Abstract
Atopic dermatitis (AD) is the most common chronic inflammatory skin disorder in the USA and worldwide. There are significant differences in the epidemiology, phenotype, and genetics of AD in different racial and ethnic subgroups. In particular, patients of African descent have been found to have higher prevalence of AD in the USA and England, whereas Hispanic Americans have lower prevalence of AD. Further, African Americans have been found to have more severe disease and more comorbid allergic disorder. Patients of African descent appear to have different genetic risk factors, with less loss-of-function filaggrin 1 mutations and more filaggrin 2 mutations than patients of Northern or Eastern European origin. Finally, AD has different clinical phenotypes in African Americans, which clinicians need to recognize for the proper diagnosis and assessment of AD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Atopic dermatitis (AD) is a chronic, intermittent inflammatory skin disease that is characterized by intensely pruritic ill-demarcated erythematous patches and plaques. There are a number of racial and ethnic differences of the prevalence, severity, genetics, phenotype, and comorbidities of AD. This is of particular importance with the growing diversification of the population in the USA and other developed countries. It is estimated that Blacks and Hispanics will represent 13.4 and 19.1 % of the US population by the year 2020, respectively [1]. The goal of this manuscript is to review the racial and ethnic differences of AD.
Prevalence of Eczema in Children
Several US population-based studies of AD prevalence in childhood have recently been performed. Analysis of the 102,353 children from the 2003 National Survey of Children’s Health (NSCH) found 10.7 % prevalence of childhood AD in the USA, with significant variation between states and districts, ranging from 8.7 to 18.1 % [2•]. Subsequently, analysis of 91,642 children from the 2007 NSCH found 12.2 % prevalence of childhood AD [3•], suggesting that the prevalence of childhood AD increased in the interval period. Indeed, analysis of data from the National Health Interview Survey (NHIS) found that the prevalence of childhood eczema continuously increased between 1997 and 2011 [4].
The International Study of Asthma and Allergies in Childhood (ISAAC) used a standardized methodology to determine the international prevalence of AD [5]. There was a wide variation in prevalence values worldwide, from 0.9 % in India to 22.5 % in Ecuador at ages 6–7 years and from 0.2 % in China to 24.6 % in Colombia at ages 13–14 years.
Prevalence of Eczema in Adults
A recent study of a registry including 7157 children and adolescents with AD demonstrated that >80 % had persistent symptoms and were using medication to treat their AD even in adulthood [6]. This suggests that AD may be more common in adults than what was previously recognized. Indeed, studies of the 2010 and 2012 NHIS including 27,157 and 34,613 adults, respectively, found 10.2 and 7.2 % 1-year prevalence of eczema in the USA. Similarly, a study of the 2005–2006 NHIS including 4972 adults found 7.4 % lifetime prevalence of eczema [7]. International studies of AD in adults found prevalence ranging from 2.0 to 6.9 % [8–12]. The wide variation of prevalence is likely attributable to a combination of methodological and regional differences.
Background for Racial and Ethnic Disparities in AD
The varying prevalence values suggest that there are multiple environmental risk factors that occur in different regions. Such risk factors include climate [3•], residence in an urban area [2], water hardness and increased water exposure [13], early-life infectious exposures [14, 15], diet [16], obesity [17–20], and skin care practices [21]. Many of these risk factors differentially impact some sociodemographic groups. For example, previous studies found higher consumption of Western diet [22] and obesity [23] and less early-life vaccination [24, 25] in African Americans/Blacks than in Caucasians. Lower water quality is more likely in areas of greater poverty and lower socioeconomic status [26]. It is possible that racial and ethnic differences with respect to the above risk factors contribute toward disparities in AD. In addition, previous studies found that Black subjects had lower levels of skin ceramides than Asians and Caucasians [27] and higher levels of transepidermal water loss than Caucasians [28]; both of which may contribute toward AD [29, 30].
