Abstract
Femoral head fractures are rare, but associated with a high complication risk. Appropriate treatment can significantly reduce complications and improve outcome. Pearls and pitfalls of the entire treatment from diagnostics through therapy and aftercare are presented within this chapter and the effect on overall outcome discussed with the current literature.
In short:
-
Younger patients (average around 40 years).
-
Most commonly observed during automobile collisions (>80%).
-
Fracture commonly results from posterior hip dislocation (10%).
-
Fracture results from chiseling mechanism; pattern depending on hip position during trauma.
-
Early closed reduction improves outcome (<6 h)
-
Immediate open reduction if closed reduction fails.
-
-
Post-reduction/Preoperative CT scan recommended.
-
Pipkin classification most common; Brumback classification also includes anterior dislocations.
-
Nonsurgical treatment associated with improved outcome only in Pipkin I fractures
-
If <2 mm dislocation, stable hip joint, and no interposed fragments
-
-
If closed reduction succeeds, surgery during delayed primary care phase recommended.
-
Main blood supply to femoral head from medial femoral circumflex artery
-
Cave: posterior approaches.
-
-
No significant outcome differences between approaches; should be tailored to fracture pattern.
-
Increased avascular necrosis in posterior approaches.
-
Increased rate of heterotopic ossification in trochanteric flip osteotomy.
-
-
Decision fragment excision vs. fixation based on:
-
Residual fragment displacement <2 mm
-
Fragment outside weight bearing region
-
Free range of motion, no interposition
-
-
Management/approach depends on fracture type
-
Pipkin I: non-operative/fragment excision.
-
Pipkin II: Fixation with either countersunk interfragmentary compression screws, headless self-compression screws, and bio-absorbable pins and screws.
-
Pipkin III: Emergency surgery, open reduction favored.
-
Pipkin IV: If fracture pattern allows trochanteric flip shows better outcome.
-
-
Postoperative care: early functional treatment; minimum of 6 weeks partial weight bearing; avoid high degrees of hip flexion.
-
Common complications are nerve injury (20% sciatic nerve in posterior dislocations), avascular necrosis, heterotopic ossification, and osteoarthritis.
-
Depending on fracture type about 50% good to excellent results can be expected.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
11.1 Epidemiology, Mechanism of Injury
The fracture of the femoral head was first described in 1869 by Birkett who saw this injury during an autopsy of a patient who fell from the second story of a building [1]. These fractures are rare and almost exclusively occur after hip joint dislocations. The resulting femoral head shearing fractures are encountered in about 10% of all posterior hip dislocations and less frequently in anterior hip dislocations [2]. The exact frequency varies from study to study between 7% and 18% [3]. Apart from the complete shearing fractures, cortical depression fractures are described. Before the routine use of computed tomography, cortical depression fractures of the femoral head without fragment dislocation were virtually never detected. Due to improved imaging modalities the incidence rate for cortical depression fractures has been shown to be over 80% for anterior hip dislocations [4], 60% for posterior dislocations [5], and even to occur in patients without dislocations [6]. In a systematic review by Giannoudis et al. the average age for over 450 patients with femoral head fractures was reported as 38.9 years [7]. The most commonly observed injury mechanism was an automobile collision (84.3%), followed by motorcycle accidents (5.1%) and falls (4.3%).
While it was classically assumed that the typical fracture pattern in femoral head fractures was a result of the pull of the foveal ligament (“staying effect”) newer studies have shown that the ligament can only pull out a small osteocartilaginous fragment. The typical fracture pattern is explained as a chiseling mechanism of the acetabular wall on the femoral head [8]. The exact fracture pattern during dorsal hip dislocation then depends on the hip position during the trauma: If the hip is flexed below 60° and adducted, typically a Pipkin type I injury results as the medial part of the femoral head is pressed against the very solid posterior acetabular wall. Abduction with the same flexion will likely result in a type II injury. If the hip is flexed >60° the femoral head is pressed against a thinner portion of the posterior acetabular wall more likely resulting in acetabular fractures and cartilaginous damage, or cortical depression fractures, of the femoral head [9]. Pipkin type III fractures usually occur in cases with prolonged exposure to different forces: The first impact dislocates the femoral head from the joint and causes a part of the femoral head to shear-off. Prolonged adduction force then leads to a femoral neck fracture with the posterior acetabular rim acting as a hypomochlion [10]. Occasionally the femoral neck fracture can also occur during the reduction maneuver. It is assumed however that the majority of mechanical damage to the femoral neck region results from the initial trauma, and initially non-displaced fractures that were simply not noted on the primary X-ray dislocate during the reduction maneuver [8].
