Abstract
Cutaneous adverse drug reactions (cADRs) encompass many types of clinical presentations, ranging from benign maculopapular eruption (MPE) to severe cutaneous adverse reactions (SCARs). The relationship between viral reactivation and drug eruptions has been widely observed and has provided a new direction for researchers to explore. In recent years, a number of studies have focused in particular on sequential human herpes virus (HHV) reactivation in drug reaction with eosinophilia and systemic symptoms (DRESS), and these studies have provided crucial evidence demonstrating that clinical presentations can be closely related to the dynamics of viral activity. The DRESS patients with long-term sequelae tended to present with viral activation, including sequential changes in serum cytokines, chemokines, and immune cells. Moreover, other cADRs might also be influenced by the reactivation of different viruses. In this study, we discuss recent progress in understanding the role of viral reactivation in cADRs and the possible pathomechanism underlying the drug-induced immune response.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cutaneous adverse drug reactions (cADRs) encompass many types of clinical presentations, ranging from benign maculopapular eruption (MPE) to severe cutaneous adverse reactions (SCARs), including Stevens–Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), drug reaction with eosinophilia and systemic symptoms (DRESS), acute generalized exanthematous pustulosis (AGEP), and generalized bullous fixed drug eruption (GBFDE) [1]. The underlying mechanisms leading to the unique clinical features and potentially life-threatening effects of SCARs have raised great interest among dermatologists and immunologists. Many studies have demonstrated that these idiosyncratic responses may be caused by complex immunological interactions among specific causative agents, T lymphocytes [2, 3], viral reactivation [4••], and the given patient’s genetic background [5].
The relationship between drug eruptions and viral infection or reactivation can be traced back to ampicillin-induced drug rash in patients with infectious mononucleosis [6], as well as the increased tendency of HIV-infected patients to develop drug eruptions [7]. In 1997, a case report first pointed out the association between human herpes virus 6 (HHV-6) and phenobarbital-induced hypersensitivity syndrome and reactive hemophagocytic syndrome [8]. The systemic hypersensitivity syndrome seen in that patient was identified as a case of DRESS, which is also sometimes known as drug-induced hypersensitivity syndrome (DIHS). Some clinical findings of DRESS/DIHS that are similar to those of viral infections (e.g., infectious mononucleosis) provide clues that associate the syndrome with viral reactivation. Since the aforementioned case report, sufficient evidence has accumulated to show the reactivation of herpes viruses, including HHV-6, Epstein–Barr virus (EBV), cytomegalovirus (CMV), herpes simplex virus (HSV), and varicella-zoster virus (VZV), in different cutaneous drug eruptions [9•]. Among all the cADRs, viral reactivation has most often been considered to play an important role in DRESS/DIHS [10••]. In this article, we will review the available evidence on the clinical and research aspects of viral reactivations in DRESS/DIHS and other cADRs.
Clinical Presentation of DRESS/DIHS
Before the identification and naming of DRESS in 1996 [11], this drug-induced systemic syndrome was given a variety of names based on the specific drugs that caused it, including anticonvulsant hypersensitivity syndrome [12], dapsone hypersensitivity (sulfone syndrome) [13], and allopurinol hypersensitivity syndrome [14]. This systemic hypersensitivity syndrome had been repeatedly reported as consisting of generalized rash with exfoliation, fever, lymphadenopathies, hematologic abnormalities, and visceral involvement until specific diagnostic criteria were proposed by, respectively, the RegiSCAR group [15] and a Japanese group [9•, 16]. Currently, the diagnosis of “DIHS” is more frequently made using the Japanese criteria. The major difference between the two diagnostic systems is the presence of HHV-6 reactivation, which was defined as one of the criteria in the Japanese system [9•, 16]. This important difference indicates a topic worth discussing: the role of viral reactivation in DRESS/DIHS.
