Abstract
Purpose of Review
Right ventricular (RV) failure is increasingly recognized as a major cause of morbidity and mortality. When RV failure is refractory to medical therapy, escalation to right-sided mechanical circulatory support (MCS) should be considered. In this review, we begin by recapitulating the hemodynamics of RV failure, then we delve into current and future right-sided MCS devices and describe their hemodynamic profiles.
Recent Findings
The field of temporary right-sided MCS continues to expand, with evolving strategies and new devices actively under development. All right-sided MCS devices bypass the RV, with each bypass configuration conferring a unique hemodynamic profile. Devices that aspirate blood directly from the RV, as opposed to the RA or the IVC, have more favorable hemodynamics and more effective RV unloading. There has been a growing interest in single-access MCS devices which do not restrict patient mobility. Additionally, a first-of-its-kind percutaneous, pulsatile, right-sided MCS device (PERKAT RV) is currently undergoing investigation in humans.
Summary
Prompt recognition of refractory RV failure and deployment of right-sided MCS can improve outcomes. The field of right-sided MCS is rapidly evolving, with ongoing efforts dedicated towards developing novel temporary devices that are single access, allow for patient mobility, and directly unload the RV, as well as more durable devices.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Right ventricular (RV) failure is a major cause of morbidity and mortality. Once a marginalized chamber, there has been mounting evidence for the prognostic importance of RV failure in various disease states, including myocardial infarction (MI), cardiogenic shock, pulmonary embolism (PE), pulmonary hypertension (PH), chronic left-sided heart failure, valvular disease, congenital heart disease, after implantation of durable left-ventricular assist devices (LVAD), and in the acute respiratory distress syndrome [1,2,3,4,5,6,7,8,9,10,11].
RV failure can manifest acutely with profound hemodynamic compromise, but it can also present insidiously with progressive end-organ dysfunction – ultimately leading to increased mortality [12]. The first attempt at managing RV failure is often medical therapy, which centers around treating reversible causes, optimizing the failing RV’s loading conditions, and augmenting its contractility. Not infrequently, however, RV failure can be refractory to medical therapy alone. In these cases, mechanical circulatory support (MCS) should be considered to restore adequate systemic perfusion and promote decongestion. When promptly deployed, right-sided MCS has been shown to improve short-term survival [13,14,15,16].
Prior to delving into current right-sided MCS options and their hemodynamic impact, it is important to review normal RV mechanics, the different mechanisms of RV failure, and the associated hemodynamics. Some of these topics have been discussed in greater detail in other parts of this issue, but a brief overview within the framework of the RV pressure–volume domain will facilitate understanding of different right-sided MCS strategies in different clinical settings.
RV Failure – Mechanisms, Hemodynamics, and Diagnosis
Pathological changes of RV preload, afterload, or contractility can lead to RV failure, especially when they persist for prolonged periods of time. RV preload and afterload can be quantified via right heart catheterization (RHC), which provides direct measurements of RV, pulmonary artery (PA), and wedge pressures, as well as cardiac output, the latter of which is used to assess pulmonary vascular resistance [17]. While RHC-derived end-diastolic pressures can be an adequate estimation of preload, it is important to note that RHC-derived PA pressures offer one measure of RV afterload. Indexes such as resistance, compliance, and impedance allow for characterization of pulmonary vasculature properties independent of RV preload and contractility [18]. RV contractility is traditionally assessed via noninvasive imaging – commonly echocardiography and cardiac magnetic resonance imaging. However, measures of RV function derived from noninvasive imaging – including stroke volume (SV), ejection fraction (EF), fractional area change (FAC), tricuspid annular systolic velocity (S′), and tricuspid annular plane systolic excursion (TAPSE) – are all dependent on loading conditions and, thus, not reliable estimates of contractility [19]. Assessment of RV end-systolic elastance (Ees) via pressure–volume (PV) analysis, where a conductance catheter is placed within the RV, is considered the gold standard, load-independent index for quantifying RV contractility (Fig. 1A, B) [20]. PV analysis is also the most accurate means of assessing diastolic function as well as the efficiency of ventriculo-arterial interactions (i.e., RV-PA coupling) [21].
Basic elements of the right ventricular pressure–volume loop. Two fundamental relationships create boundaries for the pressure–volume (PV) loop: the end-systolic PV relationship (ESPVR), which describes ventricular contractile properties, and the end-diastolic PV relationship (EDPVR), which describes ventricular diastolic function (A). ESPVR connects the ESPV coordinate with the volume-axis intercept (V0), or the unstressed blood volume of the ventricle. Afterload can be characterized by the effective arterial elastance (Ea), which connects the end-systolic coordinates and the V0 at end-diastolic volume (Ved, 0). The slope of the ESPVR is also known as end-systolic elastance (Ees) and is a measure of right ventricular (RV) contractility. The ratio of Ees to Ea represents an index of RV-pulmonary arterial (PA) coupling, which reflects the efficiency of energy transfer from the RV to the PA (B). The PV loop also provides a basis for better understanding myocardial energetics. The space within the loop is stroke work (SW), and the potential space bound within the ESPVR and the EDPVR, but outside the loop, is the potential energy (PE). The sum of SW and PE is the PV area (PVA), which correlates with total mechanical energy generated by ventricular contraction and is linearly related to myocardial oxygen consumption (C)
Under normal physiologic conditions, the RV is coupled to a low-resistance and high-compliance pulmonary circulation. In contrast to normal left ventricular (LV) physiology, the isovolumetric contraction and relaxation phases can be very brief. In addition, blood continues to flow out of the RV after the point of peak elastance on the PV diagram, such that the end-ejection and end-systolic coordinates are considerably different. As such, pressure at end-ejection may decay to the point that it approaches the end-diastolic pressure, giving the normal RV PV loop its prototypical, trapezoidal shape [22] (Fig. 1A). Like the LV, when transitioning from rest to peak exercise, the normal RV has the ability to substantially augment contractility and lusitropy. In a study of 9 healthy individuals who underwent invasive PV loop assessment during cardiopulmonary exercise testing, RV dP/dtmax, the rate of change of systolic pressure (i.e., contractility), increased fourfold from rest to peak exercise, and dP/dtmin, the rate of change of diastolic pressure (i.e., lusitropy), increased threefold from rest to peak exercise [23].
While volume overload, pressure overload, and reduced contractility often co-occur in various forms of RV failure, for the purpose of simplicity, we will briefly review the hemodynamics of each state separately.