11.2 Clinical and Radiographic Assessment
As the majority of femoral head fractures are associated with high-energy trauma and multiple injured patients it is important to identify the fracture amongst concomitant injuries. Especially in unconscious patients careful history taking and reports about the mechanism of injury from the emergency medical personnel present on the scene of the accident can assist in determining the risk for such fractures. While the clinical presentation can be misleading, fractures with posterior hip dislocation generally appear with the leg in flexion, adduction, and internal rotation giving the impression of an overall shortened extremity. In fractures with anterior dislocation the leg is generally abducted and externally rotated. These classic malpositions can be missing in the case of concomitant femoral neck fractures. Careful examination of the integument is needed to identify skin damages associated with high-energy trauma (Morel-Lavallée lesions). A detailed neurological examination should be performed in the conscious patient to determine sciatic nerve injuries associated with posterior dislocations or femoral nerve injuries associated with anterior dislocations. In the unconscious patient this examination should be performed as early as feasible; special attention needs to be paid to the neurovascular structures on the imaging.
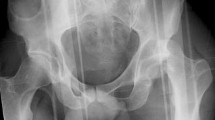
Conventional radiographs are the primary means of determining the direction of dislocation and extent of gross bony injuries. The fracture dislocation of the hip is routinely recognized in anteroposterior (ap) radiographs by the disruption of Shenton’s line (Fig. 11.1). In ap pelvic radiographs, the direction of dislocation can be determined by evaluating the size of the femoral head in relation to the contralateral, uninjured femur: Increased head size indicates that the femur is closer to the X-ray source, thus anteriorly dislocated; while posterior dislocations are closer to the radiographic film, thus appear smaller. Careful review of the femoral neck region is advisable to assess the existence of a Pipkin Type III situation that could dislocate during the reduction process. Furthermore oblique ala and obturator views can be used to determine acetabular fractures, while inlet and outlet views can be performed to detect pelvic ring injuries. Especially in the polytraumatized patient these views are commonly replaced by an immediate, pre-reduction computed tomography (CT).
CT is considered routine following closed reduction of the hip to correctly identify the fracture pattern and to decide upon the appropriate therapy (Fig. 11.1). In cases of irreducible hip dislocation, CT can be performed to determine the presence of intraarticular fragments that might prevent reduction before surgery. In general, CT can determine size, number, and location of fracture fragments as well as concomitant injuries. Some studies have recommended a special CT patient positioning to allow for CT-directed pelvic oblique conventional radiographs [11]. This has been shown to be an effective method to determine the extent of fracture displacement and congruity of the joint and is still recommended in current textbooks. However with the available technical ability to manually adjust the CT plain and three-dimensional CT reconstructions, these radiographs have no added value during primary diagnostics and should be used for follow-up purposes only.
Magnetic resonance imaging (MRI) is primarily used to determine the cartilage and vascular integrity of the femoral head. As such it has been suggested during the initial examination. Due to time constraints during the emergency treatment however its main value is during follow-up visits in determining the existence of early forms of avascular necrosis (AVN) [12]. If an injury to the external obturator muscle is suspected MRI can discover injuries to the anatomically close medial femoral circumflex artery and determine future risk of AVN.
11.3 Classification
As femoral head fractures are commonly associated with hip dislocations this is represented in the existing classification systems. The most common classification system was introduced by Pipkin in 1957 [13] (Fig. 11.2): Type I fractures are fractures where the fracture line ends caudal to the Fovea capitis femoris, whereas in Type II fractures the line ends cranial to the Fovea. This helps distinguish between fractures outside (Type I) and within (Type II) the load-bearing portion of the femoral head. In Type III fractures the femoral head fracture of either kind is associated with a femoral neck fracture. In Type IV fractures it is associated with acetabular wall fractures.
Pipkin classification of femoral head fractures; Type I: Fracture line ends caudal to the Fovea capitis femoris; Type II: Fracture line ends cranial to the Fovea; Type III: Femoral head fracture of either kind associated with femoral neck fracture; Type IV: Femoral head fracture of either kind associated with acetabular wall fractures (Haas, Norbert P., and Christian Krettek, eds. Tscherne Unfallchirurgie: Hüfte und Oberschenkel. Springer-Verlag, 2011. Adapted and reproduced with permission and copyright © of Springer)
In this system, only the more common dorso-cranial dislocations (90%) are classified. Brumback introduced a modification of the original classification 30 years later to incorporate all directions of dislocation and also therapeutic and prognostic estimations (Fig. 11.3) [14]: Type I and Type II fractures are defined like Pipkin I and II fractures, but divided into two subgroups. Subgroup A are fractures with minimal, or no acetabular rim damage and stable joint conditions after reduction. Subgroup B fractures show significant acetabular rim damage along with hip joint instability. Brumback III fractures are posterior hip dislocations with femoral neck fractures without (subgroup A) or with associated femoral head fractures (subgroup B). Type IV fractures result from anterior hip dislocations and either show an osteocartilaginous indentation (subgroup A), or a transchondral shear fracture (subgroup B). The final Type V fractures are central hip dislocations with femoral head fractures. While this classification system has been used in several larger studies [15, 16] and shown to be a valuable tool to assist outcome measurements, the clinical use of this classification is rare, in part due to its increased complexity when compared to the original Pipkin classification.
