Abstract
The Brugada Syndrome, introduced as a new clinical entity 20 years ago, has attracted great interest because of its prevalence and association with high risk of sudden death, especially in males as they enter their third and fourth decade of life. Consensus reports published in 2002 and 2005 focused on diagnostic criteria, risk stratification and approaches to therapy. More recently, the risk stratification approaches have been the subject of controversy and debate.
Over 21 years have transpired since the introduction of the concept of phase 2 reentry, the mechanism believed to underlie development of arrhythmogenesis in BrS. Thus, the entity initially introduced as “ST segment elevation and right bundle branch block (RBBB)”, which came to be known as Brugada syndrome in 1996, evolved in the experimental laboratory and in the clinic along parallel but separate tracks. While the electrocardiographic and arrhythmic manifestations of BrS are well explained by abnormal repolarization in the right ventricular outflow track (RVOT), recent data have suggested conduction impairment in the RVOT as the basis for BrS, thus generating a debate as to the basis for the pathogenicity of the syndrome.
This review provides an overview of the clinical, genetic, molecular and cellular aspects of the Brugada syndrome and the various approaches to therapy.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Twenty years have passed since Pedro and Josep Brugada introduced the syndrome of ST segment elevation and right bundle branch block (RBBB) associated with a high incidence of ventricular fibrillation (VF) as a new clinical entity [1]. Over 21 years have transpired since the introduction of the concept of phase 2 reentry (induced by sodium channel block), the mechanism believed to underlie development of arrhythmogenesis in this clinical syndrome [2,3]. Thus, the entity, which in 1996 came to be known as the Brugada syndrome [4, 5], evolved in the experimental laboratory and in the clinic along parallel but separate tracks until the late 1990s [6].
The Brugada syndrome has attracted great interest because of its prevalence and association with high risk of sudden death, especially in males as they enter their third and fourth decade of life. A consensus report published in 2002 delineated diagnostic criteria for the syndrome [7, 8]. A second consensus conference report published in 2005 focused on risk stratification schemes and approaches to therapy [9, 10]. More recently, these risk stratification approaches have been the subject of controversy and hot debate [11–15]. This review provides an overview of the genetic, molecular and cellular aspects of the Brugada syndrome and the various approaches to therapy.
Clinical Characteristics
A brief description of clinical characteristics is included to provide a perspective for our discussion of mechanisms and therapy. This subject is more thoroughly dealt with in the preceding chapter. The Brugada syndrome is characterized by an ST segment elevation in the right precordial ECG leads and a high incidence of sudden death. Worldwide prevalence of BrS is estimated to be 1 in 10,000, but is much higher in Asian and Southeast Asian countries, reaching 5–10 in 10,000 [10, 16, 17] and much lower in some Eastern European countries like Denmark, with an estimated prevalence of 1.1 in 100,000 [18]. The average age at the time of initial diagnosis or sudden death is 40 ± 22, although the range is wide with youngest patient diagnosed at 2 days of age, and the oldest at 84 [19, 20].
The electrocardiographic manifestations of the Brugada syndrome are often concealed but can be unmasked by sodium channel blockers and febrile or vagal states [5, 21–27]. Three types of repolarization patterns in the right precordial leads are recognized (Table 29.1) [7, 8]. A Type 1 ST segment elevation is characterized by a coved ST-segment elevation ≥2 mm (0.2 mV). Only a Type I ST segment elevation with or without a negative T-wave is diagnostic of Brugada syndrome. Although present in the majority of BrS cases, a negative T wave is not necessary for the diagnosis of BrS [28]. Type 2 ST segment elevation has a saddleback appearance with a high take-off ST-segment elevation of ≥2 mm followed by a trough displaying ≥1 mm ST elevation followed by either a positive or biphasic T-wave. Type 3 ST segment elevation has either a saddleback or coved appearance with an ST-segment elevation of <1 mm. These three patterns may be observed sequentially in the same patient. The BrS ECG is generally very dynamic, varying over time. Using serial ECGs, Richter et al. found that among patients initially presenting with a spontaneous Type I ST segment elevation, the BrS phenotype is only seen on every third ECG [29], Type 2 and Type 3 ST segment elevation are not diagnostic of the Brugada syndrome. According to the 2005 consensus statement, Brugada syndrome is definitively diagnosed when a Type 1 ST-segment elevation is observed in more than one right-precordial lead (V1–V3), in the presence or absence of sodium channel blocking agent, and in conjunction with one or more of the following: documented ventricular fibrillation; polymorphic ventricular tachycardia; a family history of SCD (<45 years old); coved type ECGs in family members; inducibility of ventricular tachycardia (VT) with programmed electrical stimulation; syncope; or nocturnal agonal respiration [7–10]. A recent study provided evidence that a Type I ST segment elevation or J wave in one rather than two right precordial lead may suffice to meet the criteria for diagnosis of BrS [30].
Diagnosis of Brugada syndrome is also considered positive when a Type 2 (saddleback pattern) or Type 3 ST-segment elevation is observed in more than one right precordial lead under baseline conditions and can be converted to the diagnostic Type 1 pattern upon exposure to sodium channel blocker (ST-segment elevation should be ≥2 mm). One or more of the clinical criteria described above should also be present. Drug-induced conversion of Type 3 to Type 2 ST-segment elevation is considered inconclusive for diagnosis of Brugada syndrome.
The ECG manifestations of the syndrome are often concealed, but can be unmasked using sodium channel blockers. Definitive diagnosis is difficult when the degree of basal ST-segment elevation is relatively small and the specificity of sodium channel blockers such as flecainide, ajmaline, procainamide, disopyramide, propafenone and pilsicainide [22, 31, 32] to identify patients at risk is uncertain. A comparison of intravenous ajmaline and flecainide in the same cohort of patients revealed that ajmaline is more effective in unmasking the syndrome [33]. Flecainide failed in 7 of 22 cases (32 %) unmasked by ajmaline. A greater inhibition of transient outward current (Ito) by flecainide renders it less effective than ajmaline. False positive as well as false negative responses have been reported with ajmaline, as well, although a false positive is difficult to prove [34, 35]. Itoh et al. demonstrated that a specific missense mutation in SCN5A, the gene that encodes the α subunit of the sodium channel, although responsible for the disease, prevented the ability of ajmaline to unmask the syndrome, due to loss of the ability of the drug to produce use-dependent inhibition of sodium channel current [35].
Most cases of Brugada syndrome display right precordial ST-segment elevation, although isolated cases of inferior lead [36, 37] or left precordial lead [38] ST-segment elevation have been reported in Brugada-like syndromes, in some cases associated with SCN5A mutations. In rare cases, ST segment elevation is observed in all precordial leads. The appearance of an early repolarization pattern, characterized by J point elevation, distinct J waves, slurring of the terminal part of the QRS and/or ST segment elevation, in the inferior or infero-lateral leads in patients with Type I ST segment elevation in the anterior leads has been associated with adverse prognosis [39–41]. This type of global ST segment elevation, manifesting in inferior, lateral and anterior leads, has been termed Type 3 Early Repolarization Syndrome (ERS) in a recent proposed classification of ERS [42].
Placement of the right precordial leads in a superior position (up to the second intercostal spaces above normal) can increase the sensitivity of the ECG for detecting the Brugada phenotype in some patients, both in the presence or absence of a drug challenge [43, 44] or during Holter recordings [45]. Studies are underway to ascertain whether the greater sensitivity is at the cost of a lower specificity and whether a Type I ECG in the elevated leads is as predictive of events as a Type I ECG the in the standard leads. A recent report demonstrates that as many as 1.3 % of normal Korean males display a Type 2, but not Type 1, ST segment elevation when the right precordial leads are recorded from a superior position [46].
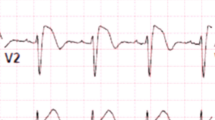
A slight prolongation of the QT-interval is sometimes observed associated with the ST segment elevation [32, 47, 48]. The QT-interval is prolonged more in the right vs. left precordial leads, presumably due to a preferential prolongation of action potential duration (APD) in right ventricular (RV) epicardium secondary to accentuation of the action potential notch [49]. A QTc >460 ms in V2 has been shown to be associated with arrhythmic risk [50]. Depolarization abnormalities including prolongation of P-wave duration, PR and QRS intervals are frequently observed, particularly in patients linked to SCN5A mutations [51]. PR prolongation likely reflects HV conduction delay [47]. QRS fragmentation, defined as three or more spikes in the QRS complex, has been found to be an independent predictor of spontaneous arrhythmic events [52, 53].
In many cases arrhythmia initiation is bradycardia-related [54]. This may contribute to the higher incidence of sudden death at night in individuals with the syndrome and may account for the success of pacing in controlling the arrhythmia in isolated cases of the syndrome [55]. Makiyama and co-workers reported that loss-of-function SCN5A mutations resulting in Brugada syndrome are distinguished by profound bradyarrhythmias [56]. Related to this observation is the recent report by Scornik and co-workers [57] demonstrating expression of the cardiac sodium channel gene, SCN5A, in intracardiac ganglia. This interesting finding suggests that a loss of function mutations in SCN5A may not only create the substrate for reentry in ventricular myocardium, but may also increase vagal activity in intracardiac ganglia, thus facilitating the development of arrhythmias in patients with the Brugada syndrome. This finding may also explain the frequent association of vasovagal syncope with BrS [58].
A polymorphic ventricular tachycardia (VT) is most commonly associated with the Brugada syndrome. Monomorphic ventricular tachycardia (VT) is observed infrequently and is generally more prevalent in children and infants [59–64].
The majority of congenital Brugada syndrome patients are believed to possess a structurally normal heart, consistent with the notion that this is a primary electrical heart disease [65]. While fibrosis and myocarditis may exacerbate or indeed trigger events in patients with the Brugada syndrome, it seems clear that in the vast majority of cases these structural changes are unrelated to arrhythmogenic right ventricular cardiomyopathy/dysplasia (ARVC/D).
Prognosis and Risk Stratification
Risk stratification of patients with the Brugada syndrome has been an issue of lively debate. It is generally accepted that Brugada syndrome patients presenting with aborted sudden death are at high risk for recurrence and that they should be protected by an implantable cardiac defibrillator (ICD). There is also little argument that a patient with Brugada syndrome presenting with syncope, particularly when the clinical history suggests an arrhythmic syncope (as opposed to typical vasovagal syncope), are at high risk. In contrast, risk stratification of asymptomatic patients has met with considerable debate [11, 15, 66–70]. Several invasive and noninvasive parameters have been proposed for identification of patients at risk of sudden death, including the presence of spontaneous Type 1 ST segment elevation, the characteristics of the S wave [71], wider QRS complexes [72], the presence of late potentials [73] or QRS fragmentation [52, 53] and inducibility of VT/VF using programmed electrical stimulation (PES) [74].
In 1998, Brugada et al. [75] reported that over a 34 month follow-up period, 27 % of previously asymptomatic patients experienced a first ventricular fibrillation or sudden cardiac death. This figure corresponds to an occurrence of life-threatening events of approximately 10 % per year. In 2002, with a mean follow-up of 27 ± 29 months, the same authors [66] reported that 8 % of previously asymptomatic patients had become symptomatic; an occurrence of a life-threatening event of 3.5 % per year. In 2005, Brugada et al. [68] reported that 6 % of asymptomatic patients displayed a first event during a mean follow-up of 42 ± 42 months, corresponding to an event rate of 1.7 % per year. This progressive decline in first event rate in previously asymptomatic patients most likely reflects a reduced severity of phenotypes referred to the Brugada registry in subsequent years. In contrast, Priori et al. in 2002 [67] reported that asymptomatic patients have a cumulative probability of 14 % for developing a cardiac arrest by age 40, corresponding to an natural history incidence of cardiac arrest of 0.35 % per year. In 2005, the same authors reported a first event rate of 3 % (4/132) over a 31 month follow-up period, corresponding to an event rate of 1 % per year [69].
The reason behind the disparity in the data generated by these two groups is not clearly evident. It was suggested by Brugada et al. [68] that the difference may be due to the inclusion by Priori and co-workers of patients with Type 2 and 3 ST segment elevation, which is not considered diagnostic of the Brugada syndrome [7–10]. Priori and co-workers argue that exclusion of Type 2 and 3 from the diagnosis of the syndrome can lead to missed diagnosis of the disease [69]. While this is clearly the case, it may be a rare occurrence, and the exclusion appears justified on the basis that it avoids a large number of false positive diagnoses. As a result of the failure to exclude individuals with Type 2 and 3 ST segment elevation, the European registry may contain many individuals who do not have the syndrome. However, a recent report by Eckardt and co-workers [70] suggests that other factors may be involved. These authors report that 1 out of 123 asymptomatic individuals with a Type 1 ECG (0.8 %) had a first arrhythmic event during a 40 ± 50 month follow-up. This translates into a first event rate of 0.24 % per year, considerably less than the other two registries. Thus, as additional data have become available, it has become clear that the prognosis of asymptomatic patients is associated with much less risk than initially perceived.
The large registry studies agree that Brugada syndrome patients at higher risk for the development of subsequent events are those presenting with a spontaneous Type 1 ST segment elevation or Brugada ECG and/or those with a previous VT/VF or Sudden Cardiac Death (SCD) [70]. The registries also agree that PES inducibility is greatest among patients with previous VT/VF or syncope. Approximately 1/3 of asymptomatic patients are inducible. In the Priori et al. [69] and Eckardt et al. [70] studies inducibility of VT/VF in asymptomatic patients was not associated with risk. The lack of association between inducibility and spontaneous VF in Brugada patients was also reported by a number of smaller studies, such as that of Kanda et al. [76].
In sharp contrast, Brugada et al. [77] found that the risk for developing VT/VF is considerably greater in patients who are inducible during PES, whether or not a Type 1 ST segment elevation was spontaneously present or whether or not they were symptomatic. The reason for the marked disparity in the predictive power of PES inducibility among the different studies is not immediately apparent. The discrepancies may be due to differences in patient characteristics and the use of multiple testing centers with non-standardized or non-comparable stimulation protocols [78]. Additional studies are clearly needed to further define risk stratification strategies for asymptomatic patients.
It is noteworthy that in experimental models of the Brugada syndrome involving the coronary-perfused wedge preparation, polymorphic VT is readily inducible with a single ventricular extrastimulus, but only when applied on the epicardial surface of the wedge. Inducibility is not possible or much more difficult when extra-stimulation is applied to the endocardial surface. The shorter refractory period of epicardium allows extra-stimuli direct access to the vulnerable window across the ventricular wall, thus facilitating the induction of reentry. These relationships suggest that PES applied to the epicardium may provide a more accurate assessment of risk than the current clinical approach in which stimuli are applied to the endocardial surface. In support of this hypothesis, Carlsson et al. reported that a Brugada syndrome patient with recurrent syncope due to polymorphic ventricular tachycardia could not be induced with right ventricular endocardial stimulation. However, epicardial stimulation from a left ventricular site through the coronary sinus led to the development of polymorphic VT [79].
Gehi et al. [80] recently reported the results of a meta-analysis of 30 prospective studies that included 1,545 patients with a Brugada ECG to assess predictors of events. The meta-analysis suggested that a history of syncope or SCD, the presence of a spontaneous Type I Brugada ECG, and male gender predict a more malignant natural history. The findings however did not support the use of a family history of SCD, the presence of an SCN5A gene mutation, or electrophysiologic study to guide the management of patients with a Brugada ECG. A similar meta-analysis by Paul et al. [81] also concluded that the inducibility of VF in asymptomatic patients is of no prognostic value.
Since the publication of the meta-analyses by Gehi et al. and Paul et al., two large multicenter studies from Japan [82] and from Europe (the FINGER study) [83] were published. The Japanese study is important because it included only probands (330 probands of whom 154 were asymptomatic) and the FINGER study was important because the number of asymptomatic patients included (n = 654) was significantly larger than the number of asymptomatic patients included in the last published series by Brugada (n = 263) and even larger than the 457 patients number compiled from 15 studies in the meta-analysis by Paul. Both studies used an EPS protocol that included two sites of stimulation [right ventricular apex (RVA) and outflow tract (RVOT)] with up to three extrastimuli, with the FINGER protocol using a minimal coupling interval of 200 ms, whereas the Japanese investigators limited the coupling interval of the extrastimulus only by ventricular refractoriness. This difference in the EPS protocol probably explains why the percentage of asymptomatic individuals with inducible VF was higher in the Japanese study than in FINGER (57 % vs. 37 %). The latter figure is very close to the 34 % inducibility rate reported by Brugada among their asymptomatic individuals.
In Finger, asymptomatic individuals with inducible VF did have more spontaneous arrhythmic events than non-inducible patients, but the event rate was very low for both groups (1.1 vs. 0.4 % event rate per year). Moreover, using multivariate analysis the EPS results were no longer (independent) predictors of outcome. Inducibility of VF was not a predictor of outcome among asymptomatic individuals in the Japanese study.
