Abstract
Background
Proteinuria is a non-specific marker of inflammation that may reflect the glomerular component of systemic capillary leak. The objective of this pilot study was to determine if postoperative proteinuria is associated with adverse outcomes following cardiac surgery with cardiopulmonary bypass.
Methods
Eligible patients were individuals undergoing cardiac surgery with cardiopulmonary bypass who did not have severe pre-existing renal dysfunction. Urine was collected after induction of anesthesia (baseline) and two to four hours after arrival to the intensive care unit (ICU). Proteinuria was measured as random protein creatinine ratio in g·mol-1. Adverse events were defineda priori as prolonged ICU stay (≥ 90th percentile) and organ dysfunction. The relationship between proteinuria and adverse events was assessed by bivariate (Chi-square or Fisher’s exact tests) and multivariable (multiple logistic regression) analyses.
Results
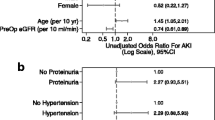
The study included 197 (of 243 eligible) patients. Postoperative proteinuria (protein creatinine ratio ≥ 30 g·mol-1) was associated with prolonged (≥ four days) ICU stay [odds ratio (OR) 7.0; 95% confidence interval (CI) 2.8-17.1] and organ dysfunction (OR 3.9; CI 1.9-8.1). After adjustment for confounders, proteinuria was associated with a 3.2-fold increase in the odds of both prolonged ICU stay (CI 1.1-9.7) and organ dysfunction (CI 1.4-7.0).
Conclusions
Proteinuria two to four hours after cardiac surgery with cardiopulmonary bypass may be a useful marker for systemic capillary leak and adverse postoperative events. Large prospective studies are needed to confirm these findings. Objectif : La protéinurie est un marqueur non spécifique de ľinflammation qui peut illustrer la composante glomérulaire ďune fuite capillaire systémique. Nous voulions déterminer si la protéinurie postopératoire est associée à des complications de la chirurgie cardiaque avec circulation extracorporelle.
Résumé
Méthode
Les patients admissibles devaient subir une opération cardiaque avec circulation extracorporelle, mais ne devaient pas présenter de dysfonction rénale sévère préexistante. Ľurine a été recueillie après ľinduction de ľanesthésie (conditions de départ) et entre deux et quatre heures après ľarrivée à ľunité des soins intensifs (USI). La protéinurie a été mesurée comme le ratio aléatoire protéine-créatinine en g·mol-1. Les événements indésirables ont été définis a priori : un séjour prolongé à ľUSI (≥ 90e percentile) et une dysfonction organique. La relation entre la protéinurie et les événements indésirables a été évaluée par des analyses bivariée (chi carré et tests exacts de Fisher) et multivariée (régression logistique multiple).
Résultats
Ľétude a porté sur 197 des 243 patients admissibles. La protéinurie postopératoire (ratio protéine créatinine ≥ 30 g·mol-1) a été associée à un séjour prolongé (≥ quatre jours) à ľUSI [risque relatif (RR) 7,0 ; intervalle de confiance de 95 % (IC) 2,8-17,1] et à une dysfonction organique (RR 3,9; IC 1,9-8,1). Après ajustements pour les facteurs de confusion, la protéinurie a été associée à 3,2 fois ďaugmentation des risques relatifs du séjour prolongé à ľUSI (IC 1,1-9,7) et de la dysfonction organique (IC 1,4-7,0).
Conclusion
La protéinurie mesurée deux à quatre heures après une intervention en chirurgie cardiaque avec circulation extracorporelle peut être un marqueur indiquant une fuite capillaire systémique et des événements postopératoires indésirables. Ces résultats devront être confirmés dans de grandes études prospectives.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Paparella D, Yau TM, Young E. Cardiopulmonary bypass induced inflammation: pathophysiology and treatment. An update. Eur J Cardiothorac Surg 2002; 21: 232–44.