The AO fracture classification system accounts for femoral head fractures within the classification of proximal femoral fractures. All femoral head fractures are classified under 31-C. Pipkin Type I and II fractures are further classified as C1, osteochondral depression fractures as C2 and combined femoral head and femoral neck fractures as C3 (Fig. 11.4).
11.4 Conservative Treatment
11.4.1 General Considerations
The clinical and radiographic outcome of femoral head fractures with concomitant hip dislocation is directly linked to the time of reduction [17, 18] and should thus be considered as a true orthopedic trauma emergency. Several studies have shown superior results if the hip is reduced within 6 h [19], or even 3 h [20]. While many reduction maneuvers for hip dislocations have been proposed, they all incorporate common mechanisms for both anterior and posterior dislocations. In anterior dislocations, the reduction is generally performed by axial pull with the hip and knee in neutral flexion/extension. For posterior dislocations, knee and hip are flexed to around 90° and axial pull in the direction of the femur is applied. Adequate pain management and sedation/relaxation is required prior to reduction to keep the occurring stresses to the femoral head as low as possible. Post-reduction CT scan should be performed to guide the ensuing management. Closed reduction is contraindicated in patients with concomitant femoral neck fractures. If closed reduction is technically not possible, immediate open reduction is recommended. A CT scan should be performed beforehand to assess the fracture situation in detail if this does not lead to substantial delays until final reduction is achieved.
11.4.2 Nonsurgical Treatment
The historically predominant conservative fracture treatment with bed rest and traction has been largely abandoned due to relatively poor results [21] and the associated socioeconomic consequences. Non-operative treatment however can be considered especially in Pipkin I fractures under certain conditions: Near anatomic reduction with fragment dislocation below 2 mm, a stable hip joint and congruent joint surfaces without interposed fragments [22]. When applying these criteria studies with limited patient numbers have shown satisfactory outcomes [23]. Even if the fragment does not completely reduce after closed reduction, non-operative treatment can be performed if the hip range of motion is not compromised by it [24], as even necrotic changes to the fragment outside the weight bearing zone seem to have no effect on the clinical outcome [18]. The same criteria can be applied to Pipkin Type II fractures. However as they are located in the weight bearing portion of the femoral head surface these fractures are exposed to increased direct pressure and shear forces that can prevent adequate closed reduction [23]. Furthermore these fractures usually contain large areas of the femoral head, thus a high likelihood for an unstable hip joint and osteoarthritis in case of incongruity or osteonecrosis is given.
If nonsurgical treatment is chosen, the patient should be limited to partial weight bearing with crutches for at least 6 weeks. Adduction and excessive internal rotation of the hip should be avoided. Follow-up radiographs after 3 and 6 weeks should be performed to determine the maintenance of adequate reduction. The CT-directed pelvic oblique radiograph technique originally published by Moed et al. can be used to determine the positioning angle of the patient to allow for a standardized, perpendicular fracture line visualization [11].
11.5 Operative Treatment
11.5.1 Approaches
11.5.1.1 General Considerations: Time to Surgery
As with other fracture entities around the proximal femur the time to surgery can have significant implications on the long-term outcome. The most time sensitive and outcome predicting factor is early joint reduction. In cases of technically impossible reduction the time to surgery should thus ideally be below the 6 h threshold if comorbidities and concomitant injuries permit. Likewise in cases with a Pipkin III type injury early reduction and femoral neck fixation is needed especially if a head preserving therapy is planned. If closed reduction is accomplished current opinion is that the definitive surgery should be performed during the delayed primary care phase ideally between the sixth and tenth day [25]. If the definitive surgery is performed after the 14th day post reduction, significantly worse operative results have to be expected.
11.5.1.2 General Considerations: Vascular Anatomy
Before committing to any approach and treatment clear visualization of the approaches anatomy and associated vascular supply of the femoral head and neck is advisable to avoid iatrogenic damage to the important vessels. The most important blood supply of the femoral head weight bearing cartilage is provided by the terminal branches of the medial femoral circumflex artery [26]. The medial circumflex artery originates from the deep femoral artery and runs between the iliopsoas and pectineus muscles along the basal part of the femoral neck. From there it continues around the inferior border of the external obturator muscle, runs posterior to its tendon and anterior to the gemellus muscles and into the hip capsule just superior to the superior gemellus muscle insertion. From there the terminal branches of the artery lie within the periosteum and enter the bone postero-superiorly just lateral to the joint cartilage. As a result of this course the main risk of injuring the medial circumflex artery is during posterior approaches [27]. Important medial blood supply from the vessels within Weibrecht’s ligament [28] is furthermore at risk during reduction of femoral head fractures and care should be taken not to injure the medial synovial fold, as it is often attached to the fragment. The lateral circumflex artery has barely any contribution to the femoral heads blood supply.
