Abstract
Neither morphology alone nor (molecular) clonality assays are at times sufficient to distinguish cutaneous lymphoma from atypical lymphoid hyperplasia or inflammation. In those instances, T-cell or B-cell clonality determined by PCR amplification of rearranged T-cell antigen receptor or immunoglobulin genes, respectively, is a useful method to more fully clarify the benign versus malignant nature of cutaneous lymphoproliferations but only in an adequate specimen. Analysis should include biopsy of a lesion in a manner to yield sufficient tissue for morphological, immunohistochemical, and molecular DNA/RNA assays. Additional flow cytometry, immunohistochemistry, and clinicopathologic criteria-based diagnosis enable a complete assessment as discussed in part I of this chapter. A complete workup should be integrated with histology and immunohistochemistry in collaboration with dermatologists, dermatopathologists, and hematopathologists using recommendations from the International Society for Cutaneous Lymphomas and World Health Organization. Although the EuroClonality consortium documents its application in only 5–15 % of all lymphoid neoplasms, we found about one-third of our consultation cases benefit from PCR clonality assays for T- and B-cell populations. Caution is warranted in interpreting the significance of clonality because of the underlying concept that neoplasms as a group may be a continuum spanning reactive dermatitis to atypical lymphoid proliferation or dyscrasia to malignant lymphoma. It should be emphasized that one benign diagnosis in a particular patient does not necessarily evolve to atypical hyperplasia followed by lymphoma. Multiple events required for malignant transformation may not occur for a particular patient. In this regard, we reinforce these concepts in part II in which we present ten examples within the spectrum of benign to malignant clonal skin lesions.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
Introduction
Cells derived from neoplastic lymphoid infiltrates usually differ from reactive benign infiltrate by expression of monotypic antigen receptor proteins or clonal deoxyribonucleic acid (DNA) segments of rearranged antigen receptor genes. Ancillary tests such as cell membrane/cytoplasmic light chain restriction, Vbeta T-cell receptor, and killer immunoglobulin receptor (KIR) immunophenotyping by flow cytometry or immunohistochemistry are used to evaluate monotypic antigen protein receptors. In addition, both B- and T-cell genes located in the nucleus are encoding antigen receptors that rearrange as the cell undergoes immunologic and functional maturation. Because cutaneous lymphomas, like those arising in the lymph nodes, show a unique set of rearranged gene segments, assays for a unique nucleic acid sequence are equivalent to a molecular fingerprint identifying a clone. Hence, neoplasms usually have expanded population of cells possessing this unique DNA sequence. A monoclonal B- or T-cell population may be revealed as a discrete peak or band by polymerase chain reaction (PCR) amplification above a background of polyclonal cell DNA. However, if any lymphoid population is scant with few cells acting as nonspecific templates, owing to an ultrasensitive assay, false positives or pseudoclonal bands may be observed. Similarly, an insufficiently sampled neoplasm may also provide a false-negative result.
In general, the main ancillary tests include cytochemistry, immunophenotyping, and molecular tests. Immunophenotyping includes flow cytometry, immunohistochemistry (IHC), and image cytometry. Cytochemistry is useful for detection of infectious agents, deposits, or intracellular inclusions. Molecular tests consist mainly of in situ hybridization (ISH) and PCR-based tests. ISH tests include detection of restricted immunoglobulin light chains or detection of microorganisms. PCR-based tests consist mainly of detection of B- and T-cell clonality using IgG and T-cell receptor gene rearrangements.
Part I. Ancillary Tools to Characterize Cutaneous Infiltrates
Molecular Fingerprint by PCR of Antigen Receptor Genes
Molecular T and B receptor gene rearrangement assays by PCR have a well-defined role in the workup, diagnosis, and monitoring of cutaneous lymphoproliferative diseases. PCR using heteroduplex and GeneScan capillary electrophoresis has largely replaced Southern blot as a standard in clinical practice and in cutaneous hematopathology (Bruggemann et al. 2007; Gallardo et al. 2008; Langerak et al. 2012; Lukowsky et al. 2010; Morales et al. 2008; Sandberg et al. 2003, 2005). Molecular studies are of critical importance when the histomorphologic and/or clinical presentation of a skin lesion has features that preclude definitive distinction between a benign process and lymphoma. Although PCR has been mostly used to detect clonality in a cellular specimen, the standardized EuroClonality consensus study elaborates on several PCR amplicon signatures that may be seen in patients with skewed immunity and enhanced immune responses either from transplantation, therapy, inflammation, or infections (Langerak et al. 2012); see Table 4.1. However, judicious use of this test in appropriate cases, with an adequate cellular sample, clinical risk estimation, and a rational algorithm, increases its positive and negative predictive value (Zhang et al. 2010).
The indications for performing this clonality test are dictated by the findings in the biopsy: presumptive morphologic diagnosis with clinical correlation. It is not useful in the following three groups of cases: (1) evidence of “other” infiltrates such as carcinoma, melanoma, sarcoma, or myelomonocytic leukemia, Hodgkin lymphoma; (2) clonal light chain restriction by flow cytometry, image cytometry, IHC, or ISH; and (3) prior diagnostic molecular studies compatible with the working diagnosis; see Table 4.2. In Table 4.2 we present our experience on the applications and indications of molecular tests and their role in cutaneous hematopathology. In that table, molecular tests are not indicated if the histology and IHC results are diagnostic of carcinoma, sarcoma, leukemia, or Hodgkin lymphoma. We also defer these tests if there was a previous diagnostic test on antecedent biopsy. In addition, if clonality has been confirmed by light chain restriction by ISH or by IHC or if the morphology is frankly malignant and dominant markers are diffusely positive that is characteristically that only in neoplasms and not a feature seen in reactive forms, we also do not order the T and B clonality tests.
Of 160 cutaneous lymphohematopoietic cases we saw in consultation in Tampa, FL, from 2010 to 2013, 50 cases (31 %) had TCR/IgG gene rearrangement studies using GeneScan capillary electrophoresis (BIOMED-2) and 110 cases (69 %) did not have the tests. Frequency of the tests are as follows: both TCR and IgG, 31, 62 %; TCR only, 17, 34 %; IgG only, 2, 4 %. Of these, 11 (22 %) were repeat biopsies/PCR with nine out of 11 cases resulting in a change in diagnosis. Repeat tests were ordered if there was clinical-pathology discordance or doubt of adequate DNA. Four of five with oligoclonal results were from shave biopsies and repeated with excision/punch biopsy which was then adequate. Of the 11, seven atypical hyperplasias with equivocal results were positive leading to diagnosis of five cutaneous B-cell lymphoma (CBCL) and two primary cutaneous small and medium cell T-cell lymphoma (PCSMTCL); two biclonal cases (IgG + TCR+; IgGoligoTCR+) with IgG + TCR- and IgG-TCR + repeat results confirmed CBCL and lymphomatoid papulosis, respectively (Table 4.2).
Overall, we believe that T and B clonality by PCR is indicated/helpful in about a third of cases. Oligoclonal/equivocal results were noted in small usually shave biopsies. Repeat tests are all useful results that need careful correlation with clinical course, histopathology, and immunostaining. In general, no change of original result supports the monoclonal or polyclonal nature. A confirmation may avoid unnecessary expensive treatment or unnecessary staging tests.
It is generally understood that the results of these molecular tests are not the gold standard that equates to a clinical diagnosis considering that these tests do not detect all neoplasms, that there are false-positive and false-negative results, and that there is a spectrum of skin lesions that evolve from benign cutaneous lymphoid hyperplasia to non-clonal atypical lymphoid hyperplasia, to prelymphomatous “ clonal dermatitis,” to frank lymphoma as determined by a combined use of clinical behavior, morphological, immunohistochemical, and molecular criteria; see Table 4.3.
Basis of PCR Antigen Receptor Gene Rearrangement Assay
The gene rearrangement sequence as a normal biology of maturing lymphocytes is illustrated in Fig. 4.1. The PCR technique employs unique nucleic acid sequences by generating a set of primers designed to hybridize with and detect family-specific common sequences, so that about seven primers are used instead of the 45 individual primers for the IgH V family or several primers for the possible total of nine variable regions the TCR gamma family.
The gene rearrangement sequence as a normal biology of maturing lymphocytes. Mechanism of antigen receptors gene rearrangement to generate a unique sequence detectable by PCR. Germ line to rearrange DNA of T cell receptor beta gene (B cell IgH similar). The diagram illustrates sequence of antigen receptor gene rearrangement to generate codes for receptor diversity (adapted from immuneweb.xxmu.edu) from: (a) germ line DNA sequence with variable, diversity, joining, and constant region segments; (b, c) Tertiary structure altered to place single D segment in close proximity to a single J segment; (d) followed by double-stranded DNA break; (e) rejoining by RAG (recombination activating gene) proteins (yellow bolt); (f) excision of intervening DNA; and (g) Tdt adds or subtracts random nucleotides (open bolt) to generate a unique rearranged DNA ending with a specific length or base pair that could be assayed by PCR technique
Examples of assay results and recommended interpretation according to the EuroClonality consortium are shown in Figs. 4.2 and 4.3 (Langerak et al. 2012).
IgH cell peaks and PCR GeneScan interpretation according to the EuroClonality consortium. The above diagram represents typical monoclonal peak with small polyclonal peaks in the background. “Profiles with one or two clear peaks or bands are called ‘clonal’, with the option to indicate that the intensities are weak or that a polyclonal background is seen.” (Langerak 2012). In Sproul and Goodlad (2012), pseudoclonality is also defined as single band/peak or doublet with little if any polyclonal background and rarely reproducible on repeat testing
A T beta and gamma gene rearrangement and PCR GeneScan interpretation. (a) When one to two peaks or bands are identified that are clearly non-reproducible, this is referred to as “pseudoclonal”; implicit in this description is that clonal signals are seen, but that they differ in size between the duplicates as shown by arrows. The last panel shows a dominant polyclonal population. (b) T gamma peaks and recommended interpretations according to the EuroClonality consortium. “Even cases that show a relatively weak clonal peak/band in a polyclonal background can be truly clonal, as long as the pattern is reproducible and preferably seen in multiple targets. Profiles with multiple (defined as three or more) peaks or bands are indicated with the description “multiple products.” Such profiles as in case 1 run 1 and 2, are non-reproducible or “pseudoclonal,” or in case 2 run 1 and run 2 as reproducible but reflect multiple consistent clones probably due to a dominant immune response” and may be reactive in nature.” (Langerak et al. 2012)
The Concept of Pseudolymphomas (Cutaneous Lymphoid Hyperplasia), Cutaneous Lymphoid Dyscrasias, and Prelymphomatous Infiltrates
Because CTCL and CBCL often evolve over a period of time from an inflammatory background, the precise boundary between lymphoma and benign could be elusive. In early diseases, cutaneous lymphomas can be difficult to distinguish from benign inflammatory dermatosis or cutaneous lymphoid hyperplasia; hence, it is useful to have descriptors that define histological niches along this continuum. It should be emphasized that one benign diagnosis in a particular patient does not necessarily evolve to atypical hyperplasia followed by lymphoma. Multiple events required for malignant transformation may not occur for a particular patient.
Definitions
Pseudolymphoma is a nonspecific term for a variety of reactive T- or B-cell infiltrates that simulate cutaneous lymphoma secondary to drugs, immune dysregulation, infection, arthropod bite, or chemical reaction or are idiopathic in origin. Cutaneous lymphoid hyperplasia is a synonymous term, often applied to pseudolymphomas with discrete benign germinal centers. When there is an overlap of clinical and histologic features of hyperplasia or inflammatory dermatosis, with atypical findings, the term pseudolymphoma is often used. A number of classification schemes have been proposed based on etiology, architecture, or immunohistology.
Using immunohistology, B-cell, T-cell, and mixed pseudolymphomas are classified if B or T cells are predominant and mixed if in between. T-cell pseudolymphoma is either epidermotropic and band-like or dermal and nodular in appearance. See Chaps. 5 and 8 for discussion (Rijlaarsdam et al. 1992).
Cutaneous T-cell lymphoid dyscrasias were coined as a unifying term for a group of idiopathic chronic dermatoses with persistent T-cell clones and have uncommon evolution to CTCL; see Table 4.4 (Guitart and Magro 2007).
Prelymphomatous infiltrate includes those skin lesions with a low but defined frequency of progression to cutaneous B- or T-cell lymphoma; see Table 4.6.
Clonality by GeneScan: monoclonal pattern is defined as one or two peaks, with a peak height substantially higher than the baseline, with or without a low-level or more prominent smear (polyclonal amplification) pattern in the background; see Figs. 4.2 and 4.3.
An oligoclonal pattern is defined as three prominent peaks, with peak height substantially higher than baseline; see Fig. 4.3. The range of analytic sensitivity (assay cannot detect clonality below the given percent of clonal cells over all lymphocytes) of the T-cell receptor gamma and beta PCR assays is 5–10 and 10–15 %, respectively.
Although the presumption is that the infiltrate in pseudolymphoma is benign or reactive, clinicians are often advised that a small percentage of this group can progress to lymphoma, and therefore, long-term follow-up is recommended (Albrecht et al. 2007; Anandasabapathy et al. 2008; Arai et al. 1999, 2005; Bergman 2010). Clinical features are used as a guide to therapy or planning in equivocal cases with “pseudoclonality” (Gilliam and Wood 2000).
The explanation for the foregoing is the well-described pathobiology of cutaneous lymphomas in which cutaneous lymphomas arise from within a population with multiple subclones (Cozzio and French 2008; Ponti et al. 2008) and lymphoid hyperplasias progress with worsening of appearance with or without evidence of a clonal population (Wood 2001; Wood et al. 1989; Kulow et al. 2002). The percentage of clonality detection increases as the lymphoma progresses to a higher stage and as histopathological score increases, especially well documented for mycosis fungoides (MF) (Guitart et al. 2001).
Interpretation of a pseudoclonal result in the face of a normal skin biopsy or discordant skin biopsy findings is interpreted by whether the infiltrate is B or T cell rich or by clinical risk assessment. If there are a small number of discrete bands consistent with oligoclonality, it is often difficult to differentiate lymphoma from a false positive (clonally restricted benign dermatitis). Correlation with immunostains is useful and false positives are often associated with scant infiltrates or infiltrates rich in opposite lineage (T clonality in B cell rich or B clonality in T-cell-rich infiltrate) (Nihal et al. 2000, 2003).
For an excellent introductory review of the role of molecular pathology in cutaneous lymphoma, see Raess and Bagg (2012). Using the heteroduplex assay, in the evaluation of patients suspected of having early MF, Murphy et al. detected identical banded patterns in serial skin biopsies from the same patient. No dominant T-cell clones were found in the inflammatory dermatoses studied (Murphy et al. 2000). In T-cell assay on paraffin-embedded skin tissue using GeneScan capillary electrophoresis (BIOMED-2), performance of both TCR gamma and TCR beta PCR is superior to the use of only one probe, if a risk assessment algorithm is followed (Zhang et al. 2010). Because of these findings and for cost-effective reasons, some centers use this sequential algorithm. For example, if the pretest risk is low-moderate according to clinical criteria and TCR gamma is not detected, TCR beta analysis is not performed. But if TCR gamma rearrangement is found, TCR beta is additionally done, and if both are positive, full support for lymphoma is reported. If TCR gamma is positive but TCR beta is negative, a repeat test is recommended. If the risk is moderate-high and a positive TCR gamma is obtained, TCR beta is not performed and the result called positive for lymphoma. If in this case, TCR gamma is initially negative, then TCR beta is performed. If negative, there is no clonal support for lymphoma, but if positive, a diagnosis of lymphoma is supported (Stanford Medical Center esoteric department 2011; Zhang et al. 2010); see Fig. 4.4.
