Abstract
Purpose
To clarify whether propofol administration during thoracic or lumbar epidural anaesthesia intensifies the haemodynamic depression associated with epidural anaesthesia.
Methods
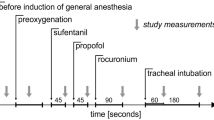
Patients (n = 45) undergoing procedures of similar magnitude were randomly divided into three study groups: a control group (n = 15) receiving general anaesthesia alone and two study groups undergoing thoracic (n = 15) and lumbar epidural anaesthesia (n = 15) before induction of general anaesthesia. All patients received 2 mg·kg−1 propofol at a rate of 200 mg·min−1, followed by a continuous infusion of 4 mg·kg−1·hr−1. Mean arterial blood pressure (MAP) and heart rate (HR) were measured at baseline, three minutes after induction, and one minute after tracheal intubation in all three groups and at 20 min after epidural anaesthesia was established in the thoracic and lumbar groups.
Results
Following epidural anaesthesia, MAP decreased from 94 ± 14 (SD) at baseline to 75 ± 11 mmHg (P < 0.0001) in the thoracic group and from 92 ± 12 to 83 ± 15 mmHg in the lumbar group. After propofol administration, MAP decreased further in the thoracic group to 63 ± 9 mmHg (P = 0.0077) and to 67 ± 10 mmHg (P = 0.0076) in the lumbar group. The MAP following propofol induction in the thoracic group (P < 0.0001) and in the lumbar group (P = 0.0001) was lower than MAP in the control group (81 ± 9 mmHg). HR decreased only in response to thoracic epidural anaesthesia (P = 0.0066).
Conclusion
The hypotensive effects of propofol are additive to those of epidural anaesthesia, resulting in a profound decrease in mean arterial pressure.
Résumé
Objectif
Déterminer si l’administration de propofol pendant une anesthésie péridurale thoracique ou lombaire intensifie la dépression hémodynamique associée à l’anesthésie péridurale.
Méthode
Des patients (n = 45) devant subir des interventions d’importance similaire ont été répartis au hasard en trois groupes : un groupe témoin (n = 15) qui a reçu seulement une anesthésie générale et deux groupes d’étude devant subir une anesthésie péridurale thoracique (n = 15) et lombaire (n = 15) avant l’induction de l’anesthésie générale. Tous les patients ont reçu 2 mg·kg−1 de propofol à 200 mg·min−1, suivi d’une perfusion continue de 4 mg·kg−1·hr−1. La tension artérielle moyenne (TAM) et la fréquence cardiaque (FC) ont fait l’objet de mesures de base, trois minutes après l’induction, et une minute après l’intubation endotrachéale chez tous les patients, de même que 20 min après que l’anesthésie péridurale thoracique et lombaire a été établie dans les deux groupes concernés.
Résultats
À la suite de l’anesthésie péridurale, la TAM de base a diminué pour passer de 94 ± 14 (SD) à 75 ± 11 mmHg (P < 0,0001) chez les patients du groupe d’anesthésie thoracique, et de 92 ± 12 à 83 ± 15 mmHg chez les patients qui ont reçu l’anesthésie lombaire. Après l’administration de propofol, la TAM a diminué encore à 63 ± 9 mmHg dans le groupe thoracique (P = 0,0077) et à 67 ± 10 mmHg (P = 0,0076) dans le groupe lombaire. La TAM, à la suite de l’induction au propofol, était plus basse dans les deux groupes d’étude thoracique (P < 0,0001) et lombaire (P = 0,0001) que la TAM du groupe témoin (81 ± 9 mmHg). La FC a diminué seulement en réaction à l’anesthésie péridurale thoracique (P = 0,0066).
Conclusion
Les effets hypotenseurs du propofol s’ajoutent à ceux de l’anesthésie péridurale, ce qui a comme résultat de diminuer la tension artérielle moyenne de façon importante.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Taniguchi M, Kasaba T, Takasaki M. Epidural anesthesia enhances sympathetic nerve activity in the unanesthetized segments in cats. Anesth Analg 1997; 84: 391–7.