11.5.1.3 Anterior Approaches
Traditionally anterior approaches such as the Smith-Petersen approach were unpopular due to misinterpreted anatomical considerations. The believe was that the more common posterior hip dislocation injures the posterior blood supply so that an anterior approach with possible damage to the ascending branch of the lateral circumflex artery would then cut all blood supply from the femoral head [21]. With the above-mentioned anatomical considerations in mind however anterior approaches have gained considerably in popularity. Studies have shown that this approach is associated with decreased operating time and blood loss [23]. Furthermore the rate of avascular necrosis of the femoral head seems to be decreased [29]. In cases of isolated femoral head fracture the associated fragment is most commonly anteromedial. The Smith-Petersen approach thus offers direct visualization of most fragments in Pipkin I and II fractures without compromising the vascular integrity of the femoral head. A radial capsulotomy at the beginning of the acetabulum usually offers sufficient fracture visualization. If improved exposure is needed, the iliac rectus femoris origin can be released. Without dislocating the hip most fractures can then be visualized by extension, abduction, and external rotation. The anterolateral Watson Jones approach offers less soft tissue trauma, but also less adaptability when it comes to extending the approach. Pipkin III fractures can be addressed by an anterolateral approach to manage both the femoral neck fracture with open reduction and also the femoral head fracture through a single incision.
Some older studies have seen higher incidence for heterotopic ossifications for anterior approaches. Swiontkowski et al. have shown an increased overall (58% vs. 25%) rate of heterotopic ossifications when comparing anterior with posterior approaches in the treatment of Pipkin I and II fractures [23]. Of the ossifications 29% were functionally significant in anterior approaches while none were functionally significant in posterior approaches. In a follow-up study the author has thus recommended to only use the distal, gluteal musculature sparing part of the Smith-Petersen approach. Newer studies have thus shown not only similar, but lower incidence rates of heterotopic ossifications for the anterior approach [29, 30].
11.5.1.4 Posterior Approaches
Posterior fracture dislocations are often associated with posterior soft tissue damage to structures such as the piriformis tendon. These structures most commonly block closed reduction. To directly address the posterior structures in irreducible fracture dislocations as well as in cases with associated posterior acetabulum fractures (Pipkin IV) the Kocher-Langenbeck approach is recommended [31]. To manage femoral head damages through a posterior approach a combination of the approach with a trochanteric flip osteotomy surgical hip dislocation is suggested. The advantage of this approach was demonstrated in a cadaver study by Gautier et al. that provided insight into the femoral heads blood supply [27]. Through this technique the obturator externus muscle is kept intact, thus preserving blood supply to the femoral head through the medial femoral circumflex artery [32]. Patient positioning and initial exposure are performed analogue to the Kocher-Langenbeck approach, with the actual transmuscular approach going through the Gipson Interval. A trochanteric step cut osteotomy is then performed from the superior edge of the greater trochanter distally to the posterior end of the vastus ridge and mobilized anteriorly. Afterwards the capsule is incised and the foveal ligament transected and excised with the hip joint in a flexed and externally rotated position. The hip can now be anteriorly dislocated and the complete femoral head can be surgically addressed. To facilitate anatomical refixation of the greater trochanter with two cortical screws drilling should be performed prior to the osteotomy.
In their original study of patients with surgical anterior hip dislocation Ganz et al. experienced no cases of avascular necrosis in 213 patients [32]. In a further study Kloen et al. compared patients treated either with an anterior, anterolateral, isolated posterior, or trochanteric flip approach [30]. They found that around 80% of the patients with trochanteric flip osteotomy had either excellent or good results. Again they noticed no avascular necrosis but a high rate (60%) of functionally significant heterotopic ossification. As such the excellent exposure of this approach is limited by the extensive soft tissue trauma and should be used in cases with posterior bony acetabulum injury combined with anterior femoral head fractures. Careful operative technique is needed to protect the femoral heads vasculature.
11.5.2 Techniques of Open Reduction and Fixation (Table 11.1)
As the surgical technique is dependent on the fracture morphology the treatment options are discussed using the more common Pipkin classification:
11.5.2.1 Pipkin Type I/II
If the above-mentioned criteria for nonsurgical management are not met (Sect. 11.4.2), the surgical treatment can be performed either by internal fixation or fragment excision. Earlier studies have generally advised for fragment excision as long as the fragment size was less than one third of the femoral head, as this has been shown to have a superior outcome compared to fragment fixation [33]. Further criteria advocating excision are the degree of fracture comminution and thus technical operability, exact fragment size, and fracture location in a non-weight bearing area of the femoral head. A cadaveric study by Holmes et al. showed that fragment excision in Pipkin Type I fractures does not change the peak load and load distribution on the acetabulum surface [34]. A recent randomized controlled trial has shown superior functional outcome scores in patients with Pipkin Type I fractures and fragment excision compared to nonsurgical treatment [35]. In light of these results Pipkin Type I fractures should mainly be treated with fragment excision. Pipkin Type II fractures and larger fragments have however been shown to significantly interfere with normal hip joint function if excised [34]. After excision the contact area was increased, mean pressures higher and displaced centrally. This is thought to increase the chance of chondral deterioration and ultimately osteoarthritis. If technical operability is given, these fracture fragments should be addressed by osteosynthesis. The approach should be tailored to the fragment location as determined on the preoperative CT scan and temporal fixation after open reduction can be achieved with Kirschner wires. Definitive fragment fixation then depends on fragment size and surgeon preference. In larger fragments extra-articularly introduced lag screws can be an option [36]. Most fractures however require fixation from within the joint. Treatment options are countersunk interfragmentary compression screws [37], headless self-compression screws [38], and bio-absorbable pins and screws [39]. Studies comparing the outcome between these treatment methods in a randomized, controlled fashion do not exist and all studies with these fixation methods suggest comparable outcomes. Only one study using 3-mm cannulated screws with washers has shown a high failure rate due to dissociation between screw and washer [29].
