Abstract
Plantar fasciitis is one of the most common pathologies treated by a foot and ankle surgeon, being the most common cause of heel pain, affecting up to 10% of the population. Nonoperative therapy is the first choice and can have good stable results over time: when this fails, surgical treatment should be indicated and is warranted. Most patients are treated conservatively with physiotherapy, medications, ice, orthotics, and local injections, but about 10% of patients undergo surgical therapy to resolve recurrent symptoms. Various surgical procedures are available for the treatment of recalcitrant plantar fasciitis. The most common surgical management typically consists of open versus endoscopic plantar fascia release. Comorbidities at the foot or lower limb are documented in association with plantar fasciitis, although these do not represent the main cause of the disorder. The endoscopic resection of the plantar fascia, with or without heel spur removal, allows good visualization of the entire plantar fascia and allows a minimally invasive technique that provides patient satisfaction and stable and acceptable outcomes.
Director of Department: Stefano Gumina
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
1 Introduction
Plantar fasciitis is a common cause of heel pain in adults. It is a soft-tissue disorder first described by William Wood in 1812 [1] and known by many pseudonyms such as jogger’s heel, heel spur syndrome, plantar fascial insertitis, calcaneal enthesopathy, subcalcaneal bursitis, subcalcaneal pain, neuritis, and calcaneodynia. This lifestyle-limiting condition can be defined as a localized inflammation of both perifascial structures and plantar fascia at the proximal attachment on the medial tuberosity of the calcaneus. It is thought to be caused by biomechanical overuse from prolonged standing or running, resulting from chronic repetitive microtears and degeneration secondary to overuse or mechanical and congenital disorders [1]. Plantar fasciitis affects up to 10% of the general population and accounts for 10–15% of all foot pain symptomatology; it is experienced at least once in the lifetime of the afflicted population [2]. Although the etiopathogenesis of plantar fasciitis is poorly understood, it is actually considered multifactorial: caused by multiple microtears resulting from an increase in stress and repeated fascia stretching, it exceeds the repair capacity of the body. Diagnosis of plantar fasciitis is based on patient history and risk factors. Among them are referenced excessive congenital disorders such as foot pronation (pes planus), high arch (pes cavus), tightness of the Achilles tendon, and intrinsic foot muscle and leg length discrepancy, while being important in daily activities such as working with prolonged standing, walking occupations (e.g., military or police personnel), excessive running, obesity with a body mass index greater than 34.5–35, and poor motor activity. Some studies have shown that plantar fasciitis is better described as plantar fasciosis because its histological changes at the calcaneal enthesis are consistent with a chronic inflammatory condition, myxoid degeneration, noninflammatory degeneration, fibroblastic hypertrophy, and chaotic vascular hyperplasia, indicating a particular histological picture known as fasciosis [3].
2 Anatomic Aspects
Anatomically, the plantar fascia is divided into three bands: medial, central, and lateral. The central band attaches proximally to the medial tuberosity of the calcaneus, separating distally into five individual small bands whose divisions attach to the sesamoids and to the plantar plate of the second through the fifth toes. First described by Hicks in 1954 as the windlass mechanism, the plantar fascia tenses during the terminal stance to toe-off phases of gait. This tension elevates and reinforces the medial longitudinal arch, which in turn allows the foot to work as a rigid lever for forward propulsion [4].
3 Findings and Physical Examination
Plantar fasciitis needs primarily a clinical diagnosis, being the onset of inferior heel pain that is insidious and worsens over time with standing and walking. The sharp pain is usually localized to the plantar-medial aspect of the heel or over a small area near the proximal insertion of the plantar fascia at the medial tuberosity of the calcaneus. Most patients suffer heel pain and tightness after standing up from bed in the morning or after a prolonged time seated, the heel pain improving with ambulation. Occasionally pain can intensify day by day, so that the patient may be obliged to continue walking or standing even for a long time. Findings suggestive of plantar fasciitis include reproducible pain with palpation of the plantar medial aspect of the heel and pain with passive dorsiflexion of the ankle and toes (windlass test). The imaging techniques useful in confirmation of plantar disorder are ultrasound (US), plain radiographs, magnetic resonance imaging (MRI), bone scintigraphy (BS), and elastography. Ultrasound (US) is often to be considered in the first step of diagnosis, remaining lower in cost, noninvasive, safe, portable, radiation free, and easy to administer compared to the other modalities. Radiographic images have been used in the process of diagnosing, relative to those cases where the presence of calcaneal bone spurs need to be confirmed. However, subcalcaneal spurs may be present also, and it is generally fundamental to evaluate the presence of a congenital or acquired deformity of the longitudinal plantar arch, which acknowledgment can represent a direct relationship to a diagnosis of plantar fasciitis. MRI has been confirmed as a reliable and validated tool to effectively diagnose plantar fasciitis, being considered a perfect means to assess and differentiate any abnormalities in its thickness.
