Abstract
Hypoxic pulmonary vasoconstriction (HPV) is an essential mechanism of the lung matching blood perfusion to ventilation during local alveolar hypoxia. HPV thus optimizes pulmonary gas exchange. In contrast chronic and generalized hypoxia leads to pulmonary vascular remodeling with subsequent pulmonary hypertension and right heart hypertrophy. Among other non-selective cation channels, the family of classical transient receptor potential channels (TRPC) has been shown to be expressed in pulmonary arterial smooth muscle cells. Among this family, TRPC6 is essential for the regulation of acute HPV in mice. Against this background, in this chapter we give an overview about the TRPC family and their role in HPV.
Access provided by Autonomous University of Puebla. Download conference paper PDF
Similar content being viewed by others
Keywords
1 Introduction
Hypoxic pulmonary vasoconstriction (HPV) is a physiological lung mechanism that directs blood perfusion from poorly ventilated to well-ventilated lung areas to optimize gas exchange.1 In contrast to the systemic circulation, in which hypoxia leads to vasodilation, HPV is unique to the pulmonary vasculature2 (Fig. 12.1a) and is triggered by mild hypoxia (alveolar pO2 < 100 mmHg).1 A disturbance of this mechanism may result in life-threatening hypoxemia3 (Fig. 12.1b). Furthermore, when hypoxia is generalized and chronic, as in many lung diseases (e.g., chronic obstructive pulmonary disease [COPD], pneumonia, fibrosis) or in residents at high altitude, the subsequent pulmonary vasoconstriction leads to chronic pulmonary hypertension, vascular remodeling, and right heart failure.4,5
Ventilation-perfusion matching by hypoxic pulmonary vasoconstriction (HPV) in the lung under (patho)physiological conditions (P = blood flow). (a) Under physiological conditions, perfusion is matched to the alveolar oxygen partial pressure (pO2) by HPV. Reproduced with permission.9 (b) Under disturbed HPV, a mismatch of blood flow and alveolar ventilation may result in hypoxemia. The blood perfusion color indicates the oxygen concentration of the blood in a graded manner: the darker the color, the higher the oxygen concentration. Large circles high alveolar pO2, small circles low alveolar pO2
Although the physiological function of HPV was originally described in 1946 by Euler and Liljestrand, the underlying oxygen-sensing and signal transduction processes remain unclear.6 Several hypothetical mechanisms for the O2-sensing in pulmonary artery smooth muscle cells (PASMC) are currently proposed, for the most part related to reactive oxygen species (ROS).7 Nicotinamide adenine dinucleotide phosphate-oxidase (NAD(P)H) oxidases, similar to that found in neutrophils, as well as mitochondria are strongly suggested to affect superoxide generation during hypoxia. However, it is unclear whether ROS generation is increased or decreased under hypoxic conditions. Moreover, there is also evidence for a hypoxia-induced increase of cyclic adenosine diphosphate-ribose (cADPR), resulting in a rise of intracellular Ca2+ ([Ca2+]i) as well as a role for cytochrome P450-dependent processes in HPV.1
The smooth muscle layer of the precapillary vessels has been identified as the effector cell type. Moreover, isolated PASMCs respond to acute hypoxia by an increase of the [Ca2+]i concentration and subsequent contraction, indicating that these cells function as sensor as well as effector cells.8
In addition to L-type voltage-operated Ca2+ channels (VOCC), nonselective cation channels have been identified as important players in the regulation of vascular tone by their role in mediating the entry of cations like Ca2+ and Na+.9 Among other nonselective cation channels, the family of classical transient receptor potential (TRPC) channels has been shown to be expressed in pulmonary arterial smooth muscle10-12 and to play a major role in the regulation of HPV under acute hypoxia.5,13,14
2 The Classical Transient Receptor Potential Family of Nonselective Cation Channels
2.1 Introduction
Transient receptor potential (TRP) channels were first discovered in the fruit fly Drosophila melanogaster and constitute a superfamily of cation channels. In contrast to vertebrates, the transduction of visual stimuli in Drosophila melanogaster is a phospholipase C-dependent process that leads to an activation of membrane channels with subsequent membrane depolarization.15,16 Interestingly, Drosophila melanogaster with a mutation in the trp locus exhibited a transient instead of a sustained response to light due to a defect in Ca2+ influx following the initial Na+ influx. The channels responsible for this light-induced Ca2+ influx were named TRP channels.17,18
