Abstract
Objective
To determine the burden of early growth faltering and understand the care practices for small and sick babies discharged from newborn units in the district.
Study design
Observational and follow-up study.
Participants
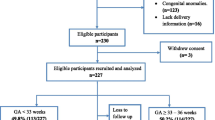
512 babies discharged from two Special Newborn Care Units (SNCUs) and four Newborn Stabilization Units (NBSUs) in two districts of Himachal Pradesh.
Methods
Anthropometric assessments, interview of mothers and Accredited Social Health Activists (ASHAs) conducted between August, 2018 and March, 2019. Change in weight-for-age z-score (ΔWAZ) of <−0.67SD between birth and assessment was used to define growth faltering.
Outcomes
Proportion of growth faltering (or catch-down growth) in small and sick babies discharged from SNCUs and NBSUs, and infant care practices.
Results
Growth faltering was observed in a significant proportion of both term (30%) and preterm (52.6%) babies between 1 to 4 months of age. Among babies with growth faltering (n=180), 73.9% received a home visit by ASHA, and only 36.7% received a follow-up visit at a facility. There were 71.3% mothers counselled at discharge (mostly informed about breast feeding). Most (96.7%) mothers did not perceive inadequate weight gain in their babies post-discharge. During home visits, ASHAs weighed 61.6% of the infants with growth faltering. Amongst infants who had growth faltering, only 49.6% of mothers had been provided information about their infant’s growth and 57.1% mothers had received breastfeeding counselling.
Conclusion
Small and sick newborn infants (both term and preterm babies) discharged from special care newborn units are at increased risk of early growth faltering. Follow-up care provided to these infants is inadequate. There is a need to strengthen both facility-based and home-based follow up of small and sick newborn infants discharged from newborn care facilities.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
National Family Health Survey (NFHS-4) 2015–16 India. Int Inst Popul Sci ICF. 2017;1–192.
World Health Organization. Survive and Thrive: Transforming Care for Every Small and Sick Newborn, 2019. WHO; 2019. Accessed April 16, 2022. Available from: https://www.who.int/maternal_child_adolescent/documents/care-smallsick-newborns-survive-thrive/en/
World Health Organization. Standards for improving Quality of Care for Small and Sick Newborns in Health Facilities, 2020. WHO; 2020. Accessed April 16, 2022. Available from: https://www.who.int/publications/i/item/9789240010765.
Lawn JE, Blencowe H, Oza S, et al. Every Newborn: progress, priorities, and potential beyond survival. Lancet. 2014;384:189–205.
Rover MM, Viera CS, Silveira RC, et al. Risk factors associated with growth failure in the follow-up of very low birth weight newborns. J Pediatr (Rio J). 2016;92:307–313.
Soni A, Fahey N, Bhutta ZA, et al. Early childhood undernutrition, preadolescent physical growth, and cognitive achievement in India: A population-based cohort study. PLoS Med. 2021;18:10.
Zhang L, Li Y, Liang S, Liu XJ, Kang FL, Li GM. Postnatal length and weight growth velocities according to Fenton reference and their associated perinatal factors in healthy late preterm infants during birth to term-corrected age: an observational study. Ital J Pediatr. 2019;45:1.
Rustogi D, Yadav S, Ramji S, Mishra TK. Growth patterns in small for gestational age babies and correlation with insulinlike growth factor-1 levels. Indian Pediatr. 2018;55:975–78.
Jain V, Kumar B, Khatak S. Catch-up and catch-down growth in term healthy indian infants from birth to two years: A prospective cohort study. Indian Pediatr. 2021;58:325–31.
Rehman AM, Gladstone BP, Verghese VP, et al. Chronic growth faltering amongst a birth cohort of Indian children begins prior to weaning and is highly prevalent at three years of age. Nutr J. 2009;8:44.
Spencer NJ. Failure to think about failure to thrive. Arch Dis Child. 2007;92:95–96.
Aneja S, Kumar P, Choudhary TS, et al. Growth faltering in early infancy: highlights from a two-day scientific consultation. BMC Proc. 2020;14:12.
Olsen EM, Skovgaard AM, Weile B, Jørgensen T. Risk factors for failure to thrive in infancy depend on the anthropometric definitions used: the Copenhagen County Child Cohort. Paediatr Perinat Epidemiol. 2007;21:418–31.
National Family Health Survey (NFHS-5) 2019–21 India. Int Inst Popul Sci ICF. 2017.
Ross ES, Krebs NF, Shroyer ALW, Dickinson LM, Barrett PH, Johnson SL. Early growth faltering in healthy term infants predicts longitudinal growth. Early Hum Dev. 2009; 85:583–8.
