Abstract
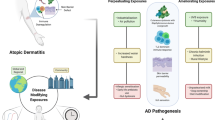
Atopic dermatitis is a chronic inflammatory skin condition including severe pruritus, xerosis, visible eczematous skin lesions that mainly begin early in life. Atopic dermatitis exerts a profound impact on the quality of life of patients and their families. The estimated lifetime prevalence of atopic dermatitis has increased 2~3 fold during over the past 30 years, especially in urban areas in industrialized countries, emphasizing the importance of life-style and environment in the pathogenesis of atopic diseases. While the interplay of individual genetic predisposition and environmental factors contribute to the development of atopic dermatitis, the recent increase in the prevalence of atopic dermatitis might be attributed to increased exposure to various environmental factors rather than alterations in human genome. In recent decades, there has been an increasing exposure to chemicals from a variety of sources. In this study, the effects of various environmental chemicals we face in everyday life - air pollutants, contact allergens and skin irritants, ingredients in cosmetics and personal care products, and food additives - on the prevalence and severity of atopic dermatitis are reviewed.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Simpson, E.L. and Hanifin, J.M. (2006) Atopic dermatitis. Med. Clin. North Am., 90, 149–167.
Kay, J., Gawkrodger, D.J., Mortimer, M.J. and Jaron, A.G. (1994) The prevalence of childhood atopic eczema in a general population. J. Am. Acad. Dermatol., 30, 35–39.
Williams, H.C. (2000) Epidemiology of atopic dermatitis. Clin. Exp. Dermatol., 25, 522–529.
Herd, R.M., Tidman, M.J., Prescott, R.J. and Hunter, J.A. (1996) Prevalence of atopic eczema in the community: the Lothian Atopic Dermatitis study. Br. J. Dermatol., 135, 18–19.
Tanei, R. (2009) Atopic dermatitis in the elderly. Inflammation Allergy Drug Targets, 8, 398–404.
Tanei, R. and Katsuoka, K. (2008) Clinical analyses of atopic dermatitis in the aged. J. Dermatol., 35, 562–569.
Williams, H.C., Burney, P.G., Hay, R.J., Archer, C.B., Shipley, M.J., Hunter, J.J., Bingham, E.A., Finlay, A.Y., Pembroke, A.C. and Graham-Brown, R.A. et al. (1994) The U.K. Working Party’s Diagnostic Criteria for Atopic Dermatitis. I. Derivation of a minimum set of discriminators for atopic dermatitis. Br. J. Dermatol., 131, 383–396.
Lewis-Jones, M.S. and Finlay, A.Y. (1995) The children’s Dermatology Life Quality Index (CDLQI): initial validation and practical use. Br. J. Dermatol., 132, 942–949.
Lewis-Jones, S. (2001) Atopic dermatitis in childhood. Hosp. Med., 62, 136–143.
Fivenson, D., Arnold, R.J., Kaniecki, D.J., Cohen, J.L., Frech, F. and Finlay, A.Y. (2002) The effect of atopic dermatitis on total burden of illness and quality of life on adults and children in a large managed care organization. J. Manag. Care Pharm., 8, 333–342.
Leung, D.Y. and Bieber, T. (2003) Atopic dermatitis. Lancet, 361, 151–160.
Williams, H.C. (2000) Epidemiology of atopic dermatitis. Clin. Exp. Dermatol., 25, 522–529.
Williams, H., Stewart, A., von Mutius, E., Cookson, W. and Anderson, H.R. (2008) Is eczema really on the increase worldwide? J. Allergy Clin. Immunol., 121, 947#x2013;954.
Strachan, D.P. (1989) Hay fever, hygiene, and household size. BMJ, 299, 1259–1260.
Akdis, C.A., Akdis, M., Bieber, T., Bindslev-Jensen, C., Boguniewicz, M., Eigenmann, P., Hamid, Q., Kapp, A., Leung, D.Y., Lipozencic, J., Luger, T.A., Muraro, A., Novak, N., Platts-Mills, T.A., Rosenwasser, L., Scheynius, A., Simons, F.E., Spergel, J., Turjanmaa, K., Wahn, U., Weidinger, S., Werfel, T. and Zuberbier, T. (2006) Diagnosis and treatment of atopic dermatitis in children and adults: European Academy of Allergology and Clinical Immunology/American Academy of Allergy, Asthma and Immunology/PRACTALL Consensus Report. J. Allergy Clin. Immunol., 118, 152–169.
