Abstract
Since the discovery of angiogenic vascular endothelial growth factor (VEGF)-A in 1983 and lymphangiogenic VEGF-C in 1997, an increasing amount of knowledge has accumulated on the essential roles of VEGF ligands and receptors in physiological and pathological angiogenesis and lymphangiogenesis. We will review the properties of VEGF ligands and receptors concentrating on their lymphatic vessel effects first in noncardiac tissues and then in normal myocardium and cardiac disease. Tissue adaptation to several stimuli such as hypoxia, pathogen invasion, and inflammation often involves coordinated changes in both blood vessels and lymphatic vessels. As lymphatic vessels are involved in the initiation and resolution of inflammation and regulation of tissue edema, VEGF family members may have important roles in myocardial lymphatics and cardiac disease.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
General Biology of the VEGF Family
VEGF-A (or VEGF) was first discovered as a tumor-secreted factor that induced vascular permeability and was therefore initially named as vascular permeability factor [1]. Subsequently, the VEGF family has expanded to a total of five mammalian ligands: placental growth factor (PlGF), VEGF-A, VEGF-B, VEGF-C, and VEGF-D [2–5].
The receptors for the VEGF family ligands include VEGFR-1, VEGFR-2, VEGFR-3, and neuropilins (NRP-1 and NRP-2). Upon binding of VEGF ligand dimers to their receptors, the corresponding receptors dimerize, phosphorylate tyrosine residues in the cytosol, and activate intracellular signaling pathways. The binding properties of VEGF ligands and the principal effects of VEGF receptors are summarized in Fig. 9.1. Heterodimerization of VEGF ligands and receptors, and splice variants and heparin-binding differences of ligands result in additional complexity and flexibility in VEGF ligand–receptor interactions [5]. Generally, the preferential expression of VEGFR-1 and VEGFR-2 in blood vascular endothelial cells (EC) and VEGFR-3 in lymphatic EC, and the binding properties of VEGF ligands to their corresponding receptors, underlies their angiogenic or lymphangiogenic predilection (Fig. 9.1). We first overview properties of the angiogenic VEGF ligands and receptors, and we then concentrate on the lymphangiogenic VEGF family members.
VEGF ligands and receptors. VEGF ligands have different binding properties to VEGF receptors. VEGFR-1 modulates VEGF responses on endothelial cells and it is a chemotactic signal for monocytes and smooth muscle cells. VEGFR-1 also has a functional role in hematopoiesis, and the soluble sVEGFR-1 inhibits VEGF effects. VEGFR-2 elicits the main mitogenic and proinflammatory effects on vascular endothelial cells but has a functional role also in hematopoietic and vascular progenitor cells. VEGFR-3 signaling principally regulates the development and functionality of lymphatic endothelial cells and migration of antigen-presenting cells. EC endothelial cell; HSC hematopoietic stem cell; NO nitric oxide; PlGF placental growth factor; SMC smooth muscle cell; VEGF vascular endothelial growth factor; VEGFR VEGF receptor; sVEGFR soluble VEGFR (Modified from Nykänen A. Vascular growth factors and progenitor cells in cardiac allograft arteriosclerosis [dissertation]. Helsinki: University of Helsinki; 2007)
Angiogenic VEGF Members (VEGF-A, VEGF-B, PlGF, VEGFR-1, VEGFR-2, NRP)
VEGF-A binds to VEGFR-1, VEGFR-2, NRP-1, and NRP-2 and is the major regulator of the angiogenic switch. VEGF is produced by a variety of adult tissues, and vascular and inflammatory cells, and is induced by hypoxia, inflammation, and several growth factors [6–11]. VEGF-A elicits its effects mainly through VEGFR-2+ vascular endothelial cells (EC) and VEGFR-1+ monocytes and macrophages. VEGF induces EC migration, proliferation, and sprouting and results in angiogenesis. VEGF is essential for embryonic vascular development [12, 13]. The importance of VEGF in angiogenesis in adult is highlighted by the clinical success of anti-VEGF approaches in the treatment of cancer and eye disease [3]. However, the results of randomized clinical trials on VEGF-A-mediated therapeutic angiogenesis have been disappointing [14]. This may at least in part relate to the findings that the VEGF-A-induced new blood vessels are often leaky. VEGF-A is indeed intimately related to inflammation through increased vascular permeability and also through direct effects on VEGFR-1+ monocytes and macrophages [5].
PlGF was first detected in human placenta [15] and it binds to VEGFR-1 and NRP-1 [16]. PlGF is not essential for normal vascular development [3, 17], but it may enhance VEGF effects particularly in pathological conditions [18, 19], and it promotes cardiac hypertrophy [20]. PlGF has a clear inflammatory role as it activates both hematopoietic stem cells [1, 21] and monocytes and macrophages through VEGFR-1 [2, 22–24].
VEGF-B is expressed in skeletal muscle and heart, and also binds to VEGFR-1 and NRP-1 [3, 16, 25, 26]. Lack of VEGF-B does not impair vascular development, but it may yield to conducting defects and size reduction in the heart, and impaired recovery after myocardial ischemia [4, 27, 28]. VEGF-B is also involved in inflammatory angiogenesis [1, 29] and in cardiac arteriogenesis [5, 30] and hypertrophy [5, 31]. VEGF-B also has metabolic effects as it regulates endothelial lipid transfer and metabolism [6–11, 31, 32] as well as the development of diabetes [12, 13, 33].
VEGFR-1 (also known as fms-like tyrosine kinase, Flt-1) is a receptor for VEGF-A, VEGF-B, and PlGF [3, 16]. In addition to the membrane-anchored VEGFR-1, a soluble form of VEGFR-1 (sVEGFR-1) also exists [14, 34, 35]. VEGFR-1 is expressed in a variety of cells including EC, smooth muscle cells, monocytes and macrophages, and hematopoietic stem cells [3, 15–17, 36] and is upregulated by hypoxia-inducible factor-1 [18, 19, 37]. VEGFR-1 has high affinity for VEGF-A but low tyrosine kinase activity, and it has been viewed as a decoy receptor and a negative regulator of VEGFR-2 in ECs [20, 38]. Accordingly, VEGFR-1 deletion results in excessive endothelial progenitor cell proliferation, vascular disorganization, and embryonic lethality [39, 40]. Although the angiogenic effects of VEGFR-1 are subtle, VEGFR-1 may regulate arteriogenesis, pathological angiogenesis, myelomonocyte cell recruitment, and lipid metabolism [31–33, 41, 42].
VEGFR-2 (also known as kinase insert domain receptor, KDR/fetal liver kinase, Flk-1) binds VEGF-A, VEGF-C, and VEGF-D. VEGFR-2 is mainly expressed on vascular EC and is considered responsible for the majority of VEGF-A-induced angiogenic and permeability effects [3, 5]. VEGFR-2 expression is essential for embryonal hematopoiesis and vasculogenesis [43, 44]. In adults, VEGFR-2 expression is usually downregulated and presents only at sites of active angiogenesis such as wound healing, tumors, and after myocardial infarction [45, 46]. In myocardial infarction and sepsis, VEGFR-2 is a major regulator of vascular permeability and cardiac dysfunction [47, 48].
