Abstract
The clusters of differentiation (CD) are cell-surface receptors involved in cellular functions like activation, adhesion, and inhibition. These ubiquitous receptors express elevated levels of CD on cells which can serve as key marker in several cancers and infectious diseases. We emphasize on CD receptors involved in cancer, infections, and immune response. In particular, we cover the physiology and pathophysiology of the CD receptor and track the latest developments in targeted delivery of therapeutics and diagnostics mediated via CD receptor.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
The immune system protects human body from being infected by invading foreign organisms by well-controlled feedback mechanisms [1]. The cluster of differentiation (CD), which is also termed as CD molecule, CD marker, or CD antigen, is a cell surface glycoprotein that plays significant role in a number of biological functions, a major role being mediating immune reactions. CD receptors are considered to be highly promising drug targets for cancer, inflammatory, immunological, and infectious diseases [2, 3]. This chapter discusses the major CD involved in enabling improved therapy. An important focus is targeted delivery by receptor-mediated endocytosis via CD44 which has been widely investigated.
2 The Receptor
The “clusters of differentiation” (CD) is a term used to denote cell surface molecules which serve as targets for immunophenotyping of cells. As far as physiology is concerned, CD antigens can behave in many ways, often acting as important receptors or ligands. Some CD antigens do not play a part in the signaling of cells, but have other features such as cell activation, cell adhesion, and cell inhibition [4, 5]. In immunophenotyping, CD antigens are widely used as cell markers, enabling cells to be characterized based on what molecules are present on their surface. These markers serve to associate different cells with specific immune functions. Over 350 unique and distinctive CD markers have been recognized by the official list of determinants [6]. A discussion on all is beyond the purview of this chapter. We focus on six receptors, namely, CD3, CD4, CD8, CD19, CD20, and CD44 which play important roles in cancer and infectious disease. Details on other CD antigens/receptors may be referred in [6].
3 The CD Antigens and Receptors
CD antigens and receptors engage in diverse roles, acting as either receptors on cells or ligands for receptors to initiate a signal cascade that could alter some cellular function.
3.1 CD3 Complex (T-Cell Receptor (TCR) Complex)
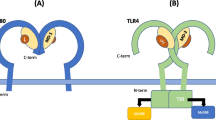
TCR complex is noncovalently coupled with a set of five immunoglobulins associated with transmembrane proteins. Five polypeptides involved are CD3γ (21–28 kDa), CD3δ (20–28 kDa), CD3ε (20–25 kDa), CD3ζ (16 kDa), and CD3η (22 kDa) shown in Fig. 13.1a. CD3 proteins have an extracellular region of the N-terminal, a transmembrane domain, and a cytoplasmic tail with immunoreceptor tyrosine activation motifs (ITAMs). There is also an immunoglobulin-like domain. The cytoplasmic region and domain of CD3 ε, CD3 γ, CD3 δ, and CD3 ζ comprise totally 10 ITAMs which make the complex extremely susceptible to antigen binding. Aspartic acid imparts a negative charge to CD3γ, CD3δ, and CD3ε. The side chain of this negatively charged amino acid interacts with the strongly loaded side chains of proteins in the TCRα and β transmembrane areas, an interaction that can either add to complicated integrity or signaling function [7,8,9,10,11,12,13,14,15].
CD3 functions as T-cell coreceptor and enables activation of the cytotoxic CD8+ and CD4+ naive T cells. The CD3 chains serve two distinct functions for activating T cells, namely, facilitating the introduction of TCR into the plasma membrane and transduction of signals following involvement through the TCR binding site. Together, the TCR and the CD3 molecules form the TCR complex. To produce an activation signal in T lymphocytes, these CD3 chains are associated with the TCR and the ζ chain. The complex functions by transmitting intracellular signals during the recognition of antigen TCR. CD3 ε is one of at least three invariant proteins associated with the TCR variable antigen recognition chains and signal transduction function. Because CD3 is necessary for the activation of T cells, drugs especially monoclonal antibodies are explored for immunosuppressant therapies [7,8,9].
3.2 CD4
CD4, a transmembrane glycoprotein (Fig.13.1b), is expressed on the cell surface as a single polypeptide having four immunoglobin (Ig)-like extracellular domains, making it a superfamily member of the Ig. It has a hydrophobic transmembrane domain with 38 amino acids comprising an extremely fundamental cytoplasmic tail, together with phosphorylated serine residues. CD4’s N-terminal Ig-like domains interact with the non-polymorphic α2 and β2 domains of MHC class II molecules, mediating functions of recognition and adhesion CD4’s cytoplasmic tail has locations that make better physical linkage with cytotoxic T lymphocytes (CTLs , a lymphocyte-specific protein tyrosine, Lck) kinase [16].
CD4, the component of the T lymphocyte receptor and coreceptor of the human immunodeficiency virus, is downmodulated when antigen or phorbol esters activate cells. Amplification of CD4 by activated T cell as a response to an enzyme-based signaling cascade generates signal by the TCR which produces various kinds of T-helper cells. Using the extracellular domain, CD4 binds with MHC class II molecules which are present on the APC. Both the TCR complex and CD4 are designated for binding to distinct areas of the MHC II molecule during antigen presentation [17].
3.3 CD8
In both humans and mice, majority of CD8 molecules expressed on T-cell surface confined by MHC class I are CD8αβ heterodimers consisting of CD8α (38 kDa chain) and CD8β (30 kDa chain) joined by disulfide linkage which are depicted in Fig.13.1c. Some intestinal T cells on the cell surface, however, express a CD8αα homodimer. The complete CD8 protein consists of one Ig-like extracellular hydrophobic domain and 26-residue cytoplasmic tail. Adherence of CD8 to the α3 MHC class I domain occurs following recognition of the TCR-domain-based recognition and adherence to TCRs. The CD8 cytoplasmic tail connection to Lck (lymphocyte-specific protein tyrosine kinase) is weak compared to CD4 [10,11,12,13,14,15, 18].
The CD8 cell surface marker protein helps to differentiate between the CTLs CD8+ and T helper (Th) cells CD4+. Involvement of CD8 in CTL coactivation has been associated with enhancing antigen sensitivity and stabilization of the TCR/MHC interaction. The CD8 coreceptor interacts with a distinct invariant region of the MHC I molecule compared to TCR, thereby enabling formation of a tripartite (TCR/peptide-major histocompatibility complex, pMHC)/CD8) complex.
3.4 CD19
CD19 antigen (95 kDa) is a transmembrane glycoprotein. It belongs to superfamily of Ig, the antigen which is categorized as a type I transmembrane protein. It consists of a single transmembrane domain, with C terminus in the cytoplasm and N terminus positioned extracellularly. It is encoded by the CD19 gene of 7.41 kilobyte situated on chromosome 16’s short arm which codes for the CD19 molecule. The extracellular component includes two Ig-like domains of type C2 separated by a narrower prospective non-Ig-like domain associated with disulfide, and additional carbohydrate sites linked to N. There is no vital homology between CD19 and other recognized proteins [19]. The structure of CD19 receptor is shown in Fig.13.1d. CD19 modulates B-cell receptor (BCR)-dependent and independent signaling. Another important role is to establish intrinsic B-cell signaling thresholds. It supports growth of antigen-independent development. It also influences the activation of B cells induced by immunoglobulin that is crucial to generate an ideal immune response. In B-cell activation, CD19 as an adaptor protein helps to incorporate signaling proteins from the cytoplasm to the membrane. It is also considered important as a signal subunit for CD19/CD21 conjugation by linking with the BCR.