Racial and Ethnic Differences of Eczema Prevalence
Several recent US population-based studies have demonstrated differences in the prevalence of eczema in some racial and ethnic groups, suggesting that African Americans/Blacks have significantly higher prevalence of eczema compared with Whites [3•, 19, 31, 32]. In contrast, these studies also found that children of Hispanic origin had significantly lower prevalence of eczema [3•, 19, 31, 32]. A recent meta-analysis of 264,326 children and adolescents from NSCH 2003–2004 and 2005–2006, NHIS 2008–2012, and NSCH 2003–2004 and 2007–2008 found that African Americans/Blacks had higher odds of eczema (pooled odds ratio 1.574, 95 % confidence interval 1.573–1.575) and Hispanics had lower odds of eczema (0.767, 0.766–0.767) compared with Whites [33]. Several older studies in the USA and England also reported higher prevalence of childhood eczema in African Americans, Afro-Caribbeans, and Blacks [34–36].
Birthplace is another important consideration when examining the epidemiology of childhood AD and differences of AD prevalence across race/ethnicity. Given that AD starts in many patients within their first 6–12 months of life, early-life exposures likely play an important role in childhood AD. Silverberg et al. studied 91,642 children from the 2007–2008 NSCH and found that foreign-born American children had dramatically lower rates of eczema (as well as asthma, hay fever, and food allergy) than US-born American children [37•]. However, foreign-born children who resided in the USA for 10 years or more had significantly higher odds of eczema and allergic disease than those who lived in the USA for a shorter period of time [37•]. This observation was true in all racial and ethnic groups, including African Americans/Blacks and Hispanic Americans. Of note, the prevalence of eczema in US-born Hispanic Americans (10.7 %) was similar to that of US-born Whites (12.1 %), whereas US-born African Americans had considerably higher prevalence (20.2 %) [37•]. Thus, foreign birthplace and perhaps lack of acculturation might be the major protective factor against childhood AD in a subset of Hispanic Americans.
However, the role of race and ethnicity in the prevalence of adult eczema is less clear. A recent meta-analysis of 83,511 adults from the 2010 and 2012 NHIS and the 2003–2004 and 2005–2006 NHANES found that African Americans/Blacks, Hispanics, and Asians all had significantly lower odds of eczema compared with Caucasians/Whites [33]. One might speculate that there are phenotypic differences of disease, such that AD may “burn out” more in African Americans/Blacks than in Whites. However, in the abovementioned registry-based study of AD persistence in children and adolescents with AD found that Whites were more likely to have a 6-month disease-free period than other racial and ethnic groups [6]. Thus, it seems more likely that the lower prevalence of adult AD in racial and ethnic minorities is related to other factors, such as differences with respect to adult-onset disease and under-diagnosis secondary to decreased access to primary and specialist care in minority patients.
Racial Differences of AD Severity
Several studies have also demonstrated racial and ethnic differences with respect to AD severity. A study of 79,667 children and adolescents from the NSCH found in bivariate analyses that African Americans/Blacks and Hispanics were more likely to report moderate-to-severe eczema than Whites [38•]. However, in multivariate analyses, eczema severity was significantly associated with lower household income, but not race/ethnicity [38•]. This suggests that socioeconomic status plays an important role in eczema severity and may underlie the observed racial differences of eczema severity.
This observation of racial/ethnic disparities in eczema severity is reminiscent of those observed in asthma. Studies of racial and ethnic disparities in asthma found that African Americans/Black have worse asthma outcomes and Hispanics have lower quality of life secondary to asthma [39]. African-American/Black children were also found to use preventive medications for asthma less often than White or Hispanic children [40] and were more likely to have lower health literacy [39]. Thus, racial/ethnic disparities also appear to occur in the severity of allergic disease.