Makimoto et al. [84] recently reported that inducibility to VF was of prognostic value only when VF was induced with one or two extrastimuli and suggested that triple extrastimulation should be avoided to prevent false-positive results. These results, however, where not confirmed by the prospective PRELUDE study [53]; the induction of VF was of no prognostic value regardless of the protocol of extrastimulation used.
Genetic Basis
Brugada syndrome shows an autosomal dominant mode of inheritance. The first gene to be linked to the syndrome is SCN5A, the gene that encodes the α subunit of the cardiac sodium channel gene [85]. Figure 29.1 highlights the diversity of SCN5A mutations associated with the Brugada syndrome. Of note, mutations in SCN5A are also responsible for the LQT3 form of the long QT syndrome and cardiac conduction disease. A number of mutations have been reported to cause overlapping syndromes; in some cases all three phenotypes are present [87]. Over 300 mutations in SCN5A have been associated with the syndrome in recent years [88].
Schematic of SCN5A, the gene that encodes the α subunit of the sodium channel, illustrating mutations linked to Brugada syndrome, long QT3 syndrome, conduction disease and atrial standstill. Some mutations are associated with combined phenotypes (From Antzelevitch and Viskin [86]. Reprinted with permission from Springer)
Only a fraction of these mutations have been studied in expression systems and shown to result in loss of function. A number of mechanisms have been delineated for the reduction in sodium channel current (INa), including [89–93]: (1) failure of the sodium channel to express due to faulty protein synthesis and/or trafficking; (2) a shift in the voltage- and time-dependence of sodium channel current (INa) activation, inactivation or reactivation; (3) entry of the sodium channel into an intermediate state of inactivation from which it recovers more slowly or (4) accelerated inactivation of the sodium channel. In in vitro expression systems, the premature inactivation of the sodium channel is sometimes observed at physiological temperatures, but not at room temperature [94]. Acceleration of INa inactivation was still more accentuated at higher than physiological temperatures, suggesting that the syndrome may be unmasked, and that patients with the Brugada syndrome may be at an increased risk, during a febrile state [94]. A number of Brugada patients displaying fever-induced polymorphic VT have been identified since the publication of this report [23, 61, 95–102].
Mutation in the SCN5A gene account for approximately 11–28 % of Brugada syndrome cases [88]. A higher incidence of SCN5A mutations has been reported in familial than in sporadic cases [90]. It is important to recognize that a negative SCN5A result does not rule out this gene as a cause, since the promoter region, cryptic splicing mutations or presence of gross rearrangements are generally not part of routine investigation. A recent report by Hong et al. [103] provided the first report of a dysfunctional sodium channel created by an intronic mutation giving rise to cryptic splice site activation in SCN5A in a family with the Brugada syndrome. The deletion of fragments of segments two and three of Domain IV of SCN5A caused complete loss of function.
Evidence in support of the hypothesis that an SCN5A promoter polymorphism common in Asians modulates variability in cardiac conduction, and may contribute to the high prevalence of Brugada syndrome in the Asian population was recently advance by Bezzina and co-workers [104]. Sequencing of the SCN5A promoter identified a haplotype variant consisting of six polymorphisms in near-complete linkage disequilibrium that occurred at an allele frequency of 22 % in Asian subjects and was absent in whites and blacks. These findings demonstrate that sodium channel transcription in the human heart may vary considerably among individuals and races and be associated with variable conduction velocity and arrhythmia susceptibility [104].
BrS has in recent years been linked to mutations in ten other genes. Calcium channel genes mutations, including those in CACNA1C (Cav1.2, BrS3), CACNB2b (Cavß2b, BrS4) and CACNA2D1 (Cavα2δ1, BrS9) are found in approximately 12–13 % of probands [105, 106]. Mutations in glycerol-3-phosphate dehydrogenase 1-like enzyme gene (GPD1L, BrS2), SCN1B (β1-subunit of Na channel, BrS5), KCNE3 (MiRP2; BrS6), SCN3B (β3-subunit of Na channel, BrS7), KCNJ8 (BrS8) and KCND3 (BrS10) are more rare [107–112]. Mutations in these genes lead to loss of function in INa and ICa, as well as to a gain of function in Ito or IK-ATP. MOG1 was recently described as a new partner of Nav1.5, playing a role in its regulation, expression and trafficking. A missense mutation in MOG1 has also been associated with BrS (BrS11) [113, 114].
It is generally accepted that identification of specific mutations may not be very helpful in formulating a diagnosis or providing a prognosis. Mutations have been reported throughout the SCN5A gene and no hotspots have been identified. It is not clear whether some mutations are associated with a greater risk of arrhythmic events or sudden death. Genetic testing is recommended for support of the clinical diagnosis, for early detection of relatives at potential risk and particularly for the purpose of advancing research and our understanding of genotype-phenotype relations [115].
Cellular and Ionic Mechanisms Underlying the Development of the Brugada Phenotype
Transmural Cellular and Ion Channel Distinctions
Ventricular myocardium is known to be comprised of at least three electrophysiologically and functionally distinct cell types: epicardial, M and endocardial cells [116, 117]. These three principal ventricular myocardial cell types differ with respect to phase 1 and phase 3 repolarization characteristics. Ventricular epicardial and M, but not endocardial, cells generally display a prominent phase 1, due to a large 4-aminopyridine (4-AP) sensitive transient outward current (Ito), giving the action potential a spike and dome or notched configuration. These regional differences in Ito, first suggested on the basis of action potential data [118], have now been directly demonstrated in canine [119], feline [120], rabbit [121], rat [122], and human [123–126] ventricular tissues and cells. Differences in the magnitude of the action potential notch and corresponding differences in Ito have also been described between right and left ventricular epicardium [127]. Similar inter-ventricular differences in Ito have also been described for canine ventricular M cells [128]. This distinction is thought to form the basis for why the Brugada syndrome, a channelopathy–mediated form of sudden death, is a right ventricular disease.
The molecular basis for the transmural distribution of Ito has long been a subject of debate. The transmural gradient of Ito in dog has been ascribed to a transmural distribution of: (1) KCND3 gene (Kv4.3), which encodes the α subunit of the Ito channel [129]; (2) KChIP2, a β subunit that co-assembles with Kv4.3 [130] and (3) IRX5, a transcriptional factor regulating KCND3 [131].
Myocytes isolated from the epicardial region of the left ventricular wall of the rabbit show a higher density of cAMP-activated chloride current when compared to endocardial myocytes [132]. Ito2, initially ascribed to a K+ current, is now thought to be primarily due to the calcium-activated chloride current (ICl(Ca)) is also thought to contribute to the action potential notch, but it is not known whether this current, differs among the three ventricular myocardial cell types [133].
Recent studies involving canine ventricular myocytes have shown that calcium current (ICa) is similar among cells isolated from epicardium, M, and endocardial regions of the left ventricular wall [134, 135]. One study however reported differences in Ca2+ channel properties between epicardial and endocardial canine ventricular cells. In that study, ICa was found to be larger in endocardial than in epicardial myocytes (3.4 ± 0.2 vs. 2.3 ±0.1 pA/pF). A low-threshold, rapidly activating and inactivating Ca2+ current that resembles the T-type current, was also recorded in all endocardial myocytes, but was small or absent in epicardial myocytes. The T-like current was comprised of two components: a Ni2+-sensitive T-type current and a tetrodotoxin-sensitive Ca2+ current [136].
The surface epicardial and endocardial layers are separated by transitional and M cells. M cells are distinguished by the ability of their action potential to prolong disproportionately relative to the action potential of other ventricular myocardial cells in response to a slowing of rate and/or in response to action potential duration (APD)-prolonging agents [116, 137, 138]. In the dog, the ionic basis for these features of the M cell include the presence of a smaller slowly activating delayed rectifier current (IKs) [139], a larger late sodium current (late INa) [140] and a larger Na-Ca exchange current (INa-Ca) [141]. In the canine heart, the rapidly activating delayed rectifier (IKr) and inward rectifier (IK1) currents are similar in the three transmural cell types. Transmural and apico-basal differences in the density of IKr channels have been described in the ferret heart [142]. IKr message and channel protein are much larger in the ferret epicardium. IKs is larger in M cells isolated from the right vs. left ventricles of the dog [128].
Cellular Basis for the Electrocardiographic J Wave
The presence of a prominent action potential notch in epicardium but not endocardium gives rise to a transmural voltage gradient during ventricular activation that manifests as a late delta wave following the QRS or what more commonly is referred to as a J wave [4] or Osborn wave. A distinct J wave is often observed under baseline conditions in the ECG of some animal species, including dogs and baboons. Humans more commonly display a J point elevation rather than a distinct J wave. A prominent J wave in the human ECG is considered pathognomonic of hypothermia [143–145] or hypercalcemia [146, 147].
A transmural gradient in the distribution of Ito is responsible for the transmural gradient in the magnitude of phase 1 and action potential notch, which in turn gives rise to a voltage gradient across the ventricular wall responsible for the inscription of the J wave or J point elevation in the ECG [118, 119, 148]. Direct evidence in support of the hypothesis that the J wave is caused by a transmural gradient in the magnitude of the Ito-mediated action potential notch derives from experiments conducted in the arterially-perfused right ventricular wedge preparation showing a correlation between the amplitude of the epicardial action potential notch and that of the J wave recorded during interventions that alter the appearance of the electrocardiographic J wave, including hypothermia, premature stimulation (restitution), and block of Ito by 4-aminopyridine (4-AP) (Fig. 29.2) [4].
Hypothermia-induced J wave. Each panel shows transmembrane action potentials from the epicardial and endocardial regions of an arterially perfused canine left ventricular wedge and a transmural ECG simultaneously recorded. (a) The relatively small action potential notch in epicardium but not in endocardium is associated with an elevated J-point at the R-ST junction (arrow) at 36 °C. (b) A decrease in the temperature of the perfusate to 29 °C results in an increase in the amplitude and width of the action potential notch in epicardium but not endocardium, leading to the development of a transmural voltage gradient that manifests as a prominent J wave on the ECG (arrow) (Modified from Yan and Antzelevitch [4], with permission from Wolters Kluwer Health)
Transmural activation within the thin wall of right ventricle (RV) is relatively rapid causing the J wave to be buried inside the QRS. Thus, although the action potential notch is most prominent in right ventricular epicardium, right ventricular myocardium would be expected to contribute relatively little to the manifestation of the J wave under normal conditions. These observations are consistent with the manifestation of the normal J wave in ECG leads in which the mean vector axis is transmurally oriented across the left ventricle and septum. Accordingly, the J wave in the dog is most prominent in leads II, III, aVR, aVF, and mid to left precordial leads V3 through V6. A similar picture is seen in the human ECG [147, 149]. In addition, vectorcardiography indicates that the J wave forms an extra loop that occurs at the junction of the QRS and T loops [150]. It is directed leftward and anteriorly, which explains its prominence in leads associated with the left ventricle.
The first description of the J wave was in the 1920s in animal experiments involving hypercalcemia [146]. The first extensive description and characterization appeared 30 years later by Osborn in a study involving experimental hypothermia in dogs [151]. The appearance of a prominent J wave in the clinic is typically associated with pathophysiological conditions, including hypothermia [143, 149] and hypercalcemia [146, 147]. The prominent J wave induced by hypothermia is the result of a marked accentuation of the spike-and-dome morphology of the action potential of M and epicardial cells (i.e., an increase in both width and magnitude of the notch). In addition to inducing a more prominent notch, hypothermia produces a slowing of conduction which permits the epicardial notch to clear the QRS so as to manifest a distinct J wave. Hypercalcemia-induced accentuation of the J wave [146, 147, 152] may also be explained on the basis of an accentuation of the epicardial action potential notch, possibly as a result of an augmentation of the calcium-activated chloride current and a decrease in ICa [153]. Accentuation of the action potential notch also underlies the electrocardiographic and arrhythmogenic manifestations of the Brugada syndrome.
Repolarization Abnormalities as the Basis for the ECG and Arrhythmic Manifestations of BrS. Exaggeration of the J Wave Is the Basis for ST Segment Elevation in BrS
An increase in net repolarizing current, whether secondary to a decrease of inward currents or an increase of outward current, accentuates the action potential notch leading to augmentation of the J wave or appearance of ST segment elevation. A further increase in net repolarizing current can result in partial or complete loss of the action potential dome, leading to a transmural voltage gradient that manifests as accentuation of the J wave or an ST segment elevation [154–156]. In regions of the myocardium exhibiting a prominent Ito, such as the right ventricular epicardium, marked accentuation of the action potential notch leads to a augmentation of the J wave, manifesting as a coved-type ST segment elevation, which is diagnostic of BrS (Fig. 29.3a, b). Because the second action potential upstroke is delayed, epicardium now repolarizes after endocardium, causing inversion of the T wave. Note that although the ECG now displays the typical BrS morphology with a covered type ST segment elevation and negative T wave, no major arrhythmogenic substrates are present. The substrate for reentry, however develops with any additional outward shift of the net current active during the early phase of the action potential. This leads to loss of the action potential dome, thus creating a dispersion of repolarization between epicardium and endocardium as well as within epicardium, between the region where the dome is lost and regions at which it is maintained (Fig. 29.3c). Sodium channel blockers like procainamide, pilsicainide, propafenone, flecainide and disopyramide cause a further outward shift of current flowing during the early phases of the action potential and are thereby effective in inducing or unmasking ST segment elevation in patients with concealed J-wave syndromes [22, 31, 158]. Sodium channel blockers like quinidine, which also inhibits Ito, reduce the magnitude of the J wave and normalize ST segment elevation [154, 159]. Loss of the action potential dome is usually heterogeneous, resulting in marked abbreviation of action potential at some sites but not others. The dome can then propagate from regions at which it is maintained to regions where it is lost, giving rise to a very closely coupled extrasystole via phase 2 reentry (Fig. 29.3d) [3]. The phase 2 reentrant beat is capable of initiating polymorphic ventricular tachycardias (VT) or ventricular fibrillation (Fig. 29.3e, f).
Cellular basis for electrocardiographic and arrhythmic manifestation of BrS. Each panel shows transmembrane action potentials from one endocardial (top) and two epicardial sites together with a transmural ECG recorded from a canine coronary-perfused right ventricular wedge preparation. (a) Control (Basic cycle length (BCL) 400 ms). (b) Combined sodium and calcium channel block with terfenadine (5 μM) accentuates the epicardial action potential notch creating a transmural voltage gradient that manifests as an exaggerated J wave or ST segment elevation in the ECG. (c) Continued exposure to terfenadine results in all-or-none repolarization at the end of phase 1 at some epicardial sites but not others, creating a local epicardial dispersion of repolarization (EDR) as well as a transmural dispersion of repolarization (TDR). (d) Phase 2 reentry occurs when the epicardial action potential dome propagates from a site where it is maintained to regions where it has been lost giving rise to a closely coupled extrasystole. (e) Extrastimulus (S1–S2 = 250 ms) applied to epicardium triggers a polymorphic VT. (f) Phase 2 reentrant extrasystole triggers a brief episode of polymorphic VT (Modified from Fish and Antzelevitch [157], with permission from Elsevier Limited)
Phase 2 reentry has been shown to occur when right ventricular epicardium is exposed to: (1) K+ channel openers such as pinacidil [160]; (2) sodium channel blockers such as flecainide [3]; (3) increased [Ca2+]o [153]; (4) calcium channel blockers such as verapamil; (5) metabolic inhibition [161]; and (6) simulated ischemia [162]. Evidence in support of a phase 2 reentrant mechanism in humans was provided by Thomsen et al. [163, 164].
Does Delayed Conduction Contribute to the ECG and Arrhythmic Manifestations of BrS?
While most investigations suggest that repolarization abnormalities underlie the pathophysiology of Brugada syndrome, recent studies suggest the possibility of delayed depolarization in the right ventricular outflow tract as a contributing mechanism to ST segment elevation or J waves associated with BrS [165, 166]. The repolarization vs. depolarization hypotheses controversy has been documented as a published debate [167].
Seemingly compelling data in support of delayed conduction in the RVOT as the basis for BrS was recently presented by Nademanee and co-workers [166]. Using an electrogram applied to the epicardial surface of the RVOT, these authors recorded late potentials, in some cases appearing as a continuous fractionated electrogram. This was interpreted as indicating delayed conduction over the anterior aspect of the RVOT epicardium. Catheter ablation over this abnormal region of the RVOT resulted in normalization of the Brugada ECG pattern over a period of up to 3 months and prevented VT/VF, both during electrophysiological studies, as well as spontaneous recurrence of VT/VF episodes. Signal averaged ECG (SAECG) recordings have also demonstrated late potentials in patients with the Brugada syndrome, especially in the anterior wall of the right ventricular outflow tract (RVOT) [168–174].