4 Management and Treatment
Most patients recover without surgery, with only lifestyle modification. Patient education into the expectation and duration of treatment from the outset is fundamental to achieve collaboration at the maximum level. Plantar fasciitis is an overuse phenomenon, and avoiding high-impact activities seems very sensible at its beginning, although patients may consider this change frustrating because this condition has an indolent course. From 85% to 90% of patients affected by plantar fasciitis can be successfully treated with conservative treatment without surgery. Although treatment may be required for 6 months or longer, about 80% of patients treated conservatively have no recurrence of pain for a long time [2]. Initial management should include sufficient foot rest with analgesic and antiflammatory drug use, as nonsteroidal antiinflammatory drugs (NSAIDs) have been shown to represent an adequate means of pain control, especially when used in combination with other kinds of treatment [5, 6]. The intermittent application of ice seems to provide some benefit to patients in association with or during other treatments. Many physical therapies are available that may mitigate and relieve heel pain associated with fascial disorder: these modalities include manual therapy, such as stretching exercises of the calf muscles. Iontophoresis, ultrasound therapy, extracorporeal radial shock wave therapy (ESWT) [7], and laser therapy [8] could be useful in pain control. Also, monophasic pulsed currents support efficiency in reducing inferior heel pain and tenderness and improving functional activities levels associated with plantar fasciitis [9]. These treatments evaluated in comparison have been demonstrated to be effective for maintaining the improvements in pain and functional ability among the patients treated with two different therapies until follow-up at 12 months [7,8,9,10]. Osteopathic manipulative treatment techniques may occasionally provide immediate improvement of plantar fasciitis symptoms; however, the continued maintenance of these results is still being discussed. In some cases, night splinting, customized inserts, shoe modification, and plantar fascia taping could be beneficial [11]. A wide variety of orthotic device options are available for the management of plantar fasciitis: the use of shoe inserts, such as silicone heel pads, felt pads, and a rubber heel cup, in combination with stretching exercises, has been shown to provide superior short-term improvement in relieving symptoms compared to stretching alone [11].
Local injections should be considered: the use of corticosteroid must be evaluated with caution, because of the potentially unfavorable risk–benefit ratio for patients and the briefness of pain relief. Although the local corticosteroid injection (CSI) technique has significantly better treatment outcomes because it is immediately available and easy to administer, both CSI and extracorporeal radial shock wave therapy (ESWT) could be preferred as the primary treatment of patients with acute plantar fasciitis [12]. Early results of platelet-rich plasma (PRP) local injection have been promising: at 12 months, PRP is significantly more effective than steroids, providing better and more durable results than CSI as a treatment option [13]. Platelet-rich plasma is produced via centrifuged autologous blood. The plasma collected is rich with platelets, which release growth factors to stimulate healing in degenerative tissue; currently, some slight evidence supports the use of platelet-rich plasma for nonhealing tendinopathies [14]. On the other hand, a systematic review and meta-analysis found corticosteroid efficacy as compared to autologous whole blood to be marginally superior in relieving pain intensity in patients at 2 and 6 weeks [15]. When conservative therapies have been ineffective and significant symptoms persist, associated with further complications such as chronic pain and arch collapse, surgery is often considered as the last resort, and it can be suited to the patient needs.
Fasciotomy results in significant changes in joint position. A decrease in arch height in a quite wide extension is not suggested for patients with preexisting pes planus because possible consequences may lead to further deterioration of foot position [16]. Overall, these biomechanical effects on the foot are still unclear. Plantar fasciotomy may appear to lead to changes in arch stability in cadaveric specimens and models, thus suggesting modifying the procedure from complete to partial release. However, what effect this may have in the longer term on human subjects in vivo has not been conclusively demonstrated. Again, surgery for plantar fasciitis is not always clinically successful, with 10–50% of patients left unsatisfied following surgery, and with poorer outcomes being obtained in those with more severe symptoms and with a longer duration of preoperative symptoms [17, 18].