Workflow algorithm for sequential use of PCR for T gamma and T beta for gene rearrangement assay for clonality in assessment in mycosis fungoides (Zhang et al. 2010)
Comparison of Sensitivity and Specificity of PCR of Several Methods
Using the BIOMED-2 method, B-cell clonality technique in formalin-fixed paraffin-embedded tissue is as follows: the DNA from the framework region 3 (FR3) sequence of the IgH genes is amplified to ascertain the presence of a clonal IgH gene rearrangement resulting in 73 % sensitivity and 100 % specificity (Hughes et al. 2001). Similarly, Morales et al. reported IgH clonality can be detected in formalin-fixed samples of CBCL with 85 % sensitivity and specificity of 96 % (Morales et al. 2008). For T cells, BIOMED-2 TCR PCR works well with DNA from paraffin-embedded tissue, in which clonality was detected 90 % on average revealing a high-clonality detection rate in CTCL, and thus is recommended for routine skin biopsy preparations (Hughes et al. 2001; Lukowsky et al. 2010; Luo et al. 2001; Meyer et al. 1997; Morales et al. 2008); see Table 4.1.
Luo et al. compared the capillary electrophoresis (CE) method with the standard denaturing gradient gel electrophoresis (DGGE) method using formalin-fixed specimens. Eleven of 12 (92 %) cases with a definitive diagnosis of T-cell lymphoma were monoclonal by CE, with 100 % concordance with the DGGE method. Of nine specimens morphologically suspicious for T-cell lymphoma, five specimens were positive by CE analysis compared with four specimens by DGGE. In addition, 14 specimens for staging from patients with known T-cell lymphoma were studied using both the CE and DGGE methods, with a concordance of 86 % (Luo et al. 2001).
Causes of Pseudolymphomas
Atypical lymphocytic infiltrates that mimic cutaneous lymphoma (i.e., pseudolymphomas) are often observed in skin biopsy specimens from patients with altered immune function or excessive lymphoid reaction to an antigen. The former may reflect systemic immune dysregulatory states such as collagen vascular disease, and the latter may be secondary to exogenous antigen introduction such vaccination, infection, and arthropod bites; see Fig. 4.5. Among the iatrogenic causes are drug therapy with agents that dysregulate normal lymphocyte function; see Table 4.7 for list of drugs (Brady et al. 1999; Jackson and Nesbit 2012). These drugs encompass those with anti-prefix such as anticonvulsants, antidepressants such as phenothiazines, antibiotics, antihypertensives such as calcium channel blockers, anti-inflammatory, antihistamines, and antilipidemic drugs. Chemokines such as interleukins, colony-stimulating factors (CSF), and inhibitors to angiotensin-converting enzyme, tyrosinases and TNF (tumor necrosis factors), are usually given in a short list; see Chap. 15.
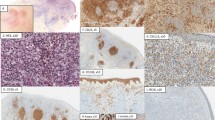
(a) Arthropod spider bite from a farmer in Pensacola, Florida, who noted a spider nicked his neck and then complained of persistent nodule for several months which was biopsied. (b) shows T-cell reaction in a perivascular nodular pattern in the upper and deep dermis with epitheliotropism in hair and eccrine areas, low power. B.CD3 and (c) mixed cell reaction, with similar pattern of CD20 B-cell stains
The appellation of lymphomatoid hypersensitivity reaction has been applied to cases of drug-associated pseudolymphoma in association with atopy, high IgE, and external contact sensitization such as metals contact reaction; see Fig. 4.6.
As mentioned, two types of T pseudolymphoma that are CTCL mimics include the band-like T and nodular pseudolymphomas. Those with a lichenoid pattern include lymphomatoid contact dermatitis (Fig. 4.7), lichen planus (Fig. 4.8), and lichen sclerosus (Fig. 4.9). Some examples of idiopathic band-like or nodular/diffuse T-cell pseudolymphoma without T- or B-cell gene rearrangement clonal results are shown in Figs. 4.10 and 4.11, for band-like and nodular/diffuse, respectively. Lichenoid benign lymphomatoid keratosis (Fig. 4.12) may show a nodular pattern and is a differential diagnosis of solitary primary cutaneous small and medium T-cell lymphoma. Many classic dermatitis with lymphoid-rich reaction in epidermis and hair follicles may histologically present as pseudolymphoma such as discoid lupus (Fig. 4.13) and lymphomatoid folliculitis (Fig. 4.14). Pathologically and clinically, distinction of such cases from cutaneous lymphoma is often difficult (Brady et al. 1999). Several unusual and specific entities that may resemble pseudolymphomas include angiolymphoid hyperplasia with eosinophilia (ALHE) or Kimura’s disease and Castleman’s disease.
Lichen planus, (a) low power, with lichenoid lymphocytic infiltrate with pigment incontinence and mild acanthosis and epitheliotropism, and (b) high power showing atypical small lymphocytes with irregular nuclei with haloes mimicking early MF, but cerebriform cells are difficult to find (Courtesy of dermatopathologist M. Patel, DermPath Dx Tampa, FL)
Lichen sclerosus, medium power, (a) biopsy from prepuce with sclerotic dense dermal pink paucicellular bottom and a lichenoid lymphocytic infiltrate. In higher power, (b) small lymphocytes, some with halo hugging the base of epidermis and tracking upward, sometimes with atypia simulating haloed lymphocytes in mycosis fungoides (Courtesy of dermatopathologist M. Patel, DermPath Dx Tampa, FL)
T pseudolymphoma with band-like pattern is among the two common patterns of T-cell pseudolymphoma. This patient has chest nodules with appearance of Grover’s disease, lacks T-cell clonality, and has a CD3+ predominant infiltrate with numerous histiocytes and pigmented macrophages. This one may mimic lichenoid or nodular pattern seen in CTCL or that seen secondary to drug hypersensitivity reactions. Other types of patterns seen in hypersensitivity lymphomatoid reactions include interface pattern, psoriasiform dermatitis with lymphoid atypia, nodular lymphoid hyperplasia with B-cell follicular pattern, angiocentric lymphocytic pattern, and finally lymphomatoid follicular mucinosis (Brady et al. 1999)
T-cell pseudolymphoma with nodular T pattern, which is distinct from the frequently described B-cell pattern because of the lack of prominent germinal centers, is composed of small- to medium-sized non-atypical lymphocytes admixed with vessels, histiocytes, plasma cells, and occasional atrophic germinal centers characterized as an often solitary nodule, not usually in the head and neck area, by high CD3:CD20 ratio and CD8 predominance, no aberrancy of T antigens, and lack of clonal T cells by PCR. Some lichenoid keratosis with deep nodules overlaps with T-cell pseudolymphoma. Presence of T-cell clonality and atypia raises concern for a solitary primary cutaneous small- to medium-sized T-cell lymphoma
Benign lichenoid keratosis is a T-cell pseudolymphoma. Variable epidermal acanthosis with closely apposed band-like dense lichenoid lymphocytic infiltrate. Variable numbers of plasma cells, histiocytes, and eosinophils were identified along with non-atypical small lymphocytes and epidermal parakeratosis, which distinguish these lesions from typical lichen planus. Presence of atypical lymphocytes and prominent epidermotropism raises concern for mycosis fungoides (Courtesy of dermatopathologist M. Patel, DermPath Dx Tampa, FL)
Benign, discoid lupus erythematosus (DLE). Basal layer epithelial vacuolar degeneration, atrophy, parakeratosis, pigment incontinence and thickened basement membrane, deep perivascular and periappendiceal lymphocytic infiltrate, and dermal fibroplasia in this long-standing lesion, with beaded basophilic pale areas positive for dermal mucin (Courtesy of dermatopathologist M. Patel, DermPath Dx Tampa, FL)
Benign lymphomatous folliculitis in a patient with follicular plugging and dermal basophilic-beaded mucinous degeneration (bottom) consistent with folliculotropic DLE. Idiopathic pseudolymphomatous folliculitis mimics folliculotropic mycosis fungoides, commonly located on the face as solitary erythematous papules or nodules characterized by regression. Here, a nodular perifollicular infiltrate of lymphocytes with infiltration of follicular structures and dermis, immunostained as a mixture of B and T cells and lack of clonality by PCR
Limitation of Molecular Tests
It is important to realize the limitation of molecular assays. Caution is warranted in interpreting results out of context. This is because it has been observed that tumor cells arise from multiple subclones which show instability or clonal heterogeneity, often obscured by a background of reactive cells, in both cutaneous B-cell and T-cell lymphomas (Ponti et al. 2008). Strategies to overcome these limitations include repeat biopsies, duplicate assays in a single biopsy, and correlation of assay results from more than one site. Repeat biopsies are often done for insufficient samples or equivocal results, and in our experience, superficial biopsy or biopsies with scant infiltrates predispose to indeterminate or possibly false-positive or false-negative test results. Equivocal, oligoclonal, or pseudoclonal results may arise as a reflection of the inherent biology and heterogeneity of these lymphoproliferations. Pitfalls include clonal heterogeneity and false negativity due, respectively, to (1) inherent multiband clonal neoplasm or (2) from a limited primer set or ineffective primer annealing due to somatic point mutations. False-positive results may be due to preferential amplification of individual amplicon within a limited pool of polyclonal cells. In specimens submitted for diagnosis, it is also important to keep in mind that detection of clonality is not by itself diagnostic of malignancy as there are many examples of “clonal dermatitis” (Nihal et al. 2000, 2003). In this regard, clinical correlation is of crucial importance: correlative histopathology with clinical information, prior history, and/or drug intake. In addition, about 14 % show clonal PCR in well-documented drug-induced pseudolymphoma (Brady et al. 1999). Performance of both tests for TCR gamma or beta gene rearrangement or even better to use a sequential gamma then beta test algorithm incorporating clinically determined low- or high-risk probability of disease, as reported and validated by Zhang et al., tends to maximize predictive value and offer cost-effective and rational workup (Zhang et al. 2010); see Fig. 4.4 for diagram of workflow.
Normal TCR gamma/delta gene segments show a restricted TCR repertoire of only 9–11 rearranged segments when compared with 67 segments for TCR beta rearrangements (van Dongen et al. 2003b). In addition, in some viral infections and after organ transplantation, immune response of T cells generates only a limited number of TCR gamma-rearranged segments which present a small number of targets for gene rearrangement assays. Hence, the results can show as few oligoclonal or multiple small bands in PCR. Contrary to some notion that this is often a failure of the test, in reality, this multiband peaks could be a reflection of the inherent biology of reactive lymphoid infiltrate in above settings (Kluin-Nelemans et al. 1998; Mariani et al. 2001). Given the highly sensitive PCR, the oligoclones which manifest in these settings are in reality part of a polyclonal response (van Dongen et al. 2003a). In high clinical risk setting, however, oligoclones may indicate a neoplastic population presenting with several dominant or transformed tumor clones (Zhang et al. 2010).
Pseudoclonality and quantity of lymphocytes: In reactive conditions, DNA in cutaneous lymphoid infiltrates produces a polyclonal pattern when amplified by PCR, but when this DNA is serially diluted, a critical level is reached when an apparent clonal peak appears. This is paralleled by microdissected lymphocytes from reactive proliferations that give rise to pseudoclonality by PCR. It is estimated that 800–2,000 lymphocytes or 20–40 ng of DNA is the threshold where pseudoclonality becomes an issue (Sproul and Goodlad 2012).
Role of Flow Cytometry and Image Cytometry
In the past decade, flow cytometric immunophenotyping has proven to be more reliable than morphologic examination in assessing for lymphoma (Sezary cells) in the peripheral blood of patients with mycosis fungoides and Sezary syndrome, as the neoplastic cells have an aberrant immunophenotype (Borowitz et al. 1993; Klemke et al. 2006; Washington et al. 2002; Meyerson 2008).
Although immunohistochemistry is the most convenient immunophenotyping method in office clinical practice, flow cytometry is the preferred method in multiparameter interrogation of cell characteristics. Included in most cutaneous hematopathology reports is the recommendation to the clinician for additional use of flow cytometry in fresh biopsied tissue for confirmation and for further workup. In flow cytometry-equipped centers, 4–8 mm skin biopsies in fresh state appear adequate for the workup of early CTCL and non-MF cutaneous lymphomas (Novelli et al. 2008; Meyerson 2008; Jokinen et al. 2011). Some biopsies may have scant infiltrate and may not yield adequate cells for analysis; however, some centers can analyze as few as 20 cells and find them to be informative (Wood 2006; Finn et al. 1998). In addition, the remaining cellular specimen can be submitted for molecular PCR analysis, after histologic evaluation.
It is also important to know the limitation of flow cytometry. T-cell antigenic alterations are not entirely specific for mycosis fungoides or Sezary syndrome and have been observed in some reactive conditions (Harmon et al. 1996). In addition, in MF there is heterogeneity with a fraction comprised of tumor cells in a background of reactive T cells, averaging 28 % of lymphocytes in skin as malignant. In about half of MF cases, fewer than 10 % are the malignant “cerebriform” component, and therefore judicious gating of these malignant cells by skillful use of flow cytometry list-mode data is a well-known strategy (Meyerson 2008; Novelli et al. 2008). Without this added manipulation, the neoplastic cells may be submerged or lost within the cluster of reactive T- or B-cell population. Furthermore, the use of numerical or intensity-based diagnostic criteria may enhance the flow cytometry sensitivity.
Discrete patterns of enumerated cells and their antigen density patterns are useful criteria. Cluster analysis of patterns revolves around three useful flow cytometry applications in skin lymphomas:
-
1.
Enumeration (quantification)
-
2.
Antigen density expression
-
3.
Documenting clonality
The following diagnostic and supportive criteria applied to flow cytometry of skin biopsy are recommended: (Meyerson 2008)
-
1.
Diagnostic evidence:
-
On CD45 × side scatter gate, discrete cluster of either:
-
CD4+ CD8−
-
CD8+ CD4−
-
CD4+ CD8+
-
CD4– CD8−
And presence additionally within this gate of :
-
Altered or absent CD2, CD3, CD4, CD5, CD7, CD8, or CD26
-
Aberrant expression of CD10 or CD158k (killer immunoglobulin receptor)
OR
-
-
2.
Presence of Clonal population by TCR Vbeta analysis
Supportive, but not diagnostic evidence:
-
Greater(>) than 50 % CD3+ CD4+ CD7negative (based on CD4 cells)
-
Greater(>) than 80 % CD3+ CD4+ CD26negative (based on CD4 cells)
-
CD4 to CD8 ratio >10:1
-
CD30 expression
-
CD25, HLADR, and CD45RA/RO uniform expression
-
Documenting clonality in a B-cell population is relatively easy by showing a skewed distribution of light chains on B lymphocytes (Fig. 4.15). For T-cell neoplasm, T-cell receptor variable region beta (Vbeta) analysis is used and available in many reference laboratories.
Flow cytometric analysis of T-cell receptor-Vbeta expression is an alternative method to assess and quantify a T-cell clone. Unlike PCR for TCR, a phenotypic signature of the neoplastic population can be monitored post-therapy by a relatively more accessible flow cytometry technique. Moreover, the flow assay will take hours instead of days, when compared with GeneScan CE PCR.
