Abstract
Sleep disturbance and coexisting pain are common experiences in a variety of disease states or chronic conditions. These symptoms affect a large number of people worldwide and have serious negative consequences on health, quality of life, and work productivity as well as the rising costs of health care. Yet, despite the prevalence of sleep and comorbid pain, there is little evidence from research upon which to build clinical guidelines or suggest best practices. Despite considerable advances in sleep and pain medicine, research studies on the nature of comorbid sleep disturbance and pain only have just begun to appear in the literature. This chapter provides a critical commentary on the progress of the generation of research evidence on sleep disturbance and pain, and summarizes, as milestones, the accumulated evidence. This review includes selected preclinical studies, experimental human and clinical studies, as well as recent studies focused on interventions designed to improve sleep and reduce pain in people with chronic pain.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Sleep is a behavioral state that usually occurs naturally every day. Pain is a common experience but, unlike sleep, does not necessarily occur on a daily basis. Acute pain is a warning signal of potential, impending, or actual tissue injury. Chronic or pathologic pain is quite different. Accumulating evidence in pain science attests to the unique reorganization of pain pathways and ongoing plasticity within the brain that are distinctly associated with different chronic pain conditions (e.g., musculoskeletal, neuropathic) [1]. From elegant research in preclinical models and clinical studies, chronic pain is characterized by altered functioning of pain transduction, transmission, and modulation pathways in the central nervous system (CNS) such that nociceptive stimuli and tissue injury are no longer required for pain to be perceived. Episodes of spontaneous pain arise, non-nociceptive stimuli evoke pain sensations, and pain is perceived long after tissues have healed [2].
Regardless of whether pain is acute or chronic, there is a common expectation that pain will lead to disturbed sleep. Indeed, surveys attest to the prevalence of sleep problems in chronic pain conditions. Less than 20 years ago, the National Sleep Foundation conducted one of the first surveys on pain-related sleep disturbance in the USA [3]. This poll found that > 50 % of respondents from a large sample of adults reported nighttime pain; nearly half of the sample reported short sleep duration of ≤ 6 h. A recent survey of sleep and mental health from community-based samples in five European countries found a 17.1 % prevalence of a painful physical condition and a 10.3 % prevalence of insomnia symptoms (e.g., difficulty in falling asleep, staying asleep, or waking up early in the morning and unable to fall back to sleep) [4]. In this study, more than 20 % of individuals with a chronic pain condition reported insomnia, but strikingly 40.2 % of individuals reporting insomnia also reported chronic pain. Sleep disturbances and insomnia were the most frequent comorbidities reported in a large Internet survey of adults with chronic pain from five Western European countries [5], and the prevalence of insomnia was higher in individuals self-reporting neuropathic pain (46 %) compared to other types of chronic pain (30 %). Sleep disturbance in chronic pain conditions varies considerably from 40 % to over 85 % depending upon the clinic population studied and methods used to measure sleep [6–10]. Sleep disturbance is common in the elderly [11] and also in children and adolescents [12]; over 50 % of youth with chronic pain conditions report symptoms consistent with insomnia [13]. Despite the prevalence of pain-related sleep problems, research on the best methods for treating pain and improving sleep, or for improving sleep and reducing pain, is quite limited. The evidence base for the clinical management of sleep problems in chronic pain conditions has just begun to appear in the literature and much more research is needed [9, 14]. Pain and coexisting sleep disturbance complaints are common, a large number of people worldwide are affected, and have serious negative consequences on health, quality of life, and work productivity as well as the rising costs of health care.
Since one of the first polysomnographic studies of sleep reported by Wittig and colleagues in 1982 [15], research on interactions between sleep and pain has grown considerably. Based on recent review of PUBMED under a broad search of “sleep and pain,” 102 published references were accessible in 1992; 693 in 2012. Given the growing literature on the interaction of the problem of sleep disturbance in patients with pain, what do we know about the extent to which pain is associated with or leads to disturbed sleep? What do we know about the extent to which disturbed sleep modulates pain? Finally, what is the evidence that improving sleep relieves pain or vice versa? Considerable advances in pain science have been made in the past decade, especially in the use of brain imaging techniques applied to studies of individuals with chronic pain, and such advances have important implications for understanding the impact of pain on sleep. However, a discussion of milestones in pain science is beyond the scope of this review [1]. The purposes of this chapter are to summarize the milestones and provide a critical commentary on the progress of generating research evidence on interactions of pain and sleep. This review includes selected preclinical studies, experimental human and clinical studies, as well as recent studies focused on interventions designed to improve sleep and reduce pain in people with chronic pain.
Sleep and Pain Interaction
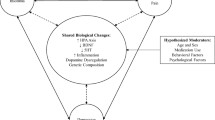
A current view of sleep and pain has evolved to a bidirectional model stipulating that disturbed sleep is a consequence of presleep pain intensity and disturbed sleep leads to enhanced post-sleep pain (Fig. 49.1a). This bidirectional model has roots in a circular model originally proposed by Moldofsky and colleagues [16] in pioneering studies of sleep disturbance in fibromyalgia. Moldofsky proposed that disturbed sleep did not cause pain, but that, once pain was manifest, disturbed sleep followed leading to a continuous cycle of pain, poor sleep, and amplified pain (Fig. 49.1b). The idea that sleep disturbance or sleep loss can amplify pain and feelings of discomfort has roots in common experience and findings from research. Sleep deprivation (SD) studies conducted in the 1930s, first, showed that 2 days of total sleep loss reduced the pain (nociceptive) threshold [17]. A more recent study has shown that sleep loss of only 4 h and specific loss of rapid eye movement (REM) sleep evoked hyperalgesia, but the mechanisms underlying the exaggerated responses to noxious stimuli remain unknown [18]. Although intuitively appealing and parsimonious, a bidirectional, linear model of pain leading to disturbed sleep and disturbed sleep leading to amplified pain is probably too simplistic. Likewise, a simple vicious cycle of pain-disturbed sleep pain fails to take into account other factors before, during, and after sleep that affect the interaction of pain and sleep (Fig. 49.1b).
a A bidirectional model assumes that higher pain intensity prior to sleep onset will lead to greater disturbed sleep; and greater disturbed sleep will lead to increased pain. b A circular model assumes that pain disturbs sleep and subsequently poor sleep affects pain. Various factors likely impact both pain and sleep and the interaction such that neither a linear nor a circular model fully accounts for the complexity of pain-related sleep disturbance
Chronic pain patients are heterogeneous, and all pain is not the same. Chronic pain is associated with many comorbidities including anxiety, depression, specific sleep disorders, poor sleep hygiene, and symptoms associated with source of the pain, such as musculoskeletal disorders [1, 19], depression [20], or neuropathic pain [1]. These patients are also at risk for undergoing multiple surgeries or other types of invasive treatments. They often consume many types of prescription and over-the-counter medications with adverse and unpredictable effects upon sleep. Further, sleep quality and duration are influenced by physical activity, fatigue, daytime naps, and lifestyle behaviors such as smoking and the consumption of caffeine and alcoholic beverages. These factors have not been assessed or accounted for in the statistical analysis in many research studies. Finally, gender differences have been observed in sleep [21] and in the prevalence of clinical pain syndromes [22]; these differences have only begun to be studied in a systematic way in patients with chronic pain [23].