In cases of technically impossible anatomic fixation of fragments in the weight bearing region, as well as in older patients, hemi- and total hip arthroplasty is a treatment option [40]. Especially in the geriatric patient this enables early rehabilitation without the risk of secondary complications such as avascular necrosis or traumatic osteoarthritis.
11.5.2.2 Pipkin III
This rare fracture type has to be addressed by emergency surgery to allow for successful reduction and fixation of both the femoral neck and head with adequate outcome. Internal fixation of the femoral neck and hip reduction can be performed by the Watson Jones approach, or any approach of the surgeon’s preference. Open reduction decreases the risk of vascular compromise [7]. If the Watson Jones approach is used the approach can subsequently serve as the approach to the femoral head in adequately located fracture situations. Whether or not surgical fixation of the femoral head is needed is dependent on the fragment size and position after reduction. In principle the same criteria apply as mentioned above (Sect. 11.4.2). Fragments smaller than 2 mm, outside the weight bearing region with near normal hip range of motion can be left untreated. Primary hemi- or total hip arthroplasty can be a treatment option in elderly patients and femoral neck fractures with large displacements [41].
11.5.2.3 Pipkin IV
The treatment and approach to these fractures is dictated by the location and severity of the acetabular fracture. Small, well-reduced fragments without interposed loose bodies can be treated conservatively in the same fashion as Pipkin I fractures. Especially in younger patients however fixation should be performed in larger and displaced fragments. The most common posterior wall fractures can be addressed through the Kocher-Langenbeck approach and possibly a separate anterior approach depending on the femoral head fragment location or through a single approach with a trochanteric flip osteotomy. This has been shown to improve outcome in Pipkin type IV fractures [16]. Pipkin IV fractures with anterior acetabular involvement can be addressed either by the ilioinguinal or the Stoppa approach with a Smith-Petersen extension [22]. The indications for hemi- or total hip arthroplasty are the same as for the previously reported Pipkin I-III fractures.
11.5.3 Results
11.5.3.1 Postoperative Care
Regardless of surgical or nonsurgical treatment several studies have shown that early mobilization yields equivalent, if not superior results to prolonged bed rest and extension treatment if the hip joint is stable [9, 30]. Early functional treatment with 20% body weight partial weight bearing with crutches is thus recommended for a minimum of 6 weeks. Early mobilization can be assisted by continuous passive motion devices as early as the first postoperative day. Especially in posterior hip dislocations flexion above 70–90° should be avoided, to decrease the load on the structurally weak part of the posterior acetabular rim. Careful, repeated physical therapy instructions on the correct postoperative behavior as well as aids such as wedge-shaped bolster should be used. If radiographic signs of fracture healing are evident after 6 weeks careful, assisted weight bearing increases combined with low impact training should be begun. Full weight bearing is generally achieved after 3 months.
11.5.3.2 Complications
The most common early complication associated with posterior hip dislocations is sciatic nerve injury (Fig. 11.5). This injury is seen in up to 20% of all fracture dislocations. The nerve damage is either caused by entrapment of the nerve between the femoral head or fracture fragments and the ischium, rupture on a fracture surface, or indirect pull and stretch [42]. In the majority of cases the damage results from direct compression through fracture fragments. The most commonly injured part of the sciatic nerve are the peroneal nerve fibers, as they are most susceptible to ischemic damage and have less stretching reserve due to the fixed course around the fibular head [43]. Immediate hip reduction is thus the most important method to reduce the pressure on the nerve. Letournel et al. have shown that in more than 2/3 of all patients with symptomatic sciatic nerve injuries no macroscopic injury can be observed [44]. Partial to total symptomatic recovery can be expected in about 70% of all patients [45].
In their 2009 meta-analysis Giannoudis et al. have shown that the postoperative infection rate for all femoral neck fractures is 3.2% [7]. They have furthermore shown that the three most common long-term complications after these fractures are femoral head necrosis (11.8%), heterotopic ossification (16.8%), and posttraumatic arthritis (20%).