Racial Differences of the Genetics of AD
Filaggrin (FLG) is broken down into natural moisturizing factor (NMF) in the stratum corneum and plays an integral role in skin barrier function [41]. FLG loss-of-function gene mutations lead to a deficiency of NMF [42] and xerosis in AD [43]. Multiple FLG mutations have been identified and shown to be a risk factor for AD [44, 45]. A study found that FLG mutations are detected in 27.5 % of White and only 5.8 % of African-American children with AD [46••]. A follow-up study from the same group demonstrated common loss-of-function mutations of the filaggrin 2 gene in African Americans, which were not present in patients of Northern and Western European ancestry; children with FLG2 loss-of-function mutations were less likely to be symptom free over time [47•]. A study of 18 African-American children with AD and ichthyosis vulgaris and 17 African-American non-atopic controls found that only 22.2 % of those with AD and 5.9 % of controls were heterozygous for FLG null mutations [48]. Together, these studies suggest that FLG2 may play an important role in AD in African Americans, but that one or more factors other than FLG mutations are responsible for AD in African Americans/Blacks and other patient subsets. Very little is known about the genetics of AD in Hispanics/Latinos in general and Hispanic Americans in particular.
Racial Differences of AD Phenotype
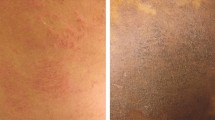
The classical presentations of AD are essentially the same across all racial and ethnic groups. However, there are a number of distinguishing features that occur more commonly in some racial and ethnic groups than others. Erythema in skin of color often appears hyperpigmented or violaceous. A previous study of Nigerian patients with AD found that 54.1 % had lichenoid lesions and 70.3 % had a perifollicular, micropapular rash, on the extensor aspects of the joints [49]. These phenotypic differences may delay the diagnosis and treatment of AD and allow for more severe disease to develop [30, 50]. When the lesions of AD resolve, they can cause persistent dyschromia or pigmentary alterations. These are almost always more pronounced in patients of racial and ethnic groups with darker skin [30].
Racial Differences of Allergic Disease in AD Patients
AD is associated with higher rates of allergic disorders, including asthma, hay fever, and food allergies [51]. These allergic disorders are mediated largely by T helper 2 (Th2)-mediated immune responses and increased levels of immunoglobulin E (IgE) [52]. While the inflammation in AD is also caused largely by Th2, there are similar Th2 responses in AD patients whether they have high IgE levels or not [53]. Thus, IgE does not appear to play a major role in the pathomechanism of AD. Rather, impaired skin barrier function in AD may allow for transcutaneous sensitization to allergens, thereby facilitating the development of systemic allergic disease. A recent study of 619 3-month-old infants who were exclusively breastfed elegantly demonstrated that AD predisposed to higher rates of food sensitization, including egg, cow’s milk, and peanuts [54]. Moreover, moderate-to-severe AD was associated with an even higher risk of food sensitization than mild AD [54]. Some authors have proposed the “atopic march,” where AD appears first in early life, followed by asthma and hay fever at later stages of life [55]. Given the abovementioned studies demonstrating increased prevalence and severity of AD in African Americans, it is logical that African-American/Black children with AD have greater risk for allergic disease.
Indeed, a birth cohort follow-up study in the Detroit metropolitan area found that African-American children at age 2 years were significantly more likely to have multiple positive IgE-specific tests; this group was also the most likely to have a diagnosis of AD [56]. Otherwise, little is known about the differential effects of AD on the development of allergic disease in African Americans/Blacks or other racial/ethnic subsets of patients.
Future Research
There is a growing body of epidemiological, clinical, and genetic evidence demonstrating racial and ethnic differences of AD. Yet, little is known about the clinical course and response to therapy in racial and ethnic minorities. A recent systematic review found that very few studies of systemic therapy in AD examined treatment efficacy in African Americans, most did not even document the racial/ethnic breakdown of their cohorts, and none of them were designed to identify the most effective therapies in African and Hispanic Americans [57]. Future clinical and therapeutic studies must include adequate representation of African Americans and other racial/ethnic subgroups in their cohorts. More well-designed prospective studies are needed to establish evidence-based guidelines for the evaluation and management of AD in all racial and ethnic subgroups.
Abbreviations
- AD:
-
Atopic dermatitis
- NSCH:
-
National Survey of Children’s Health
- NHIS:
-
National Health Interview Survey
- NHANES:
-
National Health and Nutrition Examination Survey
- ISAAC:
-
International Study of Asthma and Allergies in Childhood
- FLG:
-
Filaggrin
- NMF:
-
Natural moisturizing factor
- IgE:
-
immunoglobulin E
- Th2:
-
T helper 2
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
United States Census Bureau. Table 6. Percent of the projected population by race and Hispanic origin for the United States: 2015 to 2060 (NP2012). 2012 National Population Projections: Summary Tables. (Eds) (2012).
