Abstract
Background
Alteration in the brain mitochondrial functions have been suggested to participate, as a relevant factor, in the development of mental disorders. Therefore, the brain mitochondria may be a crucial therapeutic target in the course of depression.
Methods
Our goal was to find out the impact of two antidepressant drugs with various mechanisms of action — imipramine and fluoxetine, on the frontal cortex mitochondria-enriched fraction in an animal model of depression based on the prenatal stress procedure.
Results
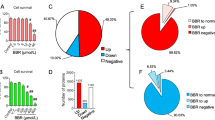
Our results confirmed that the prenatal stress caused depressive-like disturbances in the adult offspring rats, which were normalized by the chronic imipramine and fluoxetine administration. For the first time, using 2D-LC–MS/MS, we demonstrated nine differentially expressed proteins after the imipramine administration. Of these proteins, the up-regulation of the 2′,3′-cyclic-nucleotide 3′-phosphodiesterase enzyme and down-regulation of the Hypoxanthine-guanine phosphoribosyltransferase (HPRT), Ras-related proteins (Rap-1A and Rap-1B) and Transgelin-3 (NP25) were the most striking. In contrast, after the chronic fluoxetine treatment, we observed differential expression in five proteins, including the enhanced expression of component of pyruvate dehydrogenase complex and diminished of Glutathione S-transferase P (Gstp-1), as well as Maleylacetoacetate isomerase.
Conclusions
These results overcome the interesting data that brain mitochondria in the frontal cortex may constitute the target for pharmacotherapy. The multifaceted profile of both antidepressant drugs action makes difficult to elucidate the exact mechanism of imipramine and fluoxetine action in the brain mitochondria. Further study of mitochondrial dysfunction in psychiatric disorders will be base to know the possible biological consequences of our observations.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Krishnan V, Nestler EJ. Animal models of depression: molecular perspectives. Brain Imaging Behav Neurosci 2011;121–47, doi:https://doi.org/10.1007/7854_2010_108.
Herrero-Mendez A, Almeida A, Fernández E, Maestre C, Moncada S, Bolaños JP. The bioenergetic and antioxidant status of neurons is controlled by continuous degradation of a key glycolytic enzyme by APC/C-Cdh1. Nat Cell Biol 2009;11:747–52, doi:https://doi.org/10.1038/ncb1881.
Adzic M, Brkic Z, Bulajic S, Mitic M, Radojcic MB. Antidepressant action on mitochondrial dysfunction in psychiatric disorders. Drug Dev Res 2016;77:400–6, doi:https://doi.org/10.1002/ddr.21332.
Konradi C, Eaton M, MacDonald ML, Walsh J, Benes FM, Heckers S. Molecular evidence for mitochondrial dysfunction in bipolar disorder. Arch Gen Psychiatry 2004;61:300–8, doi:https://doi.org/10.1001/archpsyc.61.3.300.
Cataldo AM, McPhie DL, Lange NT, Punzell S, Elmiligy S, Ye NZ, et al. Abnormalities in mitochondrial structure in cells from patients with bipolar disorder. Am J Pathol 2010;177:575–85, doi:https://doi.org/10.2353/ajpath.2010.081068.
Clay H, Sillivan S, Konradi C. Mitochondrial dysfunction and pathology in bipolar disorder and schizophrenia. Int J Dev Neurosci 2012;29:311–24, doi:https://doi.org/10.1016/j.ijdevneu.2010.08.007.
Basta-Kaim A, Szczesny E, Glombik K, Stachowicz K, Slusarczyk J, Nalepa I, et al. Prenatal stress affects insulin-like growth factor-1 (IGF-1) level and IGF-1 receptor phosphorylation in the brain of adult rats. Eur Neuropsychopharmacol 2014;24:1546–56, doi:https://doi.org/10.1016/j.euroneuro.2014.07.002.
Szymanska M, Budziszewska B, Jaworska-Feil L, Basta-Kaim A, Kubera M, Leskiewicz M, et al. The effect of antidepressant drugs on the HPA axis activity, glucocorticoid receptor level and FKBP51 concentration in prenatally stressed rats. Psychoneuroendocrinology 2009;34:822–32, doi:https://doi.org/10.1016/j.psyneuen.2008.12.012.
Maccari S, Darnaudery M, Morley-Fletcher S, Zuena AR, Cinque C, Van Reeth O. Prenatal stress and long-term consequences: implications of glucocorticoid hormones. Neurosci Biobehav Rev 2003;27:119–27, doi:https://doi.org/10.1016/S0149-7634(03)00014-9.
Budziszewska B, Szymanska M, Leskiewicz M, Basta-Kaim A, Jaworska-Feil L, Kubera M, et al. The decrease in JNK- and p38-MAP kinase activity is accompanied by the enhancement of PP2A phosphatase level in the brain of prenatally stressed rats. J Physiol Pharmacol 2010;61:207–15.