The Volume Overloaded RV
The normal RV is a thin-walled compliant chamber (low ΔP/ΔV ratio) able to accommodate large increases in preload without significant changes in pressure. In cases where volume overload is the primary pathology, such as in primary tricuspid regurgitation (TR), pulmonic insufficiency (PI), or atrial left-to-right shunting, the shape of the RV PV loop resembles that of the normal RV (Fig. 2A) [22, 24]. This is only the case, however, for fairly acute changes in volume. As volume overload becomes more severe and persists for longer, progressive RV dilation ensues. This results in increased pericardial restraint, increased RV wall tension, and increased RV stroke work (SW) which, altogether, ultimately leads to RV systolic dysfunction [25, 26]. Increased RV SW leads to an increase in pressure–volume area (PVA), which correlates with total mechanical energy generated by ventricular contraction and is linearly related to myocardial oxygen consumption (Fig. 1C) [27]. In addition, leftward shift of the interventricular septum can occur with severe RV volume overload, leading to LV diastolic dysfunction, underfilling, and progressive hemodynamic compromise [28].
Pressure volume loops reflecting various mechanisms of right ventricular failure. The pressure volume (PV) loop of the volume overloaded right ventricle (RV) resembles that of the normal RV, but is rightward shifted along the end-diastolic PV relationship (EDPVR), reflecting increased RV end-diastolic volume and pressure (A). The PV loop of the pressure overloaded RV more closely resembles that of the left ventricle, with a higher effective arterial elastance (Ea) slope, reflecting higher afterload (B). The hypocontractile RV has a lower end-systolic PV relationship (ESPVR) slope (known as end-systolic elastance or Ees), reflecting loss of contractility (C)
The Pressure Overloaded RV
Normally coupled to the low-resistance pulmonary circulation, the RV is poorly adaptable to changes in afterload. The PV loop of the pressure-overloaded RV more closely resembles that of the normal LV, with discernable periods of isovolumetric relaxation and contraction (Fig. 2B) [22]. An acute rise in afterload, such as in massive PE, can lead to rapid RV dilation and an abrupt reduction in RV stroke volume. In states of chronically elevated afterload, such as in pulmonary arterial hypertension, the RV has time to adapt via concentric hypertrophy and eccentric remodeling, both of which tend to reduce RV wall stress, per Laplace’s law, though this is almost always imperfect and wall stress remains elevated [29]. Additionally, as the pressure overload state persists, the RV loses its contractile reserve, undergoes further eccentric remodeling and dilation, and ultimately fails [30].
The Hypocontractile RV
Ischemia, whether acute or chronic, and various nonischemic cardiomyopathies can result in intrinsic compromise of RV contractility. The hypocontractile RV is particularly prone to ventriculo-arterial uncoupling in the setting of high afterload, whereby ventricular SW cannot be efficiently transferred to the PA, leading to LV underfilling and systemic hypotension. This is particularly true when the RV loses contractility abruptly, such as with acute RV MI. In extreme cases, the RV essentially functions as a passive conduit and becomes highly dependent on preload in order to maintain adequate LV filling (Fig. 2C).
Diagnosing RV Failure
Despite the wealth of information that can be obtained from invasive PV loop analysis, it remains a tool reserved for highly specialized research settings. The clinical diagnosis of RV failure continues to rely on a combination of findings from physical examination, laboratory studies, and noninvasive imaging, as well as RHC-derived hemodynamic data [31]. Several hemodynamic measures can be used to detect RV dysfunction. These include an elevated right atrial pressure (RAP) to pulmonary artery wedge pressure (PAWP) ratio, a low RV stroke work index (RVSWI), and a low pulmonary artery pulsatility index (PAPi), the latter of which has been shown to reflect RV contractile dysfunction at the sarcomeric level [32]. While various cutoffs have been found to be indicative of severe RV failure in different clinical scenarios, an RAP/PAWP ratio > 0.86 or PAPi < 1.5 should alert the clinician to the potential need for escalation to right-sided MCS [33, 34].
Right-Sided Mechanical Circulatory Support
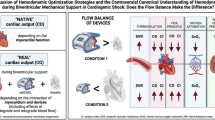
Mechanistically, all right-sided MCS devices support the circulation by bypassing the failing RV, either directly, by drawing blood from the RA or RV and transferring it to the PA, or indirectly by shifting blood from the right-sided circulation to the left-sided circulation (Table 1). By circumventing the failing RV, these devices are able to (1) increase LV preload with the goal of augmenting cardiac output (CO) and improving end-organ perfusion and (2) decongest the end-organs by unloading the right heart.
With few exceptions, right-sided MCS devices rely on a rotary pump to generate flow. As for all rotary-flow MCS devices, flow (Q) is related to the pump motor’s rotations per minute (RPM) and the pressure gradient between its inflow (preload) and outflow (afterload) [35]. This pressure gradient is referred to as the pressure head (H). As H rises, Q through the impeller drops. An understanding of this concept will be helpful in understanding device function in different settings.
The majority of right-sided MCS devices are only intended for temporary use, and patients receiving them must remain in the hospital, often in the intensive care unit setting. Several dedicated, surgically implantable, durable right-ventricular assist devices (RVADs) have been investigated but did not make it to market [36]. As an alternative, the commercially available durable LVADs have been used in the right-sided position to support long-term isolated RV or biventricular failure [37, 38].
Overview of Current Right-Sided MCS Devices, by Bypass Configuration
A) RA to PA
Impella RP
The Impella RP (right peripheral; Abiomed Inc., Danvers, MA) is a percutaneous, single-access, microaxial-flow catheter. It uses a 22F pump mounted on an 11F catheter, and it aspirates blood from the RA (inflow) and expels it into the PA (outflow), bypassing the RV. The device is inserted into a single venous access point (most commonly right femoral vein) via a 23F peel-away sheath. It is then advanced antegrade, under fluoroscopic guidance over a monorail wire, through the tricuspid and pulmonic valves and ultimately into the PA. At 33,000 RPM, the Impella RP can deliver up to 4 L/min of blood from the RA to the PA. It is not compatible with an oxygenator and thus cannot be used to support concomitant hypoxic respiratory failure.