2.2 Identification and Structural Properties of Mammalian TRP Channels
The first mammalian TRP channel closely related to Drosophila melanogaster TRP channels was identified in 1995 and founded a new TRP family called the classical or canonical TRP (TRPC) channels.19 In the ensuing years, six other TRPC family members and other TRP families, such as TRPM (for melastatin), TRPV (for vanilloid receptor), TRPP (for polycystic kidney disease (PKD) proteins), TRPML (for mucolipidins), and TRPA (for ankyrin-rich proteins) were identified. Figure 12.2a shows the phylogenetic tree of the TRP superfamily.15 The classification of the mammalian TRP proteins in these six groups results from their structure (≥90% amino acid similarity within each group), whereas the characteristic features of TRP proteins in general are the six transmembrane domains (S1-S6), cytoplasmic N- and C-termini, and a hydrophobic loop between S5 and S6, as well as cation permeability15 (Fig. 12.2b). Thus, the channel pore is thought to be formed by the loop between S5 and S6. TRP channels are homo- or heterotetramers with members of the same subfamily15 and are permeable to Na+, K+, Cs+, Li+, Ca2+, Mn2+, and Mg2+ after voltage-independent activation.20
Phylogenetic tree and plasma membrane topology of the TRP proteins. (a) Phylogenetic tree of the TRP superfamily subdivided into six families according to their amino acid homology (≥90% within each group).15 (b) Plasma membrane topology of TRP proteins: six transmembrane domains (S1-S6) with a hydrophobic putative pore region between S5 and S6 and the cytoplasmic N- and C-termini.15 (c) Plasma membrane topology and functional domains of TRPC channels. TRPC channels have typically four ankyrin repeats, a caveolin-1-binding site, and a TRPC domain as well as a calmodulin IP3-receptor-binding domain (CIRB). In addition, there is one glycosylation site in TRPC3, two glycosylation sites in TRPC6, a protein 4.1-binding domain, and an Asparagin-Histidin-Glutamat-Arginin-Phenylalanin-binding domain in TRPC4, as well as a homer domain in TRPC1. Reproduced with permission9
2.3 Characteristics of the TRPC Channel Subfamily
The seven members of the TRPC family share common structural features in addition to the six transmembrane-spanning domains (S1-S6) and the putative pore region between S5 and S6 as the typical TRP structure: four N-terminal ankyrin repeats as well as a TRP box (amino acid sequence EWKFAR) and a calmodulin inositol 1,4,5-trisphosphate (IP3)-receptor-binding (CIRB) site in the C-terminal tail. Other protein-binding domains vary between the different TRPC proteins (Fig. 12.2c). The TRPC family can be divided into three subfamilies on the basis of their amino acid homology: TRPC1, TRPC4/5, and TRPC3/6/7. TRPC2 is a pseudogene in humans but plays an important role in the sexual recognition of mice.9,21
Whereas TRPC4 and TRPC5 share approximately 65% of the amino acid sequence, the members of the TRPC3/6/7 subfamily form a structural and functional subfamily with 70-80% homology of the amino acid sequence and direct activation by diacylglycerol (DAG).9 DAG production results from activation of G protein-coupled receptors or receptor tyrosine kinases and subsequent activation of phospholipase C isoforms (PLCβ or PLCγ, respectively), leading to hydrolysis of phosphatidylinositol 4,5-bisphosphate.22 While DAG mediates cation entry through receptor-operated channels (ROCs), IP3, the second product of this signal cascade, induces Ca2+ depletion of the endoplasmatic reticulum (ER), which subsequently activates Ca2+ influx from the extracellular space through store-operated channels (SOCs), also called capacitative Ca2+ entry (CCE). SOCs are discussed as mechanisms for TRPC1, 4, and 5 as well as for TRPC3 and 7.9,23 The varying function of TRPC3 and TRPC7 as ROCs or SOCs is probably caused by the formation of heterotetrameric channels as a consequence of the interaction with other TRPC isoforms.20 Thus, TRPC channels can be gated by different stimuli, leading to multisided channel activation.24 In general, the properties of heteromultimer proteins depend on their protein composition. Furthermore, the function of TRPC channels may also depend on many additional modulators, making the mechanisms more complex.21
2.4 Expression Pattern and Function of TRPC Channels
After identification of the TRPC channel subfamily, the expression levels of TRPC family members in different organs and cell types, as well as their functional roles, have been intensely investigated.
