Abstract
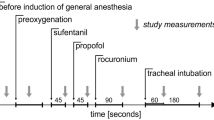
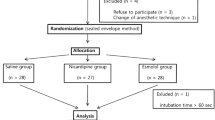
Esmolol, an ultra-short-acting cardioselective betaadrenergic blocker, was investigated in a double-blind prospective protocol for its ability to control haemodynamic responses associated with tracheal intubation after thiopentone and succinylcholine. Thirty ASA physical status I patients received a 12-minute infusion of esmolol (500 µg·kg-1·min-1 for four minutes, then 300 µg·kg-1 min-1 for 8 mnutes) or saline. Five minutes after the start of the drug/placebo infusion, anaesthesia was induced with 4 mg·kg-1 thiopentone followed by succinylcholine for tracheal intubation. Prior to induction esmolol produced significant decreases in heart rate (HR) (9.3 ± 1.8 per cent) and rate-pressure product (RPP) (13.1 ± 1.8 per cent), systolic blood pressure (SAP) (4.3 ± 1.5 per cent) and mean arterial blood pressure (MAP) (1.7 ± 2.0 per cent). Increases in HR, SAP and RPP after intubation were approximately 50 per cent less in patients given esmolol compared to patients given placebo. There were highly significant differences in HR (p < 0.0001), and RPP (p < 0.0005) and significant differences in SAP (p < 0.05) when the maximal esmolol post-intubation response was compared to the maximal placebo response. Infusion of esmolol in the dose utilized in this study significantly attenuated but did not completely eliminate cardiovascular responses to intubation.
Résumé
L’esmolol, un bloquer bêta-adrénergique cardiosélectif de courte durée d’action a été investigué dans une étude prospective à double insu pour sa capacité de contrôler les réponses hémodynamiques associées à l’intubation trachéale après thiopentone et succinylcholine. Trente patients ASA I ont requ une perfusion de 12 minutes d’esmolol (500 µg ·kg-1· min-1 pour quatre minutes, puis 300 µg ·kg-1 pour huit minutes) ou du salin. Cinq minutes après le début de la perfusion du médicament ou du placebo, l’ anesthésie était induite avec 4 mg·kg-1 de thiopentone suivi de succinylcholine pour l’intubation trachéale. Avant l’induction l’esmolol a produit une diminution significative de la fréquence cardiaque (HR) (9.3 ± 1.8 pour cent) et du produit fréquence-pression (RPP) (13.1 ±1.8 pour cent), de la tension artérielle systolique (SAP) (4.3 ± 1.5 pour cent) et de la pression artérielle mopenne (MAP) (1.7 ± 2.0 pour cent). Après l’intubation, l’augmentation dans la fréquence cardiaque, la pression artérielle systolique et la produit fréquence-pression était approximativement 50 pour cent moindre chez les patients ayant reçu de l’esmolol que chez les patients ayant regu du placebo. Il y avait une difference hautement significative dans la frequence cardiaque (p < 0.0001) et dans le produit fréquencepression (p < 0.0005) ainsi qu’une difference significative dans la pression artérielle systolique (p < 0.05) quand la réponse maximale post-intubation à l’esmolol a été comparée à la réponse maximale au placebo. La perfusion d’esmolol aux doses utilisées dans cette étude atténue significativement mais n’élimine pas complètement les réponses cardiovasculaires à l’intubation.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Reilly CS, Wood M, Wood AJJ. Comparative potencies of esmolol, a short-acting beta-blocker and propranolol in man. Anesthesiology 1984; 61: A18.
Forbes AM, Dally FG. Acute hypertension during induction of anaesthesia and endotracheal intubation in normotensive man. Br J Anaesth 1970; 42: 618- 24.
Roy WL, Edelist G, Gilbert B. Myocardial ischemia during non-cardiac surgical procedures in patients with coronary artery disease. Anesthesiology 1979; 51: 393–7.
Fox EJ, Sklar GS, Hill CH, VillanuevaR, King BD. Complications related to the pressor response to endotracheal intubation. Anesthesiology 1977; 47: 524–5.
Prys-Roberts C, Green LT, Meloche R, Foex P. Studies of anaesthesia in relation to hypertension II: haemodynamic consequences of induction and endotracheal intubation. Br J Anaesth 1971 ; 43: 531–46.
Gold MI, Brown MS, Selem JS. The effects of esmolol on hemodynamics after ketamine induction and intubation. Anesthesiology; 1984: 61: A19.
Menkhaus PG, Reves JG, Kissin I et al. Cardiovascular effects of esmolol in anesthetized humans. Anesth Analg 1985; 64: 327–34.
Dingle HR. Antihypertensive drugs and anaesthesia. Anaesthesia 1966; 21: 151–72.
Giles RW, Berger HJ,Barash PG et al. Continuous monitoring of left ventricular performance with the computerized nuclear probe during laryngoscopy and intubation before coronary artery bypass surgery. Am J Cardiol 1982; 50: 735–41.
Katz R, Bigger JT. Cardiac arrhythmias during anaesthesia and operation. Anesthesiology 1970; 33: 193–213.
