Abstract
Objectives
The objective of this article is to document patterns and trends of in-hospital mental health service use by First Nations (FN) living in rural and remote communities in the province of Manitoba.
Methods
Our sample included all Manitoba residents eligible under the Manitoba Health Services Insurance Plan living on FN reserves and those living in rural and remote communities from 1986 to 2014. Using administrative claims data, we developed multi-level models that describe hospitalization for mental health conditions shown responsive to primary healthcare interventions. We aggregated the results by First Nation Tribal Councils and remoteness to derive rates of hospitalization episodes, length of stay and readmission rates.
Results
Rates of hospitalization for mental health are increasing for FN males and females. This is particularly evident for those affiliated with the Island Lake and Keewatin Tribal Councils. The length of stay has increased. Changes in rates of readmissions were not statistically significant. FNs are admitted for mental health conditions at a younger age when compared with other Manitobans, and trends show that the FNs’ average age at admission is decreasing.
Conclusions
Our results raise serious concerns about the responsiveness of community-based mental health services for FNs in Manitoba, because of both increasing rates of episodes of hospitalization and decreasing age of admission. Given the documented lack of mental health services accessible on-reserve, levels of social distress associated with a history of oppressive policies, and continued lack of infrastructure, current trends are alarming.
Résumé
Objectifs
L’objectif de cet article est de documenter les caractéristiques et les tendances de l’utilisation des services de santé mentale en milieu hospitalier par les Premières nations (PN) vivant dans les collectivités rurales et éloignées de la province du Manitoba.
Méthodes
Notre échantillon inclus tous les résidents du Manitoba admissibles au Régime d’assurance-maladie du Manitoba vivant dans les réserves des PN et ceux vivant dans des collectivités rurales et éloignées de 1986 à 2014. À partir de données de réclamations administratives, nous avons mis au point des modèles à plusieurs niveaux décrivant l’hospitalisation pour des problèmes de santé mentale qui se sont montrés sensibles aux interventions en soins de santé primaires. Nous avons agrégé les résultats par Conseil de Tribu pour obtenir les taux d’épisodes d’hospitalisation, la durée du séjour et les taux de réadmission.
Résultats
Les taux d’hospitalisation liée à la santé mentale augmentent pour les hommes et femmes PN. Cela est particulièrement évident pour les membres des conseils tribaux d’Island Lake et de Keewatin. La durée du séjour a aussi augmenté. Les changements dans les taux de réadmission n’étaient pas statistiquement significatifs. Les PNs sont admis pour des problèmes de santé mentale plus jeunes que les autres Manitobains, et les tendances montrent que l’âge moyen des PNs continue de décroître.
Conclusions
Nos résultats soulèvent des inquiétudes quant à la réactivité des services de santé mentale communautaires pour les PNs au Manitoba, à la fois en raison de la fréquence croissante des épisodes d’hospitalisation et de la diminution de l’âge d’admission. Étant donné le manque documenté de services de santé mentale accessibles dans les réserves, le niveau de détresse sociale associé à des antécédents de politiques oppressives et le manque continu d’infrastructure, les tendances actuelles sont alarmantes.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Decades of oppressive policies and legislation have significantly harmed First Nation peoples in Canada (Bombay 2015). This is reflected in their high rates of suicide (Pollock et al. 2018), depression and anxiety (Firestone et al. 2015; Kirmayer et al. 2000) as compared with other Canadians. Residential schools, specifically, had devastating impacts on survivors, with a significant proportion of attendees having reported experiencing or witnessing emotional, verbal or physical abuse, isolation from family, harsh discipline, and loss of cultural identity and language (Loppie Reading and Wien 2009). Attendance at residential school impacted not only attendees: having a parent or grandparent attend residential school has been associated with higher rates of suicidal ideation and attempted suicides (Elias et al. 2012). The multigenerational impact of these harms and the transmission of negative physical, social, psychological, cultural and economic consequences on subsequent generations is commonly known as historic trauma resulting in unresolved grief and various expressions of post-traumatic stress disorders (Wesley-Esquimaux and Smolewski 2004).