The Impella RP was prospectively studied in 2015 in the RECOVER RIGHT trial in 30 patients with medically refractory RV failure. Impella RP support led to reduction in RAP (19.2 ± 0.7 to 12.6 ± 1 mmHg, P < 0.0001), improvement in cardiac index (1.82 ± 0.04 to 3.3 ± 0.23 L/min/m2, P < 0.001), and 73% of patients survived to 30 days or hospital discharge [39]. In 2018, Impella RP was prospectively studied in a larger cohort of 60 patients (including those from the RECOVER RIGHT trial) with redemonstration of the aforementioned results [13].
The hemodynamic effects of Impella RP are characterized by a reduction in RA pressure, an increase in PA pressures, and an increase in LV preload (Fig. 3A–C). Successful use of the Impella RP has been reported in RV failure due to acute MI, massive PE, post-cardiotomy syndrome, following LVAD implantation, and in primary graft dysfunction after orthotopic heart transplantation, among others [15, 40,41,42,43]. The most common adverse events are bleeding and hemolysis [13]. In the previously mentioned prospective analysis of 60 patients treated with Impella RP, major bleeding events occurred in 48% of patients and hemolysis occurred in 22% [13]. A notable limitation of Impella RP is the need for femoral access, which limits patient mobility. To allow for patient ambulation, a novel version of the Impella RP which can be inserted via right internal jugular approach is currently under development.
Pressure volume loops reflecting the hemodynamic impact of various forms of right-sided mechanical circulatory support. Right atrial (RA) to pulmonary artery (PA) bypass (e.g., Impella RP, Protek Duo) leads to reduction in right-ventricular end-diastolic pressure and volume (RVEDP and RVEDV), with concomitant increase in right ventricular (RV) afterload (A–C). RV to PA bypass (e.g., CentriMag, Spectrum Medical dual lumen cannula) leads to more effective RV unloading with further reduction in RV end-systolic volumes (D–F). RA to aorta (Ao) bypass (e.g., peripheral VA ECMO) leads to reduction in RVEDP without a concomitant increase in RV afterload, assuming normal left ventricular function (G–I). EDPVR, the end-diastolic PV relationship; ESPVR, the end-systolic PV relationship
TandemHeart-RV Assist Device and Protek Duo Cannula
The TandemHeart-RVAD is a dual-access, extracorporeal centrifugal-flow pump that can deliver up to 4 L/min of blood flow. It uses two 21F cannulae – the tip of one is placed in the RA (inflow), typically via left femoral vein approach, and the tip of the other is placed into the PA (outflow), typically via right femoral vein approach. When anatomic limitations preclude delivery of the outflow cannula via the femoral vein (e.g., patient height, presence of deep vein thrombosis or inferior vena cava filter), a right internal jugular approach can be used [44]. Use of the internal jugular vein ultimately led to the development of the Protek Duo cannula, which is a 29F or 31F dual lumen cannula inserted percutaneously via the right internal jugular vein and advanced into the PA [45]. The inflow lumen is positioned in the RA and the outflow lumen in the PA. These lumens are then attached to the TandemHeart pump which facilitates delivery of up to 4 L/min of blood from the RA to the PA. The major advantage of the Protek Duo cannula is the elimination of femoral access, thus allowing the patient to mobilize. Both TandemHeart-RVAD and Protek Duo-Tandem Heart can accommodate the introduction of an oxygenator into the circuit. Known as “oxy-RVAD,” this configuration can be used to support concomitant hypoxic respiratory failure [46]. The hemodynamic profile of TandemHeart-RVAD/Protek Duo is similar to that of Impella RP, with a reduction of RA pressures, an increase in PA pressures, and an increase in LV preload (Fig. 3A–C).
PERKAT RV
The PERKAT RV is the first percutaneous, pulsatile, right-sided MCS device. It is inserted into the femoral vein via an 18F catheter, and the outflow portion is advanced into the PA under fluoroscopic guidance, bypassing the RV. The PERKAT RV system relies on a standard intra-aortic balloon pump (IABP) connected to an external IABP console. The balloon is encased within a 2.2-m self-expanding nitinol stent cage, which itself is covered in one-way foil valves. The IABP balloon is electrocardiogram-gated, inflating during diastole and deflating during systole. When the balloon is deflated, blood flows from the IVC and distal veins, through the foil valves, into the stent cage. When the balloon is then inflated, the foil valves close and blood is displaced by the balloon into the PA. The PERKAT RV can generate nearly 4 L/min of flow [47, 48•]. Features of the PERKAT RV system include its smaller bore access compared to other percutaneous right-sided MCS devices, as well as its ability to provide pulsatile support to the failing RV while avoiding microvascular dysfunction that has been reported with continuous flow devices [49]. The PERKAT RV was evaluated in an animal model of right heart failure due to acute PE and was able to increase cardiac output by 60%, interestingly with no observed change in mean PA pressures [47]. This device is not yet approved for clinical use but is currently undergoing investigation in humans.
CentriMag-RVAD
The CentriMag is an extracorporeal centrifugal-flow pump that can generate up to 10 L/min of flow. The RA and PA are surgically cannulated via sternotomy or thoracotomy [50]. This proximal cannulation allows for the use of shorter and larger bore cannulae that facilitate the generation of much higher flows than percutaneously deployed devices, though this comes with the increased risks of bleeding and infection [51]. The clinical settings in which CentriMag-RVAD has most commonly been used are post-cardiotomy cardiogenic shock, primary graft dysfunction after orthotopic heart transplantation, and RV failure post-LVAD implantation [14].
Durable RVAD
Currently, there are no durable devices in clinical use that are specifically designed to support the right heart. In cases where long-term, durable, biventricular, or isolated right-sided support is needed, the current strategy is to utilize an LVAD in the right-sided position, with the inflow cannula in the RA or RV, and the outflow cannula in the PA [37]. Because the inflow cannula of the LVAD is designed to pass through a thicker and more muscular LV apex, its use on a much thinner RA or RV can result in protrusion into the inflow chamber with resultant frequent suction events. As such, the LVAD inflow cannula typically requires shortening prior to right-sided implantation, or is not fully inserted into the right-sided chamber as it would be into the LV [52]. Additionally, the high RA pressures and sub-systemic PA pressures commonly seen in severe RV failure result in low pressure head (H) and high flows (Q) which can further predispose to suction events and flow rates that can overwhelm the LV. For this reason, the LVAD outflow graft is often also restricted in order to increase resistance and reduce flow. There is ongoing debate as to whether the inflow cannula should be placed in the RV which, in principle, achieves more effective unloading, or in the RA which, in principle, potentially minimizes suction and pump thrombosis events [37, 53].
