Abstract
Very little is known about the molecular biology of CTCs. The paucity of information can be largely attributed to the technical hurdles in isolating these extremely rare cells. Despite these challenges, there is a pressing need to elucidate the molecular characteristics of these tumor cells. In this chapter, we highlight recent studies on genome-wide gene copy number analysis of CTCs and comparisons with primary tumors. These initial studies serve as groundwork for future efforts in discovery and development of novel CTC-based genomic biomarkers. Further molecular profiling of CTCs may provide novel insights into mechanisms of disease progression and tumor evolution, and open new avenues for personalized treatment.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Circulating tumor cells
- Molecular characterization
- Copy number analysis
- Array comparative genomic hybridizations
- Genomic instability
- Fluorescence-activated cell sorting
- Genomic analysis
- Copy number variation
- Metastasis
1 Introduction
Metastatic spread involves the escape of tumor cells from primary tumors into the blood stream. These tumor cells, also known as circulating tumor cells (CTCs), can migrate to distant sites and initiate metastatic disease. Since the advent of technologies to sensitively detect and count (“enumerate”) CTCs, it has been demonstrated that elevated numbers of CTCs in the blood of solid tumor patients can portend poor survival [1–5].
The underlying biology of the CTCs themselves remains poorly understood. In principle, molecular characterization of CTCs can provide new insights into the biology of cancer metastasis, as well as new biomarkers for personalized treatment. However, progress has been hindered by the formidable technical challenges in efficiently isolating these extremely rare cells (~ one CTC per billion of nucleated blood cells).
A hallmark of cancer is genomic instability [6, 7]. Genome-wide copy number aberrations can be assessed using microarrays (e.g., array comparative genomic hybridization, aCGH) [8] and more recently by next generation (massively parallel) sequencing [9]. Studies involving genome-wide copy number analysis of primary tumors have shown that certain chromosomal regions may be preferentially amplified or deleted in different types of cancers [7, 10–12].
Investigations of genomic alterations in CTCs, including comparative analysis with primary tumors, have recently been reported. In this chapter, we discuss results of genome-wide copy number analysis of CTCs in different solid tumors, including prostate, colorectal, and lung cancers.
2 Enrichment and Isolation of CTCs
2.1 EpCAM-Based Isolation
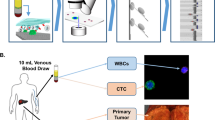
Most strategies to isolate CTCs have included EPCAM-based immunomagnetic enrichment methods (e.g., the widely used CellSearch system [13]), which involves the capture of CTCs using magnetic beads conjugated with EPCAM antibody. The enriched population, however, still retains a considerable amount of leukocytes requiring additional steps to further purify CTCs [14]. We have developed a protocol, referred to as “IE/FACS”, to isolate highly pure CTC populations from blood [15–17]. IE/FACS consists of an initial immunomagnetic enrichment step similar to that of the CellSearch system. This is followed by the addition of fluorescently labeled monoclonal antibodies specific for leukocytes (CD45) and epithelial cells (EPCAM ) to distinguish CTCs from leukocytes during sorting via fluorescence-activated cell sorting (FACS).
2.2 Non-EpCAM-Based Isolation
Alternative CTC collection strategies include those based on physical properties, e.g., size and density, which allow separation of CTCs from patients’ peripheral normal blood cells [18]. Yet another enrichment approach is based on metastatic cells’ ability to adhere and invade collagen adhesion matrix (CAM) [19]. Using a specialized tube (Vita-Cap™), CTCs adhere to CAM-coated inner walls and non-adherent blood cells are washed away. Collagenase treatment releases the CTCs as well as leukocytes that are nonspecifically attached to the matrix [20, 21].
A comprehensive discussion on the methods involving CTC enrichment and isolation is presented in Chaps. 2 and 3.
3 Genome-Wide Copy Number Analysis of CTCs
3.1 Early Breast Cancer
Since CTCs are much less frequent in early versus metastatic breast cancer, larger volumes of blood are necessary for routine screening to detect these rare tumor cells [22]. To address this limitation, a recent study demonstrated the feasibility of utilizing leukapheretic samples to capture CTCs in early breast cancer patients [23]. Examining whole circulating blood substantially increased CTC detection to about 90 % as compared to 5–24 % in ~10–30 mL of blood [22, 24]. Genomic profiling of captured single CTCs via metaphase CGH analysis detected genomic aberrations in a subset of cells. Aberrations were consistent with that of breast cancer, e.g., loss of 8p and gain of 8q. Additionally, higher levels of genomic alterations were correlated with increased risk of recurrence.