3.5 CD20
CD20 is a nonglycosylated phosphoprotein of 35 kDa which is embedded in the cell membrane. In humans, CD20 is encoded by the MS4A1gene, which belongs to the membrane-spanning 4A gene family. It possesses four domains spanning the membrane with a short extracellular segment of about 43 residues and the terminal amino and carboxy N in the cytoplasm. This orientation prevents antigen shedding. It acts as a marker in lymphocytic leukemia and lymphocyte-predominant Hodgkin lymphoma and aids in targeting of monoclonal antibodies. The structure of CD20 receptor is shown in Fig.13.1e. CD20 is discovered in the pro-B stage of healthy mature B cells, in chronic lymphocytic leukemia and in Hodgkin lymphoma occurrences. CD20 is a component of cell surface complex which regulates the transfer of calcium (Ca2+) channel-based intracellular signaling pathway. However, interruption of the encoding of the Ca2+ channel gene shows no effect on the growth of B-cells or on the execution of immune responses.
3.6 CD44
CD44 is 37-kDa protein with three domains: extracellular, intracellular, and transmembrane domains (Fig.13.1f). The extracellular domain comprising a globular protein with amino terminal (~180 aa) serves as a ligand-binding receptor mainly for hyaluronic acid (HA), a negatively charged glycosaminoglycan. It has six cysteine residues that form three disulfide bonds and sites for N glycosylation of five conserved residues in the amino acid terminal of CD44. The unconserved extracellular domain is primarily linked with carbohydrate alteration (O-glycosylation), while alternative splicing enables inclusion of additional aa sequence taken from the CD44 gene’s variable exons. The transmembrane domain is useful in mediating HA binding.
Wide distribution of tissue and several isoforms enable CD44 to play a variety of biological functions as depicted in Fig.13.2.
4 Ligand Binding and Receptor-Mediated Signaling
4.1 CD3
Antigen-based stimulation results in conformational modifications in the CD3 polypeptide cytoplasmic tails triggered by stimulating MHC/TCR interaction with protein tyrosine kinase (PTKs). These PTKs, like Lck and Fyn, are members of the Src family. They phosphorylate conserved tyrosine residues that are present on the CD3 complex’s ITAMs, to produce a protein-docking site (Zeta-chain-associated protein kinase, ZAP 70). PTKs trigger interaction between MHC/TCR which leads to modified conformation of the CD3 polypeptides in the cytoplasmic tails after antigen stimulation. CD3-integrated ZAP-70 initiates phosphorylation of transmembrane protein that serves as a linker of T cells which are activated subsequently by association with phospholipase Cγ1 (PLCγ1). Cγ-dependent pathways include signals for calcium and diacylglycerol (DAG)-initiated responses, rearrangements in cytoskeletal rearrangements and integrin activation pathways that mediate cell-to-cell and cell-to-matrix interactions [20, 21].
4.2 CD4 and CD8
TCR produce signals which are amplified by CD4 and CD8 by using their intracellular domains. MHC II recognizes CD4 and MHC I recognizes CD8 which results in phosphorylation of MHC-based engagement of TCRαβ. CD4 and CD8 are thought to function as coreceptors and are present near the TCR in the membrane which increases physical association of Lck and brings them in close proximity with the tails of the CD3 chains. The Lck causes phosphorylation of the ITAMs in the CD3 tails which results in generation of cascading event-associated intracellular signaling that leads to T-cell activation.
4.3 CD19
CD19 is mostly located on B cell and acts as BCR-associated coreceptor that enhances BCR signaling. Two signaling pathways are followed after activating the antigen which include B-cell receptor (BCR)-dependent signaling and BCR-independent signaling. First pathway includes BCR ligation through tyrosine-based CD19 phosphorylation and recruiting src homology 2 (SH2) domain. On the other hand, the CD19 receptor serves as a subunit for signal transduction for the CD19/CD21 cluster in the second pathway. These immune complexes possessing C3dg and antigen would bridge CD21, and thereby CD19, to activate the B cell.
4.4 CD20
Antibody binding to CD20 initiates movement of molecules on to lipid rafts (membrane microdomains) which are rich in cholesterol and sphingolipids (Fig.13.1e). Lipid rafts aided signal transduction, enabling receptors and signaling effectors to colocalize [22].
4.5 CD44
The involvement of CD44-associated signaling with tumorigenesis is established through HA- independent or dependent signaling pathways. Binding of low molecular weight HA can block the oncogenic pathways associated with CD44 thereby enabling tumor suppression [23,24,25].
5 Structure Activity Relationship (SAR)
The SAR data are reported only for CD44 which is among the most investigated CD receptor and is discussed in this section. Glycosaminoglycans are repeating amino-associated disaccharide units that connect the chain to key proteins in the receptor. The glycoaminoglycans heparan sulfate and chondroitin sulfate are large molecules with sulfate and carboxylate groups that are charged with a large number of anionic groups. These anionic side chains exhibit affinity for cations. Different isoforms of CD44 seem to have distinctive glycosylation patterns. CD44s have a tiny portion of chondroitin sulfate, whereas the CD44 keratinocyte molecule (CD44v3–v10) is primarily glycosylated by heparan sulfate. CD44 isoforms occur in both glycosylated and nonglycosylated forms, indicating that some of the activities of the molecule do not depend on the side chains of glycosaminoglycans. Due to their degree of glycosylation, some CD44 isoforms exceed 200 kDa. Intermittent size isoforms (110–160 kDa) are mainly expressed on epithelial cells [26, 27].
6 Pathophysiological Features of CD
CD receptor’s expression in the pathogenesis of cancer and various infectious diseases are under investigation. Many studies have demonstrated CD expression-based regulation in various diseases. Some of the major diseases related to the pathophysiological significance of CD isoforms are discussed in this chapter.
6.1 Cancer
CD19 mediates establishment of intrinsic B-cell signaling thresholds by modifying B-cell-dependent and autonomous signaling. But CD19 is a less specific marker of B-cell lineage because CD20 is five times more expressed on B cell than CD19 antigen. CD20 is associated with chronic lymphocytic leukemia and in lymphocyte-predominant Hodgkin lymphoma. Likewise, researchers demonstrated the expression of CD20, a B-cell marker in thyroid cancers including classic papillary thyroid carcinomas and high-grade thyroid cancers [28]. Pancreatic ductal adenocarcinoma (PDAC) is the most common fatal cancer of pancreas. In PDAC, multiple immune responses and related pathways including phosphorylation of CD3 are associated with progression of pancreatic ductal adenocarcinoma [29, 30]. In pancreatic cancer, the CD44 variant isoform v6 (CD44v6) expression was found elevated, which is responsible for metastasis.
Conversion of expression from CD44v to CD44s was observed during breast cancer progression in murine model. Head and neck squamous cancer cell line was associated with overexpression of CD44v3 which lead to significant increase in cell migration. In gastrointestinal cancer, CD44v9 levels were found elevated in gastric adenocarcinoma, while the CD44v (v6–10, v7–10, v8–10) were primarily found in gastric tumors when studied in the transgenic mice model of gastric carcinogenesis [31].