B) RV to PA
The hemodynamic profile of RV to PA bypass differs from that of RA to PA bypass in important ways. Direct unloading of the RV via an RV inflow leads to more effective chamber decompression and reduction in myocardial afterload to a greater extent than seen with an RA inflow (Fig. 3D–F). Additionally, the pressure–volume loops lose their isovolumetric phases, as volume decreases during both contraction and relaxation phases due to the continuous nature of the flow through the device; as such, the loops become more triangular.
Both CentriMag RVAD and durable RVAD – discussed above – can be configured such that the inflow cannula is in the RV rather than the RA.
Spectrum Medical Dual Lumen RV-PA Cannula
Spectrum Medical (Cheltenham, England) recently developed a novel dual lumen cannula that directly drains the RV. The cannula comes in 31F, 27F, or 24F sizes, which can provide approximately 5, 4, and 3 L/min of blood flow, respectively. This cannula can be connected to any extracorporeal circuit containing a rotary-flow pump and an oxygenator. The Spectrum cannula is inserted into the right internal jugular vein and advanced under fluoroscopy, with the inflow portion positioned in the RV and outflow in the PA. This dual lumen cannula provides the double advantage of direct RV decompression combined with internal jugular access which allows for patient mobilization.
C) RA to Aorta (Ao)
Peripheral VA-ECMO
Venoarterial extracorporeal membrane oxygenation (VA-ECMO) is commonly used for isolated LV failure or RV failure, biventricular failure, or other causes of cardiopulmonary collapse. Peripheral VA-ECMO systems typically employ a centrifugal pump which drains blood from the venous system, passes it through an oxygenator, and reinfuses it back into the arterial system to support both circulation and oxygenation. It consists of at least two cannulae – a drainage cannula (inflow) within the RA, typically inserted via a femoral vein approach, and a reinfusion cannula within the descending aorta, typically positioned in the iliac artery. Advanced ECMO strategies include a triple cannulation approach, such as veno-arterial-venous ECMO (VAV-ECMO) or veno-venous-arterial ECMO (VVA-ECMO). VAV-ECMO consists of venous drainage followed by reinfusion of oxygenated blood back into both the aorta and the RA, with the goal of better supporting oxygenation. VVA-ECMO consists of venous drainage from both the IVC and either the RA or PA, with reinfusion of blood into the aorta, with the goal of better unloading the right heart.
The hemodynamic impact of VA-ECMO on right-sided hemodynamics is a reduction in RAP with variable effect on PA pressures (Fig. 3G–I). On the one hand, VA-ECMO may lead to reduction in PA pressures via right-sided unloading and resultant reduction in RV SV. On the other hand, VA-ECMO increases LV afterload and, in cases of LV dysfunction, may lead to a significant rise in left atrial pressure (LAP) and secondary post-capillary pulmonary hypertension, if the LV is not adequately unloaded. As such, when LV dysfunction is present, VA-ECMO is often deployed concomitantly with another percutaneous device to decompress the LV, such as an IABP or left-sided Impella. Left atrial VA-ECMO (LAVA-ECMO) is a unique ECMO configuration which uses a venous cannula that is inserted from a femoral vein into the left atrium via single trans-septal puncture. The cannula has multiple fenestrations as it courses through the atria in order to unload both the right- and left-sided circulations. It has the major advantage of facilitating LV unloading without the need for a second device (i.e., IABP or Impella), which would require a second point of arterial access [54•, 55].
Special Considerations in Device Selection
Tricuspid Regurgitation
TR often complicates right heart failure. While primary TR leading to longstanding volume overload can be the cause of RV dysfunction, this accounts for only 8–10% of TR cases [56]. Much more commonly, TR is secondary to RV dysfunction causing progressive tricuspid annular dilatation and leaflet tethering. In patients with secondary TR, more severe RV dysfunction is associated with worse long-term survival [9]. When right-sided MCS devices that traverse the tricuspid valve are used, there is concern that existing TR may become worse or that new TR may be introduced [57]. However, this should not serve as a deterrent to using these devices, for several reasons. First, in the presence of an RV bypass device sourcing blood from the RA, TR serves to further unload the RV (Fig. 4). Second, by contributing to an ongoing state of right-sided preload excess, TR drops the pressure head across rotary-flow MCS devices that directly bypass the RV, which leads to stable, if not slightly increased, flows through these devices. Third, TR may improve with RV unloading resulting in reversal of tricuspid annular dilatation.
Pressure volume loops reflecting the impact of tricuspid regurgitation on the supported right heart. Tricuspid regurgitation (TR) in the presence of a right ventricular (RV) bypass device can serve to further unload the failing RV and decrease total RV afterload. RVF, right ventricular failure; RA, right atrium, PA, pulmonary artery, EDPVR, the end-diastolic PV relationship; ESPVR, the end-systolic PV relationship
Concomitant LV Dysfunction
The status of the LV is a major consideration when selecting a right-sided MCS device, each of which can influence left-sided hemodynamics. RA-PA and RV-PA bypass devices will increase LV preload which, in the presence of LV dysfunction, may lead to a significant rise in LAP, pulmonary edema, and post-capillary pulmonary hypertension. RA-Ao devices such as VA-ECMO can lead to significant increases in LV afterload pressure, which can result in LV distention and, similarly, elevated left-sided filling pressures and pulmonary edema. As such, when concomitant LV dysfunction is identified, biventricular support should be considered rather than isolated right-sided MCS. Many configurations for biventricular support have been employed, including bilateral TandemHeart devices, bilateral Impellas (BiPella), TandemHeart-RVAD plus left-sided Impella, or VA-ECMO plus LV vent (Impella or IABP), among others [58,59,60,61,62]. Although VA-ECMO with an LV vent is a commonly used strategy, advantages of the BiPella approach are the need for only one arterial access point and the ability to explant devices in a step-wise manner to monitor need for ongoing support.
