Abstract
Purpose
The objective of this study was to determine the clinical value and accuracy of magnetic resonance (MR)-guided vacuum-assisted breast biopsy (VAB).
Materials and methods
We retrospectively analysed 106 incidental breast lesions detected on MR imaging in 98 patients. Patients with nonpalpable suspicious lesions that were only MR visible were referred for MR-VAB performed with a 10-gauge needle. All patients with a VAB diagnosis of infiltrating carcinoma, carcinoma in situ or atypical epithelial hyperplasia were referred for surgery. Histopathology of the surgical specimen was considered the reference standard.
Results
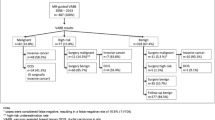
MR-guided VAB was attempted in 29/106 lesions (27%); in 2/29 patients, the procedure could not be performed owing to failure to visualise the lesion. Lesions with clearly malignant features and borderline lesions (atypical ductal hyperplasias) were identified in 12 cases (44%) and benign entities in 15 (56%). Seven of 12 (58%) malignant lesions were <10 mm. Among the 27 successful MR-VAB procedures, VAB yielded one false-negative diagnosis (4%) and underestimation (4%). MR-guided VAB sensitivity and specificity were 92% and 100%, respectively, with a positive predictive value of 100% and a negative predictive value of 93%.
Conclusions
The results of this study indicate that MR-guided VAB offers good accuracy in characterising nonpalpable breast lesions visible on MR imaging alone. Small lesion size (<1 cm) did not prove to be a limitation for the success of the procedure.
Riassunto
Obiettivo
Scopo del nostro lavoro è stato valutare l’incidenza e l’accuratezza del sistema di ago-biopsia mammaria sotto guida di risonanza magnetica (RM) con dispositivo aspirante sotto vuoto (VAB).
Materiali e metodi
Sono stati analizzati retrospettivamente 98 pazienti portatori di 106 lesioni identificate incidentalmente all’esame RM. Sono state avviate al VAB, con l’utilizzo di un ago da 10 gauge, le pazienti con alterazioni sospette alla RM, non riconoscibili con ecografia né mammografia, non palpabili, in cui la tipizzazione non poteva essere ottenuta con metodiche alternative. Tutte le pazienti con diagnosi VAB di carcinoma infiltrante, di carcinoma in situ e di iperplasia epiteliale con atipie cellulari sono state indirizzate all’intervento. Il gold standard è stato l’esame istopatologico proveniente dall’escissione chirurgica.
Risultati
Le lesioni avviate a prelievo microistologico sotto-guida RM sono state 29/106 (27%). In 2/29 casi non è stato possibile procedere al prelievo per la mancata visualizzazione della lesione. Il riscontro di patologia francamente maligna o di lesioni border-line si è verificato in 12 casi (44%), nei restanti 15 casi (56%) si è rilevata patologia benigna. Sette/12 (58%) lesioni maligne avevano diametro inferiore o uguale a 10 mm. Uno/27 casi (4%) è risultato falso negativo al VAB; 1/27 casi (4%) è stato sottostimato dal VAB. Complessivamente, il prelievo VAB sotto guida RM ha mostrato valori di sensibilità e specificità rispettivamente del 92% e 100% con valore predittivo positivo del 100% e valore predittivo negativo del 93%.
Conclusioni
Il prelievo con VAB è metodica affidabile nella tipizzazione di lesioni mammarie non palpabili, solo RM visibili. Le dimensioni della lesione inferiori a 1 cm non sono un limite per la metodica.
Article PDF
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
References/Bibliografia
Kuhl CK (2007) Current status of breast imaging. Part 1. Choice of technique, image interpretation, diagnostic accuracy, and transfer to clinical practice. Radiology 244:356–378
Morrow M (2008) Magnetic resonance imaging in the breast cancer patient: curb your enthusiasm. J Clin Oncol 26:352–353
Morrow M (2004) Magnetic resonance imaging in the preoperative evaluation of breast cancer: primum non nocere. J Am Coll Surg 198:240–241
Houssami N, Ciatto S, Macaskill P et al (2008) Accuracy and surgical impact of magnetic resonance imaging in breast cancer staging: systematic review and meta-analysis in detection of multifocal and multicentric cancer. J Clin Oncol 26:3248–3258
Solin LJ, Orel SG, Hwang WT et al (2008) Relationship of breast magnetic resonance imaging to outcome after breast-conservation treatment with radiation for women with early-stage invasive breast carcinoma or ductal carcinoma in situ. J Clin Oncol 26:386–391
Fischer U, Zachariae O, Baum F et al (2004) The influence of preoperative MRI of the breasts on recurrence rate in patients with breast cancer. Eur Radiol 14:1725–1731
Belloni E, Panizza P, De Cobelli F et al (2008) MR-guided stereotactic breast biopsy using a low cost mixed ferromagnetic-nonmagnetic coaxial system with small caliber needles (16–18 Gauge): feasibility, efficacy and safety. B-288 European Radiology, Supplement 1
Panizza P, De Cobelli F, De Gaspari A et al (2003) MR-guided stereotactic breast biopsy: technical aspects and preliminary results. Radiol Med 106:232–244
Chen X, Lehman CD, Dee KE (2004) MRI-guided breast biopsy: clinical experience with 14-gauge stainless steel core biopsy needle. AJR Am J Roentgenol 182:1075–1080
Kuhl CK, Morakkabati N, Leutner CC et al (2001) MR imaging—guided largecore (14-gauge) needle biopsy of small lesions visible at breast MR imaging alone. Radiology 220:31–39
Liberman L, Bracero N, Morris E et al (2005) MRI-guided 9-gauge vacuumassisted breast biopsy: initial clinical experience. AJR Am J Roentgenol 185:183–193
Pistolese CA, Ciarrapico AM, Della Gatta F et al (2009) Cost-effectiveness analysis of two vacuum-assisted breast biopsy systems: Mammotome and Vacora. Radiol Med 114:743–756
American College of Radiology (2003) Breast imaging reporting and data system (BI-RADS) atlas, 4th edn. American College of Radiology, Reston
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Carbognin, G., Girardi, V., Brandalise, A. et al. MR-guided vacuum-assisted breast biopsy in the management of incidental enhancing lesions detected by breast MR imaging. Radiol med 116, 876–885 (2011). https://doi.org/10.1007/s11547-011-0631-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-011-0631-7