Abstract
Pigmentary mosaicism refers to hyper or hypopigmentation due to genetic heterogenecity of cells. Pigmentary mosaicism may follow any of the patterns of cutaneous mosaicism and persist through life. Diagnosis is clinical. Associated extracutaneous manifestations have been reported in as much as 30 % of the cases.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
-
Pigmentary mosaicism refers to hyper- or hypopigmentation due to genetic heterogenecity of cells.
-
It has been referred to by many different names such as linear and whorled nevoid hyperpigmentation, segmental pigmentary disorder, nevoid hypermelanosis, or patterned pigmentation.
Pigmentary mosaicism is a term that has been used to describe variegate or irregular hyperpigmentation or hypopigmentation due to genetic heterogenecity of the cells that compose the skin. In this chapter we are going to focus on mosaic hyperpigmentation only. A mosaic state is the proposed pathogenetic mechanism of this type of hyperpigmentation although it has not been probed in all cases. Therefore some authors prefer the term patterned hyperpigmentation [1]. Pigmentary mosaicism may present conforming to the different patterns of cutaneous mosaicism as described by Happle [2].
Epidemiology
-
The exact incidence in dark-skinned individual is not known
There are no exact figures regarding the frequency of pigmentary hypermelanosis in dark skin. For any race the frequency also depends on the pattern. Phylloid hypermelanosis is the rarer variant with only a few cases published [3, 4].
Pigmentary mosaicism is usually not inherited although a few cases with several affected members in the same family point to epigenetic mosaicism (autosomal monoallelic expression) to explain the familial occurrence [5–7].
Clinical Features
-
Pigmentary mosaicism may follow any of the patterns of cutaneous mosaicism
-
May not be apparent at birth and increase for a few years until it stabilizes.
-
Many different extracutaneous abnormalities (CNS, ocular, cardiac, skeletal) have been described and investigation should be directed by clinical findings
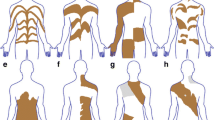
Pigmentary mosaicism manifests as hyperpigmented macules and patches that follow different patterns. They are usually present at birth although they may not become apparent until sun exposure during the first summer and may increase in number and size during the first years of life. The color may vary from light to dark brown. The patterns that have been described are linear and whorled hypermelanosis in which hyperpigmented, reticulated, streaky, narrow, and whorled macules occur along Blaschko lines (Fig. 8.1); broad band of hyperpigmentation along Blaschko lines; patchy hyperpigmented irregularly shaped macules without midline separation; checkerboard pattern, with alternating squares of pigmentary anomalies with a sharp midline separation and sometimes with a flag-like distribution (Fig. 8.2a, b) [8]; and lateralization pattern in which hyperpigmented macules affect only one side with midline separation (Table 8.1) [2, 9].
Associated extracutaneous manifestations have been reported in as much as 30 % of the cases, although this figure may reflect a reporting bias [10]. The associated findings include developmental delay, autism, seizures, microcephaly, and ocular, cardiac (ventricular septal defects and tetralogy of Fallot), and skeletal abnormalities (digit abnormalities, hemiatrophy).
The associated anomalies are so diverse that clinical investigation should be directed by clinical findings.
Pathogenesis
An enormous range of cytogenetic abnormalities has been reported in PM, including polyploidy, aneuploidy, and chromosomal deletions, insertions, and translocations. Mosaic trisomy 20, 7, 14, 18, and X-chromosomal have been reported in linear and whorled nevoid hypermelanosis [11–13]. The cytogenetic abnormalities may be only be found in fibroblast of affected skin. There is no single genotype for each phenotypic expression of pigmentary mosaicism except may be for phylloid hypermelanosis that has been more consistently related to chromosome 13 aberrations or mosaic chromosome 5p tetrasomy [4, 14] In most cases of pigmentary mosaicism a cytogenetic alteration cannot be detected and several hypotheses have been proposed to explain the abnormal pigmentation, such as comigration of genetically different cell populations, X-chromosome functional disomy, “Spreading” of X inactivation to autosomes, transposons, genetic imprinting, and phenotypic reversion [15].