For example, a population of polyclonal T cells will express a random relatively equal distribution of Vbeta proteins on the surface. Flow cytometry, in a patient with neutropenia and lymphocytosis, can detect a population with low expression of antigen such CD5 and, using backtracking, follow that population along tubes of different Vbeta probes; see Fig. 4.16. Clonality can be determined by showing an expansion of cells reacting to a single Vbeta antibody, called direct evidence, or alternatively an absence of reactivity to all panel, called indirect evidence, suggestive of a clone. Lundell et al. directly identified 77 % and indirectly in 23 % of their cases that were PCR confirmed as clonal T cells (Lundell et al. 2005) (Fig. 4.17). Commercially available Vbeta panels (such as Beta Mark TCR repertoire kit by Beckman Coulter) detect about 70 % of the Vbeta families (among a panel directed at 24 markers of Vbeta families). Earlier studies showed concordant results by using a panel covering over 65 % of the T-cell receptor-Vb repertoire. Langerak et al. showed in their study of 47 T-cell lymphoma samples that flow cytometry antibodies detected single Vbeta domain usage in 31 (66 %) and were non-reactive in 16 (34 %), showing 100 % concordance with PCR analysis of the T-cell receptor beta gene (Langerak et al. 2001). Morice et al. studied 29 T-cell lymphoproliferative disorders by flow cytometric Vbeta analysis, including ten cases of cutaneous T-cell lymphoma, and showed a good correlation with molecular methods. This group expanded their study to include 11 Sezary syndrome and six mycosis fungoides cases and showed that Vbeta analysis by flow cytometry was helpful for assessing clonality and quantifying the peripheral blood tumor burden (Morice et al. 2006). Feng et al. validated the clinical utility of flow cytometric T-cell receptor-Vbeta analysis in blood staging of mycosis fungoides and Sezary syndrome patients (Feng et al. 2010).
(a) Forward (FS) and side (SS) scatter distribution dot plot of small- to medium-sized lymphocytes on left panel with backgating selection, on right panel using (red polygon) choosing the dim CD5 and dim CD8 as the target suspicious cluster of abnormal cells (user labeled as red-colored cluster). (b) Dim CD5 and CD8+ (blue polygon) dual parameter flow cytometry enumeration, with user-selected backgating strategy as the target population
In addition, the promise of monitoring a tumor specific antigen is realized in flow cytometry analysis compared to a PCR. Killer immunoglobulin-like receptors or killer inhibitory receptors (KIR assays) for CD158k have been shown to be useful in detecting clonality in MF and Sezary syndrome. Antibody Q66 and AZ158 in flow cytometry appear to be unique to MF/Sezary and not in reactive T cells, occurring in 88–95 % of circulating cells and in 60 % of skin lesions (Bahler et al. 2008; Lundell et al. 2005; Poszepczynska-Guigne et al. 2004; Wechsler et al. 2003), and additionally useful in large granular lymphocytic leukemia (Lundell et al. 2005). Application of KIR family of CD158a-k panel or similar lectin-like receptor CD94 was noted to be useful in skin biopsy detection of NK cell lymphomas (Dukers et al. 2001) and by flow cytometry identifying restricted expression of human CD8 KIR subsets (Bjorkstrom et al. 2012).
Commonly seen in clinical practice of cutaneous hematopathology is the infrequent availability of fresh biopsied tissue that is needed by flow cytometry or the less than widespread request for a Vbeta assessment of T-cell clonality; hence, testing using molecular PCR in formalin-fixed paraffin-embedded tissue to supplement flow cytometric findings is recommended by the International Society for Cutaneous Lymphomas (Pimpinelli et al. 2005) and WHO-EORTC and WHO 2008 (Swerdlow et al. 2008).
However, when fresh tissue is not available for flow cytometry specimen, another tissue assay modality or technique may be used. Flow cytometry requires adequately sampled fresh biopsied tissue, which are not available since skin biopsies are often submitted and processed as formalin-fixed paraffin-embedded tissue. In the absence of flow cytometry, alternative strategies for enumeration and clonality analysis may include image analysis. Image cytometry is the application of image analysis in immunohistochemistry-stained tissue. These are advanced specialized tools for nuanced counting of tumor cells especially useful in biopsies already submitted in paraffin-embedded tissue. In the era of whole slide digital pathology and its applications, image cytometry ranks high as a “holy grail” in desired specialized application.
Image Cytometry
Quantitative immunohistochemistry and 2-dimensional image analysis software tools appear to be upward in outlook and poised to be clinically applicable in the distinction between entities in cutaneous hematopathology. Commercially available systems can quantify tissue immunostains. Garcia-Herrera et al. studies documented a group of patients with a histologic picture of primary cutaneous small and medium T-cell lymphoma that, however, behaved aggressively. They noted that this group could be adequately delineated from those that behaved indolently by the use of image cytometry accurately enumerating Ki-67 and CD8+ cells; see Chap. 10 on PCSMTCL discussion (Garcia-Herrera et al. 2008). This technique was successfully applied previously by Carreras et al. who quantified T regulatory cells, CD3, and CD4 T helper cells in whole-tissue sections of follicular lymphoma and reactive follicles using automated scanning microscope and image analysis systems (Ariol 2.1, SL-50; Applied Imaging Corporation, Newcastle on Tyne, United Kingdom) (Carreras et al. 2006). In addition, this technique was successfully implemented in automatically enumerating Ki67 in paraffin-embedded tissue using VirtualFlow method (PC software module provided by IHCFLOW, Inc. Lutz, FL) in Technology and Innovation (Lloyd et al. 2013). The application of the IHCFLOW technology is described in greater detail as follows since this is a relatively new technique.
The number of Ki67-positive T cells was quantified in whole-tissue sections of all samples using an automated scanning microscope and image analysis system (VirtualFlow 10.10; IHCFLOW, Inc, Lutz, FL). Quantification of the Ki67-positive cells was performed with the nuclear Ki67-module using the following strategy. First, the tissue scanning phase was performed with a 4× objective, followed by an automated 20× medium-magnification capture of the field. Subsequently, the optimal evaluation areas, which accounted for 60–100 % of the whole section, were captured by the two observers using DPlan 20× objective and three color charged-coupled device (CCD) with 1,200 × 1,600 pixels. In the next analysis phase, a nuclear high-resolution classifier which was previously trained for all facets and variables in Ki67 nuclear staining was used. The knowledge-domain-based supervised classifier consisted of a color class definition for the positive and negative nuclei, cytoplasm, and background and a shape-size class definition for the positive and negative nuclei. The color class was defined by the hue, saturation, and intensity parameters, whereas the shape class was defined by the spot width and pixel diameter parameters. The high-throughput classifier was trained in several areas within a tissue sample, often with field with 7,000–10,000 cells in order to avoid miscalculation due to differences in staining and cell composition. The classifier was always trained and recalibrated under the visual supervision of the pathologist. Ki67-positive and Ki67-negative cells were counted independently in the selected compartments. The total number of cells was recorded by adding counts for all compartments. To minimize the heterogeneous distribution of positive cells, a minimum number of ten complete regional areas were selected. Capture to analysis of each image field took 2–10 s in Intel PC, I5, 2.9 mhz CPU. In addition to Ki67, CD8 enumeration of reactive lymphocytes in B-cell lymphomas was performed using VirtualFlow image cytometry in lymph nodal mantle cell lymphomas (Cualing et al. 2007) and a large panel of skin lymphoma-associated antibodies (Fig. 4.19).
A Ki67 (a) positive immunostained lymphocytes in formalin-fixed paraffin-embedded tissue, 20× magnification, and (b) corresponding enumerated counts. Blue dot plot negative, Red dots are positive. Cell size vs. intensity (Lloyd et al. 2013). (c) MUM-1 positive lymphocyte nuclear staining in dermal lymphoid infiltrate (a) and corresponding enumerated nuclei on the right (d). Blue dot plot negative, Red dots are positive. Cell size vs. intensity (Courtesy of IHCFLOW, Lutz, FL).
Likewise, immunostain enumeration was also applied to CD30+ skin lymphomas. A panel of skin target markers in lymphomatoid papulosis (LyP), cutaneous anaplastic large cell lymphoma (ALCL), and systemic ALCL was studied by Rezania et al. (2008) (Fig. 4.19).The count statistics are shown in Table 4.8. Results with statistical significance data suggested the utility of some antibodies, like TRAF-1 in distinction of primary cutaneous CD30+ skin lymphomas and systemic CD30+ ALCL, which has also been observed by Assaf et al. (2007). EMA has also been useful in this regard with positive anaplastic large cells favoring a systemic form with skin involvement. Another application germane to this field was presented as Oral abstract 088 at 2nd world Congress of Cutaneous Lymphomas, Berlin 2013. Using the NUANCE imaging system, low-level CD30 expression was detected in CTCL and was proffered as an explanation for why anti-CD30 (brentuximab) monoclonal antibody treatment was effective in CTCL. (In Krathen MS, Bashey S, Slava K, Wood G et al., brentuximab vedotin demonstrates clinical activity in mycosis fungoides and Sezary syndrome irrespective of tissue CD30 expression by routine immunohistostaining.)
TRAF-1 immunostain on skin biopsy of patients with LyP, cALCL, and sALCL, respectively. The left panel with blue (negative, hematoxylin only) and red dot (positive brown chromogen-decorated cells) plots are the enumeration results with corresponding tissue stains in immediate right of results, respectively. Image cytometry enumeration on alternated panels from left and corresponding immunostains on its right
There has been scant literature in image cytometry application in cutaneous lymphoid infiltrates with few exceptions, despite perceived advantages (Fucich et al. 1999). The direct advantages include optimal use for enumerating the infiltrative areas typical of skin biopsy, which are almost always limited in amount or almost always fixed in formalin. These characteristics lend themselves to tests that are done in situ such as image cytometry, in contrast with a fresh tissue requirement, with disaggregation to single live cells, required in flow cytometry or laser scanning cytometry. The image analysis applications are already commercially available, and its widespread use promises a nuanced distinction between similarly looking entities using tissue-based enumeration. Definiens is an image annotation tool which is also commercially available and has wide application of image cytometry in chromogen-immunostained tissue and excels with its annotation technique (Baatz et al. 2009). VirtualFlow image cytometry software tool is similar in function but takes advantage of the already available camera-equipped microscope with microcomputer interface in typical laboratory settings plus provides a flow cytometry-like enumerated statistic with detection sensitivity from low threshold to high level (0–4+ using the 25 % quartile division) (Rezania et al. 2008) (Table 4.8).
Part II. Spectrum of Nonneoplastic Dermatitis, Atypical Phase or Dyscrasia, and Neoplastic Cutaneous Disorders
Spectrum of Dermatitis, Dyscrasia, Prelymphoma to Lymphoma
Although using morphologic criteria alone is neither sensitive nor specific (Lutzner et al. 1971; van der Loo et al. 1981), identification of defined clinical entities is initially approached using histomorphology and, when combined with clinical information and results of ancillary tests, identifies a more precise point along this benign to malignant spectrum. Guitart et al. identified eight distinct but idiopathic, clinicopathological conditions characterized by frequent clonal detection, chronic course often resistant to topical treatment, and lack of evidence or potential for CTCL and called them cutaneous T-cell lymphoid dyscrasia (Table 4.5) (Guitart and Magro 2007). We extend the list to ten partners.
Putative Partners Often Cited as a Clinical and Pathological Differential with a Continuous Spectrum of Lymphoproliferative T and B Entities from Benign to Malignant
-
1.
Benign erythroderma to clonal erythroderma dyscrasia to erythrodermic MF/Sezary syndrome
-
2.
Vitiligo to hypopigmented interface variant to hypopigmented MF
-
3.
Pityriasis lichenoides to pityriasis lichenoides dyscrasia to MF, variant possibly CD8 type
-
4.
Parapsoriasis to parapsoriasis dyscrasia to parapsoriasis grand plaque to MF
-
5.
Syringolymphoid hyperplasia with alopecia to syringolymphoid MF
-
6.
Benign follicular mucinosis to follicular mucinosis dyscrasia to follicular MF
-
7.
Lupus profundus to atypical lobular lymphocytic panniculitis to indolent subcutaneous lymphoma to subcutaneous panniculitic lymphoma
-
8.
Benign granulomatous lesions to granulomatous dyscrasia to granulomatous MF
-
9.
Cutaneous B-cell hyperplasia to atypical cutaneous B-cell hyperplasia to cutaneous B-cell lymphoma
-
10.
Solitary pseudo T-cell lymphoma to solitary T-cell nodule of uncertain significance to primary cutaneous small and medium T-cell lymphoma
Benign Erythroderma to Clonal Erythroderma Dyscrasia to Erythrodermic MF/Sezary Syndrome
Erythroderma is an inflammatory skin reaction affecting greater than 90 % of body, with an annual incidence of one per 100,000 population (Sigurdsson et al. 2001). Benign causes include eczemas, psoriasis, and drug reaction, but idiopathic erythroderma, which accounts for 15–30 %, appears to have potential to progress to MF (Akhyani et al. 2005; Botella-Estrada et al. 1994; Sigurdsson et al. 1997) (Fig. 4.20).
Chronic idiopathic erythroderma or “red man syndrome” is recalcitrant to therapy, and about 5–12 % from this group may progress to MF/Sezary syndrome (Sigurdsson et al. 1997; Vonderheid 2006). The group that developed MF fulfilled the criteria of pre-Sezary syndrome: chronic erythroderma, Sezary count less than 1,000/ul, lymphadenopathy, and increased IgE (Buechner and Winkelmann 1983; Winkelmann et al. 1984).
Another group that appears to be similar to pre-Sezary syndrome, with clonal expansion of T cells with CD4+ CD7−CD26− but which has not yet developed CTCL after 4 years follow-up, is called monoclonal T-cell dyscrasia of undetermined significance (Gniadecki and Lukowsky 2005). Of 30 patients studied, Gniadecki et al. described ten patients with idiopathic erythroderma, and five showed clonal idiopathic recalcitrant erythroderma which did not fulfill criteria for MF or Sezary syndrome. These five patients had circulating clonal T cells; one of five had both clonal skin and blood findings, with a phenotype of CD4+ CD7−CD26−, and was called clonal erythroderma dyscrasia. The following are characteristics of chronic recalcitrant erythroderma in the elderly labeled as monoclonal T-cell dyscrasia of undetermined significance: (1) symptoms persisting more than 6 months without any response to local or systemic glucocorticoid treatment; (2) monoclonal T cells with a CD7-CD45RO+ phenotype in 37–86 % of cells in the blood, Sezary count less than 5 % or less than 1,000/ul, and a low CD4/CD8 ratio; (3) no lymphadenopathy or bone marrow involvement; (4) blood with increased IgE or eosinophils; and (5) morphologically the CD7− and CD4+ cells are small lymphocytes and not cytologically typical Sezary cells. Skin biopsy shows a superficial perivascular lymphocytic infiltrate which also may be seen in true Sezary syndrome (see Chap. 6).