TRPC1 exhibits a widespread, but not ubiquitous, expression in different cell types, whereas an important role for vascular smooth muscle has been suggested that is related to the contractile and proliferative functions of muscle. However, there is evidence that TRPC1 only contributes to a heterotetrameric ion channel complexed with other TRPC isoforms. Heterologous expression studies and biochemical investigations indicated a possible association of TRPC1 with TRPC4, TRPC5, TRPC3, and TRPP2.15,24 This interaction with other TRPC isoforms seems to be required for the translocation of TRPC1 to the plasma membrane, as shown in TRPC1-TRPC4 coexpression studies.20
TRPC3 is highly expressed in brain as well as cardiac and smooth muscle cells (SMCs) and has been detected in the slow oxidative myofibers in skeletal muscle after neuromuscular activity.15 Numerous functions of TRPC3 have been suggested in agonist-induced contraction in SMCs.24 Interestingly, TRPC3 has high basal activity, which is decreased after the addition of a second glycosylated site at the extracellular portion of the channel, as found in TRPC6.15 Moreover, basal and agonist-induced cation influx into SMCs as well as smooth muscle contractility were reportedly increased after the replacement of TRPC6 by TRPC3 in TRPC6-deficient (TRPC6-/-) mice.25 Thus, protein glycosylation seems to play an important role for channel activity. TRPC3 also forms functional heteromultimeric channels with TRPC6.24
TRPC4 is particularly expressed in the endothelium, where it regulates microvascular permeability, endothelium-dependent vasorelaxation of SMCs, and gene transcription. In SMCs, TRPC4 regulates cell proliferation and contraction.20 TRPC4 as well as TRPC5 are reportedly thought to be assisted in their function as nonselective cation channels by TRPC1.15
TRPC5 was first found to be primarily expressed in the brain, but there are conflicting reports on the expression of TRPC5 in the pulmonary vasculature. Since TRPC5 is only poorly characterized, the role of this channel is unclear.15,20
TRPC6 is expressed in many tissues rich in SMCs but is most prominently expressed in lung tissue. Many studies suggest an important role of TRPC6 in vascular and pulmonary SMCs.15 Investigations in TRPC6 - / _ mice in comparison to wild-type (WT) mice have also revealed a unique role for TRPC6 in the regulation of airway and vascular smooth muscle contractility.25,26 Most interestingly, small precapillary pulmonary arteries, in contrast to large pulmonary arteries, do not express TRPC3.9 Besides a role for TRPC6 for SMC contraction, there is evidence for a role of TRPC6 in cell proliferation.24
TRPC7 was first identified in mouse brain, but expression is also found in SMCs from the aortic and renal arteries as well as in endothelial cells from the cerebral and coronary arteries.20 TRPC7 expression is also reported in the eye, spleen, and testis.15
3 Role of the TRPC Channels in Acute Hypoxic Pulmonary Vasoconstriction
3.1 Role of Ca2+Channels in Acute HPV
Under physiological conditions, acute alveolar hypoxia leads to vasoconstriction of the precapillary arteries in the lung. Therefore, a rise of [Ca2+]i in PASMCs is a key event in this process, inducing Ca2+/calmodulin-dependent activation of myosin light chain kinase, phosphorylation of the myosin light chains, actin-myosin interactions, and contraction.13,27 However, the regulation of [Ca2+]i has not yet been resolved. In general, [Ca2+]i can be increased by Ca2+ influx from the extracellular space or by release from intracellular Ca2+ stores. At least three classes of Ca2+-permeable channels in the plasma membrane are known: the L-type VOCCs, which are regulated by the resting membrane potential; the ROCs, which are activated by agonists; and SOCs, which are opened by depletion of Ca2+ from the sarcoplasmic reticulum (SR).4,28 Concerning the Ca2+ release from intracellular Ca2+ stores, IP3 receptor-mediated Ca2+ release from IP3-sensitive SR as well as ryanodine receptor-mediated Ca2+ release from ryanodine-sensitive SR are known.29