As such, the fabric of communities and families has been weakened, and in some cases torn, resulting in higher prevalence of social distress and self-harm (Bombay et al. 2009; McQuaid et al. 2017). Since the mid-1980s, federal programs have been developed for and at times with First Nation peoples who live on reserve. These programs have focused on primary care, maternal and child health, and home care, to name a few. Mental health programming has however been a point of contention, with repeated calls by First Nations for improving access to culturally safe care (Boksa et al. 2015; Royal Commission on Aboriginal Peoples 1996; Truth and Reconciliation Commission of Canada 2015).
The now-defunct Aboriginal Healing Foundation (1998– 2014) generated important literature on mental health care needs and possibilities for the development of more effective treatment modalities (Aboriginal Healing Foundation 2014), yet its impact on federal programming is difficult to detect. To date, federal mental health programming on-reserve remains limited to a patchwork of relatively small primary and secondary prevention programs (Brighter Futures, Building Healthy Communities, the National Aboriginal Youth Suicide Prevention Strategy, Health Canada First Nations and Inuit Health Branch 2012), a long-standing community-based program focused on addictions prevention and referral to treatment services (the National Native Alcohol and Drug Prevention Program) and the individual-focused Non-Insured Health Services which funds a maximum of twelve consults for individuals in need to access care: care can only be accessed from a federally approved therapist or counsellor. Traditional modalities and providers are not included. When communities face a crisis (a series of suicides for example), they may be extended access to a Short-Term Crisis Intervention Mental Health Counselling (Health Canada First Nations and Inuit Health Branch 2015) for a few days. In Manitoba, this service has been contracted out by the federal government to a single First Nation organization, without prior consultations. This change has yet to be evaluated. First Nations who temporarily or permanently live off-reserve and who retain a relationship with their First Nation community might come home to access some of these services, which are not accessible off-reserve.
First Nation individuals requiring more advanced care may access psychiatric care provided on an out-patient or in-patient basis, at no cost. These services, which are provincially funded, can be accessed through a referral from a primary care provider. In some cases, when individuals are thought at risk of self-harm or of harming others, hospitalization for emergency mental health services is also possible.
The objective of this article is to document patterns of in-hospital mental health service use by First Nations in Manitoba. We focus on selected mental health conditions, namely schizophrenic disorders, paranoid conditions and major depression, which have been shown to be responsive to community-based interventions, when available. These types of conditions are known as Ambulatory Care Sensitive Conditions (ACSC). While mental health is often not included in definitions of primary healthcare, the First Nations communities we worked with on this project have clearly stated that they consider mental health to be an integral component of their definition of primary healthcare (Kyoon-Achan et al. 2018a; Kyoon-Achan et al. 2018b).
Methods
Partnership
This study is part of a larger partnership-based program of research under the project name Innovation Supporting Transformation in Community-based Primary Healthcare Research Project in Manitoba First Nation and rural/remote communities (iPHIT), between researchers from The First Nations Health and Social Secretariat of Manitoba (FNHSSM, formed by a resolution of the Assembly of Manitoba Chiefs in 2014), the University of Manitoba Departments of Community Health Sciences and Family Medicine, and 8 Manitoba First Nation communities. The collaboration and methods of working together with our partners have been detailed in another publication (Kyoon-Achan et al. 2018). It is important to note that all partners, including representatives from the 8 First Nations, were involved in defining all research priorities, including the focus on mental health, which was the salient concern in all discussions. Results were discussed in multiple meetings with FNHSSM and university-based researchers, as well as with our eight First Nation community partners, to elicit context, deepen interpretation, ensure uptake of results by communities to support innovation, and explore solutions. Partners were involved in the interpretation and approved this publication. Ethical approval was received from the University of Manitoba Health Research Ethics Board. Approval for data access was received from the Government of Manitoba Health Information Privacy Committee and the Manitoba First Nations Health Information Research Governance Committee.