6.2 HIV
The human immunodeficiency virus type 1 (HIV-1) encephalitis causes damage to the brain by longstanding HIV infection, in which predominant cells like monocytes/macrophages are available. Angiocentric CD3+ T-cell-based endothelial injury resulted in infection of the child brain with HIV via the blood-brain barrier [32]. HIV-infection-based reduction in CD4+ T cell gradually affects immune cell homeostasis which may cause death. HIV replicates by binding to the CD4 molecule on the outer body of Th cells which leads to destruction of CD4+ T cells and gradual reduction in number of T cell [33]. While CD4 levels decline, the expansion in CD8 T cells, which occurs resulting in disturbances of the T-cell compartment, is attributed to the severe symptoms seen in HIV-infected patients. Dysregulation in the levels of CD4 and CD8 provide insights into the immunological response to acute HIV infection. CD4:CD8 ratios have profound effect on HIV disease progression which marks imbalance in CD4 T-cell regeneration and persistently elevated CD8 T-cell counts [34].
6.3 Tuberculosis
CD4 and CD8 T cell have significant role in protection from Mycobacterium tuberculosis [35,36,37]. Several reports suggest that CD4+ T cells exert a profound role in protection against Mycobacterium tuberculosis than CD8+ T cell. CD4+ T cells have several subsets, like Th1, Th2, Th17, and regulatory T cells, and all these subsets come together to enable infection management. Some CD4 subsets may distinguish between active and dormant forms in mycobacterium tuberculosis infection. CD4+ Th1 cell-based defense mechanism against infection leads to secretion of cytokines like interferon-gamma (IFN-γ) or tumor necrosis factor (TNF-α) which are involved in the recruitment and activation of monocytes and granulocytes [38].
7 Antagonist for Ligand Binding
The antagonists of CD are group of antibodies, antigen-binding portions of antibodies, small organic molecules, aptamers, or polypeptides. The efficacy of anti-CD antibodies against various cancers and HIV has been well studied. Studies with such antagonist are summarized in Table 13.1.
8 Ligands Explored
8.1 Osteopontin (OPN)
OPN binding induces CD44-mediated cell signaling which results in tumor suppression and metastasis. OPN and CD44 expression revealed positive correlation in 159 non-small cell lung cancers and 243 gastric cancer patients’ tissues. CD44 knock-down or anti-CD44 antibody reduces the secretion of OPN which prevented OPN-activated c-jun-NH2-kinase signals leading to a reduction in colorectal cancer cells clonogenicity [51, 52].
8.2 Chondroitin Sulfate (CS)
CS potentiated efficacy of gemcitabine by enhancing inhibition of bladder cancer cells. CS-g-polymer-based camptothecin micelles exhibited dual receptor-mediated uptake mechanism through CD44 via clathrin-mediated endocytosis and exhibited potentiated effect in lung cancer cells compared to free drug [53, 54].
9 Receptor-Mediated Targeting Strategies
Targeting to immune cell subsets such as CD receptor which are overexpressed in tumor conditions are more beneficial than attempts to target cancer cells directly because immune cells subsets can migrate actively into cancer cells [55]. Antibody-conjugated drugs (ADC) are considered as new therapeutics for cancer treatment and infectious diseases that comprise of CD-antibody which can specifically target disease-associated CD antigen conjugated with drug. The efficacy of ADC highly depends on intracellular-uptake-enabled apoptosis of diseased cells. Antibody-conjugated drug is internalized through receptor-mediated endocytosis, that is, clathrin/caveolae-mediated endocytosis [56,57,58].
9.1 Prodrugs
Targeted antibody-mediated prodrug therapy is an approach wherein the antibody recognizes the tumor site to enable localization following which enzymes at the site will hydrolyze the prodrug to release the anticancer agent in the tumor [59, 60]. Such antibody-directed enzyme prodrug therapy (ADEPT) provides many advantages such as amplification (increase the number of drug molecules at site of action), has bystander effect (ability of drug molecule to diffuse to neighboring cells), reduce systemic side effects and potential to overcome drug resistance [61].
Chimeric anti-CD20 antibody are highly effective in the therapy of B-cell malignancies and non-Hodgkin lymphoma (NHL) and chronic lymphocytic leukemia (CLL) either individually or as combinatorial approach with other chemotherapy treatments [62]. For example, Haisma et al. demonstrated antibody-mediated enzyme prodrug therapy by engineering monochain of fusion protein Anti-CD20 antibody and human β-Glucuronidase enzyme to convert a prodrug N-[4-doxorubicin (DOX)-N-carbonyl(-oxy ethyl) phenyl] O-β-glucuronyl carbamate into DOX at the tumor site [63].
9.2 Drug Conjugates
Conjugates can be prepared by reaction between polymer and targeting antibody/proteins or therapeutic cargoes like drug and antigens. Release of the therapeutic cargo from the conjugates at the targeted site is mediated by intracellular lysosomal enzymes after cell internalization. DOX conjugated to a copolymer of N- (2-hydroxypropyl) methacrylamide (HPMA) linked with targeting antibody such as anti-CD4, anti-CD71, reduced the MDR of DOX [64]. Targetable anti-CD3 antibody DOX-N-(2-hydroxypropyl) conjugate revealed inhibition of proliferation of human T cell and peripheral-blood lymphocyte [65]. Neomycin B-arginine conjugate (NeoR) showed 30-fold enhanced potency by inhibiting HIV particle binding to CD4 in HIV-1 strains R5 and X4 [66]. Human serum albumin (HSA)-CD4 hybrid revealed comparable in vitro binding and antiviral properties with 140-fold higher elimination half-life compared to soluble CD4 in rabbit model [67]. In another study, SAR3419 an anti-CD19 antibody was attached to the DM4 (maytansine derivative) via a cleavable disulfide linker. Mice xenograft-model-based preclinical study of maytansine derivative–anti-CD19 conjugate followed by conduction of Phase I trials revealed antitumor efficacy with acceptable safety in human B-cell lymphoma models [68]. The conjugation of proteins and DNAs or peptide nucleic acids (PNAs) has also been explored. A tetramer of anti-CD20-Fab conjugated with PNAs showed in vitro potent and specific cytotoxicity followed by induction of apoptosis of CD20+ Ramos cells [69].
9.3 Nanocarriers
9.3.1 Liposomes
Liposomes are lipid bilayer vesicles made up of natural or synthetic lipid which are used for active targeting by functionalizing with ligand. Targeted-liposome delivery of drugs enhances the interaction with the target cells by fusion with the cell membrane surface or internalization by endocytosis. Antibody-combined liposomes called immunoliposomes can be prepared by antibody lipid conjugates, covalently attaching antibody to liposomes or by adsorption on the liposomal surface.
Vaidya et al. developed tri-functional immunoliposome (TFIL) by conjugating Trastuzumab (anti-human epidermal growth factor receptor-2) and OKT-3 (anti-CD3) antibodies to DOX-loaded liposome using the micelle transfer method. TFIL revealed good cytotoxicity in breast cancer tumor cells by activating immune cells (T lymphocyte) [70]. Ishida et al. prepared sterically stabilized immunoliposomes (SIL) by attaching anti-CD19 antibody to PEG lipid derivatives which revealed stealth property enabled threefold enhancement in liposomal association efficiency with CD19+ human B cell lymphoma cells [71]. Theresa et al. demonstrated that anti-CD19 antibody-conjugated liposomal DOX improved the therapeutic efficiency without significant toxicity in immunodeficient (SCID) mice inoculated with human B-cell lymphoma (Namalwa) cells [72]. Flasher et al. examined binding ability of soluble CD4-conjugated liposomes to glycoprotein gpl20 of HIV-infected cell and revealed high association efficiency compared to unconjugated liposomes [73]. Glycosylphosphatidylinositol (GPI)-anchored form of gp120 of HIV-1 which employed GPI signal of decay acceleration factor (DAF) revealed spontaneous insertion into liposome membrane using GPI anchor. This liposome exhibited specific binding to CD4. A succinct summary of other liposome-based CD44 receptor targeting for cancer is provided in Table 13.2.
