a two-stranded trimer, in which the lateral D regions of two linearly arranged molecules form the D:D interface and both get tethered via knobs ‘A’ to the E region of the third monomer in the other strand. Therefore, a triple D-E-D complex comprises the junction between three monomers in two strands held together mainly by the A:a knob-hole bonds (Fig. 15.3) (Everse et al. 1998a). The D:D interface is formed by residues γ275-309 (Everse et al. 1998b) of which residues γ275, γ308, and γ309 are essential for addition of new monomers to each strand to form a longer linear fibrin oligomer (Marchi et al. 2006; Bowley et al. 2009). The D:D interfacial contacts form a hinge, which is localized to residues γAla279-Tyr280 in one D region and residues γAsn308-Gly309 in the other. This hinge allows bending at the D-D interface by ~ 60° or more (Zhmurov et al. 2016). Importantly, point mutations in the residues γAla279, γTyr280, γAsn308, and γGly309, which stabilize the D-D interactions, are implicated in a number of dysfibrinogenemias with impaired fibrin formation (Hanss and Biot 2001). The oligomeric strands grow longitudinally until they reach a length of a double-stranded protofibril (Fig. 15.2), a soluble intermediate product of fibrin polymerization, comprising a straight twisted filament about 0.5–0.6 µm in length made of about 20–25 monomers (Erickson and Fowler 1983; Chernysh et al. 2011). The persistence length of a protofibril is about 320 nm with a high propensity for bending and kinking (Zhmurov et al. 2018). What makes protofibrils critically important in fibrin polymerization is that they reach a threshold length to undergo lateral aggregation and thus form thicker fibrin fibers. An unusual mechanism for the early steps of fibrin polymerization has been proposed that implies formation of single-bonded ‘Y-ladder’ polymers that grow linearly before undergoing a transition to the double-stranded protofibrils (Rocco et al. 2014).

Modified from (Zhmurov et al. 2018)—published with permission from Elsevier
Structure of a double-stranded fibrin oligomer composed of five monomers stabilized mainly by the A:a knob-hole interactions that form the D-E-D complex
Formation of Fibrin Fibers
Fibrin fibers are formed as a result of two simultaneous and competing processes: further linear elongation of protofibrils and their lateral (or radial) aggregation that determine the variability of the fiber mass/length ratio. Depending on the conditions of fibrin formation, the number of protofibrils per fiber cross-section can vary from about two to several thousand (Missori et al. 2010; Yeromonahos et al. 2010). During regular side-to-side bundling, protofibrils form fibers with the axial periodicity of ~ 22.5 nm (½ of the length of a fibrin monomer), originating from the precise half-staggered molecular packing (Fig. 15.2). This localized protein densification at the transversely aligned globular D-E-D complexes is visualized as periodic cross-striation of fibrin fibers with transmission electron microscopy and atomic force microscopy (Fig. 15.4) (Weisel 1986; Yermolenko et al. 2011; Zhmurov et al. 2018). The molecular arrangement within a fibrin fiber is highly regular in the longitudinal direction, while lateral packing is less ordered (Torbet et al. 1981; Weisel et al. 1983; Weisel 1986; Caracciolo et al. 2003; Yeromonahos et al. 2010; Jansen et al. 2020).
Cross-striation of a fibrin fiber with a 22.5 nm periodicity visualized using atomic force microscopy (Yermolenko et al. 2011)—with permission from ACS Publications
The estimated spatial density of protofibrils varies depending on conditions of fibrin formation and methods applied (Yeromonahos et al. 2010). For example, increased thrombin concentration has been demonstrated to lead to decreased fiber radius and a markedly lower average protofibril content per fiber. This resulted in the formation of less compact, less dense fibrin structures, with distances between protofibrils within the fiber being larger at higher thrombin concentrations (Domingues et al. 2016). In addition, a common fibrinogen splice variant, named γ’ fibrinogen, which results from an alternative polyadenylation signal in intron 9, resulting in a γ-chain with a 16-amino-acid C-terminal extension, has also been shown to alter protofibril packing (Domingues et al. 2016). In plasma, γ’ fibrinogen mainly circulates as a heterodimer with the more common γA-chain (γA/γ’) (Wolfenstein-Todel and Mosesson 1981), with an average plasma concentration of 8–15% (Mosesson et al. 1972; Chung and Davie 1984). Domingues et al. (2016) demonstrated a reduction in protofibril packing for fibers produced using γA/γ’ compared to γA/γA fibrinogen, across a range of thrombin concentrations. The γ’ chain itself seems to influence polymerization, with specifically lateral aggregation of protofibrils being slowed down and the formation of non-uniform clots consisting of thin fibers (Gersh et al. 2009b; Allan et al. 2012). Protofibril packing is decreased in fibers containing γ’ fibrinogen, with protofibrils being packed loosely and fibers unraveling into loose fibrils with diameters of less than 10 nm, consistent with the diameter of individual protofibrils (Domingues et al. 2016). Fibers with reduced protofibril packing either due to increased thrombin concentration or the presence of γ’ fibrinogen are less stiff than more dense fibers, leading to a weakened clot architecture (Domingues et al. 2016) (Fig. 15.5). The importance and structural basis of clot mechanical properties are discussed in the next section.
Alternatively spliced γ’ fibrin(ogen) alters protofibril packing and clot structure (Pieters and Wolberg 2019)
Based on indirect evidence, it has furthermore been proposed that the lateral packing of fibrin fibers is non-uniform and that they have a dense, relatively compact core and sparse, loosely arranged protofibrils at the periphery (Li et al. 2017). Irrespective of the extent of lateral order and uniformity of protofibril packing, the protein density within fibrin fibers was estimated to be around 20–30% (Yeromonahos et al. 2010), indicating that fibers have large inter-protofibril spaces filled with liquid. Additionally, using small-angle X-ray scattering, the spatial density of protofibrils has been recently estimated to have a typical repeat distance of ~ 13 nm, independent of the fiber thickness or the number of protofibrils per fiber cross-section (Jansen et al. 2020).
Each protofibril is twisted; therefore, fibrin fibers formed during lateral aggregation of the axially oriented protofibrils are also twisted (Medved et al. 1990) with a 20-60 nm helical radius and ~ 2000 nm helical pitch (Weisel et al. 1978). New protofibrils that are added to the surface of a fiber must be stretched as their path length increases with fiber thickness. The twisting deformation of protofibrils provides a thermodynamic mechanism to limit the thickness of fibrin fibers, as they stop growing laterally when the energy necessary to stretch an added protofibril is equal to or exceeds the energy of attachment.
The particular binding sites mediating the lateral aggregation of protofibrils are unknown, but a number of structures have been indirectly shown or assumed to mediate the associations of protofibrils, namely the αC regions, B:b knob-hole complexes, the C-terminal portions of the γ chains and two adjacent β-nodules (Yang et al. 2000), the coiled-coil connectors (Okumura et al. 2006), and carbohydrate moieties (Langer et al. 1988). There are conceivable structural models for the lateral aggregation of protofibrils based on the interactions between two β-nodules of adjoining protofibrils via residues β330-375 (Yang et al. 2000) and on the involvement of the N-terminal part of the β chain, namely residues βAla68 (Mullin et al. 2000) and βGly15, the end residue of knob ‘B’, irrespective of whether FpB is cleaved or not (Hirota-Kawadobora et al. 2003). Based on the structural models of the compact part of the fibrinogen α chain and the N- termini of the β chain, their involvement in lateral aggregation of protofibrils was suggested by formation of intricate lattices together with the γ-chain (Klykov et al. 2020). In addition, detailed structural analysis of dysfibrinogenemias with impaired clot formation has revealed a crucial role for the βArg166 residue in lateral aggregation (Klykov et al. 2020).
Additional Molecular Interactions During Fibrin Polymerization
Besides the essential A:a and D:D associations, there are a number of intermolecular interactions that are not necessary for fibrin polymerization but they can modify the ultimate structure and properties of fibrin, such as B:b knob-hole interactions, homomeric oligomerization of the αC regions, and covalent crosslinking catalyzed by the plasma transglutaminase, factor XIIIa.
The thrombin-catalyzed release of FpB from the N-termini of β-chains exposes a new Gly-His-Arg-Pro motif, which is called knob ‘B’ that fits into hole ‘b’ located in the β-nodule, a part of the globular D region. The B:b interactions were reproduced and measured in vitro (Litvinov et al. 2006) but the physiological role of the B:b interactions remains uncertain. In the absence of knobs ‘B’, when thrombin cleaves off FpA from fibrinogen while release of FpB is prevented, fibrin has thinner fibers than those formed after cleavage of both fibrinopeptides, suggesting that B:b interactions contribute to lateral aggregation of protofibrils (Blombäck et al. 1978). The B:b interactions in fibrin are real because some homodimeric dysfibrinogenemias (fibrinogen variants Metz and Frankfurt XIII) from which only FpB can be cleaved (no FpA release), produce fibrin clots at low temperature exclusively via B:b bonding (Galanakis et al. 1993; Galanakis 1993). Accordingly, replacement of the γAsp364 residue in fibrinogen, making holes ‘a’ dysfunctional and preventing formation of A:a complexes, still allows fibrin clots to form slowly under the action of thrombin (Okumura et al. 2007), again confirming existance of B:b interactions in the absence of A:a bonding. Notably, holes ‘b’ can interact with knobs ‘B’ both within and between protofibrils, but, due to steric constraints, the intra-protofibril B:b contacts are less probable than the inter-protofibril B:b contacts, which explains why the B:b interactions are not necessary for initiation of fibrin polymerization and why they modulate the lateral aggregation of protofibrils (Zhmurov et al. 2018). In addition to their potential role in lateral aggregation of protofibrils, B:b interactions change the susceptibility of fibrin to enzymatic proteolysis (Doolittle and Pandi 2006). The functional importance of B:b knob-hole interactions was confirmed indirectly by formation of fibrin with distinct structure and properties in the presence of a knob ‘B’ mimetic peptide (Gly-His-Arg-Pro) conjugated with polyethyleneglycol (Brown et al. 2015).
