Abstract
Biofilms pose a serious problem to the food industry due to their high resistance to stressing conditions, including antimicrobials and disinfectants. Therefore, it is of vital importance to have methods that allow us to determine and quantify the cells of which biofilms are composed in order to determine the effectiveness of cleaning and disinfection treatments. In this chapter, we suggest two techniques, the plate counting technique and the crystal violet staining technique, as two possible indirect methods to determine in vitro biofilm mass. To overcome individual limitations, such as the plate counting technique’s disregard of the amount and localization of biomass on surfaces, or the crystal violet staining technique’s failure to differentiate between living and dead cells, we propose their combined use in order to obtain complete, valuable information on the behavior of microbial biofilms.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Key words
- Biofilms
- Food industry
- Sessile cells
- Microbial counts
- Biomass
- Plate count technique
- Crystal violet
- Exopolysaccharides
- Extracellular matrix
1 Introduction
Most bacteria have found new ways to adapt and survive under stress conditions: one such strategy is the formation of biofilms . A biofilm is a collection of sessile microbial cells that grow in a matrix of extracellular polymeric substances (exopolysaccharides [EPS ], proteins, lipids, and nucleic acids) and adhere to a surface. Biofilms can form on a wide range of biotic or abiotic surfaces, such as living tissues, industrial or drinking water pipes, medical devices, and aquatic systems, among others [1, 2]. All microorganisms, under appropriate environmental conditions, are capable of forming biofilms . However, some microorganisms are more susceptible to form biofilms than others: bacteria such as Pseudomonas, Listeria, Enterobacter, Flavobacterium, Alcaligenes, Staphylococcus, and Bacillus [3].
The main function of biofilms is to protect internal bacterial cells from external stressing conditions, such as changes in temperature or pH, UV radiation, nutrient deprivation, or antimicrobial agents [4]. With regard to antimicrobial agents, the matrix acts as a physical barrier that reduces their spread. EPS are one of the main components that make up the extracellular matrix of biofilms . They are large molecules of neutral charge with complex structures and a range of physicochemical properties that cover a wide range of functions relevant to bacterial physiology and multicellular lifestyles [5]. It has been shown that EPS production in response to oxidative, osmotic, drying, or heat stresses can improve microbial survival [6], as well as maintain the architecture and strength of biofilms [7]. Compared with their planktonic counterparts, biofilms are 10–1000 times more resistant to various disinfectants, such as sodium hypochlorite; and antimicrobials, such as ampicillin, tetracycline, and cloxacillin [8].
The process of biofilm formation is made up of five stages [9]: initial union, irreversible union, proliferation, maturation, and dispersal (Fig. 1).
In the first stage, the biofilm begins to form when several cells are reversibly attached to the surface. This initial adhesion depends on various factors such as the physicochemical properties of the surface, pH, the amount of EPS and proteins, and genetic factors that encode the motor functions. During the second stage, the binding becomes irreversible because the interaction between the bacteria and the contact surface changes from a weak bond to a permanent bond due to a higher production of EPS . From this stage onward, it is necessary to apply a powerful cutting force or chemical breakage to eliminate the biofilm [10]. Once the bacteria have adhered to the surface, the cells begin to grow and proliferate. This growth is associated with the production of EPS , which helps to strengthen the bond between the bacteria and the substrate, as well as to stabilize the colony against environmental stresses. In the maturation stage, the bacteria change their behavior and grow under sessile form in heterogeneous microcolonies that evolve to form an organized and complex structure. It can be flat or in the form of a mushroom, depending on the source of nutrients at its disposal. Finally, the biofilm allows the release of the bacteria in their planktonic form, thus equipped to colonize new niches and surfaces [10].
Biofilm formation causes adverse effects in several areas of human activity, including the food industry . Biofilms formed on industrial production lines lead to problems such as corrosion/damage to pipes and equipment [11], interference and blockage of food processes, and contamination of raw materials and products [10], all of which favor foodborne outbreaks [12]. In the vegetable industry, processes such as cutting, washing, rinsing, drying, and packaging are regarded as the main source of cross-contamination because they facilitate the entry and fixation of bacteria , thus favoring the formation of biofilms . One of the most critical points is packaging: a reported outbreak with whole melons contaminated with Listeria monocytogenes was due to unhealthy packaging conditions [10]. The formation of biofilms in the dairy industry can generate serious food safety problems and economic losses. One of the biggest problems is that microorganisms in biofilms can catalyze chemical and biological reactions, causing corrosion in metal storage tanks and pipes [13, 14]. In addition, L. monocytogenes biofilms are a potential source of contamination in the milking equipment of a dairy farm [15]. The meat industry is another major food industry that can serve as a propitious niche for the accumulation of microorganisms and the formation of biofilms . Dourou et al. [16] conducted a study to evaluate the binding, survival , and growth of Escherichia coli O157:H7 on stainless steel and high-density polyethylene surfaces typical of meat industry equipment. Their results showed that the binding of the bacteria depends on the type of substrate as well as on temperature . In particular, the greatest amount of fixation occurred not only during nonproduction hours in the meat manufacturing areas but also in the course of the storage period [10, 16].