Although traditionally ascribed to conduction delays secondary to structural defects, in cases of BrS, late potentials of the type described by Nademanee et al. more likely arise from a delayed second upstroke of the epicardial action potential in the RVOT or to a concealed phase 2 reentry [19, 167, 170]. It is noteworthy that wall motion abnormalities have also been detected in BrS patients [175]. Although such contractile abnormalities are commonly considered pathognomonic of structural disease, in the setting of BrS, they could well be the result of loss of the action potential dome in the right ventricular epicardium [170, 176]. Loss of the dome would lead to contractile dysfunction because calcium entry into the cells would be greatly diminished and sarcoplasmic reticulum calcium stores would be depleted.
It has been suggested that the rate-dependence of the ST segment elevation in BrS may be helpful in discriminating between the repolarization and depolarization hypotheses [19]. If the ST segment elevation is due predominantly to delayed conduction in the RVOT, acceleration of the rate would be expected to further aggravate conduction and thus accentuate the ST segment elevation and the RBBB morphology of the ECG. If, on the other hand, ST segment elevation or the BrS sign is secondary to accentuation of the epicardial action potential notch, acceleration of the rate would be expected to normalize the ECG, by reducing the action potential notch and restoring the action potential dome in RV epicardium. This occurs because the transient outward current, which is at the heart of this mechanism, is slow to recover from inactivation and is less available at faster rates.
Although there are relatively few reports of the effects of pacing, most investigators in the field agree that there is a tendency for the ST segment elevation associated with Brugada ECGs to normalize during an increase in heart rate, consistent with the repolarization hypothesis [177–179]. There are however also reports of ST segment elevation or J point elevation with exercise. Amin et al. recently reported J point elevation in BrS patients (both SCN5A+ and SCN5A−) during exercise [180]. The principal difference between studies showing a decrease vs. increase of the J point in response to exercise appears to be the presence of a prominent ST segment elevation at baseline in the former.
Interestingly, in BrS cases in which ST segment elevation is accompanied by notching of the QRS, the latter suggesting major conduction delay in the RVOT, exercise-induced acceleration of rate leads to further fragmentation of the QRS, but to a normalization of the ST segment elevation in all right precordial leads [167]. These findings suggest that the ST segment elevation is due to a repolarization defect and not to the clearly apparent depolarization defect responsible for the fragmentation of the QRS. Fragmentation of the QRS is associated with increased mortality and arrhythmic events in patients with coronary artery disease as well as patients with arrhythmogenic right ventricular cardiomyopathy and Brugada syndrome [181].
Kurita et al. placed monophasic action potential (MAP) electrodes on the epicardial and endocardial surfaces of the right ventricular outflow tract (RVOT) in patients with the Brugada syndrome and demonstrated an accentuated notch in the epicardial response, thus providing direct support for the repolarization hypothesis in humans [182, 183].
Additional support for the repolarization hypothesis derives from the demonstration that quinidine normalizes ST segment elevation and suppresses late potentials recorded in patients with Brugada syndrome [184–186]. These effects of the drug are presumably due to inhibition of Ito leading to reduction of the epicardial action potential notch and normalization of the repolarization heterogeneities. If the ST segment elevation or the late potentials were due to delayed conduction, quinidine-induced INa inhibition would be expected to accentuate their appearance.
Although there is no experimental model of BrS based on the depolarization hypothesis, several groups have developed a models of BrS based on the repolarization hypothesis [154, 157, 187–192].
Experimental models displaying major conduction delays have been developed by exposing wedge preparations to global ischemia [193, 194]. Progressive delay in these models leads to a gradual prolongation of the R wave and inversion of the T wave. The ECG at first glance resembles a BrS phenotype, but with closer inspection it is clear that the depolarization hypothesis does not lead to an ST segment elevation, but rather to an R wave prolongation. The marked conduction delay is due to a discontinuity in conduction in the deep subepicardium. Conduction under these conditions is exquisitely sensitive to rate, with acceleration leading to block and inexcitability. This is a common characteristic of ischemia-induced tombstone morphology of the ECG induced by coronary spasm [195], but is not characteristic of BrS A similar phenomenon is observed in right ventricular wedge preparations following exposure to hyperkalemic conditions [196].
Of note, magnetocardiograms recorded from patients with complete RBBB have been shown to generate currents from the RVOT to the upper left chest that are opposite from those recorded in patients with Brugada syndrome [197].
While the available data, both basic and clinical, point to the repolarization hypothesis, i.e., transmural voltage gradients that develop secondary to accentuation of the epicardial notch, at times leading to loss of the action potential dome, as the predominant mechanism underlying the Brugada syndrome ECG signature and arrhythmogenesis, there is no doubt that in some cases, particularly those associated with sodium channel loss of function, conduction slowing may contribute to the development of arrhythmias. There are also likely to be cases in which a conduction defect may predominate [198, 199].
Parasympathetic agonists like acetylcholine facilitate loss of the action potential dome [200] by suppressing ICa and/or augmenting potassium current. β(beta)-adrenergic agonists restore the dome by augmenting ICa. Sodium channel blockers also facilitate loss of the canine right ventricular action potential dome via a negative shift in the voltage at which phase 1 begins [2, 3]. These findings are consistent with accentuation of ST segment elevation in patients with the Brugada syndrome following vagal maneuvers or Class I antiarrhythmic agents as well as normalization of the ST segment elevation following β(beta) adrenergic agents and phosphodiesterase III inhibitors [4, 5, 201]. Loss of the action potential dome is more readily induced in right vs. left canine ventricular epicardium [127, 161, 202] because of the more prominent Ito-mediated phase 1 in action potentials in this region of the heart. This distinction is believed to be the basis for why the Brugada syndrome is a right ventricular disease.
T Wave Alternans
T wave alternans (TWA) is characterized by beat to beat alteration in the amplitude, polarity and/or morphology of the electrocardiographic T wave. TWA has been reported in patients with the Brugada syndrome (BS) and is thought to be associated with an increased risk for development of VT/VF [158, 203–209]. Experimental studies suggest that T wave alternans is due to at least two cellular mechanism, including: (1) loss of the epicardial action potential dome on alternate beats (Fig. 29.4) and (2) concealed phase 2 reentry on alternating beats (Fig. 29.5) [157, 210–212]. T wave alternans developing after administration of sodium channel blockers has also been associated with a high risk of clinical VT/VF in patients with BrS [213].
Verapamil (1 μM)-induced loss of the epicardial action potential dome in alternate beats causes T wave alternans in a canine arterially-perfused right ventricular wedge preparation. (a) At a BCL of 2,000 ms, endocardial and epicardial action potentials repolarize almost simultaneously, generating little or no T wave on the ECG. (b) Decreasing the cycle length to 900 ms induces heterogeneous loss of the epicardial action potential dome in alternate beats while the endocardial response remains constant, resulting in profound T wave alternans. (c) Decreasing the cycle length to 600 ms leads to homogeneous loss of the action potential dome on all beats, leading to ST segment elevation but no T wave alternans in the ECG (Modified from Fish and Antzelevitch [210], with permission from John Wiley and Sons)
Verapamil (1 μM)-induced concealed phase 2 reentry in alternate beats leading to T wave alternans in the coronary-perfused right ventricular wedge preparation. (a) T wave alternans occurs as a result of concealed phase 2 reentry. The dome propagates from Epi 1 to Epi 2 on alternating beats while the endocardial response remains constant. The concealed phase 2 reentry results in a negative T wave. BCL = 558 ms. (b) Increasing the cycle length to 600 ms exaggerates the T wave alternans. The phase relationship between Epi 1, Epi 2, and Endo shifts slightly, allowing the previously concealed phase 2 reentry to propagate transmurally, leading to two extrasystoles. (c) The ST segment elevation, measured 50 ms after the end of the QRS, is greater during alternans secondary to concealed phase 2 reentry compared to alternans due to alternating loss of the epicardial action potential dome (n = 10 phase 2 reentry + and 12 phase 2 reentry – episodes, *p = 0.027). (d) The size of the epicardial action potential notch magnitude (ph2 amp – ph1 amp/ph 2 amp) at BCL 2,000 ms during control was significantly smaller in preparations not displaying phase 2 reentry-induced arrhythmias versus those that did (n = 5 for each category, *p = 0.025) (Modified from Fish and Antzelevitch [210], with permission from John Wiley and Sons)
Acquired Forms of Brugada Syndrome and Modulating Factors
The electrocardiographic and arrhythmic manifestations of the Brugada syndrome can be induced and modulated by a large number of agents and factors. The Brugada ECG can be unmasked or modulated by sodium channel blockers, a febrile state, vagotonic agents, α adrenergic agonists, β adrenergic blockers, tricyclic or tetracyclic antidepressants, first generation antihistaminics (dimenhydrinate), a combination of glucose and insulin, hyperkalemia, hypokalemia, hypercalcemia, and by alcohol and cocaine toxicity (Fig. 29.6) [5, 21, 22, 214–221]. These agents may also induce acquired forms of the Brugada syndrome (Table 29.2). An up-to-date list of agents to avoid in Brugada syndrome can be found at www.BrugadaDrugs.org.
Factors predisposing to the electrocardiographic and arrhythmic manifestations of the Brugada syndrome (From Antzelevitch and Viskin [86]. Reprinted with permission from Springer)
Myocardial infarction or acute ischemia due to vasospasm involving the RVOT mimics ST-segment elevation similar to that seen in Brugada syndrome. This effect is secondary to the depression of ICa, inactivation of INa and the activation of IK-ATP during ischemia, and suggests that patients with congenital and possibly acquired forms of Brugada syndrome may be at a higher risk for ischemia-related sudden cardiac death [253, 255]. Although the coexistence of Brugada syndrome and vasospastic angina in the same patient is not rare, Chinushi et al. have failed to observe an enhanced susceptibility to VF nor a proarrhythmic effect of Ca-antagonist in this setting [256].
Hypokalemia has been suggested to be a contributing factor in the high prevalence of Sudden unexpected nocturnal death syndrome (SUDS) in the Northeastern region of Thailand where potassium deficiency is endemic [220, 257]. Serum potassium in the Northeastern population is significantly lower than that of the population in Bangkok, which lies in the central part of Thailand where potassium is abundant in the food. Hypokalemia has been reported to induce VF in a 60 year old man who had asymptomatic Brugada syndrome, without a family history of sudden cardiac death [220]. This patient was initially treated for asthma by steroids, which lowered serum potassium from 3.8 mM on admission to 3.4 and 2.9 mM on the 7th day and 8th day of admission, respectively. Both were associated with unconsciousness. VF was documented during the last episode, which reverted spontaneously to sinus rhythm. Hypokalemia may exert these effects by increasing the chemical gradient for K+ and thus the intensity of Ito.
VT/VF and sudden death in the Brugada syndrome usually occur at rest and at night. Circadian variation of sympatho-vagal balance, hormones and other metabolic factors are likely to contribute to this circadian pattern. Bradycardia, due to altered sympatho-vagal balance or other factors, may contribute to arrhythmia initiation [26, 54, 55]. Abnormal 123I-MIBG uptake in 8 (17 %) of the 17 Brugada syndrome patients but none in the control group was demonstrated by Wichter et al. [258]. Segmental reduction of 123I-MIBG in the inferior and the septal left ventricular wall was observed indicating presynaptic sympathetic dysfunction. Of note, imaging of the right ventricle, particularly the RVOT, is difficult with this technique, so that insufficient information is available concerning sympathetic function in the regions known to harbor the arrhythmogenic substrate. Moreover, it remains unclear what role the reduced uptake function plays in the arrhythmogenesis of the Brugada syndrome. If the RVOT is similarly affected, this defect may indeed alter the sympatho-vagal balance in favor of the development of an arrhythmogenic substrate [154, 200].
The Thai Ministry of Public Health Report (1990) found an association between a large meal on the night of death in Sudden unexplained nocturnal death syndrome (SUNDS) patients [257]. Consistent with this observation, a recent study by Nogami et al. found that glucose and insulin could unmask the Brugada ECG [219]. Another possibility is that sudden death in these patients is due to the increased vagal tone produced by the stomach distention. A recent study by Ikeda et al. [24] has shown that a full stomach after a large meal can unmask a Type I ECG, particularly in Brugada syndrome patients at high risks for arrhythmic events, thus suggesting that this technique may be of diagnostic and prognostic value.
Accelerated inactivation of the sodium channel caused by SCN5A mutations associated with the Brugada syndrome has been shown to be accentuated at higher temperatures [94] suggesting that a febrile state may unmask the Brugada syndrome. Indeed, several case reports have emerged recently demonstrating that febrile illness could reveal the Brugada ECG and precipitate VF [23, 95, 96, 259–261]. A report from Keller et al. [262] has identified a missense mutation, F1344S, in SCN5A in a patient with Brugada syndrome and fever-induced VT/VF. Expression of F1344S showed a shift in the voltage-dependence of activation, which was further accentuated at high temperatures mimicking fever. Thus fever may also cause a loss of function in INa by accelerating inactivation as well as producing a shift in the voltage-dependence of activation.
Anecdotal data point to hot baths as a possible precipitating factor. Of note, the Northeastern part of Thailand, where the Brugada syndrome is most prevalent, is known for its very hot climate. A study is underway to assess whether this extreme climate influences the prognosis of the disease.
Sex-Related Differences in the Manifestation of the Brugada Syndrome
Although the mutation responsible for the Brugada syndrome is equally distributed between the sexes, the clinical phenotype is eight to ten times more prevalent in males than in females. The basis for this sex-related distinction has been shown to be due to a more prominent Ito-mediated action potential notch in the right ventricular (RV) epicardium of males vs. females (Figs. 29.7 and 29.8) [263]. The more prominent Ito causes the end of phase 1 of the RV epicardial action potential to repolarize to more negative potentials in tissues and arterially perfused wedge preparations from males, facilitating loss of the action potential dome and the development of phase 2 reentry and polymorphic VT.
Sex-based and inter-ventricular differences in Ito. (a) Mean I-V relationship for Ito recorded from RV epicardial cells isolated from hearts of male and female dogs. Inset: Representative Ito current traces and voltage protocol. Ito density was significantly greater in male vs female RV epicardial cells. No sex differences were observed in LV. (b) Transmembrane action potentials recorded from isolated canine RV epicardial male and female tissue slices. BCLs 300, 500, 800, and 2,000 ms. (c) Rate dependence of phase 1 amplitude and voltage at end of phase 1 (V/phase 1, mV) in males (solid squares) vs females (solid circles) (Modified from Di Diego et al. [263] with permission from Wolters Kluwer Health)
Terfenadine induces Brugada phenotype more readily in male than female RV wedge preparations. Each panel shows action potentials recorded from two epicardial sites and one endocardial site, together with a transmural ECG. Control recordings were obtained at a BCL of 2,000 ms, whereas terfenadine data were recorded at a BCL of 800 ms after a brief period of pacing at a BCL of 400 ms. (a) Terfenadine (5 uM)-induced, heterogeneous loss of action potential dome, ST-segment elevation, and phase 2 reentry (arrow) in a male RV wedge preparation. (b) Terfenadine fails to induce Brugada phenotype in a female RV wedge preparation. (c) Polymorphic VT triggered by spontaneous phase 2 reentry in a male preparation. (d) Incidence of phase 2 reentry in male (six of seven) vs female (two of seven) RV wedge preparations when perfused with 5 uM terfenadine for up to 2 h (Modified from Di Diego et al. [263], with permission from Wolters Kluwer Health)
Clinical and basic studies suggest that testosterone plays an important role in ventricular repolarization. Ezaki and co-workers [264] recently demonstrated that ST segment elevation is relatively small and similar in males and females before puberty. After puberty, ST segment elevation in males, but not females, increased dramatically, more so in the right precordial leads and decreased gradually with advancing age. The effect of androgen-deprivation therapy on the ST segment was also evaluated in 21 prostate cancer patients. Androgen-deprivation therapy significantly decreased ST segment elevation. These results suggest that testosterone modulates the early phase of ventricular repolarization and thus ST segment elevation.
The proposed cellular mechanism for the Brugada syndrome is summarized in Fig. 29.9. Available data support the hypothesis that the Brugada syndrome results from amplification of heterogeneities intrinsic to the early phases of the action potential among the different transmural cell types. This amplification is secondary to a rebalancing of currents active during phase 1, including a decrease in INa or ICa or augmentation of any one of a number of outward currents. ST segment elevation similar to that observed in patients with the Brugada syndrome occurs as a consequence of the accentuation of the action potential notch, eventually leading to loss of the action potential dome in right ventricular epicardium, where Ito is most prominent. Loss of the dome gives rise to both a transmural as well as epicardial dispersion of repolarization. The transmural dispersion is responsible for the development of ST segment elevation and the creation of a vulnerable window across the ventricular wall, whereas the epicardial dispersion give to phase 2 reentry which provides the extrasystole that captures the vulnerable window, thus precipitating VT/VF. The VT generated is usually polymorphic, resembling a very rapid form of Torsade de Pointes.
