Abstract
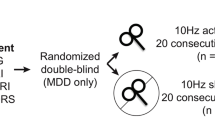
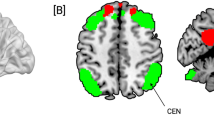
Effective repetitive transcranial magnetic stimulation (rTMS) treatment for depression has often focused on modulating the subgenual anterior cingulate cortex (sgACC), but no studies have related TMS-evoked responses in the sgACC to clinical effects following rTMS. Here we use interleaved single-pulse TMS/functional magnetic resonance imaging (fMRI) to demonstrate circuit engagement via TMS-evoked responses in the sgACC to stimulation of functionally connected cortical targets in a cohort study of unmedicated depressed patients (n = 36; ClinicalTrials.gov ID NCT04014959). Targets were identified using resting-state fMRI scans seeding the sgACC to identify individualized connectivity clusters. TMS/fMRI was assessed before and after a three-day open label intervention using intermittent theta burst stimulation (iTBS) rTMS targeting the sgACC pathway. TMS-evoked fMRI blood oxygen level-dependent (BOLD) responses in the sgACC and depression symptom scores were assessed pre- and post-intervention. Pre-intervention TMS-evoked response magnitude in the sgACC predicted depression improvement, with more negative evoked responses being associated with greater clinical improvement. Larger post-intervention changes in evoked responses were also associated with depression improvement. The prognostic sgACC associations were specific to the intervention pathway and significantly associated with depression but not anxiety improvement. Here we demonstrate causal evidence of sgACC engagement with TMS/fMRI and show the clinical relevance of engagement and modulation of the targeted prefrontal–sgACC circuit.





Similar content being viewed by others
Data availability
The baseline MRI and demographic data are available from https:/nda.nih.gov as per the National Institutes of Health funding mandate. TMS/fMRI data are not available publicly at this time due to ongoing analyses. The first author (oathes@pennmedicine.upenn.edu) can be contacted for a possible data-use agreement.
Code availability
No special code was developed for the presented analyses. The software used for processing, the statistical packages and tools are described in the text.
References
Cole, E. J. et al. Stanford accelerated intelligent neuromodulation therapy for treatment-resistant depression. Am. J. Psychiatry 177, 716–726 (2020).
Fox, M. D., Buckner, R. L., White, M. P., Greicius, M. D. & Pascual-Leone, A. Efficacy of transcranial magnetic stimulation targets for depression is related to intrinsic functional connectivity with the subgenual cingulate. Biol. Psychiatry 72, 595–603 (2012).
Cash, R. F. et al. Subgenual functional connectivity predicts antidepressant treatment response to transcranial magnetic stimulation: independent validation and evaluation of personalization. Biol. Psychiatry 86, e5–e7 (2019).
Cash, R. F., Cocchi, L., Lv, J., Fitzgerald, P. B. & Zalesky, A. Functional magnetic resonance imaging-guided personalization of transcranial magnetic stimulation treatment for depression. JAMA Psychiatry 78, 337–339 (2020).
Weigand, A. et al. Prospective validation that subgenual connectivity predicts antidepressant efficacy of transcranial magnetic stimulation sites. Biol. Psychiatry 84, 28–37 (2018).
Elbau, I. G. et al. Functional connectivity mapping for rTMS target selection in depression. Am. J. Psychiatry 180, 230–240 (2023).
Rosen, A. et al. Targeting location relates to treatment response in active but not sham rTMS stimulation. Brain Stimul. 14, 703–709 (2021).
Cash, R. F., Müller, V. I., Fitzgerald, P. B., Eickhoff, S. B. & Zalesky, A. Altered brain activity in unipolar depression unveiled using connectomics. Nat. Mental Health 1, 174–185 (2023).
Williams, N. R. et al. High-dose spaced theta-burst TMS as a rapid-acting antidepressant in highly refractory depression. Brain J. Neurol. 141, e18 (2018).
Cole, E. J. et al. Stanford Neuromodulation Therapy (SNT): a double-blind randomized controlled trial. Am. J. Psychiatry 179, 132–141 (2021).
Mayberg, H. S. et al. Reciprocal limbic-cortical function and negative mood: converging PET findings in depression and normal sadness. Am. J. Psychiatry 156, 675–682 (1999).
Rolls, E. T. et al. Functional connectivity of the anterior cingulate cortex in depression and in health. Cerebral Cortex 29, 3617–3630 (2019).
Yamashita, A. et al. Generalizable brain network markers of major depressive disorder across multiple imaging sites. PLoS Biol. 18, e3000966 (2020).
Lozano, A. M. et al. Subcallosal cingulate gyrus deep brain stimulation for treatment-resistant depression. Biol. Psychiatry 64, 461–467 (2008).
Liston, C. et al. Default mode network mechanisms of transcranial magnetic stimulation in depression. Biol. Psychiatry 76, 517–526 (2014).
Baeken, C. et al. The impact of accelerated HF-rTMS on the subgenual anterior cingulate cortex in refractory unipolar major depression: insights from 18FDG PET brain imaging. Brain Stimul. 8, 808–815 (2015).