Does Pain Lead to Disturbed Sleep?
Pain is a unique, personal, and subjective unpleasant experience with a combination of sensory, affective, and behavioral dimensions, most often, associated with actual or potential tissue damage [24]. From studies of preclinical pain models, considerable evidence has accumulated about the plasticity and heightened sensitivity of pain transduction, transmission, and modulation processes in peripheral nerves [25], neurons, and synapses in the CNS [2] in response to various types of nociceptive stimuli. Evidence from clinical studies suggests that peripheral and central sensitization contributes to pain in arthritis, temporomandibular disorders, fibromyalgia, headache, complex regional pain syndrome, visceral pain, and post-surgical pain [2].
The models used to study pain processing have been categorized into three phases representative of the type of nociceptive stimulus and the extent of tissue injury [26], and is a useful framework to assess the impact of pain on sleep. Phase 1 pain involves the transient application of a nociceptive stimulus, which produces a minimal inflammatory reaction and brief vocal (cry, ouch), behavioral (reflex withdrawal, body movement), or physiological (altered neuronal activity) responses. Phase 2 pain occurs as a result of the application of substances that induce tissue damage and inflammation that persist for varying periods of time depending upon the agent used. Phase 2 pain is associated with release of mediators in tissues from damaged cells, blood vessels, and activated peripheral nociceptors. These chemical mediators directly activate or sensitize primary afferent nerve fibers to increase transmission of nociceptive information to the spinal cord invoking hyperactive neuronal responses that underlie the development of hyperalgesia (exaggerated response to nociceptive stimuli) and allodynia (pain-related response to non-nociceptive stimuli). Phase 3 pain involves damage specifically to neurons and nerve fibers. Behavioral signs of spontaneous and evoked pain responses persist for varying periods of time as do changes in the functional properties of CNS neurons and synapses. Peripheral and central sensitization is associated with a change in the gain of pathways involved in pain transduction, transmission, and modulation such that nociceptive stimuli or tissue injury are no longer necessary for pain to be perceived.
Phase 1 Pain Studies
Studies of phase 1 pain applied to animals or human volunteers during sleep yield evidence of transient sleep disturbance. In all of the studies, the experimenter [27] or subjects reported at least moderate-level pain to nociceptive stimuli (e.g., saline infusions into muscle, finger joint pressure, cutaneous laser heat) when they were awake [28–30]. In animal studies, behavioral withdrawal responses to the application of phase 1 laser heat pain were faster during slow-wave sleep (SWS) compared to waking. The animals fell back to sleep quickly when stimulated during sleep, and showed more prolonged pain-related responses (orienting to the site, licking the paw, changing body position) and took a longer time to return to sleep during waking compared to sleep [27]. These results were interpreted as evidence of a lower-pain threshold during SWS that were attributable to disinhibitory neuronal processes known to occur during sleep.
In studies with human volunteers, application of phase 1 pain stimuli leads to electroencephalographic (EEG) cortical arousal responses or brief awakenings during sleep [28–30]. It is difficult to compare results across studies because the type, duration, and intensity of nociceptive stimuli and protocols used in each study were quite different. Cutaneous heat of moderate [30] or high intensity [28] produced more frequent cortical arousals from non-REM (NREM) stage 2 compared to SWS and REM sleep, yet subjects reported the following morning minimal awareness of having been aroused or awakened during sleep. Nociceptive and non-nociceptive stimuli both produced a similar number of awakening responses from NREM stage 2 sleep and to reduced amounts of SWS and REM sleep obtained on experimental nights [31]. Findings from a laboratory study of sleep inertia (a transitional state of lower arousal) showed a large reduction in the perception of pain immediately after subjects were awakened from REM sleep, compared both to SWS and wake [32]. In a study of laser heat stimuli applied during sleep, investigators observed arousals to 31 % of the stimuli, and 53 % of these were associated with visual motor reactions on the polysomnogram. No reductions in the latency to the first component (N2) of the cortical EEG-evoked potential were observed, but the latency to the second component (P2) was shorter, and the evoked potential amplitude was reduced during both NREM stage 2 and REM sleep [33]. Evoked potentials measured over the frontal cortex were attenuated in REM sleep, although overall morphology of the response was similar to wakefulness. Non-nociceptive stimuli give rise to similar EEG-evoked potentials over the cortex such that specificity of nociception is inferred from the nature of the stimuli applied, not from the EEG response. Further studies are warranted to determine whether patients with chronic pain are more susceptible to nociceptive stimuli during sleep. However, responses to nociceptive and non-nociceptive stimuli in patients with chronic pain are quite different from that of healthy volunteers as brain activity could be distorted by changes already present in the CNS associated with the particular chronic pain condition [1]. Given these observations, comparisons between patients with different types of chronic pain may be more informative compared to healthy controls.
Phase 2 and 3 Pain Studies
Experimentally induced preclinical studies of phase 2 and 3 pain (systemic arthritis and sciatic nerve damage) show physiological changes in sleep architecture indicative of sleep disturbance and provide evidence that pain leads to disturbed sleep, but findings are not consistent for all types of pain models tested. Sleep in arthritic animals is highly fragmented [34, 35] with increased wakefulness during the inactive and increased sleep during the active periods of the diurnal cycle [36]. Sleep disturbance was most prominent during the acute inflammatory phase of arthritis [35–37] or during the acute postoperative period following nerve injury [38, 39]. A recent study in mice found a statistically significant small amount of increased wakefulness and reduced NREM sleep at 7 days and again at 28 days post-sciatic nerve injury [40]. Disease severity was associated with greater sleep disturbance and less wakefulness with increased delta activity during sleep in the active period in arthritic animals [36]. Although neuropathic pain models induce persistent peripheral nerve denervation along with long-lasting changes in gene expression in the CNS and behavioral signs of hyperalgesia and allodynia, no changes in EEG spectral power were observed in animals for over four months after injury [39]. Preclinical neuropathic pain models are produced by a variety of types of nerve injury that could lead to distinct differences in disease severity and differential impact on sleep and changes in EEG frequency patterns during sleep .
