Abstract
Objective
The aim of this study was to identify which metabolic syndrome criteria (WHO or IDF) better reflect the presence of non-alcoholic fatty liver disease (NAFLD) and to determine the prevalence of metabolic syndrome (MS) and NAFLD.
Methods
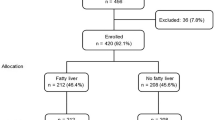
Two hundred and seventeen obese children and adolescents, 8–15 years of age (body mass index >95 p), were included in the study. Anthropometric measurements, blood pressure measurements, an oral glucose tolerance test and lipid profile were measured. MS was diagnosed according to WHO and IDF criteria. NAFLD risk ratio was assessed according to the two MS criteria.
Results
The prevalence of MS according to the IDF criteria was 43.3 %, and according to WHO criteria it was 55.2 %. NAFLD prevalence in the metabolic syndrome group according to IDF criteria was 25.5 % and this was statistically significant (p = 0.007). The prevalence of NAFLD was 20.8 % in the group with MS according to WHO criteria and this was not a statistically significant difference (p = 0.15). NAFLD hazard ratios were 7.06 (95 % CI 1.29–5.50) in the MS group according to IDF criteria and 2.02 (95 % CI 0.81–3.53) in the group with metabolic syndrome according to WHO criteria. IDF criteria were found to have a higher odds ratio.
Conclusion
The prevalence of MS depends on the diagnostic criteria used. IDF criteria give the best measure for the presence of NAFLD. NAFLD might be important as diagnostic criterion for MS.
Similar content being viewed by others
Abbreviations
- MS:
-
Metabolic syndrome
- IR:
-
Insulin resistance
- NAFLD:
-
Non-alcoholic fatty liver disease
- BMI:
-
Body mass index
- WC:
-
Waist circumference
- OGTT:
-
Oral glucose tolerance test
- LDL:
-
Low-density lipoprotein
- HDL:
-
High-density lipoprotein
- HOMA-IR:
-
Homeostasis model assessment of insulin resistance
- WHO:
-
World Health Organization criteria adapted for children
- IDF:
-
International Diabetes Federation
References
Atabek ME, Akyüz E, Selver Eklioğlu B et al (2011) The relationship between metabolic syndrome and left ventricular mass index in obese children. J Clin Res Pediatr Endocrinol 3:132–138
Pacifico L, Nobili V, Anania C et al (2011) Pediatric nonalcoholic fatty liver disease, metabolic syndrome and cardiovascular risk. World J Gastroenterol 14(17):3082–3091
Alp H, Karaarslan S, Selver Eklioğlu B et al (2013) Association between nonalcoholic fatty liver disease and cardiovascular risk in obese children and adolescents. Can J Cardiol 29(9):1118–1125
Seo HI, Cho YK, Lee WY et al (2012) Which metabolic syndrome criteria best predict the presence of non-alcoholic fatty liver disease? Diabetes Res Clin Pract 95:19–24
Kuczmarski RJ, Ogden CL, Guo SS et al (2002) 2000 CDC growth charts for the United States: methods and development. Vital Health Stat 11(246):1–190
Hatipoglu N, Ozturk A, Mazicioglu MM et al (2008) Waist circumference percentiles for 7- to 17-year-old Turkish children and adolescents. Eur J Pediatr 167:383–389
Kurtoglu S, Akin L, Kendirci M et al (2012) The absence of insulin resistance in metabolic syndrome definition leads to underdiagnosing of metabolic risk in obese patients. Eur J Pediatr 171:1331–1337
Conwell LS, Trost SG, Brown WJ et al (2004) Indexes of insulin resistance and secretion in obese children and adolescents: a validation study. Diabetes Care 27:314–319
Keskin M, Kurtoglu S, Kendirci M et al (2005) Homeostasis model assessment is more reliable than the fasting glucose/insulin ratio and quantitative insulin sensitivity check index for assessing insulin resistance among obese children and adolescents. Pediatrics 115:e500–e503
Goran MI, Gower BA (2001) Longitudinal study on pubertal insulin resistance. Diabetes 50:2444–2450
Katz A, Nambi SS, Mather K et al (2000) Quantitative insulin sensitivity check index: a simple, accurate method for assessing insulin sensitivity in humans. J Clin Endocrinol Metab 85:2402–2410