9.3.2 Nanoparticles
The diversity and physical, chemical, and biological versatility of nanoparticles can be exploited for use in targeted cancer and infectious disease therapy. The specificity of antibody-conjugated nanoparticles can be exploited to focus the delivery of drug to targeted cells overexpressing the targeted surface antigen. Biotinylated-anti-CD3 antibodies conjugated with gelatin nanoparticles are reported to achieve specific receptor-mediated endocytic cellular uptake into human T-cell leukemia cells [78]. The targeting ability of anti-human CD8 antibody coupled with PLGA (poly(lactic-co-glycolic acid) nanoparticles to CD8 expressing mammalian cells was confirmed by the presence of anti-CD8-conjugated nanoparticles in cells within 1 h while unconjugated nanoparticles took 48 h [79]. Immunonanoparticles obtained by surface functionalization of paclitaxel-loaded polymeric nanoparticles with anti-HER2 (Herceptin®) and anti-CD20 (Mabthera®) antibodies demonstrated improved anticancer drug efficacy due to active targeting using immune nanoparticles [80].
CD44 is among the more extensively evaluated receptors for targeted delivery in cancer therapy. Strategies employing CD44 targeted nanoparticles for drug delivery in cancer are enlisted in Table 13.2.
9.3.3 Micelles
Micelles are nanoscopic structures, less than 100 nm described by a hydrophobic core structure in the center and are formed by self-assembly of amphiphilic copolymers in aqueous media above a concentration called the critical micelle concentration (CMC). DOX-loaded micelles conjugated with hyaluronic acid (HA)-grafted with folic acid developed to target CD44-positive tumor, revealed significant enhancement in cellular uptake by CD44 receptor-mediated endocytosis, and promising tumor targeting in HCCLM3 (human hepatocellular carcinoma cell line) tumor-bearing nude mice [87]. In tumor-associated tissue, various glycans are often overexpressed as compared to normal tissues, which can be targeted for tumor therapy [88, 89]. Agrawal et al. conjugated hyaluronic acid with DOX-loaded PEG–PLGA (polyethylene glycol–poly lactic acid-co-glycolic acid) micelles to improve targeting in CD44 overexpressed in the Ehrlich ascites tumor-bearing mice. The developed system revealed high efficacy and also blood circulation longevity which could have facilitated high tumor accumulation [90].
9.3.4 Solid Lipid Nanoparticles (SLN)
Receptor-mediated targeting strategies for cancer or infected cells using SLN have specific applications for delivering hydrophobic cargos. For instance, Shen et al. developed paclitaxel- loaded HA-coated SLNs which provided effective intracellular delivery of paclitaxel and induced apoptosis in CD44+ cells in vitro, while in vivo study demonstrated selectively enhanced targeting in CD44 overexpressed tumor-bearing lung tissues along with enhanced antitumor activity at low doses of paclitaxel [91]. Indinavir-lipid nanoparticles (LNP) were engineered for surface modification with two CD4 binding peptides (BP4 and BP2). These CD4-binding peptides coupled on LNPs led to blockage of CD4 with considerably enhanced anti-HIV activity [92].
9.3.5 Miscellaneous
9.3.5.1 Nanosheets
Li et al. have demonstrated HA-conjugated Graphene oxide (GO) sheets loaded with a photosensitizer Chlorine6 (Ce6). Nanohybrids of HA–GO/Ce6 revealed a significantly rapid and tenfold enhanced uptake in HeLa cancer cell line in comparison to free Ce6 which was ascribed to HA-facilitated CD44-receptor-mediated endocytosis [93].
9.3.5.2 Scaffolds
Tumor-specific, anti-CD20-bound paclitaxel-loaded albumin scaffold was engineered. In vivo biodistribution study showed greater therapeutic potential than only anti-CD20 and paclitaxel-loaded albumin scaffold. Preclinical testing of this formulation demonstrated increased deposition of antibody-mediated drug in the tumor, justifying translation for clinical evaluation of this nano-antibody-targeted chemotherapy [94].
9.3.5.3 Nanoparticles as Theranostics
Molecular imaging with targeted drug delivery in cancer has been extensively used for effective therapy and diagnosis [95]. For instance, Jiefu Jin et al. studied CD44 targeted mAb (monoclonal antibody) photosensitizer complex for simultaneous detection with photo-induced therapy (PIT) in the CD44-positive triple negative xenograft model of breast cancer (TNBC) and found it promising [95]. Liposomes were loaded with DOX or a triple fusion (TF) gene containing the truncated thymidine kinase (HSV-ttk) of herpes simplex virus and the red fluorescent protein (RFP) renilla luciferase (Rluc) for imaging. These Anti-CD44 antibody-conjugated liposomes ensured targeting of CD44 hepatocellular carcinoma cells with good cytotoxicity and also revealed delay in growth of hepatocellular tumor [96]. Capolla et al. developed anti-CD20-conjugated biodegradable nanoparticles for animal imaging with drug delivery to cancerous cells. The nanoparticles exhibited good binding specificity with MEC1 cells and chronic lymphocytic leukemia patient’s cells. In vivo study proposed that the anti-CD20-conjugated nanoparticles improved tumor pharmacokinetic profiles and enhanced tumor imaging compared to nontargeted nanoparticles in human/mouse model of B-cell malignancy [97].
9.4 Clinical Studies
Monoclonal antibodies are considered as an emerging class of pharmaceuticals for targeted therapy of many human diseases such as cancer, HIV or other infectious diseases. Although many antibody-targeting strategies are developing and five antibodies are now approved for cancer or infectious diseases, more approvals are expected from among the 20 or so antibodies currently in clinical development. The efficacy of anticancer drug by targeting to site of action is being met by the exploration of a wide range CD-antigen-targeted strategies, however, there is clinical need to increase the safety [98]. In clinical trials, Besponsa® and Mylotarg™ are recently approved and >50 ADCs, which are in various phases of clinical trial as monotherapy or in combination with other anticancer drug for treatment of several types of cancer, show desirable results [99]. Clinical trial status with these receptor-mediated antibodies is listed in Table 13.3.
9.5 Advantages and Limitations
CD receptor-mediated treatments for infections and cancer revealed targeting based enhancement in efficacy which could result in long-term survival and eventual care of such diseases [105–106]. Anti-CD chemotherapeutic monoclonal antibodies (CmAbs) possess generally mild adverse effects compared to standard chemotherapy, while conjugated CmAbs precipitate serious adverse effects. These adverse effects are usually associated with the antigens which they are targeting and with the intravenous route of administration [106]. For example, bevacizumab targets tumor growth factor in the blood vessels and produces adverse effects such as high blood pressure and renal damage [107]. Rituximab treatment has infusion-related responses such as syndrome of cytokine release and syndrome of tumor lysis [108]. Other negative reactions prevalent with most CmAbs include chills, weakness, headache, nausea, vomiting, diarrhea, hypotension, and eruption.