3.2 Metastatic Breast Cancer
Our group has combined IE/FACS and array comparative genomic hybridization (aCGH) to perform the genome-wide copy number analysis of CTCs from breast cancer patients [16]. This approach involves efficient and complete isolation of CTCs for molecular profiling; in contrast, methods to capture CTCs via cell adherence, microfluidics, or immunomagnetic separation alone typically entail substantial leukocyte contamination and can compromise the ability to perform genome-wide analyses. Our approach yields genomic profiles of CTCs without significant contamination from leukocytes or non-malignant epithelial cells.
Initial assay validation using breast cancer cells spiked into healthy blood confirmed that accurate aCGH profiles were obtained from small pools of cells, including single cells and showed no evidence of leukocyte contamination. We subsequently applied this approach to blood samples from 181 metastatic breast cancer patients, 102 of which were successfully profiled. Genomic profiling of CTCs revealed numerous copy number alterations, including many previously reported in primary breast tumors, confirming the malignant nature of the CTCs.
Frequent copy number aberrations identified in our series of 102 CTC samples included gains in 1q and 8q and losses in 1p, 2q, 4q, 8p, 11q, 13q, 15q, 16q, and 18q (Fig. 10.1a). Focal amplifications included 8p11-12 (FGFR1), 8q24 (MYC), 11q13 (CNND1), 17q12 (HER2), and 20q13 (ZNF217). Comparative analysis between CTC profiles in this study versus primary breast tumor profiles from previously published aCGH datasets by Fridlyand et al. [10] (N = 62) (Fig. 10.1b) and by Chin et al. [25] (N = 137) (Fig. 10.1c) revealed high concordance of gains and losses. Recurrent focal amplifications in CTCs were also frequently observed in both Fridlyand and Chin datasets, e.g., on 8p (including FGFR1), 8q (MYC), 11q13 (including CCND1), 17q (ERBB2) and regions on 20q (including ZNF217).
Copy number analysis of breast CTCs and primary tumors. Recurrent gene copy number aberrations in (a) CTCs from 102 metastatic breast cancer patients [16] and (b) in 62 primary breast tumors [10] and (c) 137 primary breast tumors [25]. Gains and losses are shown in red and blue, respectively. (Reprinted from Magbanua et al. 2013, Cancer research 73(1):30–40)
Next, we compared our CTC CGH dataset and the Fridlyand et al. dataset [10] to explore genomic aberrations specifically prevalent in CTCs but not in primary tumors. Results of this exploratory comparative analysis suggested that specific aberrations including losses on 10q22 and 8p23 and gains on 5q13 (including CCNB1), 7q22 (including MUC12 and MUC17), 9p13 and 9q31 were significantly more frequent in CTCs compared to primary tumors (Table 10.1). Because these two datasets were totally independent (i.e., CTCs and primary tumors were not from the same patients), we also showed the feasibility of comparing aCGH profiles from CTCs versus matched primary tumors in a series of five cases .
Comparison of CTCs with matched archival primary tumors (N = 5 pairs) confirmed shared lineage as well as some divergence. Our results indicated a clear clonal relationship between primary tumors and subsequent CTCs, and the appearance of new, as well as conserved, genomic alterations. Two examples are discussed below:
Case 1. Twenty CTCs were isolated at two different time points (Days 1 and 42) from a metastatic breast cancer patient #4013, a 50-year-old female with ER/PR positive and HER2 positive disease. Comparison of the CTC profiles revealed high concordance. Focal amplifications on 8q24, 12q15, 17q12 (HER2), and 20q13 were observed in both samples (Fig. 10.2a). Next, archival primary tumor from 6 years prior to CTC analysis was obtained and analyzed via aCGH. Copy number analysis showed multiple aberrations in common with the CTC samples, including the same focal amplifications. Interestingly, some aberrations, e.g., losses in 6q, 13q, 18q, and 20p, were observed only in CTCs and not in the primary tumor suggesting that these cells had acquired additional alterations.