Non-cerebriform lymphocytes may show a monoclonal CD4+ CD7-CD45RO+ in patients with autoimmune and inflammatory diseases. Rheumatoid arthritis is a typical example (Schmidt et al. 1996). Finding clones of T cells in blood in random studies of patients without T lymphomas may indicate a group called T-cell clones of undetermined significance (Muche et al. 2003). Clonal T-cell populations of undetermined significance are more commonly found in elderly individuals, which is the age group affected by Sezary syndrome (Clambey et al. 2005). However, these clonal T cells of the elderly are derived from CD8+ memory cells which are different from the CD4+ Sezary cell phenotype.
Erythrodermic MF/Sezary Syndrome criteria are well described and include finding clonal T cells and Sezary cell counts of more than 1,000/ul in blood (Olsen et al. 2007; Pimpinelli et al. 2005; Swerdlow et al. 2008) (Fig. 4.21).
Vitiligo to Hypopigmented Interface Variant to Hypopigmented MF
Early inflammatory lesions of vitiligo show epidermotropic features mimicking hypopigmented MF. Exocytosis of lymphocytes into the lower epidermis, and lichenoid pseudolymphomatous lesions in inflammatory vitiligo, and absence of both clinical features of MF and clonality favor vitiligo over MF but sometimes the border between these disorders remains obscure. The most often cited differential diagnosis is benign vitiligo, pityriasis alba, tinea versicolor, and others (El-Darouti et al. 2006).
Guitart et al. described a hypopigmented interface variant that does not fulfill the criteria for hypopigmented MF (Guitart and Magro 2007; Pimpinelli et al. 2005) and is often asymmetric, with minimal scale and no atopic diathesis. Biopsies show basally located epidermotropic CD8+ lymphocytes; these cases respond well to phototherapy with repigmentation (Lambroza et al. 1995; Stone et al. 2001).
However, true hypopigmented lymphomas arising from patients with erythrodermic MF and Sezary syndrome are documented (Bouloc et al. 2000).
Hypopigmented MF characteristics: An overrepresentation of the hypopigmented variant of MF has been described in dark-skinned children of mostly of Asian and African-Caribbean descent although Caucasian patients are also reported (Ardigo et al. 2003). Most patients with childhood-onset hypopigmented disease have experienced no progression beyond stage IB disease (Neuhaus et al. 2000; Whittam et al. 2000), and this subgroup of hypopigmented childhood-onset MF appears to have an excellent prognosis (Fig. 4.22). See Chap. 6 for clinic picture.
(a) Hypopigmented interface variant of T-cell dyscrasia, biopsied from a mulatto teen from Ascension Is. (see Chap. 6 for clinic picture); low-power histopathology shows hypopigmented epidermis with small to intermediate cells along basal layer and perivascular upper dermal infiltrate. (b) High-power view with basal localized haloed atypical lymphocytes, which on PCR demonstrated oligoclonal T gamma bands
Clonality: Both presence (Ardigo et al. 2003) and absence of T-cell clones have been reported, and those without clones were called mimics of hypopigmented MF (Petit et al. 2003; Werner et al. 2005). All seven Caucasian patients reported by Ardigo et al. have had PCR detected T-cell clones. In general, clonality favors CTCL over inflammation. Clonality was demonstrated in 83.5 % of CTCL and in 2.3 % of benign inflammatory disease using heteroduplex PCR (p < 0.001) (Ponti et al. 2008).
Pityriasis Lichenoides to Pityriasis Lichenoides Dyscrasia to Cytotoxic Variant MF
Pityriasis lichenoides is an interface dermatitis with necrotic keratinocytes, migration of lymphocytes into all layers of the epidermis, and extravasated red cells. Pityriasis lichenoides lesions frequently contain clonal T cells. Progression to malignant lymphoma (mycosis fungoides) is rare (Boccara et al. 2012; Magro et al. 2007). The rare pityriasis lichenoides cases that progress include those reported to evolve to a CD8+ type of MF (Tomasini et al. 2002; Wenzel et al. 2005).
PLEVA (pityriasis lichenoides et varioliformis acuta) is the acute form, and PLC (pityriasis lichenoides chronica) is the chronic type, with the former showing predilection for younger patients and the latter for older patients. Clinically, hemorrhagic flares with scarring are seen in the acute form which has been described as predominantly CD8+ cytotoxic in contrast to the predominantly CD4 infiltrate in the chronic form. Phenotypic aberrancy with loss of CD7 is seen in both forms, and despite frequent demonstration of T-cell clonality by PCR, from 57 % (Weinberg et al. 2002) to 67 % (Dereure et al. 2000), most do not progress to clinical MF (Dereure et al. 2000; Kadin 2002; Weinberg et al. 2002; Ko et al. 2000; Magro et al. 2002, 2007). See Chap. 6 for figures and discussion of these cases.
CD8+ MF is a rare variant of MF occurring in less than 5 % of all MF and is associated with an indolent course and frequent poikilodermatous presentation (hypo- or hyperpigmented) (Nikolaou et al. 2009) or junctional localization (Dummer et al 2002). These could arise de novo or in association with LyP or pityriasis lichenoides or follicular MF (Diwan and Ivan 2009; Nikolaou et al. 2009; Tomasini et al. 2002; Dummer et al. 2002). These cases have to be differentiated from aggressive CD8 epidermotropic T-cell lymphoma (Agnarsson et al. 1990; Diwan and Ivan 2009; Nofal et al. 2012; Berti et al. 1999) and from the CD8+ nodular variant of PCSMTCL with predilection to the ear and nose. See Chap. 10 for discussion.
Parapsoriasis to Parapsoriasis Dyscrasia to Parapsoriasis Digitate, “En Grande” Plaque, MF
Parapsoriasis is a group of chronic dermatoses with scaly erythematous patches resembling psoriasis. It has been stated that most MF belong to the conceptual group of parapsoriasis lichenoides (Wolf et al. 2009), and those not fulfilling the MF criteria may be part of the group of parapsoriasis dyscrasias (Guitart and Magro 2007).
For those not fulfilling the criteria for a diagnosis of MF and those cases with a clinical picture of parapsoriasis with minimal epidermotropism, perivascular and interstitial small lymphocytes with insignificant atypia, and lacking Pautrier’s microabscesses but showing clonal T cells on PCR, may belong in the spectrum of parapsoriasis-lymphoid T-cell dyscrasia (Guitart and Magro 2007).
Pre-mycosis fungoides: Although controversial, some evidence indicates that “digitate and large plaque” parapsoriasis may be pre-mycosis fungoides or clinical manifestations of MF, respectively. In small “plaque” (digitate patch) type with patchy lesions, the size and shape of fingerprints have a low frequency of clonal T cells, but 10 % of cases evolve to MF (Vakeva et al. 2005; Burg and Dummer 1995; Hu and Winkelmann 1973; Haeffner et al. 1995; Muche et al. 1999). Some authors believe that cases evolve into CTCL and hence are part of the MF spectrum, but it must be stressed that such instances appear to be rare (Burg et al. 1996, 2002; Belousova et al. 2008). Conservative management is therefore recommended (Cerroni et al. 2009).
A comparison of clonality in early MF and large plaque parapsoriasis showed reproducible results by GeneScan method implying true clones instead of pseudoclonality. A monoclonal T-cell infiltrate was demonstrated by repeated TCR-gamma-PCR in lesional skin specimens in 19.2 % of parapsoriasis patients and in 66.6 % of early-stage MF cases (p = 0.013) (Klemke et al. 2002). Many, therefore, consider “large plaque psoriasis” to a be part of the early presentation of classic MF (Cerroni et al. 2009, Costa et al. 2003; Tamagawa et al. 2005). Some studies document 50 % of “large plaque psoriasis” to contain clonal T cells (Simon et al. 2000) (Fig. 4.23).
Parapsoriasis dyscrasia, showing (a) epidermis with psoriasiform hyperplasia, keratinized stratum corneum, superficial perivascular, and interstitial lymphoid infiltrate, with (b) mild atypia on high-power view showing clusters of irregular hyperchromatic lymphocytes around haloes of Langerhan’s cells. This patient’s biopsy, taken from isolated large plaques, showed T-cell clonality by PCR
Syringolymphoid Hyperplasia with Alopecia to Syringolymphoid Dyscrasia to Syringolymphoid MF
Syringolymphoid hyperplasia with alopecia has been originally described in patients with hyperplastic lymphoid lesions centered on eccrine glands with syringometaplasia (Hobbs et al. 2003; Sarkany 1969). These cases are sometimes associated with MF or follicular mucinosis (Tannous et al. 1999; Thein et al. 2004) and similar histologically to the lymphoepithelial lesions seen in Sjogren’s syndrome (Fig. 4.24). Finding atypical to cerebriform lymphoid cell infiltrate with epidermotropism and eccrinotropism in a case with syringolymphoid hyperplasia raises concern for a syringotropic cutaneous T-cell lymphoma (Burg and Schmockel 1992). Scant molecular clonality data are described (Thein et al. 2004; Tannous et al. 1999).
Some patients with syringolymphoid hyperplasia with alopecia may be asymptomatic or may have pruritic skin lesions, may not respond to corticosteroids, and may have an associated Sjogren’s syndrome (Huang et al. 1996). The clinical differential includes alopecia areata, keratosis pilaris, exanthema, and eczema and, if atypical morphology is lacking, raises a diagnostic dilemma between benign eccrinotropic pseudolymphoma and if with clonality the differential is between adnexotropic dyscrasia or syringotropic mycosis fungoides (Guitart and Magro 2007).
This group with syringolymphoid MF overlaps with some cases of folliculotropic mycosis fungoides, which is generally considered to be a variant of MF. Hobbs described two patients (Hobbs et al. 2003), Thein et al. five cases, (Thein et al. 2004) and Pileri et al. 14 cases, the largest among these series. The clinicopathologic features of these 14 patients with syringotropic MF showed a M:F of 1:4, with a median age of 59 (range, 33–83 years). Eight patients had multiple generalized lesions, and six patients had large, solitary patches or plaques in the extremities, trunk, and eyebrows. Four of these eight patients had existing MF. Histologically, these show prominent involvement of the eccrine glands, some syringometaplasia of glands surrounded by dense lymphoid infiltrates with prominent epitheliotropism. Frequent overlap with typical MF is seen since the epidermis, and hair follicles are described to be involved in 13 and 8 biopsies, respectively (Pileri et al. 2011).
Benign Follicular Mucinosis to Follicular Mucinosis Dyscrasia to Follicular MF
Follicular mucinosis refers to both benign and chronic idiopathic dermatosis in children and lymphoma-related follicular mycosis fungoides or folliculotropic MF (F-MF) in adults with associated follicular mucinosis. Clinical presentations of this MF variant of F-MF include reddish plaques with follicular accentuation, often in the head, scalp, and neck areas in contrast to the often body-suit-localized distribution of typical mycosis fungoides. Pilotropic MF is the term applied to cerebriform infiltrate in hair follicles without mucinosis.
Idiopathic follicular mucinosis was first described in 1957 by Pinkus with follow-up descriptions (Pinkus 1983) and Jablonska et al. who proposed the term “follicular mucinosis” (FM). The histology of juvenile idiopathic form of FM is characterized by follicular retention and follicular hyperkeratosis accompanied by lymphocytic infiltration with an eosinophilic component (Jablonska et al. 1959).
Role of clonal assessment: Consequently, in these cases, T-cell gene rearrangement is often ordered. Absence of clonality along with known etiology favors benign FM, but its absence with a clinically suspected lesion does not rule out follicular MF, since false-negative results occur in early or equivocal cases. However, the presence of clonality, although it favors follicular MF, does not always portend an ominous course, in a setting of follicular mucinosis. For example, Brown et al. reported a 10-year follow-up of seven patients younger than 40 years with primary FM without evidence of associated dermatoses or lymphoma of whom five had clonal T-cell receptor (TCR) gene rearrangements. After follow-up ranging from 5 to 23 years, no patient showed progression to cutaneous T-cell lymphoma and although some patients had persistent manifestations of FM despite various treatments (Brown et al. 2002). It is important to distinguish benign FM from FM associated with mycosis fungoides because the latter carries a grave prognosis (Olsen et al. 2007; van Doorn et al. 2000).
Cerroni et al. 2002 reviewed data from 44 patients with FM divided into two groups, (“idiopathic” FM; mean age 37 · 5 years) comprised 15 patients. Group 2 included 28 patients (mean age 52 · 2 years) with FM associated with mycosis fungoides (MF) or Sézary syndrome. The mean age of patients with “idiopathic” FM was lower, but there were three areas of overlap between the two groups: (1) both appear to localize on the head and neck; (2) the histopathological findings were similar; and (3) about 50 % of tested patients of each group show a monoclonal rearrangement of the TCR γ gene. Differences: One difference is 11/16 (69 %) with “idiopathic” FM had solitary lesions at presentation versus only 2/28 (7 %) with lymphoma-associated FM. Moreover, the lymphoma-associated FM shows lesions in other body sites including body-suit areas. Therefore, the authors proposed that despite overlapping criteria to differentiate “idiopathic” from lymphoma-associated FM, they suggest that “idiopathic” FM might be a localized form of T-cell lymphoma with excellent prognosis but requiring long-term follow-up. Despite and according to these results, it seems idiopathic follicular mucinosis and follicular MF may be distinguishable. For cases that are not clear-cut, it may be useful to recommend long-term follow-up for emergence of MF and similar to the recommendations for the localized variant of pagetoid reticulosis (Woringer–Kolopp disease), solitary MF, and parapsoriasis en plaque. Therefore, long-term follow-up is necessary in patients with so-called “idiopathic” FM (Cerroni et al. 2002). Other authors concur (Boer and Ackerman 2004; Boer et al. 2004). Meanwhile, true benign forms of follicular mucinosis are common in clinical practice.
Benign or reactive follicular mucinosis, when seen in adults, in contrast to the idiopathic variety common in children, may be associated with other clinical conditions such as eczema, discoid lupus erythematosus, or drug induced associated with antidepressant therapy (Magro and Crowson 1996). If the histology is mainly pilotropic, without mucinosis, a suspicion for pilotropic MF without FM is warranted especially if the infiltrate is atypical and clinically shows a body-suit distribution and a clinical picture typical of MF. Lacking atypia or typical MF appearance, pilotropic or follicular mucinosis dyscrasia is the recommended terminology by Magro et al. (Guitart and Magro 2007). In addition, patients with follicular MF are usually older than 40 years, defined histologically with perifollicular and follicular localization of atypical and cerebriform small lymphocytes with or without mucin or hyaluronic acid deposits in hair follicles (colloidal Fe or Alcian blue detection of follicular mucinosis) (Fig. 4.25).
(a) Follicular mucinosis, low-power view, with folliculotropic lymphocytes in outer root sheath and expanded root with mucinous degeneration on right of the picture. (b) Oil power magnification view of the atypical hyperchromatic small- to medium-sized lymphocytes on middle panel. (c) Colloidal Fe stain with bluish red mucinous vacuoles inside follicular spaces
Lupus Profundus to Atypical Lobular Lymphocytic Panniculitis to Indolent Subcutaneous Lymphoma to Subcutaneous Panniculitic Lymphoma
In addition, subcutaneous lymphoid dyscrasia was also referred by Guitart et al. to a group that includes lupus profundus to atypical lymphocytic lobular panniculitis to indolent panniculitic lymphomas (Magro et al. 2001, 2004, 2008; Magro and Wang 2012). The discussion below suggests that clonal T cells in a biopsy of a patient with lobular panniculitis do not necessarily equate to a lymphoma.