Proposed mechanism for the Brugada syndrome. A shift in the balance of currents serves to amplify existing heterogeneities by causing loss of the action potential dome at some epicardial, but not endocardial sites. A vulnerable window develops as a result of the dispersion of repolarization and refractoriness within epicardium as well as across the wall. Epicardial dispersion leads to the development of phase 2 reentry, which provides the extrasystole that captures the vulnerable window and initiates VT/VF via a circus movement reentry mechanism (Modified from Antzelevitch [265], with permission from Oxford University Press)
Approach to Therapy
Device Therapy
The only proven effective therapy for the Brugada syndrome is an implantable cardioverter defibrillator (ICD) (Table 29.3) [266, 283]. Recommendations for ICD implantation from the Second Consensus Conference [9, 10] are presented in Fig. 29.10 and are summarized as follows:
Indications for ICD implantation in patients with the Brugada syndrome. BS Brugada syndrome, EPS electrophysiologic study, NAR nocturnal agonal respiration, SCD sudden cardiac death (From Antzelevitch et al. [10] with permission from Wolters Kluwer Health. From Antzelevitch et al. [9] with permission from Elsevier Limited)
-
1.
Symptomatic patients with a Type 1 ST segment elevation or Brugada ECG (either spontaneously or after sodium channel blockade) who present with aborted sudden death should receive an ICD as a Class I indication without additional need for electrophysiologic study (EPS). Similar patients presenting with related symptoms such as syncope, seizure or nocturnal agonal respiration should also undergo ICD implantation as a Class I indication after vasovagal syncope has been excluded on clinical grounds and non-cardiac causes of these symptoms have been carefully ruled out. The Task Force recommended that symptomatic patients undergo EPS only for the assessment of supraventricular arrhythmia. Electrophysiologic studies to guide quinidine therapy (that is, demonstrating that readily inducible VF at baseline becomes non-inducible after quinidine therapy) may be considered for symptomatic patients unwilling or financially incapable of undergoing ICD implantation [274].
-
2.
The recommendation at the time was that asymptomatic patients with a Brugada ECG (spontaneously or after sodium channel block) should undergo EPS if there is a family history of sudden cardiac death suspected to be due to Brugada syndrome. EPS was thought to be justified when the family history is negative for sudden cardiac death if the Type 1 ST segment elevation occurs spontaneously. If inducible for ventricular arrhythmia, an ICD was recommended as a Class IIa indication for patients presenting with a spontaneous Type I ST segment elevation and as a Class IIb for patients who display a Type I ST segment elevation only after sodium block challenge. More recent data have called these recommendations into question and suggest that it might be more appropriate to consider both as Class IIb indications. As discussed above, recent data seriously challenge the prognostic value of EPS for asymptomatic patients, calling for modification of these recommendations.
Although ICD implantation is the mainstay of therapy for the Brugada syndrome, implantation can be challenging in infants and is not an adequate solution for patients residing in regions of the world where an ICD is unaffordable. Also, ICD implantation in “asymptomatic high-risk patients” is not trivial, especially because the level of risk is still being debated (see Sect. “Prognosis and Risk Stratification” above). One should recall that in the Antiarrhythmics vs Implantable Defibrillators (AVID) trial, a multicenter study of ICD implantation for patients with heart disease and malignant arrhythmias, the risk for ICD-related complications serious enough to warrant re-intervention was 12 % [284]. The rate of serious complications from ICD implantation for patients with Brugada syndrome is likely to be higher than the 12 % reported for the patients in AVID, who were relatively old (65 ± 11 years) and had a 3-year mortality rate of 25 % [285]. Patients with Brugada syndrome are younger, have a very low risk for non-arrhythmic cardiac death and will remain at risk for ICD-related complications for many more years. In particular, the risk for potentially serious complications like infection or lead-insulation break leading to inappropriate ICD shocks, will increase over the years and after repeated ICD replacements. Indeed, Sacher et al. [286] reported a 28 % rate (8 % per year) of serious complications, including a 20 % risk of inappropriate shocks, in young patients with Brugada syndrome. Therefore, although the ICD represents the most effective way to prevent arrhythmic death in Brugada syndrome, pharmacologic and other solutions may be desirable as an alternative to device therapy for select cases [275] as well as for minimizing the firing of the ICD in patients with frequent events [9, 275, 287, 288].
Although arrhythmias and sudden cardiac death generally occur during sleep or at rest and have been associated with slow heart rates, a potential therapeutic role for cardiac pacing remains largely unexplored [289].
Radiofrequency Ablation Therapy
Data concerning ablation therapy for BrS is very limited. Haissaguerre and co-workers [267] reported that focal radiofrequency ablation aimed at eliminating the ventricular premature beats that trigger VT/VF in the Brugada syndrome may be useful in controlling arrhythmogenesis. Haissaguerre also reported that regional endocardial ablation of RVOT areas normalizes the type I electrocardiogram in anecdotal cases [290].
The most extensive ablation study thus far reported involves 9 BrS patients with recurrent VF [166]. Electroanatomic mapping revealed fractionated late potentials in the anterior aspect of the RVOT epicardium. Ablation at these sites rendered VT/VF noninducible in seven of nine patients and normalization of the Brugada ECG pattern. Long-term outcomes (20 ± 6 months) were excellent, with no recurrent VT/VF in all patients. This report awaits confirmation by future studies.
Pharmacological Therapy
Because the mechanism underlying most cases of BrS, is thought to be due an net outward shift of the balance of current during the early phases of the action potential, the search for a pharmacologic treatment has been focused on rebalancing of the ion channel current active during the early phases of the epicardial action potential in the right ventricle so as to reduce the magnitude of the action potential notch and/or restore the action potential dome. Table 29.3 lists the various pharmacologic agents thus far investigated. Antiarrhythmic agents such as amiodarone and β blockers have been shown to be ineffective [75]. Class IC antiarrhythmic drugs (such as flecainide and propafenone) and Class IA agents, such as procainamide, are contraindicated because of their effects to unmask the Brugada syndrome and induce arrhythmogenesis. Disopyramide is a Class IA antiarrhythmic that has been demonstrated to normalize ST segment elevation in some Brugada patients but to unmask the syndrome in others [269].
The presence of a prominent Ito is fundamental to the mechanism underlying the Brugada syndrome. Consequently, the most prudent general approach to therapy, regardless of the ionic or genetic basis for the disease, is to partially inhibit Ito. Cardioselective and Ito-specific blockers are not currently available. 4-aminopyridine (4-AP) is an agent that is ion-channel specific at low concentrations, but is not cardioselective in that it inhibits Ito in the nervous system. Although it is effective in suppressing arrhythmogenesis in wedge models of the Brugada syndrome (Fig. 29.11) [154], it is unlikely to be of clinical benefit because of neurally-mediated adverse effects.
Effects of Ito blockers 4-AP and quinidine on pinacidil induced phase 2 reentry and VT in the arterially perfused RV wedge preparation. In both examples, 2.5 mM pinacidil produced heterogeneous loss of AP dome in epicardium, resulting in ST-segment elevation, phase 2 reentry, and VT (left); 4-AP (a) and quinidine (b) restored epicardial AP dome, reduced both transmural and epicardial dispersion of repolarization, normalized the ST segment, and prevented phase 2 reentry and VT in continued presence of pinacidil (From Yan and Antzelevitch [154], with permission from Wolters Kluwer Health)
Quinidine is an agent currently on the market in the United States and other regions of the world with significant Ito blocking properties. Accordingly, we suggested several years ago that this agent may be of therapeutic value in the Brugada syndrome [291]. Quinidine has been shown to be effective in restoring the epicardial action potential dome, thus normalizing the ST segment and preventing phase 2 reentry and polymorphic VT in experimental models of the Brugada syndrome (Fig. 29.11) [154, 292, 293]. Clinical evidence of the effectiveness of quinidine in normalizing ST segment elevation in patients with the Brugada syndrome has been reported as well [184, 273, 275, 294]. Quinidine has also been reported to be effective in suppressing arrhythmogenesis in an infant too young to receive an ICD [63].
In a prospective study of 25 Brugada syndrome patients orally administered quinidine bisulfate (1,483 ± 240 mg), Belhassen and co-workers [184] evaluated the effectiveness of quinidine in preventing inducible and spontaneous ventricular fibrillation (VF). There were 15 symptomatic patients (7 cardiac arrest survivors and 7 with unexplained syncope) and 10 asymptomatic patients. All 25 patients had inducible VF at baseline electrophysiological study. Quinidine prevented VF induction in 22 of the 25 patients (88 %). After a follow-up period of 6 months to 22.2 years, all patients were alive. Of nineteen patients treated with oral quinidine (without ICD back-up) for 6–219 months (56 ± 67 months), none developed arrhythmic events. Administration of quinidine was associated with a 36 % incidence of side effects, principally diarrhea, which resolved after drug discontinuation. The authors concluded that quinidine effectively suppresses VF induction as well as spontaneous arrhythmias in patients with Brugada syndrome and may be useful as an adjunct to ICD therapy. They also suggested that EPS-guided quinidine therapy may be used as an alternative to ICD in cases in which an ICD is refused or unaffordable as well as when patients who are well informed about the risk and benefits of ICD and EP-guided quinidine therapy prefer medical therapy to device implantation [184]. Their results are consistent with those reported by the same group in prior years [274, 275] and more recently by other investigators [276, 277, 294]. A relatively small recent study by Mizusawa et al. [295] also showed that low-dose quinidine (300–600 mg) can prevent electrophysiologic induction of VF and has a potential as an adjunctive therapy for Brugada syndrome in patients with frequent implantable cardioverter defibrillator discharges.
There is a clear need for a large randomized controlled clinical trial to assess the effectiveness of quinidine, preferably in patients with frequent events who have already received an ICD. A prospective registry for empiric quinidine therapy for asymptomatic BrS patients was recently initiated [296]. The registry encourages empiric therapy with hydroquinidine hydrochloride 300 mg twice a day. Lower doses of quinidine have been associated with higher incidence of inducibility of TdP during repeated EPS [295]. These findings are consistent with the biphasic dose-response of quinidine to induce TdP, due to a greater inhibition of IKr with relatively low concentrations and enhanced late INa block at higher concentrations of the drug [297]. A clinical trial evaluating the number of appropriate ICD shocks in Brugada syndrome patients using quinidine vs. placebo has recently been initiated (QUIDAM study).
It is noteworthy that several manufacturer’s of quinidine formulations have opted take these products off the market, prompting pleas for reconsideration of these policies in light of the need for quinidine therapy in Brugada and other syndromes, such as the short QT syndrome [298].
The quest for additional cardioselective and Ito-specific blockers is on-going. Another agent being considered for this purpose is the drug tedisamil. Tedisamil may be more potent than quinidine because it lacks the inward current blocking actions of quinidine, while potently blocking Ito. The effect of tedisamil to suppress phase 2 reentry and VT in a wedge model of the Brugada syndrome is illustrated in Fig. 29.12 [279].
Effects of Ito block with tedisamil to suppress phase 2 reentry induced by terfenadine in an arterially perfused canine RV wedge preparation. (a) Control, BCL 800 ms. (b) Terfenadine (5 μM) induces ST segment elevation as a result of heterogeneous loss of the epicardial action potential dome, leading to phase 2 reentry which triggers an episode of poly VT (BCL = 800 ms). (c) Addition of tedisamil (2 μM) normalizes the ST segment and prevents loss of the epicardial action potential dome and suppresses phase 2 reentry induced and polymorphic VT (BCL = 800 ms) (From Antzelevitch and Fish [288], with permission from Springer)
Tedisamil and quinidine are both capable of suppressing the substrate and trigger for the Brugada syndrome via their inhibition of Ito. Both, however, also block IKr and thus have the potential to induce an acquired form of the long QT syndrome. Thus these agents may substitute one form of polymorphic VT for another, particularly under conditions that promote TdP, such as bradycardia and hypokalemia. However, the majority of patients with Brugada syndrome are otherwise healthy males, for whom the risk of drug-induced Torsade de Pointes is small [299]. This effect of quinidine is minimized at high plasma levels because at these concentrations quinidine block of INa counters the effect of IKr block to increase transmural dispersion of repolarization, the substrate for the development of Torsade de Pointes (TdP) arrhythmias [117, 297, 300, 301]. High doses of quinidine (1,000–1,500 mg/day) are recommended in order to effect Ito block, without inducing TdP.
Another potential therapeutic candidate is an agent reported to be a relatively selective Ito and IKur blocker, AVE0118 [280]. AVE0118 has been shown to normalize the ECG and suppress phase 2 reentry in a wedge model of the Brugada syndrome. This drug has the advantage that it does not block IKr, and therefore does not prolong the QT interval or have the potential to induce TdP. The disadvantage of this particular drug is that it undergoes first-pass hepatic metabolism and is therefore not effective with oral administration.
Drugs that increase the calcium current, such as β adrenergic agents like isoproterenol, are useful as well [154, 201, 302]. Isoproterenol or orciprenaline, sometimes in combination with quinidine, have been shown to be effective in normalizing ST segment elevation in patients with the Brugada syndrome and in controlling electrical storms, particularly in children [43, 271–273, 275, 277, 303, 304]. A new addition to the pharmacological armamentarium is the phosphodiesterase III inhibitor, cilostazol [201, 278], which normalizes the ST segment, most likely by augmenting calcium current (ICa) as well as by reducing Ito secondary to an increase in heart rate.
Another pharmacologic approach is to augment a component of INa that is active during phase 1 of the epicardial action potential. Dimethyl Lithospermate B (dmLSB) is an extract of Danshen, a traditional Chinese herbal remedy, which slows inactivation of INa, but only during a window of time corresponding to the action potential notch. This leads to increased inward current during the early phases of the action potential. Figure 29.13 shows the effectiveness of dmLSB in eliminating the arrhythmogenic substrate responsible for the Brugada syndrome in three different experimental models of the syndrome [282]. The Brugada syndrome phenotype was created in canine arterially-perfused right ventricular wedge preparations using either terfenadine or verapamil to inhibit INa and ICa, or pinacidil to activate IK-ATP. Terfenadine, verapamil, and pinacidil each induced all-or-none repolarization at some epicardial sites but not others, leading to ST-segment elevation as well as an increase in both epicardial and transmural dispersions of repolarization. Under these conditions, phase 2 reentry developed as the epicardial action potential dome propagated from sites where it was maintained to sites at which it was lost, generating closely coupled extrasystoles and VT/VF. Addition of dmLSB (10 μM) to the coronary perfusate restored the epicardial action potential (AP) dome, reduced both epicardial and transmural dispersion of repolarization and abolished phase 2 reentry-induced extrasystoles and VT/VF in 9/9 preparations. Our data suggest that dmLSB may be a candidate for pharmacologic treatment of Brugada syndrome in cases in which an ICD is not feasible or affordable or as an adjunct to ICD use.
Effect of dmLSB to suppress the arrhythmogenic substrate of the Brugada syndrome in three experimental models. Phase 2 reentry was induced in three separate models of the Brugada syndrome. Terfenadine (5 μM, a), verapamil (5 μM, b), or pinacidil (6 μM, c) induce heterogeneous loss of the epicardial action potential dome and ST segment elevation. Phase 2 reentry occurs as the dome is propagated from Epi 1 to Epi 2, triggering either a closely coupled extrasystole or polymorphic ventricular tachycardia. In all three models, addition of dmLSB (10 μM) normalizes the ST segment and abolishes phase 2 reentry and resultant arrhythmias (From Fish et al. [282], with permission from Wolters Kluwer Health)
References
Brugada P, Brugada J. Right bundle branch block, persistent ST segment elevation and sudden cardiac death: a distinct clinical and electrocardiographic syndrome: a multicenter report. J Am Coll Cardiol. 1992;20:1391–6.
Krishnan SC, Antzelevitch C. Sodium channel block produces opposite electrophysiological effects in canine ventricular epicardium and endocardium. Circ Res. 1991;69:277–91.
Krishnan SC, Antzelevitch C. Flecainide-induced arrhythmia in canine ventricular epicardium. Phase 2 reentry? Circulation. 1993;87:562–72.
Yan GX, Antzelevitch C. Cellular basis for the electrocardiographic J wave. Circulation. 1996;93:372–9.
Miyazaki T, Mitamura H, Miyoshi S, Soejima K, Aizawa Y, Ogawa S. Autonomic and antiarrhythmic drug modulation of ST segment elevation in patients with Brugada syndrome. J Am Coll Cardiol. 1996;27:1061–70.
Antzelevitch C. The Brugada syndrome. J Cardiovasc Electrophysiol. 1998;9:513–6.
Wilde AA, Antzelevitch C, Borggrefe M, Brugada J, Brugada R, Brugada P, et al. Proposed diagnostic criteria for the Brugada syndrome. Eur Heart J. 2002;23:1648–54.