The extended and flexible αC regions of fibrin(ogen) molecules can self-interact within and between protofibrils, resulting in formation of αC polymers (Fig. 15.2) (Tsurupa et al. 2011; Protopopova et al. 2017). Similar to B:b knob-hole interactions, the αC regions promote lateral aggregation while being not essential (Weisel and Medved 2001; Tsurupa et al. 2011). Fibrin formed from des-αC-fibrinogen or fibrinogen with short αC regions has thinner fibers with more branch points than fibrin formed from the full-length fibrinogen, suggesting impaired lateral aggregation of protofibrils in the absence of long enough αC regions (Collet et al. 2005; Ping et al. 2011). However, in the absence of functional knobs ‘A’ and ‘B’ and therefore without A:a and B:b knob-hole interactions the αC-regions’ interactions appear too weak and unstable to mediate association of fibrin(ogen) molecules (Duval et al. 2020).
During and after polymerization, fibrin is covalently crosslinked by factor XIIIa, an active transglutaminase formed from inactive factor XIII by thrombin in the presence of Ca2+. The first sites to be crosslinked are located in the unstructured C-terminal tails of γ chains approximated due to D-D contacts between two linearly adjacent fibrin monomers within the same strand (Fig. 15.6). Factor XIIIa catalyzes formation of an intermolecular ε-(γ-glutamyl)-lysyl isopeptide bond between the γLys406 of one γ chain and γGln398/399 of another γ chain. Factor XIIIa forms the same type of bonds at a slower rate between lysine and glutamine residues in the αC regions associated into αC polymers within protofibrils and in the inter-protofibril space (Matsuka et al. 1996). The fibrin α and γ chains also can be crosslinked, resulting in formation of α-γ-heterodimers (Standeven et al. 2007). The covalent stabilization makes fibrin polymerization irreversible and the crosslinked fibrin clot becomes mechanically stiff and more resistant to fibrinolysis.
Formation of isopeptide bond catalyzed by factor XIIIa. The chemical reaction catalyzed by Factor XIIIa, yielding insoluble fibrin crosslinked by ε-(γ-glutamyl)-lysine bonds between the γ chains and the αC regions (Pieters and Wolberg 2019)
Formation of a Fibrin Network
As fibrin fibers thicken due to lateral aggregation of protofibrils and grow in length due to longitudinal addition of new monomers or oligomers, they also branch, which is necessary to yield a three-dimensional network (Fig. 15.2). There are at least two types of branching points formed by distinct mechanisms that may both contribute to fibrin network structure. The one called a “bilateral junction” appears when two protofibrils bundle to form a four-stranded filament and then diverge again into two separate protofibrils (Mosesson et al. 1993). The second type of branching is called a “trimolecular junction” or “equilateral junction” because it arises when a fibrin monomer binds at the end of a protofibril via only one γ-nodule, such that this partial bimolecular complex can initiate formation of a new two-stranded protofibril (Fogelson and Keener 2010). Irrespective of the mechanism, most branch points in fibrin networks consist of three fibers of about the same diameter joined together (Ryan et al. 1999). Generally, there is an inverse relation between the number of branch points in a clot and the fiber diameters (Ryan et al. 1999). In other words, in fibrin clots with thick fibers there are few branch points, while clots made up of thin fibers have many branch points. Because branching occurs during elongation of protofibrils, while fiber diameter is determined by the lateral aggregation, it can be inferred that branching and lateral aggregation compete. Alternative to the commonly accepted three-dimensional fibrin network structure, one not universally recognized, but experiment-based model of fibrin polymerization includes formation of ultrathin fibrin sheets (O’Brien et al. 2008).
As a result of combined elongation, branching, and thickening of fibrin fibers, a space-filling network is formed that macroscopically represents an insoluble hydrogel. The time point at which the gel is formed is named the clotting time of blood or plasma and used in laboratory assays as a quantitative parameter to reveal coagulation disorders, often associated with prolonged or accelerated clotting time. The gelation point corresponds to the state of clotting when only about 15–20% of soluble fibrinogen has been incorporated into the insoluble gel, implying that the fibrin network is not yet established at the time of gelation, with new fibers and branch points still being formed after the gelation point (Chernysh and Weisel 2008). The structure of ultimate fibrin clots is quantified using scanning electron microscopy, confocal microcopy, and optical spectroscopy by the mass/length ratio, diameters, and spatial density of fibers, number of branch points and distances between them (fiber length), as well as the size of the pores. All of these parameters are strongly affected by variations in the kinetics of polymerization determined by thrombin and factor XIIIa activity, the quality and quantity of fibrinogen, the presence of blood cells as well as numerous environmental factors. It is noteworthy that in vitro fibrin networks formed in static conditions at physiological fibrinogen concentrations are very porous since the mass fraction of fibrin is about 0.3%, corresponding to the normal fibrinogen level in plasma. By contrast, when a clot in formed in dynamic conditions of blood flow, the composition and structure of thrombi and thrombotic emboli, including the mass fraction and structural diversity of fibrin, are dramatically different (Chernysh et al. 2020).
Mechanical Properties of Clots
Significance of Clot Mechanical Properties
Although the mechanical properties of clots are often ignored, they are among the most important functional characteristics (Weisel 2004). In hemostasis, clots must form a seal to stem bleeding, including the force of arterial blood flow. In thrombosis, the mechanical properties of clots determine the fate of thrombi. The pressure of flowing blood can dislodge or deform a thrombus or cause it to rupture, a process called embolization, which is responsible for pulmonary embolism and some forms of ischemic stroke. Furthermore, there is now strong evidence for a correlation between clot stiffness and many (pro) thrombotic conditions (Collet et al. 2006).
Basis of Clot Mechanical Properties
Fibrin is the scaffold of clots and thrombi that is largely responsible for their mechanical properties. It forms a network that is space-spanning to support forces applied to a clot. While some proteins, like collagen or actin form fibers or filaments, they do not form a gel without the binding of other proteins. Other proteins, such as elastin and gelatin, make networks without forming fibers. Fibrin fibers form networks because the fibers branch, such that fibers diverge from each other, usually with three fibers joining at each branch point. In fact, branching is such a dominant feature of fibrin clots that fiber ends are rarely seen in clots made from normal fibrinogen (Weisel 2004).
Clots that include platelets, such as clots made from recalcified platelet-rich plasma, have a different architecture to clots from platelet-poor plasma. Since most of the thrombin is generated on the surface of the platelets, that is where fibrinogen is converted to fibrin, and hence many fibers originate from platelet aggregates, radiating like the spines of a starfish (Collet et al. 2002). Clots made from whole blood include red blood cells, which occupy a considerable volume of the clot and increase the pore size of the fibrin mesh (Gersh et al. 2009a). Clots formed in vivo can have a quite different architecture, because of the spatial initiation of clotting and because of blood flow (Fig. 15.7). Thrombi are also quite different than either in vitro clots or in vivo clots, since they are usually formed intravascularly as a result of pathological processes. However, although all these conditions have distinctive effects on clot or thrombus properties, fibrin is the structural and mechanical basis of all of them (Liang et al. 2017).
Viscoelastic Properties of Fibrin
Fibrin is called a viscoelastic polymer because it has both elastic properties, which means that strain or deformation is proportional to stress or force per area, and viscous properties, which means that stress is proportional to the rate of strain. Elastic properties, stiffness or elastic modulus or storage modulus, characterize the reversible deformation by force, while the viscous properties, plasticity or loss modulus, characterize the irreversible or inelastic properties (Weisel 2004).
Commonly, rheometers are used to measure the viscoelastic properties of fibrin. Usually shear rheometers, which impose a shear stress or shear strain on a clot, are employed, but some rheometers can also be used for compression, or others for tensile testing, or stretching. In addition, there are specialized devices in the clotting field that are not rheometers but measure clot stiffness over time and yield parameters that are used by clinicians to evaluate the formation of clots from plasma or whole blood (Luddington 2005; Ganter and Hofer 2008; Bolliger et al. 2012). These results of thromboelastography or thromboelastometry, which are more global ways to measure clot firmness, are used to diagnose patients with bleeding or thrombotic disorders.
For fibrin clots, the elastic component is generally about an order of magnitude greater than the viscous component, although the viscous component increases rapidly with frequency. Stiffness is greater for clots made from the plasma of patients with thrombotic conditions (Collet et al. 2006), while it is less for patients with hemophilia A (Leong et al. 2017).
Non-linear Elasticity and High Extensibility of Fibrin
Stress-strain curves, with applied stress plotted against the strain or induced deformation, obtained using a rheometer can be used for characterizing the elasticity of clots. The slope of the stress-strain curve is the stiffness of the clot. Fibrin exhibits strain stiffening or strain hardening, which means that the slope of the curve becomes greater with increasing strain (Storm et al. 2005; Janmey et al. 1983).