One well-documented concept for the regulation of HPV proposes that a hypoxia-induced inhibition of voltage-gated K+ (Kv) channels leads to membrane depolarization and Ca2+ entry through VOCCs.30 However, since antagonists of Kv channels did not block HPV and VOCC antagonists exhibited no or only partial prevention of the hypoxic response, the mechanism of HPV seems to be more complex.12,13 Growing evidence in the literature indicates a role for hypoxia-induced Ca2+ release from intracellular stores activating SOCs and CCE, possibly in addition to VOCCs.13,14,30 Thus, depletion of intracellular Ca2+ stores, and thereby activation of SOCs by cyclopiazonic acid (CPA) and simultaneous application of nifedipine to prevent Ca2+ influx through VOCCs, was shown to cause an increase of [Ca2+]i that was markedly enhanced under hypoxic compared to normoxic conditions.13,14,30 Moreover, the pharmacological agents SKF-96365, Ni2+, and La3+, which block influx through nonselective cation channels in PASMCs, were potent inhibitors of HPV at concentrations that did not affect VOCCs. This is the first direct evidence that nonselective cation channels may play an important role in HPV.14 Nevertheless, the VOCC inhibitor nifedipine was quite effective in preventing and reversing HPV, suggesting a hypoxia-induced influx through both SOCCs and VOCCs.14
Nonselective cation channels, which are associated with both SOCs and ROCs, are reported to be likely formed of homo- or heteromultimers of TRP proteins.31,32 Among the TRP channels, especially TRPC proteins are expressed in SMCs of distal pulmonary arteries, which are suggested to be O2 sensor and effector cells, at least of acute HPV.11 However, less is known about the functional role of TRPC channels in the pulmonary circulation.
3.2 Importance of TRPC6 Channels in Acute HPV
TRPC6 is highly expressed in lung tissue as well as pulmonary and vascular SMCs.23 Since there is a lack of specific TRPC channel blockers, a TRPC6-/- mouse model was developed by gene inactivation in embryonic stem cells to investigate functional parameters in comparison to WT mice.22,25 Interestingly, TRPC6-/- mice showed increased vascular smooth muscle contractility, suggesting a critical role for TRPC6 in regulating vascular smooth muscle tone.25
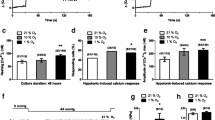
To assess the role of TRPC6 in HPV, we analyzed the pressor response in isolated ventilated and perfused lungs from WT and TRPC6-/- mice during acute (<20 min) and sustained (60 - 160 min) hypoxia.5 As shown in Fig. 12.3a, ventilation of lungs from WT mice with 1% O2 provoked a biphasic profile of pulmonary arterial pressure (PAP), with a first transient increase followed by a second progressive increase of PAP. Interestingly, the acute phase of HPV was completely absent in TRPC6- /- mice, while the sustained phase was not significantly different compared to WT mice. Thus, the general muscular contractility was not affected, the vasoconstriction induced by the thromboxane mimetic U46619 being unchanged.5 Under normoxic conditions, the PAP did not differ between WT and TRPC6-/-.5 These results clearly show the indispensable role of TRPC6 in acute HPV as well as the differential regulation of the acute and sustained phase of HPV. Moreover, since partial occlusion of alveolar ventilation provoked severe hypoxemia in TRPC6-/- mice but not in WT mice, the profound physiological relevance of TRPC6 in acute HPV was confirmed.5