Mukhopadhyay K, Mahajan R, Louis D, Narang A. Longitudinal growth of very low birth weight neonates during first year of life and risk factors for malnutrition in a developing country. Acta Paediatr. 2013;102:278–81.
Kumar H, Bhat AA, Alwadhi V, et al. Special newborn care plus project in India: Preliminary Findings from community-based follow-up of newborns discharged from facilities. Indian Pediatr. 2021;58:354–57.
INTERGROWTH-21st.The International Fetal and Newborn Growth Consortium for the 21st Century. Intergrowth 2014. Accessed June 24, 2022. Available from: https://intergrowth21.tghn.org/standards-tools/
World Health Organization. WHO Child Growth Standards, 2006.WHO; 2006. Accessed June 24, 2022. Available from: https://www.who.int/tools/child-growth-standards
Cheikh Ismail L, Knight HE, Ohuma EO, Hoch L, Chumlea WC. Anthropometric standardisation and quality control protocols for the construction of new, international, fetal and newborn growth standards: the INTERGROWTH-21st Project. BJOG. 2013;120:48–55.
13th Common Review Mission: Report. National Health Mission, Ministry of Health and Family Welfare, Governent of India, 2019.
Ramji S, Jain A. National Program for RMNCH+A: Newer strategies for improving the newborn health in India. Indian J Pediatr. 2019;86:617–21.
Bansal SC, Nimbalkar SM, Shah NA, Shrivastav RS, Phatak AG. Evaluation of knowledge and skills of home based newborn care among accredited social health activists (ASHA). Indian Pediatr. 2016;53:689–91.
Goswami VP, Rai S, Dixit S, Sarose S, Banseria R. Impact of training on ASHAs in selected districts of Madhya Pradesh. Peoples J Sci Res. 2016;9:50.
McConnell M, Ettenger A, Rothschild CW, Muigai F, Cohen J. Can a community health worker administered postnatal checklist increase health-seeking behaviors and knowledge? evidence from a randomized trial with a private maternity facility in Kiambu County, Kenya. BMC Pregnancy Childbirth. 2016;16:136.
Barua K, Baruah R. Application of growth monitoring charts by health care providers in village health and nutrition day (VHND) setting in rural Kamrup. Indian J Community Health. 2014;26:322–6.
Roth DE, Krishna A, Leung M, et al. Early childhood linear growth faltering in low-income and middle-income countries as a whole-population condition: analysis of 179 Demographic and Health Surveys from 64 countries (1993–2015). Lancet Glob Health. 2017;5:e1249–57.
Acknowledgement
We extend our sincerest gratitude to Late Dr M K Bhan and Dr VK Paul (Department of Pediatrics, AIIMS, Delhi) under whose guidance the study was conceptualized. The hospital management team, field workers, and the entire research team (Ajay Sharma, Anchal Dhiman, Kashika Sharma, Lakshmi Thakur, Medhavi Manish, Nidhi Mudgil, Rajendra P. Ola, Sanjeev Kumar, Sarita Bisht, Priyanka Devi, Priyanka Pundir, Aditi KC) that made this study possible. We would also like to thank Dr Pradeep Debata and Dr Shobhna Gupta (Safdarjung Hospital, New Delhi) who were involved in the training of the research team.
Funding
Funding: Jointly supported by Knowledge Integration and Translational Platform (KnIT) (supported by DBT-BMGF-BIRAC-Wellcome) and Gates Ventures. Project reference numbers: BIRAC/PMU/2016/KnIT/001 (PRIV010) and bgC3 — Research Services 2019 (PRIV025).
Author information
Authors and Affiliations
Contributions
Contributors: SR, HC, RDG, RMP, RG, and JJ: involved in the conceptualization of the study; SR, HC, RDG, RMP, RG along with late Dr MK Bhan: provided overall guidance across different steps involved in the study; MS: facilitated the study in the state of HP, JJ, MN, along with the research team were involved in the overall study conduct and data collection process with inputs provided by SR, HC, RDG, JJ and RJ compiled and analyzed the data, drafted the manuscript with technical inputs from SR, HC, RDG, RMP, RG, and MS in analysis and finalizing the manuscript. All the authors have reviewed and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval: Institutional Ethics Committee, Maulana Azad Medical College; No. F1/IEC/MAMC/62/02/2018/268, dated March 30, 2018.
Competing interests: None stated.
Additional information
Note: Additional matter related to this article is available with the web version at https://www.indianpediatrics.net
Rights and permissions
About this article
Cite this article
Joseph, J., Jalal, R., Nagrath, M. et al. Growth Faltering Among Discharged Babies from Inpatient Newborn Care Facilities: Learnings from Two Districts of Himachal Pradesh. Indian Pediatr 59, 763–768 (2022). https://doi.org/10.1007/s13312-022-2618-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-022-2618-y