Shaw TE, Currie GP, Koudelka CW, Simpson EL. Eczema prevalence in the United States: data from the 2003 National Survey of Children’s Health. J Invest Dermatol. 2011;131(1):67–73. This manuscript provides the first US population-based estimates of the prevalence of childhood eczema from the 2003–2004 National Survey of Children’s Health and found that African Americans/Blacks have higher prevalence of childhood eczema.
Silverberg JI, Hanifin J, Simpson EL. Climatic factors are associated with childhood eczema prevalence in the United States. J Invest Dermatol. 2013;133(7):1752–9. This manuscript studied the effects of climate on the prevalence of childhood eczema in the USA from the 2007–2008 National Survey of Children’s Health and confirmed that African Americans/Blacks have higher prevalence of childhood eczema.
Jackson KD, Howie LD, Akinbami LJ. Trends in allergic conditions among children: United States, 1997-2011. NCHS data brief. 2013;121:1–8.
Odhiambo JA, Williams HC, Clayton TO, Robertson CF, Asher MI. Global variations in prevalence of eczema symptoms in children from ISAAC Phase Three. J Allergy Clin Immunol. 2009;124(6):1251–8. e1223.
Margolis JS, Abuabara K, Bilker W, Hoffstad O, Margolis DJ. Persistence of mild to moderate atopic dermatitis. JAMA Dermatol. 2014;150(6):593–600.
Garg NK, Silverberg JI. Eczema is associated with osteoporosis and fractures in adults: a US population-based study. J Allergy Clin Immunol. 2014. doi:10.1016/j.jaci.2014.10.043.
Muto T, Hsieh SD, Sakurai Y, et al. Prevalence of atopic dermatitis in Japanese adults. Br J Dermatol. 2003;148(1):117–21.
Saeki H, Tsunemi Y, Fujita H, et al. Prevalence of atopic dermatitis determined by clinical examination in Japanese adults. J Dermatol. 2006;33(11):817–9.
Marks R, Kilkenny M, Plunkett A, Merlin K. The prevalence of common skin conditions in Australian school students: 2. Atopic dermatitis. Br J Dermatol. 1999;140(3):468–73.
Dotterud LK, Falk ES. Atopic disease among adults in Northern Russia, an area with heavy air pollution. Acta Derm Venereol. 1999;79(6):448–50.
Herd RM, Tidman MJ, Prescott RJ, Hunter JA. Prevalence of atopic eczema in the community: the Lothian atopic dermatitis study. Br J Dermatol. 1996;135(1):18–9.
Chaumont A, Voisin C, Sardella A, Bernard A. Interactions between domestic water hardness, infant swimming and atopy in the development of childhood eczema. Environ Res. 2012;116:52–7.
Silverberg JI, Kleiman E, Silverberg NB, Durkin HG, Joks R, Smith-Norowitz TA. Chickenpox in childhood is associated with decreased atopic disorders, IgE, allergic sensitization, and leukocyte subsets. Pediatr All Immu. 2012;23(1):50–8.
Silverberg JI, Norowitz KB, Kleiman E, et al. Association between varicella zoster virus infection and atopic dermatitis in early and late childhood: a case-control study. J Allergy Clin Immunol. 2010;126(2):300–5.
Nagel G, Weinmayr G, Kleiner A, Garcia-Marcos L, Strachan DP, Group IPTS. Effect of diet on asthma and allergic sensitisation in the International Study on Allergies and Asthma in Childhood (ISAAC) Phase Two. Thorax. 2010;65(6):516–22.
Silverberg JI, Kleiman E, Lev-Tov H, et al. Association between obesity and atopic dermatitis in childhood: a case-control study. J Allergy Clin Immunol. 2011;127(5):1180–6. e1181.
Silverberg JI, Silverberg NB, Lee-Wong M. Association between atopic dermatitis and obesity in adulthood. Br J Dermatol. 2012;166(3):498–504.