Although excellent progress is evident in the field of antibody engineering and cancer therapy, manufacturing costs are approximately twice the price of conventional medicines [109]. There is no doubt that CmAbs engineering has marked a major milestone in cancer therapy, and with the success rate of marketing these drugs better than that of small molecular drugs, pharmaceutical companies are anticipated to continue to move toward more specific, less harmful, and more cost-effective CmAb.
10 Conclusion
CD receptor-targeted drug delivery provides tremendous scope in clinical application. Targeting the overexpressed CD receptor represents an exciting novel approach for infectious diseases and cancer.
Abbreviations
- ADC:
-
Antibody-conjugated drug
- Anti-EpCAM:
-
Human epithelial adhesion molecule
- BCR:
-
B-cell receptor
- BP:
-
Binding peptide
- Ca2+:
-
Calcium
- CD:
-
Cluster of differentiation
- Ce6:
-
Chlorine 6
- CLL:
-
Chronic lymphocytic leukemia
- CmAbs:
-
Chemotherapeutic monoclonal antibodies
- CMC:
-
Critical micelle concentration
- CR3:
-
Complement receptor
- CS:
-
Chondroitin sulfate
- CTCL:
-
Cutaneous T-cell lymphoma
- CTLs:
-
Cytotoxic T lymphocytes
- DAF:
-
Decay acceleration factor
- DM4:
-
Maytansine derivative 4
- DOX:
-
Doxorubicin
- Fcgr:
-
Fcgamma receptor
- GEM:
-
Gemcitabine
- GO:
-
Graphene oxide
- GP120:
-
Envelope glycoprotein
- GPI:
-
glycosylphosphatidylinositol
- HA:
-
Hyaluronic acid
- HSA:
-
Human serum albumin
- HCCLM3:
-
Human hepatocellular carcinoma cell line
- HCT-116:
-
Human colorectal carcinoma cell line
- HepG2:
-
Liver hepatocellular carcinoma
- HIV-1:
-
Human immunodeficiency virus type 1
- HPMA:
-
N- (2-hydroxypropyl) methacrylamide
- HSV-ttk:
-
Herpes simplex virus truncated thymidine kinase
- IFN-γ:
-
Interferon gamma
- Ig:
-
Immunoglobin
- ITAMs:
-
Immunoreceptor tyrosine-based activation motifs
- Lck:
-
Lymphocyte-specific protein tyrosine kinase
- LNP:
-
Indinavir-lipid nanoparticles
- mAb:
-
Monoclonal antibody
- MDA-MB-231:
-
M.D. Anderson and MB stands for Metastasis Breast 231
- MDR:
-
Multidrug resistance
- MHC:
-
Major histocompatibility complex
- MS4A1:
-
Membrane Spanning 4-Domains A1
- MSNs:
-
Mesoporous silica nanoparticles
- MTX:
-
Mitoxantrone
- NeoR:
-
Neomycin B-arginine conjugate
- NHL:
-
non-Hodgkin lymphoma
- OPN:
-
Osteopontin
- PDAC:
-
Pancreatic ductal adenocarcinoma
- PEG-PLGA:
-
Polyethylene glycol–poly lactic acid-co-glycolic acid
- PEG–PLGA:
-
Polyethylene glycol–poly lactic acid-co-glycolic acid
- PIT:
-
Photo-induced therapy
- pMHC:
-
Peptide-major histocompatibility complex
- PNA:
-
Peptide nucleic acids
- PTKs:
-
Protein tyrosine kinase
- PTX:
-
Paclitaxel
- RFP:
-
Red fluorescent protein
- Rluc:
-
Renilla luciferase
- SCID:
-
Significant toxicity immunodeficient
- SH2:
-
src homology 2
- SLN:
-
Solid lipid nanoparticle
- TCR:
-
T-cell receptor
- TF:
-
Triple fusion
- TFIL:
-
Tri-functional immunoliposome
- Th:
-
T helper
- TNBC:
-
Triple negative xenograft model of breast cancer
- TNF-α:
-
Tumor necrosis factor alpha
- ZAP 70:
-
Zeta-chain-associated protein kinase
References
Zola H, editor. Medical applications of leukocyte surface molecules—the CD molecules. Molecular medicine. Springer; 2006. New York, USA.
Bernard A, Boumsell L, Dausset J, Milstein C, Schlossman SF. Leucocyte typing: human leucocyte differentiation antigens detected by monoclonal antibodies. Specification-classification-nomenclature/Typage leucocytaire Antigenes de differenciation leucocytaire humains reveles par lesanticorps monoclonaux: Rapports des etudes com. Springer Science & Business Media; 2013.
Erber WN. Human leucocyte differentiation antigens: review of the CD nomenclature. Pathology. 1990;22(2):61–9.
Zola H, Swart B, Nicholson I, Aasted B, Bensussan A, Boumsell L, et al. CD molecules 2005: human cell differentiation molecules. Blood. 2005;106(9):3123–6.
Zola H, Swart B, Banham A, Barry S, Beare A, Bensussan A, et al. CD molecules 2006—human cell differentiation molecules. J Immunol Methods. 2007;319(1–2):1–5.
Prchal J, Levi MM. Williams hematology. New York: The McGraw-Hill Companies; 2010.
Chetty R, Gatter K. CD3: structure, function, and role of immunostaining in clinical practice. J Pathol. 1994;173(4):303–7.
Alarcon B, Berkhout B, Breitmeyer J, Terhorst C. Assembly of the human T cell receptor-CD3 complex takes place in the endoplasmic reticulum and involves intermediary complexes between the CD3-gamma. delta. epsilon core and single T cell receptor alpha or beta chains. J Biol Chem. 1988;263(6):2953–61.
Clevers H, Alarcon B, Wileman T, Terhorst C. The T cell receptor/CD3 complex: a dynamic protein ensemble. Annu Rev Immunol. 1988;6(1):629–62.
Garcia KC, Adams JJ, Feng D, Ely LK. The molecular basis of TCR germline bias for MHC is surprisingly simple. Nat Immunol. 2009;10(2):143.
Godfrey DI, Rossjohn J, McCluskey J. The fidelity, occasional promiscuity, and versatility of T cell receptor recognition. Immunity. 2008;28(3):304–14.
Krangel MS. Mechanics of T cell receptor gene rearrangement. Curr Opin Immunol. 2009;21(2):133–9.
Marrack P, Scott-Browne JP, Dai S, Gapin L, Kappler JW. Evolutionarily conserved amino acids that control TCR-MHC interaction. Annu Rev Immunol. 2008;26:171–203.
Morris GP, Allen PM. How the TCR balances sensitivity and specificity for the recognition of self and pathogens. Nat Immunol. 2012;13(2):121.
Van Der Merwe PA, Dushek O. Mechanisms for T cell receptor triggering. Nat Rev Immunol. 2011;11(1):47.
Littman DR. The structure of the CD4 and CD8 genes. Annu Rev Immunol. 1987;5(1):561–84.
Ellmeier W, Sawada S, Littman DR. The regulation of CD4 and CD8 coreceptor gene expression during T cell development. Annu Rev Immunol. 1999;17(1):523–54.
Rudd CE. CD4, CD8 and the TCR-CD3 complex: a novel class of protein-tyrosine kinase receptor. Immunol Today. 1990;11:400–6.
