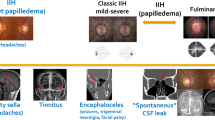
Opinion statement
A thorough assessment of vision with special attention to formal visual field testing is the cornerstone to decision making in idiopathic intracranial hypertension. After the diagnosis of idiopathic intracranial hypertension has been established, vision should be thoroughly assessed. If there is no visual loss, the patient can be followed carefully. In patients with symptoms and only a few signs (eg, mild blind-spot enlargement), acetazolamide, 1 to 2 g, or another diuretic should be initiated. In patients with progressive visual loss in whom maximal diuretic therapy fails and in those who on initial evaluation have significant recent visual loss that does not respond to maximal diuretic therapy, optic nerve sheath decompression or lumbar peritoneal shunting should be carried out. With all treatments, weight loss should be encouraged. All patients should be evaluated regularly with visual field testing.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References and Recommended Reading
Durcan FJ, Corbett JJ, Wall M: The incidence of pseudotumor cerebri: population studies in Iowa and Louisiana. Arch Neurol 1988, 45:875–877.
Corbett JJ, Savino PJ, Thompson HS, et al.: Visual loss in pseudotumor cerebri: follow-up of 57 patients from five to 41 years and a profile of 14 patients with permanent severe visual loss. Arch Neurol 1982, 39:461–474. This classic article shows visual loss in up to one third of patients with IIH and demonstrates that IIH is a chronic illness.
Corbett JJ, Thompson HS: The rational management of idiopathic intracranial hypertension. Arch Neurol 1989, 46:1049–1051. This article remains a valuable overview of treatment.
Wall M, George D: Idiopathic intracranial hypertension: a prospective study of 50 patients. Brain 1991, 114:155–180. A classic prospective study of patients with IIH.
Giuseffi V, Wall M, Siegel PZ, et al.: Symptoms and disease associations in idiopathic intracranial hypertension (pseudotumor cerebri): a case-control study. Neurology 1991, 41(2):239–244. A case-control study looking at diseases associated with IIH.
Ireland B, Corbett JJ, Wallace RB: The search for causes of idiopathic intracranial hypertension: a preliminary casecontrol study. Arch Neurol 1990, 47:315–320. The first case-control study to study the association with IIH.
Corbett JJ: Problems in the diagnosis and treatment of pseudotumor cerebri. Can J Neurol Sci 1983, 10:221–229.
Weisberg LA: Benign intracranial hypertension. Medicine 1975, 54:197–206.
Kupersmith MJ, Gamell L, Turbin R, et al.: Effect of weight loss on the course of idiopathic intracranial hypertension in women. Neurolog 1998, 50:1094–1098. One of the best articles showing that weight loss leads to improvement in symptoms and signs of IIH.
Tomsak RL, Niffenegger AS, Remler BF: Treatment of pseudotumor cerebri with Diamox (acetazolamide). J Neuroophthalmol 1988, 8:93–98.
Digr KB, Corbett JJ: Treatment of IIH. In Neuro-ophthalmic Disorders: Diagnosis and Management. Edited by Tusa RJ, Newman SR. New York: Marcel Dekker; 1995.
Schoeman JF: Childhood pseudotumor cerebri: clinical and intracranial pressure response to acetazolamide and furosemide treatment in a case series. J Child Neurol 1994, 9:130–134.
Goodwin J: Treatment of idiopathic intracranial hypertension with digoxin. Ann Neurol 28:248, 1990.
Jefferson A, Clark J: Treatment of benign intracranial hypertension by dehydrating agents with particular reference to the measurement of the blind spot area as a means of recording improvement. J Neurol Neurosurg Psychiatry 1976, 9:627–639.
Liu GT, Glaser JS, Schatz NJ: High-dose methylprednisolone and acetazolamide for visual loss in pseudotumor cerebri. Am J Ophthalmol 1994, 118(1):88–96.
Johnston I, Besser M, Morgan MK: Cerebrospinal fluid diversion in the treatment of benign intracranial hypertension. J Neurosurg 1988, 69:195–202.
Wang SJ, Silberstein SD, Patterson S, et al.: Idiopathic intracranial hypertension without papilledema. Neurolog 1998, 51:245–249.
Sergott RC, Savino PJ, Bosley TM: Optic nerve sheath decompression: a clinical review and proposed pathophysiologic mechanism. Aust N Z J Ophthalmol 1990, 18:365–373.