Case studies for genomic profiling of breast CTCs and matched primary tumor. (a) Genomic profiles of 20 CTCs isolated from two independent blood draws (days 1 and 42) and the primary tumor of patient #4013. The patient’s primary tumor was surgically removed 6 years prior to the CTC assays. Arrow indicates HER2 amplification on chromosome 17. (b) Genomic profiles of 20 CTCs, primary tumor and nodal metastasis from patient #4015. The patient’s primary tumor and lymph node were surgically removed 2.5 years prior to the CTC assays. The log2 ratio value for each BAC clone is plotted on the y-axis. The x-axis represents the genomic position of each BAC clone on the array, with chromosome numbers indicated. Vertical solid lines indicate chromosome boundaries, and vertical red dashed line represents the centromeric region dividing each chromosome into the p- or short arm (to the left of the centromere) and the q- or long arm (to the right of the centromere). Color represents gene copy number status red = loss, green = gain, blue = amplification, and black = no change. (Adapted from Magbanua et al. 2013, Cancer research 73(1):30–40)
Case 2. Twenty CTCs were isolated from a metastatic breast cancer patient #4015, a 54-year-old female with triple negative disease. Copy number analysis of CTCs showed losses in 3p, 5q, and 6q and focal amplification on 8q24, gains in 10p and 19q (Fig. 10.2b). The archival primary tumor and a lymph node metastasis from 2.5 years prior were then obtained and subjected to aCGH analysis. Copy number profiles of the primary tumor and nodal metastasis, were highly correlated with each other, but to a lesser degree with the CTC profile. CTCs exhibited additional genomic aberrations, e.g., gain in 20q and loss in 3p that were not observed in the primary tumor and nodal metastasis.
3.3 Prostate Cancer
Our group has also performed IE/FACS to isolate and analyze prostate CTCs from castration resistant prostate cancer patients [17]. Copy number analysis of CTCs from nine patients revealed a wide range of copy number aberrations, including those that have been previously reported in prostate tumors, e.g., loss in 8p and gain on 8q [11, 26] (Fig. 10.3). However, unlike primary tumors, high-level gains in a region containing the androgen receptor (AR) gene in the X chromosome was observed in seven (78 %) of the nine cases, while low level gains were observed in the remaining two (22 %) cases. Amplification of AR in CTCs is consistent with observations in castration resistant prostate solid tumors [26]. In addition, comparison of genomic profiles between CTCs from two patients with the corresponding pretreatment primary tumors revealed clonal-relatedness with some divergence including amplification of the locus containing the AR region in CTCs but not in the matched primary tissues. This study confirmed other findings by FISH analysis [27, 28] that the AR gene can be amplified in CTCs from castration resistant prostate cancer patients in association with hormone resistance.
Copy number analysis of CTCs from metastatic castration-resistant prostate cancer patients. Recurrent gene copy number aberrations in CTCs from nine patients; gains and losses are shown in green and red, respectively. Chromosome Y was not included in the analysis. (Reprinted with permission from Magbanua et al. 2012, BMC Cancer 12(1):78)
A CAM-adherence approach was used by Paris and colleagues to enrich for CTCs from blood of 13 metastatic prostate cancer patients [21]. CAM-captured cells including co-purified background leukocytes were subjected to aCGH analysis. Analysis of recurrent aberrations in CTCs from nine patients successfully profiled revealed copy number alterations in cancer related genes (e.g., POTE15 and GSTT1). In contrast to IE/FACS isolated CTCs (discussed above), amplification of the AR gene and aberrations (e.g., loss of 8p and gain of 8q) frequently seen in prostate cancers were not observed in CAM-enriched cells. Comparison of genomic profiles of CTCs with primary and metastatic tumors from two patients revealed high concordance.
3.4 Colorectal Cancer
In a study involving six metastatic colorectal cancer patients, CTCs were enriched using the CellSearch method followed by isolation of single cells via micromanipulation and aCGH analysis [29]. Analysis of genomic profiles revealed copy number aberrations in CTCs that were commonly seen in colorectal cancer, e.g., losses in 5q13–5q31 which contain the adenomatous polyposis coli (APC) gene. Despite some divergent genomic aberrations, genomic profiles of single CTCs were very similar to that of matched primary tumor and metastatic lesions. Additionally, copy number profiles revealed “private” aberrations that were unique to single cells.