Findings from these studies of phase 2 and phase 3 pain provide evidence of disturbed sleep, but isolating pain, as the “cause” of disturbed sleep, is difficult to ascertain. Systemic arthritis evokes systemic inflammation, increases body temperature, and elicits a variety of “sickness behaviors.” Signs of disturbed sleep in peripheral nerve injury are most prominent in the acute postoperative period when systemic neuroendocrine responses to tissue injury, presumably, also are present. The most parsimonious explanation of these findings is an inability to sustain uninterrupted sleep episodes. Such changes could be related to persistent altered functioning of pain pathways, attributable to peripheral and central sensitization, that are more sensitive to slight bodily movements, or to environmental stimuli. Future studies of recently developed animals’ models of stress-induced generalized pain [41], and of combined inflammation and neuropathic injury [42], have potential to advance understanding of mechanisms involved in chronic pain effects on sleep.
Clinical Studies in Chronic Pain
Most studies of pain and sleep in clinical populations have been cross-sectional observational studies comparing self-reported pain and sleep disturbance in patients with different chronic pain conditions or controls without pain. Chronic pain has well-recognized disturbing effects on self-reports of sleep quality and disturbance, but subjects often are asked about how much pain interferes with sleep, or are given a list of factors or symptoms and asked to indicate which ones they attribute to disturbing their sleep [43]. Thus, studies may be biased toward finding false-positive reports of pain-related sleep disturbance. The majority of clinical studies that have used both subjective and objective measures of sleep have been conducted on patients with musculoskeletal conditions, and most of these involved patients with fibromyalgia. Chronic pain has not been consistently associated with disturbed sleep as measured by polysomnography (PSG) or actigraphy [44–47]. In these studies, often the self-report of poor sleep quality is out of proportion to modest changes in PSG indicators of sleep [9], especially when patients are compared to sedentary control subjects of similar age [45].
Sleep studies of patients with other types of chronic pain, in particular neuropathic pain, back pain, and chronic regional pain syndrome, are few in number. A recent review of the literature in patients with chronic low back pain found self-reported generalized sleep disturbance, reduced sleep duration, quality, and satisfaction, with increased sleep latency, and problems functioning in the daytime [48]. Of note, this evidence-based review included only two studies (meeting investigator inclusion criteria) that used PSG or actigraphy sleep measures, and only in < 10 patients in each study [49, 50]. A recent small clinical study of 16 patients with chronic low back pain yielded significant differences in self-reports of sleep disturbance compared to 16 control subjects, but no differences in sleep measures obtained from actigraphy [51]. It has been estimated that nearly 80 % of adults will, at some time, eventually experience back pain and metabolic biomarkers of brain function that correlate with clinical measures of chronic back pain [1]. We need PSG and nociceptive response studies during sleep in these clinical populations.
Investigators who preformed a structured evidence-based review of the literature (41 studies of good quality) on a variety of chronic pain conditions, that included some type of sleep measure, concluded that there is strong and consistent evidence to support an etiological role of pain with sleep disturbance due to a medical condition [7]. Of these, 77 % of 21 studies showed, through statistical modeling, that pain predicted the occurrence of a sleep problem, but only three of these studies were based on prospective analysis. Studies of daily temporal associations between pain and sleep with multilevel statistical modeling techniques have advanced our knowledge about pain–sleep interactions [9]. One of the first reports of a bidirectional relation between pain and sleep was derived from a prospective study in women with fibromyalgia [52]. Based on daily diary recordings over 30 days, a night of poor sleep was followed by more pain the next day; more pain during the day was followed by night of poorer sleep. Data on reports of nighttime sleep and pain for 8 days, from a large nationally representative sample of middle-aged adults in the USA, found that hours of sleep predicted subsequent frequency of pain and pain predicted subsequent hours of sleep, but the effect of sleep on pain was stronger than the effect of pain on sleep [53].
Recent studies of temporal associations between pain and sleep provide interesting and novel findings about the complexity of pain–sleep interactions. In a laboratory study of 75 children with juvenile arthritis, age, medications, anxiety, and evening pain explained 18 % of variance in subsequent EEG sleep arousals, but neither anxiety nor pain had a significant effect on sleep microstructure [54]. In a study of 97 adolescents with chronic pain or intermittent pain (healthy subjects), actigraphy-derived estimates of sleep duration and amount of wake after sleep onset, but not sleep efficiency or self-reported sleep quality, predicted next-day pain; daytime pain intensity did not predict subsequent nighttime sleep disturbance [12]. In a study of a group of 107 heterogeneous adult chronic pain patients (74 % women), both with moderate pain and insomnia severity scores, presleep mood and cognitive arousal, but not pain, predicted subsequent self-reported sleep quality; cognitive and somatic arousal predicted actigraphy-derived sleep efficiency [55]. Self-reported sleep quality and efficiency and actigraphy-derived sleep efficiency predicted next pain upon awakening, but predictors of pain in the first half or second half of the day varied. In post-hoc analysis, depression emerged as a significant predictor of self-reported sleep quality, along with presleep arousal. Thus, although relieving pain has potential to improve sleep, at the present time, it is not clear that pain is the most salient symptom to target in planning treatments to improve sleep in patients with chronic pain. Presleep arousal is an important factor influencing sleep quality and duration in insomnia [56], and therapies addressing arousal and mood [20] could be an important target for improving sleep in chronic pain patients.
Milestones: pain to sleep interactions
-
Advances in pain research have established that chronic pain is characterized by altered functioning in pain transduction, transmission, and modulation pathways in the brain leading to persistent heightened sensitivity to pain and the perception of pain after tissues have healed.
-
In animals, reflex withdrawal responses to pain stimuli are faster during NREM sleep and somewhat attenuated during REM sleep.
-
In humans, pain stimuli, applied during sleep, leads to transient arousals and sometimes brief awakenings but in healthy subjects awakenings are rarely remembered the next morning.
-
Substantial evidence exists to support pain in the etiology of self-reported, but not objective, measures of sleep disturbance in chronic pain.
-
Presleep arousal and mood, along with pain, have emerged as important factors associated with subsequent sleep disturbance.
Does Sleep Modulate Pain?