Kelman SE, Heaps R, Wolf A, et al.: Optic nerve decompression surgery improves visual function in patients with pseudotumor cerebri. Neurosurger 1992, 30:391–395.
Acheson JF, Green WT, Sanders MD: Optic nerve sheath decompression for the treatment of visual failure in chronic raised intracranial pressure. J Neurol Neurosurg Psychiatry 1994, 57:1426–1429.
Bourman ND, Spoor TC, Ramocki JM: Optic nerve sheath decompression for pseudotumor cerebri. Arch Ophthalmol 1988, 106:1378–1383.
Tse DT, Nerad JA, Anderson RL, et al.: Optic nerve sheath fenestration: a lateral orbitotomy approach. Arch Ophthalmol 1988, 106:1458–1462.
Eggenberger ER, Miller NR, Vitale S: Lumboperitoneal shunt for the treatment of pseudotumor cerebri. Neurology 1996, 46:1524–1530. The authors report on a series of shunt placements and the associated visual outcomes.
Johnston I, Paterson A, Besser M: The treatment of benign intracranial hypertension: a review of 134 cases. Surg Neurol 1981, 16:218–224.
Rosenberg ML, Corbett JJ, Smith C, et al.: Cerebrospinal fluid diversion procedures in pseudotumor cerebri. Neurolog 1993, 43:1071–1072.
Wall M: Idiopathic intracranial hypertension. Neurol Clin 1991, 9:73–94. One of the better reviews of IIH.
Sugerman HJ, Felton WL, Salvant JB, et al.: Effects of surgically induced weight loss on idiopathic intracranial hypertension in morbid obesity. Neurology 1995, 45:1655–1659. The first study to show that surgically induced weight loss causes an improvement in signs and symptoms of IIH.
Friedman DI, Ingram P, Rogers MAM: Low tyramine diet in the treatment of idiopathic intracranial hypertension: a pilot study. Neurolog 1998, 50:A4.
Rubin RC, Henderson ES, Ommaya AK, et al.: The production of cerebrospinal fluid in man and its modification by acetazolamide. J Neurosurg 1966, 25:430–436.
Tawil R, Moxley RT, Griggs RC: Acetazolamide-induced nephrolithiasis: implications for treatment of neuromuscular disorders. Neurology 1993, 43:1105–1106.
Resor SR, Resor LD: Chronic acetazolamide monotherapy in the treatment of juvenile myoclonic epilepsy. Neurology 1990, 40:1677–1681.
Soler D, Cox T, Bullock P, et al.: Diagnosis and management of benign intracranial hypertension. Arch Dis Child 1998, 78:89–94.
Absolon MJ: Unusual presentations of benign intracranial hypertension: early treatment with oral glycerol. Br J Ophthalmol 1966, 50:683–688.
Buckell M, Walsh L: Effect of glycerol by mouth on raised intracranial pressure in man. Lancet 1964, 2(7370):1151–1152.
Burgett RA, Purvin VA, Kawasaki A: Lumboperitoneal shunting for pseudotumor cerebri. Neurology 1997, 49:734–739. This article describes a well-conducted series of lumbar shunting with visual outcome data.
Duthel R, Nuti C, Motuo-Fotso MJ, et al.: Complications of lumboperitoneal shunts: a retrospective study of a series of 195 patients (214 procedures). Neurochirurgie 1996, 42:83–89.
Corbett JJ, Nerad JA, Tse DT, et al.: Results of optic nerve sheath fenestration for pseudotumor cerebri: the lateral orbitotomy approach. Arch Ophthalmol 1988, 106:1391–1397.
Goh KY, Schatz NJ, Glaser JS: Optic nerve sheath fenestration for pseudotumor cerebri. J Neuroophthalmol 1997, 17:86–91.
Plotnik JL, Kosmorsky GS: Operative complications of optic nerve sheath decompression. Ophthalmology 1993, 100:683–690.
Panagoupoulos G, Angeliki G, Piaditis G, et al.: Treatment of benign intracranial hypertension with octreotide. Neurology 1998, 50:A5.
Luongo C, Mignini R, Vicario C, et al.: Hyperbaric oxygen therapy in the treatment of benign intracranial hypertension: follow-up of a preliminary study. Minerva Anestesiol 1992, 58(4 suppl 1):97–98.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Digre, K.B. Idiopathic intracranial hypertension. Curr Treat Options Neurol 1, 74–81 (1999). https://doi.org/10.1007/s11940-999-0035-3
Issue Date:
DOI: https://doi.org/10.1007/s11940-999-0035-3