Lupus profundus or lupus panniculitis is characterized by multiple nodules, plaques, ulceration, and histology of discoid lupus or not with lipoatrophy and septal and lobular panniculitis, along with karyorrhexis, lymphocytic infiltrates with plasma cells and vasculopathy, as well as mucin deposits (Fig. 4.26). These cases show no clonal T cells (Massone et al. 2005). It is a chronic disease, frequently in adult women with or without lupus epidermal changes, presence of hyaline fat necrosis and hyalinization of lobules and septa, and frequent lymphocytic infiltrates at the periphery of fat lobules, in contrast to the typical findings of rimming of lymphocytes in fat lobules and clonal T cells in subcutaneous panniculitic T-cell lymphoma. In a setting of immunosuppression or organ transplant, infection-related panniculitis is a differential diagnosis characterized by frequent neutrophil-rich infiltrate and granulomatous inflammation, in contrast to the lymphoid-rich infiltrate of lupus panniculitis. Alcohol or chronic pancreatitis-related panniculitis may be considered within the contextual setting, in a male patient with an elevated lipase serology, and presents with painful panniculitis in extremities. Biopsy usually shows presence of ghost necrotic adipocytes.
Atypical lymphocytic lobular panniculitis(ALLP) is a subcutaneous lymphoid dyscrasia often in young male patients with painless nodules in the extremities (Magro et al. 2004), unrelated to lupus panniculitis, histologically with eccrinotropic and lymphohistiocytic infiltrate, nuclear atypia, and focal necrosis associated with clonal T cells (Fig. 4.27). Constitutional symptoms herald overlap with subcutaneous panniculitic T-cell lymphoma(SPTCL) (Guitart and Magro 2007). Both conditions have persistent clonal T cells, small-intermediate size atypical lymphocytes, and aberrant loss of T antigens. However, several differences are seen. SPTCL has a severe angiodestructive pattern with vessel thrombosis, karyorrhectic debris, rimming of hyperchromatic lymphocytes, and fat necrosis, but not seen in ALLP; with less lymphocytic infiltration in ALLP; and with inconspicuous hemophagocytosis in ALLP. Mixed CD4:CD8 with decreased ratio is seen more in ALLP compared to the CD8 predominance in SPTCL or double CD4 and CD8 loss in gamma delta T-cell lymphoma, another cytotoxic lymphoma with frequent panniculitic localization. In addition, presence of germinal centers, prominent mucin deposits, and hyalinosis of fat lobules is more in favor of lupus panniculitis and not ALLP or SPTCL.
Atypical lobular lymphocytic panniculitis, (a) with lymphoid-rich lobular panniculitis, and on molecular test, the lymphocytes are monoclonal T cells by GeneScan PCR but clinically presented with a solitary nodule with no evidence of lymphoma over the years. (b) High-power view with atypical hyperchromatic lymphocytes, permeating interstitial spaces, without rimming of fat spaces. (c) Subcutaneous panniculitic T-cell lymphoma, T alpha–beta cell phenotype, with lobular and septal panniculitis, and minimal dermal involvement, medium-power view. (d) High-power view showing rimming of fat cells with hyperchromatic pleomorphic small- and medium-sized lymphocytes and mixed with cytophagic histiocytes with karyorrhexis and cytophagic granular debris
Additionally, histologically finding “beanbag” cytophagic histiocytes in panniculus raises the differential diagnosis of cytophagic histiocytic panniculitis, especially in a setting with fever and hemorrhagic diathesis (Fig. 4.28) (Requena and Sanchez 2001; Winkelmann 1980; Craig et al. 1998). Cytophagic histiocytic panniculitis (CHP) is a reactive process secondary to a variety of diseases (neoplastic and nonneoplastic) associated with cytophagocytosis, “ beanbag” histiocytes – composed of macrophages with phagocytosed erythrocytes and leucocytes bulging the cytoplasm – and lobular panniculitis. Most CHP are possibly the clinical harbinger of SPTCL.
(a) Cytophagic histiocytic panniculitis, high-power view, of angiocentric lymphoid infiltrate with admixed erythro-cytophagic histiocytes (arrow), and mostly non-atypical small round lymphocytes clustered on vessels and in between fat cells, in a patient with hemophagocytic syndrome, and (b) Giemsa-stained bone marrow imprint with a histiocyte (arrow) with red cell and platelets phagocytosis
There is an overlap between clonal ALLP and clonal CHP, and some of these cases may be part of the early SPTCL. In both CHP and SPTCL, T lymphocytes and histiocytes infiltrate the lobules in sheets or lacelike pattern. A CD4-secreted phagocytic-inducing factor (PIF) may account for the cytophagic properties of the benign histiocytes in CHP. A mixed CD4 CD8 population may be seen in early SPTCL simulating ALLP. Although bone marrow may not show T-cell lymphoma, hemophagocytic syndrome may be seen. Presence of an atypical aggressive clinical presentation with T-cell clonality, CD8 cytotoxic infiltrates, and fatal hemophagocytic syndrome suggests a diagnosis of subcutaneous panniculitic T-cell lymphoma (Gonzalez et al. 1991; Salhany et al. 1998).
Benign Granulomatous Lesions to Granulomatous Dyscrasia to Granulomatous MF
Granulomas are seen in about 2 % of either B-cell or T-cell lymphomas of skin (Scarabello et al. 2002). Histiocytic infiltrates of single cells and clusters are a common component of pseudolymphomas and in the presence of a pseudoclone may lead to a false diagnosis of granulomatous cutaneous lymphoma (Fig. 4.29) (Boer et al. 2008). Significant granulomatous infiltrates comprise at least 25 % of the skin biopsy (Scarabello et al 2002). Giant cells may accompany these clusters or be part of an epithelioid granulomatous infiltrate. Lymphocyte-poor epithelioid granulomas in skin raise sarcoidosis as the primary diagnosis, but lymphoid-rich epithelioid granulomas are most concerning for lymphoma-associated granulomas.
In a setting of mycosis fungoides with granulomas, granulomatous MF and granulomatous slack skin disease are considerations. The histology of these two types is overlapping, but clinically bulky skin folds in intertriginous (groins, scrotal, and axillary) areas favor granulomatous slack skin disease, which tends to have a more favorable long-term course. Recently, a t(3:9) (q12p24) karyotypic marker has been described in GSS (Ikonomou et al. 2007).
A diffuse, nodular, and perivascular pattern is seen in granulomatous MF, and in one of five patients, CD30+ transformed nodules of large MF cells were associated with granulomatous MF. Granulomatous MF typically presents with hyperpigmented or reddish plaques or nodules in an adult male with a 1.5M:F ratio and median age of 46 years (22–71). Histologically, a granuloma annulare-like pattern is not seen and most cases are CD4+ and CD8 negative, similar to MF. Unlike typical MF, epidermotropism in granulomatous MF is absent in half of the cases. Distinction is important because the granulomatous MF variant shows increased extracutaneous spread, therapy resistance, and associated transformed MF and hence shows a decreased disease-specific survival rate of 66 % compared to non-granulomatous Alibert–Bazin MF (Kempf et al. 2008). Large vessel infiltration and multinucleated giant cells are noted in one-third of cases (LeBoit et al. 1988) (Fig. 4.30). Sarcoid-like granulomas are seen in most of the dermis. A juvenile granulomatous variant with onset in childhood appears to have a higher risk for development of another lymphoma.
Most cases (87 %) of granulomatous MF contain clonal T cells, which is a useful distinction from cutaneous sarcoidosis (Kempf et al. 2008). However, finding clonal T cells in a granulomatous dermal lesion is not always diagnostic of granulomatous MF. In a setting of known treatments, a drug-induced granulomatous dyscrasia is a consideration, given that antigen loss and clonal T cells are also present in this group. “Drug-induced lymphoid and granulomatous lymphoid dyscrasia” were recently described in ten patients with reversible lesions by Magro et al. as belonging to the group with persistent T-cell clonal granulomatous dermatitis that resemble granulomatous MF histologically (Magro et al. 2003, 2010).
Cutaneous B-Cell Hyperplasia to Atypical Cutaneous B-Cell Hyperplasia to Cutaneous B-Cell Lymphoma
A cutaneous B-cell hyperplastic pattern with clonal population by PCR was well described (Nihal et al. 2000, 2003) suggesting a continuum of hyperplasia to lymphoma, perhaps analogous to the concept of dyscrasia. We have observed this in practice on repeated biopsies of patients with long-standing cutaneous lymphoid hyperplasia that show slowly progressive histoimmunologic changes that evolve to a B-cell lymphoma (Kulow et al. 2002). We observed an intervening period we call atypical cutaneous lymphoid hyperplasia where histology shows disorganized germinal centers, haphazard mixture of Bcl6+ centroblast clusters with interfollicular T cells, increasing CD20 positive clusters, and deep localization of nodules (Fig. 4.31).The concept of progression from premalignant to malignant B-cell disorder is already well accepted in plasma cell dyscrasia as in the MGUS to myeloma spectrum and in blood lymphocytosis with monoclonal lymphocytosis of uncertain significance to CLL.
Atypical cutaneous lymphoid hyperplasia (ACLH). (a) Large multinodular infiltrate with a top heavy pattern extending to the border of subcutaneous tissue, with fragmented and disorganized germinal centers surrounded by darker mantle zone. The loss of typical biphasic pattern of a normal germinal center (arrow) is often the harbinger of atypical cutaneous B-cell hyperplasia. The figure immediately below A shows atypical pleomorphic cells within a germinal center, a cytologic feature of atypical cutaneous lymphoid hyperplasia. (b) Bcl6-disorganized pattern in ACLH reflective of histology. (c) Similarly, change in Ki67 polarized normal pattern to a haphazard or disorganized pattern is also seen in both ACLH and cutaneous lymphoma. (d). Normal medium-power histology of cutaneous hyperplastic germinal center favoring a benign pattern with the, (e), corresponding polarized Ki67 normal staining with organized polarity of high and low gradation
Solitary Pseudo T-Cell Lymphoma to Solitary T-Cell Nodule of Uncertain Significance to Primary Cutaneous Small and Medium T-Cell Lymphoma
In a study of a large group of PCSMTCL, with many showing clonal T cells, the same group of Beltraminelli et al. upon review of 136 and Leinweber et al. in 26 patients proposed the term “solitary T-cell nodule of uncertain significance” because it appears in both studies to show very rare progression to skin malignancy or skin recurrence in solitary cases. In the group of 136 patients with (male to female = 1:1; median age: 53 years, age range: 3–90 years) cutaneous lesions classified as small-/medium-sized pleomorphic T-cell lymphoma, all but three patients presented with solitary nodules located mostly on the head and neck area . Histopathologic features showed nodular or diffuse infiltrates of small- to medium-sized pleomorphic T lymphocytes, and monoclonal T-cell receptor gamma gene was found in 60 % of tested cases (Fig. 4.32). Follow-up data of 45 patients revealed that 41 patients were alive without lymphoma after a median time of 63 months (range: 1–357 months), whereas four were alive with cutaneous disease (range: 2–16 months). Because of these findings, “cutaneous nodular proliferation of pleomorphic T lymphocytes of undetermined significance” was recommended as properly descriptive of these cases, akin to monoclonal lymphocytosis of uncertain significance and monoclonal gammopathy of uncertain significance in the B-CLL-group and myeloma spectrum, respectively (Beltraminelli et al. 2009; Leinweber et al. 2009)
Conclusion
Despite the judicious use of molecular genetics and flow cytometry, the distinction of benign dermatitis from malignant lymphoma may not be possible in a select few cases, because of the prevailing widely held notion that lymphoid clones may be found in cutaneous biopsies along the clinical spectrum from benign dermatitis to frank lymphoma. Detected clones may be small but because of the ultrasensitive PCR technique are easily recovered from a reactive milieu. Several approaches to clarify an equivocal molecular result in the face of clinical and immunopathological findings may be employed, as we have found useful in cutaneous hematopathology community practice.
We noted in general that this approach is welcome and encouraged by practicing dermatologists who refer challenging biopsies. Hence, confirmation of “true” monoclonality versus clonality in pseudolymphoma is important, and the following strategy and/or recommendations are made:
-
1.
Search for monoclonal gene rearrangements showing identical results from multiple skin biopsy sites, if there are multiple lesions, concurrently or on follow-up.
-
2.
Look for monoclonal identical bands or peaks noted from GeneScan histograms in skin and extracutaneous tissues, such as lymph node or blood.
-
3.
When confronted with suspiciously insufficient DNA from unrepresentative samples, request repeat or excisional biopsy of the entire lesion, or a larger lesion may be a clinically important confirmatory approach. Shave and punch biopsy of a large lesion is often performed to minimize cutaneous morbidity, but if the biopsy turns out to be lymphohematopoietic, a more representative excision or excision of the mass may be a more representative specimen.
-
4.
On repeated T or B-cell gene rearrangements, change in status of clonality and change of status from negative to positive, from biclonal to monoclonal, and from monoclonal to polyclonal are all useful results that require correlation with the clinical course, histopathology, and immunophenotyping. In general, no change of original result supports the monoclonal or polyclonal nature. Confirmation may avoid unnecessary expensive treatment or unneeded expensive laboratory or staging workup (Cualing and Morgan 2013).
-
5.
Clonal identity or persistence of identical monoclonal band clone from dual sites concurrently or from sequential biopsy of different or same sites provides firm evidence of a stable clone of T cells favoring neoplasm over reactive clonal dermatitis (Mahalingam 2003; Thurber et al. 2007; Wood 2001; Zhang et al. 2010) and may reveal transformation of a cutaneous lymphoid hyperplasia to a frank lymphoma in B-cell neoplasm (Kulow et al. 2002).
In those cases with a benign clinical course or a solitary long-standing lesion, despite the finding of confirmed clonality, the positive result may not necessarily be diagnostic of lymphoma, especially when the lesion has disappeared, regressed, or did not progress over several months or years of follow-up. An example may be because of very indolent and unprogressive behavior of some of the cases diagnosed as PCSMTCL; these cases, especially if they are solitary or not monoclonal, may be called “cutaneous nodular proliferation of pleomorphic T lymphocytes of undetermined significance” or “solitary small- to medium-sized pleomorphic T-cell nodules of undetermined significance” as a tenable interpretation (Beltraminelli et al. 2009; Leinweber et al. 2009).
The concept that there is a spectrum of findings between frank reactive inflammatory mimics of lymphoma to clonal dermatitis to frank lymphoma is not new, as we and other authors have reported. However, very few of the persistent clonal but reactive cases progress to lymphoma, and conservative but watchful management appears to be the best plan (Wood 2001; Kulow et al. 2002; Gniadecki 2004; Gniadecki and Lukowsky 2005; Burg et al. 2001, 2005; Guitart and Magro 2007).
References
Agar NS, Wedgeworth E, Crichton S, Mitchell TJ, Cox M, Ferreira S, Robson A, Calonje E, Stefanato CM, Wain EM, Wilkins B, Fields PA, Dean A, Webb K, Scarisbrick J, Morris S, Whittaker SJ. Survival outcomes and prognostic factors in mycosis fungoides/Sezary syndrome: validation of the revised International Society for Cutaneous Lymphomas/European Organisation for Research and Treatment of Cancer staging proposal. J Clin Oncol. 2010;28(31):4730–9.
Agnarsson BA, Vonderheid EC, Kadin ME. Cutaneous T cell lymphoma with suppressor/cytotoxic (CD8) phenotype: identification of rapidly progressive and chronic subtypes. J Am Acad Dermatol. 1990;22(4):569–77.
