Summary
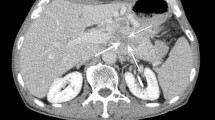
This study investigated the accuracy of MRI features in differentiating the pathological grades of pancreatic neuroendocrine neoplasms (PNENs). A total of 31 PNENs patients were retrospectively evaluated, including 19 cases in grade 1, 5 in grade 2, and 7 in grade 3. Plain and contrastenhanced MRI was performed on all patients. MRI features including tumor size, margin, signal intensity, enhancement patterns, degenerative changes, duct dilatation and metastasis were analyzed. Chi square tests, Fisher’s exact tests, one-way ANOVA and ROC analysis were conducted to assess the associations between MRI features and different tumor grades. It was found that patients with older age, tumors with higher TNM stage and without hormonal syndrome had higher grade of PNETs (all P<0.05). Tumor size, shape, margin and growth pattern, tumor pattern, pancreatic and bile duct dilatation and presence of lymphatic and distant metastasis as well as MR enhancement pattern and tumor-topancreas contrast during arterial phase were the key features differentiating tumors of all grades (all P<0.05). ROC analysis revealed that the tumor size with threshold of 2.8 cm, irregular shape, pancreatic duct dilatation and lymphadenopathy showed satisfactory sensitivity and specificity in distinguishing grade 3 from grade 1 and grade 2 tumors. Features of peripancreatic tissue or vascular invasion, and distant metastasis showed high specificity but relatively low sensitivity. In conclusion, larger size, poorlydefined margin, heterogeneous enhanced pattern during arterial phase, duct dilatation and the presence of metastases are common features of higher grade PNENs. Plain and contrast-enhanced MRI provides the ability to differentiate tumors with different pathological grades.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Halfdanarson TR, Rabe KG, Rubin J, et al. Pancreatic neuroendocrine tumors (PNETs): incidence, prognosis and recent trend toward improved survival. Ann Oncol, 2008,19(10):1727–1733
Zhou C, Zhang J, Zheng Y, et al. Pancreatic neuroendocrine tumors: a comprehensive review. Int J Cancer, 2012,131(5):1013–1022
Milan SA, Yeo CJ. Neuroendocrine tumors of the pancreas. Curr Opin Oncol, 2012,24(1):46–55
Bosman FT, Carneiro F, Hruban RH, et al. WHO classification of tumours of the digestive system. Lyon: IARC Press,2010,322–326
Rindi G, Kloppel G, Alhman H, et al. TNM staging of foregut (neuro) endocrine tumors: a consensus proposal including a grading system. Virchows Arch, 2006,449(4):395–401
Gunther RW, Klose KJ, Ruckert K, et al. Islet-cell tumors: detection of small lesions with computed tomography and ultrasound. Radiology, 1983,148(2):485–488
Ichikawa T, Peterson MS, Federle MP, et al. Islet cell tumor of the pancreas: biphasic CT versus MR imaging in tumor detection. Radiology, 2000,216(1):163–171
Semelka RC, Custodio CM, Cem Balci N, et al. Neuroendocrine tumors of the pancreas: spectrum of appearances on MRI. JMRI, 2000,11(2):141–148
de Herder WW, Kwekkeboom DJ, Valkema R, et al. Neuroendocrine tumors and somatostatin: imaging techniques. J EndocrinolI nvest, 2005,28(11 Suppl):132–136
Manfredi R, Bonatti M, Mantovani W, et al. Nonhyperfunctioning neuroendocrine tumours of the pancreas: MR imaging appearance and correlation with their biological behaviour. Eur Radiol, 2013,23(11):3029–3039
Kim DW, Kim HJ, Kim KW, et al. Neuroendocrine neoplasms of the pancreas at dynamic enhanced CT: comparison between grade 3 neuroendocrine carcinoma and grade 1/2 neuroendocrine tumour. Eur Radiol, 2015,25(5):1375–1383
Takumi K, Fukukura Y, Higashi M, et al. Pancreatic neuroendocrine tumors: Correlation between the contrastenhanced computed tomography features and the pathological tumor grade. Eur J Radiol, 2015,84(8):1436–1443
Bushnell DL, Baum RP. Standard imaging techniques for neuroendocrine tumors. Endocrinol Metab Clin North Am, 2011,40(1):153–162
Caramella C, Dromain C, de Baere T, et al. Endocrine pancreatic tumours: which are the most useful MRI sequences? Euro Radiol, 2010,20(11):2618–2627
Herwick S, Miller FH, Keppke AL. MRI of islet cell tumors of the pancreas. AJR Am J Roentgenol, 2006, 187(5):W472–W480
Panzuto F, Falconi M, Nasoni S, et al. Staging of digestive endocrine tumours using helical computed tomography and somatostatin receptor scintigraphy. Ann Oncol, 2003,14(4):586–591
Dromain C, Deandreis D, Scoazec JY, et al. Imaging of neuroendocrine tumors of the pancreas. Diagn Interv Imaging, 2016,97(12):1241–1257
Gallotti A, Johnston RP, Bonaffini PA, et al. Incidental neuroendocrine tumors of the pancreas: MDCT findings and features of malignancy. AJR, 2013,200(2):355–362
Marion-Audibert AM, Barel C, Gouysse G, et al. Low microvessel density is an unfavorable histoprognostic factor in pancreatic endocrine tumors. Gastroenterology, 2003,125(4):1094–1104
Zhang J, Jia Z, Li Q, et al. Elevated expression of vascular endothelial growth factor correlates with increased angiogenesis and decreased progression-free survival among patients with low-grade neuroendocrine tumors. Cancer, 2007,109(8):1478–1486
Kim JH, Eun HW, Kim YJ, et al. Staging accuracy of MR for pancreatic neuroendocrine tumor and imaging findings according to the tumor grade. Abdom Imaging, 2013,38(5):1106–1114
Rodallec M, Vilgrain V, Couvelard A, et al. Endocrine pancreatic tumours and helical CT: contrast enhancement is correlated with microvascular density, histoprognostic factors and survival. Pancreatology, 2006,6(1-2): 77–85
Xu LN, Xu YY, Gao DW. Impact of operative and perioperative factors on the long-term prognosis of primary liver cancer patients undergoing epatectomy. J Huazhong Univ Sci Technol Med Sci, 2016,36(4):523–528
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jin, F., Wang, K., Qin, Tt. et al. Pancreatic neuroendocrine neoplasms: Correlation between MR features and pathological tumor grades. J. Huazhong Univ. Sci. Technol. [Med. Sci.] 37, 587–595 (2017). https://doi.org/10.1007/s11596-017-1777-x
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-017-1777-x