Wilde AA, Antzelevitch C, Borggrefe M, Brugada J, Brugada R, Brugada P, et al. Proposed diagnostic criteria for the Brugada syndrome: consensus report. Circulation. 2002;106:2514–9.
Antzelevitch C, Brugada P, Borggrefe M, Brugada J, Brugada R, Corrado D, et al. Brugada syndrome: report of the second consensus conference: endorsed by the Heart Rhythm Society and the European Heart Rhythm Association. Circulation. 2005;111:659–70.
Antzelevitch C, Brugada P, Borggrefe M, Brugada J, Brugada R, Corrado D, et al. Brugada syndrome: report of the second consensus conference. Heart Rhythm. 2005;2:429–40.
Viskin S, Rogowski O. Asymptomatic Brugada syndrome: a cardiac ticking time-bomb? Europace. 2007;9:707–10.
Wilde AA, Viskin S. EP testing does not predict cardiac events in Brugada syndrome. Heart Rhythm. 2011;8:1598–600.
Wilde AA, Viskin S. Rebuttal to EP testing predicts cardiac events in patients with Brugada syndrome. Heart Rhythm. 2011;8:1797.
Brugada J, Brugada R, Brugada P. Electrophysiologic testing predicts events in Brugada syndrome patients. Heart Rhythm. 2011;8:1595–7.
Brugada J, Brugada R, Brugada P. Rebuttal to EP testing does not predict cardiac events in patients with Brugada syndrome. Heart Rhythm. 2011;8:1796.
Hermida JS, Lemoine JL, Aoun FB, Jarry G, Rey JL, Quiret JC. Prevalence of the Brugada syndrome in an apparently healthy population. Am J Cardiol. 2000;86:91–4.
Miyasaka Y, Tsuji H, Yamada K, Tokunaga S, Saito D, Imuro Y, et al. Prevalence and mortality of the Brugada-type electrocardiogram in one city in Japan. J Am Coll Cardiol. 2001;38:771–4.
Holst AG, Jensen HK, Eschen O, Henriksen FL, Kanters J, Bundgaard H, et al. Low disease prevalence and inappropriate implantable cardioverter defibrillator shock rate in Brugada syndrome: a nationwide study. Europace. 2012;14:1025–9.
Antzelevitch C. Brugada syndrome. Pacing Clin Electrophysiol. 2006;29:1130–59.
Brugada P, Brugada J, Brugada R. The Brugada syndrome. Card Electrophysiol Rev. 2002;6:45–8.
Brugada P, Brugada J, Brugada R. Arrhythmia induction by antiarrhythmic drugs. Pacing Clin Electrophysiol. 2000;23:291–2.
Brugada R, Brugada J, Antzelevitch C, Kirsch GE, Potenza D, Towbin JA, et al. Sodium channel blockers identify risk for sudden death in patients with ST-segment elevation and right bundle branch block but structurally normal hearts. Circulation. 2000;101:510–5.
Antzelevitch C, Brugada R. Fever and the Brugada syndrome. Pacing Clin Electrophysiol. 2002;25:1537–9.
Ikeda T, Abe A, Yusa S, Nakamura K, Ishiguro H, Mera H, et al. The full stomach test as a novel diagnostic technique for identifying patients at risk for Brugada syndrome. J Cardiovasc Electrophysiol. 2006;17:602–7.
Makimoto H, Nakagawa E, Takaki H, Yamada Y, Okamura H, Noda T, et al. Augmented ST-segment elevation during recovery from exercise predicts cardiac events in patients with Brugada syndrome. J Am Coll Cardiol. 2010;56:1576–84.
Mizumaki K, Fujiki A, Tsuneda T, Sakabe M, Nishida K, Sugao M, et al. Vagal activity modulates spontaneous augmentation of ST elevation in daily life of patients with Brugada syndrome. J Cardiovasc Electrophysiol. 2004;15:667–73.
Morita H, Zipes DP, Morita ST, Wu J. Temperature modulation of ventricular arrhythmogenicity in a canine tissue model of Brugada syndrome. Heart Rhythm. 2007;4:188–97.
Take Y, Morita H, Wu J, Nagase S, Morita S, Toh N, et al. Spontaneous electrocardiogram alterations predict ventricular fibrillation in Brugada syndrome. Heart Rhythm. 2011;8:1014–21.
Richter S, Sarkozy A, Veltmann C, Chierchia GB, Boussy T, Wolpert C, et al. Variability of the diagnostic ECG pattern in an ICD patient population with Brugada syndrome. J Cardiovasc Electrophysiol. 2009;20:69–75.
Richter S, Sarkozy A, Paparella G, Henkens S, Boussy T, Chierchia GB, et al. Number of electrocardiogram leads displaying the diagnostic coved-type pattern in Brugada syndrome: a diagnostic consensus criterion to be revised. Eur Heart J. 2010;31:1357–64.
Shimizu W, Antzelevitch C, Suyama K, Kurita T, Taguchi A, Aihara N, et al. Effect of sodium channel blockers on ST segment, QRS duration, and corrected QT interval in patients with Brugada syndrome. J Cardiovasc Electrophysiol. 2000;11:1320–9.
Priori SG, Napolitano C, Gasparini M, Pappone C, Della BP, Brignole M, et al. Clinical and genetic heterogeneity of right bundle branch block and ST-segment elevation syndrome: a prospective evaluation of 52 families. Circulation. 2000;102:2509–15.
Wolpert C, Echternach C, Veltmann C, Antzelevitch C, Thomas GP, Sphel S, et al. Intravenous drug challenge using flecainide and ajmaline in patients with Brugada syndrome. Heart Rhythm. 2005;2:254–60.
Hong K, Brugada J, Oliva A, Berruezo-Sanchez A, Potenza D, Pollevick GD, et al. Value of electrocardiographic parameters and ajmaline test in the diagnosis of Brugada syndrome caused by SCN5A mutations. Circulation. 2004;110:3023–7.
Itoh H, Shimizu M, Takata S, Mabuchi H, Imoto K. A novel missense mutation in the SCN5A gene associated with Brugada syndrome bidirectionally affecting blocking actions of antiarrhythmic drugs. J Cardiovasc Electrophysiol. 2005;16:486–93.
Kalla H, Yan GX, Marinchak R. Ventricular fibrillation in a patient with prominent J (Osborn) waves and ST segment elevation in the inferior electrocardiographic leads: a Brugada syndrome variant? J Cardiovasc Electrophysiol. 2000;11:95–8.
Ogawa M, Kumagai K, Yamanouchi Y, Saku K. Spontaneous onset of ventricular fibrillation in Brugada syndrome with J wave and ST-segment elevation in the inferior leads. Heart Rhythm. 2005;2:97–9.
Horigome H, Shigeta O, Kuga K, Isobe T, Sakakibara Y, Yamaguchi I, et al. Ventricular fibrillation during anesthesia in association with J waves in the left precordial leads in a child with coarctation of the aorta. J Electrocardiol. 2003;36:339–43.
Kamakura S, Ohe T, Nakazawa K, Aizawa Y, Shimizu A, Horie M, et al. Long-term prognosis of probands with Brugada-pattern ST-elevation in leads V1-V3. Circ Arrhythm Electrophysiol. 2009;2:495–503.
Nam GB, Kim YH, Antzelevitch C. Augmentation of J waves and electrical storms in patients with early repolarization. N Engl J Med. 2008;358:2078–9.
Nam GB, Ko KH, Kim J, Park KM, Rhee KS, Choi KJ, et al. Mode of onset of ventricular fibrillation in patients with early repolarization pattern vs. Brugada syndrome. Eur Heart J. 2010;31:330–9.
Antzelevitch C, Yan GX. J wave syndromes. Heart Rhythm. 2010;7:549–58.
Shimizu W, Matsuo K, Takagi M, Tanabe Y, Aiba T, Taguchi A, et al. Body surface distribution and response to drugs of ST segment elevation in Brugada syndrome: clinical implication of eighty-seven-lead body surface potential mapping and its application to twelve-lead electrocardiograms. J Cardiovasc Electrophysiol. 2000;11:396–404.
Sangwatanaroj S, Prechawat S, Sunsaneewitayakul B, Sitthisook S, Tosukhowong P, Tungsanga K. New electrocardiographic leads and the procainamide test for the detection of the Brugada sign in sudden unexplained death syndrome survivors and their relatives. Eur Heart J. 2001;22:2290–6.
Shimeno K, Takagi M, Maeda K, Tatsumi H, Doi A, Yoshiyama M. Usefulness of multichannel Holter ECG recording in the third intercostal space for detecting type 1 Brugada ECG: comparison with repeated 12-lead ECGs. J Cardiovasc Electrophysiol. 2009;20:1026–31.
Shin SC, Ryu S, Lee JH, Chang BJ, Shin JK, Kim HS, et al. Prevalence of the Brugada-type ECG recorded from higher intercostal spaces in healthy Korean males. Circ J. 2005;69:1064–7.
Alings M, Wilde A. “Brugada” syndrome: clinical data and suggested pathophysiological mechanism. Circulation. 1999;99:666–73.
Bezzina C, Veldkamp MW, van Den Berg MP, Postma AV, Rook MB, Viersma JW, et al. A single Na+ channel mutation causing both long-QT and Brugada syndromes. Circ Res. 1999;85:1206–13.
Pitzalis MV, Anaclerio M, Iacoviello M, Forleo C, Guida P, Troccoli R, et al. QT-interval prolongation in right precordial leads: an additional electrocardiographic hallmark of Brugada syndrome. J Am Coll Cardiol. 2003;42:1632–7.
Castro Hevia J, Antzelevitch C, Tornés Bárzaga F, Dorantes Sánchez M, Dorticós Balea F, Zayas Molina R, et al. Tpeak-Tend and Tpeak-Tend dispersion as risk factors for ventricular tachycardia/ventricular fibrillation in patients with the Brugada syndrome. J Am Coll Cardiol. 2006;47:1828–34.
Smits JP, Eckardt L, Probst V, Bezzina CR, Schott JJ, Remme CA, et al. Genotype-phenotype relationship in Brugada syndrome: electrocardiographic features differentiate SCN5A-related patients from non-SCN5A-related patients. J Am Coll Cardiol. 2002;40:350–6.
Morita H, Kusano KF, Miura D, Nagase S, Nakamura K, Morita ST, et al. Fragmented QRS as a marker of conduction abnormality and a predictor of prognosis of Brugada syndrome. Circulation. 2008;118:1697–704.
Priori SG, Gasparini M, Napolitano C, Della BP, Ottonelli AG, Sassone B, et al. Risk stratification in Brugada syndrome: results of the PRELUDE (PRogrammed ELectrical stimUlation preDictive valuE) registry. J Am Coll Cardiol. 2012;59:37–45.
Kasanuki H, Ohnishi S, Ohtuka M, Matsuda N, Nirei T, Isogai R, et al. Idiopathic ventricular fibrillation induced with vagal activity in patients without obvious heart disease. Circulation. 1997;95:2277–85.
Proclemer A, Facchin D, Feruglio GA, Nucifora R. Recurrent ventricular fibrillation, right bundle-branch block and persistent ST segment elevation in V1-V3: a new arrhythmia syndrome? A clinical case report. G Ital Cardiol. 1993;23:1211–8.
Makiyama T, Akao M, Tsuji K, Doi T, Ohno S, Takenaka K, et al. High risk for bradyarrhythmic complications in patients with Brugada syndrome caused by SCN5A gene mutations. J Am Coll Cardiol. 2005;46:2100–6.
Scornik FS, Desai M, Brugada R, Guerchicoff A, Pollevick GD, Antzelevitch C, et al. Functional expression of “cardiac-type” Nav1.5 sodium channel in canine intracardiac ganglia. Heart Rhythm. 2006;3:842–50.
Patruno N, Pontillo D. Brugada syndrome and vasovagal syncope. Pacing Clin Electrophysiol. 2006;29:215.
Shimada M, Miyazaki T, Miyoshi S, Soejima K, Hori S, Mitamura H, et al. Sustained monomorphic ventricular tachycardia in a patient with Brugada syndrome. Jpn Circ J. 1996;60:364–70.
Pinar BE, Garcia-Alberola A, Martinez SJ, Sanchez Munoz JJ, Valdes CM. Spontaneous sustained monomorphic ventricular tachycardia after administration of ajmaline in a patient with Brugada syndrome. Pacing Clin Electrophysiol. 2000;23:407–9.
Dinckal MH, Davutoglu V, Akdemir I, Soydinc S, Kirilmaz A, Aksoy M. Incessant monomorphic ventricular tachycardia during febrile illness in a patient with Brugada syndrome: fatal electrical storm. Europace. 2003;5:257–61.
Mok NS, Chan NY. Brugada syndrome presenting with sustained monomorphic ventricular tachycardia. Int J Cardiol. 2004;97:307–9.
Probst V, Evain S, Gournay V, Marie A, Schott JJ, Boisseau P, et al. Monomorphic ventricular tachycardia due to brugada syndrome successfully treated by hydroquinidine therapy in a 3-year-old child. J Cardiovasc Electrophysiol. 2006;17:97–100.
Sastry BK, Narasimhan C, Soma Raju B. Brugada syndrome with monomorphic ventricular tachycardia in a one-year-old child. Indian Heart J. 2001;53:203–5.
Remme CA, Wever EFD, Wilde AAM, Derksen R, Hauer RNW. Diagnosis and long-term follow-up of Brugada syndrome in patients with idiopathic ventricular fibrillation. Eur Heart J. 2001;22:400–9.
Brugada J, Brugada R, Antzelevitch C, Towbin J, Nademanee K, Brugada P. Long-term follow-up of individuals with the electrocardiographic pattern of right bundle-branch block and ST-segment elevation in precordial leads V1 to V3. Circulation. 2002;105:73–8.
Priori SG, Napolitano C, Gasparini M, Pappone C, Della BP, Giordano U, et al. Natural history of Brugada syndrome: insights for risk stratification and management. Circulation. 2002;105:1342–7.
Brugada P, Brugada R, Brugada J. Patients with an asymptomatic Brugada electrocardiogram should undergo pharmacological and electrophysical testing. Circulation. 2005;112:279–85.
Priori SG, Napolitano C. Management of Patients with Brugada syndrome should not be based on programmed electrical stimulation. Circulation. 2005;112:285–91.
Eckardt L, Probst V, Smits JP, Bahr ES, Wolpert C, Schimpf R, et al. Long-term prognosis of individuals with right precordial ST-segment-elevation Brugada syndrome. Circulation. 2005;111:257–63.
Atarashi H, Ogawa S, Idiopathic Ventricular Fibrillation Investigators. New ECG criteria for high-risk Brugada syndrome. Circ J. 2003;67:8–10.
Junttila MJ, Brugada P, Hong K, Lizotte E, de Zutter M, Sarkozy A, et al. Differences in 12-lead electrocardiogram between symptomatic and asymptomatic Brugada syndrome patients. J Cardiovasc Electrophysiol. 2008;19:380–3.
Morita H, Takenaka-Morita S, Fukushima-Kusano K, Kobayashi M, Nagase S, Kakishita M, et al. Risk stratification for asymptomatic patients with brugada syndrome. Circ J. 2003;67:312–6.
Viskin S. Inducible ventricular fibrillation in the Brugada syndrome: diagnostic and prognostic implications. J Cardiovasc Electrophysiol. 2003;14:458–60.
Brugada J, Brugada R, Brugada P. Right bundle-branch block and ST-segment elevation in leads V1 through V3. A marker for sudden death in patients without demonstrable structural heart disease. Circulation. 1998;97:457–60.
Kanda M, Shimizu W, Matsuo K, Nagaya N, Taguchi A, Suyama K, et al. Electrophysiologic characteristics and implications of induced ventricular fibrillation in symptomatic patients with Brugada syndrome. J Am Coll Cardiol. 2002;39:1799–805.
Brugada J, Brugada R, Brugada P. Determinants of sudden cardiac death in individuals with the electrocardiographic pattern of Brugada syndrome and no previous cardiac arrest. Circulation. 2003;108:3092–6.
Eckardt L, Kirchhof P, Johna R, Haverkamp W, Breithardt G, Borggrefe M. Wolff-Parkinson-White syndrome associated with Brugada syndrome. Pacing Clin Electrophysiol. 2001;24:1423–4.
Carlsson J, Erdogan A, Schulte B, Neuzner J, Pitschner HF. Possible role of epicardial left ventricular programmed stimulation in Brugada syndrome. Pacing Clin Electrophysiol. 2001;24:247–9.
Gehi AK, Duong TD, Metz LD, Gomes JA, Mehta D. Risk stratification of individuals with the brugada electrocardiogram: a meta-analysis. J Cardiovasc Electrophysiol. 2006;17:577–83.