Akhyani M, Ghodsi ZS, Toosi S, Dabbaghian H. Erythroderma: a clinical study of 97 cases. BMC Dermatol. 2005;5:5.
Albrecht J, Fine LA, Piette W. Drug-associated lymphoma and pseudolymphoma: recognition and management. Dermatol Clin. 2007;25(2):233–44, vi.
Anandasabapathy N, Pulitzer M, Epstein W, Rosenman K, Latkowski JA. Pseudolymphoma evolving into diffuse large B-cell lymphoma. Dermatol Online J. 2008;14(5):22.
Arai E, Okubo H, Tsuchida T, Kitamura K, Katayama I. Pseudolymphomatous folliculitis: a clinicopathologic study of 15 cases of cutaneous pseudolymphoma with follicular invasion. Am J Surg Pathol. 1999;23(11):1313–9.
Arai E, Shimizu M, Hirose T. A review of 55 cases of cutaneous lymphoid hyperplasia: reassessment of the histopathologic findings leading to reclassification of 4 lesions as cutaneous marginal zone lymphoma and 19 as pseudolymphomatous folliculitis. Hum Pathol. 2005;36(5):505–11.
Arai E, Shimizu M, Tsuchida T, Izaki S, Ogawa F, Hirose T. Lymphomatoid keratosis: an epidermotropic type of cutaneous lymphoid hyperplasia: clinicopathological, immunohistochemical, and molecular biological study of 6 cases. Arch Dermatol 2007;143:53–9.
Ardigo M, Borroni G, Muscardin L, Kerl H, Cerroni L. Hypopigmented mycosis fungoides in Caucasian patients: a clinicopathologic study of 7 cases. J Am Acad Dermatol 2003;49:264–70.
Assaf C, Hirsch B, Wagner F, Lucka L, Grunbaum M, Gellrich S, Lukowsky A, Sterry W, Stein H, Durkop H. Differential expression of TRAF1 aids in the distinction of cutaneous CD30-positive lymphoproliferations. J Invest Dermatol. 2007;127(8):1898–904.
Baatz M, Zimmermann J, Blackmore CG. Automated analysis and detailed quantification of biomedical images using Definiens Cognition Network Technology. Comb Chem High Throughput Screen. 2009;12(9):908–16.
Bahler DW, Hartung L, Hill S, Bowen GM, Vonderheid EC. CD158k/KIR3DL2 is a useful marker for identifying neoplastic T-cells in Sezary syndrome by flow cytometry. Cytometry B Clin Cytom. 2008;74(3):156–62.
Belousova IE, Vanecek T, Samtsov AV, Michal M, Kazakov DV. A patient with clinicopathologic features of small plaque parapsoriasis presenting later with plaque-stage mycosis fungoides: report of a case and comparative retrospective study of 27 cases of “nonprogressive” small plaque parapsoriasis. J Am Acad Dermatol. 2008;59(3):474–82.
Beltraminelli H, Leinweber B, Kerl H, Cerroni L. Primary cutaneous CD4+ small-/medium-sized pleomorphic T-cell lymphoma: a cutaneous nodular proliferation of pleomorphic T lymphocytes of undetermined significance? A study of 136 cases. Am J Dermatopathol. 2009;31(4):317–22.
Bergman R. Pseudolymphoma and cutaneous lymphoma: facts and controversies. Clin Dermatol. 2010;28(5):568–74.
Berti E, Tomasini D, Vermeer MH, Meijer CJ, Alessi E, Willemze R. Primary cutaneous CD8-positive epidermotropic cytotoxic T cell lymphomas. A distinct clinicopathological entity with an aggressive clinical behavior. Am J Pathol. 1999;155(2):483–92.
Bjorkstrom NK, Beziat V, Cichocki F, Liu LL, Levine J, Larsson S, Koup RA, Anderson SK, Ljunggren HG, Malmberg KJ. CD8 T cells express randomly selected KIRs with distinct specificities compared with NK cells. Blood. 2012;120(17):3455–65.
Boccara O, Blanche S, de PY, Brousse N, Bodemer C, Fraitag S. Cutaneous hematologic disorders in children. Pediatr Blood Cancer 2012;58:226–32.
Boer A, Ackerman AB. Alopecia mucinosa or follicular mucinosis – the problem is terminology! J Cutan Pathol. 2004;31(2):210–1.
Boer A, Guo Y, Ackerman AB. Alopecia mucinosa is mycosis fungoides. Am J Dermatopathol. 2004;26(1):33–52.
Boer A, Tirumalae R, Bresch M, Falk TM. Pseudoclonality in cutaneous pseudolymphomas: a pitfall in interpretation of rearrangement studies. Br J Dermatol. 2008;159(2):394–402.
Borowitz MJ, Weidner A, Olsen EA, Picker LJ. Abnormalities of circulating T-cell subpopulations in patients with cutaneous T-cell lymphoma: cutaneous lymphocyte-associated antigen expression on T cells correlates with extent of disease. Leukemia. 1993;7(6):859–63.
Botella-Estrada R, Sanmartin O, Oliver V, Febrer I, Aliaga A. Erythroderma. A clinicopathological study of 56 cases. Arch Dermatol. 1994;130(12):1503–7.
Boudova L, Kazakov DV, Sima R, Vanecek T, Torlakovic E, Lamovec J, et al. Cutaneous lymphoid hyperplasia and other lymphoid infiltrates of the breast nipple: a retrospective clinicopathologic study of fifty-six patients. Am J Dermatopathol. 2005;27(5):375–86.
Bouloc A, Fau-Larue MH, Lenormand B, Meunier F, Wechsler J, Thomine E, et al. Polymerase chain reaction analysis of immunoglobulin gene rearrangement in cutaneous lymphoid hyperplasias. French Study Group for Cutaneous Lymphomas. Arch Dermatol. 1999;135(2):168–72.
Bouloc A, Grange F, fau-Larue MH, Dieng MT, Tortel MC, Avril MF, Revuz J, Bagot M, Wechsler J. Leucoderma associated with flares of erythrodermic cutaneous T-cell lymphomas: four cases. The French Study Group of Cutaneous Lymphomas. Br J Dermatol. 2000;143(4):832–6.
Brady SP, Magro CM, az-Cano SJ, Wolfe HJ. Analysis of clonality of atypical cutaneous lymphoid infiltrates associated with drug therapy by PCR/DGGE. Hum Pathol. 1999;30(2):130–6.
Brown HA, Gibson LE, Pujol RM, Lust JA, Pittelkow MR. Primary follicular mucinosis: long-term follow-up of patients younger than 40 years with and without clonal T-cell receptor gene rearrangement. J Am Acad Dermatol. 2002;47(6):856–62.
Bruggemann M, White H, Gaulard P, Garcia-Sanz R, Gameiro P, Oeschger S, Jasani B, Ott M, Delsol G, Orfao A, Tiemann M, Herbst H, Langerak AW, Spaargaren M, Moreau E, Groenen PJ, Sambade C, Foroni L, Carter GI, Hummel M, Bastard C, Davi F, fau-Larue MH, Kneba M, van Dongen JJ, Beldjord K, Molina TJ. Powerful strategy for polymerase chain reaction-based clonality assessment in T-cell malignancies Report of the BIOMED-2 Concerted Action BHM4 CT98-3936. Leukemia. 2007;21(2):215–21.
Buechner SA, Winkelmann RK. Pre-Sezary erythroderma evolving to Sezary syndrome. A report of seven cases. Arch Dermatol. 1983;119(4):285–91.
Burg G, Dummer R. Small plaque (digitate) parapsoriasis is an ‘abortive cutaneous T-cell lymphoma’ and is not mycosis fungoides. Arch Dermatol. 1995;131(3):336–8.
Burg G, Dummer R, Haeffner A, Kempf W, Kadin M. From inflammation to neoplasia: mycosis fungoides evolves from reactive inflammatory conditions (lymphoid infiltrates) transforming into neoplastic plaques and tumors. Arch Dermatol 2001;137:949–52.
Burg G, Dummer R, Kempf W. Dyscrasias with “undetermined significance”. Arch Dermatol. 2005;141(3):382–4.
Burg G, Dummer R, Nestle FO, Doebbeling U, Haeffner A. Cutaneous lymphomas consist of a spectrum of nosologically different entities including mycosis fungoides and small plaque parapsoriasis. Arch Dermatol. 1996;132(5):567–72.
Burg G, Kempf W, Haeffner A, Dobbeling U, Nestle FO, Boni R, Kadin M, Dummer R. From inflammation to neoplasia: new concepts in the pathogenesis of cutaneous lymphomas. Recent Results Cancer Res. 2002;160:271–80.
Burg G, Schmockel C. Syringolymphoid hyperplasia with alopecia–a syringotropic cutaneous T-cell lymphoma? Dermatology. 1992;184(4):306–7.
Camilot D, Arnez ZM, Luzar B, Pizem J, Zgavec B, Falconieri G. Cutaneous pseudolymphoma following tattoo application: report of two new cases of a potential lymphoma mimicker. Int J Surg Pathol. 2012;20(3):311–5.
Carreras J, Lopez-Guillermo A, Fox BC, Colomo L, Martinez A, Roncador G, Montserrat E, Campo E, Banham AH. High numbers of tumor-infiltrating FOXP3-positive regulatory T cells are associated with improved overall survival in follicular lymphoma. Blood. 2006;108(9):2957–64.
Cerroni L, Fink-Puches R, Back B, Kerl H. Follicular mucinosis: a critical reappraisal of clinicopathologic features and association with mycosis fungoides and Sezary syndrome. Arch Dermatol. 2002;138(2):182–9.
Cerroni L, Gatter K, Kerl H. Skin lymphoma: the illustrated guide. 3rd ed. Hoboken, NJ, USA: Wiley-Blackwell; 2009.
Clambey ET, van Dyk LF, Kappler JW, Marrack P. Non-malignant clonal expansions of CD8+ memory T cells in aged individuals. Immunol Rev. 2005;205:170–89.
Costa C, Gallardo F, Bellosillo B, Espinet B, Pujol RM, Barranco C, Serrano S, Sole F. Analysis of T-cell receptor gamma gene rearrangements by PCR-Genescan and PCR-polyacrylamide gel electrophoresis in early-stage mycosis fungoides/large-plaque parapsoriasis. Dermatology. 2003;207(4):418–9.
Cozzio A, French LE. T-cell clonality assays: how do they compare? J Invest Dermatol. 2008;128(4):771–3.
Craig AJ, Cualing H, Thomas G, Lamerson C, Smith R. Cytophagic histiocytic panniculitis – a syndrome associated with benign and malignant panniculitis: case comparison and review of the literature. J Am Acad Dermatol. 1998;39(5 Pt 1):721–36.
Cualing HD, Morgan MB. Experience and lessons from use of molecular clonality PCR tests in cutaneous hematopathology practice. Arch Pathol Lab Med. Archives of Pathology & Laboratory Medicine: October 2013, Vol. 137, No. 10, pp. 1343–1526. doi: http://dx.doi.org/10.5858/arpa.2013-0354-AB)
Cualing HD, Zhong E, Moscinski L. “Virtual flow cytometry” of immunostained lymphocytes on microscopic tissue slides: iHCFlow tissue cytometry. Cytometry B Clin Cytom. 2007;72(1):63–76.
Dabiri S, Morales A, Ma L, Sundram U, Kim YH, Arber DA, et al. The frequency of dual TCR-PCR clonality in granulomatous disorders. J Cutan Pathol. 2011;38(9):704–9.
Dereure O, Levi E, Kadin ME. T-Cell clonality in pityriasis lichenoides et varioliformis acuta: a heteroduplex analysis of 20 cases. Arch Dermatol. 2000;136(12):1483–6.
Diwan H, Ivan D. CD8-positive mycosis fungoides and primary cutaneous aggressive epidermotropic CD8-positive cytotoxic T-cell lymphoma. J Cutan Pathol. 2009;36(3):390–2.
Dukers DF, Vermeer MH, Jaspars LH, Sander CA, Flaig MJ, Vos W, Willemze R, Meijer CJ. Expression of killer cell inhibitory receptors is restricted to true NK cell lymphomas and a subset of intestinal enteropathy-type T cell lymphomas with a cytotoxic phenotype. J Clin Pathol. 2001;54(3):224–8.
Dummer R, Kamarashev J, Kempf W, Haffner AC, Hess-Schmid M, Burg G. Junctional CD8+ cutaneous lymphomas with nonaggressive clinical behavior: a CD8+ variant of mycosis fungoides? Arch Dermatol. 2002;138(2):199–203.
Eisendle K, Zelger B. The expanding spectrum of cutaneous borreliosis. G Ital Dermatol Venereol. 2009;144(2):157–71.
El-Darouti MA, Marzouk SA, Azzam O, Fawzi MM, bdel-Halim MR, Zayed AA, Leheta TM. Vitiligo vs. hypopigmented mycosis fungoides (histopathological and immunohistochemical study, univariate analysis). Eur J Dermatol. 2006;16(1):17–22.
Feng B, Jorgensen JL, Jones D, Chen SS, Hu Y, Medeiros LJ, Wang SA. Flow cytometric detection of peripheral blood involvement by mycosis fungoides and Sezary syndrome using T-cell receptor Vbeta chain antibodies and its application in blood staging. Mod Pathol. 2010;23(2):284–95.
Finn WG, Peterson LC, James C, Goolsby CL. Enhanced detection of malignant lymphoma in cerebrospinal fluid by multiparameter flow cytometry. Am J Clin Pathol. 1998;110(3):341–6.
Flaig MJ, Schuhmann K, Sander CA. Impact of molecular analysis in the diagnosis of cutaneous lymphoid infiltrates. Semin Cutan Med Surg. 2000;19(2):87–90.
Fucich LF, Freeman SF, Boh EE, McBurney E, Marrogi AJ. Atypical cutaneous lymphocytic infiltrate and a role for quantitative immunohistochemistry and gene rearrangement studies. Int J Dermatol. 1999;38(10):749–56.
Fujimura T, Hidaka T, Hashimoto A, Aiba S. Dermoscopy findings of pseudolymphomatous folliculitis. Case Rep Dermatol. 2012;4(2):154–7.
Gallardo F, Bellosillo B, Serrano S, Pujol RM. Genotypic analysis in primary cutaneous lymphomas using the standardized BIOMED-2 polymerase chain reaction protocols. Actas Dermosifiliogr. 2008;99(8):608–20.
Garcia-Herrera A, Colomo L, Camos M, Carreras J, Balague O, Martinez A, Lopez-Guillermo A, Estrach T, Campo E. Primary cutaneous small/medium CD4+ T-cell lymphomas: a heterogeneous group of tumors with different clinicopathologic features and outcome. J Clin Oncol. 2008;26(20):3364–71.
Gilliam AC, Wood GS. Cutaneous lymphoid hyperplasias. Semin Cutan Med Surg. 2000;19(2):133–41.
Gniadecki R. Neoplastic stem cells in cutaneous lymphomas: evidence and clinical implications. Arch Dermatol. 2004;140(9):1156–60.
Gniadecki R, Lukowsky A. Monoclonal T-cell dyscrasia of undetermined significance associated with recalcitrant erythroderma. Arch Dermatol. 2005;141(3):361–7.