Novak, N. and Simon, D. (2011) Atopic dermatitis - from new pathophysiologic insights to individualzed therapy. Allergy, 66, 830–839.
Suárez-Fariñas, M., Tintle, S.J., Shemer, A., Chiricozzi, A., Nograles, K., Cardinale, I., Duan, S., Bowcock, A.M., Krueger, J.G. and Guttman-Yassky, E. (2011) Nonlesional atopic dermatitis skin is characterized by broad terminal differentiation defects and variable immune abnormalities. J Allergy Clin. Immunol., 127, 954–964.
Eyerich, K. and Novak, N. (2013) Immunology of atopic eczema: overcoming the Th1/Th2 paradigm. Allergy, 68, 974–982.
Pastar, Z., Lipozencić, J. and Ljubojević, S. (2005) Etiopathogenesis of atopic dermatitis-an overview. Acta Dermatovenerol. Croat., 13, 54–62.
Bonness, S. and Bieber, T. (2007) Molecular basis of atopic dermatitis. Curr. Opin. Allergy Clin. Immunol., 7, 382–386.
Ober, C. and Yao, T.C. (2011) The genetics of asthma and allergic disease: a 21st century perspective. Immunol. Rev., 242, 10–30.
Lawson, V., Lewis-Jones, M.S., Finlay, A.Y., Reid, P. and Owens, R.G. (1998) The family impact of childhood atopic dermatitis: the Dermatitis Family Impact Questionnaire. Br. J. Dermatol., 138, 107–113.
Renz, H., Conrad, M., Brand, S., Teich, R., Garn, H. and Pfefferle, P.I. (2011) Allergicdiseases, gene-environment interactions. Allergy, 66 Suppl 95, 10–12.
McFadden, J.P., White, J.M., Basketter, D.A. and Kimber, I. (2009) Does hapten exposure predispose to atopic disease? The hapten-atopy hypothesis. Trends Immunol., 30, 67–74.
McFadden, J.P., Dearman, R.J., White, J.M., Basketter, D.A. and Kimber, I. (2011) The Hapten-Atopy hypothesis II: the ‘cutaneous hapten paradox’. Clin. Exp. Allergy, 41, 327–337.
McFadden, J.P., Basketter, D.A., Dearman, R.J., Puangpet, P. and Kimber, I. (2014) Hapten-chemicalatopy hypothesis III: the potential role of airborne chemicals. Br. J. Dermatol., 170, 45–51.
Drasch, G., Schupp, I., Höfl, H., Reinke, R. and Roider, G. (1994) Mercury burden of human fetal and infant tissues. Eur. J. Pediatr., 153, 607–610.
Jung, K.H., Hsu, S.I., Yan, B., Moors, K., Chillrud, S.N., Ross, J., Wang, S., Perzanowski, M.S., Kinney, P.L., Whyatt, R.M., Perera, F.P. and Miller, R.L. (2012) Childhood exposure to fine particulate matter and black carbon and the development of new wheeze between ages 5 and 7 In an urban prospective cohort. Environ. Int., 45, 44–50.
Spira-Cohen, A., Chen, L.C., Kendall, M., Lall, R. and Thurston, G.D. (2011) Personal exposures to traffic-related air pollution and acute respiratory health among Bronx schoolchildren with asthma. Environ. Health Perspect., 119, 559–565.
Silverman, R.A. and Ito, K. (2010) Age-related association of fine particles and ozone with severe acute asthma in New York City. J. Allergy Clin. Immunol., 125, 367–373.
Montnemery, P., Nihlén, U., Göran Löfdahl, C., Nyberg, P. and Svensson, A. (2003) Prevalence of self-reported eczema in relation to living environment, socio-economic status and respiratory symptoms assessed in a questionnaire study. BMC Dermatol., 3, 4.
Pénard-Morand, C., Raherison, C., Charpin, D., Kopferschmitt, C., Lavaud, F., Caillaud, D. and Annesi-Maesano, I. (2010) Long-term exposure to close-proximity air pollution and asthma and allergies in urban children. Eur. Respir. J., 36, 33–40.
Lee, Y.L., Su, H.J., Sheu, H.M., Yu, H.S. and Guo, Y.L. (2008) Traffic-related air pollution, climate, and prevalence of eczema in Taiwanese school children. J. Invest. Dermatol., 128, 2412–2420.