Since fibrin is highly extensible, clots will tend to stretch rather than break. Fibrin in a plasma clot that is crosslinked with Factor XIIIa can be stretched about threefold before rupture (Brown et al. 2009). Fracture resistance of fibrin has not been much studied, but it depends strongly on the red blood cell content, which may be significant in vivo for embolization (Riha et al. 1999). Remarkably, the strain stiffening and extensibility of fibrin clots is also observed in stretching of individual fibrin fibers (Liu et al. 2006; Guthold et al. 2007; Liu et al. 2010). The elastic modulus of individual fibrin fibers is strongly dependent on the fiber diameter, indicating that the packing of the protofibrils is different in thick and thin fibers, as discussed above (Li et al. 2016). The strain stiffening in individual fibers allows the strain load to be distributed more evenly over the network of fibers, from the highly strained and hence stiffer fibers to less strained fibers (Hudson et al. 2010).
The non-linear elasticity of clots has also been observed in compression. Initially, fibrin clots decrease in stiffness with compression, as fibers perpendicular to the direction of compression bend and buckle (Kim et al. 2014). With further increasing compression, there is a striking non-linear increase in clot stiffness, as fibers parallel to the direction of compression encounter each other with an increase in network density from criss-crossing fibers.
The physiological significance of fibrin stiffening likely arises because clots will deform in response to forces, but then be protected from damage when they become stiffer at higher forces. Furthermore, mechanical stress and the resulting deformation of clots make them more resistant to fibrinolysis, which may be one reason for lesser efficacy of thrombolytic treatments of thrombi in some conditions. Moreover, the combination of histone-DNA complexes mimicking neutrophil extracellular traps, and fibrin makes those clots stiffer and more resistant to fibrinolysis (Longstaff et al. 2013).
Multiscale Fibrin Mechanics
The mechanical properties of clots can only be understood by consideration of their structure at a wide range of spatial scales, including macroscopic, fiber network, individual fiber, and molecular levels (Fig. 15.8). At the macroscopic scale, fibrin’s strain stiffening and high extensibility have already been discussed. In addition, clots display a large decrease in volume with both stretching and compression, which is due to water expulsion and network densification (Brown et al. 2009). One reason for this phenomenon may be negative normal stress, because fibers buckle more easily than they stretch (Kang et al. 2009). However, a more significant explanation is likely due to a molecular structural transition that will be discussed further below.
The diagram shows the structural changes that occur upon stretching the cylindrical fibrin clot at different spatial scales, including macroscopic volume shrinkage, network rearrangement, and protein unfolding (Purohit et al. 2011)—with permission from Elsevier
At the network level, plasma clots have a strikingly porous structure with a mass fraction of protein of only about 0.25%. In addition, the structure of these clots is highly dependent on the conditions of polymerization. High thrombin concentrations make clots with thin fibers and many branch points that are stiffer than clots at lower thrombin levels, while at low ionic strength or high calcium ion concentration or high pH, clots have thicker fibers and fewer branch points and are softer (Weisel and Litvinov 2013; Weisel and Litvinov 2017). All of these clots are initially made up of a branching isotropic network, with no preferred orientation of fibers. With stretching, the fibers align along the direction of strain. In addition, the fibers become thinner and self-associate. With compression, the fibers become oriented in the direction perpendicular to the direction of compression and become shorter because of criss-crossing (Kim et al. 2014). As a result, the shear modulus or stiffness of the clot in response to shear strain, increases dramatically, since the fibers are now oriented and more highly branched.
At the fiber level during stretching, fibers are increasingly under large strains after they become oriented. Fibers under compression bend and buckle in the direction of applied stress. As more fibers buckle, there are fewer fibers to sustain loads, so the stiffness decreases.
In recent years, there have been a plethora of studies of clot mechanics at the molecular level to such an extent that a description of these results deserves its own section, which follows.
Molecular Structural Basis of Fibrin Mechanics
With stretching of clots, after the initial reorientation and alignment of fibers along the direction of applied force, there must be changes in the molecular structure of fibrin. There are three major candidates for such molecular changes: unfolding of the γC regions, unfolding of the α-helical coiled coil, stretching of the mostly unstructured connector of the αC region. There is still disagreement on the roles that each of these structural changes play, but it now seems likely that all occur to at least some extent. From the crystal structure of fibrinogen and taking into account the disulfide bonds that restrict the extent of stretching, it can be predicted that hypothetically the full unfolding of the molecule would result in a 4.7-fold elongation (Zhmurov et al. 2011).
Small angle X-ray scattering (SAXS) patterns of fibrin are characterized by a periodicity of 22.5 nm, because of the half-staggering of 45 nm molecules. It was expected that stretching of clots would result in an increase of this periodicity. Although some early studies appeared to show such an increase, it now seems clear that there is little if any increase in periodicity (Brown et al. 2009). However, there is a broadening of the 22.5 nm peak, indicating that there is an increase in disorder of the packing. These results are consistent with stochastic unfolding of an increasing number of molecules with strain. This behavior was replicated with a two-state model in which some molecules randomly extend and unfold while others remain folded (Brown et al. 2009).
Single molecule force spectroscopy, particularly using atomic force microscopy, has been used to study protein unfolding and characterize unfolding transitions through analysis of force-distance curves. However, it is nearly impossible to interpret the results from such experiments with fibrinogen molecules or naturally occurring fibrin polymers, because these structures are quite complex and many different unfolding events are possible. As a partial solution, tandems or single-stranded fibrinogen oligomers were prepared by cross-linking of fibrinogen end-to-end with Factor XIIIa (Zhmurov et al. 2011). An additional part of the solution to understanding the experimental results has been to combine them with Molecular Dynamics simulations and modeling of the unfolding transitions from the known X-ray crystallographic structures. With this dual approach, it was discovered that there is unfolding of the C-terminal γC nodules, accompanied by reversible extension and refolding of coiled-coil connectors, which act as springs to take up the slack from unfolding of globular regions (Zhmurov et al. 2011).
Since fibrinogen is a fibrous protein with two relatively long axially aligned α-helical coiled-coils, they are an obvious candidate for unfolding, especially since it has been demonstrated that other fibrous proteins, such as keratin can unfold with applied force. The α-helical coiled-coils in fibrin undergo a transition from α-helix to β-sheet with either stretching or compression (Fig. 15.9) (Litvinov et al. 2012).
Force-induced mechanical transition of α-helices (red) into β-sheets (blue) in the fibrin(ogen) triple-helical coiled-coils (Weisel and Litvinov 2017)—with permission from Springer Nature
There is considerable evidence for the contribution of the αC regions to clot mechanical properties. Factor XIIIa crosslinking of the αC regions makes clots much stiffer and decreases their plasticity (Collet et al. 2005). Studies of fibrinogens from different species with different lengths indicates that the contribution of this part of the molecule is important (Falvo et al. 2008). In addition, there is evidence that the fast elastic recoil of fibrin fibers may arise from the αC regions (Hudson et al. 2013). Study of changes in the SAXS pattern of fibrin with shear strain also show little change in periodicity. From analysis of the forces applied to fibrin molecules and the measured unfolding response of fibrin to forces, it has been proposed that in these experiments there was no unfolding of domains, but instead stretching of the unstructured part of the αC region (Vos et al. 2020).
Modeling Fibrin Mechanical Properties
Models of the mechanical properties of filamentous networks are one way to take experimental data and use it to understand and predict fibrin mechanics. One such model uses a system of connected fibers with known force-extension curves. Although the fibrin network is not modeled explicitly in terms of its known structure, this model captures the stress-strain relationship of fibrin clots, using the measured force-extension curves for individual fibers (Brown et al. 2009). In this model, the fibrin molecules are considered to be a two-state system that can either be folded, where it’s modeled as a linear spring, or unfolded, where it’s a worm-like chain. This model fits the experimental data very well, if the observed decrease in volume is incorporated into the model.
Another model assumes that fibrin fibers are semiflexible and are subject to thermal fluctuations that are reduced in response to stretching (Storm et al. 2005). This model can also be used to predict clot mechanical properties, starting with known force-extension curves for individual fibers. Several models utilize the concept of wormlike semiflexible polymers, some of which do not include the idea of fibrin unfolding, which may depend on the type and degree of deformation (Piechocka et al. 2010). Other models only described the mechanical properties of individual fibers and do not attempt to model the clot network. Models of compression and shear often differ from those for extension. With both compression and tension, criss-crossing of fibers and strong interactions between them are an important part of the models (Kim et al. 2014; Britton et al. 2019). Some models for compression of fibrin clots use the theory of foams or cellular solids (Kim et al. 2016). Other models have considered non-affine deformations that occur in certain types of clots, depending on the conditions of formation (Kang et al. 2009). Finally, an additional level of complexity is the consideration of cyclic loading, which is more complex because irreversible changes occur (Liang et al. 2017).
