Abstract
Purpose: To determine the minimum effective dose of dexamethasone in preventing nausea and vomiting associated with epidural morphine for post-Cesarean analgesia.
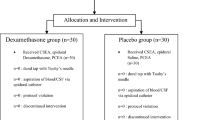
Method: One hundred and eighty parturients (n=45 in each of four groups) requiring epidural morphine for post-Cesarean analgesia were enrolled in this randomized, double-blinded, placebo-controlled study. At the end of surgery, parturients received either dexamethasone, at doses of 10 mg, 5 mg, 2.5 mg, or salineiv. Three milligrams epidural morphine were given to all parturients for postoperative analgesia. The incidence of PONV and side effects were estimated for 24 hr after delivery by blinded, trained nurse anesthetists.
Results: Parturients who received dexamethasone, either 10 mg or 5 mg were different from those who received saline alone in the following parameters: the total incidence of nausea and vomiting, incidence of >4 vomiting episodes, number the of parturients requiring rescue antiemetics, and the total number of parturients with no vomiting and/or no antiemetic medication (P<0.05 toP<0.01). The differences between dexamethasone 10 mg and 5 mg were not significant. Dexamethasone 2.5 mg was partially effective.
Conclusion: Dexamethasone, 5 mgiv, is suggested as the minimum effective dose in preventing nausea and vomiting associated with epidural morphine for post-Cesarean analgesia.
Résumé
Objectif: Déterminer la dose efficace minimale de dexaméthasone à utiliser pour prévenir les nausées et les vomissements liés à l’administration épidurale de morphine comme analgésie post-césarienne.
Méthode: Cent quatre-vingt parturientes (n=45 dans chacun des quatre groupes), nécessitant une analgésie épidurale post-césarienne avec morphine, ont participé à l’étude randomisée et à double insu contre placebo. Elles ont reçu, à la fin de l’opération, soit 10 mg, 5 mg ou 2,5 mg de dexaméthasone, soit une solution saléeiv. Toutes ont reçu 3 mg de morphine comme analgésie postopératoire épidurale. L’incidence des NVPO et des effets secondaires a été évaluée pendant vingt-quatre heures après l’accouchement par des infirmières impartiales diplômées en anesthésie.
Résultats: Les parturientes qui ont reçu 10 mg ou 5 mg de dexaméthasone ont présenté des caractéristiques différentes de celles qui ont reçu le placebo pour les paramètres suivants: l’incidence totale de nausées et de vomissements, l’incidence d’épisodes de vomissements >4, le nombre de patientes qui ont eu besoin d’antiémétiques de secours et le nombre total de parturientes sans vomissements et/ou sans médication antiémétique (P<0,05àP<0,01). Aucune différence significative n’était liée aux doses de 10 mg et de 5 mg de dexaméthasone. La dexaméthasone à 2,5 mg n’a été que partiellement efficace.
Conclusion: La dexaméthasone, administrée en doses de 5 mgiv, est suggérée comme la dose efficace minimale pour prévenir les nausées et les vomissements associés à l’analgésie épidurale post-césarienne avec de la morphine.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Cousins MJ, Mather LE. Intrathecal and epidural administration of opioids. Anesthesiology 1984; 61: 276–310.
Ngan Kee WD, Lam KK, Chen PP, Gin T. Epidural meperidine after Cesarean section. A dose-response study. Anesthesiology 1996; 85: 289–94.
Grass JA, Sakima NT, Schmidt R, Michitsch R, Zuckerman RL, Harris AP. A randomized, doubleblind, dose-response comparison of epidural fentanyl versus sufentanil analgesia after Cesarean section. Anesth Analg 1997; 85: 365–71.
Fuller JG, McMorland GH, Douglas MJ, Palmer L. Epidural morphine for analgesia after Caesarean section: a report of 4880 patients. Can J Anaesth 1990; 37: 636–40.
Harrison DM, Sinatra R, Morgese L, Chung JH. Epidural narcotic and patient-controlled analgesia for post-Cesarean section pain relief. Anesthesiology 1988; 68: 454–7.
Sanansilp V, Areewatana S, Tonsukchai N. Droperidol and the side effects of epidural morphine after Cesarean section. Anesth Analg 1998; 86: 532–7.
Kotelko DM, Rottman RL, Wright WC, Stone JJ, Yamashiro AY, Rosenblatt RM. Transdermal scopolamine decreases nausea and vomiting following Cesarean section in patients receiving epidural morphine. Anesthesiology 1989; 71: 675–8.
Chaney MA. Side effects of intrathecal and epidural opiods. Can J Anaesth 1995; 42: 891–903.