Weaning Strategies
Prior to deployment of any MCS, the goal should be clearly defined – be that as bridge to recovery, more durable MCS, or transplantation. When the goal is recovery, frequent reassessment of the ongoing necessity of MCS is crucial, particularly given the complications associated with prolonged use of these devices. Unlike left-sided MCS for which an abundance of device-based weaning protocols have been proposed, there is a paucity of data with regards to weaning right-sided MCS. Although there will be variations by device type and indication for implant, the general principles for readiness-to-wean from right-sided MCS consist of an improvement in clinical status, hemodynamic parameters (RAP reduction, PAPi elevation), markers of end-organ perfusion (kidney and liver function), and ventricular function [63]. Weaning success and readiness-to-explant are assessed based on stability of the above parameters on minimal device flow [40]. Due to challenges with echocardiographic assessment of RV function – secondary to RV geometry, location behind the sternum, and load-dependent hemodynamics – many studies have not used clear cutoffs to define what constitutes a sufficient improvement in RV function. With that said, most echocardiographic predictors of successful right-sided MCS weaning come from studies on VA-ECMO, in which three-dimensional RV EF of > 24.6% or improvement in S′ > 10% from baseline have both been associated with higher weaning success [64, 65]. Overall, weaning protocols for right-sided MCS remains an ongoing area of investigation with need for device-based algorithms [66].
Conclusion
RV failure is a major cause of morbidity and mortality. Prompt recognition of refractory RV failure and deployment of right-sided MCS can improve outcomes. All right-sided MCS devices bypass the RV, with each bypass configuration conferring a unique hemodynamic profile. Devices that aspirate blood directly from the RV, as opposed to the RA or the IVC, have more favorable hemodynamics and more effective RV unloading. The field of right-sided MCS is rapidly evolving, with ongoing efforts dedicated towards developing novel devices that are single-access and allow for patient mobilization, as well as more durable right-sided support.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Reddy S, Bernstein D. Molecular mechanisms of right ventricular failure. Circulation. 2015;132(18):1734–42. https://doi.org/10.1161/CIRCULATIONAHA.114.012975.
Haddad F, Doyle R, Murphy DJ, Hunt SA. Right ventricular function in cardiovascular disease, part II: pathophysiology, clinical importance, and management of right ventricular failure. Circulation. 2008;117(13):1717–31. https://doi.org/10.1161/CIRCULATIONAHA.107.653584.
Mehta SR, Eikelboom JW, Natarajan MK, Diaz R, Yi C, Gibbons RJ, Yusuf S. Impact of right ventricular involvement on mortality and morbidity in patients with inferior myocardial infarction. J Am Coll Cardiol. 2001;37(1):37–43. https://doi.org/10.1016/s0735-1097(00)01089-5.
Zehender M, Kasper W, Kauder E, Schönthaler M, Geibel A, Olschewski M, Just H. Right ventricular infarction as an independent predictor of prognosis after acute inferior myocardial infarction. N Engl J Med. 1993;328(14):981–8. https://doi.org/10.1056/NEJM199304083281401.
Jacobs AK, Leopold JA, Bates E, Mendes LA, Sleeper LA, White H, Davidoff R, Boland J, Modur S, Forman R, Hochman JS. Cardiogenic shock caused by right ventricular infarction: a report from the SHOCK registry. J Am Coll Cardiol. 2003;41(8):1273–9. https://doi.org/10.1016/s0735-1097(03)00120-7.
Haddad F, Peterson T, Fuh E, Kudelko KT, de Jesus PV, Skhiri M, Vagelos R, Schnittger I, Denault AY, Rosenthal DN, Doyle RL, Zamanian RT. Characteristics and outcome after hospitalization for acute right heart failure in patients with pulmonary arterial hypertension. Circ Heart Fail. 2011;4(6):692–9. https://doi.org/10.1161/CIRCHEARTFAILURE.110.949933.
Ghio S, Gavazzi A, Campana C, Inserra C, Klersy C, Sebastiani R, Arbustini E, Recusani F, Tavazzi L. Independent and additive prognostic value of right ventricular systolic function and pulmonary artery pressure in patients with chronic heart failure. J Am Coll Cardiol. 2001;37(1):183–8. https://doi.org/10.1016/s0735-1097(00)01102-5.
Yeh DD, Schmidt ACS, Eisman AS, Serfas JD, Naqvi M, Youniss MA, Ryfa AD, Khan AA, Safi L, Tabtabai SR, Bhatt AB, Lewis GD. Impaired right ventricular reserve predicts adverse cardiac outcomes in adults with congenital right heart disease. Heart. 2018;104(24):2044–50. https://doi.org/10.1136/HEARTJNL-2017-312572.
Dietz MF, Prihadi EA, van der Bijl P, Ajmone Marsan N, Delgado V, Bax JJ. Prognostic implications of staging right heart failure in patients with significant secondary tricuspid regurgitation. JACC Heart Fail. 2020;8(8):627–36. https://doi.org/10.1016/j.jchf.2020.02.008.
Kormos RL, Teuteberg JJ, Pagani FD, Russell SD, John R, Miller LW, Massey T, Milano CA, Moazami N, Sundareswaran KS, Farrar DJ. Right ventricular failure in patients with the HeartMate II continuous-flow left ventricular assist device: incidence, risk factors, and effect on outcomes. J Thorac Cardiovasc Surg. 2010;139(5):1316–24. https://doi.org/10.1016/j.jtcvs.2009.11.020.
Sato R, Dugar S, Cheungpasitporn W, Schleicher M, Collier P, Vallabhajosyula S, Duggal A. The impact of right ventricular injury on the mortality in patients with acute respiratory distress syndrome: a systematic review and meta-analysis. Crit Care. 2021;25(1):172. https://doi.org/10.1186/s13054-021-03591-9.
Konstam MA, Kiernan MS, Bernstein D, Bozkurt B, Jacob M, Kapur NK, Kociol RD, Lewis EF, Mehra MR, Pagani FD, Raval AN, Ward C. Evaluation and management of right-sided heart failure: a Scientific Statement From the American Heart Association. Circulation. 2018;137(20):e578–622. https://doi.org/10.1161/CIR.0000000000000560.
Anderson M, Morris DL, Tang D, Batsides G, Kirtane A, Hanson I, Meraj P, Kapur NK, O’Neill W. Outcomes of patients with right ventricular failure requiring short-term hemodynamic support with the Impella RP device. J Hear lung Transplant Off Publ Int Soc Hear Transplant. 2018;37(12):1448–58. https://doi.org/10.1016/j.healun.2018.08.001.
Bhama JK, Bansal U, Winger DG, Teuteberg JJ, Bermudez C, Kormos RL, Bansal A. Clinical experience with temporary right ventricular mechanical circulatory support. J Thorac Cardiovasc Surg. 2018;156(5):1885–91. https://doi.org/10.1016/j.jtcvs.2018.04.094.