Morgenstern, V., Zutavern, A., Cyrys, J., Brockow, I., Koletzko, S., Krämer, U., Behrendt, H., Herbarth, O., von Berg, A., Bauer, C.P., Wichmann, H.E. and Heinrich, J. (2008) Atopic diseases, allergic sensitization, and exposure to trafficrelated air pollution in children. Am. J. Respir. Crit. Care Med., 177, 1331–1337.
Jedrychowski, W., Perera, F., Maugeri, U., Mrozek-Budzyn, D., Miller, R.L., Flak, E., Mroz, E., Jacek, R. and Spengler, J.D. (2011) Effects of prenatal and perinatal exposure to fine air pollutants and maternal fish consumption on the occurrence of infantile eczema. Int. Arch. Allergy Immunol., 155, 275–281.
Just, A.C., Whyatt, R.M., Perzanowski, M.S., Calafat, A.M., Perera, F.P., Goldstein, I.F., Chen, Q., Rundle, A.G. and Miller, R.L. (2012) Prenatal exposure to butylbenzyl phthalate and early eczema in an urban cohort. Environ. Health Perspect., 120, 1475–1480.
Kim, J., Kim, E.H., Oh, I., Jung, K., Han, Y., Cheong, H.K. and Ahn, K. (2013) Symptoms of atopic dermatitis are influenced by outdoor air pollution. J. Allergy Clin. Immunol., 132, 495–498.
Song, S., Lee, K., Lee, Y.M., Lee, J.H., Lee, S.I., Yu, S.D. and Paek, D. (2011) Acute health effects of urban fine and ultrafine particles on children with atopic dermatitis. Environ. Res., 111, 394–399.
Triggiani, M., Loffredo, S., Granata, F., Staiano, R.I. and Marone, G. (2011) Modulation of mast cell and basophil functions by benzene metabolites. Curr. Pharm. Des., 17, 3830–3835.
Lehmann, I., Rehwagen, M., Diez, U., Seiffart, A., Rolle-Kampczyk, U., Richter, M., Wetzig, H., Borte, M. and Herbarth, O. (2001) Enhanced in vivo IgE production and T cell polarization toward the type 2 phenotype in association with indoor exposure to VOC: results of the LARS study. Int. J. Hyg. Environ. Health, 204, 211–221.
Gillis, B., Gavin, I.M., Arbieva, Z., King, S.T., Jayaraman, S. and Prabhakar, B.S. (2007) Identification of human cell responses to benzene and benzene metabolites. Genomics, 90, 324–333.
Eberlein-Konig, B., Przybilla, B., Kuhnl, P., Pechak, J., Gebefugi, I., Kleinschmidt, J. and Ring, J. (1998) Influence of airborne nitrogen dioxide or formaldehyde on parameters of skin function and cellular activation in patients with atopic eczema and control subjects. J. Allergy Clin. Immunol., 101, 141–143.
Huss-Marp, J., Eberlein-König, B., Breuer, K., Mair, S., Ansel, A., Darsow, U., Krämer, U., Mayer, E., Ring, J. and Behrendt, H. (2006) Influence of short-term exposure to airborne Der p 1 and volatile organic compounds on skin barrier function and dermal blood flow in patients with atopic eczema and healthy individuals. Clin. Exp. Allergy, 36, 338–345.
Herbarth, O., Fritz, G.J., Rehwagen, M., Richter, M., Roder, S. and Schlink, U. (2006) Association between indoor renovation activities and eczema in early childhood. Int. J. Hyg. Environ. Health, 209, 241–247.
Lee, J.H., Suh, J., Kim, E.H., Cho, J.B., Park, H.Y., Kim, J., Ahn, K., Cheong, H.K. and Lee, S.I. (2012) Surveillance of home environment in children with atopic dermatitis: a questionnaire survey. Asian Pac. Allergy, 2, 59–66.
Lee, J.Y., Seo, J.H., Kwon, J.W., Yu, J., Kim, B.J., Lee, S.Y., Kim, H.B., Kim, W.K., Kim, K.W., Shin, Y.J. and Hong, S.J. (2012) Exposure to gene-environment interactions before 1 year of age may favor the development of atopic dermatitis. Int. Arch. Allergy Immunol., 157, 363–371.
Bornehag, C.G., Sundell, J., Weschler, C.J., Sigsgaard, T., Lundgren, B., Hasselgren, M. and Hägerhed-Engman, L. (2004) The association between asthma and allergic symptoms in children and phthalates in house dust: a nested case-control study. Environ. Health Perspect., 112, 1393–1397.
