Abstract
Pharyngoplasty represents one of the most widely performed surgical procedures for the treatment of obstructive sleep apnea (OSA) in the presence of palate–oropharyngeal collapse. The learning curve for pharyngoplasties is steep and success is conditional on the correct use of the sutures and the careful application of the surgical steps in a narrow surgical field. The use of synthetic models may be conveniently and safely employed for hands-on surgical practice in pharyngoplasties, especially when fresh frozen cadaveric specimens are not available. We present the “Pharyngolab”, a new simulator for pharyngoplasties.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Surgery for velopharyngeal Obstructive Sleep Apnea (OSA) started with uvulopalatopharyngoplasty or UPPP [1], which had a huge worldwide diffusion for at least 2 decades: UPPP involved the trimming/resection of the inferior part of the soft palate with the goal of creating space and enlarging the oropharyngeal inlet, but with remarkable long term side effects, such as dysphagia, globus sensation, persistent dryness, and voice changes.
Over the last 15–20 years, UPPP became progressively less popular, because the mentioned side effects were not accompanied by a satisfactory therapeutic efficacy: UPPP had a reported success rate of approximately 40–60% for improving mild to moderate OSA [2]. The recent evolution regarding pharyngoplasty techniques has been focused on the concept of obtaining the expansion and stabilization of the pharyngeal airspace through the treatment of the soft palate and lateral pharyngeal walls (LPW) collapse rather than through ablation of the redundant pharyngeal soft tissue [3].
The modern surgical approach started with Cahali [4], who understood that in OSA the real challenge was not to create space in the retropalatal space, but to fight the velopharyngeal hyper-collapsibility. His Lateral Pharyngoplasty was the first of the modern techniques that aims at centrifugal scarring. Lateral pharyngoplasty involves the transection of the palatopharyngeal muscle (PPM) and the splitting of the superior constrictor muscle (SCM).
The Expansion sphincter pharyngoplasty (ESP) was described by Pang and Woodson in 2007 [5]: it involves the caudal transection of PPM which is rotated and fixed superolaterally to the soft palate muscles. Up to date ESP is considered by most of the authors the gold standard for surgical treatment of velopharyngeal OSA.
The use of knotless barbed sutures has been introduced in OSA oropharyngeal surgery by Mantovani et al. [6]: barbed sutures are conceived to distribute tension along the full length of the thread route and to create dynamic vectors inside the soft tissue without the necessity of knots and avoiding subsequent ischaemic damage. Mantovani also introduced the rigid holds, where the palate–pharyngeal structures need to be suspended with barbed sutures (posterior nasal spine, pterygoid hamulus, palatal apneurosis, and pterygo-mandibular raphae). A customized surgical approach to OSA with three different barbed pharyngoplasties [7,8,9,10,11], each dedicated to a specific pattern of palato-oropharyngeal collapse, demonstrated an impressive success rate: the Barbed Anterior Pharyngoplasty (BAPh) for the antero-posterior collapse, the Barbed Roman Blinds Technique (BRBT) for the transversal collapse, and the Alianza (the combination of the BAPh and the BRBT) for the circular collapse.
The use of barbed sutures allows the surgeon to lift and stiffen the soft palate and to stabilize lateral pharyngeal walls to counteract their hyper-collapsibility during sleep while preserving their anatomical and functional integrity.
Several other barbed pharyngoplasty techniques have been described in the last 5–6 years. The most popular is the barbed reposition pharyngoplasty (BRP), described by Vicini et al.: the BRT is a palatal and pharyngeal lifting technique, an attempt to shorten, tense and conglomerate the redundant soft tissues of the soft palate and pharynx, by pulling up the soft palate and lateral pharyngeal structures toward the pterygomandibular raphe and posterior nasal spine [12, 13].
The most recent barbed pharyngoplasty technique is the Modified reposition pharyngoplasty (MRP), described by Carrasco et al. [14]: the main innovation of MRP is that it involves the removal at the supra-tonsillar fat.
Mastering both the surgical steps required to remodel the palato-oropharyngeal anatomical structures and the correct use of the sutures is key for this surgery. However, the learning curve is steep due to the limited surgical oropharyngeal workspace.
Human cadaver surgical skills training offers the highest fidelity simulation of the operating environment, but unfortunately the cost of biologic samples is prohibitive for many residency programs; furthermore, the availability of fresh human cadavers is limited by ethical and regulatory issues.
For this reason, low-cost, easy-to-build and easy-to-handle synthetic surgical models reproducing the palato-oropharyngeal anatomy were developed to expedite the surgical learning curve of residents and fellows when fresh frozen cadaveric specimens are not available [15]. The “Barbed Snore Surgery Simulator” designed by Rinaldi et al. [15] is a simple model mainly consisting of two components:
-
a finely detailed resin skeleton, the same size as an adult male skull, with the mandible fixed bilaterally with screws to the glenoid fossa allowing for adjustable inter-incisor distance;
-
a synthetic soft palate, manually shaped from a three-layer (simulating mucosal, submucosal and muscular layers) silicone model (approximately 3 × 4 × 1 cm) and glued on to the resin skeleton.