Laffey JG, Boylan JF, Cheng DC. The systemic inflammatory response to cardiac surgery. Anesthesiology 2002; 97: 215–52.
Evans G, Greaves I. Microalbuminemia as predictor of outcome. Shows promise but large prospective trials are needed. BMJ 1999; 318: 207–8.
Zikria BA, Bascom JU. Mechanisms of multiple system organ failure.In: Zikria BA, Oz MO, Carlson RW (Eds). Reperfusion Injuries and Clinical Capillary Leak Syndrome. Armonk: Futura Publishing Company; 1994: 443, 489.
Szakmany T, Molnar Z. Increased glomerular permeability and pulmonary dysfunction following major surgery: correlation of microalbuminuria and PaO2/FiO2 ratio. Acta Anaesthesiol Scand 2004; 48: 704–10.
Koike K, Aiboshi J, Shinozawa Y, Sekine K, Endo T, Yamamoto Y. Correlation of glomerular permeability, endothelial injury, and postoperative multiple organ dysfunction. Surg Today 2004; 34: 811–6.
Gosling P, Brudney S, McCrath L, Riseboro S, Manji M. Mortality prediction at admission to intensive care: a comparison of microalbuminuria with acute physiology scores after 24 hours. Crit Care Med 2003; 31: 98–103.
Thorevska N, Sabahi R, Upadya A, Manthous C, Amoateng-Adjepong Y. Microalbuminuria in criticallyill medical patients: prevalence, predictors, and prognostic significance. Crit Care Med 2003; 31: 1075–81.
Bianchi RA, Silva NA, Natal ML, Romero MC. Utility of base deficit, lactic acid, microalbuminuria, and C-reactive protein in the early detection of complications in the immediate postoperative evolution. Clin Biochem 2004; 37: 404–7.
De Gaudio AR,Spina R, DiFlippo A,Feri M. Glomerular permeability and trauma: a correlation between microalbuminuria and injury severity score. Crit Care Med 1999; 27: 2105–8.
Pallister I, Gosling P, Kaya A, Bradley S. Prediction of posttraumatic adult respiratory distress syndrome by albumin excretion rate eight hours after admission. J Trauma 1997; 42: 1056–61.
Brudney CS, Gosling P, Manji M. Pulmonary and renal function following cardiopulmonary bypass is associated with systemic capillary leak. J Cardiothorac Vasc Anesth 2005; 19: 188–92.
Karkouti K, Wijeysundera DN, Yau TM, et al. Platelet transfusions are not associated with increased morbidity or mortality in cardiac surgery. Can J Anesth 2006; 53: 279–87.
American Society of Anesthesiologists. Practice guidelines for blood component therapy. A report by the American Society of Anesthesiologists Task Force on Blood Component Therapy. Anesthesiology 1996; 84: 732–47.
National Kidney Foundation. K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification and stratification. Am J Kidney Dis 2002; 39(Suppl 1): S1–266.
Jensen JS, Borch-Johnsen K, Jensen G, Feldt-Rasmussen B. Microalbuminuria reflects a generalized transvascular albumin leakiness in clinically healthy subjects. Clin Sci 1995; 88: 629–33.
Sarti A, De Gaudio R,Messineo A, Cuttini M, Ventura A. Glomerular permeability after surgical trauma in children: relationship between microalbuminuria and surgical stress score. Crit Care Med 2001; 29: 1626–9.
Jensen JS, Clausen P, Borch-Johnsen K, Jensen G, Feldt-Rasmussen B. Detecting microalbuminuria by urinary albumin/creatinine concentration ratio. Nephrol Dial Transplant 1997; 12(Suppl 2): 6–9.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Karkouti, K., Shayan, S., Wijeysundera, D.N. et al. Prognostic value of postoperative proteinuria in cardiac surgery: a pilot study. Can J Anesth 53, 500–506 (2006). https://doi.org/10.1007/BF03022624
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03022624