Sleep Effects on Pain
During sleep, an individual is unaware of environmental surroundings with reduced responsiveness to sensory stimuli. Arousal thresholds and response duration vary as a function of stimulus type and strength, sleep stage, time of night, age, and other factors. The literature on sleep modulation of sensory stimuli was reviewed previously and suggested that responses to nociceptive stimuli are preserved during NREM sleep, but gated to some extent during REM sleep [57]. In that review, reference was made to a series of studies of brainstem neurons in the region of the ventromedial reticular formation that previously had been implicated as one of the important sources for the mediation of descending nociceptive (pain) modulation or facilitation and hypothesized to inhibit nociception during sleep [58]. Research on brainstem neurons, OFF cells (anti-nociceptive) and ON cells (pro-nociceptive) have shown distinct patterns of spontaneous activity during waking, NREM, and REM sleep in rats [59] and more recently in mice [60]. OFF cells are continuously active during NREM sleep, sporadically active in wakefulness, and silent during REM sleep. ON cells are continuously active during waking, virtually silent during NREM sleep, and most active during REM sleep. Based on these response properties, one would expect that behavioral responses to noxious stimuli would be reduced during NREM sleep compared to wakefulness. However, paw withdrawal latencies to a radiant heat stimulus were faster during NREM sleep compared to wakefulness, and behavioral responses (e.g., licking the paw, moving about the cage) were suppressed during NREM sleep and exaggerated during waking [27]. In a recent study in mice [60], paw withdrawals to nociceptive heat were more reliably observed during sleep compared to wakefulness and associated with greater phasic activity of OFF cells prior to motor responses. Thus, rather than suppressing nociception , OFF cells appear to facilitate reflex motor protective withdrawal responses. However, how these neurons and others implicated in suppressing or facilitating pain responses would respond in the context of chronic pain has not been reported.
Sleep Loss Effects on Pain
Selective REM SD was one of the first types of sleep loss effects on pain studied. These experiments in rodents consistently have shown faster withdrawal latencies to noxious stimuli interpreted as reduced “pain” thresholds during [61], immediately after several days of deprivation [62–64], and after several days of recovery sleep [65]. Some evidence exists for reduced efficacy of opioid-mediated descending pain modulation in REM SD [66].
Increased pain perception or sensitivity has been observed in most experimental sleep loss studies in human volunteers, but such changes have not been consistently observed across studies involving the same type of nociceptive stimulus or similar SD protocols. One of the first total sleep deprivation (TSD) studies in human volunteers showed a progressive decrease in the threshold to pressure (von Frey hair), but not non-nociceptive stimuli [17]. One recent study has shown that the threshold to radiant heat pain was reduced after each of two nights of TSD compared to control subjects permitted usual sleep [67]; while the perception of reported pain on a visual analog scale was increased, the pain threshold was not altered after TSD in another study [68]. Selective SWS deprivation for three nights has been shown to increase muscle tenderness and reduce the threshold to pressure stimuli compared to baseline in young, primarily male, [69] and middle aged, female, subjects [70], but this change was not observed in another study [71]. Shorter latencies to radiant heat stimulus of 32 % have been observed after a single night of total sleep loss, after 4-h sleep loss, and after selective REM SD compared to non-REM deprivation [18]. Onen and colleagues [72] studied pain tolerance after one night of TSD followed by two consecutive nights of selective interruption of SW or REM sleep in counterbalanced order and a night of recovery sleep. Pressure, but not thermal, pain tolerance thresholds were reduced significantly after one night of TSD and remained lower after both SWS and REM sleep interruption nights, although the scores were not statistically different compared to baseline. After recovery sleep, there was a large increase in pressure pain tolerance scores, which was correlated with the amount of SWS during recovery. In one of the only reports of TSD in patients with chronic somatoform pain (e.g., without physical etiology) investigators reported increased pain perception, but without any change in pain thresholds to heat or pressure stimuli [73].
Compared to TSD, or selective sleep stage deprivation, inadequate or insufficient sleep is more common; one in three adults is estimated to sleep < 7 h per night [74]; thus, experimental studies of short sleep duration may provide data more applicable to sleep experienced in chronic pain conditions. In one of the few experimental studies of only women volunteers, neither three nights of interrupted sleep nor three nights of restricted, yet consolidated, sleep, both followed by a night of total sleep loss, led to any reliable group differences in pressure pain thresholds despite a 50 % reduction in total sleep time and increased sleepiness in both groups [75]. This study also assessed spontaneous pain symptoms and pain inhibitory processes using a test of diffuse noxious inhibitory controls (DNIC). In DNIC, the perception of a second nociceptive stimulus (e.g., pressure) is inhibited by the previous application of a nociceptive stimulus (cold) at a distant site. Only the group subjected to interrupted sleep showed an increase in spontaneous reports of pain symptoms and reduced pain inhibition. Another study involving assessment of endogenous pain-inhibitory processes after one night of experimental 4-h sleep restriction showed a 30 % increase in pain ratings, while reductions were observed in the amplitudes of laser-evoked EEG potentials; subjects were less able to inhibit pain when their attention was not focused on pain stimulus [76]. In a similar study of pain distraction, healthy individuals who habitually slept < 6.5 h, in the month preceding testing, had reduced pain inhibition, while playing video games, but they showed increased skin flare and augmented hyperalgesic responses to a heat-capsaicin stimulus compared to those who slept > 6.5 h [77]. In one of the only sleep restriction studies, found in the literature of patients with chronic pain, compared to control subjects, one night of 4-h sleep restriction augmented pain perception along with an increase in the number of painful arthritic joints, but fatigue, depression, and anxiety were also increased the next day [65]. With mild sleep loss, pain perception is augmented, both in healthy subjects and in patients with chronic pain, but increased pain perception is not always accompanied by evidence of altered pain thresholds. Such an increase in pain perception might be related to reduced functioning of pain-inhibitory processing.
Sleep Disorders and Pain
Sleep disorders often are associated with disturbed and fragmented sleep, and, in the case of insomnia, with short sleep duration, but few studies have measured pain perception or responses to nociceptive stimuli. Following the report of chronic pain by Ohayon [4] in a large percentage of people with insomnia, there is increased interest studying pain in primary and comorbid insomnia. Haack and colleagues [78] recently have shown that patients with primary insomnia reported twice as many days of spontaneous pain, showed reduced thresholds to heat and pressure pain, and both reduced pain facilitation and inhibition compared to control subjects. The results from this study were interpreted as evidence of subclinical pain and chronic activation of pain inhibitory mechanisms that produced a ceiling effect under challenging conditions. Additional research is necessary to confirm or refute this hypothesis.
Possible Mechanisms of Sleep Effects on Pain
Few studies have examined mechanisms that might underlie changes in pain perception with sleep loss [20]. Activation of inflammatory processes with increased circulating proinflammatory cytokines is one plausible mechanism that has been studied after sleep loss [79]. Increased C-reactive protein, an inflammatory biomarker of cardiovascular disease risk, was observed both after total sleep loss of 88 h or after 10 consecutive days of sleep restricted to 4 h nightly [80]. Increased plasma levels of interleukin-6, but not that of tumor necrosis factor alpha, have been observed following 10 days of 4-h sleep restriction [81], and increased urinary metabolites of prostaglandin E2 (PGE2) have been observed after 3 days of TSD [82]. In both studies, subjects reported spontaneous increased pain symptoms after several days of sleep loss. PGE2 is an important mediator of inflammation in peripheral tissues, capable of increasing peripheral nerve sensitivity [25] and neuron excitability in the spinal cord [83]. Proinflammatory cytokines released from circulating lymphocytes lead to release of cytokines by glia, in the spinal cord, and an increase in chemical mediators (e.g., excitatory amino acids, prostaglandins, nerve growth factors, and nitric oxide) that facilitate nociception and pain processing in the CNS [84]. Glia, rather than neurons, may be the biological basis of sickness behavior and therapies directed toward the upregulation of anti-inflammatory cytokines have been shown to reduce pain in animal studies [84].