3.5 Lung Cancer
A similar CellSearch-based approach was used to isolate single CTCs from 11 lung cancer patients [30]. Copy number data was inferred from next generation low pass whole genome sequencing (0.1× coverage). Comparisons of copy number profiles revealed high similarities of genomic profiles among single CTCs from the same patient and among patients. Clonal-relatedness was observed when single cell profiles were compared to primary tumors and available metastatic lesions from the same patient. Interestingly, distinct global copy number profiles were observed between small-cell lung cancer and lung adenocarcinoma.
3.6 Melanoma
A study by Chiu and colleagues [31] demonstrated the feasibility of genome-wide copy number profiling of CTCs from melanoma patients with regional metastasis. Antibodies against melanoma-associated cell surface gangliosides were utilized to capture circulating melanoma cells instead of epithelial markers. Array CGH analysis of putative circulating melanoma cells revealed copy number gains (e.g., 2q35) and losses (e.g., 6q25.3 and 9q34.3) that were observed in all patient samples. Similar copy number aberrations were seen in circulating melanoma cells and in regional metastasis from the same patient. Interestingly, CTC-associated copy number aberrations were also identified in distant metastasis from advanced melanoma patients, suggesting that certain genomic aberrations are selected for in the course of disease progression. Finally, a biomarker panel composed of five CTC-associated genomic aberrations was able to identify stage IIIB/C melanoma patients with poor clinical outcome.
4 Discussion and Summary
Mechanisms involved in cancer progression, including distant metastasis and resistance to treatment, remain elusive. CTCs accessed from the blood may provide insights into how cancers spread and why patients fail to respond to therapies.
In-depth molecular analysis of CTC is fundamental to the elucidation of their role in metastasis. This includes the systematic survey of genomic aberrations throughout the genome, e.g., chromosome gains, losses and focal amplifications, which are hallmarks of malignancy [7]. Initial characterizations of CTCs using fluorescence in situ hybridization (FISH) showed the feasibility of assaying for particular amplification events in CTCs [32–34]. More recently, genome-wide copy number analyses have been reported. The results of these studies, as summarized in this chapter, provide clear evidence that cancer-associated genomic changes can be detected in CTCs [16, 17, 23, 29–31]
Approaches for isolation of CTCs are based on different biological and physical parameters, which may lead to a bias towards certain CTC populations [18, 35]. For example, CTCs from castration resistant prostate cancer patients captured via CAM-adherence [21] and EPCAM-based [17] methods revealed distinct copy number profiles. It is therefore important to consider the limitations of the capture methods utilized when analyzing CTC genotypes/phenotypes.
The genetic relationship between CTCs and solid tumor tissues obtained from the same patient may shed new light on the mechanisms involved in tumor evolution and progression. Comparative studies between CTCs and corresponding primary and metastatic lesions have confirmed clonal-relatedness [16, 17, 21, 29, 30]. Identification of specific molecular signatures and genetic changes that occur in CTCs could lead to new targets for anti-metastatic therapies and druggable biomarkers.
In the treatment of advanced cancer patients, reliance upon biomarkers obtained from primary tumors has always been a problematic and questionable practice. Recent studies have confirmed that CTCs have the potential to acquire new genomic aberrations, including those potentially associated with disease progression and treatment resistance [16, 29, 30, 34]. CTC-based biomarkers, therefore, may provide more relevant information about molecular target status as well as disease behavior. In the future, clinicians may be able to draw upon molecular profiles of CTCs to provide a more individualized and efficacious treatment.
In conclusion, molecular characterization of CTCs provides an opportunity to develop biomarkers for metastatic breast cancer treatment that are more accessible (via blood sampling as a “liquid biopsy”) and more relevant (reflecting changes associated with metastasis and disease progression) than primary tumor tissue. CTC-based assays can in principle provide easily accessible biomarker information and may be more insightful than those based on primary tumors due to greater relevance to metastatic disease, serial sampling ability, and contemporaneous acquisition with cancer progression. Employing new and powerful approaches including genome-wide profiling of CTCs may provide new insights into mechanisms of disease progression and treatment response/resistance, and open new avenues for biomarker development and personalized treatment.