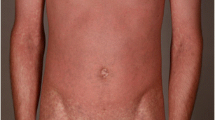
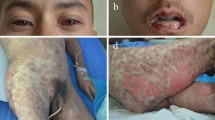
The symptoms of DRESS/DIHS typically begin 2–6 weeks after drug exposure [10••], but a long latency of onset is not uncommon for allopurinol-induced DRESS/DIHS [17]. Patients with typical symptoms are initially characterized by facial edema, generalized morbilliform eruption, and multiple lymphadenopathies. The rash later turns into large, coalescing erythematous patches and infiltrated plaques with different degrees of purpuric discoloration [10••]. Internal organ involvement distinguishes DRESS/DIHS from other SCARs. The most frequently involved organs are the liver and kidneys, with significant higher rates of involvement for those organs compared with those for the lung, central nervous system, and heart. Furthermore, eosinophilia and atypical lymphocytosis are commonly present in the blood [18]. Other laboratory findings include decreased B cell counts, hypogammaglobulinemia [19, 20], and hyperferritinemia [21]. It is frequently observed that a patient might experience initial paradoxical worsening in the first week after withdrawal of the culprit drug, as well as episodes of exacerbation in the following week [22]. Long-term follow-up of patients with DRESS/DIHS has revealed that several chronic complications may develop many years after resolution of the disease, such as autoimmune diseases and organ dysfunction [23•]. Histologically, diffuse or superficial lymphocytic infiltration characterizes the cutaneous lesions of DRESS/DIHS patients. Other features indicating different extents of inflammation include epidermal spongiosis, interface dermatitis with basal vacuolar degeneration or lichenoid infiltration, various degrees of dyskeratosis, and plump endothelial cells occasionally accompanied by red blood cell extravasation [10••]. Recently, one study showed that those patients who exhibit severe dyskeratosis on a skin biopsy examination tend to have more serious systemic involvement. Infiltrations of eosinophils or atypical lymphocytes, however, are not correlated with the severity of peripheral eosinophilia or atypical lymphocytosis [24]. Because pathological findings may be nondiagnostic, histological differential diagnosis between DRESS/DIHS, MPE, and viral exanthem still relies on clinical history and symptoms.
Viral Reactivations in DRESS/DIHS
After the first report of HHV-6 infection in a case of phenobarbital-induced hypersensitivity syndrome and reactive hemophagocytic syndrome in 1997 [8], two independent Japanese groups reported reactivation of HHV-6 in DIHS cases in 1998 [25, 26]. They also provided direct evidence showing the presence of HHV-6 DNA in peripheral blood mononuclear cells and skin lesions. Since then, many reports have identified the presence of HHV-6 in biopsy specimens taken from involved organs, including the liver [27], kidney [28], and lymph nodes [29, 30]. The rate of HHV-6 reactivation in patients with DRESS/DIHS has been investigated in several large case series. According to the results of studies with larger numbers of patients, the reactivation rate of HHV-6 ranges from 21.7 to 100 % [4••, 15, 31••, 32–34, 35••]. It has also been demonstrated, however, that severe DRESS/DIHS cases tend to have a relatively high viral reactivation rate of up to 85.7 % [15]. Furthermore, the reactivation of HHV-6 has often been observed to occur concurrently with severe disease presentation and a tendency towards disease flaring [4••, 33]. In one study, increased replication of HHV-6 DNA was revealed by quantitative polymerase chain reaction (qPCR) to occur at around 2–3 weeks after the onset of skin rash, often coincident with the clinical symptoms of recurrent fever or hepatitis, and then followed by an elevation of anti-HHV-6 immunoglobulin G (IgG) titer [33]. While many studies have underlined the fundamental importance of HHV-6 in DRESS/DIHS, reactivation of several other herpes viruses, including EBV, CMV, and HHV-7 have also been observed in patients with DRESS/DIHS [15, 31••, 32–34, 35••, 36]. The reactivation rates of different herpes viruses found by different studies are summarized in Table 1. One report showed the sequential activation of herpes viruses in four patients, starting with HHV-6 or EBV, followed by EBV or HHV-7, and then followed finally by CMV [36]. Recently, our group and Shiohara’s group confirmed the dynamic reactivations of herpes viruses in SCAR patients and highlighted the differences in the reactivation patterns among different types of SCARs. Both studies confirmed that HHV-6 reactivation was specific for DRESS/DIHS, while EBV and CMV reactivations could be observed in various cADRs [4••, 35••]. It is well known that HHVs share an important characteristic of being able to remain in a latent or persistent state in the human host [9•, 10••]. Furthermore, reactivation of herpes viruses usually occurs during periods of immunosuppression and may cause clinical symptoms or diseases [37]. Because