Herberth, G., Bauer, M., Gasch, M., Hinz, D., Röder, S., Olek, S., Kohajda, T., Rolle-Kampczyk, U., von Bergen, M., Sack, U., Borte, M. and Lehmann, I. (2014) Maternal and cord blood miR-223 expression associates with prenatal tobacco smoke exposure and low regulatory T-cell numbers. J. Allergy Clin. Immunol., 133, 543–550.
Hinz, D., Bauer, M., Röder, S., Olek, S., Huehn, J., Sack, U., Borte, M., Simon, J.C., Lehmann, I. and Herberth, G. (2012) Cord blood Tregs with stable FOXP3 expression are influenced by prenatal environment and associated with atopic dermatitis at the age of one year. Allergy, 67, 380–389.
Lehmann, I., Thoelke, A., Rehwagen, M., Rolle-Kampczyk., U, Schlink, U., Schulz, R., Borte, M., Diez, U. and Herbarth, O. (2002) The influence of maternal exposure to volatile organic compounds on the cytokine secretion profile of neonatal T cells. Environ. Toxicol., 17, 203–210.
Wang, I.J., Chen, S.L., Lu, T.P., Chuang, E.Y. and Chen, P.C. (2013) Prenatal smoke exposure, DNA methylation, and childhood atopic dermatitis. Clin. Exp. Allergy, 43, 535–543.
Wang, I.J., Guo, Y.L., Lin, T.J., Chen, P.C. and Wu, Y.N. (2010) GSTM1, GSTP1, prenatal smoke exposure, and atopic dermatitis. Ann. Allergy Asthma Immunol., 105, 124–129.
Yi, O., Kwon, H.J., Kim, H., Ha, M., Hong. S.J., Hong, Y.C., Leem, J.H., Sakong, J., Lee, C.G., Kim, S.Y. and Kang, D. (2012) Effect of environmental tobacco smoke on atopic dermatitis among children in Korea. Environ. Res., 113, 40–45.
Jedrychowski, W., Perera, F., Maugeri, U., Mrozek-Budzyn, D., Miller, R.L., Flak, E., Mroz, E., Jacek, R. and Spengler, J.D. (2011) Effects of prenatal and perinatal exposure to fine air pollutants and maternal fish consumption on the occurrence of infantile eczema. Int. Arch. Allergy Immunol., 155, 275–281.
Herr, C.E., Dostal, M., Ghosh, R., Ashwood, P., Lipsett, M., Pinkerton, K.E., Sram, R. and Hertz-Picciotto, I. (2010) Air pollution exposure during critical time periods in gestation and alterations in cord blood lymphocyte distribution: a cohort of livebirths. Environ. Health, 9, 46.
Dong, G.H., Chen, T., Liu, M.M., Wang, D., Ma, Y.N., Ren, W.H., Lee, Y.L., Zhao, Y.D. and He, Q.C. (2011) Gender differences and effect of air pollution on asthma in children with and without allergic predisposition: northeast Chinese children health study. PLoS One, 6, e22470.
Takenaka, H., Zhang, K., Diaz-Sanchez, D., Tsien, A. and Saxon, A. (1995) Enhanced human IgE production results from exposure to the aromatic hydrocarbons from diesel exhaust: direct effects on B-cell IgE production. J. Allergy Clin. Immunol., 95, 103–115.
Inoue, K.I., Takano, H., Yanagisawa, R., Sakurai, M., Abe, S., Yoshino, S., Yamaki, K. and Yoshikawa, T. (2007) Effects of components derived from diesel exhaust particles on lung physiology related to antigen. Immunopharmacol. Immunotoxicol., 29, 403–412.
Martin, S.F. (2012) Contact dermatitis: from pathomechanisms to immunotoxicology. Exp. Dermatol., 21, 382–389.
Thyssen, J.P., Linneberg, A., Menné, T. and Johansen, J.D. (2007) The epidemiology ofcontact allergy in general population – prevalence and main findings. Contact Dermatitis, 57, 287–299.
Basko-Plluska, J.L., Thyssen, J.P. and Schalock, P.C. (2011) Cutaneous and systemic hypersensitivity reactions to metallic implants. Dermatitis, 22, 65–79.
Koller, L.D. (1980) Immunotoxicology of heavy metals. Int. J. Immunopharmacol., 2, 269–279.
Costa, M., Cantoni, O., de Mars, M. and Swartzendruber, D.E. (1982) Toxic metal produce an S-phase-specific cell cycle block. Res. Commun. Chem. Pathol. Pharmacol., 38, 405–419.