References
Cristofanilli M, Budd GT, Ellis MJ, Stopeck A, Matera J, Miller MC, Reuben JM, Doyle GV, Allard WJ, Terstappen LW, Hayes DF (2004) Circulating tumor cells, disease progression, and survival in metastatic breast cancer. N Engl J Med 351(8):781–791
Liu MC, Shields PG, Warren RD, Cohen P, Wilkinson M, Ottaviano YL, Rao SB, Eng-Wong J, Seillier-Moiseiwitsch F, Noone AM, Isaacs C (2009) Circulating tumor cells a useful predictor of treatment efficacy in metastatic breast cancer. J Clin Oncol 27(31):5153–5159
Cohen SJ, Punt CJ, Iannotti N, Saidman BH, Sabbath KD, Gabrail NY, Picus J, Morse M, Mitchell E, Miller MC, Doyle GV, Tissing H, Terstappen LW, Meropol NJ (2008) Relationship of circulating tumor cells to tumor response, progression-free survival, and overall survival in patients with metastatic colorectal cancer. J Clin Oncol 26(19):3213–3221
Danila DC, Heller G, Gignac GA, Gonzalez-Espinoza R, Anand A, Tanaka E, Lilja H, Schwartz L, Larson S, Fleisher M, Scher HI (2007) Circulating tumor cell number and prognosis in progressive castration-resistant prostate cancer. Clin Cancer Res 13(23):7053–7058
de Bono JS, Scher HI, Montgomery RB, Parker C, Miller MC, Tissing H, Doyle GV, Terstappen LW, Pienta KJ, Raghavan D (2008) Circulating tumor cells predict survival benefit from treatment in metastatic castration-resistant prostate cancer. Clin Cancer Res 14(19):6302–6309. doi:10.1158/1078-0432.CCR-08-0872, 14/19/6302 [pii]
Hanahan D, Weinberg RA (2011) Hallmarks of cancer the next generation. Cell 144(5):646–674. doi:10.1016/j.cell.2011.02.013
Albertson DG, Collins C, McCormick F, Gray JW (2003) Chromosome aberrations in solid tumors. Nat Genet 34(4):369–376
Pinkel D, Albertson DG (2005) Comparative genomic hybridization. Annu Rev Genomics Hum Genet 6:331–354
Wood HM, Belvedere O, Conway C, Daly C, Chalkley R, Bickerdike M, McKinley C, Egan P, Ross L, Hayward B, Morgan J, Davidson L, MacLennan K, Ong TK, Papagiannopoulos K, Cook I, Adams DJ, Taylor GR, Rabbitts P (2010) Using next-generation sequencing for high resolution multiplex analysis of copy number variation from nanogram quantities of DNA from formalin-fixed paraffin-embedded specimens. Nucleic Acids Res 38(14):e151. doi:10.1093/nar/gkq510
Fridlyand J, Snijders AM, Ylstra B, Li H, Olshen A, Segraves R, Dairkee S, Tokuyasu T, Ljung BM, Jain AN, McLennan J, Ziegler J, Chin K, Devries S, Feiler H, Gray JW, Waldman F, Pinkel D, Albertson DG (2006) Breast tumor copy number aberration phenotypes and genomic instability. BMC Cancer 6:96
Liu W, Laitinen S, Khan S, Vihinen M, Kowalski J, Yu G, Chen L, Ewing CM, Eisenberger MA, Carducci MA, Nelson WG, Yegnasubramanian S, Luo J, Wang Y, Xu J, Isaacs WB, Visakorpi T, Bova GS (2009) Copy number analysis indicates monoclonal origin of lethal metastatic prostate cancer. Nat Med 15(5):559–565. doi:10.1038/nm.1944
Nakao K, Mehta KR, Fridlyand J, Moore DH, Jain AN, Lafuente A, Wiencke JW, Terdiman JP, Waldman FM (2004) High-resolution analysis of DNA copy number alterations in colorectal cancer by array-based comparative genomic hybridization. Carcinogenesis 25(8):1345–1357. doi:10.1093/carcin/bgh134
Attard G, de Bono JS (2011) Utilizing circulating tumor cells challenges and pitfalls. Curr Opin Genet Dev 21(1):50–58. doi:10.1016/j.gde.2010.10.010