of the varied severity of DRESS, topical potent or very potent corticosteroids may be a treatment option for patients with mild disease [38]. Systemic corticosteroid therapy, as the current mainstay of treatment for DRESS/DIHS, has been investigated for its effect on HHV reactivation in patients with DRESS/DIHS. In our recent study, we did not find any significant relationship between viral reactivation and the dosage of systemic corticosteroids [4••]. With regard to viral reactivation, higher viral reactivation rates and viral loads of HHV-6 and CMV, followed by prolonged durations of viral reactivation, have been observed in DRESS/DIHS patients receiving corticosteroids [35••]. In contrast, patients in a steroid-treated group showed lower expression levels of EBV DNA than patients in a non-steroid treated group [35••]. Because EBV has been associated with the pathogenesis of autoimmune diseases, it was speculated that using corticosteroids in the treatment of DRESS/DIHS may provide potential preventive and protective effects against the development of autoimmune sequelae [35••]. As such, slowly tapering off corticosteroids over a long period of time while monitoring viral loads has been recommended [39]. Because clinical trials to prove the safety and efficacy of systemic corticosteroids in treating DRESS/DIHS are still lacking, further study is needed to confirm the aforementioned hypothesis regarding their potential protective effects against autoimmune sequelae.
The Roles of Viral Reactions and the Immunopathogenesis of DRESS
The question whether viral reactivation is an initiator of DRESS/DIHS or a consequence caused by the drug-induced immune response has been debated. In recent years, many studies have sought to dissect the role of viral reactivation in the pathogenesis of DRESS/DIHS. It has been shown, for example, that the atypical lymphocytes in DRESS/DIHS patients are predominantly composed of CD8+ T cells [22], with significantly higher counts as compared to patients with SJS/TEN [40]. In addition, changes in cytokine levels have been observed in smaller numbers of DRESS/DIHS patients, with those patients exhibiting elevated levels of the inflammatory cytokines tumor necrosis factor (TNF)-α and interleukin (IL)-6 before or during HHV-6 reactivation [41, 42]. A significantly higher level of interferon (IFN)-γ in patients with DRESS/DIHS has also been detected in comparison with SJS/TEN cases [40]. Although these findings seem to be consistent with the concept that HHV-6 reactivation is a consequence of exaggerated drug-induced immunological effects, the wide range of days between symptom onset and blood collection makes interpretation difficult. Meanwhile, we have recently reported that significantly lower levels of many proinflammatory cytokines and chemokines, including IL-1β, IL-2, IL-6, IFN-γ, and TNF-α, were observed less than 10 days after skin rash onset in DRESS patients with HHV-6 reactivation when compared to those without HHV-6 reactivation. Significant elevation of these mediators was detected after HHV-6 reactivation, while increased levels of CXCL10 preceded the viral reactivation [4••]. CXCL10, also known as interferon gamma-induced protein 10, is secreted by different cell types in peripheral tissue, including keratinocytes and hepatocytes, in response to IFN-γ [43]. It has been shown to facilitate the recruitment of antiviral specific cytotoxic T lymphocytes into the target tissue [44]. From the observation of other diseases, CXCL10 has been associated with interface dermatitis and the pathogenesis of viral infections, which may be protected or promoted by the chemokine [43, 45].
The concept of viral reactivation and antiviral response in DRESS/DIHS was further explored by the identification of an anti-EBV CD8+ T lymphocyte. Samples were taken from ten patients with carbamazepine, minocycline, oxcarbazepine, sulfamethoxazole, or sulfasalazine-induced DRESS/DIHS, and nearly half of the amino acid sequences of TCRβ complementarity determining region 3 (CDR3) detected from circulating CD8+ T lymphocytes showed homology with CDR3 of EBV-specific CD8+ T lymphocytes. These expanded CD8+ T lymphocytes showing the same T cell repertoire were found in the skin lesions, livers, and blood of the patients, and their presence in these locations may have caused the symptoms of DRESS/DIHS. Furthermore, EBV-transformed B lymphocytes generated from patients’ peripheral blood mononuclear cells (PBMCs) and treated with common causative agents of DRESS/DIHS can increase their production of EBV [32]. These findings indicate that EBV may participate in the pathogenesis of DRESS/DIHS at an earlier stage. At this point, then, the following questions still exist. (1) In which stage do the drug-activated T cells cross-activate the viral-specific T lymphocytes? (2) Can oligoclonal expansion of viral-specific T cells also be detected with regard to HHV-6 or CMV? Further study is needed to address these questions.