Paul M, Gerss J, Schulze-Bahr E, Wichter T, Vahlhaus C, Wilde AA, et al. Role of programmed ventricular stimulation in patients with Brugada syndrome: a meta-analysis of worldwide published data. Eur Heart J. 2007;28:2126–33.
Yamagata K, Horie M, Ogawa S, Aizawa Y, Kusano KF, Ohe T, et al. Clinical phenotype and prognosis of probands with Brugada syndrome in relation to SCN5A mutation Japanese Brugada Syndrome Multicenter Registry. Circulation. 2009;120:S697.
Probst V, Veltmann C, Eckardt L, Meregalli PG, Gaita F, Tan HL, et al. Long-term prognosis of patients diagnosed with Brugada syndrome: results from the FINGER Brugada syndrome registry. Circulation. 2010;121:635–43.
Makimoto H, Kamakura S, Aihara N, Noda T, Nakajima I, Yokoyama T, et al. Clinical impact of the number of extrastimuli in programmed electrical stimulation in patients with Brugada type 1 electrocardiogram. Heart Rhythm. 2012;9(2):242–8.
Chen Q, Kirsch GE, Zhang D, Brugada R, Brugada J, Brugada P, et al. Genetic basis and molecular mechanisms for idiopathic ventricular fibrillation. Nature. 1998;392:293–6.
Antzelevitch C, Viskin S. Brugada syndrome: cellular mechanisms and approached to therapy. In: Gussak I, Antzelevitch C, editors. Electrical diseases of the heart: genetics, mechanisms, treatment, prevention. London: Springer; 2008. p. 500–35.
Grant AO, Carboni MP, Neplioueva V, Starmer CF, Memmi M, Napolitano C, et al. Long QT syndrome, Brugada syndrome, and conduction system disease are linked to a single sodium channel mutation. J Clin Invest. 2002;110:1201–9.
Kapplinger JD, Tester DJ, Alders M, Benito B, Berthet M, Brugada J, et al. An international compendium of mutations in the SCN5A encoded cardiac sodium channel in patients referred for Brugada syndrome genetic testing. Heart Rhythm. 2010;7:33–46.
Balser JR. The cardiac sodium channel: gating function and molecular pharmacology. J Mol Cell Cardiol. 2001;33:599–613.
Schulze-Bahr E, Eckardt L, Breithardt G, Seidl K, Wichter T, Wolpert C, et al. Sodium channel gene (SCN5A) mutations in 44 index patients with Brugada syndrome: different incidences in familial and sporadic disease. Hum Mutat. 2003;21:651–2.
Bezzina CR, Wilde AA, Roden DM. The molecular genetics of arrhythmias. Cardiovasc Res. 2005;67:343–6.
Tan HL, Bezzina CR, Smits JP, Verkerk AO, Wilde AA. Genetic control of sodium channel function. Cardiovasc Res. 2003;57:961–73.
Antzelevitch C, Brugada P, Brugada J, Brugada R. Brugada syndrome: from cell to bedside. Curr Probl Cardiol. 2005;30:9–54.
Dumaine R, Towbin JA, Brugada P, Vatta M, Nesterenko DV, Nesterenko VV, et al. Ionic mechanisms responsible for the electrocardiographic phenotype of the Brugada syndrome are temperature dependent. Circ Res. 1999;85:803–9.
Saura D, Garcia-Alberola A, Carrillo P, Pascual D, Martinez-Sanchez J, Valdes M. Brugada-like electrocardiographic pattern induced by fever. Pacing Clin Electrophysiol. 2002;25:856–9.
Porres JM, Brugada J, Urbistondo V, Garcia F, Reviejo K, Marco P. Fever unmasking the Brugada syndrome. Pacing Clin Electrophysiol. 2002;25:1646–8.
Mok NS, Priori SG, Napolitano C, Chan NY, Chahine M, Baroudi G. A newly characterized SCN5A mutation underlying Brugada syndrome unmasked by hyperthermia. J Cardiovasc Electrophysiol. 2003;14:407–11.
Ortega-Carnicer J, Benezet J, Ceres F. Fever-induced ST-segment elevation and T-wave alternans in a patient with Brugada syndrome. Resuscitation. 2003;57:315–7.
Patruno N, Pontillo D, Achilli A, Ruggeri G, Critelli G. Electrocardiographic pattern of Brugada syndrome disclosed by a febrile illness: clinical and therapeutic implications. Europace. 2003;5:251–5.
Peng J, Cui YK, Yuan FH, Yi SD, Chen ZM, Meng SR. Fever and Brugada syndrome: report of 21 cases. Di Yi Jun Yi Da Xue Xue Bao. 2005;25:432–4.
Dulu A, Pastores SM, McAleer E, Voigt L, Halpern NA. Brugada electrocardiographic pattern in a postoperative patient. Crit Care Med. 2005;33:1634–7.
Aramaki K, Okumura H, Shimizu M. Chest pain and ST elevation associated with fever in patients with asymptomatic Brugada syndrome fever and chest pain in Brugada syndrome. Int J Cardiol. 2005;103:338–9.
Hong K, Guerchicoff A, Pollevick GD, Oliva A, Dumaine R, de Zutter M, et al. Cryptic 5′ splice site activation in SCN5A associated with Brugada syndrome. J Mol Cell Cardiol. 2005;38:555–60.
Bezzina CR, Shimizu W, Yang P, Koopmann TT, Tanck MW, Miyamoto Y, et al. Common sodium channel promoter haplotype in Asian subjects underlies variability in cardiac conduction. Circulation. 2006;113:338–44.
Antzelevitch C, Pollevick GD, Cordeiro JM, Casis O, Sanguinetti MC, Aizawa Y, et al. Loss-of-function mutations in the cardiac calcium channel underlie a new clinical entity characterized by ST-segment elevation, short QT intervals, and sudden cardiac death. Circulation. 2007;115:442–9.
Burashnikov E, Pfeiffer R, Barajas-Martinez H, Delpon E, Hu D, Desai M, et al. Mutations in the cardiac L-type calcium channel associated J wave syndrome and sudden cardiac death. Heart Rhythm. 2010;7:1872–82.
London B, Michalec M, Mehdi H, Zhu X, Kerchner L, Sanyal S, et al. Mutation in glycerol-3-phosphate dehydrogenase 1 like gene (GPD1-L) decreases cardiac Na+ current and causes inherited arrhythmias. Circulation. 2007;116:2260–8.
Watanabe H, Koopmann TT, Le Scouarnec S, Yang T, Ingram CR, Schott JJ, et al. Sodium channel β1 subunit mutations associated with Brugada syndrome and cardiac conduction disease in humans. J Clin Invest. 2008;118:2260–8.
Delpón E, Cordeiro JM, Núñez L, Thomsen PEB, Guerchicoff A, Pollevick GD, et al. Functional effects of KCNE3 mutation and its role in the development of Brugada syndrome. Circ Arrhythm Electrophysiol. 2008;1:209–18.
Medeiros-Domingo A, Tan BH, Crotti L, Tester DJ, Eckhardt L, Cuoretti A, et al. Gain-of-function mutation S422L in the KCNJ8-encoded cardiac K(ATP) channel Kir6.1 as a pathogenic substrate for J-wave syndromes. Heart Rhythm. 2010;7:1466–71.
Giudicessi JR, Ye D, Tester DJ, Crotti L, Mugione A, Nesterenko VV, et al. Transient outward current (Ito) gain-of-function mutations in the KCND3-encoded Kv4.3 potassium channel and Brugada syndrome. Heart Rhythm. 1032;8:1024.
Cranefield PF, Hoffman BF. Conduction of the cardiac impulse. II. Summation and inhibition. Circ Res. 1971;28:220–33.
Kattygnarath D, Maugenre S, Neyroud N, Duthoit G, Denjoy I, Martins RP, et al. MOG1 mutations associated with Brugada syndrome electrocardiogram pattern. Circulation. 2009;120:S686 (Abstract).
Kattygnarath D, Maugenre S, Neyroud N, Balse E, Ichai C, Denjoy I, et al. MOG1: a new susceptibility gene for Brugada syndrome. Circ Cardiovasc Genet. 2011;4:261–8.
Tester DJ, Ackerman MJ. Genetic testing for potentially lethal, highly treatable inherited cardiomyopathies/channelopathies in clinical practice. Circulation. 2011;123:1021–37.
Antzelevitch C, Sicouri S, Litovsky SH, Lukas A, Krishnan SC, DiDiego JM, et al. Heterogeneity within the ventricular wall. Electrophysiology and pharmacology of epicardial, endocardial, and M cells. Circ Res. 1991;69:1427–49.
Antzelevitch C, Shimizu W, Yan GX, Sicouri S, Weissenburger J, Nesterenko VV, et al. The M cell: its contribution to the ECG and to normal and abnormal electrical function of the heart. J Cardiovasc Electrophysiol. 1999;10:1124–52.
Litovsky SH, Antzelevitch C. Transient outward current prominent in canine ventricular epicardium but not endocardium. Circ Res. 1988;62:116–26.
Liu DW, Gintant GA, Antzelevitch C. Ionic bases for electrophysiological distinctions among epicardial, midmyocardial, and endocardial myocytes from the free wall of the canine left ventricle. Circ Res. 1993;72:671–87.
Furukawa T, Myerburg RJ, Furukawa N, Bassett AL, Kimura S. Differences in transient outward currents of feline endocardial and epicardial myocytes. Circ Res. 1990;67:1287–91.
Fedida D, Giles WR. Regional variations in action potentials and transient outward current in myocytes isolated from rabbit left ventricle. J Physiol. 1991;442:191–209.
Clark RB, Bouchard RA, Salinas-Stefanon E, Sanchez-Chapula J, Giles WR. Heterogeneity of action potential waveforms and potassium currents in rat ventricle. Cardiovasc Res. 1993;27:1795–9.
Wettwer E, Amos GJ, Posival H, Ravens U. Transient outward current in human ventricular myocytes of subepicardial and subendocardial origin. Circ Res. 1994;75:473–82.
Nabauer M, Beuckelmann DJ, Uberfuhr P, Steinbeck G. Regional differences in current density and rate-dependent properties of the transient outward current in subepicardial and subendocardial myocytes of human left ventricle. Circulation. 1996;93:168–77.
Glukhov AV, Fedorov VV, Lou Q, Ravikumar VK, Kalish PW, Schuessler RB, et al. Transmural dispersion of repolarization in failing and nonfailing human ventricle. Circ Res. 2010;106:981–91.
Antzelevitch C. M cells in the human heart. Circ Res. 2010;106:815–7.
Di Diego JM, Sun ZQ, Antzelevitch C. Ito and action potential notch are smaller in left vs. right canine ventricular epicardium. Am J Physiol. 1996;271:H548–61.
Volders PG, Sipido KR, Carmeliet E, Spatjens RL, Wellens HJ, Vos MA. Repolarizing K+ currents ITO1 and IKs are larger in right than left canine ventricular midmyocardium. Circulation. 1999;99:206–10.
Zicha S, Xiao L, Stafford S, Cha TJ, Han W, Varro A, et al. Transmural expression of transient outward potassium current subunits in normal and failing canine and human hearts. J Physiol. 2004;561:735–48.
Rosati B, Pan Z, Lypen S, Wang HS, Cohen I, Dixon JE, et al. Regulation of KChIP2 potassium channel beta subunit gene expression underlies the gradient of transient outward current in canine and human ventricle. J Physiol. 2001;533:119–25.
Costantini DL, Arruda EP, Agarwal P, Kim KH, Zhu Y, Zhu W, et al. The homeodomain transcription factor Irx5 establishes the mouse cardiac ventricular repolarization gradient. Cell. 2005;123:347–58.
Takano M, Noma A. Distribution of the isoprenaline-induced chloride current in rabbit heart. Pflugers Arch. 1992;420:223–6.
Zygmunt AC. Intracellular calcium activates chloride current in canine ventricular myocytes. Am J Physiol. 1994;267:H1984–95.
Cordeiro JM, Greene L, Heilmann C, Antzelevitch D, Antzelevitch C. Transmural heterogeneity of calcium activity and mechanical function in the canine left ventricle. Am J Physiol Heart Circ Physiol. 2004;286:H1471–9.
Banyasz T, Fulop L, Magyar J, Szentandrassy N, Varro A, Nanasi PP. Endocardial versus epicardial differences in L-type calcium current in canine ventricular myocytes studied by action potential voltage clamp. Cardiovasc Res. 2003;58:66–75.
Wang HS, Cohen IS. Calcium channel heterogeneity in canine left ventricular myocytes. J Physiol. 2003;547:825–33.
Sicouri S, Antzelevitch C. A subpopulation of cells with unique electrophysiological properties in the deep subepicardium of the canine ventricle. The M cell. Circ Res. 1991;68:1729–41.
Anyukhovsky EP, Sosunov EA, Rosen MR. Regional differences in electrophysiologic properties of epicardium, midmyocardium and endocardium: in vitro and in vivo correlations. Circulation. 1996;94:1981–8.
Liu DW, Antzelevitch C. Characteristics of the delayed rectifier current (IKr and IKs) in canine ventricular epicardial, midmyocardial, and endocardial myocytes. A weaker IKs contributes to the longer action potential of the M cell. Circ Res. 1995;76:351–65.
Zygmunt AC, Eddlestone GT, Thomas GP, Nesterenko VV, Antzelevitch C. Larger late sodium conductance in M cells contributes to electrical heterogeneity in canine ventricle. Am J Physiol. 2001;281:H689–97.
Zygmunt AC, Goodrow RJ, Antzelevitch C. INaCa contributes to electrical heterogeneity within the canine ventricle. Am J Physiol Heart Circ Physiol. 2000;278:H1671–8.
Brahmajothi MV, Morales MJ, Reimer KA, Strauss HC. Regional localization of HERG, the channel protein responsible for the rapid component of the delayed rectifier, K+ current in the ferret heart. Circ Res. 1997;81:128–35.
Clements SD, Hurst JW. Diagnostic value of ECG abnormalities observed in subjects accidentally exposed to cold. Am J Cardiol. 1972;29:729–34.
Thompson R, Rich J, Chmelik F, Nelson WL. Evolutionary changes in the electrocardiogram of severe progressive hypothermia. J Electrocardiol. 1977;10:67–70.
RuDusky BM. The electrocardiogram in hypothermia-the J wave and the Brugada syndrome. Am J Cardiol. 2004;93:671–2.
Kraus F. Ueber die wirkung des kalziums auf den kreislauf. Dtsch Med Wochenschr. 1920;46:201–3.
Sridharan MR, Horan LG. Electrocardiographic J wave of hypercalcemia. Am J Cardiol. 1984;54:672–3.
Antzelevitch C, Sicouri S, Lukas A, Nesterenko VV, Liu DW, Di Diego JM. Regional differences in the electrophysiology of ventricular cells: physiological and clinical implications. In: Zipes DP, Jalife J, editors. Cardiac electrophysiology: from cell to bedside. 2nd ed. Philadelphia: W.B. Saunders Co; 1994. p. 228–45.
Eagle K. Images in clinical medicine. Osborn waves of hypothermia. N Engl J Med. 1994;10:680.
Emslie-Smith D, Sladden GE, Stirling GR. The significance of changes in the electrocardiogram in hypothermia. Br Heart J. 1959;21:343–51.
Osborn JJ. Experimental hypothermia: respiratory and blood pH changes in relation to cardiac function. Am J Physiol. 1953;175:389–98.
Sridharan MR, Johnson JC, Horan LG, Sohl GS, Flowers NC. Monophasic action potentials in hypercalcemic and hypothermic “J” waves-a comparative study. Am Fed Clin Res. 1983;31:219.
Di Diego JM, Antzelevitch C. High [Ca2+]-induced electrical heterogeneity and extrasystolic activity in isolated canine ventricular epicardium. Phase 2 reentry. Circulation. 1994;89:1839–50.
Yan GX, Antzelevitch C. Cellular basis for the Brugada syndrome and other mechanisms of arrhythmogenesis associated with ST segment elevation. Circulation. 1999;100:1660–6.
Antzelevitch C, Yan GX. Cellular and ionic mechanisms responsible for the Brugada syndrome. J Electrocardiol. 2000;33(Suppl):33–9.
Yan GX, Lankipalli RS, Burke JF, Musco S, Kowey PR. Ventricular repolarization components on the electrocardiogram: cellular basis and clinical significance. J Am Coll Cardiol. 2003;42:401–9.
Fish JM, Antzelevitch C. Role of sodium and calcium channel block in unmasking the Brugada syndrome. Heart Rhythm. 2004;1:210–7.
Morita H, Morita ST, Nagase S, Banba K, Nishii N, Tani Y, et al. Ventricular arrhythmia induced by sodium channel blocker in patients with Brugada syndrome. J Am Coll Cardiol. 2003;42:1624–31.
Gussak I, Antzelevitch C, Bjerregaard P, Towbin JA, Chaitman BR. The Brugada syndrome: clinical, electrophysiologic and genetic aspects. J Am Coll Cardiol. 1999;33:5–15.