Fujii Y, Tanaka H, Toyooka H. Granisetron-dexamethasone combination reduces postoperative nausea and vomiting. Can J Anaesth 1995; 42: 387–90.
López-Olaondo L, Carrascosa F, Pueyo FJ, Monedero P, Busto N, Sáez A. Combination of ondansetron and dexamethasone in the prophylaxis of postoperative nausea and vomiting. Br J Anaesth 1996; 76: 835–40.
Jiménez-Jiménez FJ, García-Ruiz PJ, Molina JA. Drug-induced movement disorders. Drug Saf 1997; 16: 180–204.
Brunton LL. Drugs affecting gastrointestinal function.In: Hardman JG, Limbird LE, Molinoff PB, Ruddon RW, Hardman JG, Limbird LE, Molinoff PB, Ruddon RW, Gillman AG (Eds.). Goodman and Gillman’s The Pharmacological Basis of Therapeutics, 9th ed. New York: McGraw-Hill, 1996: 899–936.
Wang J-J, Ho S-T, Lee S-C, Liu Y-C, Liu Y-H, Liao Y-C. The prophylactic effect of dexamethasone on post-operative nausea and vomiting in women undergoing thyroidectomy: a comparison of droperidol with saline. Anestha Analg 1999; 89: 200–3.
Tzeng JI, Wang JJ, Ho ST, Tang CS, Liu YC, Lee SC. Dexamethasone for the prophylaxis of nausea and vomiting after epidural morphine for post-Caesarean section analgesia: a comparison of droperidol with saline. Br J Anaesth 2000; 85: 1–4.
Splinter WM, Roberts DJ. Prophylaxis for vomiting by children after tonsillectomy: dexamethasone versus perphenazine. Anesth Analg 1997; 85: 534–7.
Wang JJ, Ho ST, Liu YH, et al. Dexamethasone reduces nausea and vomiting after laparoscopic cholecystectomy. Br J Anaesth 1999; 83: 772–5.
Fujii Y, Tanaka H, Toyooka H. The effects of dexamethasone on antiemetics in female patients undergoing gynecologic surgery. Anesth Analg 1997; 85: 913–7.
Henzi I, Walder B, Tramér MR. Dexamethasone for the prevention of postoperative nausea and vomiting: a quantitative systemic review. Anesth Analg 2000; 90: 186–94.
Lerman J. Study design in clinical research: sample size estimation and power analysis. Can J Anaesth 1996; 43: 184–91.
Schimmer BP, Parker KL. Adrenocorticotropic hormone; adrencortical steroids and their synthetic analogs; inhibitors of the synthesis and actions of adrenocortical hormones.In: Hardman JG, Limbird LE, Molinoff PB, Ruddon RW, Gillman AG (Eds.). Goodman and Gillman’s Pharmacological Basis of Therapeutics, 9th ed. New York: McGraw-Hill, 1996: 1459–85.
Morimoto M, Morita N, Ozawa H, Yokoyama K, Kawata M. Distribution of glucocorticoid receptor immunoreactivity and mRNA in the rat brain: an immunohistochemical andin situ hybridization study. Neurosci Res 1996; 26: 235–69.
Funder JW. Mineralcorticoid receptors and glucocorticoid receptors. Clin Endocrinol 1996; 45: 651–6.
Watcha MF, White PF. Postoperative nausea and vomiting. Its etiology, treatment, and prevention. Anesthesiology 1992; 77: 162–84.
Cohen MM, Duncan PG, DeBoer DP, Tweed WA. The postoperative interview: assessing risk factors for nausea and vomiting. Anesth Analg 1994; 78: 7–16.
Wang J-J, Ho S-T, Tzeng J-I, Tang C-S. The effect of timing of dexamethasone administration on its efficacy as a prophylatic antiemetic for postoperative nausea and vomiting. Anesth Analg 2000; 91: 136–9.
Cook AM, Patterson H, Nicholls J, Huddart RA. Avascular necrosis in patients treated with BEP chemotherapy for testicular tumours. Clin Oncol 1999; 11: 126–7.
Author information
Authors and Affiliations
Corresponding author
Additional information
The work was done in the Tri-Service General Hospital, National Defense Medical Center, Taipei, Taiwan.
Rights and permissions
About this article
Cite this article
Wang, JJ., Ho, ST., Wong, CS. et al. Dexamethasone prophylaxis of nausea and vomiting after epidural morphine for post-Cesarean analgesia. Can J Anaesth 48, 185–190 (2001). https://doi.org/10.1007/BF03019733
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03019733