Abstract
Purpose:
Comparison of the amount of irradiated lung tissue volume and mass in patients with breast cancer treated with an optimized tangential-field technique with and without a deep inspiration breath-hold (DIBH) technique and its impact on the normal-tissue complication probability (NTCP).
Material and Methods:
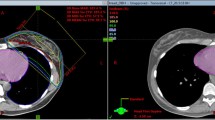
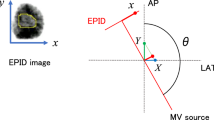
Computed tomography datasets of 60 patients in normal breathing (NB) and subsequently in DIBH were compared. With a Real-Time Position Management Respiratory Gating System (RPM), anteroposterior movement of the chest wall was monitored and a lower and upper threshold were defined. Ipsilateral lung and a restricted tangential region of the lung were delineated and the mean and maximum doses calculated. Irradiated lung tissue mass was computed based on density values. NTCP for lung was calculated using a modified Lyman-Kutcher-Burman (LKB) model.
Results:
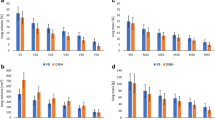
Mean dose to the ipsilateral lung in DIBH versus NB was significantly reduced by 15%. Mean lung mass calculation in the restricted area receiving ≤ 20 Gy (M20) was reduced by 17% in DIBH but associated with an increase in volume. NTCP showed an improvement in DIBH of 20%. The correlation of individual breathing amplitude with NTCP proved to be independent.
Conclusion:
The delineation of a restricted area provides the lung mass calculation in patients treated with tangential fields. DIBH reduces ipsilateral lung dose by inflation so that less tissue remains in the irradiated region and its efficiency is supported by a decrease of NTCP.
Zusammenfassung
Ziel:
Vergleichende Bestimmung von bestrahltem Lungenvolumen und bestrahlter Lungenmasse in Normalatmung (NB) und tiefer Inspiration (DIBH) bei PatientInnen mit Brustkrebs, die mit tangentialen Feldern bestrahlt wurden, und ihrem Einfluss auf die Normalgewebskomplikationswahrscheinlichkeit (NTCP).
Material und Methodik:
Computertomographiedatensätze von 60 PatientInnen wurden in NB und DIBH miteinander verglichen. Mit einem „Real-Time Position Management Respiratory Gating System“ (RPM) wurden die anteroposteriore Thoraxbewegung aufgezeichnet und untere und obere Schwellenwerte definiert. Die ipsilaterale Lunge sowie eine beschränkte tangentiale Lungenregion wurden konturiert und die mittlere und maximale Dosis berechnet. Die bestrahlte Lungenmasse wurde mittels Dichteberechnung bestimmt. Die NTCP für die Lunge wurde mit einem modifizierten Lyman-Kutcher-Burman-(LKB-)Modell errechnet.
Ergebnisse:
Die mittlere ipsilaterale Lungendosis war in DIBH gegenüber NB signifikant um 15% reduziert. Die mittlere Lungenmasse (errechnet nach Tabelle 1), die ≤ 20 Gy (M20) erhielt, war in DIBH um 17% reduziert, während das Lungenvolumen deutlich vergrößert war (Tabelle 2). NTCP zeigte in tiefer Inspiration eine Verbesserung von 20% (Abbildung 1). Der Zusammenhang der individuellen Atmungsamplitudenzunahme zwischen NB und DIBH mit dem vergrößerten Lungenvolumen konnte dargestellt werden (Abbildung 2), während keine Korrelation zwischen der individuell erreichten Atmungsamplitude mit der NTCP aufgezeigt werden konnte (Abbildung 3).
Schlussfolgerung:
Die Konturierung eines beschränkten Teils der ipsilateralen Lunge ermöglicht die Bestimmung der bestrahlten Lungenmasse bei Bestrahlung mit tangentialen Feldern. Bei tiefer Inspiration verbleibt ein geringerer Anteil an Lungengewebe im Feld und führt zu einer Reduktion der ipsilateralen Lungendosis, unterstützt durch eine Abnahme der NTCP.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Abo-Madyan Y, Polednik M, Rahn A, et al. Improving dose homogeneity in large breasts by IMRT. Efficacy and dosimetric accuracy of different techniques. Strahlenther Onkol 2008;184:86–92.
Ben-David MA, Sturtz DE, Griffith KA, et al. Long-term results of conservative surgery and radiotherapy for ductal carcinoma in situ using lung density correction: the University of Michigan experience. Breast J 2007;13:392–400.
Burman C, Kutcher GJ, Emami B, Goitein M. Fitting of normal tissue tolerance data to an analytic function. Int J Radiat Oncol Biol Phys 1991;21:123–35.
Butler LE, Forster KM, Stevens CW, et al. Dosimetric benefits of respiratory gating: a preliminary study. Appl Clin Med Phys 2004;5:16–24.
Cozzi L, Fogliata A, Buffa F, Bieri S. Dosimetric impact of computed tomography calibration on a commercial treatment planning system for external radiation therapy. Radiother Oncol 1998;48:335–8.
Denissova SI, Yewondwossen MH, Andrew JW, et al. A gated deep inspiration breath-hold radiation therapy technique using a linear position transducer. J Appl Clin Med Phys 2005;6:61–70.
Fogliata A, Nicolini G, Vanetti E, et al. The impact of photon dose calculation algorithms on expected dose distributions in lungs under different respiratory phases. Phys Med Biol 2008;53:2375–90.
Forster KM, Starkschall G, Butler L, et al. The dose mass histogram: a tool for evaluating thoracic treatment plans. Med Phys 2001;28:1228–9.
Gulybán A, Kovács P, Sebestyén Z, et al. Multisegmented tangential breast fields: a rational way to treat breast cancer. Strahlenther Onkol 2008;184:262–9.