Gonzalez CL, Medeiros LJ, Braziel RM, Jaffe ES. T-cell lymphoma involving subcutaneous tissue. A clinicopathologic entity commonly associated with hemophagocytic syndrome. Am J Surg Pathol. 1991;15(1):17–27.
Guitart J, Magro C. Cutaneous T-cell lymphoid dyscrasia: a unifying term for idiopathic chronic dermatoses with persistent T-cell clones. Arch Dermatol. 2007;143(7):921–32.
Guitart J, Kennedy J, Ronan S, Chmiel JS, Hsiegh YC, Variakojis D. Histologic criteria for the diagnosis of mycosis fungoides: proposal for a grading system to standardize pathology reporting. J Cutan Pathol. 2001;28(4):174–83.
Haeffner AC, Smoller BR, Zepter K, Wood GS. Differentiation and clonality of lesional lymphocytes in small plaque parapsoriasis. Arch Dermatol. 1995;131(3):321–4.
Harmon CB, Witzig TE, Katzmann JA, Pittelkow MR. Detection of circulating T cells with CD4+ CD7- immunophenotype in patients with benign and malignant lymphoproliferative dermatoses. J Am Acad Dermatol. 1996;35(3 Pt 1):404–10.
Hobbs JL, Chaffins ML, Douglass MC. Syringolymphoid hyperplasia with alopecia: two case reports and review of the literature. J Am Acad Dermatol. 2003;49(6):1177–80.
Holm N, Flaig MJ, Yazdi AS, Sander CA. The value of molecular analysis by PCR in the diagnosis of cutaneous lymphocytic infiltrates. J Cutan Pathol. 2002;29(8):447–52.
Hu CH, Winkelmann RK. Digitate dermatosis. A new look at symmetrical, small plaque parapsoriasis. Arch Dermatol. 1973;107(1):65–9.
Huang CL, Kuo TT, Chan HL. Acquired generalized hypohidrosis/anhidrosis with subclinical Sjogren’s syndrome: report of a case with diffuse syringolymphoid hyperplasia and lymphocytic sialadenitis. J Am Acad Dermatol. 1996;35(2 Pt 2):350–2.
Hughes J, Weston S, Bennetts B, Prasad M, Angulo R, Jaworskit R, Jolles S, Kossard S, Fox S, Benson E. The application of a PCR technique for the detection of immunoglobulin heavy chain gene rearrangements in fresh or paraffin-embedded skin tissue. Pathology. 2001;33(2):222–5.
Ikonomou IM, Aamot HV, Heim S, Fossa A, Delabie J. Granulomatous slack skin with a translocation t(3;9)(q12;p24). Am J Surg Pathol. 2007;31(5):803–6.
Jablonska S, Chorzelski T, LANCUCKI J. Mucinosis follicularis. Hautarzt. 1959;10:27–33.
Jackson S, and Nesbit L. Differential diagnosis for the dermatologist. 2nd ed. New York: Springer; 2012.
Jokinen CH, Fromm JR, Argenyi ZB, Olerud J, Wood BL, Greisman HA. Flow cytometric evaluation of skin biopsies for mycosis fungoides. Am J Dermatopathol. 2011;33(5):483–91.
Kadin ME. T-cell clonality in pityriasis lichenoides: evidence for a premalignant or reactive immune disorder? Arch Dermatol. 2002;138(8):1089–90.
Kakizaki A, Fujimura T, Numata I, Hashimoto A, Aiba S. Pseudolymphomatous folliculitis on the nose. Case Rep Dermatol. 2012;4(1):27–30.
Kazakov DV, Kutzner H, Palmedo G, Boudova L, Michaelis S, Michal M, et al. Primary cutaneous lymphoproliferative disorders with dual lineage rearrangement. Am J Dermatopathol. 2006;28(5):399–409.
Kazakov DV, Belousova IE, Kacerovska D, Sima R, Vanecek T, Vazmitel M, et al. Hyperplasia of hair follicles and other adnexal structures in cutaneous lymphoproliferative disorders: a study of 53 cases, including so-called pseudolymphomatous folliculitis and overt lymphomas. Am J Surg Pathol. 2008;32(10):1468–78.
Kempf W, Levi E, Kamarashev J, et al. Fascin expression in CD30-positive cutaneous lymphoproliferative disorders. J Cutan Pathol. 2002;29:295–300.
Kempf W, Ostheeren-Michaelis S, Paulli M, Lucioni M, Wechsler J, Audring H, Assaf C, Rudiger T, Willemze R, Meijer CJ, Berti E, Cerroni L, Santucci M, Hallermann C, Berneburg M, Chimenti S, Robson A, Marschalko M, Kazakov DV, Petrella T, Fraitag S, Carlotti A, Courville P, Laeng H, Knobler R, Golling P, Dummer R, Burg G. Granulomatous mycosis fungoides and granulomatous slack skin: a multicenter study of the Cutaneous Lymphoma Histopathology Task Force Group of the European Organization For Research and Treatment of Cancer (EORTC). Arch Dermatol. 2008;144(12):1609–17.
Kerl K. Histopathological patterns indicative of distinct adverse drug reactions. Chem Immunol Allergy. 2012;97:61–78.
Klemke CD, Dippel E, Dembinski A, Ponitz N, Assaf C, Hummel M, Stein H, Goerdt S. Clonal T cell receptor gamma-chain gene rearrangement by PCR-based GeneScan analysis in the skin and blood of patients with parapsoriasis and early-stage mycosis fungoides. J Pathol. 2002;197(3):348–54.
Klemke CD, Fritzsching B, Franz B, Kleinmann EV, Oberle N, Poenitz N, Sykora J, Banham AH, Roncador G, Kuhn A, Goerdt S, Krammer PH, Suri-Payer E. Paucity of FOXP3+ cells in skin and peripheral blood distinguishes Sezary syndrome from other cutaneous T-cell lymphomas. Leukemia. 2006;20(6):1123–9.
Kluin-Nelemans HC, Kester MG, van deCorput L, Boor PP, Landegent JE, van Dongen JJ, Willemze R, Falkenburg JH. Correction of abnormal T-cell receptor repertoire during interferon-alpha therapy in patients with hairy cell leukemia. Blood. 1998;91(11):4224–31.
Ko JW, Seong JY, Suh KS, Kim ST. Pityriasis lichenoides-like mycosis fungoides in children. Br J Dermatol. 2000;142(2):347–52.
Kulow BF, Cualing H, Steele P, VanHorn J, Breneman JC, Mutasim DF, Breneman DL. Progression of cutaneous B-cell pseudolymphoma to cutaneous B-cell lymphoma. J Cutan Med Surg. 2002;6(6):519–28.
Lambroza E, Cohen SR, Phelps R, Lebwohl M, Braverman IM, DiCostanzo D. Hypopigmented variant of mycosis fungoides: demography, histopathology, and treatment of seven cases. J Am Acad Dermatol. 1995;32(6):987–93.
Langerak AW, van Den BR, Wolvers-Tettero IL, Boor PP, van Lochem EG, Hooijkaas H, van Dongen JJ. Molecular and flow cytometric analysis of the Vbeta repertoire for clonality assessment in mature TCRalphabeta T-cell proliferations. Blood. 2001;98(1):165–73.
Langerak AW, Groenen PJ, Bruggemann M, Beldjord K, Bellan C, Bonello L, Boone E, Carter GI, Catherwood M, Davi F, fau-Laure MH, Diss T, Evans PA, Gameiro P, Garcia SR, Gonzalez D, Grand D, Hakansson A, Hummel M, Liu H, Lombardia L, Macintyre EA, Milner BJ, Montes-Moreno S, Schuuring E, Spaargaren M, Hodges E, van Dongen JJ. EuroClonality/BIOMED-2 guidelines for interpretation and reporting of Ig/TCR clonality testing in suspected lymphoproliferations. Leukemia. 2012;26(10):2159–71.
LeBoit PE, Zackheim HS, White Jr CR. Granulomatous variants of cutaneous T-cell lymphoma. The histopathology of granulomatous mycosis fungoides and granulomatous slack skin. Am J Surg Pathol. 1988;12(2):83–95.
Leinweber B, Beltraminelli H, Kerl H, Cerroni L. Solitary small- to medium-sized pleomorphic T-cell nodules of undetermined significance: clinical, histopathological, immunohistochemical and molecular analysis of 26 cases. Dermatology. 2009;219(1):42–7.
Lloyd M, Burke N, Kalantapour F, Niesen M, Hall A, Pennypacker K, Citron B, Chiam P, Vernard A, Mohasweta D, Mohapatra S, Cualing H, Blanck G. Quantitative morphological and molecular pathology 1 of the human thymus correlate with infant cause of death. Technology and Innovation – Proceedings of the National Academy of Inventors™, Tampa, University of South Florida (in press).
Lukowsky A, Muche JM, Sterry W, Audring H. Detection of expanded T cell clones in skin biopsy samples of patients with lichen sclerosus et atrophicus by T cell receptor-gamma polymerase chain reaction assays. J Invest Dermatol. 2000;115(2):254–9.
Lukowsky A, Muche JM, Mobs M, Assaf C, Humme D, Hummel M, Sterry W, Steinhoff M. Evaluation of T-cell clonality in archival skin biopsy samples of cutaneous T-cell lymphomas using the biomed-2 PCR protocol. Diagn Mol Pathol. 2010;19(2):70–7.
Lundell R, Hartung L, Hill S, Perkins SL, Bahler DW. T-cell large granular lymphocyte leukemias have multiple phenotypic abnormalities involving pan-T-cell antigens and receptors for MHC molecules. Am J Clin Pathol. 2005;124(6):937–46.
Luo V, Lessin SR, Wilson RB, Rennert H, Tozer C, Benoit B, Leonard DG. Detection of clonal T-cell receptor gamma gene rearrangements using fluorescent-based PCR and automated high-resolution capillary electrophoresis. Mol Diagn. 2001;6(3):169–79.
Lutzner MA, Hobbs JW, Horvath P. Ultrastructure of abnormal cells in Sezary syndrome, mycosis fungoides, and parapsoriasis en plaque. Arch Dermatol. 1971;103(4):375–86.
Magro CM, Crowson AN. Drug-induced immune dysregulation as a cause of atypical cutaneous lymphoid infiltrates: a hypothesis. Hum Pathol. 1996;27(2):125–32.
Magro CM, Wang X. Indolent primary cutaneous gamma/delta T-cell lymphoma localized to the subcutaneous panniculus and its association with atypical lymphocytic lobular panniculitis. Am J Clin Pathol. 2012;138(1):50–6.
Magro CM, Crowson AN, Harrist TJ. Atypical lymphoid infiltrates arising in cutaneous lesions of connective tissue disease. Am J Dermatopathol. 1997;19(5):446–55.
Magro CM, Crowson AN, Kovatich AJ, Burns F. Lupus profundus, indeterminate lymphocytic lobular panniculitis and subcutaneous T-cell lymphoma: a spectrum of subcuticular T-cell lymphoid dyscrasia. J Cutan Pathol. 2001;28(5):235–47.
Magro C, Crowson AN, Kovatich A, Burns F. Pityriasis lichenoides: a clonal T-cell lymphoproliferative disorder. Hum Pathol. 2002;33(8):788–95.
Magro CM, Crowson AN, Kovatich AJ, Burns F. Drug-induced reversible lymphoid dyscrasia: a clonal lymphomatoid dermatitis of memory and activated T cells. Hum Pathol. 2003;34(2):119–29.
Magro CM, Crowson AN, Byrd JC, Soleymani AD, Shendrik I. Atypical lymphocytic lobular panniculitis. J Cutan Pathol. 2004;31(4):300–6.
Magro CM, Crowson AN, Morrison C, Li J. Pityriasis lichenoides chronica: stratification by molecular and phenotypic profile. Hum Pathol 2007;38:479–90.
Magro CM, Schaefer JT, Morrison C, Porcu P. Atypical lymphocytic lobular panniculitis: a clonal subcutaneous T-cell dyscrasia. J Cutan Pathol. 2008;35(10):947–54.
Magro CM, Cruz-Inigo AE, Votava H, Jacobs M, Wolfe D, Crowson AN. Drug-associated reversible granulomatous T cell dyscrasia: a distinct subset of the interstitial granulomatous drug reaction. J Cutan Pathol. 2010;37 Suppl 1:96–111.
Mahalingam M. Atypical cutaneous lymphocytic infiltrate--aucicellularity and ‘pseudo’clonality. J Cutan Pathol. 2003;30(8):521.
Mariani S, Coscia M, Even J, Peola S, Foglietta M, Boccadoro M, Sbaiz L, Restagno G, Pileri A, Massaia M. Severe and long-lasting disruption of T-cell receptor diversity in human myeloma after high-dose chemotherapy and autologous peripheral blood progenitor cell infusion. Br J Haematol. 2001;113(4):1051–9.
Massone C, Kodama K, Salmhofer W, Abe R, Shimizu H, Parodi A, Kerl H, Cerroni L. Lupus erythematosus panniculitis (lupus profundus): clinical, histopathological, and molecular analysis of nine cases. J Cutan Pathol. 2005;32(6):396–404.
Melotti CZ, Amary MF, Sotto MN, Diss T, Sanches JA. Polymerase chain reaction-based clonality analysis of cutaneous B-cell lymphoproliferative processes. Clinics (Sao Paulo). 2010;65(1):53–60.
Meyer JC, Hassam S, Dummer R, Muletta S, Dobbeling U, Dommann SN, Burg G. A realistic approach to the sensitivity of PCR-DGGE and its application as a sensitive tool for the detection of clonality in cutaneous T-cell proliferations. Exp Dermatol. 1997;6(3):122–7.
Meyerson HJ. Flow cytometry for the diagnosis of mycosis fungoides. G Ital Dermatol Venereol. 2008;143(1):21–41.
Morales AV, Arber DA, Seo K, Kohler S, Kim YH, Sundram UN. Evaluation of B-cell clonality using the BIOMED-2 PCR method effectively distinguishes cutaneous B-cell lymphoma from benign lymphoid infiltrates. Am J Dermatopathol. 2008;30(5):425–30.
Morice WG, Katzmann JA, Pittelkow MR, El-Azhary RA, Gibson LE, Hanson CA. A comparison of morphologic features, flow cytometry, TCR-Vbeta analysis, and TCR-PCR in qualitative and quantitative assessment of peripheral blood involvement by Sezary syndrome. Am J Clin Pathol. 2006;125(3):364–74.
Muche JM, Lukowsky A, Heim J, Friedrich M, Audring H, Sterry W. Demonstration of frequent occurrence of clonal T cells in the peripheral blood but not in the skin of patients with small plaque parapsoriasis. Blood. 1999;94(4):1409–17.
Muche JM, Sterry W, Gellrich S, Rzany B, Audring H, Lukowsky A. Peripheral blood T-cell clonality in mycosis fungoides and nonlymphoma controls. Diagn Mol Pathol. 2003;12(3):142–50.
Murphy M, Signoretti S, Kadin ME, Loda M. Detection of TCR-gamma gene rearrangements in early mycosis fungoides by non-radioactive PCR-SSCP. J Cutan Pathol 2000;27:228-34.
Nakamura M, Kabashima K, Tokura Y. Pseudolymphomatous folliculitis presenting with multiple nodules. Eur J Dermatol. 2009;19(3):263–4.
Neuhaus IM, Ramos-Caro FA, Hassanein AM. Hypopigmented mycosis fungoides in childhood and adolescence. Pediatr Dermatol. 2000;17(5):403–6.