Histology usually shows hyperpigmentation of the basal keratinocytes with normal number of melanocytes.
Treatment
-
No effective treatment has been described
There is no effective treatment for pigmentary mosaicism.
Prognosis
The hyperpigmented macules persist throughout life. The prognosis is marked by the associated extracutaneous findings.
Conclusion
Pigmentary mosaicism is a common usually sporadic disorder. Many different names have been used to describe it due to the fact that clinically it may manifest in any of the five patterns of cutaneous mosaicism described by Happle [9].
References
Thapa R. Pigmentary mosaicism: an update. Indian J Dermatol. 2008;53(2):96–7.
Happle R. Mosaicism in human skin. Understanding the patterns and mechanisms. Arch Dermatol. 1993;129(11):1460–70.
Happle R. Phylloid hypermelanosis: an unusual form of pigmentary mosaicism. Dermatology. 2010;220(2):183–5.
Oiso N, Tsuruta D, Imanishi H, et al. Phylloid hypermelanosis and melanocytic nevi with aggregated and disfigured melanosomes: causal relationship between phylloid pigment distribution and chromosome 13 abnormalities. Dermatology. 2010;220(2):169–72.
Happle R. Monoallelic expression on autosomes may explain an unusual heritable form of pigmentary mosaicism: a historical case revisited. Clin Exp Dermatol. 2009;34(7):834–7.
Al Aboud A, Al Aboud K, Al Hawsawi K, Al Aboud D, Ramesh V. Pigmentary mosaicism of hyperpigmented type in two sisters. Skinmed. 2005;4(2):120–1.
Horn D, Happle R, Neitzel H, Kunze J. Pigmentary mosaicism of the hyperpigmented type in two half-brothers. Am J Med Genet. 2002;112(1):65–9.
Stoll C, Alembik Y, Grosshans E, de Saint MA. An unusual human mosaic for skin pigmentation. Genet Couns. 2002;13(3):281–7.
Happle R. Dohi Memorial Lecture. New aspects of cutaneous mosaicism. J Dermatol. 2002;29(11):681–92.
Nehal KS, PeBenito R, Orlow SJ. Analysis of 54 cases of hypopigmentation and hyperpigmentation along the lines of Blaschko. Arch Dermatol. 1996;132(10):1167–70.
Hong SP, Ahn SY, Lee WS. Linear and whorled nevoid hypermelanosis: unique clinical presentations and their possible association with chromosomal abnormality inv (9). Arch Dermatol. 2008;144(3):415–6.
Hartmann A, Hofmann UB, Hoehn H, Broecker EB, Hamm H. Postnatal confirmation of prenatally diagnosed trisomy 20 mosaicism in a patient with linear and whorled nevoid hypermelanosis. Pediatr Dermatol. 2004;21(6):636–41.
Verghese S, Newlin A, Miller M, Burton BK. Mosaic trisomy 7 in a patient with pigmentary abnormalities. Am J Med Genet. 1999;87(5):371–4.
Hansen LK, Brandrup F, Rasmussen K. Pigmentary mosaicism with mosaic chromosome 5p tetrasomy. Br J Dermatol. 2003;149(2):414–6.
Taibjee SM, Bennett DC, Moss C. Abnormal pigmentation in hypomelanosis of Ito and pigmentary mosaicism: the role of pigmentary genes. Br J Dermatol. 2004;151(2):269–82.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer Science+Business Media New York
About this chapter
Cite this chapter
Baselga, E. (2015). Pigmentary Mosaicism. In: Silverberg, N., Durán-McKinster, C., Tay, YK. (eds) Pediatric Skin of Color. Springer, New York, NY. https://doi.org/10.1007/978-1-4614-6654-3_8
Download citation
DOI: https://doi.org/10.1007/978-1-4614-6654-3_8
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4614-6653-6
Online ISBN: 978-1-4614-6654-3
eBook Packages: MedicineMedicine (R0)