Neuropilin receptors NRP1 and NRP2 are involved in neuronal development and bind semaphorins [16]. Neuropilins also interact with VEGF signaling as NRP1 is a co-receptor for VEGFR-1 and VEGFR-2, and NRP2 for VEGFR-3 [16]. In the vascular system, NRP1 is expressed predominantly in arteries and potentiates the binding and activity of VEGF-A on VEGFR-2 [49]. Interaction of VEGFR-3 and its co-receptor NRP2 modulates the function of veins and lymphatic vessels [50, 51]. NRP1 also participates in lymphatic vessel and valve development through semaphorin interaction [52].
Although the VEGF ligands and receptors described above are considered mainly angiogenic, some overlap on lymphangiogenic effects have been described [53]. The reason for this overlap may be in part the fact that VEGF-A recruits macrophages that may in turn drive lymphangiogenesis [54].
Lymphangiogenic VEGF Members (VEGF-C and VEGF-D, VEGFR-3, NRP)
VEGF-C binds to VEGFR-2 and VEGFR-3 and is a major regulator in the development of lymphatic vasculature [2, 55–57]. VEGF-C is produced as a precursor protein that undergoes proteolytic modification [58]. It is produced in areas of active lymphangiogenesis in the embryo, and the expression is maintained in lung, heart, liver, and kidney in the adult [59]. VEGF-C is not activated by hypoxia, but is increased by serum and its components, platelet-derived growth factor, epidermal growth factor, and transforming growth factor-β [60]. VEGF-C mRNA is also upregulated by proinflammatory cytokines TNF-α, IL-1α, and IL-β [61]. Inflammatory cells such as macrophages, dendritic cells, and CD4+ T lymphocytes are a rich source of VEGF-C [54, 62–65].
Loss of one VEGF-C allele causes prominent lymphatic hypoplasia, whereas loss of both VEGF-C alleles results in embryonic lethality [66]. Similarly, inhibition of VEGF-C/D/R3 signaling in the adult regresses existing lymphatic vessels and results in lymphedema [67]. In contrast, VEGF-C overexpression results in lymphatic hyperplasia [2, 57] and in therapeutic lymphangiogenesis in lymphedema [68]. VEGF-C is upregulated in many cancers and participates in lymphatic metastasis of tumors [69, 70]. Interestingly, salt-induced hypertension is counteracted by macrophage VEGF-C upregulation and tissue lymphangiogenesis [71]. Another noteworthy finding suggests that, in addition to clear lymphatic effects, VEGF-C may also have angiogenic effects through VEGFR-2 binding, by regulating a subtype of vascular EC that express VEGFR-3 [72–74], and also by attracting VEGF-A-producing macrophages [75].
VEGF-C is intimately involved in many inflammatory conditions that involve lymphangiogenesis such as bacterial infection [62], rheumatoid arthritis [76], skin inflammation [77], and organ transplantation [64, 78, 79]. In addition to inducing lymphangiogenesis, VEGF-C modifies lymphatic vessel properties by, for example, upregulating CCL21—a chemokine that attracts CCR7+ tumor cells and dendritic cells [64, 80]. VEGF-C has also direct effects on VEGFR-3+ dendritic cells and induces their migration [81] and maturation [78]. VEGF-C thus modifies immune reactions through direct effects on lymphatic EC and also on macrophages and dendritic cells [64, 78, 81, 82]. In addition to participating in antigen-presenting cell traffic and the initiation of immune responses, VEGF-C-induced lymphangiogenesis may also balance tissue inflammation by promoting lymphatic drainage and the resolution of tissue inflammation [83–85].
Human VEGF-D binds to VEGFR-2 and VEGFR-3, whereas mouse VEGF-D binds only to VEGFR-3 [86]. Like VEGF-C, VEGF-D also undergoes proteolytical modification, is involved in lymphangiogenesis, and has angiogenic properties. In contrast to VEGF-C, VEGF-D is not essential for the development of lymphatic vessels [87]. Adenovirally delivered VEGF-D induces a potent angiogenic and lymphangiogenic response in skeletal muscle and is associated with elevated vascular permeability [88], but the relative effects on angiogenesis and lymphangiogenesis may depend on the tissue used [89]. VEGF-D is involved in the metastatic spread of cancer [90].
VEGFR-3 binds VEGF-C and VEGF-D, and it is a key regulator for lymphatic growth [2, 66]. VEGFR-3 signaling regulates cardiovascular development in embryos [91], but later in development and in adulthood, it more selectively regulates the growth and maintenance of lymphatic vessels [67]. VEGFR-3 may also have angiogenic effects in adults, since VEGFR-3 is expressed in stalk cells [72, 74], and VEGFR-3+ macrophages produce VEGF-A as well [75]. VEGFR-3 is defective in primary lymphedema [92, 93] and is induced in vascular malformations [94]. VEGFR-3 is also upregulated during lymphangiogenesis in cancer, wound healing, and inflammation [95]. Inflammation upregulates lymphatic EC VEGFR-3 expression trough the activation of inflammatory transcription factor NF-κB. This renders the VEGFR-3+ lymphatic ECs responsive to VEGF-C and VEGF-D [96]. In addition to lymphatic EC, VEGFR-3 is also expressed in macrophages and dendritic cells and regulates their migration [63, 81, 97].
Neuropilins are co-receptors for VEGFR-2 and VEGFR-3. NRP2 binds VEGF-C and VEGF-D, and is a co-receptor for VEGFR-3. In addition to its effects on veins, NRP2 also regulates lymphatic vessel sprouting [50, 51] and is upregulated in vascular malformations [94]. The other neuropilin NRP1 is also involved in lymphatic vessel maturation and valve formation, but this involves semaphorin and not VEGF-A [52].
Lymphatic-Specific VEGF Expression and Signaling in the Heart
VEGF Expression and Signaling in Cardiac Lymphatics During Embryogenesis and in Healthy Adult
The developing vasculature of the heart requires a variety of signals, including endothelial growth factors. The details of lymphatic development are very well described, mainly in noncardiac tissues of mouse, but the general features seem to be universal.
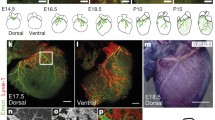
The first LECs differentiate from venous endothelial cells at midgestation, induced by VEGF-C [66, 98]. The LECs are distinguished by expression of specific molecules such as prospero-related homeodomain transcription factor (Prox1), vascular endothelial growth factor receptor-3 (VEGFR-3), the membrane glycoprotein podoplanin, and lymphatic vessel hyaluronan receptor-1 [66, 98, 99]. In mouse, starting from embryonic day (E) 9.5, a complex sequential activation of the transcription factor SOX18, Prox1, and the venous nuclear receptor COUP-TFII initiates the LEC differentiation program in the anterior cardinal vein [66, 98].
The paracrine secretion of VEGF-C is crucial for the further dorsolateral sprouting, migration, and survival of the first LECs and the formation of lymph sacs [66]. The VEGF-C co-receptor neuropilin-2 (NRP-2) and the Eph tyrosine kinase ligand ephrin B2 are required for efficient sprouting of lymphatic capillaries [51, 100]. The Notch1-Dll4 signaling pathway is essential for postnatal lymphatic development [101]. Interestingly, in adult tissues, lymphatic sprouting induced by VEGF-C is not restricted by Notch, whereas VEGF does not promote efficient lymphatic sprouting unless Notch signaling is inhibited [102].
According to the study of endothelial growth factor distribution in the human fetal heart [103], their localizations at different gestational ages are similar. Lymphatic vessels are only detected in the epicardial layer, and they are negative for VEGFR-1 but strongly positive for both VEGFR-2 and VEGFR-3. Very weak VEGFR-3 signals are also observed in some myocardial capillaries but not in the endocardium in 13- to 30-week fetuses. However, the VEGFR-3 expression seems to be downregulated in the blood vessels during the first trimester. Thus, although VEGFR-3 is needed for early cardiovascular development [104], it later serves a more specialized biological function mainly in lymphatic endothelia [103].