Clot Properties and Disease
The primary function of fibrin clot formation, is to prevent unwanted blood loss by forming, together with platelet adhesion and aggregation and other blood cells, a stable plug at the site of vascular injury. The structural and mechanical fibrin clot properties described above are critical for successful hemostasis. Alteration in these properties can consequently result in pathological vascular coagulation, such as thrombosis or alternatively, bleeding. The consistent findings of altered clot properties in both venous and arterial thrombotic conditions provide a plausible mechanistic link between clot structure and thrombosis, although causality remains to be confirmed. In keeping with the Mendelian randomization approach, there is some evidence linking a number of fibrinogen variants that alter fibrin clot properties to cardiovascular diseases. In addition, recent reports providing evidence that altered clot properties predict the development of cardiovascular complications and even malignancy, may provide support for its potential causal role in disease.
Fibrin Clot Properties and Pathological Intravascular Coagulation
Clots with densely-packed, thin fibers, with a stiffer network arrangement, reduced permeability (smaller pore sizes) and enhanced resistance to fibrinolysis have consistently been found in a variety of cardiovascular and other diseases (Fig. 15.10). Examples are:
-
Arterial thrombosis: ischemic stroke (Undas et al. 2010; Undas and Ariens 2011; Bridge et al. 2014), coronary artery disease (Mills et al. 2002; Collet et al. 2006; Undas and Ariens 2011; Bridge et al. 2014; Undas 2016), peripheral arterial disease (Undas and Ariens 2011; Litvinov and Weisel 2016; Undas 2016), acute coronary syndrome (Undas et al. 2008; Undas 2016), no-reflow phenomena after acute MI (Undas 2016), and in-stent thrombosis (Undas 2016; Kattula et al. 2017).
-
Venous thrombosis and thromboembolism: deep vein thrombosis, pulmonary embolism (Bridge et al. 2014), and cerebral venous sinus thrombosis (Undas 2016). Differences in clot properties between deep vein thrombosis patients not developing thromboembolism and those who do, suggest a potential role for clot properties in embolism risk (Bridge et al. 2014).
-
Chronic inflammatory diseases: inflammatory bowel disease (Undas 2016), antiphospholipid syndrome (Undas 2016), rheumatoid arthritis (Undas and Ariens 2011; Ariens 2013), chronic obstructive pulmonary disease (Undas and Ariens 2011; Ariens 2013), and systemic lupus erythematosus (Litvinov et al. 2019). Fibrin plays an important role in innate immunity and can contribute to inflammation by recruiting inflammatory cells and enhancing leukocyte reactivity by binding to the Mac-1 integrin (Trezzini et al. 1988; Altieri et al. 1990; Flick et al. 2004).
-
Other: chronic heart failure with sinus rhythm (Palka et al. 2010), atrial fibrillation (Undas 2016), arterial hypertension (Undas 2016), aortic aneurysm (Ariens 2013; Bridge et al. 2014), disseminated intravascular coagulation (Litvinov and Weisel 2016), diabetes mellitus (Bridge et al. 2014; Undas 2016), end stage renal disease (Ariens 2013; Undas 2016), cancer (Undas 2016), and liver diseases such as cirrhosis (Hugenholtz et al. 2016), in part due to intrinsic changes in the fibrinogen molecule such as post-translational modifications (Lisman and Ariens 2016; De Vries et al. 2020).
-
Atherosclerosis – fibrin deposits in plaque contribute to plaque growth and (in) stability (Lepedda et al. 2009; Borissoff et al. 2011; Ariens 2013).
In addition, a number of fibrinogen variants resulting in altered clot properties have been linked to cardiovascular disease. The most common of these is γ’ fibrinogen. Fibrinogen γ’ forms clots with larger pores, decreased protofibril packing within fibers, less stiff fibers, and with a heterogeneous clot structure resistant to lysis (Fig. 15.5) (Allan et al. 2012; Domingues et al. 2016). Although still inconclusive, current evidence suggest that increased levels of γ’ fibrinogen are associated with arterial thrombosis and decreased levels with venous thrombosis (Macrae et al. 2016). Other fibrinogen variants resulting in altered fibrin structure and/or function with demonstrated association with disease include fibrinogen AαThr312Ala (atrial fibrillation and venous thromboembolism), BβArg448Lys (coronary artery disease severity and stroke) and Bβ-455G/A (ischemic stroke and coronary artery disease) as well as the Factor XIIIA Val34Leu polymorphism (myocardial infarction and deep vein thrombosis) (Scott et al. 2004; Bridge et al. 2014; Chen et al. 2014). Clinically, congenital fibrinogen disorders are classified as quantitative (affecting fibrinogen concentration) or qualitative (affecting fibrinogen functionality) or a combination of both and can be asymptomatic or have a thrombotic or bleeding phenotype. For a detailed description of the clinical diagnosis and classification of congenital fibrinogen disorders please refer to Casini et al. (2018).
Recent prospective evidence of fibrin clot properties predicting disease severity and outcome provides compelling evidence that fibrin clot properties are not only associated with disease but likely play a causative role. Sumaya et al. (2018) found in a cohort of 4,345 acute coronary syndrome patients that in vitro plasma clots that were resistant to lysis, independently predicted death after adjusting for known cardiovascular risk factors at one-year follow-up. A study on 320 first-event deep vein thrombosis patients, found that reduced clot permeability (Ks) and prolonged clot lysis times independently predicted recurrent deep vein thrombosis at 44-month follow-up (Cieslik et al. 2018). Also in antiphospholipid syndrome patients (n = 126), denser fibrin networks independently predicted recurrent thromboembolic events in multivariate analysis (Celinska-Lowenhoff et al. 2018). Furthermore, in 369 unprovoked venous thromboembolism patients, those with the above-mentioned prothrombotic clot phenotype had an increased risk of cancer development within three years of follow-up (Mrozinska et al. 2019).
Also in the clinical setting, the diagnostic use of fibrin clot properties in the management of perioperative bleeding has gained traction. Standard coagulation tests that estimate coagulation factor activity such as prothrombin and partial thromboplastin times have been supplemented with methods such as thromboelastography or thromboelastometry, which measure clot formation kinetics and mechanical properties, as mentioned above (White 2018).
Fibrin Clot Properties and Bleeding
Conversely, fibrin clot structure has also been associated with bleeding. As opposed to the more prothrombotic clot phenotype described above, fibrin clots associated with bleeding are typically weaker and generally contain looser and less rigid networks of thicker fibers that are more susceptible to fibrinolysis. Bleeding resulting from a number of congenital dysfibrinogenemias and hemophilia, amongst others, have been ascribed to these clot properties (He et al. 2003; Wolberg et al. 2005; Leong et al. 2017; Casini et al. 2018). For example, the fibrin clot properties described above, have been demonstrated to distinguish severe FXI deficient patients as “bleeders” or “non-bleeders” (Zucker et al. 2014). Similarly, in hemophilia A and C, differences in fibrin clot structure are also used to assess clinical outcomes such as bleeding (Cawthern et al. 1998).
Summary
The molecular structure of fibrinogen has largely been resolved using crystallography and modeling/computation. Although certain aspects pertaining to lateral aggregation and clot growth remain to be elucidated, extensive research into fibrin polymerization has significantly enhanced our understanding of the fundamental mechanisms of clot formation and dissolution. This knowledge, together with the identification of the structural origins of the mechanical properties of fibrin has proved to be useful in various diseases with thrombotic or bleeding complications. It currently forms the basis of a number of diagnostic tools pertaining to thrombosis and/or bleeding risk and also provides a novel therapeutic target as a means to modulate blood clotting in clinical medicine. In short, fibrin is a remarkable and versatile biomaterial with a plethora of potential biological uses.