Femoral head avascular necrosis typically occurs within the first 2 years after femoral head fractures. Long before conventional radiographic changes can be noticed, the MRI can determine early changes associated with avascular necrosis. Common signs are edema, wavy, low signal lines with fatty centers, the double line sign, and later on osteochondral fragmentation. Prolonged compromise of the initial vascularity of the femoral head is regarded as a main risk factor for osteonecrosis [46]. In this regard early reduction of an associated hip dislocation is the key element to reduce this risk. However several studies have shown that despite early reduction osteonecroses were seen [47], suggesting that the etiology is multifactorial. A major risk factor is direct osteochondral trauma from the initial injury, as well as the reduction [17]. Therefore multiple, unsuccessful closed reduction maneuvers have to be avoided. Current studies also suggest that the medial femoral circumflex artery can be damaged if the obturator externus muscle is injured. Older studies have suggested that anterior surgical approaches might compromise vascular integrity [17]. This was however soon refuted by newer studies [33].
The second most common long-term complication is heterotopic ossification (Fig. 11.6) which some authors have seen in as many as 80% of all cases [47]. Associated risk factors are pronounced muscle damage, traumatic brain injury, and insufficient soft tissue management. Furthermore fracture patterns requiring extensive approaches with long operating times seem to be associated with more heterotopic ossifications. Some studies report the incidence of heterotopic ossification to be higher in anterior approaches possibly due to aggressive muscle stripping from the ilium during this approach [22]. The underlying exact mechanism remains unknown. To prevent this complication either oral non-steroidal anti-inflammatory (NSAR) drugs or single dose radiation with seven Gray is suggested. Radiation is however hard to perform, especially in multiple injured, hemodynamically unstable patients. Radiation therapy has to be performed immediately preoperative, or within the first postoperative hours. Common oral NSAR regimes are either 50 mg twice daily or 25 mg of Indomethacin three times a day over 6 weeks postoperatively. It was shown that this effectively reduces the risk of severe heterotopic ossification [46]. As some studies have shown that prolonged NSAR treatment can compromise bone healing [48], newer studies suggest this prophylaxis only in the presence of extensive muscle damage, traumatic brain injury, or prolonged mechanical ventilation [22].
By far the most common complication after hip dislocations with or without associated fractures is posttraumatic osteoarthritis. The development of posttraumatic osteoarthritis is associated with the severity of the initial trauma [49], the amount of direct injury to the joint cartilage [50], and the postoperative congruity of the articular surface [51]. Accordingly the risk of osteoarthritis development is different among the various fracture types: While some degree of osteoarthritis is seen in almost all patients with Pipkin III fractures, or ventral dislocations, only as much as 50% of patients with Pipkin I, II, or IV fractures show this complication [14, 46].
11.6 Results
Due to the rarity of the injury many of the published studies report case series with small patient numbers, different treatment options, inhomogeneous follow-up, non-standardized outcome measures and different classification systems, thus limiting the comparability of the reported results. In one of the earliest larger studies Thompson and Epstein reported <10% of good results in patients with femoral head fractures [5]. Within this article they introduced an outcome measure for radiographic, as well as clinical results that include gross radiographic appearance, as well as pain, range of motion, and walking ability. In order to achieve good or excellent results only minimal joint line narrowing and osteophyte formation is allowed radiographically while clinically at least 75% range of motion have to be achievable without any associated pain (Table 11.2).
This score is the most predominant score in the current literature and has been used to stratify the outcome in larger reviews. Studies applying the modern management principles mentioned above have shown some improvements in the clinical and radiographic outcome when compared to the earlier treatment results. Intermediate term follow-up studies (mean follow-up of 33 months) with sufficient patient numbers (>30 patients) have shown good and excellent results in over 55% of all patients [30, 33]. These numbers are confirmed by current reviews [7, 52]. In these studies the incidence of poor outcome increased with increasing fracture type (Pipkin I through IV). A non-significant tendency towards better outcome in surgically treated fractures was seen, however limited data suggest better outcome for Pipkin Type I fractures with conservative treatment. No statistically significant outcome differences were seen between anterior, posterior, and trochanteric flip approaches. Trochanteric flip osteotomy presented with an increased odds ratio for heterotopic ossification, while posterior approaches had a higher incidence of avascular necrosis. Due to this trend towards better outcome and less complication some authors favor the anterior approaches in the current literature [22]. It should be noted however that the primary decision on the approach is dictated by the fracture pattern. Interestingly only one study has used a validated, patient centered health status survey (SF-12) to quantify the outcome after femoral head fractures [29]. No relationship between the SF-12 score and time to surgery, surgical approach, or treatment method was seen, in part due to the low patient number (n = 17).
For future studies the use of validated, comparable outcome measures (Thompson Epstein score, Merle d’Aubigne and Postel Score, Harris Hip Score, SF-35, EQ 5d) paired with a multicenter approach is needed to generate sufficient statistical power required to truly evaluate treatment and fracture specific outcome.
References
Birkett J. Description of a dislocation of the head of the femur, complicated with its fracture; with remarks. Med Chir Trans. 1869;52:133–8.
Duquennoy A, Decoulx J, Capron JC, Torabi DJ. Les luxations traumatiques de la hanche avec fracture de la tête fémorale. À propos de 28 observations. Rev Chir Orthop. 1975;61:209–19.
Yang RS, Tsuang YH, Hang YS, Liu TK. Traumatic dislocation of the hip. Clin Orthop Relat Res. 1991;265:218–27.