Pantel K, Brakenhoff RH, Brandt B (2008) Detection, clinical relevance and specific biological properties of disseminating tumour cells. Nat Rev Cancer 8(5):329–340. doi:10.1038/nrc2375
Magbanua MJ, Park JW (2013) Isolation of circulating tumor cells by immunomagnetic enrichment and fluorescence-activated cell sorting (IE/FACS) for molecular profiling. Methods 64(2):114–118. doi:10.1016/j.ymeth.2013.07.029
Magbanua MJ, Sosa EV, Roy R, Eisenbud LE, Scott JH, Olshen A, Pinkel D, Rugo HS, Park JW (2013) Genomic profiling of isolated circulating tumor cells from metastatic breast cancer patients. Cancer Res 73(1):30–40. doi:10.1158/0008-5472.CAN-11-3017
Magbanua MJ, Sosa EV, Scott JH, Simko J, Collins C, Pinkel D, Ryan CJ, Park JW (2012) Isolation and genomic analysis of circulating tumor cells from castration resistant metastatic prostate cancer. BMC Cancer 12:78. doi:10.1186/1471-2407-12-78
Alix-Panabieres C, Pantel K (2013) Circulating tumor cells liquid biopsy of cancer. Clin Chem 59(1):110–118. doi:10.1373/clinchem.2012.194258
Yamada KM, Cukierman E (2007) Modeling tissue morphogenesis and cancer in 3D. Cell 130(4):601–610. doi:10.1016/j.cell.2007.08.006
Lu J, Fan T, Zhao Q, Zeng W, Zaslavsky E, Chen JJ, Frohman MA, Golightly MG, Madajewicz S, Chen WT (2010) Isolation of circulating epithelial and tumor progenitor cells with an invasive phenotype from breast cancer patients. Int J Cancer 126(3):669–683. doi:10.1002/ijc.24814
Paris PL, Kobayashi Y, Zhao Q, Zeng W, Sridharan S, Fan T, Adler HL, Yera ER, Zarrabi MH, Zucker S, Simko J, Chen WT, Rosenberg J (2009) Functional phenotyping and genotyping of circulating tumor cells from patients with castration resistant prostate cancer. Cancer Lett 277(2):164–173
Lucci A, Hall CS, Lodhi AK, Bhattacharyya A, Anderson AE, Xiao L, Bedrosian I, Kuerer HM, Krishnamurthy S (2012) Circulating tumour cells in non-metastatic breast cancer a prospective study. Lancet Oncol 13(7):688–695. doi:10.1016/S1470-2045(12)70209-7
Fischer JC, Niederacher D, Topp SA, Honisch E, Schumacher S, Schmitz N, Zacarias Fohrding L, Vay C, Hoffmann I, Kasprowicz NS, Hepp PG, Mohrmann S, Nitz U, Stresemann A, Krahn T, Henze T, Griebsch E, Raba K, Rox JM, Wenzel F, Sproll C, Janni W, Fehm T, Klein CA, Knoefel WT, Stoecklein NH (2013) Diagnostic leukapheresis enables reliable detection of circulating tumor cells of nonmetastatic cancer patients. Proc Natl Acad Sci U S A 110(41):16580–16585. doi:10.1073/pnas.1313594110
Franken B, de Groot MR, Mastboom WJ, Vermes I, van der Palen J, Tibbe AG, Terstappen LW (2012) Circulating tumor cells, disease recurrence and survival in newly diagnosed breast cancer. Breast Cancer Res 14(5):R133. doi:10.1186/bcr3333
Chin K, DeVries S, Fridlyand J, Spellman PT, Roydasgupta R, Kuo WL, Lapuk A, Neve RM, Qian Z, Ryder T, Chen F, Feiler H, Tokuyasu T, Kingsley C, Dairkee S, Meng Z, Chew K, Pinkel D, Jain A, Ljung BM, Esserman L, Albertson DG, Waldman FM, Gray JW (2006) Genomic and transcriptional aberrations linked to breast cancer pathophysiologies. Cancer Cell 10(6):529–541
Visakorpi T, Hyytinen E, Koivisto P, Tanner M, Keinanen R, Palmberg C, Palotie A, Tammela T, Isola J, Kallioniemi OP (1995) In vivo amplification of the androgen receptor gene and progression of human prostate cancer. Nat Genet 9(4):401–406. doi:10.1038/ng0495-401