References
Allan P, Uitte de Willige S, Abou-Saleh RH, Connell SD, Ariens RA (2012) Evidence that fibrinogen gamma’ directly interferes with protofibril growth: implications for fibrin structure and clot stiffness. J Thromb Haemost 10(6):1072–1080. https://doi.org/10.1111/j.1538-7836.2012.04717.x
Altieri DC, Agbanyo FR, Plescia J, Ginsberg MH, Edgington TS, Plow EF (1990) A unique recognition site mediates the interaction of fibrinogen with the leukocyte integrin Mac-1 (CD11b/CD18). J Biol Chem 265(21):12119–12122
Ariens RA (2013) Fibrin(ogen) and thrombotic disease. J Thromb Haemost 11(Suppl 1):294–305. https://doi.org/10.1111/jth.12229
Blombäck B, Hessel B, Hogg D, Therkildsen L (1978) A two-step fibrinogen–fibrin transition in blood coagulation. Nature 275(5680):501–505. https://doi.org/10.1038/275501a0
Bolliger D, Seeberger MD, Tanaka KA (2012) Principles and practice of thromboelastography in clinical coagulation management and transfusion practice. Transfus Med Rev 26(1):1–13. https://doi.org/10.1016/j.tmrv.2011.07.005
Borissoff JI, Spronk HM, ten Cate H (2011) The hemostatic system as a modulator of atherosclerosis. N Engl J Med 364(18):1746–1760. https://doi.org/10.1056/NEJMra1011670
Bowley SR, Okumura N, Lord ST (2009) Impaired protofibril formation in fibrinogen gamma N308K is due to altered D: D and “A:a” interactions. Biochemistry 48(36):8656–8663. https://doi.org/10.1021/bi900239b
Bridge KI, Philippou H, Ariens R (2014) Clot properties and cardiovascular disease. Thromb Haemost 112(5):901–908. https://doi.org/10.1160/th14-02-0184
Britton S, Kim O, Pancaldi F, Xu Z, Litvinov RI, Weisel JW, Alber M (2019) Contribution of nascent cohesive fiber-fiber interactions to the non-linear elasticity of fibrin networks under tensile load. Acta Biomater 94:514–523. https://doi.org/10.1016/j.actbio.2019.05.068
Brown JH, Volkmann N, Jun G, Henschen-Edman AH, Cohen C (2000) The crystal structure of modified bovine fibrinogen. Proc Natl Acad Sci USA 97(1):85–90. https://doi.org/10.1073/pnas.97.1.85
Brown AE, Litvinov RI, Discher DE, Purohit PK, Weisel JW (2009) Multiscale mechanics of fibrin polymer: gel stretching with protein unfolding and loss of water. Science 325(5941):741–744. https://doi.org/10.1126/science.1172484
Brown AC, Baker SR, Douglas AM, Keating M, Alvarez-Elizondo MB, Botvinick EL, Guthold M, Barker TH (2015) Molecular interference of fibrin’s divalent polymerization mechanism enables modulation of multiscale material properties. Biomaterials 49:27–36. https://doi.org/10.1016/j.biomaterials.2015.01.010
Caracciolo G, De Spirito M, Castellano AC, Pozzi D, Amiconi G, De Pascalis A, Caminiti R, Arcovito G (2003) Protofibrils within fibrin fibres are packed together in a regular array. Thromb Haemost 89(4):632–636
Casini A, Undas A, Palla R, Thachil J, de Moerloose P (2018) Diagnosis and classification of congenital fibrinogen disorders: communication from the SSC of the ISTH. J Thromb Haemost 16(9):1887–1890. https://doi.org/10.1111/jth.14216
Cawthern KM, van ‘t Veer C, Lock JB, DiLorenzo ME, Branda RF, Mann KG (1998) Blood coagulation in hemophilia A and hemophilia C. Blood 91(12):4581–4593
Celinska-Lowenhoff M, Zabczyk M, Iwaniec T, Plens K, Musial J, Undas A (2018) Reduced plasma fibrin clot permeability is associated with recurrent thromboembolic events in patients with antiphospholipid syndrome. Rheumatology (Oxford) 57(8):1340–1349. https://doi.org/10.1093/rheumatology/key089
Chen F, Qiao Q, Xu P, Fan B, Chen Z (2014) Effect of factor XIII-A Val34Leu polymorphism on myocardial infarction risk: a meta-analysis. Clin Appl Thromb Hemost 20(8):783–792. https://doi.org/10.1177/1076029613504130
Chernysh IN, Weisel JW (2008) Dynamic imaging of fibrin network formation correlated with other measures of polymerization. Blood 111(10):4854–4861. https://doi.org/10.1182/blood-2007-08-105247
Chernysh IN, Nagaswami C, Weisel JW (2011) Visualization and identification of the structures formed during early stages of fibrin polymerization. Blood 117(17):4609–4614. https://doi.org/10.1182/blood-2010-07-297671
Chernysh IN, Nagaswami C, Peshkova AD, Kosolapova S, Cuker A, Cines DB, Cambor CL, Litvinov RI, Weisel JW (2020) The distinctive structure and composition of arterial and venous thrombi and pulmonary emboli. Sci Rep 10(1):5112. https://doi.org/10.1038/s41598-020-59526-x
Chung DW, Davie EW (1984) Gamma and gamma’ chains of human fibrinogen are produced by alternative mRNA processing. Biochemistry 23(18):4232–4236. https://doi.org/10.1021/bi00313a033
Cieslik J, Mrozinska S, Broniatowska E, Undas A (2018) Altered plasma clot properties increase the risk of recurrent deep vein thrombosis: a cohort study. Blood 131(7):797–807. https://doi.org/10.1182/blood-2017-07-798306
Cohen C, Parry DA (1990) Alpha-helical coiled coils and bundles: how to design an alpha-helical protein. Proteins 7(1):1–15. https://doi.org/10.1002/prot.340070102
Collet JP, Montalescot G, Lesty C, Weisel JW (2002) A structural and dynamic investigation of the facilitating effect of glycoprotein IIb/IIIa inhibitors in dissolving platelet-rich clots. Circ Res 90(4):428–434. https://doi.org/10.1161/hh0402.105095
Collet J-P, Moen JL, Veklich YI, Gorkun OV, Lord ST, Montalescot G, Weisel JW (2005) The αC domains of fibrinogen affect the structure of the fibrin clot, its physical properties, and its susceptibility to fibrinolysis. Blood 106(12):3824–3830. https://doi.org/10.1182/blood-2005-05-2150
Collet JP, Allali Y, Lesty C, Tanguy ML, Silvain J, Ankri A, Blanchet B, Dumaine R, Gianetti J, Payot L, Weisel JW, Montalescot G (2006) Altered fibrin architecture is associated with hypofibrinolysis and premature coronary atherothrombosis. Arterioscler Thromb Vasc Biol 26(11):2567–2573. https://doi.org/10.1161/01.ATV.0000241589.52950.4c
De Vries JJ, Snoek CJM, Rijken DC, De Maat MPM (2020) Effects of post-translational modifications of fibrinogen on clot formation, clot structure, and fibrinolysis. Arterioscler Thromb Vasc Biol 40 (in press). https://doi.org/10.1161/atvbaha.119.313626
Domingues MM, Macrae FL, Duval C, McPherson HR, Bridge KI, Ajjan RA, Ridger VC, Connell SD, Philippou H, Ariens RA (2016) Thrombin and fibrinogen gamma’ impact clot structure by marked effects on intrafibrillar structure and protofibril packing. Blood 127(4):487–495. https://doi.org/10.1182/blood-2015-06-652214
Doolittle RF, Pandi L (2006) Binding of synthetic B knobs to fibrinogen changes the character of fibrin and inhibits its ability to activate tissue plasminogen activator and its destruction by plasmin. Biochemistry 45(8):2657–2667. https://doi.org/10.1021/bi0524767
Duval C, Profumo A, Aprile A, Salis A, Millo E, Damonte G, Gauer JS, Ariëns RAS, Rocco M (2020) Fibrinogen αC-regions are not directly involved in fibrin polymerization as evidenced by a “Double-Detroit” recombinant fibrinogen mutant and knobs-mimic peptides. J Thromb Haemost 18(4):802–814. https://doi.org/10.1111/jth.14725
Erickson HP, Fowler WE (1983) Electron microscopy of fibrinogen, its plasmic fragments and small polymers. Ann N Y Acad Sci 408:146–163. https://doi.org/10.1111/j.1749-6632.1983.tb23242.x
Everse SJ, Spraggon G, Doolittle RF (1998a) A three-dimensional consideration of variant human fibrinogens. Thromb Haemost 80(1):1–9
Everse SJ, Spraggon G, Veerapandian L, Riley M, Doolittle RF (1998b) Crystal structure of fragment double-D from human fibrin with two different bound ligands. Biochemistry 37(24):8637–8642. https://doi.org/10.1021/bi9804129
Falvo MR, Millard D, O’Brien ET 3rd, Superfine R, Lord ST (2008) Length of tandem repeats in fibrin’s alphaC region correlates with fiber extensibility. J Thromb Haemost 6(11):1991–1993. https://doi.org/10.1111/j.1538-7836.2008.03147.x
Flick MJ, Du X, Witte DP, Jirouskova M, Soloviev DA, Busuttil SJ, Plow EF, Degen JL (2004) Leukocyte engagement of fibrin(ogen) via the integrin receptor alphaMbeta2/Mac-1 is critical for host inflammatory response in vivo. J Clin Invest 113(11):1596–1606. https://doi.org/10.1172/jci20741
Fogelson AL, Keener JP (2010) Toward an understanding of fibrin branching structure. Phys Rev E: Stat, Nonlin, Soft Matter Phys 81(5):051922. https://doi.org/10.1103/PhysRevE.81.051922