Based on the results of the studies reviewed, it is not clear whether changes in pain perception and nociceptive thresholds with experimental sleep loss are attributable to total sleep loss, selective loss of a particular stage, restricting hours of sleep, or to sleepiness that inevitably accompanies sleep loss [85]. Sleepiness is one of the most reliable effects of experimental sleep loss. In fact, compared to well rested subjects, sleepy (as determined by multiple sleep latency tests) healthy subjects, after 8 h of sleep, showed increased pain sensitivity [86] and in a subsequent study, when subjects had extended time in bed, increased total sleep time correlated with reduced sleepiness and pain sensitivity [87]. As noted above, protective withdrawal reflexes to nociceptive stimuli are faster during NREM sleep and after experimental sleep loss when animals are “sleepiest.” Cytokines participate in the regulation of physiological sleep and are released after tissue injury, infection, and sleep loss [88]. Cytokines have a clear diurnal rhythm and reach the highest circulating levels during sleep [79]. It is possible that activation of cytokines during physiological sleep could participate in disinhibitory processes in the brainstem, which facilitate reflex withdrawal responses, yet protect sleep by not engaging sustained arousal responses? In addition to pain and sleepiness, cytokines have been associated with depressed mood, fatigue, impaired cognition, and memory—all symptoms that manifest with sleep loss. Thus, although activation of inflammatory processes is a plausible mechanism for increased pain sensitivity with sleep loss, further research is required to ascertain the role of cytokines and other inflammatory biomarkers to explain heightened pain following a night of disturbed sleep in patients with chronic pain, and in relation to levels of sleepiness.
Milestones: sleep to pain interactions.
-
Latencies to EEG cortical responses to pain stimuli remain intact during sleep, although the amplitude of evoked potentials is attenuated, and reduced during REM sleep.
-
In animals, REM SD is associated with reduced pain thresholds, possibly associated with reduced pain inhibitory processes.
-
In humans, increased perception of pain is associated with loss of total sleep, selective stages of sleep, or reduced sleep amounts.
-
Increased pain perception varies by type of pain stimulus (heat vs. pressure) and is not consistently accompanied by changes in pain threshold or physiological responses (e.g., changes in EEG-evoked potentials).
-
Sleep loss may reduce pain inhibitory processes.
-
Insomnia is associated with heightened pain sensitivity.
-
Increased sleep reduces daytime sleepiness and pain sensitivity.
-
Activation of inflammatory processes might be one mechanism underlying increased pain after sleep loss and with increased sleepiness.
Do Treatments for Sleep Modulate Pain?
In patients with chronic pain, pain is associated with disturbed sleep, and disturbed sleep augments pain. A recent evidence-based review concluded that pain is important in the etiology of sleep disturbances in patients with chronic pain and advocated that therapies to reduce pain ought to improve sleep [7]. Although treatments to reduce pain have potential to improve sleep, many medications commonly used to manage pain (opioids, antidepressants, anticonvulsants) have untoward and unpredictable effects on sleep [43, 89, 90]. Further, many of these medications produce sedation along with reducing pain, and, thus, attempts to assess the impact of such treatments on pain and sleep are complicated and potentially confounded [43]. In addition, many studies focused on managing pain, including studies of cognitive behavioral therapy specifically for pain, only focus on pain as an outcome and not on valid and reliable measures of sleep [9].
In the past few years, there is increased interest in studying the impact of treatments targeting sleep, and measuring pain outcomes [14]. Such efforts are supported by observations that reduced complaints of non-restorative sleep predicted reduced pain in a community sample of patients with chronic pain [91], and increased sleep time has been shown to lower pain sensitivity in experimental studies of sleep extension [87]. A recent review of selected clinical studies revealed that pharmacological management of insomnia with hypnotics (four studies of benzodiazepine receptor agonists; one study of benzodiazpene) improved sleep, but did not necessarily reduce pain in patients with fibromyalgia or arthritis [14]. In this review, three studies had been published on effects of cognitive-behavioral therapies for insomnia (CBT-I) in patients with nonmalignant chronic pain, fibromyalgia , and osteoarthritis with mixed results; sleep improved but pain was not reduced in all studies compared to control subjects. A more recent study evaluated the effect of CBT-I on sleep measures and on pain severity and interference with daytime functioning in a sample of middle-aged adults with nonmalignant chronic neck or back pain who developed insomnia after the onset of pain [92]. Self-reported sleep efficiency improved and sleep latency and wake after sleep onset were reduced, but total sleep time was unchanged after 8 weeks of therapy compared to attention controls. Pain severity and interference with daytime functioning were both reduced after 6 weeks compared to baseline, but pain severity was not statistically significantly different compared to controls. No follow-up data were reported. A major component of CBT-I is restricting time in bed to the reported time the patient actually reports sleeping. The amount of time in bed is advanced as total sleep time and sleep efficiency improve. CBT-I has shown improvements in self-reported and actigraphy measures of sleep quality and efficiency in fibromyalgia [93] but no changes in pain were reported. In patients with chronic pain, restricting sleep augments pain perception as shown by experimental studies noted above. CBT-I has long-lasting durable effects on sleep in primary and comorbid insomnia, and it is plausible, that only with sufficient practice over time would pain intensity subside as sleep time and quality increased. Notably, in the secondary analysis of the primary data from older adults with osteoarthritis at 1-year follow-up, CBT-I was associated with sustained improved sleep and reduced pain [94]. Thus, it has been hypothesized that sleep could be analgesic [94]. However, rather than being directly “analgesic,” sleep might assist in the maintenance or resetting of pain inhibitory processes, which apparently can be reduced in association with experimental sleep restriction or associated with habitual short sleeping.
At this time, perhaps the major milestone in research, about whether improving sleep can reduce pain, is the recognition that interventions targeting only pain or only sleep and subsequently only measuring pain or sleep outcomes, respectively, are inadequate to address both comorbidities. To that end, the results of a pilot study have shown feasibility for combining CBT for pain with CBT-I in patients with chronic pain and insomnia. Preliminary results did not support the superiority of the combined approach over CBT-I for improving sleep, fatigue and mood, or for CBT for improving pain outcomes [95]. Based only on findings of a single small feasibility study, it is premature to evaluate whether a combination of CBT-pain and CBT-I will improve outcomes, but such studies do hold promise for future research. However, given observations above in patients with chronic pain, combination therapies addressing presleep arousal and mood, are likewise important to consider in future studies. Although there are few milestones to acknowledge about therapies for sleep having a positive impact on pain perception, there is increasing interest among investigators from many disciplines in addressing this question.