Ward RJ, Allen GD, Deveny U et al. Halothane and the cardiovascular response to endotracheal intubation. Anesth Analg 1965; 44: 248–52.
Ganthler J, Bosomworth P, Page D et al. Effect of endotracheal intubation on electrocardiographic patterns during halothane anesthesia. Anesth Analg 1962; 41: 466–70.
Kaplan JA, King SB. The precordial electrocardiographic lead (V) in patients who have coronaryartery disease. Anesthesiology 1976; 45: 570–4.
Russell WJ, Morris RG, Frewin DB, Drew SE. Changes in plasma catecholamine concentrations during endotracheal intubation. Br J Anaesth 1981; 53: 837–9.
Derbyshire DR, Chmielewski D, Fell D, Vater M, Achola K, Smith G. Plasma catecholamine response to tracheal intubation. Br J Anaesth 1983; 55: 855–9.
Cork RC, Weiss JL, Hameroff SR, Bentley J. Pretreatment with low-dose fentanyl for rapid sequence intubation. Anesth Analg 1984; 63: 60–4.
Dohi S, Nishikawa T, Ujike Y, Mayumi T. Circulatory responses to airway stimulation and cervical epidural blockade. Anesthesiology 1982; 57: 359–63.
Delaney TJ, Kistner JR, Lake CL, Miller ED, Jr. Myocardial function during halothane and enflurane in patients with coronary artery disease. Anesth Analg 1980; 59: 240–4.
Martin DE, Rosenberg H, Aukburg SJ et al. Lowdose fentanyl blunts circulatory responses to tracheal intubation. Anesth Analg 1982; 61: 680–4.
Dahlgren N, Messeter K. Treatment of stress response to laryngoscopy and intubation with fentanyl. Anaesthesia 1981; 36: 1022–6.
Kautto UM. Attenuation of the circulatory response to laryngoscopy and intubation by fentanyl. Acta Anaesthesiol Scand 1982; 26: 217–21.
Barash PG, Giles R, MarxP, Berger H, Zaret B. Intubation: is low dose fentanyl really effective? Anesth Analg 1982; 61: 168–9.
Parker EO, Ross AL. Low dose fentanyl: effect on thiopental requirements and hemodynamic response during induction and intubation. Anesthesiology 1982; 57: A322.
Hamill JF, Bedford RF, Weaver DC, Colohan AR. Lidocaine before endotracheal intubation: intravenous or laryngotracheal? Anesthesiology 1981; 55: 578–81.
Abou-Madi MN,Kezler H,Yacoub JM. Cardiovascular reactions to laryngoscopy and intubation following small and large intravenous doses of lidocaine. Can Anaesth Soc J 1977; 24: 12–9.
Stoelting RK. Circulatory changes during direct laryngoscopy and tracheal intubation: influence of duration of laryngoscopy with and withour prior lidocaine. Anesthesiology 1977; 47: 381–4.
Denlinger JK, Ellison N, Ominski AJ. Effect of intratracheal lidocaine on circulatory responses to tracheal intubation. Anesthesiology 1974; 41: 409–12.
Abou-Madi M, Kezler H, Yacoub O. A method for prevention of cardiovascular reactions to laryngoscopy and intubation. Can Anaesth Soc J 1975; 22: 316–29.
Kautto UM, Heinonen J. Attenuation of circulatory response to laryngoscopy and tracheal intubation: a comparison of two methods of topical anaesthesia. Acta Anaesthesiol Scand 1982; 26: 599–602.
Stoelting RK. Attenuation of blood pressure response to laryngoscopy and tracheal intubation with sodium nitroprusside. Anesth Analg 1979; 58: 116–9.
Coriat P, Daloz M, Bousseau D, Fusciardi J, Echter E, Viars P. Prevention of intraoperative ischemia during noncardiac surgery with nitroglycerin. Anesthesiology 1984; 61: 193–6.
Thomson IR, Mutch WAC, Culligan JD. Failure of intravenous nitroglycerin to prevent intraoperative ischemia during fentanylpancuronium anesthesia. Anesthesiology 1984; 61: 385–93.
Prys-Roberts, C, Foex P, Biro GP, Roberts JG. Studies of anaesthesia in relation to hypertension. V. Adrenergic beta-receptor blockade. Br J Anaesth 1973; 45: 671–680.
Gatt S, Hurley R, Fox J, Feldman HS, Moller RA, Covino BG. Evaluation of acute cardiovascular effects of esmolol in the dog-awake and anesthetized with halothane and enflurane. Anesthesiology 1984; 51: A17.
Reves JG, Kissin I, Fournier S. Effects of esmolol, a short-acting beta-blocker in enflurane anesthetized dogs. Anesthesiology 1983; 59: A58.
Author information
Authors and Affiliations
Additional information
This investigation was supported by a grant from American Critical Care, McGaw Park, Illinois.
Rights and permissions
About this article
Cite this article
Liu, P.L., Gatt, S., Gugino, L.D. et al. Esmolol for control of increases in heart rate and blood pressure during tracheal intubation after thiopentone and succinylcholine. Can Anaesth Soc J 33, 556–562 (1986). https://doi.org/10.1007/BF03014260
Issue Date:
DOI: https://doi.org/10.1007/BF03014260