Fowler WE, Erickson HP (1979) Trinodular structure of fibrinogen. Confirmation by both shadowing and negative stain electron microscopy. J Mol Biol 134(2):241–249. https://doi.org/10.1016/0022-2836(79)90034-2
Galanakis DK (1993) Inherited dysfibrinogenemia: emerging abnormal structure associations with pathologic and nonpathologic dysfunctions. Semin Thromb Hemost 19(4):386–395. https://doi.org/10.1055/s-2007-993290
Galanakis DK, Henschen A, Peerschke EI, Kehl M (1989) Fibrinogen Stony Brook, a heterozygous A alpha 16Arg—Cys dysfibrinogenemia. Evaluation of diminished platelet aggregation support and of enhanced inhibition of fibrin assembly. J Clin Invest 84(1):295–304. https://doi.org/10.1172/jci114154
Galanakis D, Spitzer S, Scharrer I (1993) Unusual A alpha 16Arg– > Cys dysfibrinogenaemic family: absence of normal A alpha-chains in fibrinogen from two of four heterozygous siblings. Blood Coagul Fibrinolysis 4(1):67–71
Ganter MT, Hofer CK (2008) Coagulation monitoring: current techniques and clinical use of viscoelastic point-of-care coagulation devices. Anesth Analg 106(5):1366–1375. https://doi.org/10.1213/ane.0b013e318168b367
Gersh KC, Nagaswami C, Weisel JW (2009a) Fibrin network structure and clot mechanical properties are altered by incorporation of erythrocytes. Thromb Haemost 102(6):1169–1175. https://doi.org/10.1160/th09-03-0199
Gersh KC, Nagaswami C, Weisel JW, Lord ST (2009b) The presence of gamma’ chain impairs fibrin polymerization. Thromb Res 124(3):356–363. https://doi.org/10.1016/j.thromres.2008.11.016
Guthold M, Liu W, Sparks EA, Jawerth LM, Peng L, Falvo M, Superfine R, Hantgan RR, Lord ST (2007) A comparison of the mechanical and structural properties of fibrin fibers with other protein fibers. Cell Biochem Biophys 49(3):165–181. https://doi.org/10.1007/s12013-007-9001-4
Hall CE, Slayter HS (1959) The fibrinogen molecule: its size, shape, and mode of polymerization. J Biophys Biochem Cytol 5(1):11–16. https://doi.org/10.1083/jcb.5.1.11
Hanss M, Biot F (2001) A database for human fibrinogen variants. Ann N Y Acad Sci 936:89–90. https://doi.org/10.1111/j.1749-6632.2001.tb03495.x
He S, Blomback M, Jacobsson Ekman G, Hedner U (2003) The role of recombinant factor VIIa (FVIIa) in fibrin structure in the absence of FVIII/FIX. J Thromb Haemost 1(6):1215–1219. https://doi.org/10.1046/j.1538-7836.2003.00242.x
Henschen A, McDonagh J (1986) Chapter 7 fibrinogen, fibrin and factor XIII. In: Neuberger A, van Deenen LLM (eds) New comprehensive biochemistry, vol 13. Elsevier, pp 171–241. https://doi.org/10.1016/s0167-7306(08)60053-8
Hirota-Kawadobora M, Terasawa F, Yonekawa O, Sahara N, Shimizu E, Okumura N, Katsuyama T, Shigematsu H (2003) Fibrinogens Kosai and Ogasa: Bβ15Gly → Cys (GGT → TGT) substitution associated with impairment of fibrinopeptide B release and lateral aggregation. J Thromb Haemost 1(2):275–283. https://doi.org/10.1046/j.1538-7836.2003.00052.x
Hudson NE, Houser JR, O’Brien ET, Taylor RM, Superfine R, Lord ST, Falvo MR (2010) Stiffening of individual fibrin fibers equitably distributes strain and strengthens networks. Biophys J 98(8):1632–1640. https://doi.org/10.1016/j.bpj.2009.12.4312
Hudson NE, Ding F, Bucay I, O’Brien ET, Gorkun OV, Superfine R, Lord ST, Dokholyan NV, Falvo MR (2013) Submillisecond elastic recoil reveals molecular origins of fibrin fiber mechanics. Biophys J 104(12):2671–2680. https://doi.org/10.1016/j.bpj.2013.04.052
Hugenholtz GC, Macrae F, Adelmeijer J, Dulfer S, Porte RJ, Lisman T, Ariens RA (2016) Procoagulant changes in fibrin clot structure in patients with cirrhosis are associated with oxidative modifications of fibrinogen. J Thromb Haemost 14(5):1054–1066. https://doi.org/10.1111/jth.13278
Janmey PA, Amis EJ, Ferry JD (1983) Rheology of fibrin clots. VI. Stress relaxation, creep, and differential dynamic modulus of fine clots in large shearing deformations. J Rheol 27(2):135–153. https://doi.org/10.1122/1.549722
Jansen KA, Zhmurov A, Vos BE, Portale G, Merino DH, Litvinov RI, Tutwiler V, Kurniawan NA, Bras W, Weisel JW, Barsegov V, Koenderink GH (2020) Molecular packing structure of fibrin fibers resolved by X-ray scattering and molecular modeling. Soft Matter 16:8272–8283. https://doi.org/10.1039/d0sm00916d
Kang H, Wen Q, Janmey PA, Tang JX, Conti E, MacKintosh FC (2009) Nonlinear elasticity of stiff filament networks: strain stiffening, negative normal stress, and filament alignment in fibrin gels. J Phys Chem B 113(12):3799–3805. https://doi.org/10.1021/jp807749f
Kattula S, Byrnes JR, Wolberg AS (2017) Fibrinogen and fibrin in hemostasis and thrombosis. Arterioscler Thromb Vasc Biol 37(3):e13–e21. https://doi.org/10.1161/atvbaha.117.308564
Kim OV, Litvinov RI, Weisel JW, Alber MS (2014) Structural basis for the nonlinear mechanics of fibrin networks under compression. Biomaterials 35(25):6739–6749. https://doi.org/10.1016/j.biomaterials.2014.04.056
Kim OV, Liang X, Litvinov RI, Weisel JW, Alber MS, Purohit PK (2016) Foam-like compression behavior of fibrin networks. Biomech Model Mechanobiol 15(1):213–228. https://doi.org/10.1007/s10237-015-0683-z
Klykov O, van der Zwaan C, Heck AJR, Meijer AB, Scheltema RA (2020) Missing regions within the molecular architecture of human fibrin clots structurally resolved by XL-MS and integrative structural modeling. Proc Natl Acad Sci U S A 117(4):1976–1987. https://doi.org/10.1073/pnas.1911785117
Köhler S, Schmid F, Settanni G (2015) The internal dynamics of fibrinogen and its implications for coagulation and adsorption. PLoS Comput Biol 11(9):e1004346–e1004346. https://doi.org/10.1371/journal.pcbi.1004346
Kollman JM, Pandi L, Sawaya MR, Riley M, Doolittle RF (2009) Crystal structure of human fibrinogen. Biochemistry 48(18):3877–3886. https://doi.org/10.1021/bi802205g
Kostelansky MS, Betts L, Gorkun OV, Lord ST (2002) 2.8 A crystal structures of recombinant fibrinogen fragment D with and without two peptide ligands: GHRP binding to the “b” site disrupts its nearby calcium-binding site. Biochemistry 41(40):12124–12132. https://doi.org/10.1021/bi0261894
Langer BG, Weisel JW, Dinauer PA, Nagaswami C, Bell WR (1988) Deglycosylation of fibrinogen accelerates polymerization and increases lateral aggregation of fibrin fibers. J Biol Chem 263(29):15056–15063
Leong L, Chernysh IN, Xu Y, Sim D, Nagaswami C, de Lange Z, Kosolapova S, Cuker A, Kauser K, Weisel JW (2017) Clot stability as a determinant of effective factor VIII replacement in hemophilia A. Res Pract Thromb Haemost 1(2):231–241. https://doi.org/10.1002/rth2.12034
Lepedda AJ, Cigliano A, Cherchi GM, Spirito R, Maggioni M, Carta F, Turrini F, Edelstein C, Scanu AM, Formato M (2009) A proteomic approach to differentiate histologically classified stable and unstable plaques from human carotid arteries. Atherosclerosis 203(1):112–118. https://doi.org/10.1016/j.atherosclerosis.2008.07.001
Li W, Sigley J, Pieters M, Helms CC, Nagaswami C, Weisel JW, Guthold M (2016) Fibrin fiber stiffness is strongly affected by fiber diameter, but not by fibrinogen glycation. Biophys J 110(6):1400–1410. https://doi.org/10.1016/j.bpj.2016.02.021
Li W, Sigley J, Baker SR, Helms CC, Kinney MT, Pieters M, Brubaker PH, Cubcciotti R, Guthold M (2017) Nonuniform internal structure of fibrin fibers: Protein density and bond density strongly decrease with increasing diameter. Biomed Res Int 2017:6385628–6385628. https://doi.org/10.1155/2017/6385628
Liang X, Chernysh I, Purohit PK, Weisel JW (2017) Phase transitions during compression and decompression of clots from platelet-poor plasma, platelet-rich plasma and whole blood. Acta Biomater 60:275–290. https://doi.org/10.1016/j.actbio.2017.07.011
Lisman T, Ariens RA (2016) Alterations in fibrin structure in patients with liver diseases. Semin Thromb Hemost 42(4):389–396. https://doi.org/10.1055/s-0036-1572327
Litvinov RI, Weisel JW (2016) What is the biological and clinical relevance of fibrin? Semin Thromb Hemost 42(4):333–343. https://doi.org/10.1055/s-0036-1571342
Litvinov RI, Gorkun OV, Owen SF, Shuman H, Weisel JW (2005) Polymerization of fibrin: specificity, strength, and stability of knob-hole interactions studied at the single-molecule level. Blood 106(9):2944–2951. https://doi.org/10.1182/blood-2005-05-2039