Some studies have looked for explanations of the unique manifestations in DRESS/DIHS cases, such as late onset, B cell depletion, hypogammaglobulinemia, and the sequential reactivation of HHVs. It is worth noting that the decrease in B-lymphocyte counts and serum total immunoglobulin levels is often detected in the early stage of DRESS/DIHS [40]. Recently, the immunomodulatory function of regulatory T cells (Treg) has been implicated in DRESS/DIHS [3]. In that study, functional Treg expansion was detected at the acute stage of DRESS/DIHS. During the acute stage, the number of Treg cells was more abundant in the skin of DRESS/DIHS cases then that in TEN cases. Then, upon resolution, it was observed that the Treg cells lost their suppressive function [3]. In accordance with the findings of a previous study, one case of DIHS showed that HHV-6-infected cells from the lymph node were CD3 (+), CD4 (+), CD25 (+), and FoxP3 (+), resembling the surface markers of Treg cells [29]. On the other hand, the novel role of plasmacytoid dendritic cells (pDCs) in the antiviral response and autoimmunity has also been implicated in DRESS/DIHS. A study on pDCs in DIHS patients showed changes in the number of pDCs at about 3 to 4 weeks after disease onset, with a decrease of pDCs in peripheral blood but an increase of their expression in skin specimens [46]. Because the function of pDCs in regulating B cell growth and differentiation has been well-established in healthy people [47], this reduction of pDCs in the peripheral blood may be a possible reason for B cell depletion and hypogammaglobulinemia in DRESS/DIHS patients. The alteration of Treg cells and pDCs may provide an explanation for the clinical uniqueness of DRESS/DIHS and the further development of autoimmune sequelae [39]. However, due to the technical impracticability in blood sampling before symptom onset and the lack of an animal model for DRESS/DIHS, further well-designed research studies will be necessary to uncover the precise mechanisms involved.
Viral Reactivations and Long-Term Outcomes of DRESS
In our long-term follow-up study of DRESS/DIHS patients, we found that the overall cumulative incidence of long-term sequelae was 11.5 % [23•]. Recently, Kano et al. published the results of a multicenter survey conducted by the Asian Research Committee on Severe Cutaneous Adverse Reactions (ASCAR) [48•]. In accordance with our previous observations, the most frequently encountered chronic sequela was autoimmune thyroiditis, including Graves’ disease and Hashimoto’s thyroiditis, followed by type 1 diabetes mellitus (DM) and long-term dialysis resulting from the worsening of pre-existing renal failure. The interval between the onset of DRESS/DIHS and the development of type 1 DM was around 1 to 2 months, while the time interval for the detection of autoimmune thyroiditis varied from 2 months to 3 years. Other autoimmune diseases, such as systemic lupus erythematosus, autoimmune hemolytic anemia, alopecia areata, and vitiligo were also observed in the cohort as late complications [48•]. As mentioned above, the DRESS/DIHS patients with long-term sequelae tended to present with viral activation, including sequential changes in serum cytokines, chemokines, and immune cells [4••, 48•]. In contrast to the results of long-term follow-ups of DRESS/DIHS patients, the long-term sequelae of SJS/TEN patients have shown different patterns of chronic complications. Patients who have recovered from SJS/TEN commonly experience complications such as ocular and cutaneous sequelae but experience autoimmune sequelae less frequently [49]. The distinct patterns of viral reactivations and cytokine profiles may partly cause the clinical difference between DRESS/DIHS and SJS/TEN.
The Roles of Viral Reactivation in Other cADRs
Compared with DRESS/DIHS, SJS/TEN is less frequently associated with viral infection or reactivation. Only sporadic cases of SJS/TEN associated with viral infection have been reported, including cases involving varicella-zoster virus (VZV), HSV, EBV, HHV-6, and Merkel cell polyomavirus [50–53].