Involvement of TRPC6 in acute hypoxic pulmonary vasoconstriction. (a) Time course of the increase in pulmonary arterial pressure (ΔPAP) in isolated, buffer-perfused, and ventilated mouse lungs (filled circles WT; open circles TRPC6-/-) during 160 min of hypoxic ventilation (1% O2). Control lungs were ventilated normoxically (filled triangles WT; open triangles TRPC6-/-). *1 indicates a significant difference (p < 0.05) between WT and TRPC6-/- mice after applying acute hypoxia; *2 indicates significant differences (p < 0.05) between normoxic (WT and TRPC6-/-) and hypoxic (WT and TRPC6-/-) mice. (b) Time course of [Ca2+]i in primary cultured PASMCs from WT and TRPC6-/- mice on exposure to hypoxia. Cells were loaded with fura-2 and analyzed by single-cell fluorescence imaging. Horizontal bars indicate endothelin priming (4 nM ET-1) and hypoxic perfusion (hypoxia) of PASMCs. Reproduced with permission5
3.3 Role of TRPC6 Channels in the Increase of Intracellular Ca2+ Concentration in Acute HPV
To investigate the cellular mechanism of the TRPC6 dependency of HPV, alterations of [Ca2+]i were investigated in hypoxia-incubated PASMCs from TRPC6-/- and WT mice, using an established method based on fluorescence imaging of single cells loaded with the fluorescent dye fura-2.33,34 The expression level of the TRPC subtypes was unchanged in the PASMCs from TRPC6-/- mice except for TRPC6, as expected.5 In contrast to WT PASMCs, the hypoxia-induced rise of [Ca2+]i after priming with endothelin 1 (ET-1) was completely absent in PASMCs from TRPC6-/- (Fig. 12.3b).5 The “priming” with a low dose of vasoactive agents such as angiotensin II, ET-1, or prostaglandin F2α turned out to be a prerequisite for HPV.35-37
Interestingly, the observed increase of [Ca2+]i in WT PASMCs was completely dependent on extracellular Ca2+, although ET-1 caused a rise of [Ca2+]i in both cell types in the absence of extracellular Ca2+.5 This finding challenges the suggested contribution of SOCs and CCE to the regulation of HPV12-14 and may be related to the fact that PASMCs of the precapillary resistance vessels were investigated in this study.
However, since the potent blocker of VOCC nicardipine almost completely inhibited Ca2+ entry in WT PASMCs and acute HPV in isolated lungs, the increase of [Ca2+]i appears to be mostly attributable to VOCCs.5 Then, what role do TRPC6 channels play? As described in the literature, TRPC6 channels are predominantly permeable to Na+, and only a small percentage of the whole-cell current is caused by Ca2+ in the presence of extracellular Na+.38 In contrast to VOCCs, TRPC6 channels are permeable for Mn2+. Thus, the hypoxia-induced influx of non-Ca2+ ions through TRPC6 channels was analyzed by a method called Mn2+ quenching. These experiments showed that hypoxia induced an increase in the Mn2+ quenching rate as a result of increased Mn2+ influx in WT but not in TRPC6-/- PASMCs.5 This result is in line with the concept that Na+ influx through TRPC6 channels leads to membrane depolarization and activation of VOCCs.38-40 Moreover, an increase of intracellular Na+ has been shown to block the Kv channels41 known to activate VOCCs. The important role of Kv channels was demonstrated by the impairment of HPV in mice lacking the Kv channel.4,42
3.4 Activation of TRPC6 Channels in Acute HPV
The receptor-operated, store-independent TRPC6 channel was the first ion channel shown to be DAG activated in a membrane-delimited fashion, independently of protein kinase C. However, the exact location of the DAG-binding site in the TRPC6 protein is still unresolved. In addition, sensitivity to the arachidonic acid metabolite 20-hydroxyeicosatetraenoic acid (HETE) as well as an activating effect by Ca2+/calmodulin or protein phosphorylation have been reported.23