DeLee JC, Evans JA, Thomas J. Anterior dislocation of the hip and associated femoral-head fractures. J Bone Joint Surg Am. 1980;62(6):960–4.
Thompson VP, Epstein HC. Traumatic dislocation of the hip; a survey of two hundred and four cases covering a period of twenty-one years. J Bone Joint Surg Am. 1951;33-A(3):746–78; passim.
Yoon PW, Jeong HS, Yoo JJ, Koo KH, Yoon KS, Kim HJ. Femoral head fracture without dislocation by low-energy trauma in a young adult. Clin Orthop Surg. 2011;3(4):336–41. https://doi.org/10.4055/cios.2011.3.4.336.
Giannoudis PV, Kontakis G, Christoforakis Z, Akula M, Tosounidis T, Koutras C. Management, complications and clinical results of femoral head fractures. Injury. 2009;40(12):1245–51. https://doi.org/10.1016/j.injury.2009.10.024.
Goulet JA, Levin PE. Hip dislocations. In: Skeletal trauma: basic science, management, and reconstruction, vol. 3. Philadelphia: Saunders; 2003. p. 1657–69.
Lang-Stevenson A, Getty CJ. The Pipkin fracture-dislocation of the hip. Injury. 1987;18(4):264–9.
Brumback RJ, Holt ES, McBride MS, Poka A, Bathon GH, Burgess AR. Acetabular depression fracture accompanying posterior fracture dislocation of the hip. J Orthop Trauma. 1990;4(1):42–8.
Moed BR, Maxey JW. Evaluation of fractures of the femoral head using the CT-directed pelvic oblique radiograph. Clin Orthop Relat Res. 1993;296:161–7.
Henle P, Kloen P, Siebenrock KA. Femoral head injuries: which treatment strategy can be recommended? Injury. 2007;38(4):478–88. https://doi.org/10.1016/j.injury.2007.01.023.
Pipkin G. Treatment of grade IV fracture-dislocation of the hip. J Bone Joint Surg Am. 1957;39-A(5):1027–42; passim.
Brumback RJ, Kenzora JE, Levitt LE, Burgess AR, Poka A. Fractures of the femoral head. Hip. 1987;1987:181–206.
Prokop A, Helling HJ, Hahn U, Udomkaewkanjana C, Rehm KE. Biodegradable implants for Pipkin fractures. Clin Orthop Relat Res. 2005;432:226–33.
Solberg BD, Moon CN, Franco DP. Use of a trochanteric flip osteotomy improves outcomes in Pipkin IV fractures. Clin Orthop Relat Res. 2009;467(4):929–33. https://doi.org/10.1007/s11999-008-0505-z.
Epstein HC, Wiss DA, Cozen L. Posterior fracture dislocation of the hip with fractures of the femoral head. Clin Orthop Relat Res. 1985;201:9–17.
Hougaard K, Thomsen PB. Traumatic posterior dislocation of the hip--prognostic factors influencing the incidence of avascular necrosis of the femoral head. Arch Orthop Trauma Surg. 1986;106(1):32–5.
Schweikert CH, Weigand H. Hüftkopfkalottenfrakturen. Hefte Unfallheilkd. 1979;140:188–200.
Schiedel F, Rieger H, Joosten U, Meffert R. Wenn die Hüfte nicht “nur” luxiert. Unfallchirurg. 2006;109(7):538–44.
Epstein HC. Posterior fracture-dislocations of the hip; long-term follow-up. J Bone Joint Surg Am. 1974;56(6):1103–27.
Droll KP, Broekhuyse H, O’Brien P. Fracture of the femoral head. J Am Acad Orthop Surg. 2007;15(12):716–27.
Swiontkowski MF, Thorpe M, Seiler JG, Hansen ST. Operative management of displaced femoral head fractures: case-matched comparison of anterior versus posterior approaches for Pipkin I and Pipkin II fractures. J Orthop Trauma. 1992;6(4):437–42.
Thannheimer A, Gutsfeld P, Buhren V. Current therapy options for fractures of the femoral head. Chirurg. 2009;80(12):1140–6. https://doi.org/10.1007/s00104-009-1738-4.
Pape HC, Rice J, Wolfram K, Gansslen A, Pohlemann T, Krettek C. Hip dislocation in patients with multiple injuries. A followup investigation. Clin Orthop Relat Res. 2000;377:99–105.
Harrison MH, Schajowicz F, Trueta J. Osteoarthritis of the hip: a study of the nature and evolution of the disease. J Bone Joint Surg. 1953;35-B(4):598–626.
Gautier E, Ganz K, Krugel N, Gill T, Ganz R. Anatomy of the medial femoral circumflex artery and its surgical implications. J Bone Joint Surg. 2000;82(5):679–83.
Gojda J, Bartonicek J. The retinacula of Weitbrecht in the adult hip. Surg Radiol Anat. 2012;34(1):31–8. https://doi.org/10.1007/s00276-011-0829-3.
Stannard JP, Harris HW, Volgas DA, Alonso JE. Functional outcome of patients with femoral head fractures associated with hip dislocations. Clin Orthop Relat Res. 2000;377:44–56.