Fine R, Zhang J, Stevens H. Prenatal stress and inhibitory neuron systems: implications for neuropsychiatric disorders. Mol Psychiatry 2014;19:641–51, doi:https://doi.org/10.1038/mp.2014.35.
Szczesny E, Basta-Kaim A, Slusarczyk J, Trojan E, Glombik K, Regulska M, et al. The impact of prenatal stress on insulin-like growth factor-1 and pro-inflammatory cytokine expression in the brains of adult male rats: the possible role of suppressors of cytokine signaling proteins. J Neuroimmunol 2014;1–10, doi:https://doi.org/10.1016/j.jneuroim.2014.08.001.
Detka J, Kurek A, Kucharczyk M, Głombik K, Basta-Kaim A, Kubera M, et al. Brain glucose metabolism in an animal model of depression. Neuroscience 2015;295:198–208, doi:https://doi.org/10.1016/j.neuroscience.2015.03.046.
Głombik K, Stachowicz A, Slusarczyk J, Trojan E, Budziszewska B, Suski M, et al. Maternal stress predicts altered biogenesis and the profile of mitochondrial proteins in the frontal cortex and hippocampus of adult offspring rats. Psychoneuroendocrinology 2015;60:151–62, doi:https://doi.org/10.1016/j.psyneuen.2015.06.015.
Manoli I, Alesci S, Blackman MR, Su YA, Rennert OM, Chrousos GP. Mitochondria as key components of the stress response. Trends Endocrinol Metab 2007;18:190–8, doi:https://doi.org/10.1016/j.tem.2007.04.004.
Escames G, López LC, García JA, García-Corzo L, Ortiz F, Acuña-Castroviejo D. Mitochondrial DNA and inflammatory diseases. Hum Genet 2012;131:161–73, doi:https://doi.org/10.1007/s00439-011-1057-y.
Villa RF, Ferrari F, Bagini L, Gorini A, Brunello N, Tascedda F. Mitochondrial energy metabolism of rat hippocampus after treatment with the antidepressants desipramine and fluoxetine. Neuropharmacology 2017;121:30–8, doi:https://doi.org/10.1016/j.neuropharm.2017.04.025.
Głombik K, Stachowicz A, Olszanecki R, Slusarczyk J, Trojan E, Lasoń W, et al. The effect of chronic tianeptine administration on the brain mitochondria: direct links with an animal model of depression. Mol Neurobiol 2016;1–12, doi:https://doi.org/10.1007/s12035-016-9807-4.
Glombik K, Stachowicz A, Trojan E, Olszanecki R, Slusarczyk J, Suski M, et al. Evaluation of the effectiveness of chronic antidepressant drug treatments in the hippocampal mitochondria — a proteomic study in an animal model of depression. Prog Neuropsychopharmacol Biol Psychiatry 2017;78:51–60, doi:https://doi.org/10.1016/j.pnpbp.2017.05.014.
Souza ME, Polizello AC, Uyemura SA, Castro-Silva O, Curti C. Effect of fluoxetine on rat liver mitochondria. Biochem Pharmacol 1994;48:535–41.
Weinbach EC, Costa JL, Nelson BD, Claggett CE, Hundal T, Bradley D, et al. Effects of tricyclic antidepressant drugs on energy-linked reactions in mitochondria. Biochem Pharmacol 1986;35:1445–51.
Zhang WH, Wang H, Wang X, Narayanan MV, Stavrovskaya IG, Kristal BS, et al. Nortriptyline protects mitochondria and reduces cerebral ischemia/hypoxia injury. Stroke 2008;39:455–62, doi:https://doi.org/10.1161/STROKEAHA.107.496810.
Charles E, Hammadi M, Kischel P, Delcroix V, Demaurex N, Castelbout C, et al. The antidepressant fluoxetine induces necrosis by energy depletion and mitochondrial calcium overload. Oncotarget 2016;8:3181–96, doi:https://doi.org/10.18632/oncotarget.13689.
Mukherjee J, Das MK, Yang ZY, Lew R. Evaluation of the binding of the radiolabeled antidepressant drug, 18F-fluoxetine in the rodent brain: an in vitro and in vivo study. Nucl Med Biol 1998;25:605–10.
de Oliveira MR. Fluoxetine and the mitochondria: a review of the toxicological aspects. Toxicol Lett 2016;258:185–91, doi:https://doi.org/10.1016/j.toxlet.2016.07.001.
Marks DM, Shah MJ, Patkar AA, Masand PS, Park G-Y, Pae C-U. Serotonin-norepinephrine reuptake inhibitors for pain control: premise and promise. Curr Neuropharmacol 2009;7:331–6, doi:https://doi.org/10.2174/157015909790031201.