Design
In this study, we conceptualize that disproportionate rates of hospitalizations for conditions that could be managed at the community level if services were available, are an indication of a barrier to accessing needed services (Lavoie et al. 2010; Lavoie et al. 2019). We are using hospitalizations for selected mental health conditions (schizophrenic disorders, paranoid conditions and major depressions) as a proxy for access to effective out-patient (and thus primary healthcare-based) mental health services.
Data source
We used administrative health data (1986–2014) from the Manitoba Population Research Data Repository housed at the Manitoba Centre for Health Policy (MCHP), University of Manitoba. The repository is a comprehensive collection of administrative, registry, survey and other data that include the vast majority of residents of Manitoba, including residents of First Nations’ communities. The datasets we used included vital statistics; the population health registry file for the provincial insured population; the hospital discharge abstracts; and census data. The study encompassed all Manitoba residents aged 0 to 74 years of age eligible to receive health benefits under the Manitoba Health Services Insurance Plan, including those living on Manitoba’s 63 First Nation reserves.
Sample
We defined First Nation communities as those recognized as Indian Reserves under the Indian Act (Indigenous and Northern Affairs Canada 2017). While narrow, we justify using this definition because we are concerned with access to primary health care locally, which is defined by federal policy, and want to report findings in ways that support First Nation innovations at the provincial level. We further broke down findings by Tribal Councils and report findings accordingly to support self-determination in decision-making.
Rural and remote communities are somewhat more difficult to define. There is no single, universally accepted definition of concepts such as rural and remote. Most definitions generally focus on geography, population density or access to services such as healthcare. The “right” definition is context-dependent. For the purpose of this study, we included under the rubric “rural and remote communities” all MB communities with a population of less than 8000 (n = 183), to provide a useful comparator to MB First Nation communities, which each have fewer than 8000 residents. Table 1 provides population size for each category.
Six-digit postal codes were used to identify the population served by each community. Registered members of First Nations represent 96.6% of the overall on-reserve population; others are non-status, Métis or non-Indigenous individuals who depend on the same services. The resulting on-reserve First Nation population varied from 54,999 (1986) to 73,372 (2014) as a result of population growth.
Variables
The main dependent variable for this study was hospitalizations for mental health-related ACSC, which are known to be serious, major, long-term or chronic in other investigations (British Columbia Provincial Health Officer 2009; Caminal et al. 2004; Canadian Institute for Health Information 2007). Four different measures of hospitalization were used:
-
Rates of episodes of hospital care: the number of hospitalization episodes from admission to discharge. Hospitalizations were treated as a single episode when readmission to another hospital occurred within 1 day, to account for transfers from one hospital to another.
-
Rates of length of stay per admission: the average of the number of days in hospital for each episode of care.
-
30-day readmission rates: readmission within 30 days of discharge from the initial admission.
-
Average age of admission across populations.
Analysis
We used generalized estimating equation (GEE) models to analyze our data, controlling for age, sex, and socio-economic status (SES), to identify trends (change over time from 1986 to 2014) and differences in hospitalization rates for ACSC. We present our results in a 5-year rolling average to attenuate yearly variations and instead highlight trends. This is an accepted reporting method when dealing with small sample size.
Results
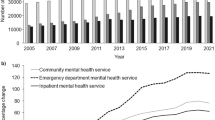
Table 2 and Fig. 1 show that rates of episodes of care for mental health-related ACSC are the highest and increasing for First Nation communities (3.40% change, p < 0.0001). Although we analyzed results for all of Manitoba and for non-reserve small (remote and non-remote) Manitoban communities, results for those communities did not show statistically significant change. For First Nation communities, the increasing trend appears to have begun around 1999. Results for First Nation communities were significantly different from those for all of Manitoba (p = 0.0103).
As Table 3 shows, rates of episodes of care for mental health-related ACSC are increasing at a faster rate for First Nations males (5.81% change between 1986 and 2014) than for First Nation females (2.16% change).