Since the recombinant TRPC6 channels heterologously expressed in human embryonic kidney (HEK) 293 cells were not activated by hypoxia, a direct activation of TRPC6 channels by hypoxia could be excluded.5 Interestingly, a fluorescent DAG sensor expressed in PASMCs revealed the localization of DAG in the cytosol under normoxic conditions. Under hypoxia, DAG was translocated to the plasma membrane, suggesting gating of TRPC6 via DAG. In addition, a DAG kinase inhibitor activated the TRPC6 channels, supporting the hypothesis of hypoxia-induced DAG accumulation mediated by inhibition of DAG kinase or phospholipases.5 Speculatively, the activation of TRPC6 in HPV may occur via ROS as it has been proposed that the O2-sensing mechanism underlying HPV involves ROS.5 NAD(P)H oxidase isoforms, different from those found in neutrophils, as well as mitochondria have been shown to be involved in the regulation of HPV in this regard. However, it is still unclear whether ROS generation is increased or decreased under hypoxic conditions.1 Moreover, a role for a decreased adenosine monophosphate/adenosine triphosphate ratio as well as a role for cytochrome P450-dependent processes have been suggested for HPV.1,43
3.5 Hypothesis of the Mechanism of Acute HPV
A hypothetic model of the signal transduction pathway in PASMCs underlying acute HPV is described in Fig. 12.4. Initial priming of ET-1 activates PLC, producing a basal DAG concentration without activation of TRPC6 itself, but which is required for hypoxia-induced TRPC6 activation. Hypoxia-induced DAG accumulation results from the activation of PLCs1 or phospholipase D (PLD)2 or inhibition of DAG-degrading DAG kinases,3 probably induced by changes in ROS production, and ultimately leads to Na+ influx through TRPC6 channels. A subsequent membrane depolarization, probably also caused by Na+-induced inhibition of Kv channels, activates Ca2+ influx through VOCCs, resulting in contraction of the PASMCs.
Hypothetical model of the signal transduction pathway underlying acute hypoxic pulmonary vasoconstriction in PASMCs. According to this model, hypoxia-induced diacylglycerol (DAG) accumulation causes a cation influx through TRPC6. The DAG increase may be caused by activation of either phospholipase C (1), phospholipase D (2) or by inhibition of DAG-degrading DAG kinases (3). ET-1 endothelin-1; ATII angiotensin II; PGF2α prostaglandin F2α; Gq/11 G protein type q and 11; PLC phospholipase C; PIP 2 phosphatidylinositol 4,5-bisphosphate; IP 3 inositol-1,4,5 trisphosphate; VOCC voltage gated calcium channel; ER endoplasmatic reticulum; IP 3 -R IP3-receptor; PLD phospholipase D; ROS reactive oxygen species; PA phosphatidic acid; PAP phosphatidic acid phosphatase; CaM calmodulin; MLCK myosin-light chain kinase. Reproduced with permission9
4 Conclusion
HPV is an important mechanism in the lung that has been under investigation for more than 60 years. The nonselective cation channel TRPC6 has been identified as playing an essential role in this mechanism, as demonstrated by a complete absence of the acute response to hypoxia in mice lacking this ion channel. Therefore, the TRPC6 channels offer a promising therapeutic target for pharmacological intervention in the control of pulmonary hemodynamics and gas exchange.
References
Weissmann N, Sommer N, Schermuly RT, Ghofrani HA, Seeger W, Grimminger F (2006) Oxygen sensors in hypoxic pulmonary vasoconstriction. Cardiovasc Res 71:620-629
Ward JPT, Aaronson PI (1999) Mechanisms of hypoxic pulmonary vasoconstriction: can anyone be right? Respir Physiol 115:261-271
Naeije R, Brimioulle S (2001) Physiology in medicine: importance of hypoxic pulmonary vasoconstriction in maintaining arterial oxygenation during acute respiratory failure. Crit Care 5:67-71