Di Diego JM, Antzelevitch C. Pinacidil-induced electrical heterogeneity and extrasystolic activity in canine ventricular tissues. Does activation of ATP-regulated potassium current promote phase 2 reentry? Circulation. 1993;88:1177–89.
Antzelevitch C, Sicouri S, Lukas A, Di Diego JM, Nesterenko VV, Liu DW, et al. Clinical implications of electrical heterogeneity in the heart: the electrophysiology and pharmacology of epicardial, M, and endocardial cells. In: Podrid PJ, Kowey PR, editors. Cardiac arrhythmia: mechanism, diagnosis and management. Baltimore: William & Wilkins; 1995. p. 88–107.
Lukas A, Antzelevitch C. Phase 2 reentry as a mechanism of initiation of circus movement reentry in canine epicardium exposed to simulated ischemia. Cardiovasc Res. 1996;32:593–603.
Thomsen PE, Joergensen RM, Kanters JK, Jensen TJ, Haarbo J, Hagemann A, et al. Phase 2 reentry in man. Heart Rhythm. 2005;2:797–803.
Antzelevitch C. In vivo human demonstration of phase 2 reentry. Heart Rhythm. 2005;2:804–6.
Postema PG, van Dessel PF, Kors JA, Linnenbank AC, van Harpen G, Ritsema van Eck HJ, et al. Local depolarization abnormalities are the dominant pathophysiologic mechanism for type 1 electrocardiogram in Brugada syndrome: a study of electrocardiograms, vectorcardiograms, and body surface potential maps during ajmaline provocation. J Am Coll Cardiol. 2010;55:789–97.
Nademanee K, Veerakul G, Chandanamattha P, Chaothawee L, Ariyachaipanich A, Jirasirirojanakorn K, et al. Prevention of ventricular fibrillation episodes in Brugada syndrome by catheter ablation over the anterior right ventricular outflow tract epicardium. Circulation. 2011;123:1270–9.
Wilde AA, Postema PG, Di Diego JM, Viskin S, Morita H, Fish JM, et al. The pathophysiological mechanism underlying Brugada syndrome: depolarization versus repolarization. J Mol Cell Cardiol. 2010;49:543–53.
Futterman LG, Lemberg L. Brugada. Am J Crit Care. 2001;10:360–4.
Fujiki A, Usui M, Nagasawa H, Mizumaki K, Hayashi H, Inoue H. ST segment elevation in the right precordial leads induced with class IC antiarrhythmic drugs: insight into the mechanism of Brugada syndrome. J Cardiovasc Electrophysiol. 1999;10:214–8.
Antzelevitch C. Late potentials and the Brugada syndrome. J Am Coll Cardiol. 2002;39:1996–9.
Nagase S, Kusano KF, Morita H, Fujimoto Y, Kakishita M, Nakamura K, et al. Epicardial electrogram of the right ventricular outflow tract in patients with the Brugada syndrome: using the epicardial lead. J Am Coll Cardiol. 2002;39:1992–5.
Eckardt L, Bruns HJ, Paul M, Kirchhof P, Schulze-Bahr E, Wichter T, et al. Body surface area of ST elevation and the presence of late potentials correlate to the inducibility of ventricular tachyarrhythmias in Brugada syndrome. J Cardiovasc Electrophysiol. 2002;13:742–9.
Ikeda T, Takami M, Sugi K, Mizusawa Y, Sakurada H, Yoshino H. Noninvasive risk stratification of subjects with a brugada-type electrocardiogram and no history of cardiac arrest. Ann Noninvasive Electrocardiol. 2005;10:396–403.
Mizobuchi M, Enjoji Y, Nakamura S, Muranishi H, Utsunomiya M, Funatsu A, et al. Ventricular late potential in patients with apparently normal electrocardiogram; predictor of Brugada syndrome. Pacing Clin Electrophysiol. 2010;33:266–73.
Takagi M, Aihara N, Kuribayashi S, Taguchi A, Shimizu W, Kurita T, et al. Localized right ventricular morphological abnormalities detected by electron-beam computed tomography represent arrhythmogenic substrates in patients with the Brugada syndrome. Eur Heart J. 2001;22:1032–41.
Antzelevitch C. Brugada syndrome: historical perspectives and observations. Eur Heart J. 2002;23:676–8.
Esperer HD, Hoos O, Hottenrott K. Syncope due to Brugada syndrome in a young athlete. Br J Sports Med. 2007;41:180–1.
Guevara-Valdivia ME, Iturralde Torres P, De Micheli A, Colin Lizalde L, Medeiros Domingo A, Gonzalez-Hermosillo JA. Electrocardiographic changes during stress test in a patient with “Brugada syndrome”. Arch Cardiol Mex. 2001;71:66–72.
Stix G, Bella PD, Carbucicchio C, Schmidinger H. Spatial and temporal heterogeneity of depolarization and repolarization may complicate implantable cardioverter defibrillator therapy in Brugada syndrome. J Cardiovasc Electrophysiol. 2000;11:516–21.
Amin AS, de Groot EAA, Ruijter JM, Wilde AAM, Tan HT. Exercise-induced ECG changes in Brugada syndrome. Circ Arrhythm Electrophysiol. 2009;2:531–9.
Das MK, El Masry H. Fragmented QRS and other depolarization abnormalities as a predictor of mortality and sudden cardiac death. Curr Opin Cardiol. 2010;25:59–64.
Antzelevitch C, Brugada P, Brugada J, Brugada R, Shimizu W, Gussak I, et al. Brugada syndrome: a decade of progress. Circ Res. 2002;91:1114–9.
Kurita T, Shimizu W, Inagaki M, Suyama K, Taguchi A, Satomi K, et al. The electrophysiologic mechanism of ST-segment elevation in Brugada syndrome. J Am Coll Cardiol. 2002;40:330–4.
Belhassen B, Viskin S. Pharmacologic approach to therapy of Brugada syndrome: quinidine as an alternative to ICD therapy? In: Antzelevitch C, Brugada P, Brugada J, Brugada R, editors. The Brugada syndrome: from bench to bedside. Oxford: Blackwell Futura; 2004. p. 202–11.
Belhassen B, Glick A, Viskin S. Efficacy of quinidine in high-risk patients with Brugada syndrome. Circulation. 2004;110:1731–7.
Watanabe H, Chinushi M, Osaki A, Okamura K, Izumi D, Komura S, et al. Elimination of late potentials by quinidine in a patient with Brugada syndrome. J Electrocardiol. 2006;39:63–6.
Fish JM, Antzelevitch C. Cellular and ionic basis for the sex-related difference in the manifestation of the Brugada syndrome and progressive conduction disease phenotypes. J Electrocardiol. 2003;36:173–9.
Aiba T, Shimizu W, Hidaka I, Uemura K, Noda T, Zheng C, et al. Cellular basis for trigger and maintenance of ventricular fibrillation in the Brugada syndrome model: high-resolution optical mapping study. J Am Coll Cardiol. 2006;47:2074–85.
Shimizu W, Yan GX, Antzelevitch C. The Brugada syndrome: clinical findings and cellular mechanism. In: Sekiguchi M, Fontaine G, editors. Arryth-mogenic Right Ventricular Cardiomyopathy: ARVC and Related Disorders. Springer-Verlag, Tokyo, Japan: Springer; 2009.
Aiba T, Hidaka I, Shimizu W, Uemura K, Inagaki M, Sugimachi M, et al. Steep repolarization gradient is required for development of phase 2 reentry and subsequent ventricular tachyarrhythmias in a model of the Brugada syndrome: high-resolution optical mapping study. Circulation. 2004;110:III–318 (Abstract).
Morita H, Zipes DP, Fukushima-Kusano K, Nagase S, Nakamura K, Morita ST, et al. Repolarization heterogeneity in the right ventricular outflow tract: correlation with ventricular arrhythmias in Brugada patients and in an in vitro canine Brugada model. Heart Rhythm. 2008;5:725–33.
Morita H, Zipes DP, Morita ST, Wu J. Genotype-phenotype correlation in tissue models of Brugada syndrome simulating patients with sodium and calcium channelopathies. Heart Rhythm. 2010;7:820–7.
Di Diego JM, Antzelevitch C. Cellular basis for ST-segment changes observed during ischemia. J Electrocardiol. 2003;36(Suppl):1–5.
Di Diego JM, Fish JM, Antzelevitch C. Brugada syndrome and ischemia-induced ST-segment elevation. Similarities and differences. J Electrocardiol. 2005;38:14–7.
Childers R. R wave amplitude in ischemia, injury, and infarction. J Electrocardiol. 1996;29:171–8.
Cordeiro JM, Mazza M, Goodrow R, Ulahannan N, Antzelevitch C, Di Diego JM. Functionally distinct sodium channels in ventricular epicardial and endocardial cells contribute to a greater sensitivity of the epicardium to electrical depression. Am J Physiol Heart Circ Physiol. 2008;295:H154–62.
Kandori A, Shimizu W, Yokokawa M, Noda T, Kamakura S, Miyatake K, et al. Identifying patterns of spatial current dispersion that characterise and separate the Brugada syndrome and complete right-bundle branch block. Med Biol Eng Comput. 2004;42:236–44.
Hoogendijk MG, Potse M, Linnenbank AC, Verkerk AO, Den Ruijter HM, van Amersfoorth SC, et al. Mechanism of right precordial ST-segment elevation in structural heart disease: Excitation failure by current-to-load mismatch. Heart Rhythm. 2010;7:238–48.
Marquez MF, Bisteni A, Medrano G, De Micheli A, Guevara M, Iturralde P, et al. Dynamic electrocardiographic changes after aborted sudden death in a patient with Brugada syndrome and rate-dependent right bundle branch block. J Electrocardiol. 2005;38:256–9.
Litovsky SH, Antzelevitch C. Differences in the electrophysiological response of canine ventricular subendocardium and subepicardium to acetylcholine and isoproterenol. A direct effect of acetylcholine in ventricular myocardium. Circ Res. 1990;67:615–27.
Tsuchiya T, Ashikaga K, Honda T, Arita M. Prevention of ventricular fibrillation by cilostazol, an oral phosphodiesterase inhibitor, in a patient with Brugada syndrome. J Cardiovasc Electrophysiol. 2002;13:698–701.
Lukas A, Antzelevitch C. Differences in the electrophysiological response of canine ventricular epicardium and endocardium to ischemia: role of the transient outward current. Circulation. 1993;88:2903–15.
Nishizaki M, Fujii H, Sakurada H, Kimura A, Hiraoka M. Spontaneous T wave alternans in a patient with Brugada syndrome-responses to intravenous administration of class I antiarrhythmic drug, glucose tolerance test, and atrial pacing. J Cardiovasc Electrophysiol. 2005;16:217–20.
Tada H, Nogami A, Shimizu W, Naito S, Nakatsugawa M, Oshima S, et al. ST segment and T wave alternans in a patient with Brugada syndrome. Pacing Clin Electrophysiol. 2000;23:413–5.
Chinushi M, Washizuka T, Okumura H, Aizawa Y. Intravenous administration of class I antiarrhythmic drugs induced T wave alternans in a patient with Brugada syndrome. J Cardiovasc Electrophysiol. 2001;12:493–5.
Chinushi Y, Chinushi M, Toida T, Aizawa Y. Class I antiarrhythmic drug and coronary vasospasm-induced T wave alternans and ventricular tachyarrhythmia in a patient with Brugada syndrome and vasospastic angina. J Cardiovasc Electrophysiol. 2002;13:191–4.
Takagi M, Doi A, Takeuchi K, Yoshikawa J. Pilsicanide-induced marked T wave alternans and ventricular fibrillation in a patient with Brugada syndrome. J Cardiovasc Electrophysiol. 2002;13:837.
Ohkubo K, Watanabe I, Okumura Y, Yamada T, Masaki R, Kofune T, et al. Intravenous administration of class I antiarrhythmic drug induced T wave alternans in an asymptomatic Brugada syndrome patient. Pacing Clin Electrophysiol. 2003;26:1900–3.
Morita H, Nagase S, Kusano K, Ohe T. Spontaneous T wave alternans and premature ventricular contractions during febrile illness in a patient with Brugada syndrome. J Cardiovasc Electrophysiol. 2002;13:816–8.
Fish JM, Antzelevitch C. Cellular mechanism and arrhythmogenic potential of T-wave alternans in the Brugada syndrome. J Cardiovasc Electrophysiol. 2008;19:301–8.
Morita H, Zipes DP, Lopshire J, Morita ST, Wu J. T wave alternans in an in vitro canine tissue model of Brugada syndrome. Am J Physiol Heart Circ Physiol. 2006;291:H421–8.
Morita H, Zipes DP, Wu J. Brugada syndrome: insights of ST elevation, arrhythmogenicity, and risk stratification from experimental observations. Heart Rhythm. 2009;6:S34–43.
Tada T, Kusano KF, Nagase S, Banba K, Miura D, Nishii N, et al. Clinical significance of macroscopic T-wave alternans after sodium channel blocker administration in patients with Brugada syndrome. J Cardiovasc Electrophysiol. 2008;19:56–61.
Babaliaros VC, Hurst JW. Tricyclic antidepressants and the Brugada syndrome: an example of Brugada waves appearing after the administration of desipramine. Clin Cardiol. 2002;25:395–8.
Goldgran-Toledano D, Sideris G, Kevorkian JP. Overdose of cyclic antidepressants and the Brugada syndrome. N Engl J Med. 2002;346:1591–2.
Tada H, Sticherling C, Oral H, Morady F. Brugada syndrome mimicked by tricyclic antidepressant overdose. J Cardiovasc Electrophysiol. 2001;12:275.
Pastor A, Nunez A, Cantale C, Cosio FG. Asymptomatic Brugada syndrome case unmasked during dimenhydrinate infusion. J Cardiovasc Electrophysiol. 2001;12:1192–4.
Ortega-Carnicer J, Bertos-Polo J, Gutierrez-Tirado C. Aborted sudden death, transient Brugada pattern, and wide QRS dysrhythmias after massive cocaine ingestion. J Electrocardiol. 2001;34:345–9.
Nogami A, Nakao M, Kubota S, Sugiyasu A, Doi H, Yokoyama K, et al. Enhancement of J-ST-segment elevation by the glucose and insulin test in Brugada syndrome. Pacing Clin Electrophysiol. 2003;26:332–7.
Araki T, Konno T, Itoh H, Ino H, Shimizu M. Brugada syndrome with ventricular tachycardia and fibrillation related to hypokalemia. Circ J. 2003;67:93–5.
Akhtar M, Goldschlager NF. Brugada electrocardiographic pattern due to tricyclic antidepressant overdose. J Electrocardiol. 2006;39:336–9.
Krishnan SC, Josephson ME. ST segment elevation induced by class IC antiarrhythmic agents: underlying electrophysiologic mechanisms and insights into drug-induced proarrhythmia. J Cardiovasc Electrophysiol. 1998;9:1167–72.
Gasparini M, Priori SG, Mantica M, Napolitano C, Galimberti P, Ceriotti C, et al. Flecainide test in Brugada syndrome: a reproducible but risky tool. Pacing Clin Electrophysiol. 2003;26:338–41.
Takenaka S, Emori T, Koyama S, Morita H, Fukushima K, Ohe T. Asymptomatic form of Brugada syndrome. Pacing Clin Electrophysiol. 1999;22:1261–3.
Shimizu W, Aiba T, Kurita T, Kamakura S. Paradoxic abbreviation of repolarization in epicardium of the right ventricular outflow tract during augmentation of Brugada-type ST segment elevation. J Cardiovasc Electrophysiol. 2001;12:1418–21.
Matana A, Goldner V, Stanic K, Mavric Z, Zaputovic L, Matana Z. Unmasking effect of propafenone on the concealed form of the Brugada phenomenon. Pacing Clin Electrophysiol. 2000;23:416–8.
Fragakis N, Iliadis I, Papanastasiou S, Lambrou A, Katsaris G. Brugada type electrocardiographic changes induced by concomitant use of lithium and propafenone in patient with Wolff-Parkinson-White syndrome. Pacing Clin Electrophysiol. 2007;30:823–5.
Chutani S, Imran N, Grubb B, Kanjwal Y. Propafenone-induced Brugada-like ECG changes mistaken as acute myocardial infarction. Emerg Med J. 2008;25:117–8.
Rolf S, Bruns HJ, Wichter T, Kirchhof P, Ribbing M, Wasmer K, et al. The ajmaline challenge in Brugada syndrome: diagnostic impact, safety, and recommended protocol. Eur Heart J. 2003;24:1104–12.
Sarkozy A, Caenepeel A, Geelen P, Peytchev P, de Zutter M, Brugada P. Cibenzoline induced Brugada ECG pattern. Europace. 2005;7:537–9.