Litvinov RI, Gorkun OV, Galanakis DK, Yakovlev S, Medved L, Shuman H, Weisel JW (2006) Polymerization of fibrin: direct observation and quantification of individual B:b knob-hole interactions. Blood 109(1):130–138. https://doi.org/10.1182/blood-2006-07-033910
Litvinov RI, Yakovlev S, Tsurupa G, Gorkun OV, Medved L, Weisel JW (2007) Direct evidence for specific interactions of the fibrinogen alphaC-domains with the central E region and with each other. Biochemistry 46(31):9133–9142. https://doi.org/10.1021/bi700944j
Litvinov RI, Faizullin DA, Zuev YF, Weisel JW (2012) The α-helix to β-sheet transition in stretched and compressed hydrated fibrin clots. Biophys J 103(5):1020–1027. https://doi.org/10.1016/j.bpj.2012.07.046
Litvinov RI, Kononova O, Zhmurov A, Marx KA, Barsegov V, Thirumalai D, Weisel JW (2018) Regulatory element in fibrin triggers tension-activated transition from catch to slip bonds. Proc Natl Acad Sci U S A 115(34):8575–8580. https://doi.org/10.1073/pnas.1802576115
Litvinov RI, Nabiullina RM, Zubairova LD, Shakurova MA, Andrianova IA, Weisel JW (2019) Lytic susceptibility, structure, and mechanical properties of fibrin in systemic lupus erythematosus. Front Immunol 10:1626. https://doi.org/10.3389/fimmu.2019.01626
Liu W, Jawerth LM, Sparks EA, Falvo MR, Hantgan RR, Superfine R, Lord ST, Guthold M (2006) Fibrin fibers have extraordinary extensibility and elasticity. Science 313(5787):634. https://doi.org/10.1126/science.1127317
Liu W, Carlisle CR, Sparks EA, Guthold M (2010) The mechanical properties of single fibrin fibers. J Thromb Haemost 8(5):1030–1036. https://doi.org/10.1111/j.1538-7836.2010.03745.x
Longstaff C, Varju I, Sotonyi P, Szabo L, Krumrey M, Hoell A, Bota A, Varga Z, Komorowicz E, Kolev K (2013) Mechanical stability and fibrinolytic resistance of clots containing fibrin, DNA, and histones. J Biol Chem 288(10):6946–6956. https://doi.org/10.1074/jbc.M112.404301
Luddington RJ (2005) Thrombelastography/thromboelastometry. Clin Lab Haematol 27(2):81–90. https://doi.org/10.1111/j.1365-2257.2005.00681.x
Macrae FL, Domingues MM, Casini A, Ariens RA (2016) The (patho)physiology of fibrinogen gamma’. Semin Thromb Hemost 42(4):344–355. https://doi.org/10.1055/s-0036-1572353
Madrazo J, Brown JH, Litvinovich S, Dominguez R, Yakovlev S, Medved L, Cohen C (2001) Crystal structure of the central region of bovine fibrinogen (E5 fragment) at 1.4-A resolution. Proc Natl Acad Sci USA 98(21):11967–11972. https://doi.org/10.1073/pnas.211439798
Marchi RC, Carvajal Z, Boyer-Neumann C, Anglés-Cano E, Weisel JW (2006) Functional characterization of fibrinogen Bicêtre II: a gamma 308 Asn– > Lys mutation located near the fibrin D: D interaction sites. Blood Coagul Fibrinolysis 17(3):193–201. https://doi.org/10.1097/01.mbc.0000220241.22714.68
Marsh JJ, Guan HS, Li S, Chiles PG, Tran D, Morris TA (2013) Structural insights into fibrinogen dynamics using amide hydrogen/deuterium exchange mass spectrometry. Biochemistry 52(32):5491–5502. https://doi.org/10.1021/bi4007995
Matsuka YV, Medved LV, Migliorini MM, Ingham KC (1996) Factor XIIIa-catalyzed cross-Linking of recombinant αC fragments of human fibrinogen. Biochemistry 35(18):5810–5816. https://doi.org/10.1021/bi952294k
Medved L, Weisel JW (2009) Recommendations for nomenclature on fibrinogen and fibrin. J Thromb Haemost 7(2):355–359. https://doi.org/10.1111/j.1538-7836.2008.03242.x
Medved L, Ugarova T, Veklich Y, Lukinova N, Weisel J (1990) Electron microscope investigation of the early stages of fibrin assembly. Twisted protofibrils and fibers. J Mol Biol 216(3):503–509. https://doi.org/10.1016/0022-2836(90)90376-w
Mills JD, Ariens RA, Mansfield MW, Grant PJ (2002) Altered fibrin clot structure in the healthy relatives of patients with premature coronary artery disease. Circulation 106(15):1938–1942. https://doi.org/10.1161/01.cir.0000033221.73082.06
Missori M, Papi M, Maulucci G, Arcovito G, Boumis G, Bellelli A, Amiconi G, De Spirito M (2010) Cl—and F—anions regulate the architecture of protofibrils in fibrin gel. Eur Biophys J 39(6):1001–1006. https://doi.org/10.1007/s00249-009-0492-3
Mosesson MW, Finlayson JS, Umfleet RA (1972) Human fibrinogen heterogeneities. 3. Identification of chain variants. J Biol Chem 247(16):5223–5227
Mosesson MW, DiOrio JP, Siebenlist KR, Wall JS, Hainfeld JF (1993) Evidence for a second type of fibril branch point in fibrin polymer networks, the trimolecular junction. Blood 82(5):1517–1521
Mrozinska S, Cieslik J, Broniatowska E, Malinowski KP, Undas A (2019) Prothrombotic fibrin clot properties associated with increased endogenous thrombin potential and soluble P-selectin predict occult cancer after unprovoked venous thromboembolism. J Thromb Haemost 17(11):1912–1922. https://doi.org/10.1111/jth.14579
Mullin JL, Gorkun OV, Lord ST (2000) Decreased lateral aggregation of a variant recombinant fibrinogen provides insight into the polymerization mechanism. Biochemistry 39(32):9843–9849. https://doi.org/10.1021/bi000045c
O’Brien ET, Falvo MR, Millard D, Eastwood B, Taylor RM, Superfine R (2008) Ultrathin self-assembled fibrin sheets. Proc Natl Acad Sci U S A 105(49):19438–19443. https://doi.org/10.1073/pnas.0804865105
Okumura N, Gorkun OV, Lord ST (1997) Severely impaired polymerization of recombinant fibrinogen gamma-364 Asp – > His, the substitution discovered in a heterozygous individual. J Biol Chem 272(47):29596–29601. https://doi.org/10.1074/jbc.272.47.29596
Okumura N, Terasawa F, Hirota-Kawadobora M, Yamauchi K, Nakanishi K, Shiga S, Ichiyama S, Saito M, Kawai M, Nakahata T (2006) A novel variant fibrinogen, deletion of Bβ111Ser in coiled-coil region, affecting fibrin lateral aggregation. Clin Chim Acta 365(1):160–167. https://doi.org/10.1016/j.cca.2005.08.014
Okumura N, Terasawa F, Haneishi A, Fujihara N, Hirota-Kawadobora M, Yamauchi K, Ota H, Lord ST (2007) B:b interactions are essential for polymerization of variant fibrinogens with impaired holes ‘a’1. J Thromb Haemost 5(12):2352–2359. https://doi.org/10.1111/j.1538-7836.2007.02793.x
Palka I, Nessler J, Nessler B, Piwowarska W, Tracz W, Undas A (2010) Altered fibrin clot properties in patients with chronic heart failure and sinus rhythm: a novel prothrombotic mechanism. Heart 96(14):1114–1118. https://doi.org/10.1136/hrt.2010.192740
Piechocka IK, Bacabac RG, Potters M, Mackintosh FC, Koenderink GH (2010) Structural hierarchy governs fibrin gel mechanics. Biophys J 98(10):2281–2289. https://doi.org/10.1016/j.bpj.2010.01.040
Pieters M, Wolberg AS (2019) Fibrinogen and fibrin: An illustrated review. Res Pract Thromb Haemost 3(2):161–172. https://doi.org/10.1002/rth2.12191
Ping L, Huang L, Cardinali B, Profumo A, Gorkun OV, Lord ST (2011) Substitution of the human αC region with the analogous chicken domain generates a fibrinogen with severely impaired lateral aggregation: fibrin monomers assemble into protofibrils but protofibrils do not assemble into fibers. Biochemistry 50(42):9066–9075. https://doi.org/10.1021/bi201094v
Protopopova AD, Barinov NA, Zavyalova EG, Kopylov AM, Sergienko VI, Klinov DV (2015) Visualization of fibrinogen αC regions and their arrangement during fibrin network formation by high-resolution AFM. J Thromb Haemost 13(4):570–579. https://doi.org/10.1111/jth.12785
Protopopova AD, Litvinov RI, Galanakis DK, Nagaswami C, Barinov NA, Mukhitov AR, Klinov DV, Weisel JW (2017) Morphometric characterization of fibrinogen’s αC regions and their role in fibrin self-assembly and molecular organization. Nanoscale 9(36):13707–13716. https://doi.org/10.1039/c7nr04413e
Purohit PK, Litvinov RI, Brown AEX, Discher DE, Weisel JW (2011) Protein unfolding accounts for the unusual mechanical behavior of fibrin networks. Acta Biomater 7(6):2374–2383. https://doi.org/10.1016/j.actbio.2011.02.026
Riha P, Wang X, Liao R, Stoltz JF (1999) Elasticity and fracture strain of whole blood clots. Clin Hemorheol Microcirc 21(1):45–49
Rocco M, Molteni M, Ponassi M, Giachi G, Frediani M, Koutsioubas A, Profumo A, Trevarin D, Cardinali B, Vachette P, Ferri F, Pérez J (2014) A comprehensive mechanism of fibrin network formation involving early branching and delayed single-to double-strand transition from coupled time-resolved X-ray/light-scattering detection. J Am Chem Soc 136(14):5376–5384. https://doi.org/10.1021/ja5002955