Summary and Recommendations
Evidence from self-reported data support a cyclical model of pain-poor sleep pain in chronic pain, but data from objective measures of sleep are less convincing. More research is required to elucidate the nature of sleep disturbance and pain using both self-report and objective measures of sleep and baseline and evoked measures of pain in patients with different types of chronic pain. Far less is known about the nature and extent of sleep disturbance, for example, in chronic back pain, chronic neuropathic pain, complex regional pain syndrome, and even in sleep disturbance pain in cancer survivors. There is increasing evidence that patients with some types of chronic pain show evidence of brain degeneration and atrophy [1], which would make the design of interventions to improve sleep and pain more complex and challenging. Studies are needed that test the efficacy of interventions focused on both reducing pain and improving sleep with a goal of improving functional health outcomes in patients with these comorbidities.
References
Apkarian AV, Baliki MN, Geha PV. Towards a theory of chronic pain. Prog Neurobiol. 2009;87:81–97.
Woolf CJ. Central sensitization: implications for the diagnosis and treatment of pain. Pain. 2011;152:S2–15.
National Sleep Foundation. Adult public’s experiences with nighttime pain. Princeton: Gallup Organization; 1996.
Ohayon MA. Relationship between chronic painful physical condition and insomnia. J Psychiatric Res. 2005;39:151–9.
Langley PC, Van Litsenburg C, Cappelleri JC, Carroll D. The burden associated with neuropathic pain in Western Europe. J Med Econ. 2013;16:85–95.
Becker N, Thomsen AB, Olsen AK, Sjogren P, Bech P, Eriksen J. Pain epidemiology and health related quality of life in chronic non-malignant pain patients referred to a Danish multidisciplinary pain center. Pain. 1997;73:393–400.
Fishbain DA, Cole B, Lewis JE, Gao J. What is the evidence for chronic pain being etiologically associated with the DSM-IV category of sleep disorder due to general medical condition? A structured evidence-based review. Pain Med. 2010;11:158–79,
Morin CM, Gibson D, Wade J. Self-reported sleep and mood disturbance in chronic pain patients. Clin J Pain. 1988;14:311–4.
Okifuji A, Hare BD. Do sleep disorders contribute to pain sensitivity? Curr Rheumatol Rep. 2011;13:528–34.
Pilowsky I, Crettenden I, Townley M. Sleep disturbance in pain clinic patients. Pain. 1985;23:27–33.
Chen Q, Hayman LL, Shmerling RH, Bean JF, Leveille SG. Characteristics of chronic pain associated with sleep difficulty in older adults: the maintenance of balance, independent living, intellect, and zest in the elderly (MOBLIZE) Boston study. J Am Geriatr Soc. 2011 59;1385–92.
Lewandowski AS, Palermo TM, de la Motte S, Fu R. Temporal daily associations between pain and sleep in adolescents with chronic pain versus healthy adolescents. Pain. 2010;151:220–5.
Palermo TM, Law E, Churchill SS, Walker A. Longitudinal course and impact of insomnia symptoms in adolescents with and without chronic pain. J Pain. 2012;13:1099–106
Roehrs T. Does effective management of sleep disorders improve pain symptoms? Drugs. 2009;69(Suppl 2):5–11.
Wittig RM, Zorick FJ, Blumer D, Heilbronn M, Roth T. Disturbed sleep in patients complaining of chronic pain. J Nerv Ment Dis. 1982;170:429–31.
Moldofsky H, Scarisbrick P, England R, Smythe HA. Musculoskeletal symptoms and non-REM sleep disturbance in patients with fibrositis syndrome and healthy subjects. Psychosom Med. 1975;37:341–51.
Cooperman NR, Mullin FJ, Kleitman N. Studies of the physiology of sleep XI. Further observations on the effects of prolonged sleeplessness. Am J Physiol. 1934;107:589–93.
Roehrs T, Hyde M, Blaisdell B, Greenwald M, Roth T. Sleep loss and REM sleep loss are hyperalgesic. Sleep. 2006;29:145–51.
Lavigne GJ, Nashed A, Manzini C, Carra MC. Does sleep differ among patients with common musculoskeletal pain disorders? Curr Rheumatol Rep. 2011a;13:535–42.
Finan PH, Smith MT. The comorbidity of insomnia, chronic pain, and depression: dopamine as a putative mechanism. Sleep Med Rev. 2012;doi:10.1016/j.smrv.2012.03.003.
Mong JA, Baker FC, Mahoney MM, Paul KN, Schwartz MD, Semba K, et al. Sleep, rhythms, and the endocrine brain: infl uence of sex and gonadal hormones. J Neurosci. 2011;31:16107–16.
Manson JE. Pain: sex differences and implications for treatment. Meta Clin Exper. 2010;59:S16–20.
Lavigne GJ, Okura K, Abe S, Colombo R, Huynh N, Montplaisir JY, et al. Gender specificity of the slow wave sleep lost in chronic widespread musculoskeletal pain. Sleep Med. 2011b;12:179–85.
Basbaum AI, Jessell TM. The perception of pain. In: Kandel ER, Schwartz JA, Jessell TM, editors. Principles of neural science. 4th edn. New York: McGraw-Hill; 2000. p. 474–91.
Reichling DB, Levine JD. Critical role of nociceptor plasticity in chronic pain. TINS. 2009;32:611–8.
Jeong Y, Holden JE. Commonly used preclinical models of pain. West. J Nurs Res. 2008;30: 350–64.
Mason P, Escobebo I, Gurgin C, Bergan J, Lee JH, Last EJ, et al. Nociceptive responsiveness during slow-wave sleep and waking in the rat. Sleep. 2001;24:32–8.
Bentley AJ, Newton S, Zio CD. Sensitivity of sleep stages to painful thermal stimuli. J Sleep Res. 2003;12:143–7.
Drewes AM, Nielsen KD, Arendt-Nielsen L, Birket-Smith L, Hansen LM. The effect of cutaneous and deep pain on the electroencephalogram during sleep—an experimental study. Sleep. 1997;20:632–40.
Lavigne G, Zucconi M, Castronovo C, Manzini C, Marchettini P, Smirne S. Sleep arousal response to experimental thermal stimulation during sleep in human subjects free of pain and sleep problems. Pain. 2000;84:283–90.
Lavigne GJ, Brousseau M, Kato T, Mayer P, Manzini C, Guitard F, Montplaisir J. Experimental pain perception remains equally active over all sleep stages. Pain. 2004;110: 646–55.