Trojan E, Głombik K, Slusarczyk J, Budziszewska B, Kubera M, Roman A, et al. The beneficial impact of antidepressant drugs on prenatal stress-evoked malfunction of the insulin-like growth factor-1 (IGF-1) protein family in the olfactory bulbs of adult rats. Neurotox Res 2016;29:288–98, doi:https://doi.org/10.1007/s12640-015-9575-3.
Maccari S, Morley-Fletcher S. Effects of prenatal restraint stress on the hypothalamus-pituitary-adrenal axis and related behavioural and neurobiological alterations. Psychoneuroendocrinology 2007;32:10–5, doi:https://doi.org/10.1016/j.psyneuen.2007.06.005.
Detke MJ, Rickels M, Lucki I. Active behaviors in the rat forced swimming test differentially produced by serotonergic and noradrenergic antidepressants. Psychopharmacology (Berl) 1995;121:66–72, doi:https://doi.org/10.1007/BF02245592.
Porsolt RD, Anton G, Blavet N, Jalfre M. Behavioural despair in rats: a new model sensitive to antidepressant treatments. Eur J Pharmacol 1978;47:379–91, doi:https://doi.org/10.1016/0014-2999(78)90118-8.
Jung-Testas I, Baulieu EE. Steroid hormone receptors and steroid action in rat glial cells of the central and peripheral nervous system. J Steroid Biochem Mol Biol 1998;65:243–51.
Hroudova J, Fisar Z. Activities of respiratory chain complexes and citrate synthase influenced by pharmacologically different antidepressants and mood stabilizers. Neuroendocrinol Lett 2010;31:336–42.
Kedracka-Krok S, Fic E, Jankowska U, Jaciuk M, Gruca P, Papp M, et al. Effect of chronic mild stress and imipramine on the proteome of the rat dentate gyrus. J Neurochem 2010;113:848–59, doi:https://doi.org/10.1111/j.1471-4159.2010.06652.x.
Yang L, Kan EM, Lu J, Wu C, Ling E-A. Expression of 2′, 3′-cyclic nucleotide 3′-phosphodiesterase (CNPase) and its roles in activated microglia in vivo and in vitro. J Neuroinflammation 2014;11:148, doi:https://doi.org/10.1186/s12974-014-0148-9.
Edgar NM, Touma C, Palme R, Sibille E. Resilient emotionality and molecular compensation in mice lacking the oligodendrocyte-specific gene Cnp1. Transl Psychiatry 2011;1:e42, doi:https://doi.org/10.1038/tp.2011.40.
Peirce TR, Bray NJ, Williams NM, Norton N, Moskvina V, Preece A, et al. Convergent evidence for 2′,3′-cyclic nucleotide 3′-phosphodiesterase as a possible susceptibility gene for schizophrenia. Arch Gen Psychiatry 2006;63:18, doi:https://doi.org/10.1001/archpsyc.63.1.18.
Vlkolinský R, Cairns N, Fountoulakis M, Lubec G. Decreased brain levels of 2′, 3′-cyclic nucleotide-3′-phosphodiesterase in down syndrome and Alzheimer’s disease. Neurobiol Aging 2001;22:547–53, doi:https://doi.org/10.1016/S0197-4580(01)00218-4.
Yan J, Li F, Ingram DA, Quilliam LA. Rap1a is a key regulator of fibroblast growth factor 2-induced angiogenesis and together with Rap1b controls human endothelial cell functions. Mol Cell Biol 2008;28:5803–10, doi:https://doi.org/10.1128/MCB.00393-08.
Stork PJS, Fu Z, Lee SH, Simonetta A, Hansen J, Sheng M, et al. Does Rap1 deserve a bad rap? Trends Biochem Sci 2003;28:267–75, doi:https://doi.org/10.1111/j.1471-4159.2006.04195.x.
Fu Z, Lee SH, Simonetta A, Hansen J, Sheng M, Pak DTS. Differential roles of Rap1 and Rap2 small GTPases in neurite retraction and synapse elimination in hippocampal spiny neurons. J Neurochem 2007;100:118–31, doi:https://doi.org/10.1111/j.1471-4159.2006.04195.x.
Zhu JJ, Qin Y, Zhao M, Van Aelst L, Malinow R. Ras and Rap control AMPA receptor trafficking during synaptic plasticity. Cell 2002;110:443–55, doi:https://doi.org/10.1016/S0092-8674(02)00897-8.
Huang C-C, You J-L, Wu M-Y, Hsu K-S. Rap1-induced p38 mitogen-activated protein kinase activation facilitates AMPA receptor trafficking via the GDI.Rab5 complex: potential role in (s)-3,5-dihydroxyphenylglycine-induced long term depression. J Biol Chem 2004;279:12286–92, doi:https://doi.org/10.1074/jbc.M312868200.