Kini VR, Vedam SS, Keall PJ, et al. Patient training in respiratory-gated radiotherapy. Med Dosim 2003;28:7–11.
Korreman S, Pedersen A, Aarup L, et al. Reduction of cardiac and pulmonary complication probabilities after breathing adapted radiotherapy for breast cancer. Int J Radiat Oncol Biol Phys 2006;65:1375–80.
Korreman S, Pedersen A, Nøttrup T, et al. Breathing adapted radiotherapy for breast cancer: comparison of free breathing gating with the breath-hold technique. Radiother Oncol 2005;76:311–8.
Krengli M, Sacco M, Loi G, et al. Pulmonary changes after radiotherapy for conservative treatment of breast cancer: a prospective study. Int J Radiat Oncol Biol Phys 2008;70:1460–7.
Kubo HD, Wang L. Introduction of audio gating to further reduce organ motion in breathing synchronized radiotherapy. Med Phys 2002;29:345–50.
Kutcher GJ, Burman C. Calculation of complication probability factors for non-uniform normal tissue irradiation. Int J Radiat Oncol Biol Phys 1989;16:1623–30.
Kwa SLK, Lebesque JV, Theuws JCM, et al. Radiation pneumonitis as a function of mean lung dose: an analysis of pooled data of 540 PTs. Int J Radiat Oncol Biol Phys 1998;28:575–81.
Lind PA, Wennberg B, Gagliardi G, Fornander T. Pulmonary complications following different radiotherapy techniques for breast cancer, and the association of irradiated lung volume and dose. Breast Cancer Res Treat 2001;68:199–210.
Lind PA, Wennberg B, Gagliardi G, et al. ROC curves and evaluation of radiation-induced pulmonary toxicity in breast cancer. Int J Radiat Oncol Biol Phys 2006;64:765–70.
Ludwig V, Schwab F, Guckenberger M, et al. Comparison of wedge versus segmented techniques in whole breast irradiation. Effects on dose exposure outside the treatment volume. Strahlenther Onkol 2008;184:307–12.
Lyman JT. Complication probability as assessed from dose-volume histograms. Radiat Res 1985;104:13–9.
Mavroidis P, Plataniotis G, Gorka MA, Lind BK. Comments on “Reconsidering the definition of a dose-volume histogram” — dose-mass histogram (DMH) versus dose-volume histogram (DVH) for predicting radiation-induced pneumonitis. Phys Med Biol 2006;51:L43–50.
Minor GI, Yashar CM, Spanos WJ Jr, et al. The relationship of radiation pneumonitis to treated lung volume in breast conservation therapy. Breast J 2006;12:48–52.
Pierce LJ, Griffith KA, Hayman JA, et al. Conservative surgery and radiotherapy for stage I/II breast cancer using lung density correction: 10-year and 15-year results. Int J Radiat Oncol Biol Phys 2005;61:1317–27.
Semenenko VA, Li XA. Lyman-Kutcher-Burman NTCP model parameters for radiation pneumonitis and xerostomia based on combined analysis of published clinical data. Phys Med Biol 2008;53:737–55.
START Trialists’ Group, Bentzen SM, Agrawal RK, Aird EG, et al. The UK Standardisation of Breast Radiotherapy (START) Trial A of radiotherapy hypofractionation for treatment of early breast cancer: a randomised trial. Lancet Oncol 2008;9:331–41.
START Trialists’ Group, Bentzen SM, Agrawal RK, Aird EG, et al. The UK Standardisation of Breast Radiotherapy (START) Trial B of radiotherapy hypofractionation for treatment of early breast cancer: a randomised trial. Lancet 2008;371:1098–107.
Stranzl H, Zurl B. Postoperative irradiation of left-sided breast cancer patients and cardiac toxicity. Does deep inspiration breath-hold (DIBH) technique protect the heart? Strahlenther Onkol 2008;184:354–8.
Stranzl H, Zurl B, Langsenlehner T, Kapp KS. Wide tangential fields including the internal mammary lymph nodes in patients with left-sided breast cancer. Strahlenther Onkol 2009;185:155–60.
Theuws JCM, Kwa SLS, Wagenaar AC, et al. Dose-effect relations for early local pulmonary injury after irradiation for malignant lymphoma and breast cancer. Radiother Oncol 1998;48:33–43.
Thomas SJ. Relative electron density calibration of CT scanners for radiotherapy treatment planning. Br J Radiol 1999;72:781–6.
Tucker SL, Liu HH, Liao Z, et al. Analysis of radiation pneumonitis risk using a generalized Lyman model. Int J Radiat Oncol Biol Phys 2008;72:568–74.
Vågane R, Danielsen T, Fosså SD, et al. Late regional density changes of the lung after radiotherapy for breast cancer. Radiother Oncol 2009;90:148–52.
Varian Medical Systems. RPM respiratory gating system reference guide. Palo Alto: Varian Medical Systems, 2007.
Willner J, Jost A, Baier K, Flentje M. A little to a lot or a lot to a little? An analysis of pneumonitis risk from dose-volume histogram parameters of the lung in patients with lung cancer treated with 3-D conformal radiotherapy. Strahlenther Onkol 2003;179:548–56.
Yuan R, Mayo JR, Hogg JC, et al. The effects of radiation dose and CT manufacturer on measurements of lung densitometry. Chest 2007;132:617–23.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zurl, B., Stranzl, H., Winkler, P. et al. Quantitative Assessment of Irradiated Lung Volume and Lung Mass in Breast Cancer Patients Treated with Tangential Fields in Combination with Deep Inspiration Breath Hold (DIBH). Strahlenther Onkol 186, 157–162 (2010). https://doi.org/10.1007/s00066-010-2064-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-010-2064-y