Only a few studies have described the pattern of VEGF receptor expression in the lymphatics of healthy adult heart [64, 105, 106]. In a study by Geissler et al. [105], human myocardial biopsies have been used for immunohistochemical stainings of VEGFR-3-positive lymphatics: the density of VEGFR-3-positive vessels was calculated to be around 50 per mm2, and their average diameter was about 3 microns. As described for the healthy adult rat heart, the density of VEGFR-3-positive vessels is generally lower in the myocardium than in the epicardial area. In addition, vessel VEGFR-3 immunoreactivity colocalizes with LYVE-1 expression, although not all LYVE-1-positive vessels express VEGFR-3 [64].
In Heart Transplantation (Allorecognition and Rejection)
In transplantation, the transfer of antigen-presenting cells from vascularized allografts to secondary lymphoid organs—both spleen and lymph nodes—is critical for the priming of alloreactive T cells and the development of alloimmune responses [107, 108]. Lymphatic vessels provide easy access for inflammatory cells and their unilateral movement from peripheral tissues to secondary lymphoid organs. Thus, the lymphatic network forms a link between innate and adaptive immunity, thereby having extraordinary importance in a setting of transplantation.
A descriptive study of human patients undergoing heart transplantation shows that lymphatic endothelial markers undergo significant alterations after the transplantation, suggesting a significant change in lymphatic endothelial phenotype. Furthermore, episodes of acute allograft rejection seem to be associated with a significantly lower density of VEGFR-3-positive lymphatics after heart transplantation [106]. A recent experimental study [64] provides detailed information on lymphatic behavior in rejecting hearts: acute rejection decreases the epicardial lymphatic vessel density and chronic rejection doubles the myocardial lymphatic vessel density. Importantly, lymphangiogenesis in transplanted organs may not be only a secondary effect of chronic inflammation. Instead, lymphatic vessels also appear to have a regulatory role in the initiation of alloimmune reactions. VEGFR-3 inhibition decreases dendritic cell recruitment to the spleen and the development of the subsequent alloimmune response, thus improving cardiac allograft survival. In addition, treatment with neutralizing monoclonal VEGFR-3 antibodies decreases allograft inflammation and the development of arteriosclerosis in a chronic rejection model. According to the study, it appears possible that VEGFR-3 inhibition has direct effects on dendritic cell migration. VEGFR-3 also seems to regulate leukocyte traffic and alloimmunity through direct effects on allograft VEGFR-3-positive lymphatic vessels by upregulating allograft CCL21 production [64]. The range of currently known directions for VEGF-C signaling in a setting of transplantation is represented in Fig. 9.2.
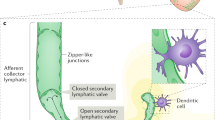
VEGF-C–VEGFR-3 signaling in a setting of transplantation. VEGF-C modifies lymphatic vessel properties by upregulating CCL21—a chemokine that attracts CCR7+ dendritic cells. VEGF-C also has direct effects on VEGFR-3+ dendritic cells and induces their maturation and unilateral migration through the lymphatic network to secondary lymphoid organs. Thus, VEGF-C plays an important role in the initiation of direct alloimmune recognition through direct effects on lymphatic endothelial cells and antigen-presenting cells. VEGF-C may also have angiogenic effects through VEGFR-2 binding; its role in transplantation remains unclear. BEC blood endothelial cell; CCL-21 chemokine ligand 21; LEC lymphatic endothelial cell; CCR-7 C-C chemokine receptor type 7; DC dendritic cell; MHC II major histocompatibility complex class II; VEGFR-2 VEGF receptor 2; VEGFR-3 VEGF receptor 3; TCR T cell receptor
Thus, VEGF-C/VEGFR-3 signaling seems to have important effects on proximal events in cardiac allograft alloimmunity and arteriosclerosis. Therefore, VEGFR-3 inhibition could be used as a novel lymphatic vessel-targeted immunomodulatory therapy to regulate alloimmune activation after solid organ transplantation. Further studies that particularly describe the mechanistic role of lymphatic vessel activation in the ischemia-reperfusion injury and allograft rejection are needed.
In Myocardial Infarction
In the human heart, myocardial remodeling after myocardial infarction (MI) results in scar formation through several sequential stages of myocardial necrosis, granulation, and fibrosis [109]. The viable cardiomyocytes around the lesion express cytoprotective proteins and cytokines which facilitate the healing of the affected lesion [110, 111]. VEGF is critical for angiogenesis in the healing area [112]: it is promptly expressed in the surviving cardiomyocytes around the infracted lesion after the onset of MI, and angiogenesis in the lesion begins at 4–5 h and continues up to day 90 [110].
A study by Ishikawa et al. [113] demonstrates that lymphatic vessels are not detected in stages with coagulation necrosis, but a few lymphatics first appear in the peripheral region adjacent to viable myocytes in the early granulation period. Lymphatic density subsequently increases in the mature granulation period and is thereafter maintained during scar formation. After the onset of myocardial infarction, lymphangiogenesis lags behind blood vessel angiogenesis, whereas VEGF-C is expressed in the cardiomyocytes around the lesion at all stages of myocardial remodeling. The results of this study suggest that during the entire process of myocardial infarction healing, blood vessels supply the blood and nutrients mainly during the granulation period, but lymphatics participate mainly in fibrosis maturation and scar formation through the drainage of excessive proteins and fluid, probably mediated by VEGF-C.
In Atherosclerosis and Degenerative Valve Disease
Recently there has been an emerging body of evidence linking lymphangiogenesis to atherosclerosis. Lymphatic vessels are found at sites of atherosclerosis, which is associated with inflammation and lipid accumulation in arterial walls [114, 115]. Arterial smooth muscle cells constitutively produce lymphangiogenic factors, and lymphatic vessels are present in the adventitia of arteries adjacent to small blood vessels, called the vasa vasorum, which are expanded in atherosclerotic plaques [116, 117]. However, according to the study of Nakano et al. [117], impaired lymphangiogenesis may contribute to plaque progression. Here, VEGF-A and VEGF-C might synergistically contribute to angiogenesis in coronary atherosclerotic plaques. So, in atherosclerotic lesions, the imbalance of angiogenesis and lymphangiogenesis in favor of angiogenesis seems to contribute to sustained inflammatory reactions during human coronary atherogenesis.
In atherosclerosis, lymphatic vessels might have an important role in the efflux of interstitial fluids, fats, and inflammatory cells from the wall of the coronary artery, slowing down the development of atherosclerotic lesions. It remains to be investigated whether therapeutic targeting of lymphangiogenesis might reveal an antiatherosclerotic tool.
Aortic valve stenosis (AS) is another degenerative disease of the heart, where the pathogenesis is linked to lymphangiogenic factors. Pathological features of AS are calcification [118], extracellular matrix remodeling, and valvular accumulation of lipids and inflammatory cells [119]. In contrast to normal avascular aortic valves, stenotic aortic valves are vascularized [120]. Importantly, neovessels may contribute to the progression of AS by facilitating the entry of inflammatory cells and lipids into the leaflets [121]. The study of Syväranta et al. [122] demonstrates that lymphangiogenesis is a part of the pathogenesis of AS and shows that myofibroblasts and endothelial cells are responsible for the valvular production of lymphangiogenic growth factors VEGF-C and VEGF-D. Furthermore, mast-cell-derived compounds degrade VEGF-C, suggesting their anti-lymphangiogenic potential. Similar to atherosclerotic lesions, in AS, the balance between angiogenesis and lymphangiogenesis may disadvantageously favor the accumulation of inflammatory cells and lipids into the lesions, thus possibly leading to disease progression.