Sellgren J, Pontén J, Wallin BG. Percutaneous recording of muscle nerve sympathetic activity during propofol, nitrous oxide, and isoflurane anesthesia in humans. Anesthesiology 1990; 73: 20–7.
Pagel PS, Warltier DC. Negative isotrophic effects of propofol as evaluated by the regional preload recruitable stroke work relationship in chronically instrumented dogs. Anesthesiology 1993; 78: 100–8.
Robinson BJ, Ebert TJ, O’Brien TJ, Colinco MD, et al. Mechanisms whereby propofol mediates peripheral vasodilation in humans. Anesthesiology 1991; 86: 64–72.
Goodchild CS, Serrao JM. Cardiovascular effects of propofol in the anaesthetized dog. Br J Anaesth 1989; 63: 87–92.
Smith I, Monk TG, White PF, Ding Y. Propofol infusion during regional anesthesia: sedative, amnestic, and anxiolytic properties. Anesth Analg 1994; 79: 313–9.
Wilson E, David A, Mackenzie N, Grant IS. Sedation during spinal anaesthesia: comparison of propofol and midazolam. Br J Anaesth 1990; 64: 48–52.
Fanard L, Van Steenberge A, Demeire, van der Puyl F. Comparison between propofol and midazolam as sedative agents for surgery under regional anaesthesia. Anaesthesia 1988; 43(Suppl): 87–9.
Luchetti M, Palomba R, Sica G, Massa G, et al. Effectiveness and safety of combined epidural and general anesthesia for laparoscopic cholecystectomy. Reg Anesth 1996; 21: 465–9.
Jessop E, Grounds RM, Morgan M, Lumley J. Comparison of infusions of propofol and methohexitone to provide light general anaesthesia during surgery with regional blockade. Br J Anaesth 1985; 57: 1173–7.
McCrae AF, Wildsmith JAW. Prevention and treatment of hypotension during central neural block. Br J Anaesth 1993; 70: 672–80.
Lewis M, Thomas P, Wilkes RG. Hypotension during epidural analgesia for Caesarean section. Anaesthesia 1983; 38: 250–3.
Coates DP, Monk CR, Prys-Roberts C, Turtle M. Hemodynamic effects of infusions of the emulsion formulation of propofol during nitrous oxide anesthesia in humans. Anesth Analg 1987; 66: 64–70.
Rolly G, Versichelen L, Huyghe L, Mungroop. Effect of speed of injection on induction of anaesthesia using propofol. Br J Anaesth 1985; 57: 743–6.
Kirkpatrick T, Cockshott ID, Douglas EJ, Nimmo WE. Pharmacokinetics of propofol (diprivan) in elderly patients. Br J Anaesth 1988; 60: 146–50.
Gepts E, Camu F, Cockshott ID, Douglas EJ. Disposition of propofol administered as constant rate intravenous infusions in humans. Anesth Analg 1987; 66: 1256–63.
Vermeyen KM, Erpels FA, Janssen LA, Beeckman CP, et al. Propofol-fentanyl anaesthesia for coronary bypass surgery in patients with good left ventricular function. Br J Anaesth 1987; 59: 1115–20.
Roekaerts PMHJ, Huygen FJPM, de Lange S. Infusion of propofol versus midazolam for sedation in the intensive care unit following coronary artery surgery. J Cardiothorac Vasc Anesth 1993; 7: 142–7.
Cullen PM, Turtle M, Prys-Roberts C, Way WL, Dye J. Effect of propofol anesthesia on baroreflex activity in humans. Anesth Analg 1987; 66: 1115–20.
Ebert TJ, Muzi M, Berens R, Goff D, Kampine JP. Sympathetic responses to induction of anesthesia in humans with propofol of etomidate. Anesthesiology 1992; 76: 725–33.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Kasaba, T., Kondou, O., Yoshimura, Y. et al. Haemodynamic effects of induction of general anaesthesia with propofol during epidural anaesthesia. Can J Anaesth 45, 1061–1065 (1998). https://doi.org/10.1007/BF03012392
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03012392