Kieć-Świerczyńska, M., Kręcisz, B., Chomiczewska, D. and Sobala, W. (2012) Trends inallergy to the 10 most frequent contact allergens in patients examinedat the Nofer Institute, Lodz, Poland in 1996–2009. Post. Dermatol. Alergol., 1, 19–24.
Garg, S., McDonagh, A.J. and Gawkrodger, D.J. (2009) Age-and sex-relatedvariations in allergic contact dermatitis to common allergens. Contact Dermatitis, 61, 46–47.
Friberg, L., Kullman, L., Lind, B. and Nylander, M. (1986) Mercury in the central nervous system in relation to amalgam fillings. Lakartidringen, 83, 519–522.
Nylander, M. (1986) Mercury in pituitary glands of dentists. Lancet, 1, 442.
Glomski, C.A., Brody, H. and Pillay, S.K. (1971) Distribution and concentration of mercury in autopsy specimens of human brain. Nature, 232, 200–201.
Klimańska, M., Żmudzińska, M., Jenerowicz, D. and Czarnecka-Operacz, M. (2011) The importance of exposure to contact allergens in patients withallergic contact dermatitis. Post. Dermatol. Alergol., 3, 203–211.
Ortiz, K.J. and Yiannias, J.A. (2004) Contact dermatitis to cosmetics, fragrances, and botanicals. Dermatol. Ther., 17, 264–271.
Kind, F., Scherer, K. and Bircher, A.J. (2012) Contact dermatitis to paraphenylenediaminein hair dye following sensitiza-tion to black hennatattoos – an ongoing problem. J. Dtsch. Dermatol. Ges., 10, 572–578.
Yim, E., Baquerizo Nole, K.L. and Tosti, A. (2014) Contact dermatitis caused by preservatives. Dermatitis, 25, 215–231.
Lever, R. (2001) The role of food in atopic eczema. J. Am. Acad. Dermatol., 45(Suppl 1), S57–60.
Lack, G. (2008) Clinical practice. Food allergy. N Engl. J. Med., 359, 1252–1260.
Hanifin, J.M. (1997) Critical evaluation of food and mite allergy in the management of atopic dermatitis. J. Dermatol., 24, 495–503.
Worth, A. and Sheikh, A. (2010) Food allergy and atopic eczema. Curr. Opin. Allergy Clin. Immunol., 10, 226–230.
Bjorkstén, B. (2005) Genetic and environmental risk factors for the development of food allergy. Curr. Opin. Allergy Clin. Immunol., 5, 249–253.
Rosińska-Więckowicz, A. and Czarnecka-Operacz, M. (2011) Disease extentand severity in patients with atopic dermatitis and food allergy. Post. Dermatol. Alergol., 5, 382–388.
Zaknun, D., Schroecksnadel, S., Kurz, K. and Fuchs, D. (2012) Potential role ofantioxidant food supplements, preser-vatives and colorants in thepathogenesis of allergy and asthma. Int. Arch. Allergy Immunol., 157, 113–124.
Young, E., Patel, S., Stoneham, M., Rona, R. and Wilkinson, J.D. (1987) The prevalence of reaction to food additives in a survey population. J. R. Coll. Physicians Lond., 21, 241–247.
Fuglsang, G., Madsen, C., Saval, P. and Osterballe, O. (1993) Prevalence of intolerance to food additives among Danish school children. Pediatr. Allergy Immunol., 4, 123#x2013;129.
Fuglsang, G., Madsen, G., Halken, S., Jørgensen, S., Ostergaard, P.A. and Osterballe, O. (1994) Adverse reactions to food additives in children with atopic symptoms. Allergy, 49, 31–37.
Park, H.W., Park, C.H., Park, S.H., Park, J.Y., Park, H.S., Yang, H.J., Ahn, K.M., Kim, K.H., Oh, J.W., Kim, K.E., Pyun, B.Y., Lee, H.B. and Min, K.U. (2008) Dermatologic adverse reactions to 7 common food additives in patients with allergic diseases: a double-blind, placebo-controlled study. J. Allergy Clin. Immunol., 121, 1059–1061.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
This is an Open-Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Kim, K. Influences of Environmental Chemicals on Atopic Dermatitis. Toxicol Res. 31, 89–96 (2015). https://doi.org/10.5487/TR.2015.31.2.089
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.5487/TR.2015.31.2.089