Zhou L-J, Ord DC, Hughes AL, Tedder TF. Structure and domain organization of the CD19 antigen of human, mouse, and guinea pig B lymphocytes. Conservation of the extensive cytoplasmic domain. J Immunol. 1991;147(4):1424–32.
Pitcher LA, Van Oers NS. T-cell receptor signal transmission: who gives an ITAM? Trends Immunol. 2003;24(10):554–60.
Smith-Garvin JE, Koretzky GA, Jordan MS. T cell activation. Annu Rev Immunol. 2009;27:591–619.
Cartron G, Watier H, Golay J, Solal-Celigny P. From the bench to the bedside: ways to improve rituximab efficacy. Blood. 2004;104(9):2635–42.
Louderbough JM, Schroeder JA. Understanding the dual nature of CD44 in breast cancer progression. Mol Cancer Res. 2011;9(12):1573–86.
Louderbough JM, Brown JA, Nagle RB, Schroeder JA. CD44 promotes epithelial mammary gland development and exhibits altered localization during cancer progression. Genes Cancer. 2011;2(8):771–81.
Misra S, Heldin P, Hascall VC, Karamanos NK, Skandalis SS, Markwald RR, et al. Hyaluronan–CD44 interactions as potential targets for cancer therapy. FEBS J. 2011;278(9):1429–43.
Naor D, Sionov RV, Ish-Shalom D. CD44: structure, function and association with the malignant process. Adv Cancer Res. 1997;71:241–319; Elsevier.
Sneath R, Mangham D. The normal structure and function of CD44 and its role in neoplasia. Mol Pathol. 1998;51(4):191.
Bychkov A, Jung CK. Aberrant expression of CD20 in thyroid cancer and its clinicopathologic significance. Hum Pathol. 2018;71:74–83.
Khatri I, Ganguly K, Sharma S, Carmicheal J, Kaur S, Batra SK, et al. Systems biology approach to identify novel genomic determinants for pancreatic cancer pathogenesis. Sci Rep. 2019;9(1):123.
Fedorchenko O, Stiefelhagen M, Peer-Zada AA, Barthel R, Mayer P, Eckei L, et al. CD44 regulates the apoptotic response and promotes disease development in chronic lymphocytic leukemia. Blood. 2013;121(20):4126–36.
Chen C, Zhao S, Karnad A, Freeman JW. The biology and role of CD44 in cancer progression: therapeutic implications. J Hematol Oncol. 2018;11(1):64.
Katsetos CD, Fincke JE, Legido A, Lischner HW, de Chadarevian J-P, Kaye EM, et al. Angiocentric CD3+ T-cell infiltrates in human immunodeficiency virus type 1-associated central nervous system disease in children. Clin Diagn Lab Immunol. 1999;6(1):105–14.
Vidya Vijayan K, Karthigeyan KP, Tripathi SP, Hanna LE. Pathophysiology of CD4+ T-cell depletion in HIV-1 and HIV-2 infections. Front Immunol. 2017;8:580.
Pahwa S, Read JS, Yin W, Matthews Y, Shearer W, Diaz C, et al. CD4/CD8 ratio for diagnosis of HIV-1 infection in infants: the Women and Infants Transmission Study. Pediatrics. 2008;122(2):331.
Flynn JL, Goldstein MM, Triebold KJ, Koller B, Bloom BR. Major histocompatibility complex class I-restricted T cells are required for resistance to Mycobacterium tuberculosis infection. Proc Natl Acad Sci. 1992;89(24):12013–7.
Tascon RE, Stavropoulos E, Lukacs KV, Colston MJ. Protection against Mycobacterium tuberculosis infection by CD8+ T cells requires the production of gamma interferon. Infect Immun. 1998;66(2):830–4.
Stenger S, Modlin RL. T cell mediated immunity to Mycobacterium tuberculosis. Curr Opin Microbiol. 1999;2(1):89–93.
Prezzemolo T, Guggino G, La Manna MP, Di Liberto D, Dieli F, Caccamo N. Functional signatures of human CD4 and CD8 T cell responses to Mycobacterium tuberculosis. Front Immunol. 2014;5:180.
Bolt S, Routledge E, Lloyd I, Chatenoud L, Pope H, Gorman SD, et al. The generation of a humanized, non-mitogenic CD3 monoclonal antibody which retains in vitro immunosuppressive properties. Eur J Immunol. 1993;23(2):403–11.
Carpenter PA, Appelbaum FR, Corey L, Deeg HJ, Doney K, Gooley T, et al. A humanized non–FcR-binding anti-CD3 antibody, visilizumab, for treatment of steroid-refractory acute graft-versus-host disease. Blood. 2002;99(8):2712–9.
Bruno CJ, Jacobson JM. Ibalizumab: an anti-CD4 monoclonal antibody for the treatment of HIV-1 infection. J Antimicrob Chemother. 2010;65(9):1839–41.
Kuritzkes DR, Jacobson J, Powderly WG, Godofsky E, DeJesus E, Haas F, et al. Antiretroviral activity of the anti-CD4 monoclonal antibody TNX-355 in patients infected with HIV type 1. J Infect Dis. 2004;189(2):286–91.
Rider DA, Havenith CE, de Ridder R, Schuurman J, Favre C, Cooper JC, et al. A human CD4 monoclonal antibody for the treatment of T-cell lymphoma combines inhibition of T-cell signaling by a dual mechanism with potent Fc-dependent effector activity. Cancer Res. 2007;67(20):9945–53.
Reusch U, Duell J, Ellwanger K, Herbrecht C, Knackmuss SH, Fucek I, et al., editors. A tetravalent bispecific TandAb (CD19/CD3), AFM11, efficiently recruits T cells for the potent lysis of CD19+ tumor cells. MAbs; 2015: Taylor & Francis. Oxfordshire United Kingdom
Breton CS, Nahimana A, Aubry D, Macoin J, Moretti P, Bertschinger M, et al. A novel anti-CD19 monoclonal antibody (GBR 401) with high killing activity against B cell malignancies. J Hematol Oncol. 2014;7(1):33.
Blanc V, Bousseau A, Caron A, Carrez C, Lutz RJ, Lambert JM. SAR3419: an anti-CD19-Maytansinoid immunoconjugate for the treatment of B-cell malignancies. Clin Cancer Res. 2011;17(20):6448–58.
Sun X, Widdison W, Mayo M, Wilhelm S, Leece B, Chari R, et al. Design of antibody− maytansinoid conjugates allows for efficient detoxification via liver metabolism. Bioconjug Chem. 2011;22(4):728–35.
Kiprijanov SM. Bispecific antibodies and immune therapy targeting. Drug Deliv Oncol. 2012:441–82.
Lin TS. Ofatumumab: a novel monoclonal anti-CD20 antibody. Pharmgenomics Pers Med. 2010;3:51.
Mott PJ, Lazarus AH. CD44 antibodies and immune thrombocytopenia in the amelioration of murine inflammatory arthritis. PLoS One. 2013;8(6):e65805.
Rao G, Wang H, Li B, Huang L, Xue D, Wang X, et al. Reciprocal interactions between tumor-associated macrophages and CD44-positive cancer cells via osteopontin/CD44 promote tumorigenicity in colorectal cancer. Clin Cancer Res. 2013;19(4):785–97.