Daya VG, Bentley AJ. Perception of experimental pain is reduced after provoked waking from rapid eye movement sleep. J Sleep Res. 2010;19:317–22.
Bastuji H, Perchet C, Legrain V, Montes C, Garcia-Larrea L. Laser evoked responses to painful stimulation persist during sleep and predict subsequent arousals. Pain. 2008;137:589–99.
Andersen ML, Tufik S. Altered sleep and behavioral patterns of arthritic rats. Sleep Res Online. 2000;34:161–7.
Landis CA, Robinson CR, Levine JD. Sleep fragmentation in the arthritic rat. Pain. 1988;34:93–9.
Landis CA, Levine JD, Robinson CR. Decreased slow-wave and paradoxical sleep in a rat model of chronic pain. Sleep. 1989;12:167–77.
Colpaert FC. Evidence that adjuvant arthritis in the rat is associated with chronic pain. Pain. 1987;28:201–22.
Andersen ML, Tufik S. Sleep patterns over 21-day period in rats with chronic constriction of sciatic nerve. Brain Res. 2003;984:84–92.
Kontinen VK, Ahnaou A, Drinkenburg WH, Meert TF. Sleep and EEG patterns in the chronic constriction injury model of neuropathic pain. Physiol Behav. 2003;78:241–6.
Narita M, Nikura K, Nanjo-Niikura K, Narita M, Furuya M, Yamashita A, et al. Sleep disturbances in a neuropathic pain-like condition in the mouse are associated with altered GABAergic transmission in the cingulate cortex. Pain. 2011;153:1358–72
Green PG, Alvarez P, Gear RW, Mendoza D, Levine JD. Further validation of a model of fibromyalgia syndrome in the rat. J Pain. 2011;12:811–8.
Allchornea AJ, Goodinga HL, Michellb R, Fleetwood-Walkera SM. A novel model of combined neuropathic and inflammatory pain displaying long-lasting allodynia and spontaneous pain-like behavior. Neurosci Res. 2012;74:230–8.
Smith MT, Haythornthwaite JA. How do sleep disturbance and chronic pain inter-relate? Insights from the longitudinal and cognitive-behavioral clinical trials literature. Sleep Med Rev. 2004;8:119–32.
Carette S, Oakson G, Guimont C, Steriade M. Sleep electroencephalography and the clinical response to amitriptyline in patients with fibromyalgia. Arthritis Rheum. 1995;38:1211–7.
Landis CA, Lentz MJ, Tsuji J, Buchwald D, Shaver JLF. Pain, psychological variables, sleep quality and natural killer cell activity in midlife women with and without fibromyalgia. Brain Behav Immun. 2004;18:304–13.
Leventhal L, Freundlich B, Lewis J, Gillen K, Henry J, Dinges D. Controlled study of sleep parameters in patients with fibromyalgia. J Clin Rheumatol. 1995;1:110–3.
Menefee LA, Cohen MJM, Anderson WR, Doghramji K, Frank ED, Lee H. Pain Med. 2000;1:156–72.
Kelly GA, Blake C, Power CK, Keeffe DO, Fullen BM. The association between chronic low back pain and sleep: a systematic review. Clin J Pain. 2011;27:169–81.
Harmon K, Pivik RT, D’Eon JL, Wilson KG, Swenson JR, Matsunaga L. Sleep in depressed and nondepressed participants with low back pain: electroencephalographic and behavior findings. Sleep. 2002;25:775–83.
Lavie P, Epstein R, Tzischinsky O, Gilad D, Nahir M, Lorber M, et al. Actigraphic measurements of sleep in rheumatoid arthritis: comparison of patients with low back pain and healthy controls. J Rheumatol. 1992;19:362–5.
Van de Water AT, Eadie J, Hurley DA. Investigation of sleep disturbance in chronic low back pain: an age-and gender-matched case-control study over a 7-night period. Man Ther. 2011;16:550–6.
Affleck G, Urrows S, Tennen H, Higgins P, Abeles M. Sequential daily relations of sleep, pain intensity, and attention to pain among women with fibromyalgia. Pain. 1996;68:363–8.
Edwards RR, Almeida DM, Klick B, Haythornthwaite JA, Smith MT. Duration of sleep contributes to next-day pain report in the general population. Pain. 2008;37:202–7.
Ward TM, Brandt PA, Archbold KH, Lentz MJ, Ringold S, Wallace CA, et al. Polysomnography and self-reported sleep, pain, fatigue, and anxiety in children with active and inactive juvenile rheumatoid arthritis. J Ped Psychol. 2008;33:232–41.
Tang NKY, Goodchild CE, Sanborn AN, Howard J, Salkovskis PM. Deciphering the temporal link between pain and sleep in a heterogeneous chronic pain patient sample: a multilevel daily process study. Sleep. 2012;35:675–87.
Harvey AG. A cognitive model of insomnia. Behav Res Ther. 2002;40:869–93.
Landis CA. Sleep, pain, fibromyalgia and chronic fatigue syndrome. In: Montagna P, Chokroverty S, editors. Handbook of clinical neurology, vol 38 Sleep disorders, Part 1. Edinburgh: Elsevier; 2011. p. 613–37.
Foo H, Mason P. Brainstem modulation of pain during sleep and waking. Sleep Med Rev. 2003;7:145–54.
Leung CG, Mason P. Physiological properties of medullary raphe neurons during sleep and waking. J Neurophysiol. 1999;81:584–95.
Hellman KM, Mason P. Opioids pro-nociceptive modulation mediated by raphe magnus. J Neurosci. 2012; 32:13668–78.
Onen S, Alloui A, Jourcan D, Eschalier A, Dubray C. Effects of rapid eye movement (REM) sleep deprivation on pain sensitivity in the rat. Brain Res. 2001b;900:261–7.
Hicks RA, Moore JD, Findley P, Hirshfield C, Humphrey V. REM sleep deprivation and pain thresholds in rats. Percep Motor Skills. 1978;47:848–50.
Hicks RA, Coleman DD, Ferrante F, Sahatjian M, Hawkins J. Pain thresholds in rats during recovery from REM sleep deprivation. Percep Motor Skills. 1979;48:687–90.
May ME, Harvey MT, Valdovinos MG, Kline IV, RH, Wiley RG, Kennedy CH. Nociceptor and age specific effects on REM sleep deprivation induced hyperalgesia. Behav Brain Res. 2005;159:89–94.
Irwin MR, Olmstead R, Carrillo C, Sadeghi N, FitzGerald JD, Ranganath VK, et al. Sleep loss exacerbates fatigue, depression, and pain in rheumatoid arthritis. Sleep. 2012;35:537–43.
Ukponmwan OE, Rupreht J, Dzoljic MR. REM sleep deprivation decreases the antinociceptive property of enkephalinase-inhibition, morphine, and cold-water swim. Gen Pharmac. 1984;15:255–8.
