Summary
Background
The concept of initiating fibrinolytic therapy in patients who cannot undergo immediate percutaneous coronary intervention (PCI) in the setting of acute ST-segmentelevation myocardial infarction (STEMI) has been proposed as a strategy to improve outcomes. However, evidence supporting the use of this strategy is not conclusive, and the results of recent randomized controlled trials are apparently contradictory. Probably, the time points of administration of the adjunctive thrombolytics and antiplatelet agents and the time loss until coronary intervention have a major influence on the discrepancy of outcomes in different trials. Therefore, the relationship between therapeutic time intervals and outcome in patients treated with facilitated PCI has been analyzed.
Methods
In this single center retrospective study, 131 patients with STEMI were treated with a combined pharmaco-mechanical reperfusion strategy using half-dose r-tPA combined with a glycoprotein (GP) IIb/IIIa antagonist prior to PCI. Specific time points were recorded for each patient, including the time of symptom onset, the time of first medical contact, the start of intravenous thrombolysis, the time of administration of the GP IIb/IIIa antagonist and the start of coronary intervention. We then examined the relationship between the time delay from symptom onset to the initiation of various steps of treatment and the residual myocardial damage as expressed by the severity of both global and regional myocardial dysfunction calculated from a left ventriculography study performed 3 months later.
Results
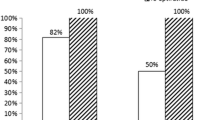
The median time from symptom onset to the first medical contact, with 25th and 75th percentiles in parentheses, was 1.25 h (0.75, 3), from symptom onset to initiation of thrombolytic therapy 2.25 h (1.25, 3), to initiation of GP IIb/ IIIa inhibitor therapy 3.5 h (2, 5.69), and to the start of coronary intervention 4.81 h (2.85, 7.91). The time between symptom onset and initiation of both thrombolytic therapy and coronary intervention was significantly related to the global ejection fraction and to the extent of regional hypokinesia at the 3-month follow-up (p<0.05). The time to the initiation of GP IIb/IIIa inhibitors was only significantly related to the global ejection fraction (p<0.05), while the time to the first medical contact did not show a similar relationship (p>0.05). Furthermore, we observed a significant relationship between the infarct-related artery (IRA) patency at the initial angiogram and the residual regional myocardial damage at follow-up; normokinesia at follow- up was found in 61.3% of patients with an initially patent IRA and in 41.2% of patients with an initially occluded IRA, whereas severe hypokinesia was found in 13.8% and 37.3%, respectively (p<0.05).
Conclusion
In patients with STEMI treated with a facili tated PCI strategy using half dose r-tPA in combination with a glycoprotein IIb/IIIa receptor blocker, the 3-month global and regional residual myocardial dysfunction is significantly related to the time elapsed between the onset of symptoms and the start of both fibrinolytic therapy and coronary intervention.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Antman EM, Anbe DT, Armstrong PW et al (2004) ACC/AHA Guidelines for the management of patients with ST-elevation myocardial infarctionexecutive summary: a report of the American College of Cardiology/ American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1999 Guidelines for the Management of Patients With Acute Myocardial Infarction). Circulation 110:588–636
Assessment of the Safety and Efficacy of a New Treatment Strategy with Percutaneous Coronary Intervention (ASSENT-4 PCI) Investigators (2006) Primary versus tenecteplase-facilitated percutaneous coronary intervention in patients with ST-segment elevation acute myocardial infarction (ASSENT-4 PCI): randomised trial. Lancet 367(9510):569–578
Fibrinolytic Therapy Trialist (FTT) Collaborative Group (1994) Indications for fibrinolytic therapy in suspected acute myocardial infarction: collaborative overview of early mortality and major morbidity results from all randomized trials of more than 1000 patients. Lancet 343:311– 322
Keeley EC, Boura JA, Grines CL (2003) Primary angioplasty versus intravenous thrombolytic therapy for acute myocardial infarction: a quantitative review of 23 randomised trials. Lancet 361:13–20
Le May MR, Wells GA, Labinaz M et al (2005) Combined angioplasty and pharmacological intervention versus thrombolysis alone in acute myocardial infarction (CAPITAL AMI study). J Am Coll Cardiol 46(3):417–424
Montalescot G, Barragan T, Wittenberg O et al for the ADMIRAL Investigators (2001) Platelet glycoprotein IIb/IIIa inhibition with coronary stenting for acute myocardial infarction. N Engl J Med 344:1895–1903
Nallamothu BK, Bates ER, Herrin J et al (2005) for the NRMI Investigators. Times to Treatment in Transfer Patients Undergoing Primary Percutaneous Coronary Intervention in the United States. National Registry of Myocardial Infarction (NRMI)-3/4 Analysis. Circulation 111:761–767
O'Neill WW, Weintraub R, Grines CL et al (1992) A prospective, placebocontrolled, randomized trial of intravenous streptokinase and angioplasty versus lone angioplasty therapy of acute myocardial infarction. Circulation 86:1710–1717
Schuler J, Maier B, Behrens S, Thimme W (2006) Present treatment of acute myocardial infarction in patients over 75 years. Data from the Berlin Myocardial Infarction Registry (BHIR). Clin Res Cardiol 95:360–367
Sheehan FH, Bolson EL, Dodge HT et al (1986) Advantages and applications of the centerline method for characterizing regional ventricular function. Circulation 74:293–305
The GUSTO V Investigators (2001) Reperfusion therapy for acute myocardial infarction with fibrinolytic therapy or combination reduced fibrinolytic therapy and platelet glycoprotein IIb/IIIa inhibition: the GUSTO V randomized trial. Lancet 357:1905– 1914
The TIMI Study Group (1989) Comparison of invasive and conservative strategies after treatment with intravenous tissue plasminogen activator in acute myocardial infarction. Results of the Thrombolysis In Myocardial Infarction (TIMI) Phase II trial. N Eng J Med 320:618–627
Toelg R, Witt M, Schwarz B et al (2006) Comparison of carvidolol and metoprolol in patients with acute myocardial infarction undergoing primary coronary intervention. The PASSAT Study. Clin Res Cardiol 95:31–41
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Meyborg, P., Abdel-Wahab, M., Herrmann, G. et al. Relationship between therapeutic time intervals and intermediate term left ventricular systolic function in patients treated with facilitated percutaneous coronary intervention for acute myocardial infarction. Clin Res Cardiol 96, 94–102 (2007). https://doi.org/10.1007/s00392-007-0465-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-007-0465-9