Philip, N. S. et al. Network mechanisms of clinical response to transcranial magnetic stimulation in posttraumatic stress disorder and major depressive disorder. Biol. Psychiatry 83, 263–272 (2018).
Oathes, D. J. et al. Resting fMRI guided TMS results in subcortical and brain network modulation indexed by interleaved TMS/fMRI. Exp. Brain Res. 239, 1165–1178 (2021).
Siddiqi, S. H. et al. Distinct symptom-specific treatment targets for circuit-based neuromodulation. Am. J. Psychiatry 177, 435–446 (2020).
Drysdale, A. T. et al. Resting-state connectivity biomarkers define neurophysiological subtypes of depression. Nat. Med. 23, 28–38 (2017).
Sydnor, V. J. et al. Cortical-subcortical structural connections support transcranial magnetic stimulation engagement of the amygdala. Sci. Adv. 8, eabn5803 (2022).
O’Reardon, J. P. et al. Efficacy and safety of transcranial magnetic stimulation in the acute treatment of major depression: a multisite randomized controlled trial. Biol. Psychiatry 62, 1208–1216 (2007).
Blumberger, D. M. et al. Effectiveness of theta burst versus high-frequency repetitive transcranial magnetic stimulation in patients with depression (THREE-D): a randomised non-inferiority trial. Lancet 391, 1683–1692 (2018).
Oathes, D. J. et al. Combining transcranial magnetic stimulation with functional magnetic resonance imaging for probing and modulating neural circuits relevant to affective disorders. WIREs Cogn. Sci. 12, e1553 (2021).
Chen, A. C. et al. Causal interactions between fronto-parietal central executive and default-mode networks in humans. Proc. Natl Acad. Sci. USA 110, 19944–19949 (2013).
Gratton, C., Lee, T. G., Nomura, E. M. & D’Esposito, M. The effect of theta-burst TMS on cognitive control networks measured with resting state fMRI. Front. Syst. Neurosci. 7, 124 (2013).
Duprat, R. J. et al. Resting fMRI-guided TMS evokes subgenual anterior cingulate response in depression. Preprint at https://www.biorxiv.org/content/10.1101/2022.09.08.507012v1 (2022).
Avants, B. B., Tustison, N. & Song, G. Advanced normalization tools (ANTS). Insight J. 2, 1–35 (2009).
Avants, B. B. et al. A reproducible evaluation of ANTs similarity metric performance in brain image registration. NeuroImage 54, 2033–2044 (2011).
Smith, S. M. & Brady, J. M. SUSAN—a new approach to low level image processing. Int. J. Comput. Vision 23, 45–78 (1997).
Karabanov, A. et al. Consensus paper: probing homeostatic plasticity of human cortex with non-invasive transcranial brain stimulation. Brain Stimul. 8, 993–1006 (2015).
Ziemann, U. & Siebner, H. R. Inter-subject and inter-session variability of plasticity induction by non-invasive brain stimulation: boon or bane? Brain Stimul. 8, 662–663 (2015).
Müller-Dahlhaus, F. & Ziemann, U. Metaplasticity in human cortex. Neuroscientist 21, 185–202 (2015).
Stokes, M. G. et al. Distance-adjusted motor threshold for transcranial magnetic stimulation. Clin. Neurophysiol. 118, 1617–1625 (2007).
Lovibond, P. F. & Lovibond, S. H. The structure of negative emotional states: comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories. Behav. Res. Ther. 33, 335–343 (1995).
Acknowledgements
This work was funded in part by the National Institute of Mental Health grants nos. MH120811 and MH116920 (D.J.O.) and U01109991 (Y.I.S.) as well as a Brain Behavior Research Foundation NARSAD Young Investigator grant (D.J.O.). The funders had no role in the design and conduct of the study; collection, management, analysis and interpretation of data; nor were they involved in the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Contributions
D.J.O. conceived the research and designed the experiments. D.J.O. secured funding. R.J.-P.D., M.S., H.L. and J.A.D. collected data. D.J.O. analyzed data with analysis tools and input from K.A.L. D.J.O. and Y.I.S. supervised the intervention sessions. R.J.-P.D. and X.L. processed and quality-controlled the imaging data with supervision from D.J.O. R.J.-P.D., J.R. and D.J.O. generated figures. All authors contributed manuscript reviews and edits.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Mental Health thanks Florian Müller-Dahlhaus, Shan Siddiqi and the other, anonymous, reviewers for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary Results, Tables 1–4 and Figs. 1–5.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Oathes, D.J., Duprat, R.JP., Reber, J. et al. Non-invasively targeting, probing and modulating a deep brain circuit for depression alleviation. Nat. Mental Health 1, 1033–1042 (2023). https://doi.org/10.1038/s44220-023-00165-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s44220-023-00165-2
- Springer Nature America, Inc.
This article is cited by
-
Interleaved TMS/fMRI shows that threat decreases dlPFC-mediated top-down regulation of emotion processing
NPP—Digital Psychiatry and Neuroscience (2024)
-
Elevating the field for applying neuroimaging to individual patients in psychiatry
Translational Psychiatry (2024)
-
Chronometric TMS-fMRI of personalized left dorsolateral prefrontal target reveals state-dependency of subgenual anterior cingulate cortex effects
Molecular Psychiatry (2024)