In Heart Failure
The two most frequent causes of terminal heart failure are dilated (DCM) and ischemic (ICM) cardiomyopathy. The investigation of microvascular structures in cardiac remodeling has mostly been limited to the sequela of myocardial ischemia and infarction rather than in terminal heart failure. Nevertheless, the role of lymphatic system in the failing myocardium might be of increased importance, since the hemodynamics, fluid, and pressure balance are severely damaged. However, there are barely any publications available about lymphatics in the failing heart, except for several descriptional reports.
The study of Aharinejad et al. [123] provides evidence that VEGF-C mRNA levels are upregulated in both forms of cardiomyopathy and that after cardiac transplantation, these mRNA levels returned to the baseline level of nonfailing cardiac tissues in DCM or decreased even below the baseline level in ICM. A further study [124] describes the distribution of several lymphatic and blood markers, including VEGFRs, in DCM and ICM, comparing them to nonfailing hearts.
Whether any therapeutic manipulation of lymphatic function could improve impaired myocardial function by draining the failing myocardium remains so far an exciting speculation.
In Inflammation
In adulthood, lymphangiogenesis and elevated VEGFR-3 expression coincide with various inflammatory conditions including cancer [125], wound healing [126], and chronic inflammatory diseases. Increased lymphatic vessel density has been documented in chronic airway infection [62], psoriasis [127], and arthritis [76]. VEGF-C and VEGF-D are elevated during inflammation, being produced by a variety of cells residing at inflamed sites, including macrophages [62, 128, 129], dendritic cells and neutrophils [62], mast cells and fibroblasts [130], and tumor cells [129].
Generally, the role of lymphatic activation and lymphangiogenesis in inflammatory settings is considered to be positive. It facilitates the resolution of tissue edema and enhances immune responses by promoting macrophage and dendritic cell mobilization [56, 62]. The lymphatic vascular system and the molecular pathways regulating inflammatory responses are intimately associated. Lymphatic vessels react to tissue inflammation with morphological changes in lymphatic endothelial cell phenotype (such as overexpression of adhesion molecules [131] or VEGFR-3 [96]), induction of proinflammatory cytokines production, as well as chronologically delayed increase of lymphatic vessel density (lymphangiogenesis) [96].
LECs at least in some tissues constitutively express NF-κB [132]. Activation of the NF-κB pathway in LECs upregulates Prox1 and VEGFR-3, which renders the lymphatic vessels more sensitive to VEGF-C and VEGF-D produced by leukocytes [96]. VEGFR-3 signaling is activated upon binding of vascular endothelial growth factor-C (VEGF-C) or the related factor, VEGF-D [133]. NF-κB is activated, for example, downstream of Toll-like receptor 4 binding to lipopolysaccharide in the LECs, thus inducing the activation and production of leukocyte chemoattractants such as CCL2, CCL5, and CX3CL1, which in turn promotes leukocyte homing to the lymphatic vessels and eventually to the draining lymph node [134].
Inflamed lymphatic endothelium promotes the exit of leukocytes from tissue to afferent lymph through newly induced expression of the adhesion molecules ICAM-1 and VCAM-1, which were previously thought to be specific for blood vessel transmigration [131].
Furthermore, the studies of anatomical distribution for the cardiac lymphatics in diseased heart demonstrate increased lymphatic densities in infective endocarditis, myocarditis, and progressive atherosclerosis. Thus, lymphatic growth accompanies chronic inflammation, tissue degeneration, infarction, calcification, and formation of connective tissue [115]. Although not investigated yet for these disease states, the role of lymphatic-specific VEGF signaling seems to be crucial and warrants further analysis and a search for potential therapeutic targeting. The properties of lymphatic-specific VEGF expression and signaling in the heart are briefly summarized in Table 9.1.
Summary
While the critical role of angiogenic VEGF family members in cardiovascular development and disease is already appreciated, the involvement of lymphangiogenic VEGF ligands and receptors, and cardiac lymphatics, in cardiac physiology and pathology is only starting to unfold. With the rapid development of lymphatic vessel markers, better understanding of basic lymphatic vessel biology, and the use of novel genetic and pharmacological tools to activate or inhibit lymphangiogenic VEGF-C/D/R3 signaling, future studies may reveal novel lymphatic-targeted therapeutic strategies in ischemic, degenerative, and inflammatory heart disease.
References
Senger DR, Galli SJ, Dvorak AM, Perruzzi CA, Harvey VS, Dvorak HF (1983) Tumor cells secrete a vascular permeability factor that promotes accumulation of ascites fluid. Science 219:983–985
Jeltsch M, Kaipainen A, Joukov V, Meng X, Lakso M, Rauvala H, Swartz M, Fukumura D, Jain RK, Alitalo K (1997) Hyperplasia of lymphatic vessels in VEGF-C transgenic mice. Science 276:1423–1425
Carmeliet P, Jain RK (2011) Molecular mechanisms and clinical applications of angiogenesis. Nature 473:298–307
Alitalo A, Detmar M (2012) Interaction of tumor cells and lymphatic vessels in cancer progression. Oncogene 31:4499–4508
Koch S, Claesson-Welsh L (2012) Signal transduction by vascular endothelial growth factor receptors. Cold Spring Harb Perspect Med 2:a006502
Berse B, Brown LF, Van de Water L, Dvorak HF, Senger DR (1992) Vascular permeability factor (vascular endothelial growth factor) gene is expressed differentially in normal tissues, macrophages, and tumors. Mol Biol Cell 3:211–220
Ferrara N, Winer J, Burton T (1990) Aortic smooth muscle cells express and secrete vascular endothelial growth factor. Growth Factors 5:141–148
Freeman MR, Schneck FX, Gagnon ML, Corless C, Soker S, Niknejad K et al (1995) Peripheral blood T lymphocytes and lymphocytes infiltrating human cancers express vascular endothelial growth factor: a potential role for T cells in angiogenesis. Cancer Res 55:4140–4145
McCourt M, Wang JH, Sookhai S, Redmond HP (1999) Proinflammatory mediators stimulate neutrophil-directed angiogenesis. Arch Surg 134:1325–1331