In our own recent report, we collected data from 17 SJS/TEN, 13 MPE, 5 GBFDE, and 4 EMM patients [4••]. All the patients survived the acute stage except for one SJS/TEN overlap patient who died of shock and multiple organ failure with a severity of illness score (SCORTEN) of 5 at day 1 of hospitalization. We found that EBV reactivation was detected in patients distributed in all the cADR groups. Specifically, the EBV reactivation rates were 29.4 % for SJS/TEN, 53.8 % for MPE, 80 % for GBFDE, and 50 % for EMM. The CMV reactivation rates, meanwhile, were 11.8 % for SJS/TEN and 0 % for the other cADRs. Only two patients (1 SJS patient on day 5 and 1 DRESS/DIHS patient on day 94) had HHV-7 reactivation, which was not associated with clinical aggravation of their symptoms [4••]. In a retrospective cohort study from Japan, increased EBV viral load was more frequently observed in SJS/TEN cases than in DRESS/DIHS cases (40 vs. <10 %, respectively) [35••]. However, there was no correlation between the EBV viral load and the clinical severity of SJS/TEN. The tendency to maintain an increased level of viral load after clinical resolution of the disease was also only found in patients with SJS/TEN. In contrast to the Japanese study [35••], our own observations of viral reactivation among different cADRs did not observe similar changes in EBV reactivation [4••]. Even though the discrepancy between the results of the two studies may have resulted from different definitions of reactivation and other variations between the two laboratories, we assumed that EBV reactivation may not be universally associated with SJS/TEN. AGEP is commonly caused by drugs, with drugs being implicated in more than 90 % of cases [54]. It is characterized by the acute onset of numerous nonfollicular pustules arising from diffuse erythematous base, fever, and leukocytosis. The duration between drug administration and symptom onset is typically short, around 24–48 h, and the skin eruptions are often resolved within 1 week after drug discontinuation [55]. Viral reactivation, as an infrequently encountered cause, was rarely reported in patients with AGEP. The offending viruses included enterovirus, EBV, CMV [54], and parvovirus B19 [56, 57]. Because of their rarity, the precise mechanisms of reactivations of these viruses remain unknown.
Conclusion
Over the past two decades, the rapid accumulation of new evidence has contributed to our understanding of the role of viral reactivation in the clinical manifestations and pathogenesis of drug eruptions. The close relationship between viral reactivation and DRESS/DIHS provides us with new insights into the multifactorial nature of drug hypersensitivity. However, further research is still needed to explore the link between initial drug-induced T cell activation, viral reactivation, and antiviral response.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance,•• Of major importance
Roujeau JC. Clinical heterogeneity of drug hypersensitivity. Toxicology. 2005;209(2):123–9.
Pichler WJ. Consequences of drug binding to immune receptors: Immune stimulation following pharmacological interaction with immune receptors (T-cell receptor for antigen or human leukocyte antigen) with altered peptide-human leukocyte antigen or peptide. Dermatol Sinica. 2013;31(4):181–90.
Takahashi R, Kano Y, Yamazaki Y, et al. Defective regulatory T cells in patients with severe drug eruptions: timing of the dysfunction is associated with the pathological phenotype and outcome. J Immunol. 2009;182(12):8071–9.
Chen YC, Chiang HH, Cho YT, et al. Human herpes virus reactivations and dynamic cytokine profiles in patients with cutaneous adverse drug reactions—a prospective comparative study. Allergy. 2015;70(5):568–75. This study confirmed that HHV-6 reactivation is specific for DRESS/DIHS, while EBV and CMV reactivations could be observed in various cADRs.
Chung WH, Hung SI, Chen YT. Human leukocyte antigens and drug hypersensitivity. Curr Opin Allergy Clin Immunol. 2007;7(4):317–23.
Pullen H, Wright N, Murdoch JM. Hypersensitivity reactions to antibacterial drugs in infectious mononucleosis. Lancet. 1967;2(7527):1176–8.
Coopman SA, Johnson RA, Platt R, et al. Cutaneous disease and drug reactions in HIV infection. N Engl J Med. 1993;328(23):1670–4.