The main limitation of this simulator was the impossibility to work on lateral pharyngeal wall, thus providing a training model only for pharyngoplasty techniques addressing the soft palate (such as the Barbed Anterior Pharyngoplasty). Another limitation is represented by the technical difficulty in replacing a new synthetic soft palate at the end of the simulation.
The new simulator
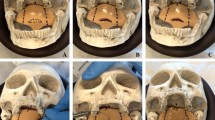
The authors have developed a new synthetic simulator (patent pending), the “Pharyngolab” (Fig. 1), which provides more anatomical details and the possibility to work even on the lateral pharyngeal walls, thus allowing to simulate all the barbed pharyngoplasty techniques, such as Alianza, BRP, and MRP and also many non-barbed techniques, such as ESP (Videos 1–4).
“Pharyngolab” is a three-dimensional synthetic model with a base (A) where to fix the removable and disposable cards containing the soft tissues, namely, the soft palate and lateral pharyngeal walls. Once the card has been secured to the base (B), it is possible to place the superstructure (which reproduces the oral cavity) over the base (C), securing it with two anti-release devices (D)
The simulator also ensures an easy and fast procedure to regenerate the soft tissues at the end of the simulation.
The “Pharyngo-Lab” is a three-dimensional synthetic model (Fig. 1) with a base (A) where to fix the removable and disposable cards containing the soft tissues, namely, the soft palate and lateral pharyngeal walls. Once the card has been secured to the base (B), it is possible to place the superstructure (which reproduces the oral cavity) over the base (C), securing it with two anti-release devices (D). At the end of the simulation, the superstructure can be removed to replace a new card and perform a new simulation.
We assessed the suitability of the Pharyngolab among 5 ENT specialists, with no surgical expertise in the field of pharyngoplasties, guided by a skilled surgeon in the execution of two different pharyngoplasty techniques: Alianza and ESP. All the surgeons completed the surgical simulations; the feedback from the participants was very positive, with a mean general impression of 9 points (out of 10) and a mean recommendation score of 9.5 for further use. The new simulator appeared to be very convenient for surgical training, with a high rate of approval and a highly recognized utility in transforming the simulated surgical steps into daily surgical practice.
The tissue consistency and anatomical proportions were compared to human anatomy through visual and palpatory impression by an expert surgeon who performed more than two hundred pharyngoplasty procedures. The main reported limitation of the Pharyngolab was the tissue consistence which resulted slightly different from that of a human, thus the application of excessive tension on the sutures leaded to the tearing of the tissues. Despite the limits of a synthetic simulator, the Pharyngolab seemed to reproduce a suitable anatomy and tissue consistence for surgical simulation. A minimum of 5 simulations on the Pharyngolab appeared adequate to allow the trainees to begin performing “supervised” pharyngoplasty on patients.
Conclusions
Training competent and professional surgeons efficiently and effectively requires innovation and modernization of educational methods [16]. With the growth of technology and the decrease in hands-on experience, there has been an increase in interest in using simulation.
The acquisition of surgical skills requires consistent practice, and evidence suggests that many of the technical skills can be learnt away from the operating theatre [17]. In addition, the more skilled surgeons could benefit from training in new techniques and technologies.
Palato-oropharyngeal remodeling surgery has become central in OSA surgical management.
The learning curve for pharyngoplasty is steep and success is conditional on the correct use of the sutures and the careful application of the surgical steps in a narrow surgical field. The use of synthetic models may be conveniently and safely employed for hands-on surgical practice.
The new improved simulator “Pharyngolab” allows the trainee to simulate many pharyngoplasty techniques (with or without barbed sutures), also providing more anatomical details and being more comparable in feel and use to real conditions.
