Abstract
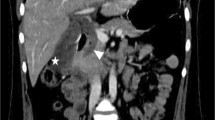
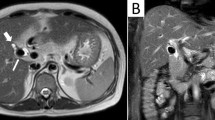
Pseudoaneurysm of the hepatic artery due to cholecystitis may be very rare, and in our survey of the literature, the present case report is the first case of such a pseudoaneurysm. A 64-year-old woman presented with upper gastrointestinal bleeding and severe epigastric pain. Upper gastrointestinal tract endoscopy revealed blood coming out of the papilla of Vater. Color-Doppler ultrasound imaging showed a pulsatile wave pattern in an echogenic lesion inside the gallbladder. Contrast-enhanced computed tomography demonstrated a 3-cm pseudoaneurysm in the distended gallbladder. Angiography disclosed extravasation originating from the right hepatic artery. Emergency selective transcatheter arterial embolization was performed, with intravascular stainless steel microcoils, and complete occlusion of the pseudoaneurysm was achieved. The patient underwent cholecystectomy with resection of the extrahepatic bile duct and biliary reconstruction in a Roux-en-Y fashion. Macroscopically, the resected gallbladder contained clotted blood and multiple cholesterol stones. Microscopically, the mucosa of the gallbladder showed extensive necrosis and many inflammatory cells. The final diagnosis was pseudoaneurysm of the hepatic artery associated with calculous gangrenous cholecystitis. Although the mechanism of the pseudoaneurysm remains speculative, severe inflammatory reaction in the gallbladder may have infiltrated the liver parenchyma and may have eroded the wall of the hepatic artery, thus forming a pseudoaneurysm. Hemobilia is one of the important differential diagnoses when unexplained gastrointestinal bleeding is observed, especially in patients with hepatobiliary diseases.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Akatsu, T., Hayashi, S., Egawa, T. et al. Hepatic artery pseudoaneurysm associated with cholecystitis that ruptured into the gallbladder. J Gastroenterol 39, 900–903 (2004). https://doi.org/10.1007/s00535-003-1408-0
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s00535-003-1408-0