A change in operative technique has been noted in the literature, with endoscopic plantar fascia release (EPFR) becoming a viable alternative to the previously established open procedures. Based on the findings of noninflammatory vascular dysfunction, newer treatments for recalcitrant plantar fasciitis have been aimed at focal stimulation and localized angiogenesis. Because it is considered a fasciosis, radiofrequency coblation has been successfully proposed as a minimally invasive treatment modality for chronic plantar fasciitis. Radiofrequency microtenotomy is demonstrated as effective at relieving pain, improving function, achieving patient satisfaction, and meeting patient expectations as plantar fasciotomy [19]. Plantar fasciotomy is perceived as a risky procedure leading to deterioration in foot stability in time. Surgery for plantar fasciitis remains an appropriate treatment option for a patient who does not respond to conservative therapeutic options, achieving reasonable success in the long term, with stable results that do not seem to deteriorate over time even when surgery is conducted within 1 or 2 years from symptom onset [20]. The disadvantages of surgery include incision care, immobilization, and potential complications such as arch flattening, nerve injury, calcaneal fracture, length of recovery time, and reflex sympathetic dystrophy.
5 Endoscopic Procedure
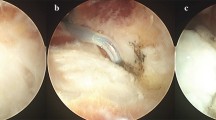
To assess endoscopic treatment, the patient is in supine position with the foot outside the external border of the surgical bed. Spinal or triple-nerve block anesthesia is performed. A tourniquet is recommended to avoid the risk of lack of visualization because of bleeding, which comes from the deep venous vein net, strongly represented on the plantar side of the foot. The instrumentation is the same for carpal tunnel release: a slotted cannula, a blunt trochar, a retrograde hook scalpel, and a regular 30° scope. Skin demarcation of the posterior aspect of medial malleolus and anterior calcaneus, plantar arch, plantar fascia insertion, and small venous vessels should be outlined before surgery (Fig. 32.1). The first portal is placed medially at the upper insertion of the plantar fascia. Through this portal the blunt trochar is passed (Fig. 32.2) until it emerges under the skin projection of the fascia insertion on the lateral side of the heel (Fig. 32.3). The lateral portal is now opened to permit the trochar to advance. The slotted cannula is advanced alongside the trochar, from lateral to medial until emerging medially (Fig. 32.4). When the trochar is removed and the cannula cleaned, the arthroscope is placed to present a visualization of the entire fascia (Fig. 32.5). The central toward the medial portion of the plantar fascia is explored with a hook probe (Fig. 32.6) and then resected from lateral to medial, keeping the scope placed laterally (Fig. 32.7). After a final cleanup of the cannula, resection is evaluated with the hook probe detecting the integrity of the flexor hallucis brevis muscle by moving the toe (see Video 32.1). Skin portals are closed with sutures. An ankle bandage is applied for 1 day. Partial weight-bearing is possible with crutches for 2 weeks until complete weight-bearing is permitted.
Traps | Tricks |
|---|---|
Do not consider surgery as first therapeutic choice | Primarily make a correct clinical diagnosis |
Patient requires therapy with immediate effect on pain | Consider in advance changes in lifestyle and type of shoes |
Difficult blind procedure with scope if not performed without blood loss | Use of tourniquet makes a low time-consuming procedure |
Frequent postoperative heel discomfort makes patient unsatisfied | Orthotic devices such as silicone heel pads, felt pads, and rubber heel cup should be indicated for a long period after surgery |
Key Points
-
Plantar fasciitis is primarily a clinical diagnosis and requires a physical examination for differential diagnosis.
-
Female patients, middle-aged patients, long-distance runners, military personnel, obese patients, and individuals with a cavus or planus foot deformity are at increased risk for developing plantar fasciitis.
-
Lifestyle changes are strongly recommended as first treatment.
-
Conservative therapies are recommended for the initial management of plantar fasciitis.
-
Among symptomatic patients with low satisfaction and high expectations, 10% can be submitted to plantar surgical release, by fasciotomy or radiofrequency microtenotomy.
References
DeMaio M, Paine R, Mangine RE, Drez D Jr. Plantar fasciitis. Orthopedics. 1993;16(10):1153–63.
Riddle DL, Schappert SM. Volume of ambulatory care visits and patterns of care for patients diagnosed with plantar fasciitis: a national study of medical doctors. Foot Ankle Int. 2004;25(5):303–10.
Thomas JL, Christensen JC, Kravitz SR, et al.; American College of Foot and Ankle Surgeons Heel Pain Committee. The diagnosis and treatment of heel pain: a clinical practice guideline, revision 2010. J Foot Ankle Surg. 2010;49(3 Suppl):S1–S19.