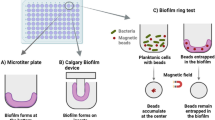
To investigate and evaluate the behavior of biofilms with the purpose of ensuring food safety , it is vitally important to carry out microbiological controls designed to collect all relevant microbiological information. This will enable the assurance of food safety , and the assessment of the susceptibility of biofilms to various treatments such as antimicrobials and disinfectants. Biofilm detection methods can be classified into two types: direct and indirect (Fig. 2) [13].
The first type is based on the direct observation of microbial biofilms , which includes techniques such as electrochemical impedance spectroscopy, epifluorescence microscopy, or scanning electron microscopy, among others (Fig. 2). Direct methods , however, can lead to an underestimation of biofilm levels by refraining to measure thickness, and/or by overestimating the areas covered by the cells, as is the case with epifluorescence microscopy. In addition, these methods are usually difficult to implement in the food industry . On the other hand, indirect methods (such as traditional plate counting, the staining of biofilm biomass with crystal violet or safranin , ATP determination techniques, or metabolic assays) require the detachment of biofilms from the surface. These indirect methods are more appropriate for routine studies on the presence and quantification of biofilms in the food industry . The plate count method is one of the culture methods most widely used to estimate cell viability and physiology, as well as to determine colony-forming units (CFU) in agar media. It likewise allows us to isolate cells for future studies [17]. However, this method has two main drawbacks:
-
1.
It does not provide information about the amount of biomass , which can lead to mechanical problems, such as pipe obstruction [18].
-
2.
It requires a proper disaggregation of the biofilms : if several cells form a single colony, the technique underestimates the cell population.
The dye staining method to determine biofilm biomass offers a number of advantages: (1) versatility, since it can be applied to a wide range of different bacterial species; (2) high-throughput capability, which facilitates simultaneous testing of a number of different conditions; and (3) the possibility of quantifying the biofilm biomass and examining its distribution. Nevertheless, it also has two important disadvantages: (1) bias in the quantification of biofilm cells due to washing, and (2) it only provides the total biomass , without differentiating the physiological state of sessile cells (e.g., whether they are alive or dead) [18, 19].
In this chapter, we explain the methodology of evaluating microbial counts and biofilm mass for in vitro biofilm testing on polystyrene and stainless steel surfaces. We also provide a number of recommendations in order to avoid each of these methods ’ disadvantages. In addition, we propose the combination of both methods as a means of obtaining a more complete picture of a biofilm ’s state.
2 Materials
2.1 Quantification of Biofilms by Plate Count Technique
-
1.
Culturing tools: micropipettes, plastic 1.5-mL tubes, and petri dishes (90 mm).
-
2.
24-well polystyrene and stainless steel plates.
-
3.
Adhesive PCR Plate Seals.
-
4.
Nutritive Agar (NA) medium for counting sessile cells of biofilms .
-
5.
Vortex.
-
6.
Distilled sterile water for washing.
-
7.
0.1% (w/v) Peptone Water (PW) solution or Phosphate-Buffered Saline (PBS) as diluent. To prepare the solutions, the required quantities were diluted in sterile distilled water according to the manufacturer’s instructions.
-
8.
PW or PBS solution with 1% (v/v) Tween 20. To prepare the solution, the corresponding volume of Tween 20 was added with a micropipette, drop by drop and very slowly. As this is a very viscous surfactant, it is recommended to use a trimmed tip (0.5–1 cm) to facilitate addition.
-
9.
Ultrasonic bath.
-
10.
Incubator.
2.2 Quantification of Biofilms by Crystal Violet Staining Assay
-
1.
Laboratory tools: micropipettes, pipettes, and polystyrene macro cuvette.
-
2.
Distilled sterile water for washing.
-
3.
0.1% (w/v) Crystal Violet solution. To prepare the solution, the required quantities were diluted in sterile distilled water.
-
4.
30% (v/v) glacial acetic acid solution. To prepare the solution, the required quantities were diluted in sterile distilled water.
-
5.
Spectrophotometer for measuring absorbance (595 nm).