Imamura Y, Matsumoto N, Kondo S, Kitayama H, Noda M. Possible involvement of Rap1 and Ras in glutamatergic synaptic transmission. Neuroreport 2003;14:1203–7, doi:https://doi.org/10.1097/01.wnr.0000081872.45938.1f.
Zhu Y, Pak D, Qin Y, Mccormack SG, Kim MJ, Baumgart JP, et al. Rap2-JNK removes synaptic AMPA receptors during depotentiation. Neuron 2005;46:905–16, doi:https://doi.org/10.1016/j.neuron.2005.04.037.
Pan B-X, Vautier F, Ito W, Bolshakov VY, Morozov A. Enhanced corticoamygdala efficacy and suppressed fear in absence of rap1. J Neurosci 2008;28:2089–98, doi:https://doi.org/10.1523/JNEUROSCI.5156-07.2008.
Kelly K. The RGK family: a regulatory tail of small GTP-binding proteins. Trends Cell Biol 2005;15:640–3, doi:https://doi.org/10.1016/j.tcb.2005.10.002.
Yang T, Terman JR. Regulating small G protein signaling to coordinate axon adhesion and repulsion. Small GTPases 2012;4:1–8, doi:https://doi.org/10.4161/sgtp.22765.
Ren WZ, Ng GY, Wang RX, Wu PH, O’Dowd BF, Osmond DH, et al. The identification of NP25: a novel protein that is differentially expressed by neuronal subpopulations. Brain Res Mol Brain Res 1994;22:173–85.
Mori K, Muto Y, Kokuzawa J, Yoshioka T, Yoshimura S, Iwama T, et al. Neuronal protein NP25 interacts with F-actin. Neurosci Res 2004;48:439–46, doi:https://doi.org/10.1016/j.neures.2003.12.012.
Ge L, Zhu M-M, Yang J-Y, Wang F, Zhang R, Zhang J-H, et al. Differential proteomic analysis of the anti-depressive effects of oleamide in a rat chronic mild stress model of depression. Pharmacol Biochem Behav 2015;131:77–86, doi:https://doi.org/10.1016/j.pbb.2015.01.017.
Carboni L, Vighini M, Piubelli C, Castelletti L, Milli A, Domenici E. Proteomic analysis of rat hippocampus and frontal cortex after chronic treatment with fluoxetine or putative novel antidepressants: CRF1 and NK1 receptor antagonists. Eur Neuropsychopharmacol 2006;16:521–37, doi:https://doi.org/10.1016/j.euroneuro.2006.01.007.
Meek S, Thomson AJ, Sutherland L, Sharp MGF, Thomson J, Bishop V, et al. Reduced levels of dopamine and altered metabolism in brains of HPRT knockout rats: a new rodent model of Lesch-Nyhan Disease. Sci Rep 2016;6:25592, doi:https://doi.org/10.1038/srep25592.
Jha MK, Jeon S, Suk K. Pyruvate dehydrogenase kinases in the nervous system: their principal functions in neuronal-glial metabolic interaction and neurometabolic disorders. Curr Neuropharmacol 2012;10:393–403, doi:https://doi.org/10.2174/157015912804143586.
Denton RM, Mccormack JG, Burnett P, Edgell NJ, Moule SK, Diggle TA. The hormonal regulation of pyruvate dehydrogenase complex. Adv Enzyme Regul 1996;36:183–98.
Chang HR, Tsai JP, Yang SF, Lin CK, Lian JD. Glutathione S-transferase M1 gene polymorphism is associated with susceptibility to impaired long-term allograft outcomes in renal transplant recipients. World J Surg 2013;37:466–72, doi:https://doi.org/10.1007/s00268-012-1815-6
Barańczyk-Kuźma A, Kuźma M, Gutowicz M, Kaźmierczak B, Sawicki J. Glutathione S-transferase pi as a target for tricyclic antidepressants in human brain. Acta Biochim Pol 2004;51:207–12 045101207.
Barańczyk-Kuźma A, Sawicki J, Kuźma M, Jagiełło J. Tricyclic antidepressants as inhibitors of brain glutathione-S-transferase. Pol Merkur Lekarski 2001;11:472–5, doi:https://doi.org/10.1016/S0968-0004(03)00087-2.
Author information
Authors and Affiliations
Corresponding author
Supplementary data
Rights and permissions
About this article
Cite this article
Głombik, K., Stachowicz, A., Trojan, E. et al. Mitochondrial proteomics investigation of frontal cortex in an animal model of depression: Focus on chronic antidepressant drugs treatment. Pharmacol. Rep 70, 322–330 (2018). https://doi.org/10.1016/j.pharep.2017.11.016
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.pharep.2017.11.016