Elder M, Blank N, Kaki A, Alraies MC, Grines CL, Kajy M, Hasan R, Mohamad T, Schreiber T. Mechanical circulatory support for acute right ventricular failure in the setting of pulmonary embolism. J Interv Cardiol. 2018;31(4):518–24. https://doi.org/10.1111/joic.12503.
Machuca TN, de Perrot M. Mechanical support for the failing right ventricle in patients with precapillary pulmonary hypertension. Circulation. 2015;132(6):526–36. https://doi.org/10.1161/CIRCULATIONAHA.114.012593.
Sayer GT, Semigran MJ. Right ventricular performance in chronic congestive heart failure. Cardiol Clin. 2012;30(2):271–82. https://doi.org/10.1016/j.ccl.2012.03.011.
Tedford RJ. Determinants of right ventricular afterload (2013 Grover Conference series). Pulm Circ. 2014;4(2):211–9. https://doi.org/10.1086/676020.
Newman JH, Brittain EL, Robbins IM, Hemnes AR. Effect of acute arteriolar vasodilation on capacitance and resistance in pulmonary arterial hypertension. Chest. 2015;147(4):1080–5. https://doi.org/10.1378/chest.14-1461.
Brimioulle S, Wauthy P, Ewalenko P, Rondelet B, Vermeulen F, Kerbaul F, Naeije R. Single-beat estimation of right ventricular end-systolic pressure-volume relationship. Am J Physiol Circ Physiol. 2003;284(5):H1625–30. https://doi.org/10.1152/ajpheart.01023.2002.
Brener MI, Masoumi A, Ng VG, Tello K, Bastos MB, Cornwell WK 3rd, Hsu S, Tedford RJ, Lurz P, Rommel K-P, Kresoja K-P, Nagueh SF, Kanwar MK, Kapur NK, Hiremath G, Sarraf M, Van Den Enden AJM, Van Mieghem NM, Heerdt PM, Hahn RT, Kodali SK, Sayer GT, Uriel N, Burkhoff D. Invasive right ventricular pressure-volume analysis: basic principles, clinical applications, and practical recommendations. Circ Heart Fail. 2022;15(1):e009101. https://doi.org/10.1161/CIRCHEARTFAILURE.121.009101.
Redington AN, Gray HH, Hodson ME, Rigby ML, Oldershaw PJ. Characterisation of the normal right ventricular pressure-volume relation by biplane angiography and simultaneous micromanometer pressure measurements. Br Heart J. 1988;59(1):23–30. https://doi.org/10.1136/hrt.59.1.23.
Cornwell WK, Tran T, Cerbin L, Coe G, Muralidhar A, Hunter K, Altman N, Ambardekar AV, Tompkins C, Zipse M, Schulte M, O’Gean K, Ostertag M, Hoffman J, Pal JD, Lawley JS, Levine BD, Wolfel E, Kohrt WM, Buttrick P. New insights into resting and exertional right ventricular performance in the healthy heart through real-time pressure-volume analysis. J Physiol. 2020;598(13):2575–87. https://doi.org/10.1113/JP279759.
Sanz J, Sánchez-Quintana D, Bossone E, Bogaard HJ, Naeije R. Anatomy, function, and dysfunction of the right ventricle: JACC state-of-the-art review. J Am Coll Cardiol. 2019;73(12):1463–82. https://doi.org/10.1016/j.jacc.2018.12.076.
Borlaug BA, Reddy YNV. The role of the pericardium in heart failure: implications for pathophysiology and treatment. JACC Hear Fail. 2019;7(7):574–85. https://doi.org/10.1016/j.jchf.2019.03.021.
Havlenova T, Skaroupkova P, Miklovic M, Behounek M, Chmel M, Jarkovska D, Sviglerova J, Stengl M, Kolar M, Novotny J, Benes J, Cervenka L, Petrak J, Melenovsky V. Right versus left ventricular remodeling in heart failure due to chronic volume overload. Sci Rep. 2021;11(1):17136. https://doi.org/10.1038/s41598-021-96618-8.
Takaoka H, Takeuchi M, Odake M, Yokoyama M. Assessment of myocardial oxygen consumption (Vo2) and systolic pressure-volume area (PVA) in human hearts. Eur Heart J. 1992;13(Suppl E):85–90. https://doi.org/10.1093/eurheartj/13.suppl_e.85.
Naeije R, Badagliacca R. The overloaded right heart and ventricular interdependence. Cardiovasc Res. 2017;113(12):1474–85. https://doi.org/10.1093/cvr/cvx160.
Bogaard HJ, Abe K, Vonk Noordegraaf A, Voelkel NF. The right ventricle under pressure: cellular and molecular mechanisms of right-heart failure in pulmonary hypertension. Chest. 2009;135(3):794–804. https://doi.org/10.1378/chest.08-0492.
Vonk-Noordegraaf A, Haddad F, Chin KM, Forfia PR, Kawut SM, Lumens J, Naeije R, Newman J, Oudiz RJ, Provencher S, Torbicki A, Voelkel NF, Hassoun PM. Right heart adaptation to pulmonary arterial hypertension: physiology and pathobiology. J Am Coll Cardiol. 2013;62(25, Supplement):D22–33. https://doi.org/10.1016/j.jacc.2013.10.027.
Ryan JJ, Tedford RJ. Diagnosing and treating the failing right heart. Curr Opin Cardiol. 2015;30(3):292–300. https://doi.org/10.1097/HCO.0000000000000164.
Aslam MI, Jani V, Lin BL, Dunkerly-Eyring B, Livingston CE, Ramachandran A, Ranek MJ, Bedi KC, Margulies KB, Kass DA, Hsu S. Pulmonary artery pulsatility index predicts right ventricular myofilament dysfunction in advanced human heart failure. Eur J Heart Fail. 2021;23(2):339–41. https://doi.org/10.1002/ejhf.2084.
Saxena A, Garan AR, Kapur NK, O’Neill WW, Lindenfeld J, Pinney SP, Uriel N, Burkhoff D, Kern M. Value of hemodynamic monitoring in patients with cardiogenic shock undergoing mechanical circulatory support. Circulation. 2020;141(14):1184–97. https://doi.org/10.1161/CIRCULATIONAHA.119.043080.