3 Methods
To form the biofilms , 24-well polystyrene and stainless steel plates with 2 mL of culture in each well were used. To avoid dehydration of the biofilms , 1 mL of sterile distilled water was added to the external wells. Biofilm formation could be studied at different temperatures and for determined time periods as a function of the microorganism investigated. It was subsequently possible to determine biofilm formation following these methods .
3.1 Quantification of the Biofilms by Plate Count Technique
This assay allows to determine the proportion of living and dead cells within the biofilm . After forming the biofilm in 24-well plates, the supernatant was removed from the wells, and the biofilms were carefully washed two or three times with 3 mL of sterile distilled water (1.5 times with respect to the initial volume of culture) to remove any remaining planktonic cells and culture medium (see Note 1). Then, 2 mL of 0.1% PW or PBS with 1% Tween 20 was added to each well and the biofilms were resuspended with the micropipette (see Note 2). Next, to facilitate the disintegration of sessile cell aggregates from the biofilms , the plates (covered with adhesive PCR plate seals) were sonicated in an ultrasonic bath for 10 min at 40 kHz (see Note 3). Depending on the microorganism, biofilm can form many or few aggregates. For this reason, it is recommended to homogenize for several seconds and then check under the microscope for the presence or absence of aggregates (see Note 4). If there are aggregates, the vortex time for serial dilution can be increased.
After sonication treatment, 100 μL was taken from samples and, if necessary, of the corresponding decimal dilutions in 0.1% PW or PBS. The extract was resuspended for 10 s in a vortex, and 100 μL thereof was inoculated into sterile petri dishes. The NA medium was immediately added for mass homogenization seeding. After solidification of the agar, the plates were incubated in an inverted position, applying the specific time and temperature conditions for each microorganism. After the incubation period, the colonies on each plate were counted. We normally look for dilution factors that allow us to work in a range of 30–300 CFU per plate to ensure that the count is made without errors. The count values can be provided as CFU/well after applying the appropriate dilution factors.
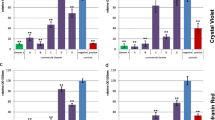
In Fig. 3 we can observe the example of a biofilm count at different incubation times. At 48 h, there were 106 CFU/well. Then, the cell population grew to a maximum of 107 CFU/well and remained stable until 144 h. In this case, an example of the most appropriate decimal dilution factors at 48 h would be -2, -3 and -4. This allows us to cover a wider range when counting the colonies.
3.2 Quantification of Biofilm Mass by Crystal Violet Staining Assay
Violet crystal staining assay allows for the measurement of a biofilm ‘s total cell biomass (comprised by the extracellular matrix , living cells, and dead cells). After the formation of the biofilm on microtiter plates, the supernatant of the wells was discarded. The plates were carefully washed one or two times with sterile distilled water (see Note 1) to remove the planktonic cells that had not firmly adhered to the biofilm (see Subheading 3.1). They were left to dry at room temperature (20–25 °C) for at least 12 h. Next, to dye the biofilm biomass , 2 mL (a volume equal to the initial volume of culture) of 0.1% crystal violet solution was added and allowed to incubate for at least 15 min at room temperature (20–25 °C). After this period, the supernatant was removed (see Note 1), and the wells were washed two or three times with 3 mL of sterile distilled water (1.5 times the initial volume of culture) to remove the crystal violet residue. It was then left to dry at room temperature for at least 12 h. At this point, the crystal violet staining method allows us to visualize the distribution of the biofilm (Fig. 4).
In order to quantify the biomass , 2 mL of the 30% glacial acetic acid solution was added to dissolve the violet crystal biomass , and the absorbance was measured at 595 nm using a spectrophotometer . To determine the biofilm ’s optical density , it is important to note that the absorbance values generally lie within a linear range between 0 and 1 (see Note 5). It is advisable to only consider the OD595 (Optical Density at 595 nm) values within this range. Dilutions can be made with the same solution of glacial acetic acid (30%). It is recommended to apply dilution factors such as 1/2, 1/4, or 1/8 or, if necessary, to apply a higher factor to ensure that the OD595 values of each sample lie within that 0–1 range, applying its corresponding dilution factor in the final results.
However, it should be noted that this microbial suspension will not allow us to perform plate counts, because the method practically destroys the biofilm ’s sessile cells .
In Fig. 5, we can observe an example of the OD595 of the biomass of biofilms at different times. The biomass increases along the entire incubation time. At 120 h, the biomass has increased to three times more than at 48 h; and at 144 h the biomass is more than double that observed at 120 h.