Attard G, Swennenhuis JF, Olmos D, Reid AH, Vickers E, A’Hern R, Levink R, Coumans F, Moreira J, Riisnaes R, Oommen NB, Hawche G, Jameson C, Thompson E, Sipkema R, Carden CP, Parker C, Dearnaley D, Kaye SB, Cooper CS, Molina A, Cox ME, Terstappen LW, de Bono JS (2009) Characterization of ERG, AR and PTEN gene status in circulating tumor cells from patients with castration-resistant prostate cancer. Cancer Res 69(7):2912–2918. doi:10.1158/0008-5472.CAN-08-3667
Leversha MA, Han J, Asgari Z, Danila DC, Lin O, Gonzalez-Espinoza R, Anand A, Lilja H, Heller G, Fleisher M, Scher HI (2009) Fluorescence in situ hybridization analysis of circulating tumor cells in metastatic prostate cancer. Clin Cancer Res 15(6):2091–2097
Heitzer E, Auer M, Gasch C, Pichler M, Ulz P, Hoffmann EM, Lax S, Waldispuehl-Geigl J, Mauermann O, Lackner C, Hofler G, Eisner F, Sill H, Samonigg H, Pantel K, Riethdorf S, Bauernhofer T, Geigl JB, Speicher MR (2013) Complex tumor genomes inferred from single circulating tumor cells by array-CGH and next-generation sequencing. Cancer Res 73(10):2965–2975. doi:10.1158/0008-5472.CAN-12-4140
Ni X, Zhuo M, Su Z, Duan J, Gao Y, Wang Z, Zong C, Bai H, Chapman AR, Zhao J, Xu L, An T, Ma Q, Wang Y, Wu M, Sun Y, Wang S, Li Z, Yang X, Yong J, Su XD, Lu Y, Bai F, Xie XS, Wang J (2013) Reproducible copy number variation patterns among single circulating tumor cells of lung cancer patients. Proc Natl Acad Sci U S A. doi:10.1073/pnas.1320659110
Chiu CG, Nakamura Y, Chong KK, Huang SK, Kawas NP, Triche T, Elashoff D, Kiyohara E, Irie RF, Morton DL, Hoon DS (2014) Genome-wide characterization of circulating tumor cells identifies novel prognostic genomic alterations in systemic melanoma metastasis. Clin Chem 60:875–885. doi:10.1373/clinchem.2013.213611
Engel H, Kleespies C, Friedrich J, Breidenbach M, Kallenborn A, Schondorf T, Kolhagen H, Mallmann P (1999) Detection of circulating tumour cells in patients with breast or ovarian cancer by molecular cytogenetics. Br J Cancer 81(7):1165–1173
Fehm T, Sagalowsky A, Clifford E, Beitsch P, Saboorian H, Euhus D, Meng S, Morrison L, Tucker T, Lane N, Ghadimi BM, Heselmeyer-Haddad K, Ried T, Rao C, Uhr J (2002) Cytogenetic evidence that circulating epithelial cells in patients with carcinoma are malignant. Clin Cancer Res 8(7):2073–2084
Meng S, Tripathy D, Shete S, Ashfaq R, Haley B, Perkins S, Beitsch P, Khan A, Euhus D, Osborne C, Frenkel E, Hoover S, Leitch M, Clifford E, Vitetta E, Morrison L, Herlyn D, Terstappen LW, Fleming T, Fehm T, Tucker T, Lane N, Wang J, Uhr J (2004) HER-2 gene amplification can be acquired as breast cancer progresses. Proc Natl Acad Sci U S A 101(25):9393–9398
Park JW (2011) Disseminated tumor cells the method is the message. Breast Cancer Res Treat 125(3):739–740. doi:10.1007/s10549-010-1107-5
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer Science+Business Media New York
About this chapter
Cite this chapter
Magbanua, M.J.M., Park, J.W. (2016). Genome-Wide Gene Copy Number Analysis of Circulating Tumor Cells. In: Cote, R., Datar, R. (eds) Circulating Tumor Cells. Current Cancer Research. Springer, New York, NY. https://doi.org/10.1007/978-1-4939-3363-1_10
Download citation
DOI: https://doi.org/10.1007/978-1-4939-3363-1_10
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4939-3361-7
Online ISBN: 978-1-4939-3363-1
eBook Packages: MedicineMedicine (R0)