References
Fujita S, Conway W, Zorick F, Roth T (1981) Surgical correction of anatomic abnormalities in obstructive sleep apnea syndrome: uvulopalatopharyngoplasty. Otolaryngol Head Neck Surg 89(6):923–934. https://doi.org/10.1177/019459988108900609
Mantovani M, Rinaldi V, Salamanca F, Torretta S, Carioli D, Gaffuri M, Pignataro L (2015) Should we stop performing uvulopalatopharyngoplasty? Indian J Otolaryngol Head Neck Surg 67(Suppl 1):161–162. https://doi.org/10.1007/s12070-014-0800-9
Sorrenti G, Pelligra I, Albertini R, Caccamo G, Piccin O (2018) Functional expansion pharyngoplasty: technical update by unidirectional barbed sutures. Clin Otolaryngol 43(5):1419–1421. https://doi.org/10.1111/coa.13105
Cahali MB (2003) Lateral pharyngoplasty: a new treatment for obstructive sleep apnea hypopnea syndrome. Laryngoscope 113(11):1961–1968. https://doi.org/10.1097/00005537-200311000-00020
Pang KP, Woodson BT (2007) Expansion sphincter pharyngoplasty: a new technique for the treatment of obstructive sleep apnea. Otolaryngol Head Neck Surg 137(1):110–114. https://doi.org/10.1016/j.otohns.2007.03.014
Mantovani M, Minetti A, Torretta S, Pincherle A, Tassone G, Pignataro L (2013) The, “Barbed Roman Blinds” technique: a step forward. Acta Otorhinolaryngol Ital 33(2):128
Mantovani M, Rinaldi V, Torretta S, Carioli D, Salamanca F, Pignataro L (2016) Barbed Roman blinds technique for the treatment of obstructive sleep apnea: how we do it? Eur Arch Otorhinolaryngol 273(2):517–523. https://doi.org/10.1007/s00405-015-3726-2
Rinaldi V, Costantino A, Moffa A, Cassano M, Mantovani M, Casale M, Pignataro L (2019) Postoperative pain and wound healing after Coblation-Assisted Barbed Anterior Pharyngoplasty (CABAPh): an observational study. Indian J Otolaryngol Head Neck Surg 71(Suppl 2):1157–1162. https://doi.org/10.1007/s12070-018-01577-8
Rinaldi V, Moffa A, Sabatino L, Cassano M, Passarelli PC, Mantovani M, Pignataro L, Casale M (2020) The efficacy of barbed sutures for anterior pharyngoplasty: technical aspects and preliminary results. J Biol Regul Homeost Agents 34(5 Suppl. 3):123–126 (Technology in Medicine)
Mantovani M, Pignataro L (2020) Barbed snore surgery (BSS). In: Sps S (ed) Sleep apnea and snoring—surgical and non-surgical therapy, 2nd edn. Elsevier, Amsterdam
Mantovani M, Carioli D, Torretta S, Rinaldi V, Ibba T, Pignataro L (2017) Barbed snore surgery for concentric collapse at the velum: the Alianza technique. J Craniomaxillofac Surg 45(11):1794–1800. https://doi.org/10.1016/j.jcms.2017.08.007
Montevecchi F, Meccariello G, Firinu E, Rashwan MS, Arigliani M, De Benedetto M, Palumbo A, Bahgat Y, Bahgat A, Lugo Saldana R, Marzetti A, Pignataro L, Mantovani M, Rinaldi V, Carrasco M, Freire F, Delgado I, Salamanca F, Bianchi A, Onerci M, Agostini P, Romano L, Benazzo M, Baptista P, Salzano F, Dallan I, Nuzzo S, Vicini C (2018) Prospective multicentre study on barbed reposition pharyngoplasty standing alone or as a part of multilevel surgery for sleep apnoea. Clin Otolaryngol 43(2):483–488. https://doi.org/10.1111/coa.13001
Babademez MA, Gul F, Kale H, Sancak M (2019) Technical update of barbed pharyngoplasty for retropalatal obstruction in obstructive sleep apnoea. J Laryngol Otol 133(7):622–626. https://doi.org/10.1017/S0022215119001518
Carrasco Llatas M, Valenzuela Gras M, Martínez Ruiz de Apodaca P, Dalmau Galofre J (2021) Modified reposition pharyngoplasty for OSAS treatment: How we do it and our results. Acta Otorrinolaringol Esp (Engl Ed). 72(3):152–157. https://doi.org/10.1016/j.otorri.2020.02.010 (English, Spanish)
Rinaldi V, Costantino A, Moffa A, Baptista P, Sabatino L, Casale M (2019) “Barbed snore surgery” simulator: a low-cost surgical model. Eur Arch Otorhinolaryngol 276(8):2345–2348. https://doi.org/10.1007/s00405-019-05497-3
Evans CH, Schenarts KD (2016) Evolving educational techniques in surgical training. Surg Clin N Am 96(1):71–88. https://doi.org/10.1016/j.suc.2015.09.005
Tan SS, Sarker SK (2011) Simulation in surgery: a review. Scott Med J 56(2):104–109. https://doi.org/10.1258/smj.2011.011098
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on sleep apnea syndrome. Guest editors: Manuele Casale, Rinaldi Vittorio.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary File1 (MP4 158183 kb)
Supplementary File2 (MP4 94661 kb)
Supplementary File3 (MP4 32435 kb)
Supplementary File4 (MP4 70630 kb)
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rinaldi, V., Mancini, G., de Apodaca, P.MR. et al. “Pharyngolab”: a new surgical simulator for pharyngoplasties. Eur Arch Otorhinolaryngol 280, 1339–1342 (2023). https://doi.org/10.1007/s00405-022-07667-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-022-07667-2