Nihal M, Mikkola D, Wood GS. Detection of clonally restricted immunoglobulin heavy chain gene rearrangements in normal and lesional skin: analysis of the B cell component of the skin-associated lymphoid tissue and implications for the molecular diagnosis of cutaneous B cell lymphomas. J Mol Diagn. 2000;2(1):5–10.
Nihal M, Mikkola D, Horvath N, Gilliam AC, Stevens SR, Spiro TP, Cooper KD, Wood GS. Cutaneous lymphoid hyperplasia: a lymphoproliferative continuum with lymphomatous potential. Hum Pathol. 2003;34(6):617–22.
Nikolaou VA, Papadavid E, Katsambas A, Stratigos AJ, Marinos L, Anagnostou D, Antoniou C. Clinical characteristics and course of CD8+ cytotoxic variant of mycosis fungoides: a case series of seven patients. Br J Dermatol. 2009;161(4):826–30.
Nofal A, bdel-Mawla MY, Assaf M, Salah E. Primary cutaneous aggressive epidermotropic CD8(+) T-cell lymphoma: Proposed diagnostic criteria and therapeutic evaluation. J Am Acad Dermatol. 2012;67(4):748–59.
Novelli M, Fierro MT, Quaglino P, Comessatti A, Lisa F, Ponti R, Savoia P, Bernengo MG. Flow cytometry immunophenotyping in mycosis fungoides. J Am Acad Dermatol. 2008;59(3):533–4.
Olsen E, Vonderheid E, Pimpinelli N, Willemze R, Kim Y, Knobler R, Zackheim H, Duvic M, Estrach T, Lamberg S, Wood G, Dummer R, Ranki A, Burg G, Heald P, Pittelkow M, Bernengo MG, Sterry W, Laroche L, Trautinger F, Whittaker S. Revisions to the staging and classification of mycosis fungoides and Sezary syndrome: a proposal of the International Society for Cutaneous Lymphomas (ISCL) and the cutaneous lymphoma task force of the European Organization of Research and Treatment of Cancer (EORTC). Blood. 2007;110(6):1713–22.
Petit T, Cribier B, Bagot M, Wechsler J. Inflammatory vitiligo-like macules that simulate hypopigmented mycosis fungoides. Eur J Dermatol. 2003;13(4):410–2.
Pfaltz K, Kerl K, Palmedo G, Kutzner H, Kempf W. Clonality in sarcoidosis, granuloma annulare, and granulomatous mycosis fungoides. Am J Dermatopathol. 2011;33(7):659–62.
Pileri A, Facchetti F, Rutten A, Zumiani G, Boi S, Fink-Puches R, Cerroni L. Syringotropic mycosis fungoides: a rare variant of the disease with peculiar clinicopathologic features. Am J Surg Pathol. 2011;35(1):100–9.
Pimpinelli N, Olsen EA, Santucci M, Vonderheid E, Haeffner AC, Stevens S, Burg G, Cerroni L, Dreno B, Glusac E, Guitart J, Heald PW, Kempf W, Knobler R, Lessin S, Sander C, Smoller BS, Telang G, Whittaker S, Iwatsuki K, Obitz E, Takigawa M, Turner ML, Wood GS. Defining early mycosis fungoides. J Am Acad Dermatol. 2005;53(6):1053–63.
Pinkus H. Alopecia mucinosa. Additional data in 1983. Arch Dermatol. 1983;119(8):698–9.
Ponti R, Fierro MT, Quaglino P, Lisa B, Paola FC, Michela O, Paolo F, Comessatti A, Novelli M, Bernengo MG. TCRgamma-chain gene rearrangement by PCR-based GeneScan: diagnostic accuracy improvement and clonal heterogeneity analysis in multiple cutaneous T-cell lymphoma samples. J Invest Dermatol. 2008;128(4):1030–8.
Poszepczynska-Guigne E, Schiavon V, D’Incan M, Echchakir H, Musette P, Ortonne N, Boumsell L, Moretta A, Bensussan A, Bagot M. CD158k/KIR3DL2 is a new phenotypic marker of Sezary cells: relevance for the diagnosis and follow-up of Sezary syndrome. J Invest Dermatol. 2004;122(3):820–3.
Raess PW, Bagg A. The role of molecular pathology in the diagnosis of cutaneous lymphomas. Patholog Res Int. 2012;2012:913523.
Requena L, Sanchez YE. Panniculitis. Part II. Mostly lobular panniculitis. J Am Acad Dermatol. 2001;45(3):325–61.
Rezania D, Sagatys E, Glass F, Kadin M, Cualing H. Cutaneous lymphocyte antigen and TRAF-1 are useful in differentiating lymphomatoid papulosis, cutaneous ALCL and systemic ALCL. Am Soc Hematol, Abstracts 50th annual meeting. San Francisco, CA 2008
Rijlaarsdam JU, Scheffer E, Meijer CJ, Willemze R. Cutaneous pseudo-T-cell lymphomas. A clinicopathologic study of 20 patients. Cancer. 1992;69(3):717–24.
Salhany KE, Macon WR, Choi JK, Elenitsas R, Lessin SR, Felgar RE, Wilson DM, Przybylski GK, Lister J, Wasik MA, Swerdlow SH. Subcutaneous panniculitis-like T-cell lymphoma: clinicopathologic, immunophenotypic, and genotypic analysis of alpha/beta and gamma/delta subtypes. Am J Surg Pathol. 1998;22(7):881–93.
Sandberg Y, Heule F, Lam K, Lugtenburg PJ, Wolvers-Tettero IL, van Dongen JJ, Langerak AW. Molecular immunoglobulin/T- cell receptor clonality analysis in cutaneous lymphoproliferations. Experience with the BIOMED-2 standardized polymerase chain reaction protocol. Haematologica. 2003;88(6):659–70.
Sandberg Y, van Gastel-Mol EJ, Verhaaf B, Lam KH, van Dongen JJ, Langerak AW. BIOMED-2 multiplex immunoglobulin/T-cell receptor polymerase chain reaction protocols can reliably replace Southern blot analysis in routine clonality diagnostics. J Mol Diagn. 2005;7(4):495–503.
Sarkany I. Patchy alopecia, anhidrosis, eccrine gland wall hypertrophy and vasculitis. Proc R Soc Med. 1969;62(2):157–9.
Scarabello A, Leinweber B, Ardigo M, Rutten A, Feller AC, Kerl H, Cerroni L. Cutaneous lymphomas with prominent granulomatous reaction: a potential pitfall in the histopathologic diagnosis of cutaneous T- and B-cell lymphomas. Am J Surg Pathol. 2002;26(10):1259–68.
Schiller PI, Flaig MJ, Puchta U, Kind P, Sander CA. Detection of clonal T cells in lichen planus. Arch Dermatol Res. 2000;292(11):568–9.
Schmidt D, Goronzy JJ, Weyand CM. CD4+ CD7-CD28- T cells are expanded in Rheumatoid Arthritis and are characterized by autoreactivity. J Clin Invest. 1996;97(9):2027–37.
Sigurdsson V, Toonstra J, van Vloten WA. Idiopathic erythroderma: a follow-up study of 28 patients. Dermatology. 1997;194(2):98–101.
Sigurdsson V, Steegmans PH, van Vloten WA. The incidence of erythroderma: a survey among all dermatologists in The Netherlands. J Am Acad Dermatol. 2001;45(5):675–8.
Simon M, Flaig MJ, Kind P, Sander CA, Kaudewitz P. Large plaque parapsoriasis: clinical and genotypic correlations. J Cutan Pathol. 2000;27(2):57–60.
Sproul A, Goodlad JR. Clonality Testing of cutaneous lymphoid infiltrates: practicalities, pitfalls and potential uses. J Haematopathol. 2012;5(1):69–82.
Stone ML, Styles AR, Cockerell CJ, Pandya AG. Hypopigmented mycosis fungoides: a report of 7 cases and review of the literature. Cutis. 2001;67(2):133–8.
Swerdlow SJ, Campo E, Harris NL, Jaffe ES, Pileri S, Stein H, Thiele J, Vardiman JW (eds) WHO classification of tumors of haematopoieitic and lymphoid tissues. 4th ed. Geneva, Switzerland: Who Press; 2008.
Tamagawa R, Katoh N, Shimazaki C, Okano A, Yamada S, Ichihashi K, Masuda K, Kishimoto S. Lymphoma with large-plaque parapsoriasis treated with PUVA. Eur J Dermatol. 2005;15(4):265–7.
Tannous Z, Baldassano MF, Li VW, Kvedar J, Duncan LM. Syringolymphoid hyperplasia and follicular mucinosis in a patient with cutaneous T-cell lymphoma. J Am Acad Dermatol. 1999;41(2 Pt 2):303–8.
Tee SI, Martinez-Escaname M, Zuriel D, Fried I, Wolf I, Massone C, et al. Acrodermatitis chronica atrophicans with pseudolymphomatous infiltrates. Am J Dermatopathol. 2013;35(3):338–42. doi: 10.1097/DAD.0b013e31826b7487.
Thein M, Ravat F, Orchard G, Calonje E, Russell-Jones R. Syringotropic cutaneous T-cell lymphoma: an immunophenotypic and genotypic study of five cases. Br J Dermatol. 2004;151(1):216–26.
Thurber SE, Zhang B, Kim YH, Schrijver I, Zehnder J, Kohler S. T-cell clonality analysis in biopsy specimens from two different skin sites shows high specificity in the diagnosis of patients with suggested mycosis fungoides. J Am Acad Dermatol. 2007;57(5):782–90.
Tomasini D, Zampatti C, Palmedo G, Bonfacini V, Sangalli G, Kutzner H. Cytotoxic mycosis fungoides evolving from pityriasis lichenoides chronica in a seventeen-year-old girl. Report of a case. Dermatology. 2002;205(2):176–9.
Vakeva L, Sarna S, Vaalasti A, Pukkala E, Kariniemi AL, Ranki A. A retrospective study of the probability of the evolution of parapsoriasis en plaques into mycosis fungoides. Acta Derm Venereol. 2005;85(4):318–23.
van der Loo EM, Cnossen J, Meijer CJ. Morphological aspects of T cell subpopulations in human blood: characterization of the cerebriform mononuclear cells in healthy individuals. Clin Exp Immunol. 1981;43(3):506–16.
van Dongen JJ, Langerak AW, Bruggemann M, Evans PA, Hummel M, Lavender FL, Delabesse E, Davi F, Schuuring E, Garcia-Sanz R, van Krieken JH, Droese J, Gonzalez D, Bastard C, White HE, Spaargaren M, Gonzalez M, Parreira A, Smith JL, Morgan GJ, Kneba M, Macintyre EA. Design and standardization of PCR primers and protocols for detection of clonal immunoglobulin and T-cell receptor gene recombinations in suspect lymphoproliferations: report of the BIOMED-2 Concerted Action BMH4-CT98-3936. Leukemia. 2003;17(12):2257–317.
van Doorn R, Van Haselen CW, van V, V et al. Mycosis fungoides: disease evolution and prognosis of 309 Dutch patients. Arch Dermatol 2000;136:504–10.
Vonderheid EC. On the diagnosis of erythrodermic cutaneous T-cell lymphoma. J Cutan Pathol. 2006;33 Suppl 1:27–42.
Washington LT, Huh YO, Powers LC, Duvic M, Jones D. A stable aberrant immunophenotype characterizes nearly all cases of cutaneous T-cell lymphoma in blood and can be used to monitor response to therapy. BMC Clin Pathol. 2002;2(1):5.
Wechsler J, Bagot M, Nikolova M, Parolini S, Martin-Garcia N, Boumsell L, Moretta A, Bensussan A. Killer cell immunoglobulin-like receptor expression delineates in situ Sezary syndrome lymphocytes. J Pathol. 2003;199(1):77–83.
Weinberg JM, Kristal L, Chooback L, Honig PJ, Kramer EM, Lessin SR. The clonal nature of pityriasis lichenoides. Arch Dermatol. 2002;138(8):1063–7.
Weiss LM, Wood GS, Ellisen LW, Reynolds TC, Sklar J. Clonal T-cell populations in pityriasis lichenoides et varioliformis acuta (Mucha-Habermann disease). Am J Pathol. 1987;126(3):417–21.
Wenzel J, Gutgemann I, Distelmaier M, Uerlich M, Mikus S, Bieber T, Tuting T. The role of cytotoxic skin-homing CD8+ lymphocytes in cutaneous cytotoxic T-cell lymphoma and pityriasis lichenoides. J Am Acad Dermatol. 2005;53(3):422–7.
Werner B, Brown S, Ackerman AB. “Hypopigmented mycosis fungoides” is not always mycosis fungoides! Am J Dermatopathol. 2005;27(1):56–67.
Whittam LR, Calonje E, Orchard G, Fraser-Andrews EA, Woolford A, Russell-Jones R. CD8-positive juvenile onset mycosis fungoides: an immunohistochemical and genotypic analysis of six cases. Br J Dermatol. 2000;143(6):1199–204.
Winkelmann RK. Panniculitis with cellular phagocytosis. Chronic form of histiocytic panniculitis with fever, pancytopenia, polyserositis and lethal hemorrhagic diathesis. Hautarzt. 1980;31(11):588–94.
Winkelmann RK, Buechner SA, az-Perez JL. Pre-Sezary syndrome. J Am Acad Dermatol. 1984;10(6):992–9.
Wolf IH, Kerl K, Cerroni L, Kerl H. Parapsoriasis lichenoides/parapsoriasis variegata–a new concept. J Dtsch Dermatol Ges. 2009;7(11):993–5.
Wood GS. Analysis of clonality in cutaneous T cell lymphoma and associated diseases. Ann N Y Acad Sci. 2001;941:26–30.
Wood B. 9-color and 10-color flow cytometry in the clinical laboratory. Arch Pathol Lab Med. 2006;130(5):680–90.
Wood GS, Ngan BY, Tung R, Hoffman TE, Abel EA, Hoppe RT, Warnke RA, Cleary ML, Sklar J. Clonal rearrangements of immunoglobulin genes and progression to B cell lymphoma in cutaneous lymphoid hyperplasia. Am J Pathol. 1989;135(1):13–9.
Zhang B, Beck AH, Taube JM, Kohler S, Seo K, Zwerner J, Viakhereva N, Sundram U, Kim YH, Schrijver I, Arber DA, Zehnder JL. Combined use of PCR-based TCRG and TCRB clonality tests on paraffin-embedded skin tissue in the differential diagnosis of mycosis fungoides and inflammatory dermatoses. J Mol Diagn. 2010;12(3):320–7.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer Science+Business Media New York
About this chapter
Cite this chapter
Cualing, H.D., Kadin, M.E. (2014). Role of Molecular Genetics and Flow Cytometry Analysis in Cutaneous Hematopathology Including Application in Ten Disease Categories: Using Molecular and Immunophenotyping Techniques in Evaluation of Hyperplasia, Atypical Infiltrates, and Frank Lymphomas. In: Cualing, H., Kadin, M., Hoang, M., Morgan, M. (eds) Cutaneous Hematopathology. Springer, New York, NY. https://doi.org/10.1007/978-1-4939-0950-6_4
Download citation
DOI: https://doi.org/10.1007/978-1-4939-0950-6_4
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4939-0949-0
Online ISBN: 978-1-4939-0950-6
eBook Packages: MedicineMedicine (R0)