Melter M, Reinders ME, Sho M, Pal S, Geehan C, Denton MD et al (2000) Ligation of CD40 induces the expression of vascular endothelial growth factor by endothelial cells and monocytes and promotes angiogenesis in vivo. Blood 96:3801–3808
Tomizawa S, Maruyama K, Nagasawa N, Suzuki S, Kuroume T (1984) Studies of vascular permeability factor derived from T lymphocytes and inhibitory effect of plasma on its production in minimal change nephrotic syndrome. Nephron 41:157–160
Carmeliet P, Ferreira V, Breier G, Pollefeyt S, Kieckens L, Gertsenstein M et al (1996) Abnormal blood vessel development and lethality in embryos lacking a single VEGF allele. Nature 380:435–439
Ferrara N, Carver-Moore K, Chen H, Dowd M, Lu L, O'Shea KS et al (1996) Heterozygous embryonic lethality induced by targeted inactivation of the VEGF gene. Nature 380:439–442
Giacca M, Zacchigna S (2012) VEGF gene therapy: therapeutic angiogenesis in the clinic and beyond. Gene Ther 19:622–629
Maglione D, Guerriero V, Viglietto GG, Delli-Bovi PP, Persico MGM (1991) Isolation of a human placenta cDNA coding for a protein related to the vascular permeability factor. Proc Natl Acad Sci USA 88:9267–9271
Koch S (2012) Neuropilin signalling in angiogenesis. Biochem Soc Trans 40:20–25
Gigante B, Tarsitano M, Cimini V, De Falco S, Persico MG (2003) Placenta growth factor is not required for exercise-induced angiogenesis. Angiogenesis 7:277–284
Carmeliet P, Moons L, Luttun A, Vincenti V, Compernolle V, De Mol M et al (2001) Synergism between vascular endothelial growth factor and placental growth factor contributes to angiogenesis and plasma extravasation in pathological conditions. Nat Med 7:575–583
Park JE, Chen HH, Winer J, Houck KA, Ferrara N (1994) Placenta growth factor. Potentiation of vascular endothelial growth factor bioactivity, in vitro and in vivo, and high affinity binding to Flt-1 but not to Flk-1/KDR. J Biol Chem 269:25646–25654
Accornero F, van Berlo JH, Benard MJ, Lorenz JN, Carmeliet P, Molkentin JD (2011) Placental growth factor regulates cardiac adaptation and hypertrophy through a paracrine mechanism. Circ Res 109:272–280
Rafii S, Avecilla S, Shmelkov S, Shido K, Tejada R, Moore MAS et al (2003) Angiogenic factors reconstitute hematopoiesis by recruiting stem cells from bone marrow microenvironment. Ann N Y Academy Sci 996:49–60
Adini A, Kornaga T, Firoozbakht F, Benjamin LE (2002) Placental growth factor is a survival factor for tumor endothelial cells and macrophages. Cancer Res 62:2749–2752
Barleon B, Sozzani S, Zhou D, Weich HA, Mantovani A, Marmé D (1996) Migration of human monocytes in response to vascular endothelial growth factor (VEGF) is mediated via the VEGF receptor flt-1. Blood 87:3336–3343
Clauss M, Weich H, Breier G, Knies U, Röckl W, Waltenberger J et al (1996) The vascular endothelial growth factor receptor Flt-1 mediates biological activities: implications for a functional role of placenta growth factor in monocyte activation and chemotaxis. J Biol Chem 271:17629–17634
Olofsson B, Pajusola K, von Euler G, Chilov D, Alitalo K, Eriksson U (1996) Genomic organization of the mouse and human genes for vascular endothelial growth factor B (VEGF-B) and characterization of a second splice isoform. J Biol Chem 271:19310–19317
Olofsson B, Pajusola K, Kaipainen A, von Euler G, Joukov V, Saksela O et al (1996) Vascular endothelial growth factor B, a novel growth factor for endothelial cells. Proc Natl Acad Sci USA 93:2576–2581
Aase K, von Euler G, Li X, Pontén A, Thorén P, Cao R et al (2001) Vascular endothelial growth factor-B-deficient mice display an atrial conduction defect. Circulation 104:358–364
Bellomo D, Headrick JP, Silins GU, Paterson CA, Thomas PS, Gartside M et al (2000) Mice lacking the vascular endothelial growth factor-B gene (Vegfb) have smaller hearts, dysfunctional coronary vasculature, and impaired recovery from cardiac ischemia. Circ Res 86:29–35
Mould AW, Tonks ID, Cahill MM, Pettit AR, Thomas R, Hayward NK et al (2003) Vegfb gene knockout mice display reduced pathology and synovial angiogenesis in both antigen-induced and collagen-induced models of arthritis. Arthritis Rheum 48:2660–2669
Bry M, Kivelä R, Holopainen T, Anisimov A, Tammela T, Soronen J et al (2010) Vascular endothelial growth factor-B acts as a coronary growth factor in transgenic rats without inducing angiogenesis, vascular leak, or inflammation. Circulation 122:1725–1733
Kärpänen T, Bry M, Ollila HM, Seppänen-Laakso T, Liimatta E, Leskinen H et al (2008) Overexpression of vascular endothelial growth factor-B in mouse heart alters cardiac lipid metabolism and induces myocardial hypertrophy. Circ Res 103:1018–1026
Hagberg CE, Falkevall A, Wang X, Larsson E, Huusko J, Nilsson I et al (2010) Vascular endothelial growth factor B controls endothelial fatty acid uptake. Nature 464:917–921
Hagberg CE, Mehlem A, Falkevall A, Muhl L, Fam BC, Ortsäter H et al (2012) Targeting VEGF-B as a novel treatment for insulin resistance and type 2 diabetes. Nature 490:426–430
Ambati BK, Nozaki M, Singh N, Takeda A, Jani PD, Suthar T et al (2006) Corneal avascularity is due to soluble VEGF receptor-1. Nature 443:993–997
Kendall RL, Thomas KA (1993) Inhibition of vascular endothelial cell growth factor activity by an endogenously encoded soluble receptor. Proc Natl Acad Sci USA 90:10705–10709
Couper LL, Bryant SR, Eldrup-Jørgensen J, Bredenberg CE, Lindner V (1997) Vascular endothelial growth factor increases the mitogenic response to fibroblast growth factor-2 in vascular smooth muscle cells in vivo via expression of fms-like tyrosine kinase-1. Circ Res 81:932–939
Gerber HP, Condorelli F, Park J, Ferrara N (1997) Differential transcriptional regulation of the two vascular endothelial growth factor receptor genes. Flt-1, but not Flk-1/KDR, is up-regulated by hypoxia. J Biol Chem 272:23659–23667
Hiratsuka S, Minowa O, Kuno J, Noda T, Shibuya M (1998) Flt-1 lacking the tyrosine kinase domain is sufficient for normal development and angiogenesis in mice. Proc Natl Acad Sci USA 95:9349–9354
Fong GH, Rossant J, Gertsenstein M, Breitman ML (1995) Role of the Flt-1 receptor tyrosine kinase in regulating the assembly of vascular endothelium. Nature 376:66–70
Fong GH, Zhang L, Bryce DM, Peng J (1999) Increased hemangioblast commitment, not vascular disorganization, is the primary defect in flt-1 knock-out mice. Development 126:3015–3025
Luttun A, Tjwa M, Moons L, Wu Y, Angelillo-Scherrer A, Liao F et al (2002) Revascularization of ischemic tissues by PlGF treatment, and inhibition of tumor angiogenesis, arthritis and atherosclerosis by anti-Flt1. Nat Med 8:831–840