Optical density (OD595) of Bacillus cereus biofilm biomass after 48 h, 120 h, and 144 h of incubation . The biofilms were formed on stainless steel plates. The values obtained at 144 h have been multiplied by the corresponding dilution factors used to adjust to the 0–1 linear range of absorbance values
If we combine the results from microbial counts and crystal violet staining (Fig. 6), we can see that in the interval of 120–144 h, although the bacterial counts remain constant at 107 CFU/well, there was an increase in biomass due to the production of EPS , the main component of the extracellular matrix .
Logarithmic count (CFU/well) ( ) and optical density
(OD595) (
) and optical density
(OD595) ( ) of Bacillus cereus biofilm
biomass
at 48 h, 120 h and 144 h. The biofilms
were incubated in stainless steel plates. The values of OD595 obtained at 144 h have been multiplied by the corresponding dilution factors used to adjust to the 0–1 linear range of absorbance values
) of Bacillus cereus biofilm
biomass
at 48 h, 120 h and 144 h. The biofilms
were incubated in stainless steel plates. The values of OD595 obtained at 144 h have been multiplied by the corresponding dilution factors used to adjust to the 0–1 linear range of absorbance values
In conclusion, the plate count method is a traditional approach that allows us to know a biofilm ’s CFU per well, and thus, its food safety implications. It can be complemented with the quantification of biomass by the crystal violet staining method to visualize the hotspots of biofilm formation and provide a measurement of the amount of biofilm . This allows us to correlate the number of colonies with extracellular matrix production (EPS , proteins, lipids, and nucleic acids), thereby providing us with additional information about the biofilm ’s behavior. In addition, a greater increase of EPS can improve the degree of protection of the cells. This would have negative implications on food safety , since the effectiveness of cleaning and disinfection processes would be reduced. By combining both methods , we can overcome the disadvantages of each individual method and gain a better understanding of biofilms .
4 Notes
-
1.
The supernatant can be removed in various ways depending on the biofilm ’s shape, firmness, and adhesion. The plate can be turned over and gently tapped, removing all the supernatant at once. Alternatively, it can be removed with a pipette or micropipette. For washing, it is recommended to use the micropipette. It is highly important to do this slowly, drop by drop, taking care not to break the biofilm . The volume of sterile distilled water depends on the methodology used to form the biofilm . In case a different methodology is used, the volume of sterile distilled water required for the washings should be proportional to the initial volume of culture. The number of washes depends on the strength of the biofilm : if it is weak, one wash is recommended; if it is strong, two or three washes might be necessary.
-
2.
Tween 20 is a surfactant used to assist in the breakdown of sessile cells from biofilms when applying ultrasound treatment.
-
3.
It is highly important to control the bath temperature , which should not be too high (<30 °C) to avoid cell inactivation. On the other hand, one should also make sure that the parafilm is well attached to the plate to avoid possible contamination and water ingress during treatment.
-
4.
To observe the aggregation of cells, another suggestion is to do a count in the Thoma cell counting chamber under the microscope, and then to compare the results obtained with the plate count.
-
5.
The linear range of absorbance values depends on equipment and on laboratory conditions. Situations vary from one laboratory to another. Therefore, it is recommended to make a standard line to determine the most appropriate linear range for each situation.
References
Donlan RM (2002) Biofilms: microbial life on surfaces. Emerg Infect Dis 8(9):881–890. https://doi.org/10.3201/eid0809.020063
O’Toole G, Kaplan HB, Kolter R (2000) Biofilm formation as microbial development. Annu Rev Microbiol 54(1):49–79. https://doi.org/10.1146/annurev.micro.54.1.49
Mattilasandholm T, Wirtanen G (1992) Biofilm formation in the industry—a review. Food Rev Int 8(4):573–603. https://doi.org/10.1080/87559129209540953
Pagán R, García-Gonzalo D (2015) Influence of environmental factors on bacterial biofilm formation in the food industry: a review. Postdoc J 3(6):3–13. https://doi.org/10.14304/surya.jpr.v3n6.2