Ryan EA, Mockros LF, Weisel JW, Lorand L (1999) Structural origins of fibrin clot rheology. Biophys J 77(5):2813–2826. https://doi.org/10.1016/S0006-3495(99)77113-4
Scott EM, Ariens RA, Grant PJ (2004) Genetic and environmental determinants of fibrin structure and function: relevance to clinical disease. Arterioscler Thromb Vasc Biol 24(9):1558–1566. https://doi.org/10.1161/01.ATV.0000136649.83297.bf
Spraggon G, Everse SJ, Doolittle RF (1997) Crystal structures of fragment D from human fibrinogen and its crosslinked counterpart from fibrin. Nature 389(6650):455–462. https://doi.org/10.1038/38947
Standeven KF, Carter AM, Grant PJ, Weisel JW, Chernysh I, Masova L, Lord ST, Ariëns RAS (2007) Functional analysis of fibrin γ-chain cross-linking by activated factor XIII: determination of a cross-linking pattern that maximizes clot stiffness. Blood 110(3):902–907. https://doi.org/10.1182/blood-2007-01-066837
Storm C, Pastore JJ, MacKintosh FC, Lubensky TC, Janmey PA (2005) Nonlinear elasticity in biological gels. Nature 435(7039):191–194. https://doi.org/10.1038/nature03521
Sumaya W, Wallentin L, James SK, Siegbahn A, Gabrysch K, Bertilsson M, Himmelmann A, Ajjan RA, Storey RF (2018) Fibrin clot properties independently predict adverse clinical outcome following acute coronary syndrome: a PLATO substudy. Eur Heart J 39(13):1078–1085. https://doi.org/10.1093/eurheartj/ehy013
Torbet J, Freyssinet JM, Hudry-Clergeon G (1981) Oriented fibrin gels formed by polymerization in strong magnetic fields. Nature 289(5793):91–93. https://doi.org/10.1038/289091a0
Trezzini C, Jungi TW, Kuhnert P, Peterhans E (1988) Fibrinogen association with human monocytes: evidence for constitutive expression of fibrinogen receptors and for involvement of Mac-1 (CD18, CR3) in the binding. Biochem Biophys Res Commun 156(1):477–484. https://doi.org/10.1016/s0006-291x(88)80866-0
Tsurupa G, Mahid A, Veklich Y, Weisel JW, Medved L (2011) Structure, stability, and interaction of fibrin αC-domain polymers. Biochemistry 50(37):8028–8037. https://doi.org/10.1021/bi2008189
Undas A (2016) How to assess fibrinogen levels and fibrin clot properties in clinical practice? Semin Thromb Hemost 42(4):381–388. https://doi.org/10.1055/s-0036-1579636
Undas A, Ariens RA (2011) Fibrin clot structure and function: a role in the pathophysiology of arterial and venous thromboembolic diseases. Arterioscler Thromb Vasc Biol 31(12):e88–99. https://doi.org/10.1161/atvbaha.111.230631
Undas A, Szuldrzynski K, Stepien E, Zalewski J, Godlewski J, Tracz W, Pasowicz M, Zmudka K (2008) Reduced clot permeability and susceptibility to lysis in patients with acute coronary syndrome: effects of inflammation and oxidative stress. Atherosclerosis 196(2):551–557. https://doi.org/10.1016/j.atherosclerosis.2007.05.028
Undas A, Slowik A, Wolkow P, Szczudlik A, Tracz W (2010) Fibrin clot properties in acute ischemic stroke: relation to neurological deficit. Thromb Res 125(4):357–361. https://doi.org/10.1016/j.thromres.2009.11.013
Veklich YI, Gorkun OV, Medved LV, Nieuwenhuizen W, Weisel JW (1993) Carboxyl-terminal portions of the alpha chains of fibrinogen and fibrin. Localization by electron microscopy and the effects of isolated alpha C fragments on polymerization. J Biol Chem 268(18):13577–13585
Vos BE, Martinez-Torres C, Burla F, Weisel JW, Koenderink GH (2020) Revealing the molecular origins of fibrin’s elastomeric properties by in situ X-ray scattering. Acta Biomater 104:39–52. https://doi.org/10.1016/j.actbio.2020.01.002
Weisel JW (1986) The electron microscope band pattern of human fibrin: various stains, lateral order, and carbohydrate localization. J Ultrastruct Mol Struct Res 96(1–3):176–188. https://doi.org/10.1016/0889-1605(86)90019-4
Weisel JW (2004) The mechanical properties of fibrin for basic scientists and clinicians. Biophys Chem 112(2–3):267–276. https://doi.org/10.1016/j.bpc.2004.07.029
Weisel JW, Litvinov RI (2013) Mechanisms of fibrin polymerization and clinical implications. Blood 121(10):1712–1719. https://doi.org/10.1182/blood-2012-09-306639
Weisel JW, Litvinov RI (2017) Fibrin formation, structure and properties. Sub-cellular biochemistry 82:405–456. https://doi.org/10.1007/978-3-319-49674-0_13
Weisel JW, Medved L (2001) The structure and function of the alpha C domains of fibrinogen. Ann NY Acad Sci 936:312–327. https://doi.org/10.1111/j.1749-6632.2001.tb03517.x
Weisel JW, Warren SG, Cohen C (1978) Crystals of modified fibrinogen: size, shape and packing of molecules. J Mol Biol 126(2):159–183. https://doi.org/10.1016/0022-2836(78)90357-1
Weisel JW, Phillips GN Jr, Cohen C (1983) The structure of fibrinogen and fibrin: II. Architecture of the fibrin clot. Ann N Y Acad Sci 408:367–379. https://doi.org/10.1111/j.1749-6632.1983.tb23257.x
Weisel JW, Stauffacher CV, Bullitt E, Cohen C (1985) A model for fibrinogen: domains and sequence. Science 230(4732):1388–1391. https://doi.org/10.1126/science.4071058
White NJ (2018) Clot structure predicts recurrent thrombosis. Blood 131(7):715–716. https://doi.org/10.1182/blood-2018-01-824169
Williams RC (1981) Morphology of bovine fibrinogen monomers and fibrin oligomers. J Mol Biol 150(3):399–408. https://doi.org/10.1016/0022-2836(81)90555-6
Wolberg AS, Allen GA, Monroe DM, Hedner U, Roberts HR, Hoffman M (2005) High dose factor VIIa improves clot structure and stability in a model of haemophilia B. Br J Haematol 131(5):645–655. https://doi.org/10.1111/j.1365-2141.2005.05820.x
Wolfenstein-Todel C, Mosesson MW (1981) Carboxy-terminal amino acid sequence of a human fibrinogen gamma-chain variant (gamma’). Biochemistry 20(21):6146–6149. https://doi.org/10.1021/bi00524a036
Yang Z, Mochalkin I, Doolittle RF (2000) A model of fibrin formation based on crystal structures of fibrinogen and fibrin fragments complexed with synthetic peptides. Proc Natl Acad Sci U S A 97(26):14156–14161. https://doi.org/10.1073/pnas.97.26.14156
Yee VC, Pratt KP, Côté HC, Trong IL, Chung DW, Davie EW, Stenkamp RE, Teller DC (1997) Crystal structure of a 30 kDa C-terminal fragment from the gamma chain of human fibrinogen. Structure 5(1):125–138. https://doi.org/10.1016/s0969-2126(97)00171-8
Yermolenko IS, Lishko VK, Ugarova TP, Magonov SN (2011) High-resolution visualization of fibrinogen molecules and fibrin fibers with atomic force microscopy. Biomacromol 12(2):370–379. https://doi.org/10.1021/bm101122g
Yeromonahos C, Polack B, Caton F (2010) Nanostructure of the fibrin clot. Biophys J 99(7):2018–2027. https://doi.org/10.1016/j.bpj.2010.04.059
Zhmurov A, Brown AE, Litvinov RI, Dima RI, Weisel JW, Barsegov V (2011) Mechanism of fibrin(ogen) forced unfolding. Structure 19(11):1615–1624. https://doi.org/10.1016/j.str.2011.08.013
Zhmurov A, Protopopova AD, Litvinov RI, Zhukov P, Mukhitov AR, Weisel JW, Barsegov V (2016) Structural basis of interfacial flexibility in fibrin oligomers. Structure 24(11):1907–1917. https://doi.org/10.1016/j.str.2016.08.009
Zhmurov A, Protopopova AD, Litvinov RI, Zhukov P, Weisel JW, Barsegov V (2018) Atomic structural models of fibrin oligomers. Structure 26(6):857–868.e854. https://doi.org/10.1016/j.str.2018.04.005
Zucker M, Seligsohn U, Salomon O, Wolberg AS (2014) Abnormal plasma clot structure and stability distinguish bleeding risk in patients with severe factor XI deficiency. J Thromb Haemost 12(7):1121–1130. https://doi.org/10.1111/jth.12600
Zuev YF, Litvinov RI, Sitnitsky AE, Idiyatullin BZ, Bakirova DR, Galanakis DK, Zhmurov A, Barsegov V, Weisel JW (2017) Conformational flexibility and self-association of fibrinogen in concentrated solutions. J Phys Chem B 121(33):7833–7843. https://doi.org/10.1021/acs.jpcb.7b05654
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Litvinov, R.I., Pieters, M., de Lange-Loots, Z., Weisel, J.W. (2021). Fibrinogen and Fibrin. In: Harris, J.R., Marles-Wright, J. (eds) Macromolecular Protein Complexes III: Structure and Function. Subcellular Biochemistry, vol 96. Springer, Cham. https://doi.org/10.1007/978-3-030-58971-4_15
Download citation
DOI: https://doi.org/10.1007/978-3-030-58971-4_15
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-58970-7
Online ISBN: 978-3-030-58971-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)