Alberti KG, Zimmet PZ (1998) Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med 15:539–553
Zimmet P, Alberti KG, Kaufman F et al (2007) IDF Consensus Group. The metabolic syndrome in children and adolescents—an IDF consensus report. Pediatr Diabetes 8:299–306
Cook S, Auinger P, Li C et al (2008) Metabolic syndrome rates in United States adolescents, from the National Health and Nutrition Examination Survey, 1999–2002. J Pediatr 152:165–170
Love-Osborne KA, Nadeau KJ, Sheeder J et al (2008) Presence of the metabolic syndrome in obese adolescents predicts impaired glucose tolerance and nonalcoholic fatty liver disease. J Adolesc Health 42:543–548
Caballería L, Pera G, Rodríguez L, Auladell MA, Bernad J, Canut S, Torán P (2012) Metabolic syndrome and nonalcoholic fatty liver disease in a Spanish population: influence of the diagnostic criteria used. Eur J Gastroenterol Hepatol 24(9):1007–1011
Strauss RS, Barlow SE, Dietz WH (2000) Prevalence of abnormal serum aminotransferase values in overweight and obese adolescents. J Pediatr 136:727–733
Sartorio A, Del Col A, Agosti F et al (2007) Predictors of non-alcoholic fatty liver disease in obese children. Eur J Clin Nutr 61:877–883
Chan DF, Li AM, Chu WC et al (2004) Hepatic steatosis in obese Chinese children. Int J Obes Relat Metab Disord 28:1257–1263
Gökçe S, Atbinici Z, Aycan Z, Cınar HG, Zorlu P (2013) The relationship between pediatric nonalcoholic fatty liver disease and cardiovascular risk factors and increased risk of atherosclerosis in obese children. Pediatr Cardiol 34:308–315
Uchil D, Pipalia D, Chawla M et al (2009) Non-alcoholic fatty liver disease (NAFLD)—the hepatic component of metabolic syndrome. J Assoc Physicians India 57:201–204
Hamaguchi M, Takeda N, Kojima T et al (2012) Identification of individuals with non-alcoholic fatty liver disease by the diagnostic criteria for the metabolic syndrome. World J Gastroenterol 7(18):1508–1516
Chen SH, He F, Zhou HL et al (2011) Relationship between nonalcoholic fatty liver disease and metabolic syndrome. J Dig Dis 12:125–130
Weiss R, Dziura J, Burgert TS et al (2004) Obesity and the metabolic syndrome in children and adolescents. N Engl J Med 350:2362–2374
Cizmecioğlu FM, Hatun S, Kalaça S (2008) Metabolic syndrome in obese Turkish children and adolescents: comparison of two diagnostic models. Turk J Pediatr 50:359–365
Isomaa B, Almgren P, Tuomi T et al (2001) Cardiovascular morbidity and mortality associated with the metabolic syndrome. Diabetes Care 24:683–689
Cook S, Weitzman M, Auinger P, Nguyen M, Dietz WH (2003) Prevalence of a metabolic syndrome phenotype in adolescents: findings from the third National Health and Nutrition Examination Survey, 1988–1994. Arch Pediatr Adolesc Med 157:821–827
Cruz ML, Weigensberg MJ, Huang TT et al (2004) The metabolic syndrome in overweight Hispanic youth and the role of insulin sensitivity. J Clin Endocrinol Metab 89:108–113
Atabek ME, Pirgon O, Kurtoglu S (2006) Prevalence of metabolic syndrome in obese Turkish children and adolescents. Diabetes Res Clin Pract 72:315–321
Fu JF, Shi HB, Liu LR et al (2011) Non-alcoholic fatty liver disease: an early mediator predicting metabolic syndrome in obese children? World J Gastroenterol 14(17):735–742
Ying X, Jiang Y, Qian Y et al (2012) Association between insulin resistance, metabolic syndrome and nonalcoholic fatty liver disease in Chinese adults. Iran J Public Health 41:45–49
Boyraz M, Cekmez F, Karaoglu A, Cinaz P, Durak M, Bideci A (2013) Serum adiponectin, leptin, resistin and RBP4 levels in obese and metabolic syndrome children with nonalcoholic fatty liver disease. Biomark Med 7:737–745
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Atabek, M.E., Selver Eklioglu, B. & Akyürek, N. Which metabolic syndrome criteria best predict non-alcoholic fatty liver disease in children?. Eat Weight Disord 19, 495–501 (2014). https://doi.org/10.1007/s40519-014-0129-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-014-0129-0