Caro-Astorga J, Álvarez-Mena A, Hierrezuelo J, Guadix JA, Heredia-Ponce Z, Arboleda-Estudillo Y, González-Munoz E, de Vicente A, Romero D (2020) Two genomic regions encoding exopolysaccharide production systems have complementary functions in B. cereus multicellularity and host interaction. Sci Rep 10(1):1000. https://doi.org/10.1038/s41598-020-57970-3
Chung JW, Altman E, Beveridge TJ, Speert DP (2003) Colonial morphology of Burkholderia cepacia complex genomovar III: implications in exopolysaccharide production, pilus expression, and persistence in the mouse. Infect Immun 71(2):904–909. https://doi.org/10.1128/iai.71.2.904-909.2003
Limoli DH, Jones CJ, Wozniak DJ (2015) Bacterial extracellular polysaccharides in biofilm formation and function. Microbiol Spectr 3(3). https://doi.org/10.1128/microbiolspec.MB-0011-2014
Davies D (2003) Understanding biofilm resistance to antibacterial agents. Nat Rev Drug Discov 2(2):114–122. https://doi.org/10.1038/nrd1008
Fang K, Park O-J, Hong SH (2020) Controlling biofilms using synthetic biology approaches. Biotechnol Adv 40:107518. https://doi.org/10.1016/j.biotechadv.2020.107518
Srey S, Jahid IK, Ha SD (2013) Biofilm formation in food industries: a food safety concern. Food Control 31(2):572–585. https://doi.org/10.1016/j.foodcont.2012.12.001
Jia R, Unsal T, Xu D, Lekbach Y, Gu T (2019) Microbiologically influenced corrosion and current mitigation strategies: a state of the art review. Int Biodeterior Biodegradation 137:42–58. https://doi.org/10.1016/j.ibiod.2018.11.007
Galié S, García-Gutiérrez C, Miguélez EM, Villar CJ, Lombó F (2018) Biofilms in the food industry: health aspects and control methods. Front Microbiol 9:898. https://doi.org/10.3389/fmicb.2018.00898
González-Rivas F, Ripolles-Avila C, Fontecha-Umaña F, Ríos-Castillo AG, Rodríguez-Jerez JJ (2018) Biofilms in the spotlight: detection, quantification, and removal methods. Compr Rev Food Sci Food Saf 17(5):1261–1276. https://doi.org/10.1111/1541-4337.12378
Blaschek HP, Wang HH, Agle ME (eds) (2007) Biofilms in the food environment, 1st edn. Blackwell Publishing/IFT Press, Ames
Latorre A, Van Kessel J, Karns J, Zurakowski M, Pradhan A, Boor K, Jayarao BM, Houser B, Daugherty C, Schukken Y (2010) Biofilm in milking equipment on a dairy farm as a potential source of bulk tank milk contamination with Listeria monocytogenes. J Dairy Sci 93(6):2792–2802. https://doi.org/10.3168/jds.2009-2717
Dourou D, Beauchamp CS, Yoon Y, Geornaras I, Belk KE, Smith GC, Nychas G-JE, Sofos JN (2011) Attachment and biofilm formation by Escherichia coli O157:H7 at different temperatures, on various food-contact surfaces encountered in beef processing. Int J Food Microbiol 149(3):262–268. https://doi.org/10.1016/j.ijfoodmicro.2011.07.004
Li L, Mendis N, Trigui H, Oliver JD, Faucher SP (2014) The importance of the viable but non-culturable state in human bacterial pathogens. Front Microbiol 5:258. https://doi.org/10.3389/fmicb.2014.00258
Azeredo J, Azevedo NF, Briandet R, Cerca N, Coenye T, Costa AR, Desvaux M, Di Bonaventura G, Hébraud M, Jaglic Z (2017) Critical review on biofilm methods. Crit Rev Microbiol 43(3):313–351. https://doi.org/10.1080/1040841x.2016.1208146
O’Toole GA (2011) Microtiter dish biofilm formation assay. J Vis Exp 47:2437. https://doi.org/10.3791/2437
Acknowledgments
This research was supported by the Agencia Estatal de Investigación (Spain) (PGC2018-093789-B-I00), by the European Social Fund, by the Aragonese Office of Science, University and Knowledge Society (research contract to N.M.), and by the Spanish Ministry of Science and Innovation (FPU17/02441 to E.P.; FPU15/02703 to D.B.).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 The Author(s), under exclusive license to Springer Science+Business Media, LLC, part of Springer Nature
About this chapter
Cite this chapter
Gascón, E., Merino, N., Pagán, E., Berdejo, D., Pagán, R., García-Gonzalo, D. (2021). Assessment of In Vitro Biofilms by Plate Count and Crystal Violet Staining: Is One Technique Enough?. In: Magnani, M. (eds) Detection and Enumeration of Bacteria, Yeast, Viruses, and Protozoan in Foods and Freshwater. Methods and Protocols in Food Science . Humana, New York, NY. https://doi.org/10.1007/978-1-0716-1932-2_6
Download citation
DOI: https://doi.org/10.1007/978-1-0716-1932-2_6
Published:
Publisher Name: Humana, New York, NY
Print ISBN: 978-1-0716-1931-5
Online ISBN: 978-1-0716-1932-2
eBook Packages: Springer Protocols