Silverberg JI, Simpson EL. Association between obesity and eczema prevalence, severity and poorer health in US adolescents. Dermatitis. 2014;25(4):172–81.
Zhang A, Silverberg JI. Association of atopic dermatitis with overweight and obesity: a systematic review and meta-analysis. Journal of the American Academy of Dermatology, In Press (2014).
Simpson EL, Chalmers JR, Hanifin JM, et al. Emollient enhancement of the skin barrier from birth offers effective atopic dermatitis prevention. J Allergy Clin Immunol. 2014;134(4):818–23.
Block JP, Scribner RA, DeSalvo KB. Fast food, race/ethnicity, and income: a geographic analysis. Am J Prev Med. 2004;27(3):211–7.
Strauss RS, Pollack HA. Epidemic increase in childhood overweight, 1986-1998. JAMA. 2001;286(22):2845–8.
Kenyon TA, Matuck MA, Stroh G. Persistent low immunization coverage among inner-city preschool children despite access to free vaccine. Pediatrics. 1998;101(4 Pt 1):612–6.
From the Centers for Disease Control and Prevention. Vaccination coverage by race/ethnicity and poverty level among children aged 19-35 months—United States, 1996. JAMA. 1997;278(20):1655–6.
Subbaraman R, Shitole S, Shitole T, et al. The social ecology of water in a Mumbai slum: failures in water quality, quantity, and reliability. BMC Public Health. 2013;13:173.
Jungersted JM, Hogh JK, Hellgren LI, Jemec GB, Agner T. Ethnicity and stratum corneum ceramides. Br J Dermatol. 2010;163(6):1169–73.
Wesley NO, Maibach HI. Racial (ethnic) differences in skin properties: the objective data. Am J Clin Dermatol. 2003;4(12):843–60.
Proksch E, Folster-Holst R, Brautigam M, Sepehrmanesh M, Pfeiffer S, Jensen JM. Role of the epidermal barrier in atopic dermatitis. J Dtsch Dermatol Ges. 2009;7(10):899–910.
Vachiramon V, Tey HL, Thompson AE, Yosipovitch G. Atopic dermatitis in African American children: addressing unmet needs of a common disease. Pediatr Dermatol. 2012;29(4):395–402.
Silverberg JI, Silverberg NB. Childhood atopic dermatitis and warts are associated with increased risk of infection: a US population-based study. J Allergy Clin Immunol. 2014;133(4):1041–7.
Silverberg JI. Association between childhood atopic dermatitis, malnutrition and low bone mineral density: a US population based study. Pediatr All Immu. 2014. doi:10.1111/pai.12315.
Silverberg JI, Paller AS. Association between eczema and stature in 9 US population-based studies. JAMA Dermatol. 2014. doi:10.1001/jamadermatol.2014.3432.
Schachner L, Ling NS, Press S. A statistical analysis of a pediatric dermatology clinic. Pediatr Dermatol. 1983;1(2):157–64.
Davis LR, Marten RH, Sarkany I. Atopic eczema in European and Negro West Indian infants in London. Br J Dermatol. 1961;73:410–4.
Williams HC, Pembroke AC, Forsdyke H, Boodoo G, Hay RJ, Burney PG. London-born black Caribbean children are at increased risk of atopic dermatitis. J Am Acad Dermatol. 1995;32(2 Pt 1):212–7.
Silverberg JI, Simpson EL, Durkin HG, Joks R. Prevalence of allergic disease in foreign-born American children. JAMA Pediatr. 2013;167(6):554–60. This manuscript analyzed data from the 2007–2008 National Survey of Children’s Health and demonstrated that foreign birthplace in all races and ethnicities is protective against childhood eczema.
Silverberg JI, Simpson EL. Associations of childhood eczema severity: a US population-based study. Dermatitis. 2014;25(3):107–14. This manuscript analyzed data from the 2007–2008 National Survey of Children’s Health and found that African Americans/Blacks have higher rates of moderate-to-severe childhood eczema.