Kunderman B, Spernal J, Huber MT, Krieg JC, Lautenbacher S. Sleep deprivation affects thermal pain thresholds but not somatosensory thresholds in healthy volunteers. Psychosom Med. 2004;66:932–7.
Azevedo E, Manzano GM, Silva A, Martins R, Andersen ML, Tufik S. The effects of total and REM sleep deprivation on laser evoked potential threshold and pain perception. Pain. 2011;152:2052–8.
Moldofsky H, Scarisbrick P. Induction of neurasthenic musculoskeletal pain syndrome by selective sleep stage deprivation. Psychosom Med. 1976;38:35–43.
Lentz MJ, Landis CA, Rothermer J, Shaver JLF. Effects of selective slow wave sleep disruption on musculoskeletal pain and fatigue in middle-aged women. J Rheumatol. 1999;26:1586–92.
Older SA, Battafarano DF, Canning CA, Ward JA, Grady EP, Derman S, et al. The effects of delta wave sleep interruption on pain thresholds and fibromyalgia-like symptoms on healthy subjects; correlations with insulin-like growth factor I. J Rheumatol. 1999;25:1180–6.
Onen S, Alloui A, Gross A, Eschallier A, Dubray C. The effects of total sleep deprivation, selective sleep interruption and sleep recovery on pain tolerance thresholds in healthy subjects. J Sleep Res. 2001a;10:35–42.
Busch V, Hass J, Cronlein T, Pieh C, Geisler P, Hajak G, et al. Sleep deprivation in chronic somatoform pain—effects on mood and pain regulation. Psychiatry Res. 2012;195:134–43.
McKnight-Eily, LR, Liu Y, Perry GS, Presley-Cantrell LR, Strine TW, Lu H, et al. Perceived insuffi cient rest or sleep among adults—United States, 2008. Atlanta: Div of Adult and Community Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. 2008.
Smith MT, Edwards RR, McCann UD, Haythornthwaite JA. The effects of sleep deprivation on pain inhibition and spontaneous pain in women. Sleep. 2007;30:494–505.
Tiede W, Mageri W, Baumgartner U, Durrer B, Ehlert U, Treede R-D. Sleep restriction attenuates amplitudes and attentional modulation of pain-related evoked potentials, but augments pain ratings of healthy volunteers. Pain. 2010;148:36–42.
Campbell CM, Bounds SC, Simango MB, Witmer KR, Campbell JN, Edwards RR, et al. Self-reported sleep duration associated with distraction analgesia, hyperemia, and secondary hyperalgesia in the heat-capsaicin nociceptive model. Euro J Pain. 2011;15:561–7.
Haack M, Scott-Sutherland J, Santangelo G, Simpson NS, Sethna N, Mullington JM. Pain sensitivity and modulation in primary insomnia. Eur J Pain. 2012;16:522–33.
Simpson N, Dinges DF. Sleep and inflammation. Nut Rev. 2007;11:S244–52.
Meier-Ewert HK, Ridker PM, Rifai R, Regan MM, Price NJ, Dinges DF, et al. Effect of sleep loss on C-reactive protein, an inflammatory marker of cardiovascular risk. J Am Coll. Card. 2004;43:678–83.
Haack M, Sanchez E, Mullington JM. Elevated inflammatory markers in response to prolonged sleep restriction are associated with increased pain experience in healthy volunteers. Sleep. 2007;30:1145–52.
Haack M, Lee E, Cohen DA, Mullington JA. Activation of the prostaglandin system in response to sleep loss in healthy humans: potential of increased spontaneous pain. Pain. 2009;145:136–41.
Fornasari D. Pain mechanisms in patients with chronic pain. Clin Drug Investig. 2012;32(Suppl 1):45–52.
Watkins LR, Maier S. Immune regulation of central nervous system functions: from sickness responses to pathological pain. J Int Med. 2005;257:139–55.
Roehrs T, Roth T. Sleep and pain: interaction of two vital functions. . Sem Neurol. 2005;25:106–16. (In: Roos KL, Avidan AY, editors).
Chhangani BS, Roehrs TA, Harris EJ, Hyde M, Drake C, Hudgel DW, et al. Pain sensitivity in sleepy pain-free normals. Sleep. 2009;32:1011–7.
Roehrs T, Harris E, Randall S, Roth T. Sensitivity and recovery from mild chronic sleep loss. Sleep. 2012;35:1667–72.
Clinton JM, Davis CJ, Zielinski MR, Jewett KA, Krueger JM. Biochemical regulation of sleep and sleep biomarkers. J Clin Sleep Med. 2011;7:S38–42.
Mystakidou K, Clark AJ, Fischer J, Lam A, Pappert K, Richarz U. Treatment of chronic pain by long-acting opioids and effects on sleep. Pain Practice. 2011;3:282–9.
Turk DC, Cohen MJM. Sleep as a marker in the effective management of chornic osteoarthritis pain and opioid analgesics. Semin Arthritis Rheum. 2010;39:477–90.
Davies KA, Macfarlane GJ, Nicholl BI, Dickens C, Morriss R, Day D, et al. Restorative sleep predicts the resolution of chronic widespread pain: results from the EPIFUND study. Rheumatology. 2008;47:1809–13.
Jungquist CR, O’Brien C, Matteson-Rusby S, Smith MT, Pigeon W, Xia Y, et al. The efficacy of cognitive behavioral therapy for insomnia in patients with chronic pain. Sleep Med. 2010;11:302–9.
Edinger JD, Wohlegemuth WK, Krystal AD, Rice JR. Behavioral insomnia therapy for fibromyalgia patients: a randomized clinical trial. Arch Int Med. 2005;165:2527–35.
Vitiello MV, Rybarczyk B, Von Korff M, Stepanski EJ. Cognitive behavioral therapy for insomnia improves sleep and decreases pain in older adults with co-morbid insomnia and osteoarthritis. J Clin Sleep Med. 2009;5:355–62.
Pigeon WR, Moynihan J, Matteson-Rusby S, Jungquist CR, Xia Y, Tu X, et al. Comparative effectiveness of CBT interventions for co-morbid chronic pain and insomnia: a pilot study. Beh Res Ther. 2012;50:685–9.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer Science+Business Media, LLC
About this chapter
Cite this chapter
Landis, C. (2015). Sleep and Pain: Milestones and Advances from Research. In: Chokroverty, S., Billiard, M. (eds) Sleep Medicine. Springer, New York, NY. https://doi.org/10.1007/978-1-4939-2089-1_49
Download citation
DOI: https://doi.org/10.1007/978-1-4939-2089-1_49
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4939-2088-4
Online ISBN: 978-1-4939-2089-1
eBook Packages: MedicineMedicine (R0)