Descamps V, Bouscarat F, Laglenne S, et al. Human herpesvirus 6 infection associated with anticonvulsant hypersensitivity syndrome and reactive haemophagocytic syndrome. Br J Dermatol. 1997;137(4):605–8.
Shiohara T. The role of viral infection in the development of severe drug eruptions. Dermatol Sinica. 2013;31(4):205–10. This paper summarized the major findings of viral infection/reactivation in DiHS.
Chen YC, Cho YT, Chang CY, et al. Drug reaction with eosinophilia and systemic symptoms: a drug-induced hypersensitivity syndrome with variable clinical features. Dermatol Sinica. 2013;31(4):196–204. This paper summarized the history, clinical presentation, histopathology and pathogenesis of DRESS.
Bocquet H, Bagot M, Roujeau JC. Drug-induced pseudolymphoma and drug hypersensitivity syndrome (Drug Rash with Eosinophilia and Systemic Symptoms: DRESS). Semin Cutan Med Surg. 1996;15(4):250–7.
Handfield-Jones SE, Jenkins RE, Whittaker SJ, et al. The anticonvulsant hypersensitivity syndrome. Br J Dermatol. 1993;129(2):175–7.
Tomecki KJ, Catalano CJ. Dapsone hypersensitivity: the sulfone syndrome revisited. Arch Dermatol. 1981;117(1):38–9.
Singer JZ, Wallace SL. The allopurinol hypersensitivity syndrome: unnecessary morbidity and mortality. Arthritis Rheum. 1986;29(1):82–7.
Eshki M, Valeyrie-Allanore L, Musette P, et al. Twelve-year analysis of severe cases of drug reaction with eosinophilia and systemic symptoms: a cause of unpredictable multiorgan failure. Arch Dermatol. 2009;145(1):67–72.
Shiohara T, Iijima M, Ikezawa Z, et al. The diagnosis of a DRESS syndrome has been sufficiently established on the basis of typical clinical features and viral reactivations. Br J Dermatol. 2007;156(5):1083–4.
Chen YC, Chiu HC, Chu CY. Drug reaction with eosinophilia and systemic symptoms: a retrospective study of 60 cases. Arch Dermatol. 2010;146(12):1373–9.
Cacoub P, Musette P, Descamps V, et al. The DRESS syndrome: a literature review. Am J Med. 2011;124(7):588–97.
Kano Y, Inaoka M, Shiohara T. Association between anticonvulsant hypersensitivity syndrome and human herpesvirus 6 reactivation and hypogammaglobulinemia. Arch Dermatol. 2004;140(2):183–8.
Boccara O, Valeyrie-Allanore L, Crickx B, et al. Association of hypogammaglobulinemia with DRESS (Drug Rash with Eosinophilia and Systemic Symptoms). Eur J Dermatol. 2006;16(6):666–8.
Ben m’rad M, Leclerc-Mercier S, Blanche P, et al. Drug-induced hypersensitivity syndrome: clinical and biologic disease patterns in 24 patients. Medicine (Baltimore). 2009;88(3):131–40.
Shiohara T, Inaoka M, Kano Y. Drug-induced hypersensitivity syndrome (DIHS): a reaction induced by a complex interplay among herpesviruses and antiviral and antidrug immune responses. Allergol Int. 2006;55(1):1–8.
Chen YC, Chang CY, Cho YT, et al. Long-term sequelae of drug reaction with eosinophilia and systemic symptoms: a retrospective cohort study from Taiwan. J Am Acad Dermatol. 2013;68(3):459–65. This study demonstrated the overall cumulative incidence of long-term sequelae in DRESS/DIHS.
Chi MH, Hui RC, Yang CH, et al. Histopathological analysis and clinical correlation of drug reaction with eosinophilia and systemic symptoms (DRESS). Br J Dermatol. 2014;170(4):866–73.
Suzuki Y, Inagi R, Aono T, et al. Human herpesvirus 6 infection as a risk factor for the development of severe drug-induced hypersensitivity syndrome. Arch Dermatol. 1998;134(9):1108–12.