Pipp F, Heil M, Issbrücker K, Ziegelhoeffer T, Martin S, van den Heuvel J et al (2003) VEGFR-1-selective VEGF homologue PlGF is arteriogenic: evidence for a monocyte-mediated mechanism. Circ Res 92:378–385
Kaipainen A, Korhonen J, Pajusola K, Aprelikova O, Persico MG, Terman BI et al (1993) The related FLT4, FLT1, and KDR receptor tyrosine kinases show distinct expression patterns in human fetal endothelial cells. J Exp Med 178:2077–2088
Shalaby F, Rossant J, Yamaguchi TP, Gertsenstein M, Wu XF, Breitman ML et al (1995) Failure of blood-island formation and vasculogenesis in Flk-1-deficient mice. Nature 376:62–66
Li J, Brown LF, Hibberd MG, Grossman JD, Morgan JP, Simons M (1996) VEGF, flk-1, and flt-1 expression in a rat myocardial infarction model of angiogenesis. Am J Physiol 270:H1803–H1811
Shibuya M (1994) Role of VEGF-flt receptor system in normal and tumor angiogenesis. Adv Cancer Res 67:281–316
Weis S, Shintani S, Weber A, Kirchmair R, Wood M, Cravens A et al (2004) Src blockade stabilizes a Flk/cadherin complex, reducing edema and tissue injury following myocardial infarction. J Clin Invest 113:885–894
Yano K, Liaw PC, Mullington JM, Shih S-C, Okada H, Bodyak N et al (2006) Vascular endothelial growth factor is an important determinant of sepsis morbidity and mortality. J Exp Med 203:1447–1458
Soker S, Takashima S, Miao HQ, Neufeld G, Klagsbrun M (1998) Neuropilin-1 is expressed by endothelial and tumor cells as an isoform-specific receptor for vascular endothelial growth factor. Cell 92:735–745
Kärpänen T, Heckman CA, Keskitalo S, Jeltsch M, Ollila H, Neufeld G et al (2006) Functional interaction of VEGF-C and VEGF-D with neuropilin receptors. FASEB J 20:1462–1472
Xu Y, Yuan L, Mak J, Pardanaud L, Caunt M, Kasman I et al (2010) Neuropilin-2 mediates VEGF-C-induced lymphatic sprouting together with VEGFR3. J Cell Biol 188:115–130
Jurisic G, Hajjami HM, Karaman S, Ochsenbein AM, Alitalo A, Siddiqui SS et al (2012) An unexpected role of semaphorin3a-neuropilin-1 signaling in lymphatic vessel maturation and valve formation. Circ Res 111:426–436
Nagy JA, Vasile E, Feng D, Sundberg C, Brown LF, Detmar MJ et al (2002) Vascular permeability factor/vascular endothelial growth factor induces lymphangiogenesis as well as angiogenesis. J Exp Med 196:1497–1506
Cursiefen C, Chen L, Borges LP, Jackson D, Cao J, Radziejewski C et al (2004) VEGF-A stimulates lymphangiogenesis and hemangiogenesis in inflammatory neovascularization via macrophage recruitment. J Clin Invest 113:1040–1050
Alitalo K (2011) The lymphatic vasculature in disease. Nat Med 17:1371–1380
Kim H, Kataru RP, Koh GY (2012) Regulation and implications of inflammatory lymphangiogenesis. Trends Immunol 33:350–356
Oh SJ, Jeltsch MM, Birkenhäger R, McCarthy JE, Weich HA, Christ B et al (1997) VEGF and VEGF-C: specific induction of angiogenesis and lymphangiogenesis in the differentiated avian chorioallantoic membrane. Dev Biol 188:14–24
Joukov V, Pajusola K, Kaipainen A, Chilov D, Lahtinen I, Kukk E et al (1996) A novel vascular endothelial growth factor, VEGF-C, is a ligand for the Flt4 (VEGFR-3) and KDR (VEGFR-2) receptor tyrosine kinases. EMBO J 15:290–298
Kukk E, Lymboussaki A, Taira S, Kaipainen A, Jeltsch M, Joukov V et al (1996) VEGF-C receptor binding and pattern of expression with VEGFR-3 suggests a role in lymphatic vascular development. Development 122:3829–3837
Enholm B, Paavonen K, Ristimäki A, Kumar V, Gunji Y, Klefstrom J et al (1997) Comparison of VEGF, VEGF-B, VEGF-C and Ang-1 mRNA regulation by serum, growth factors, oncoproteins and hypoxia. Oncogene 14:2475–2483
Ristimäki A, Narko K, Enholm B, Joukov V, Alitalo K (1998) Proinflammatory cytokines regulate expression of the lymphatic endothelial mitogen vascular endothelial growth factor-C. J Biol Chem 273:8413–8418
Baluk P, Tammela T, Ator E, Lyubynska N, Achen MG, Hicklin DJ et al (2005) Pathogenesis of persistent lymphatic vessel hyperplasia in chronic airway inflammation. J Clin Invest 115:247–257
Hamrah P, Chen L, Zhang Q, Dana MR (2003) Novel expression of vascular endothelial growth Ffctor receptor (VEGFR)-3 and VEGF-C on corneal dendritic cells. Am J Pathol 163:12–22
Nykanen AI, Sandelin H, Krebs R, Keränen MAI, Tuuminen R, Kärpänen T et al (2010) Targeting lymphatic vessel activation and CCL21 production by vascular endothelial growth factor receptor-3 inhibition has novel immunomodulatory and antiarteriosclerotic effects in cardiac allografts. Circulation 121:1413–1422
Schoppmann SF, Birner P, Stöckl J, Kalt R, Ullrich R, Caucig C et al (2002) Tumor-associated macrophages express lymphatic endothelial growth factors and are related to peritumoral lymphangiogenesis. Am J Pathol 161(3):947–956
Karkkainen MJ, Haiko P, Sainio K, Partanen J, Taipale J, Petrova TV et al (2004) Vascular endothelial growth factor C is required for sprouting of the first lymphatic vessels from embryonic veins. Nat Immunol 5:74–80
Makinen T, Jussila L, Veikkola T, Karpanen T, Kettunen MI, Pulkkanen KJ et al (2001) Inhibition of lymphangiogenesis with resulting lymphedema in transgenic mice expressing soluble VEGF receptor-3. Nat Med 7:199–205
Szuba A, Skobe M, Karkkainen MJ, Shin WS, Beynet DP, Rockson NB et al (2002) Therapeutic lymphangiogenesis with human recombinant VEGF-C. FASEB J 16:1985–1987
Mandriota SJ, Jussila L, Jeltsch M, Compagni A, Baetens D, Prevo R et al (2001) Vascular endothelial growth factor-C-mediated lymphangiogenesis promotes tumour metastasis. EMBO J 20:672–682
Skobe M, Hawighorst T, Jackson DG, Prevo R, Janes L, Velasco P et al (2001) Induction of tumor lymphangiogenesis by VEGF-C promotes breast cancer metastasis. Nat Med 7:192–198
Machnik A, Neuhofer W, Jantsch J, Dahlmann A, Tammela T, Machura K et al (2009) Macrophages regulate salt-dependent volume and blood pressure by a vascular endothelial growth factor-C-dependent buffering mechanism. Nat Med 15:545–552
Benedito R, Rocha SF, Woeste M, Zamykal M, Radtke F, Casanovas O et al (2012) Notch-dependent VEGFR3 upregulation allows angiogenesis without VEGF-VEGFR2 signalling. Nature 484(7392):110–114
Saaristo A, Veikkola T, Enholm B, Hytönen M, Arola J, Pajusola K et al (2002) Adenoviral VEGF-C overexpression induces blood vessel enlargement, tortuosity, and leakiness but no sprouting angiogenesis in the skin or mucous membranes. FASEB J 16:1041–1049