Hicks JH. The mechanics of the foot. II: the plantar aponeurosis and the arch. J Anat. 1954;88(1):25–30.
Wolgin M, Cook C, Graham C, et al. Conservative treatment of plantar heel pain: long-term follow-up. Foot Ankle Int. 1994;15(3):97–102.
Gill LH, Kiebzak GM. Outcome of nonsurgical treatment for plantar fasciitis. Foot Ankle Int. 1996;17(9):527–32.
Grecco MV, Brech GC, D’Andrea Greve JM. One-year treatment follow-up of plantar fasciitis: radial shockwaves vs. conventional physiotherapy. Clinics. 2013;68(8):1089–95.
Macias DM, Coughlin MJ, Zang K, Stevens FR, Jastifer JR, Doty JF. Low-level laser therapy at 635 nm for treatment of chronic plantar fasciitis: a placebo-controlled, randomized study. J Foot Ankle Surg. 2015;54:768–72.
Alotaibi AK, Petrofsky JS, Daher NS, Lohman E, Laymon M, Syed HM. Effect of monophasic pulsed current on heel pain and functional activities caused by plantar fasciitis. Med Sci Monit. 2015;21:833–9.
Thompson JV, Saini SS, Reb CW, Daniel JN. Diagnosis and management of plantar fasciitis. J Am Osteopath Assoc. 2014;114(12):900–6.
Pfeffer G, Bacchetti P, Deland J, et al. Comparison of custom and prefabricated orthoses in the initial treatment of proximal plantar fascitis. Foot Ankle Int. 1999;20(4):214–21.
Mardani-Kivi M, Mobarakeh MK, Hassanzadeh Z, Mirbolook A, Asadi K, Ettehad H, Hashemi-Motlagh K, Saheb-Ekhtiari K, Fallah-Alipour K. Treatment outcomes of corticosteroid injection and extracorporeal shock wave therapy as two primary therapeutic methods for acute plantar fasciitis: a prospective randomized clinical trial. J Foot Ankle Surg. 2015;54:1047–52.
Jaina K, Murphy PN, Clough TM. Platelet rich plasma versus corticosteroid injection for plantar fasciitis: a comparative study. Foot. 2015;25:235–7.
Sampson S, Gerhardt M, Mandelbaum B. Platelet rich plasma injection grafts for musculoskeletal injuries: a review. Curr Rev Musculoskelet Med. 2008;1(3–4):165–74.
Tsikopoulos K, Tsikopoulos A, Natsis K. Autologous whole blood or corticosteroid injections for the treatment of epicondylopathy and plantar fasciopathy? A systematic review and meta-analysis of randomized controlled trials. Phys Ther Sport. 2016;22:114e–22e.
Kitaoka HB, Luo ZP, An KN. Mechanical behavior of the foot and ankle after plantar fascia release in the unstable foot. Foot Ankle Int. 1997;18:8–15.
Jerosch J, Schunck J, Liebsch D, Filler T. Indication, surgical technique and results of endoscopic release in plantar fasciitis. Knee Surg Sports Traumatol Arthrosc. 2004;12:471–7.
Lundeen RO, Aziz S, Burks JB, Rose JM. Endoscopic plantar fasciotomy: a retrospective analysis of results in 53 patients. J Foot Ankle Surg. 2000;39:208–17.
Chen Chou AC, Yung Chuan S, Hsien Ching SD, Rikhraj Singh I, Koo K. Radiofrequency microtenotomy is as effective as plantar fasciotomy in the treatment of recalcitrant plantar fasciitis. Foot Ankle Surg. 2016;22:270–3.
Wheeler P, Boyd K, Shipton M. Surgery for patients with recalcitrant plantar fasciitis: good results at short-, medium-, and long-term follow-up. Orthop J Sports Med. 2014;2(3):2325967114527901.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
1 Electronic Supplementary Material
Endoscopic plantar fascitis (MP4 175,338 kb)
Plantar fascitis (MP4 94,022 kb)
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Allegra, F., Corsini, G., Paglialunga, C. (2020). Endoscopic Treatment of Plantar Fasciitis. In: Allegra, F., Cortese, F., Lijoi, F. (eds) Ankle Joint Arthroscopy. Springer, Cham. https://doi.org/10.1007/978-3-030-29231-7_32
Download citation
DOI: https://doi.org/10.1007/978-3-030-29231-7_32
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-29230-0
Online ISBN: 978-3-030-29231-7
eBook Packages: MedicineMedicine (R0)