Lala A, Guo Y, Xu J, Esposito M, Morine K, Karas R, Katz SD, Hochman JS, Burkhoff D, Kapur NK. Right ventricular dysfunction in acute myocardial infarction complicated by cardiogenic shock: a hemodynamic analysis of the Should We Emergently Revascularize Occluded Coronaries for Cardiogenic Shock (SHOCK) Trial and Registry. J Card Fail. 2018;24(3):148–56. https://doi.org/10.1016/j.cardfail.2017.10.009.
Moazami N, Fukamachi K, Kobayashi M, Smedira NG, Hoercher KJ, Massiello A, Lee S, Horvath DJ, Starling RC. Axial and centrifugal continuous-flow rotary pumps: a translation from pump mechanics to clinical practice. J Hear lung Transplant Off Publ Int Soc Hear Transplant. 2013;32(1):1–11. https://doi.org/10.1016/j.healun.2012.10.001.
Meyns B, Ector J, Rega F, Droogne W, Vanhaecke J, Vanhemelrijck J, Griffith B, Dowling R, Zucker M, Burkhoff D. First human use of partial left ventricular heart support with the Circulite synergy micro-pump as a bridge to cardiac transplantation. Eur Heart J. 2008;29(20):2582. https://doi.org/10.1093/eurheartj/ehn202.
Shehab S, Macdonald PS, Keogh AM, Kotlyar E, Jabbour A, Robson D, Newton PJ, Rao S, Wang L, Allida S, Connellan M, Granger E, Dhital K, Spratt P, Jansz PC, Hayward CS. Long-term biventricular HeartWare ventricular assist device support—case series of right atrial and right ventricular implantation outcomes. J Hear lung Transplant Off Publ Int Soc Hear Transplant. 2016;35(4):466–73. https://doi.org/10.1016/j.healun.2015.12.001.
Bernhardt AM, De By TMMH, Reichenspurner H, Deuse T. Isolated permanent right ventricular assist device implantation with the HeartWare continuous-flow ventricular assist device: first results from the European Registry for Patients with Mechanical Circulatory Support. Eur J cardio-thoracic Surg Off J Eur Assoc Cardio-thoracic Surg. 2015;48(1):158–62. https://doi.org/10.1093/ejcts/ezu406.
Anderson MB, Goldstein J, Milano C, Morris LD, Kormos RL, Bhama J, Kapur NK, Bansal A, Garcia J, Baker JN, Silvestry S, Holman WL, Douglas PS, O’Neill W. Benefits of a novel percutaneous ventricular assist device for right heart failure: the prospective RECOVER RIGHT study of the Impella RP device. J Hear lung Transplant Off Publ Int Soc Hear Transplant. 2015;34(12):1549–60. https://doi.org/10.1016/j.healun.2015.08.018.
Cheung AW, White CW, Davis MK, Freed DH. Short-term mechanical circulatory support for recovery from acute right ventricular failure: clinical outcomes. J Hear Lung Transplant. 2014;33(8):794–9. https://doi.org/10.1016/j.healun.2014.02.028.
Randhawa VK, Hoffman K, Bock A, Bhat P, Young L, Rossi J, Campbell J, Bott-Silverman C, Soltesz EG, Tong MZY, Unai S, Nair R, Estep JD, Perez AL. Impella RP as a bridge to cardiac transplant for refractory late right ventricular failure in setting of left ventricular assist device. ESC Hear Fail. 2020;7(4):1972–5. https://doi.org/10.1002/ehf2.12685.
Taha A, Mohammedzein A, Kimbugwe J, Carthel K, Brabham D. Impella RP: a promising intervention in acute right ventricular failure caused by massive pulmonary embolism. JACC Case reports. 2019;1(4):622–5. https://doi.org/10.1016/j.jaccas.2019.09.009.
Jagadeesan VS, Davidson LJ, Churyla A, Benzuly KH. Catheter-based embolectomy prior to right ventricular mechanical circulatory support placement after heart transplantation. ESC Hear Fail. 2020;7(5):3215–8. https://doi.org/10.1002/ehf2.12948.
Kiernan MS, Krishnamurthy B, Kapur NK. Percutaneous right ventricular assist via the internal jugular vein in cardiogenic shock complicating an acute inferior myocardial infarction. J Invasive Cardiol. 2010;22(2):E23–6.
Aggarwal V, Einhorn BN, Cohen HA. Current status of percutaneous right ventricular assist devices: first-in-man use of a novel dual lumen cannula. Catheter Cardiovasc Interv Off J Soc Card Angiogr Interv. 2016;88(3):390–6. https://doi.org/10.1002/ccd.26348.
Bermudez CA, Lagazzi L, Crespo MM. Prolonged support using a percutaneous OxyRVAD in a patient with end-stage lung disease, pulmonary hypertension, and right cardiac failure. ASAIO J. 2016;62(4):e37-40. https://doi.org/10.1097/MAT.0000000000000343.
Kretzschmar D, Schulze PC, Ferrari MW. Concept, evaluation, and future perspectives of PERKAT® RV—a novel right ventricular assist device. J Cardiovasc Transl Res. 2019;12(2):150–4. https://doi.org/10.1007/s12265-018-9834-9.
• Ferrari MW, Schulze PC, Kretzschmar D. Acute right heart failure: future perspective with the PERKAT RV pulsatile right ventricular support device. Ther Adv Cardiovasc Dis. 2020;14:1753944719895902. https://doi.org/10.1177/1753944719895902. (This work highlights a first-of-its-kind percutaneous, pulsatile, right-sided MCS device.)
Saito T, Miyagawa S, Toda K, Yoshikawa Y, Fukushima S, Saito S, Yoshioka D, Sakata Y, Daimon T, Sawa Y. Effect of continuous-flow mechanical circulatory support on microvasculature—remodeling in the failing heart. Artif Organs. 2019;43(4):350–62. https://doi.org/10.1111/aor.13348.
John R, Long JW, Massey HT, Griffith BP, Sun BC, Tector AJ, Frazier OH, Joyce LD. Outcomes of a multicenter trial of the Levitronix CentriMag ventricular assist system for short-term circulatory support. J Thorac Cardiovasc Surg. 2011;141(4):932–9. https://doi.org/10.1016/j.jtcvs.2010.03.046.
Bhama JK, Kormos RL, Toyoda Y, Teuteberg JJ, McCurry KR, Siegenthaler MP. Clinical experience using the Levitronix CentriMag system for temporary right ventricular mechanical circulatory support. J Hear lung Transplant Off Publ Int Soc Hear Transplant. 2009;28(9):971–6. https://doi.org/10.1016/j.healun.2009.04.015.