Tohyama H, Yahata Y, Hashimoto K, et al. Severe hypersensitivity syndrome due to sulfasalazine associated with reactivation of human herpesvirus 6. Arch Dermatol. 1998;134(9):1113–7.
Mennicke M, Zawodniak A, Keller M, et al. Fulminant liver failure after vancomycin in a sulfasalazine-induced DRESS syndrome: fatal recurrence after liver transplantation. Am J Transplant. 2009;9(9):2197–202.
Miyashita K, Shobatake C, Miyagawa F, et al. Involvement of human herpesvirus 6 infection in renal dysfunction associated with DIHS/DRESS. Acta Derm Venereol. 2015; doi:10.2340/00015555-2149. [Epub ahead of print].
Mine S, Suzuki K, Sato Y, et al. Evidence for human herpesvirus-6B infection of regulatory T-cells in acute systemic lymphadenitis in an immunocompetent adult with the drug reaction with eosinophilia and systemic symptoms syndrome: a case report. J Clin Virol. 2014;61(3):448–52.
Saraya T, Mikoshiba M, Kamiyama H, et al. Evidence for reactivation of human herpesvirus 6 in generalized lymphadenopathy in a patient with drug-induced hypersensitivity syndrome. J Clin Microbiol. 2013;51(6):1979–82.
Kardaun SH, Sekula P, Valeyrie-Allanore L, et al. Drug reaction with eosinophilia and systemic symptoms (DRESS): an original multisystem adverse drug reaction. Results from the prospective RegiSCAR study. Br J Dermatol. 2013;169(5):1071–80. This large international study summarized the clinical presentations of DRESS/DIHS.
Picard D, Janela B, Descamps V, et al. Drug reaction with eosinophilia and systemic symptoms (DRESS): a multiorgan antiviral T cell response. Sci Transl Med. 2010;2(46):46ra62.
Tohyama M, Hashimoto K, Yasukawa M, et al. Association of human herpesvirus 6 reactivation with the flaring and severity of drug-induced hypersensitivity syndrome. Br J Dermatol. 2007;157(5):934–40.
Oskay T, Karademir A, Ertürk OI. Association of anticonvulsant hypersensitivity syndrome with herpesvirus 6, 7. Epilepsy Res. 2006;70(1):27–40.
Ishida T, Kano Y, Mizukawa Y, et al. The dynamics of herpesvirus reactivations during and after severe drug eruptions: their relation to the clinical phenotype and therapeutic outcome. Allergy. 2014;69(6):798–805. This study demonstrated that higher viral reactivation rates and viral loads of HHV-6 and CMV were observed in DRESS/DIHS patients receiving corticosteroids, followed by a prolonged time period of viral reactivation. On the contrary, patents in the steroid treatment group showed a lower EBV DNA than in the non-steroid treated group.
Kano Y, Hiraharas K, Sakuma K, et al. Several herpesviruses can reactivate in a severe drug-induced multiorgan reaction in the same sequential order as in graft-versus-host disease. Br J Dermatol. 2006;155(2):301–6.
De Bolle L, Naesens L, De Clercq E. Update on human herpesvirus 6 biology, clinical features, and therapy. Clin Microbiol Rev. 2005;18(1):217–45.
Funck-Brentano E, Duong TA, Bouvresse S, et al. Therapeutic management of DRESS: a retrospective study of 38 cases. J Am Acad Dermatol. 2015;72(2):246–52.
Shiohara T, Ushigome Y, Kano Y, et al. Crucial role of viral reactivation in the development of severe drug eruptions: a comprehensive review. Clin Rev Allergy Immunol. 2014; doi: 10.1007/s1201601484213.
Hirahara K, Kano Y, Mitsuyama Y, et al. Differences in immunological alterations and underlying viral infections in two well-defined severe drug eruptions. Clin Exp Dermatol. 2010;35(8):863–8.
Yoshikawa T, Fujita A, Yagami A, et al. Human herpesvirus 6 reactivation and inflammatory cytokine production in patients with drug-induced hypersensitivity syndrome. J Clin Virol. 2006;37 Suppl 1:S92–6.
Uno H, Kabashima K, Tohyama M, et al. TNF-α as a useful predictor of human herpesvirus-6 reactivation and indicator of the disease process in drug-induced hypersensitivity syndrome (DIHS)/drug reaction with eosinophilia and systemic symptoms (DRESS). J Dermatol Sci. 2014;74(2):177–9.