Tammela T, Zarkada G, Nurmi H, Jakobsson L, Heinolainen K, Tvorogov D et al (2011) VEGFR-3 controls tip to stalk conversion at vessel fusion sites by reinforcing Notch signalling. Nat Cell Biol 13:1202–1213
Chung ES, Chauhan SK, Jin Y, Nakao S, Hafezi-Moghadam A, Van Rooijen N et al (2009) Contribution of macrophages to angiogenesis induced by vascular endothelial growth factor receptor-3-specific ligands. Am J Pathol 175:9–19
Zhang Q, Lu Y, Proulx ST, Guo R, Yao Z, Schwarz EM et al (2007) Increased lymphangiogenesis in joints of mice with inflammatory arthritis. Arthritis Res Ther 9:118
Shi VY, Bao L, Chan LS (2012) Inflammation-driven dermal lymphangiogenesis in atopic dermatitis is associated with CD11b+ macrophage recruitment and VEGF-C up-regulation in the IL-4-transgenic mouse model. Microcirculation 19:567–579
Hajrasouliha AR, Funaki T, Sadrai Z, Hattori T, Chauhan SK, Dana R (2012) Vascular endothelial growth factor-C promotes alloimmunity by amplifying antigen presenting cell maturation and lymphangiogenesis. Invest Ophthalmol Vis Sci 53(3):1244–1250
Krebs R, Tikkanen JM, Ropponen JO, Jeltsch M, Jokinen JJ, Herttuala SY et al (2012) Critical role of VEGF-C/VEGFR-3 signaling in innate and adaptive immune responses in experimental obliterative bronchiolitis. Am J Pathol 181:1607–1620
Issa A, Le TX, Shoushtari AN, Shields JD, Swartz MA (2008) Vascular endothelial growth factor-C and C-C chemokine receptor 7 in tumor cell-lymphatic cross-talk promote invasive phenotype. Cancer Res 69:349–357
Chen L, Hamrah P, Cursiefen C, Zhang Q, Pytowski B, Streilein JW et al (2004) Vascular endothelial growth factor receptor-3 mediates induction of corneal alloimmunity. Nat Med 10:813–815
Skobe M, Hamberg LM, Hawighorst T, Schirner M, Wolf GL, Alitalo K et al (2001) Concurrent induction of lymphangiogenesis, angiogenesis, and macrophage recruitment by vascular endothelial growth factor-C in melanoma. Am J Pathol 159:893–903
Huggenberger R, Siddiqui SS, Brander D, Ullmann S, Zimmermann K, Antsiferova M et al (2011) An important role of lymphatic vessel activation in limiting acute inflammation. Blood 117:4667–4678
Huggenberger R, Ullmann S, Proulx ST, Pytowski B, Alitalo K, Detmar M (2010) Stimulation of lymphangiogenesis via VEGFR-3 inhibits chronic skin inflammation. J Exp Med 207:2255–2269
Zhou Q, Guo R, Wood R, Boyce BF, Liang Q, Wang YJ et al (2011) Vascular endothelial growth factor C attenuates joint damage in chronic inflammatory arthritis by accelerating local lymphatic drainage in mice. Arthritis Rheum 63:2318–2328
Baldwin ME, Catimel B, Nice EC, Roufail S, Hall NE, Stenvers KL et al (2001) The specificity of receptor binding by vascular endothelial growth factor-d is different in mouse and man. J Biol Chem 276:19166–19171
Baldwin ME, Halford MM, Roufail S, Williams RA, Hibbs ML, Grail D et al (2005) Vascular endothelial growth factor D is dispensable for development of the lymphatic system. Mol Cell Biol 25:2441–2449
Rissanen TT, Markkanen JE, Gruchala M, Heikura T, Puranen A, Kettunen MI et al (2003) VEGF-D is the strongest angiogenic and lymphangiogenic effector among VEGFs delivered into skeletal muscle via adenoviruses. Circ Res 92:1098–1106
Byzova TV, Goldman CK, Jankau J, Chen J, Cabrera G, Achen MG et al (2002) Adenovirus encoding vascular endothelial growth factor-D induces tissue-specific vascular patterns in vivo. Blood 99:4434–4442
Stacker SA, Caesar C, Baldwin ME, Thornton GE, Williams RA, Prevo R et al (2001) VEGF-D promotes the metastatic spread of tumor cells via the lymphatics. Nat Med 7:186–191
Dumont DJ, Jussila L, Taipale J, Lymboussaki A, Mustonen T, Pajusola K et al (1998) Cardiovascular failure in mouse embryos deficient in VEGF receptor-3. Science 282:946–949
Irrthum A, Karkkainen MJ, Devriendt K, Alitalo K, Vikkula M (2000) Congenital hereditary lymphedema caused by a mutation that inactivates VEGFR3 tyrosine kinase. Am J Hum Genet 67:7–17
Karkkainen MJ, Ferrell RE, Lawrence EC, Kimak MA, Levinson KL, McTigue MA et al (2000) Missense mutations interfere with VEGFR-3 signalling in primary lymphoedema. Nat Genet 25:153–159
Partanen TA, Vuola P, Jauhiainen S, Lohi J, Salminen P, Pitkäranta A et al (2013) Neuropilin-2 and vascular endothelial growth factor receptor-3 are up-regulated in human vascular malformations. Angiogenesis 16(1):137–46
Martínez-Corral I, Olmeda D, Diéguez-Hurtado R, Tammela T, Alitalo K, Ortega S (2012) In vivo imaging of lymphatic vessels in development, wound healing, inflammation, and tumor metastasis. Proc Natl Acad Sci USA 109:6223–6228
Flister MJ, Wilber A, Hall KL, Iwata C, Miyazono K, Nisato RE et al (2010) Inflammation induces lymphangiogenesis through up-regulation of VEGFR-3 mediated by NF-kappaB and Prox1. Blood 115:418–429
Maruyama K, Ii M, Cursiefen C, Jackson DG, Keino H, Tomita M et al (2005) Inflammation-induced lymphangiogenesis in the cornea arises from CD11b-positive macrophages. J Clin Invest 115:2363–2372
Wigle JT, Oliver G (1999) Prox1 function is required for the development of the murine lymphatic system. Cell 98:769–778
Albrecht I, Christofori G (2011) Molecular mechanisms of lymphangiogenesis in development and cancer. Int J Dev Biol 55:483–494
Mäkinen T, Adams RH, Bailey J, Lu Q, Ziemiecki A, Alitalo K et al (2005) PDZ interaction site in ephrinB2 is required for the remodeling of lymphatic vasculature. Genes Dev 19:397–410
Niessen K, Zhang G, Ridgway JB, Chen H, Kolumam G, Siebel CW et al (2011) The Notch1-Dll4 signaling pathway regulates mouse postnatal lymphatic development. Blood 118:1989–1997
Zheng W, Tammela T, Yamamoto M, Anisimov A, Holopainen T, Kaijalainen S et al (2011) Notch restricts lymphatic vessel sprouting induced by vascular endothelial growth factor. Blood 118:1154–1162
Partanen TA, Mäkinen T, Arola J, Suda T, Weich HA, Alitalo K (1999) Endothelial growth factor receptors in human fetal heart. Circulation 100:583–586
Dumont DJ, Jussila L, Taipale J, Lymboussaki A, Mustonen T, Pajusola K et al (1998) Cardiovascular failure in mouse embryos deficient in VEGF receptor-3. Science 282:946–949
Geissler HJ, Bloch W, Förster SF, Mehlhorn U, Krahwinkel A, Kroener A et al (2003) Morphology and density of initial lymphatics in human myocardium determined by immunohistochemistry. Thorac Cardiovasc Surg 51:244–248
Geissler HJ, Dashkevich A, Fischer UM, Fries JWU, Kuhn-Régnier F, Addicks K et al (2006) First year changes of myocardial lymphatic endothelial markers in heart transplant recipients. Eur J Cardiothorac Surg 29:767–771