Karimov JH, Sunagawa G, Horvath D, Fukamachi K, Starling RC, Moazami N. Limitations to chronic right ventricular assist device support. Ann Thorac Surg. 2016;102(2):651–8. https://doi.org/10.1016/j.athoracsur.2016.02.006.
Marasco SF, Stornebrink RK, Murphy DA, Bergin PJ, Lo C, McGiffin DC. Long-term right ventricular support with a centrifugal ventricular assist device placed in the right atrium. J Card Surg. 2014;29(6):839–42. https://doi.org/10.1111/jocs.12440.
• Singh-Kucukarslan G, Raad M, Al-Darzi W, Cowger J, Brice L, Basir MB, O’Neill WW, Alaswaad K, Eng MH. Hemodynamic effects of left-atrial venous arterial extra-corporeal membrane oxygenation (LAVA-ECMO). ASAIO J. Published online December 2021. https://doi.org/10.1097/MAT.0000000000001628. (This work highlights left atrial VA-ECMO (LAVA-ECMO), a unique ECMO configuration which can unload both the right and left heart without need for a second point of arterial access.)
Kotani Y, Chetan D, Rodrigues W, Sivarajan VB, Gruenwald C, Guerguerian A-M, Van Arsdell GS, Honjo O. Left atrial decompression during venoarterial extracorporeal membrane oxygenation for left ventricular failure in children: current strategy and clinical outcomes. Artif Organs. 2013;37(1):29–36. https://doi.org/10.1111/j.1525-1594.2012.01534.x.
Prihadi EA, Delgado V, Leon MB, Enriquez-Sarano M, Topilsky Y, Bax JJ. Morphologic types of tricuspid regurgitation: characteristics and prognostic implications. JACC Cardiovasc Imaging. 2019;12(3):491–9. https://doi.org/10.1016/j.jcmg.2018.09.027.
Salna M, Garan AR, Kirtane AJ, Karmpaliotis D, Green P, Takayama H, Sanchez J, Kurlansky P, Yuzefpolskaya M, Colombo PC, Naka Y, Takeda K. Novel percutaneous dual-lumen cannula-based right ventricular assist device provides effective support for refractory right ventricular failure after left ventricular assist device implantation. Interact Cardiovasc Thorac Surg. 2020;30(4):499–506. https://doi.org/10.1093/icvts/ivz322.
Nagy CD, Jumean MF, Pham DT, Kiernan MS, Denofrio D, Kapur NK. Percutaneous circulatory support for biventricular failure. Circ Cardiovasc Interv. 2013;6(2):e12–4. https://doi.org/10.1161/CIRCINTERVENTIONS.112.000018.
Aghili N, Bader Y, Vest AR, Kiernan MS, Kimmelstiel C, DeNofrio D, Kapur NK. Biventricular circulatory support using 2 axial flow catheters for cardiogenic shock without the need for surgical vascular access. Circ Cardiovasc Interv. 2016;9(6).https://doi.org/10.1161/CIRCINTERVENTIONS.116.003636.
Kapur NK, Jumean M, Ghuloom A, Aghili N, Vassallo C, Kiernan MS, DeNofrio D, Pham DT. First successful use of 2 axial flow catheters for percutaneous biventricular circulatory support as a bridge to a durable left ventricular assist device. Circ Heart Fail. 2015;8(5):1006–8. https://doi.org/10.1161/CIRCHEARTFAILURE.115.002374.
Rajagopal V, Steahr G, Wilmer CI, Raval NY. A novel percutaneous mechanical biventricular bridge to recovery in severe cardiac allograft rejection. J Hear lung Transplant Off Publ Int Soc Hear Transplant. 2010;29(1):93–5. https://doi.org/10.1016/j.healun.2009.09.015.
Atwater BD, Nee LM, Gimelli G. Long-term survival using intra-aortic balloon pump and percutaneous right ventricular assist device for biventricular mechanical support of cardiogenic shock. J Invasive Cardiol. 2008;20(7):E205–7.
Randhawa VK, Al-Fares A, Tong MZY, Soltesz EG, Hernandez-Montfort J, Taimeh Z, Weiss AJ, Menon V, Campbell J, Cremer P, Estep JD. A pragmatic approach to weaning temporary mechanical circulatory support: a state-of-the-art review. JACC Hear Fail. 2021;9(9):664–73. https://doi.org/10.1016/j.jchf.2021.05.011.
Huang K-C, Lin L-Y, Chen Y-S, Lai C-H, Hwang J-J, Lin L-C. Three-dimensional echocardiography–derived right ventricular ejection fraction correlates with success of decannulation and prognosis in patients stabilized by venoarterial extracorporeal life support. J Am Soc Echocardiogr. 2018;31(2):169–79. https://doi.org/10.1016/j.echo.2017.09.004.
Kim D, Jang WJ, Park TK, Cho YH, Choi J-O, Jeon E-S, Yang JH. Echocardiographic predictors of successful extracorporeal membrane oxygenation weaning after refractory cardiogenic shock. J Am Soc Echocardiogr Off Publ Am Soc Echocardiogr. 2021;34(4):414-422.e4. https://doi.org/10.1016/j.echo.2020.12.002.
Roscoe A, Zochios V. Echocardiography in Weaning Right Ventricular Mechanical Circulatory Support: Are We Measuring The Right Stuff? J Cardiothorac Vasc Anesth. 2022;36(2):362–6. https://doi.org/10.1053/j.jvca.2021.09.045.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Human and Animal Rights and Informed Consent.
This article does not contain any studies with human or animal subjects performed by any of the authors.
Conflict of Interest
Dr. Alkhunaizi declares no conflicts of interest. Dr. Burkhoff has received institutional educational grant support from Abiomed as well as consulting fees from CardioDyme Inc and from Abbott Laboratories. Dr. Brener is supported by an ACC/Merck Research Fellowship and has received consulting fees from Artract Medical and Osprey Medical.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Focus on the Right Heart.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Alkhunaizi, F.A., Burkhoff, D. & Brener, M.I. Right-Sided Mechanical Circulatory Support – A Hemodynamic Perspective. Curr Heart Fail Rep 19, 334–345 (2022). https://doi.org/10.1007/s11897-022-00562-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11897-022-00562-1