Weir EK, Olschewski A (2006) Role of ion channels in acute and chronic responses of the pulmonary vasculature to hypoxia. Cardiovasc Res 71:630-641
Weissmann N, Dietrich A, Fuchs B et al (2006) Classical transient receptor potential channel 6 (TRPC6) is essential for hypoxic pulmonary vasoconstriction and alveolar gas exchange. Proc Natl Acad Sci U S A 103:19093-19098
Weissmann N, Grimminger F, Walmrath D, Seeger W (1995) Hypoxic vasoconstriction in buffer-perfused rabbit lungs. Respir Physiol 100:159-169
Sham JSK (2002) Hypoxic pulmonary vasoconstriction: ups and downs of reactive oxygen species. Circ Res 91:649-651
Weissmann N, Grimminger F, Olschewski A, Seeger W (2001) Hypoxic pulmonary vasoconstriction: a multifactorial response? Am J Physiol Lung Cell Mol Physiol 281:L314-L317
Dietrich A, Kalwa H, Fuchs B, Grimminger F, Weissmann N (2007) Gudermann T. In vivo TRPC functions in the cardiopulmonary vasculature. Cell Calcium 42:233-244
McDaniel SS, Platoshyn O, Wang J et al (2001) Capacitative Ca2+ entry in agonist-induced pulmonary vasoconstriction. Am J Physiol Lung Cell Mol Physiol 280:L870-L880
Wang J, Shimoda LA, Sylvester JT (2004) Capacitative calcium entry and TRPC channel proteins are expressed in rat distal pulmonary arterial smooth muscle. Am J Physiol Lung Cell Mol Physiol 286:L848-L858
Ward JPT, Robertson TP, Aaronson PI (2005) Capacitative calcium entry: a central role in hypoxic pulmonary vasoconstriction? Am J Physiol Lung Cell Mol Physiol 289:L2-L4
Wang J, Shimoda LA, Weigand L, Wang W, Sun D, Sylvester JT (2005) Acute hypoxia increases intracellular [Ca2+] in pulmonary arterial smooth muscle by enhancing capacitative Ca2+ entry. Am J Physiol Lung Cell Mol Physiol 288:L1059-L1069
Weigand L, Foxson J, Wang J, Shimoda LA, Sylvester JT (2005) Inhibition of hypoxic pulmonary vasoconstriction by antagonists of store-operated Ca2+ and nonselective cation channels. Am J Physiol Lung Cell Mol Physiol 289:L5-L13
Dietrich A, Chubanov V, Kalwa H, Rost BR, Gudermann T (2006) Cation channels of the transient receptor potential superfamily: their role in physiological and pathophysiological processes of smooth muscle cells. Pharmacol Ther 112:744-760
Hardie RC, Minke B (1993) Novel Ca2+ channels underlying transduction in Drosophila photoreceptors: implications for phosphoinositide-mediated Ca2+ mobilization. Trends Neurosci 16:371-376
Montell C, Rubin GM (1989) Molecular characterization of the Drosophila trp locus: a putative integral membrane protein required for phototransduction. Neuron 2:1313-1323
Minke B, Selinger Z (1996) The roles of trp and calcium in regulating photoreceptor function in Drosophila. Curr Opin Neurobiol 6:459-466
Zhu X, Chu PB, Peyton M, Birnbaumer L (1995) Molecular cloning of a widely expressed human homologue for the Drosophila trp gene. FEBS Lett 373:193-198
Firth AL, Remillard CV, Yuan JX-J (2007) TRP channels in hypertension. Biochim Biophys Acta 1772:895-906
Targos B, Ska J, Pomorski P (2005) Store-operated calcium entry in physiology and pathology of mammalian cells. Acta Biochim Pol 52:379-409
Freichel M, Vennekens R, Olausson J et al (2004) Functional role of TRPC proteins in vivo: lessons from TRPC-deficient mouse models. Biochem Biophys Res Commun 322:1352-1358
Dietrich A, Schnitzler M, Kalwa H, Storch U, Gudermann T (2005) Functional characterization and physiological relevance of the TRPC3/6/7 subfamily of cation channels. Naunyn Schmiedebergs Arch Pharmacol 371:257-265
Beech DJ (2005) Emerging functions of 10 types of TRP cationic channel in vascular smooth muscle. Clin Exp Pharmacol Physiol 32:597-603
Dietrich A, Mederos YS, Gollasch M et al (2005) Increased vascular smooth muscle contractility in TRPC6-/- mice. Mol Cell Biol 25:6980-6989