Pietras A, Katz AM, Ekström EJ, Wee B, Halliday JJ, Pitter KL, et al. Osteopontin-CD44 signaling in the glioma perivascular niche enhances cancer stem cell phenotypes and promotes aggressive tumor growth. Cell Stem Cell. 2014;14(3):357–69.
Ferro M, Giuberti G, Zappavigna S, Perdonà S, Facchini G, Sperlongano P, et al. Chondroitin sulphate enhances the antitumor activity of gemcitabine and mitomycin-C in bladder cancer cells with different mechanisms. Oncol Rep. 2012;27(2):409–15.
Liu Y-S, Chiu C-C, Chen H-Y, Chen S-H, Wang L-F. Preparation of chondroitin sulfate-g-poly (ε-caprolactone) copolymers as a CD44-targeted vehicle for enhanced intracellular uptake. Mol Pharm. 2014;11(4):1164–75.
Schmid D, Park CG, Hartl CA, Subedi N, Cartwright AN, Puerto RB, et al. T cell-targeting nanoparticles focus delivery of immunotherapy to improve antitumor immunity. Nat Commun. 2017;8(1):1747.
Chalouni C, Doll S. Fate of antibody-drug conjugates in cancer cells. J Exp Clin Cancer Res. 2018;37(1):20.
Hellmann I, Waldmeier L, Bannwarth-Escher M-C, Maslova K, Wolter FI, Grawunder U, et al. Novel antibody drug conjugates targeting tumor-associated receptor tyrosine kinase ROR2 by functional screening of fully human antibody libraries using Transpo-mAb display on progenitor B cells. Front Immunol. 2018;9:2490.
Kalim M, Chen J, Wang S, Lin C, Ullah S, Liang K, et al. Intracellular trafficking of new anticancer therapeutics: antibody–drug conjugates. Drug Des Devel Ther. 2017;11:2265.
Niculescu-Duvaz I, Springer C. Antibody-directed enzyme prodrug therapy (ADEPT): a review. Adv Drug Deliv Rev. 1997;26(2–3):151–72.
Xu G, McLeod HL. Strategies for enzyme/prodrug cancer therapy. Clin Cancer Res. 2001;7(11):3314–24.
Bagshawe KD. Antibody-directed enzyme prodrug therapy. In: Prodrugs: Springer; 2007. p. 525–40. New York, USA
Hammer O, editor. CD19 as an attractive target for antibody-based therapy. MAbs; 2012: Taylor & Francis. Oxfordshire United Kingdom
Haisma HJ, Sernee MF, Hooijberg E, Brakenhoff RH, vd Meulen-Muileman IH, Pinedo HM, et al. Construction and characterization of a fusion protein of single-chain anti-CD20 antibody and human β-glucuronidase for antibody-directed enzyme prodrug therapy. Blood. 1998;92(1):184–90.
Št’astný M, Strohalm J, Plocova D, Ulbrich K, Řı́hová B. A possibility to overcome P-glycoprotein (PGP)-mediated multidrug resistance by antibody-targeted drugs conjugated to N-(2-hydroxypropyl) methacrylamide (HPMA) copolymer carrier. Eur J Cancer. 1999;35(3):459–66.
Ulbrich K, Strohalm J, Šubr V, Plocová D, Duncan R, Říhová B, editors. Polymeric conjugates of drugs and antibodies for site-specific drug delivery. Macromolecular Symposia; 1996: Wiley Online Library. New Jersey,USA
Cabrera C, Gutiérrez A, Barretina J, Blanco J, Litovchick A, Lapidot A, et al. Anti-HIV activity of a novel aminoglycoside-arginine conjugate. Antivir Res. 2002;53(1):1–8.
Yeh P, Landais D, Lemaitre M, Maury I, Crenne J-Y, Becquart J, et al. Design of yeast-secreted albumin derivatives for human therapy: biological and antiviral properties of a serum albumin-CD4 genetic conjugate. Proc Natl Acad Sci. 1992;89(5):1904–8.
Raufi A, Ebrahim AS, Al-Katib A. Targeting CD19 in B-cell lymphoma: emerging role of SAR3419. Cancer Manag Res. 2013;5:225.
Kazane SA, Axup JY, Kim CH, Ciobanu M, Wold ED, Barluenga S, et al. Self-assembled antibody multimers through peptide nucleic acid conjugation. J Am Chem Soc. 2012;135(1):340–6.
Vaidya T, Straubinger RM, Ait-Oudhia S. Development and evaluation of tri-functional immunoliposomes for the treatment of HER2 positive breast cancer. Pharm Res. 2018;35(5):95.
Ishida T, Iden DL, Allen TM. A combinatorial approach to producing sterically stabilized (stealth) immunoliposomal drugs. FEBS Lett. 1999;460(1):129–33.
Allen TM, Mumbengegwi DR, Charrois GJ. Anti-CD19-targeted liposomal doxorubicin improves the therapeutic efficacy in murine B-cell lymphoma and ameliorates the toxicity of liposomes with varying drug release rates. Clin Cancer Res. 2005;11(9):3567–73.
Flasher D, Konopka K, Chamow SM, Dazin P, Ashkenazi A, Pretzer E, et al. Liposome targeting to human immunodeficiency virus type 1-infected cells via recombinant soluble CD4 and CD4 immunoadhesin (CD4-IgG). Biochim Biophys Acta Biomembr. 1994;1194(1):185–96.
Lu L, Ding Y, Zhang Y, Ho RJ, Zhao Y, Zhang T, et al. Antibody-modified liposomes for tumor-targeting delivery of timosaponin AIII. Int J Nanomedicine. 2018;13:1927.
Eliaz RE, Szoka FC. Liposome-encapsulated doxorubicin targeted to CD44: a strategy to kill CD44-overexpressing tumor cells. Cancer Res. 2001;61(6):2592–601.
Jiang T, Zhang Z, Zhang Y, Lv H, Zhou J, Li C, et al. Dual-functional liposomes based on pH-responsive cell-penetrating peptide and hyaluronic acid for tumor-targeted anticancer drug delivery. Biomaterials. 2012;33(36):9246–58.
Alshaer W, Hillaireau H, Vergnaud J, Ismail S, Fattal E. Functionalizing liposomes with anti-CD44 aptamer for selective targeting of cancer cells. Bioconjug Chem. 2014;26(7):1307–13.
Dinauer N, Balthasar S, Weber C, Kreuter J, Langer K, von Briesen H. Selective targeting of antibody-conjugated nanoparticles to leukemic cells and primary T-lymphocytes. Biomaterials. 2005;26(29):5898–906.
Bicho A, Peça IN, Roque A, Cardoso MM. Anti-CD8 conjugated nanoparticles to target mammalian cells expressing CD8. Int J Pharm. 2010;399(1–2):80–6.
Cirstoiu-Hapca A, Bossy-Nobs L, Buchegger F, Gurny R, Delie F. Differential tumor cell targeting of anti-HER2 (Herceptin®) and anti-CD20 (Mabthera®) coupled nanoparticles. Int J Pharm. 2007;331(2):190–6.
Sargazi A, Shiri F, Keikha S, Majd MH. Hyaluronan magnetic nanoparticle for mitoxantrone delivery toward CD44-positive cancer cells. Colloids Surf B: Biointerfaces. 2018;171:150–8.