Liu M, Guo S, Hibbert JM, et al. CXCL10/IP-10 in infectious disease pathogenesis and potential therapeutic implications. Cytokine Growth Factor Rev. 2011;22(3):121–30.
Agostini C, Facco M, Siviero M, et al. CXC chemokines IP-10 and mig expression and direct migration of pulmonary CD8+/CXCR3+ T cells in the lungs of patients with HIV infection and T-cell alveolitis. Am J Respir Crit Care Med. 2000;162(4):1466–73.
Flier J, Boorsma DM, van Beek PJ, et al. Differential expression of CXCR3 targeting chemokines CXCL10, CXCL9, and CXCL11 in different types of skin inflammation. J Pathol. 2001;194(4):398–405.
Sugita K, Tohyama M, Watanabe H, et al. Fluctuation of blood and skin plasmacytoid dendritic cells in drug-induced hypersensitivity syndrome. J Allergy Clin Immunol. 2010;126(2):408–10.
Shaw J, Wang YH, Ito T, et al. Plasmacytoid dendritic cells regulate B-cell growth and differentiation via CD70. Blood. 2010;115(15):3051–7.
Kano Y, Tohyama M, Aihara M, et al. Sequelae in 145 patients with drug-induced hypersensitivity syndrome/drug reaction with eosinophilia and systemic symptoms: survey conducted by the Asian Research Committee on Severe Cutaneous Adverse Reactions (ASCAR). J Dermatol. 2015;42(3):276–82. This is the largest study demonstrated the long-term sequelae of DRESS/DIHS.
Yang CW, Cho YT, Chen KL, et al. Long-term sequelae of Stevens-Johnson syndrome/toxic epidermal necrolysis. Acta Derm Venereol (Stockh) 2015 (Accepted, in press).
Bay A, Akdeniz N, Calka O, et al. Primary varicella infection associated with Stevens-Johnson syndrome in a Turkish child. J Dermatol. 2005;32(9):745–50.
Brunet-Possenti F, Steff M, Marinho E, et al. Stevens-Johnson syndrome concurrent with primary Epstein-Barr virus infection. Ann Dermatol Venereol. 2013;140(2):112–5.
Teraki Y, Murota H, Izaki S. Toxic epidermal necrolysis due to zonisamide associated with reactivation of human herpesvirus 6. Arch Dermatol. 2008;144(2):232–5.
Maximova N, Granzotto M, Kiren V, et al. First description of Merkel Cell polyomavirus DNA detection in a patient with Stevens-Johnson syndrome. J Med Virol. 2013;85(5):918–23.
Speeckaert MM, Speeckaert R, Lambert J, et al. Acute generalized exanthematous pustulosis: an overview of the clinical, immunological and diagnostic concepts. Eur J Dermatol. 2010;20(4):425–33.
Szatkowski J, Schwartz RA. Acute generalized exanthematous pustulosis (AGEP): a review and update. J Am Acad Dermatol. 2015;doi:10.1016/j.jaad.2015.07.017. [Epub ahead of print]
Ofuji S, Yamamoto O. Acute generalized exanthematous pustulosis associated with a human parvovirus B19 infection. J Dermatol. 2007;34(2):121–3.
Calistru AM, Lisboa C, Cunha AP, et al. Acute generalized exanthematous pustulosis to amoxicillin associated with parvovirus B19 reactivation. Cutan Ocul Toxicol. 2012;31(3):258–61.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Dr. Che-Wen Yang, Dr. Yi-Chun Chen, Dr. Yung-Tsu Cho, and Dr. Chia-Yu Chu declare that they have no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical collection on Cutaneous Drug Reactions
Rights and permissions
About this article
Cite this article
Yang, CW., Chen, YC., Cho, YT. et al. The Role of Viral Reactivation in Drug Reaction with Eosinophilia and Systemic Symptoms and Other Cutaneous Adverse Drug Reactions (cADRs). Curr Derm Rep 5, 5–11 (2016). https://doi.org/10.1007/s13671-016-0124-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13671-016-0124-y