Kloen P, Siebenrock KA, Raaymakers ELFB, Marti RK, Ganz R. Femoral head fractures revisited. Eur J Trauma. 2002;28(4):221–33.
McKee MD, Garay ME, Schemitsch EH, Kreder HJ, Stephen DJ. Irreducible fracture-dislocation of the hip: a severe injury with a poor prognosis. J Orthop Trauma. 1998;12(4):223–9.
Ganz R, Gill TJ, Gautier E, Ganz K, Krugel N, Berlemann U. Surgical dislocation of the adult hip a technique with full access to the femoral head and acetabulum without the risk of avascular necrosis. J Bone Joint Surg. 2001;83(8):1119–24.
Marchetti ME, Steinberg GG, Coumas JM. Intermediate-term experience of Pipkin fracture-dislocations of the hip. J Orthop Trauma. 1996;10(7):455–61.
Holmes WJ, Solberg B, Bay BK, Laubach JE, Olson SA. Biomechanical consequences of excision of displaced Pipkin femoral head fractures. J Orthop Trauma. 2000;14(2):149–50.
Chen ZW, Lin B, Zhai WL, Guo ZM, Liang Z, Zheng JP, et al. Conservative versus surgical management of Pipkin type I fractures associated with posterior dislocation of the hip: a randomised controlled trial. Int Orthop. 2011;35(7):1077–81. https://doi.org/10.1007/s00264-010-1087-4.
Mostafa MM. Femoral head fractures. Int Orthop. 2001;25(1):51–4.
Ross JR, Gardner MJ. Femoral head fractures. Curr Rev Musculoskelet Med. 2012;5(3):199–205. https://doi.org/10.1007/s12178-012-9129-8.
Murray P, McGee HM, Mulvihill N. Fixation of femoral head fractures using the Herbert screw. Injury. 1988;19(3):220–1.
Jukkala-Partio K, Partio EK, Hirvensalo E, Rokkanen P. Absorbable fixation of femoral head fractures. A prospective study of six cases. Ann Chir Gynaecol. 1998;87(1):44–8.
Roeder LF Jr, DeLee JC. Femoral head fractures associated with posterior hip dislocation. Clin Orthop Relat Res. 1980;147:121–30.
Kozin SH, Kolessar DJ, Guanche CA, Marmar EC. Bilateral femoral head fracture with posterior hip dislocation. Orthop Rev. 1994;Suppl:20–4.
Rehm KE. Acetabulumfrakturen–posttraumatische und postoperative Nervenschäden. Hefte Unfallheilkd. 1985;174:472–6.
Trojan E. Gefäß-und Nervenverletzungen bei Frakturen und luxationen im Beckenbereich. Hefte Unfallheilkd. 1979;140:44–8.
Letournel E, Judet R. Fractures ofthe acetabulum (Translated and edited by Elson RA). Berlin: Springer; 1981.
Cornwall R, Radomisli TE. Nerve injury in traumatic dislocation of the hip. Clin Orthop Relat Res. 2000;377:84–91.
Hougaard K, Thomsen PB. Traumatic posterior fracture-dislocation of the hip with fracture of the femoral head or neck, or both. J Bone Joint Surg Am. 1988;70(2):233–9.
Schwarzkopf SR, Dreinhofer KE, Haas NP, Tscherne H. Isolated hip dislocation of traumatic origin. Unfallchirurg. 1996;99(3):168–74.
Burd TA, Hughes MS, Anglen JO. Heterotopic ossification prophylaxis with indomethacin increases the risk of long-bone nonunion. J Bone Joint Surg. 2003;85(5):700–5.
Upadhyay SS, Moulton A. The long-term results of traumatic posterior dislocation of the hip. J Bone Joint Surg. 1981;63B(4):548–51.
Borrelli J Jr. Chondrocyte apoptosis and posttraumatic arthrosis. J Orthop Trauma. 2006;20(10):726–31. https://doi.org/10.1097/01.bot.0000249882.77629.5c.
Bhandari M, Matta J, Ferguson T, Matthys G. Predictors of clinical and radiological outcome in patients with fractures of the acetabulum and concomitant posterior dislocation of the hip. J Bone Joint Surg. 2006;88(12):1618–24. https://doi.org/10.1302/0301-620X.88B12.17309.
Akula M, Giannoudis P, Gopal S, Pagoti R. Pipkin fractures–clinical outcomes. J Bone Joint Surg Br. 2010;92(SUPP IV):543.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Braun, B.J., Holstein, J.H., Pohlemann, T. (2019). Pipkin Fractures. In: Büchler, L., Keel, M. (eds) Fractures of the Hip. Fracture Management Joint by Joint. Springer, Cham. https://doi.org/10.1007/978-3-030-18838-2_11
Download citation
DOI: https://doi.org/10.1007/978-3-030-18838-2_11
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-18837-5
Online ISBN: 978-3-030-18838-2
eBook Packages: MedicineMedicine (R0)