Hosseinzadeh H, Atyabi F, Varnamkhasti BS, Hosseinzadeh R, Ostad SN, Ghahremani MH, et al. SN38 conjugated hyaluronic acid gold nanoparticles as a novel system against metastatic colon cancer cells. Int J Pharm. 2017;526(1–2):339–52.
Yu M, Jambhrunkar S, Thorn P, Chen J, Gu W, Yu C. Hyaluronic acid modified mesoporous silica nanoparticles for targeted drug delivery to CD44-overexpressing cancer cells. Nanoscale. 2013;5(1):178–83.
Chen Z, Li Z, Lin Y, Yin M, Ren J, Qu X. Bioresponsive hyaluronic acid-capped mesoporous silica nanoparticles for targeted drug delivery. Chem Eur J. 2013;19(5):1778–83.
Xu C, He W, Lv Y, Qin C, Shen L, Yin L. Self-assembled nanoparticles from hyaluronic acid–paclitaxel prodrugs for direct cytosolic delivery and enhanced antitumor activity. Int J Pharm. 2015;493(1–2):172–81.
Li J, Huo M, Wang J, Zhou J, Mohammad JM, Zhang Y, et al. Redox-sensitive micelles self-assembled from amphiphilic hyaluronic acid-deoxycholic acid conjugates for targeted intracellular delivery of paclitaxel. Biomaterials. 2012;33(7):2310–20.
Yang Y, Zhao Y, Lan J, Kang Y, Zhang T, Ding Y, et al. Reduction-sensitive CD44 receptor-targeted hyaluronic acid derivative micelles for doxorubicin delivery. Int J Nanomedicine. 2018;13:4361.
Wu R-L, Sedlmeier G, Kyjacova L, Schmaus A, Philipp J, Thiele W, et al. Hyaluronic acid-CD44 interactions promote BMP4/7-dependent Id1/3 expression in melanoma cells. Sci Rep. 2018;8(1):14913.
Chen S, Yang K, Tuguntaev RG, Mozhi A, Zhang J, Wang PC, et al. Targeting tumor microenvironment with PEG-based amphiphilic nanoparticles to overcome chemoresistance. Nanomedicine. 2016;12(2):269–86.
Yadav AK, Mishra P, Mishra AK, Mishra P, Jain S, Agrawal GP. Development and characterization of hyaluronic acid–anchored PLGA nanoparticulate carriers of doxorubicin. Nanomedicine. 2007;3(4):246–57.
Shen H, Shi S, Zhang Z, Gong T, Sun X. Coating solid lipid nanoparticles with hyaluronic acid enhances antitumor activity against melanoma stem-like cells. Theranostics. 2015;5(7):755.
Endsley AN, Ho RJ. Enhanced anti-HIV efficacy of Indinavir after inclusion in CD4 targeted lipid nanoparticles. J Acquir Immune Defic Syndr (1999). 2012;61(4):417.
Li F, Park S-J, Ling D, Park W, Han JY, Na K, et al. Hyaluronic acid-conjugated graphene oxide/photosensitizer nanohybrids for cancer targeted photodynamic therapy. J Mater Chem B. 2013;1(12):1678–86.
Nevala WK, Butterfield JT, Sutor SL, Knauer DJ, Markovic SN. Antibody-targeted paclitaxel loaded nanoparticles for the treatment of CD20+ B-cell lymphoma. Sci Rep. 2017;7:45682.
Kim HS, Cho HR, Choi SH, Woo JS, Moon WK. In vivo imaging of tumor transduced with bimodal lentiviral vector encoding human ferritin and green fluorescent protein on a 1.5 T clinical magnetic resonance scanner. Cancer Res. 2010;70(18):7315–24.
Wang X, Yang L, Chen Z, Shin DM. Application of nanotechnology in cancer therapy and imaging. CA Cancer J Clin. 2008;58(2):97–110.
Capolla S, Garrovo C, Zorzet S, Lorenzon A, Rampazzo E, Spretz R, et al. Targeted tumor imaging of anti-CD20-polymeric nanoparticles developed for the diagnosis of B-cell malignancies. Int J Nanomedicine. 2015;10:4099.
Carter P. Improving the efficacy of antibody-based cancer therapies. Nat Rev Cancer. 2001;1(2):118.
Hoffmann RM, Coumbe BG, Josephs DH, Mele S, Ilieva KM, Cheung A, et al. Antibody structure and engineering considerations for the design and function of Antibody Drug Conjugates (ADCs). Oncoimmunology. 2018;7(3):e1395127.
A study of BI-1206 in combination with rituximab in subjects with indolent B-cell non-Hodgkin lymphoma [updated April 1, 2019; cited 2019 June 1]. Available from: https://clinicaltrials.gov/ct2/show/NCT03571568?term=BI-1206+with+Rituximab&rank=2.
Burges A, Wimberger P, Kümper C, Gorbounova V, Sommer H, Schmalfeldt B, et al. Effective relief of malignant ascites in patients with advanced ovarian cancer by a trifunctional anti-EpCAM× anti-CD3 antibody: a phase I/II study. Clin Cancer Res. 2007;13(13):3899–905.
Dose-response study of Ibalizumab (monoclonal antibody) plus optimized background regimen in patients with HIV-1 (TMB-202) [updated May 5, 2014; cited 2019 June 1]. Available from: https://clinicaltrials.gov/ct2/show/NCT00784147.
HuMax-CD4 in non-cutaneous T-cell lymphoma [updated July 11, 2018; cited 2019 June 1]. Available from: https://clinicaltrials.gov/ct2/show/NCT00877656.
Rituximab in treating patients with non-Hodgkin’s lymphoma or Hodgkin’s disease [updated July 11, 2018; cited 2019 June 1]. Available from: https://clinicaltrials.gov/ct2/show/NCT00003849.
Porter DL, Hwang W-T, Frey NV, Lacey SF, Shaw PA, Loren AW, et al. Chimeric antigen receptor T cells persist and induce sustained remissions in relapsed refractory chronic lymphocytic leukemia. Sci Transl Med. 2015;7(303):303ra139.
Hansel TT, Kropshofer H, Singer T, Mitchell JA, George AJ. The safety and side effects of monoclonal antibodies. Nat Rev Drug Discov. 2010;9(4):325.
Gressett SM, Shah SR. Intricacies of bevacizumab-induced toxicities and their management. Ann Pharmacother. 2009;43(3):490–501.
Coiffier B, Lepage E, Brière J, Herbrecht R, Tilly H, Bouabdallah R, et al. CHOP chemotherapy plus rituximab compared with CHOP alone in elderly patients with diffuse large-B-cell lymphoma. N Engl J Med. 2002;346(4):235–42.
Craik DJ, Fairlie DP, Liras S, Price D. The future of peptide-based drugs. Chem Biol Drug Des. 2013;81(1):136–47.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 American Association of Pharmaceutical Scientists
About this chapter
Cite this chapter
Kotak, D.J., Todke, P.A., Dandekar, P., Devarajan, P.V. (2019). CD Receptor and Targeting Strategies. In: Devarajan, P., Dandekar, P., D'Souza, A. (eds) Targeted Intracellular Drug Delivery by Receptor Mediated Endocytosis. AAPS Advances in the Pharmaceutical Sciences Series, vol 39. Springer, Cham. https://doi.org/10.1007/978-3-030-29168-6_13
Download citation
DOI: https://doi.org/10.1007/978-3-030-29168-6_13
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-29167-9
Online ISBN: 978-3-030-29168-6
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)