Sel S, Rost BR, Yildirim AO et al (2008) Loss of classical transient receptor potential 6 channel reduces allergic airway response. Clin Exp Allergy 38:1548-1558
Ward JPT, Snetkov VA, Aaronson PI (2004) Calcium, mitochondria and oxygen sensing in the pulmonary circulation. Cell Calcium 36:209-220
Sweeney M, Yuan JX-J (2000) Hypoxic pulmonary vasoconstriction: role of voltage-gated potassium channels. Respir Res 1:40-48
Landsberg JW, Yuan JX-J (2004) Calcium and TRP channels in pulmonary vascular smooth muscle cell proliferation. News Physiol Sci 1944-1950
Aaronson PI, Robertson TP, Knock GA et al (2006) Hypoxic pulmonary vasoconstriction: mechanisms and controversies. J Physiol 570:53-58
Beech DJ, Muraki K, Flemming R (2004) Non-selective cationic channels of smooth muscle and the mammalian homologues of Drosophila TRP. J Physiol 559:685-706
Birnbaumer L, Zhu X, Jiang M et al (1996) On the molecular basis and regulation of cellular capacitative calcium entry: roles for Trp proteins. Proc Natl Acad Sci U S A 93:15195-15202
Marshall C, Mamary AJ, Verhoeven AJ, Marshall BE (1996) Pulmonary artery NADPH-oxidase is activated in hypoxic pulmonary vasoconstriction. Am J Respir Cell Mol Biol 15:633-644
Waypa GB, Chandel NS, Schumacker PT (2001) Model for hypoxic pulmonary vasoconstriction involving mitochondrial oxygen sensing. Circ Res 88:1259-1266
Waypa GB, Marks JD, Mack MM, Boriboun C, Mungai PT, Schumacker PT (2002) Mitochondrial reactive oxygen species trigger calcium increases during hypoxia in pulmonary arterial myocytes. Circ Res 91:719-726
Sham JSK, Crenshaw BR Jr, Deng LH, Shimoda LA, Sylvester JT (2000) Effects of hypoxia in porcine pulmonary arterial myocytes: roles of KV channel and endothelin-1. Am J Physiol Lung Cell Mol Physiol 279:L262-L272
Turner JL, Kozlowski RZ (1997) Relationship between membrane potential, delayed rectifier K+ currents and hypoxia in rat pulmonary arterial myocytes. Exp Physiol 82:629-645
Estacion M, Sinkins WG, Jones SW, Applegate MA, Schilling WP (2006) Human TRPC6 expressed in HEK 293 cells forms non-selective cation channels with limited Ca2+ permeability. J Physiol 572:359-377
Gudermann T, Mederos y Schnitzler M, Dietrich A (2004) Receptor-operated cation entry - more than esoteric terminology? Sci STKE 2004:e35
Soboloff J, Spassova M, Xu W, He LP, Cuesta N, Gill DL (2005) Role of endogenous TRPC6 channels in Ca2+ signal generation in A7r5 smooth muscle cells. J Biol Chem 280:39786-39794
French RJ, Wells JB (1977) Sodium ions as blocking agents and charge carriers in the potassium channel of the squid giant axon. J Gen Physiol 70:707-724
Archer SL, London B, Hampl V et al (2001) Impairment of hypoxic pulmonary vasoconstriction in mice lacking the voltage-gated potassium channel Kv1.5. FASEB J 15:1801-1803
Keserü B, Barbosa-Sicard E, Popp R et al (2008) Epoxyeicosatrienoic acids and the soluble epoxide hydrolase are determinants of pulmonary artery pressure and the acute hypoxic pulmonary vasoconstrictor response. FASEB J 22:4306-4315
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2010 Humana Press, a part of Springer Science+Business Media, LLC
About this paper
Cite this paper
Fuchs, B., Dietrich, A., Gudermann, T., Kalwa, H., Grimminger, F., Weissmann, N. (2010). The Role of Classical Transient Receptor Potential Channels in the Regulation of Hypoxic Pulmonary Vasoconstriction. In: Yuan, JJ., Ward, J. (eds) Membrane Receptors, Channels and Transporters in Pulmonary Circulation. Advances in Experimental Medicine and Biology, vol 661. Humana Press, Totowa, NJ. https://doi.org/10.1007/978-1-60761-500-2_12
Download citation
DOI: https://doi.org/10.1007/978-1-60761-500-2_12
Published:
Publisher Name: Humana Press, Totowa, NJ
Print ISBN: 978-1-60761-499-9
Online ISBN: 978-1-60761-500-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)