Chinushi M, Tagawa M, Nakamura Y, Aizawa Y. Shortening of the ventricular fibrillatory intervals after administration of verapamil in a patient with Brugada syndrome and vasospastic angina. J Electrocardiol. 2006;39:331–5.
Aouate P, Clerc J, Viard P, Seoud J. Propranolol intoxication revealing a Brugada syndrome. J Cardiovasc Electrophysiol. 2005;16:348–51.
Matsuo K, Shimizu W, Kurita T, Inagaki M, Aihara N, Kamakura S. Dynamic changes of 12-lead electrocardiograms in a patient with Brugada syndrome. J Cardiovasc Electrophysiol. 1998;9:508–12.
Sicouri S, Antzelevitch C. Sudden cardiac death secondary to antidepressant and antipsychotic drugs. Expert Opin Drug Saf. 2008;7:181–94.
Bigwood B, Galler D, Amir N, Smith W. Brugada syndrome following tricyclic antidepressant overdose. Anaesth Intensive Care. 2005;33:266–70.
Monteban-Kooistra WE, van Den Berg MP, Tulleken JE, Ligtenberg JJ, Meertens JH, Zijlstra JG. Brugada electrocardiographic pattern elicited by cyclic antidepressants overdose. Intensive Care Med. 2006;32:281–5.
Meert A, Vermeersch N, Beckers R, Hoste W, Brugada P, Hubloue I. Brugada-like ECG pattern induced by tricyclic antidepressants. Eur J Emerg Med. 2010;17:325–7.
Bolognesi R, Tsialtas D, Vasini P, Conti M, Manca C. Abnormal ventricular repolarization mimicking myocardial infarction after heterocyclic antidepressant overdose. Am J Cardiol. 1997;79:242–5.
Rouleau F, Asfar P, Boulet S, Dube L, Dupuis JM, Alquier P, et al. Transient ST segment elevation in right precordial leads induced by psychotropic drugs: relationship to the Brugada syndrome. J Cardiovasc Electrophysiol. 2001;12:61–5.
Yap YG, Behr ER, Camm AJ. Drug-induced Brugada syndrome. Europace. 2009;11:989–94.
Darbar D, Yang T, Churchwell K, Wilde AA, Roden DM. Unmasking of Brugada syndrome by lithium. Circulation. 2005;112:1527–31.
Chandra PA, Chandra AB. Brugada syndrome unmasked by lithium. South Med J. 2009;102:1263–5.
Pirotte MJ, Mueller JG, Poprawski T. A case report of Brugada-type electrocardiographic changes in a patient taking lithium. Am J Emerg Med. 2008;26:113.
Strohmer B, Schernthaner C. Brugada syndrome unmasked by lithium therapy. Wien Klin Wochenschr. 2007;119:282.
Laske C, Soekadar SR, Laszlo R, Plewnia C. Brugada syndrome in a patient treated with lithium. Am J Psychiatry. 2007;164:1440–1.
Josephson IR, Lederer WJ, Hartmann HA. Letter regarding article by Darbar et al, “unmasking of Brugada syndrome by lithium”. Circulation. 2006;113:e408.
Lopez-Barbeito B, Lluis M, Delgado V, Jimenez S, Diaz-Infante E, Nogue-Xarau S, et al. Diphenhydramine overdose and Brugada sign. Pacing Clin Electrophysiol. 2005;28:730–2.
Littmann L, Monroe MH, Svenson RH. Brugada-type electrocardiographic pattern induced by cocaine. Mayo Clin Proc. 2000;75:845–9.
Vernooy K, Delhaas T, Cremer OL, Di Diego JM, Oliva A, Timmermans C, et al. Electrocardiographic changes predicting sudden death in propofol-related infusion syndrome. Heart Rhythm. 2006;3:131–7.
Vaccarella A, Vitale P, Presti CA. General anaesthesia in a patient affected by Brugada syndrome. Minerva Anestesiol. 2008;74:149–52.
Phillips N, Priestley M, Denniss AR, Uther JB. Brugada-type electrocardiographic pattern induced by epidural bupivacaine. Anesth Analg. 2003;97:264–7.
Vernooy K, Sicouri S, Dumaine R, Hong K, Oliva A, Burashnikov E, et al. Genetic and biophysical basis for bupivacaine-induced ST segment elevation and VT/VF. Anesthesia unmasked Brugada syndrome. Heart Rhythm. 2006;3:1074–8.
Noda T, Shimizu W, Taguchi A, Satomi K, Suyama K, Kurita T, et al. ST-segment elevation and ventricular fibrillation without coronary spasm by intracoronary injection of acetylcholine and/or ergonovine maleate in patients with Brugada syndrome. J Am Coll Cardiol. 2002;40:1841–7.
Nishizaki M, Fujii H, Ashikaga T, Yamawake N, Sakurada H, Hiraoka M. ST-T wave changes in a patient complicated with vasospastic angina and Brugada syndrome: differential responses to acetylcholine in right and left coronary artery. Heart Vessels. 2008;23:201–5.
Oliva A, Hu D, Viskin S, Carrier T, Cordeiro JM, Barajas-Martinez H, et al. SCN5A mutation associated with acute myocardial infarction. Leg Med (Tokyo). 2009;11 Suppl 1:S206–9.
Chinushi M, Furushima H, Tanabe Y, Washizuka T, Aizawaz Y. Similarities between Brugada syndrome and ischemia-induced ST-segment elevation. Clinical correlation and synergy. J Electrocardiol. 2005;38(Suppl):18–21.
Nimmannit S, Malasit P, Chaovakul V, Susaengrat W, Vasuvattakul S, Nilwarangkur S. Pathogenesis of sudden unexplained nocturnal death (lai tai) and endemic distal renal tubular acidosis. Lancet. 1991;338:930–2.
Wichter T, Matheja P, Eckardt L, Kies P, Schafers K, Schulze-Bahr E, et al. Cardiac autonomic dysfunction in Brugada syndrome. Circulation. 2002;105:702–6.
Gonzalez Rebollo G, Madrid H, Carcia A, Garcia de Casto A, Moro AM. Reccurrent ventricular fibrillation during a febrile illness in a patient with the Brugada Syndrome. Rev Esp Cardiol. 2000;53:755–7.
Madle A, Kratochvil Z, Polivkova A. The Brugada syndrome. Vnitr Lek. 2002;48:255–8.
Kum L, Fung JWH, Chan WWL, Chan GK, Chan YS, Sanderson JE. Brugada syndrome unmasked by febrile illness. Pacing Clin Electrophysiol. 2002;25:1660–1.
Keller DI, Huang H, Zhao J, Frank R, Suarez V, Delacretaz E, et al. A novel SCN5A mutation, F1344S, identified in a patient with Brugada syndrome and fever-induced ventricular fibrillation. Cardiovasc Res. 2006;70:521–9.
Di Diego JM, Cordeiro JM, Goodrow RJ, Fish JM, Zygmunt AC, Peréz GJ, et al. Ionic and cellular basis for the predominance of the Brugada syndrome phenotype in males. Circulation. 2002;106:2004–11.
Ezaki K, Nakagawa M, Taniguchi Y, Nagano Y, Teshima Y, Yufu K, et al. Gender differences in the ST segment: effect of androgen-deprivation therapy and possible role of testosterone. Circ J. 2010;74:2448–54.
Antzelevitch C. The Brugada syndrome: diagnostic criteria and cellular mechanisms. Eur Heart J. 2001;22:356–63.
Brugada J, Brugada R, Brugada P. Pharmacological and device approach to therapy of inherited cardiac diseases associated with cardiac arrhythmias and sudden death. J Electrocardiol. 2000;33(Suppl):41–7.
Haissaguerre M, Extramiana F, Hocini M, Cauchemez B, Jais P, Cabrera JA, et al. Mapping and ablation of ventricular fibrillation associated with long-QT and Brugada syndromes. Circulation. 2003;108:925–8.
van Den Berg MP, Wilde AA, Viersma TJW, Brouwer J, Haaksma J, van der Hout AH, et al. Possible bradycardic mode of death and successful pacemaker treatment in a large family with features of long QT syndrome type 3 and Brugada syndrome. J Cardiovasc Electrophysiol. 2001;12:630–6.
Chinushi M, Aizawa Y, Ogawa Y, Shiba M, Takahashi K. Discrepant drug action of disopyramide on ECG abnormalities and induction of ventricular arrhythmias in a patient with Brugada syndrome. J Electrocardiol. 1997;30:133–6.
Sharif-Kazemi MB, Emkanjoo Z, Tavoosi A, Kafi M, Kheirkhah J, Alizadeh A, Sadr-Ameli MA.Electrical storm in Brugada syndrome during pregnancy. Pacing Clin Electrophysiol. 2011; 34(2):e18–21.
Kyriazis K, Bahlmann E, van der Schalk H, Kuck KH. Electrical storm in Brugada syndrome successfully treated with orciprenaline; effect of low-dose quinidine on the electrocardiogram. Europace. 2009;11:665–6.
Haghjoo M, Arya A, Heidari A, Sadr-Ameli MA. Suppression of electrical storm by oral quinidine in a patient with Brugada syndrome. J Cardiovasc Electrophysiol. 2005;16:674.
Alings M, Dekker L, Sadee A, Wilde A. Quinidine induced electrocardiographic normalization in two patients with Brugada syndrome. Pacing Clin Electrophysiol. 2001;24:1420–2.
Belhassen B, Viskin S, Fish R, Glick A, Setbon I, Eldar M. Effects of electrophysiologic-guided therapy with class IA antiarrhythmic drugs on the long-term outcome of patients with idiopathic ventricular fibrillation with or without the Brugada syndrome. J Cardiovasc Electrophysiol. 1999;10:1301–12.
Belhassen B, Viskin S, Antzelevitch C. The Brugada syndrome: is an implantable cardioverter defibrillator the only therapeutic option? Pacing Clin Electrophysiol. 2002;25:1634–40.
Hermida JS, Denjoy I, Clerc J, Extramiana F, Jarry G, Milliez P, et al. Hydroquinidine therapy in Brugada syndrome. J Am Coll Cardiol. 2004;43:1853–60.
Mok NS, Chan NY, Chi-Suen CA. Successful use of quinidine in treatment of electrical storm in Brugada syndrome. Pacing Clin Electrophysiol. 2004;27:821–3.
Kanlop N, Chattipakorn S, Chattipakorn N. Effects of cilostazol in the heart. J Cardiovasc Med (Hagerstown). 2011;12:88–95.
Fish JM, Extramiana F, Antzelevitch C. Tedisamil abolishes the arrhythmogenic substrate responsible for VT/VF in an experimental model of the Brugada syndrome. Heart Rhythm. 2004;1(1S):S158 (Abstract).
Fish JM, Extramiana F, Antzelevitch C. AVE0118, an Ito and IKur blocker, suppresses VT/VF in an experimental model of the Brugada syndrome. Circulation. 2004;110(17):III-193 (Abstract).
de La Coussaye JE, Bassoul B, Brugada J, Albat B, Peray PA, Gagnol JP, et al. Reversal of electrophysiologic and hemodynamic effects induced by high dose of bupivacaine by the combination of clonidine and dobutamine in anesthetized dogs. Anesth Analg. 1992;74(5):703–11.
Fish JM, Welchons DR, Kim YS, Lee SH, Ho WK, Antzelevitch C. Dimethyl lithospermate B, an extract of danshen, suppresses arrhythmogenesis associated with the Brugada syndrome. Circulation. 2006;113:1393–400.
Brugada P, Brugada R, Brugada J, Geelen P. Use of the prophylactic implantable cardioverter defibrillator for patients with normal hearts. Am J Cardiol. 1999;83:98D–100.
Kron J, Herre J, Renfroe EG, Rizo-Patron C, Raitt M, Halperin B, et al. Lead- and device-related complications in the antiarrhythmics versus implantable defibrillators trial. Am Heart J. 2001;141:92–8.
AVID Investigators. A comparison of antiarrhythmic-drug therapy with implantable defibrillators in patients resuscitated from near-fatal ventricular arrhythmias. The antiarrhythmics versus implantable defibrillators (AVID) investigators. N Engl J Med 1997;337:1576–83.
Sacher F, Probst V, Iesaka Y, Jacon P, Laborderie J, Mizon-Gerard F, et al. Outcome after implantation of a cardioverter-defibrillator in patients with Brugada syndrome: a multicenter study. Circulation. 2006;114:2317–24.
Antzelevitch C, Brugada P, Brugada J, Brugada R. The Brugada syndrome: from bench to bedside. Oxford: Blackwell Futura; 2005.
Antzelevitch C, Fish JM. Therapy for the Brugada syndrome. Handb Exp Pharmacol. 2006;171:305–30.
Nakazato Y, Suzuki T, Yasuda M, Daida H. Manifestation of brugada syndrome after pacemaker implantation in a patient with sick sinus syndrome. J Cardiovasc Electrophysiol. 2004;15:1328–30.
Shah AJ, Hocini M, Lamaison D, Sacher F, Derval N, Haissaguerre M. Regional substrate ablation abolishes Brugada syndrome. J Cardiovasc Electrophysiol. 2011;22:1290–1.
Antzelevitch C, Brugada P, Brugada J, Brugada R, Nademanee K, Towbin JA. Clinical approaches to tachyarrhythmias. The Brugada syndrome. Armonk: Futura Publishing Company; 1999.
Grant AO. Electrophysiological basis and genetics of Brugada syndrome. J Cardiovasc Electrophysiol. 2005;16 Suppl 1:S3–7.
Minoura Y, Di Diego JM, Barajas-Martinez H, Zygmunt AC, Hu D, Sicouri S, et al. Ionic and cellular mechanisms underlying the development of acquired Brugada syndrome in patients treated with antidepressants. J Cardiovasc Electrophysiol. 2012;23:423–32.
Marquez MF, Rivera J, Hermosillo AG, Iturralde P, Colin L, Moragrega JL, et al. Arrhythmic storm responsive to quinidine in a patient with Brugada syndrome and vasovagal syncope. Pacing Clin Electrophysiol. 2005;28:870–3.
Mizusawa Y, Sakurada H, Nishizaki M, Hiraoka M. Effects of low-dose quinidine on ventricular tachyarrhythmias in patients with Brugada syndrome: low-dose quinidine therapy as an adjunctive treatment. J Cardiovasc Pharmacol. 2006;47:359–64.
Viskin S, Wilde AA, Tan HL, Antzelevitch C, Shimizu W, Belhassen B. Empiric quinidine therapy for asymptomatic Brugada syndrome: time for a prospective registry. Heart Rhythm. 2009;6:401–4.
Wu L, Guo D, Li H, Hackett J, Yan GX, Jiao Z, et al. Role of late sodium current in modulating the proarrhythmic and antiarrhythmic effects of quinidine. Heart Rhythm. 2008;5:1726–34.
Viskin S, Antzelevitch C, Marquez MF, Belhassen B. Quinidine: a valuable medication joins the list of ‘endangered species’. Europace. 2007;12:1105–6.
Zeltser D, Justo D, Halkin A, Prokhorov V, Heller K, Viskin S. Torsade de pointes due to noncardiac drugs: most patients have easily identifiable risk factors. Medicine (Baltimore). 2003;82:282–90.
Antzelevitch C, Shimizu W. Cellular mechanisms underlying the long QT syndrome. Curr Opin Cardiol. 2002;17:43–51.
Belardinelli L, Antzelevitch C, Vos MA. Assessing predictors of drug-induced torsade de pointes. Trends Pharmacol Sci. 2003;24:619–25.
Antzelevitch C. The Brugada syndrome: ionic basis and arrhythmia mechanisms. J Cardiovasc Electrophysiol. 2001;12:268–72.
Suzuki H, Torigoe K, Numata O, Yazaki S. Infant case with a malignant form of Brugada syndrome. J Cardiovasc Electrophysiol. 2000;11:1277–80.
Tanaka H, Kinoshita O, Uchikawa S, Kasai H, Nakamura M, Izawa A, et al. Successful prevention of recurrent ventricular fibrillation by intravenous isoproterenol in a patient with Brugada syndrome. Pacing Clin Electrophysiol. 2001;24:1293–4.
Acknowledgement.
Supported by grant HL47678 from NHLBI, grant C026424 from NYSTEM and NYS and Florida Grand Lodges F. & A. M.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2013 Springer-Verlag London
About this chapter
Cite this chapter
Antzelevitch, C., Viskin, S. (2013). Brugada Syndrome: Cellular Mechanisms and Approaches to Therapy. In: Gussak, I., Antzelevitch, C. (eds) Electrical Diseases of the Heart. Springer, London. https://doi.org/10.1007/978-1-4471-4881-4_29
Download citation
DOI: https://doi.org/10.1007/978-1-4471-4881-4_29
Published:
Publisher Name: Springer, London
Print ISBN: 978-1-4471-4880-7
Online ISBN: 978-1-4471-4881-4
eBook Packages: MedicineMedicine (R0)