Lakkis FG, Arakelov A, Konieczny BT, Inoue Y (2000) Immunologic “ignorance” of vascularized organ transplants in the absence of secondary lymphoid tissue. Nat Med 6:686–688
Larsen CP, Morris PJ, Austyn JM (1990) Migration of dendritic leukocytes from cardiac allografts into host spleens. A novel pathway for initiation of rejection. J Exp Med 171:307–314
Lodge-Patch I (1951) The ageing of cardiac infarcts, and its influence on cardiac rupture. Br Heart J 13:37–42
Ishikawa Y, Akasaka Y, Ishii T, Itoh K, Masuda T, Zhang L et al (2000) Sequential changes in localization of repair-related proteins (heat shock protein 70, ubiquitin and vascular endothelial growth factor) in the different stages of myocardial infarction. Histopathology 37:546–554
Ishikawa Y, Komiyama K, Masuda S, Murakami M, Akasaka Y, Ito K et al (2005) Expression of type V secretory phospholipase A in myocardial remodelling after infarction. Histopathology 47:257–267
Banai S, Jaklitsch MT, Shou M, Lazarous DF, Scheinowitz M, Biro S, Epstein SE et al (1994) Angiogenic-induced enhancement of collateral blood flow to ischemic myocardium by vascular endothelial growth factor in dogs. Circulation 89:2183–2189
Ishikawa Y, Akishima-Fukasawa Y, Ito K, Akasaka Y, Tanaka M, Shimokawa R et al (2007) Lymphangiogenesis in myocardial remodelling after infarction. Histopathology 51:345–353
Libby P, Ridker PM, Hansson GK, Leducq Transatlantic Network on Atherothrombosis (2009) Inflammation in atherosclerosis: from pathophysiology to practice. J Am Coll Cardiol 54:2129–2138
Kholová I, Dragneva G, Cermáková P, Laidinen S, Kaskenpää N, Hazes T et al (2011) Lymphatic vasculature is increased in heart valves, ischaemic and inflamed hearts and in cholesterol-rich and calcified atherosclerotic lesions. Eur J Clin Invest 41:487–497
Gräbner R, Lötzer K, Döpping S, Hildner M, Radke D, Beer M et al (2009) Lymphotoxin beta receptor signaling promotes tertiary lymphoid organogenesis in the aorta adventitia of aged ApoE-/- mice. J Exp Med 206:233–248
Nakano T, Nakashima Y, Yonemitsu Y, Sumiyoshi S, Chen Y-X, Akishima Y et al (2005) Angiogenesis and lymphangiogenesis and expression of lymphangiogenic factors in the atherosclerotic intima of human coronary arteries. Hum Pathol 36:330–340
Mohler ER, Gannon F, Reynolds C, Zimmerman R, Keane MG, Kaplan FS (2001) Bone formation and inflammation in cardiac valves. Circulation 103:1522–1528
Otto CM, Kuusisto J, Reichenbach DD, Gown AM, O'Brien KD (1994) Characterization of the early lesion of “degenerative” valvular aortic stenosis: histological and immunohistochemical studies. Circulation 90:844–853
Soini Y, Salo T, Satta J (2003) Angiogenesis is involved in the pathogenesis of nonrheumatic aortic valve stenosis. Hum Pathol 34:756–763
Syväranta S, Helske S, Laine M, Lappalainen J, Kupari M, Mäyränpää MI et al (2010) Vascular endothelial growth factor-secreting mast cells and myofibroblasts: a novel self-perpetuating angiogenic pathway in aortic valve stenosis. Arterioscler Thromb Vasc Biol 30:1220–1227
Syväranta S, Helske S, Lappalainen J, Kupari M, Kovanen PT (2012) Lymphangiogenesis in aortic valve stenosis—novel regulatory roles for valvular myofibroblasts and mast cells. Atherosclerosis 221:366–374
Aharinejad S, Schäfer R, Hofbauer R, Abraham D, Blumer R, Miksovsky A et al (2001) Impact of cardiac transplantation on molecular pathology of ET-1, VEGF-C, and mitochondrial metabolism and morphology in dilated versus ischemic cardiomyopathic patients. Transplantation 72:1043–1049
Dashkevich A, Bloch W, Antonyan A, Goebel H, Fries JUW, Schlensak C et al (2010) Immunohistochemical study of remodeling of myocardial lymphatic and blood microvascular structures in terminal heart failure: differences between ischemic and dilated cardiomyopathy. Lymphology 43:110–117
Whitehurst B, Flister MJ, Bagaitkar J, Volk L, Bivens CM, Pickett B et al (2007) Anti-VEGF-A therapy reduces lymphatic vessel density and expression of VEGFR-3 in an orthotopic breast tumor model. Int J Cancer 121:2181–2191
Paavonen K, Puolakkainen P, Jussila L, Jahkola T, Alitalo K (2010) Vascular endothelial growth factor receptor-3 in lymphangiogenesis in wound healing. Am J Pathol 156:1499–1504
Kunstfeld R, Hirakawa S, Hong Y-K, Schacht V, Lange-Asschenfeldt B, Velasco P et al (2004) Induction of cutaneous delayed-type hypersensitivity reactions in VEGF-A transgenic mice results in chronic skin inflammation associated with persistent lymphatic hyperplasia. Blood 104:1048–1057
Cursiefen C, Chen L, Borges LP, Jackson D, Cao J, Radziejewski C et al (2004) VEGF-A stimulates lymphangiogenesis and hemangiogenesis in inflammatory neovascularization via macrophage recruitment. J Clin Invest 113:1040–1050
Iwata C, Kano MR, Komuro A, Oka M, Kiyono K, Johansson E et al (2007) Inhibition of cyclooxygenase-2 suppresses lymph node metastasis via reduction of lymphangiogenesis. Cancer Res 67:10181–10189
Ristimäki A, Narko K, Enholm B, Joukov V, Alitalo K (1998) Proinflammatory cytokines regulate expression of the lymphatic endothelial mitogen vascular endothelial growth factor-C. J Biol Chem 273:8413–8418
Johnson LA, Clasper S, Holt AP, Lalor PF, Baban D, Jackson DG (2006) An inflammation-induced mechanism for leukocyte transmigration across lymphatic vessel endothelium. J Exp Med 203:2763–2777
Saban MR, Mémet S, Jackson DG, Ash J, Roig AA, Israël A et al (2004) Visualization of lymphatic vessels through NF-kappaB activity. Blood 104:3228–3230
Veikkola T, Jussila L, Mäkinen T, Karpanen T, Jeltsch M, Petrova TV et al (2001) Signalling via vascular endothelial growth factor receptor-3 is sufficient for lymphangiogenesis in transgenic mice. EMBO J 20:1223–1231
Kang S, Lee S-P, Kim KE, Kim H-Z, Mémet S, Koh GY (2009) Toll-like receptor 4 in lymphatic endothelial cells contributes to LPS-induced lymphangiogenesis by chemotactic recruitment of macrophages. Blood 113:2605–2613
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2013 Springer Science+Business Media New York
About this chapter
Cite this chapter
Dashkevich, A., Lemström, K.B., Nykänen, A.I. (2013). VEGF Receptor Signaling in the Cardiac Lymphatics. In: Karunamuni, G. (eds) The Cardiac Lymphatic System. Springer, New York, NY. https://doi.org/10.1007/978-1-4614-6774-8_9
Download citation
DOI: https://doi.org/10.1007/978-1-4614-6774-8_9
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4614-6773-1
Online ISBN: 978-1-4614-6774-8
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)