Curtis LM, Wolf MS, Weiss KB, Grammer LC. The impact of health literacy and socioeconomic status on asthma disparities. J Asthma. 2012;49(2):178–83.
McDaniel MK, Waldfogel J. Racial and ethnic differences in the management of childhood asthma in the United States. J Asthma. 2012;49(8):785–91.
Rawlings AV, Harding CR. Moisturization and skin barrier function. Dermatol Ther. 2004;17(1):43–8.
Kezic S, Kemperman PM, Koster ES, et al. Loss-of-function mutations in the filaggrin gene lead to reduced level of natural moisturizing factor in the stratum corneum. J Invest Dermatol. 2008;128(8):2117–9.
O’Regan GM, Sandilands A, McLean WH, Irvine AD. Filaggrin in atopic dermatitis. J Allergy Clin Immunol. 2009;124(3 Suppl 2):R2–6.
Henderson J, Northstone K, Lee SP, et al. The burden of disease associated with filaggrin mutations: a population-based, longitudinal birth cohort study. J Allergy Clin Immunol. 2008;121(4):872–7. e879.
Weidinger S, O’Sullivan M, Illig T, et al. Filaggrin mutations, atopic eczema, hay fever, and asthma in children. J Allergy Clin Immunol. 2008;121(5):1203–9. e1201.
Margolis DJ, Apter AJ, Gupta J, et al. The persistence of atopic dermatitis and filaggrin (FLG) mutations in a US longitudinal cohort. J Allergy Clin Immunol. 2012;130(4):912–7. This study found that patients of African descent are less likely to have the common filaggrin gene null mutations that patients of Northern or Eastern European descent.
Margolis DJ, Gupta J, Apter AJ, et al. Filaggrin-2 variation is associated with more persistent atopic dermatitis in African American subjects. J Allergy Clin Immunol. 2014;133(3):784–9. This study demonstrated novel null mutations of the filaggrin 2 gene in patients of African descent.
Polcari I, Becker L, Stein SL, Smith MS, Paller AS. Filaggrin gene mutations in African Americans with both ichthyosis vulgaris and atopic dermatitis. Pediatr Dermatol. 2014;31(4):489–92.
Nnoruka EN. Current epidemiology of atopic dermatitis in south-eastern Nigeria. Int J Dermatol. 2004;43(10):739–44.
Ben-Gashir MA, Hay RJ. Reliance on erythema scores may mask severe atopic dermatitis in black children compared with their white counterparts. Br J Dermatol. 2002;147(5):920–5.
Silverberg JI, Simpson EL. Association between severe eczema in children and multiple comorbid conditions and increased healthcare utilization. Pediatr All Immu. 2013;24(5):476–86.
Jansen HM, Kapsenberg ML. T-cell regulation in allergic reactions. Neth J Med. 1994;45(6):319–28.
Suarez-Farinas M, Dhingra N, Gittler J, et al. Intrinsic atopic dermatitis shows similar TH2 and higher TH17 immune activation compared with extrinsic atopic dermatitis. J All Clin Immu. 2013;132(2):361–70.
Flohr C, Perkin M, Logan K, et al. Atopic dermatitis and disease severity are the main risk factors for food sensitization in exclusively breastfed infants. J Invest Dermatol. 2014;134(2):345–50.
Spergel JM, Paller AS. Atopic dermatitis and the atopic march. J All Clin Immu. 2003;112(6):S118–127.
Havstad S, Johnson CC, Kim H, et al. Atopic phenotypes identified with latent class analyses at age 2 years. J All Clin Immu. 2014;134(3):722–7. e722.
Bhattacharya T, Silverberg JI. Efficacy of systemic treatments for atopic dermatitis in racial and ethnic minorities in the United States. JAMA Dermatol. 2014;150(11):1232–4.
Compliance with Ethics Guidelines
Conflict of Interest
JI Silverberg declares no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Epidemiology
Rights and permissions
About this article
Cite this article
Silverberg, J.I. Racial and Ethnic Disparities in Atopic Dermatitis. Curr Derm Rep 4, 44–48 (2015). https://doi.org/10.1007/s13671-014-0097-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13671-014-0097-7