Table 4 shows the rates of episodes of care for mental health-related ACSC across Manitoba’s seven Tribal Councils and other independent (not Tribal Council affiliated) communities, broken down by sex. For First Nation males, rates were found to be increasing across all Tribal Councils and with independent communities, with the exception of those communities affiliated with the Dakota Ojibway Tribal Council. For First Nation females, results also showed increased rates of hospitalization, in the Island Lake Tribal Council, Keewatin Tribal Council, Southeast Resource Development Council and West Region Tribal Council.
As Table 5 and Fig. 2 show, rates of length of stay are slowly increasing for First Nation communities (0.88% change, p = 0.0466). Results for other communities were not statistically significant. Although the length of stay for First Nation communities appears to be shorter than for other communities, the difference was found not to be statistically significant (p = 0.4955).
We analyzed rates of readmission for mental health ACSC to hospital within 30 days of an episode of care. As shown in Table 6, rates of readmission were found to be decreasing and statistically significant only for all of Manitoba (p = 0.01340) and for rural communities that are also remote (p = 0.00). Statistically significant changes could only be detected for Independent First Nation communities (decreasing, 2.71% change, p = 0.00). This may be related to the small sample size and resultant small number of events to analyze.
Finally, we looked for the age at the time of admission for a mental health–related ACSC. Table 7 clearly shows that the age at the time of admission is decreasing (results were statistically significant for all categories of communities) across all communities in Manitoba. The age of admission for First Nation communities was also found to be significantly lower when compared with that for all of Manitoba (p = 0.01).
Discussion
Our study has shown that rates of hospitalization for mental health-related ACSC are increasing for Manitoba First Nations, with the greatest increase being borne by First Nation males. Our results also clearly show that some Tribal Councils are experiencing higher rates of hospitalizations than others. It also appears that the length of hospital stay for First Nations is slowly increasing. Despite this, it remains shorter than for all of Manitoba: these results may simply reflect that the majority of the Manitoba population lives in larger urban environments compared with First Nations. As a matter of practice, Manitoba residents from rural and remote communities, including First Nations, tend to be hospitalized at a lower threshold of acuity than their urban counterparts, simply because the urban population can more readily access specialized care on an out-patient basis than their rural and remote counterparts. Alternatively, these results could suggest a revolving door situation, where needs remain after discharge, leading to readmission. Although we could not detect statistically significant findings when looking at readmission rates for First Nations, this may be due to the small sample size. Additionally, an increase in length of stay for First Nations may signal increased acuity for those hospitalized. First Nation community partners reported noticing such a trend (Kyoon-Achan et al. 2018a; Kyoon-Achan et al. 2018b). While acknowledging these confounders, we also note that the age at the time of hospitalization is decreasing, signaling increased acuity at a younger age. This, along with increased rates of hospitalization for First Nations men, points to a concerning trend.
Our study shows that patterns of hospitalization for mental health ACSC have changed over time. The year 1999 seems to mark a shift, with gradual increases in adjusted rates of hospitalization for mental healthcare. The reasons for this are however unclear. Watson et al. (2005) studied the use of mental health services in Manitoba from 1992 to 2001, but did not report such a shift. Additional research may be required to identify whether this shift is related to new needs, better identification of ongoing needs, simply a shift in how mental health services are provided and used, or other events such as the impact of disclosures of sexual abuse in residential schools (the first public disclosure has been attributed to then Grand Chief of the Assembly of Manitoba Chiefs, Phil Fontaine, in October 1990).
It is important to note that this study has a number of limitations. To begin, the administrative data we accessed do not provide contextual information on physicians’ patterns of referral to in-hospital care for mental health conditions (Roos 1992). Still, there is no reason to expect a systematic bias in referral patterns across communities. As well, our reporting of findings by types of community and by Tribal Councils glosses over differences between communities: administrative data provide limited information on confounders, such as policy events or shifts in hospitalization practices for certain diagnoses, local governance structures and innovative programs. Where such information might be accessible, limitation in terms of sample size would result in findings being undetectable statistically. Occasionally, such differences have been noted and are not reported in publications because First Nation partners do not want potentially stigmatizing findings reported publicly on a per community basis. Another limitation is associated with the design itself: ecologic designs such as the one used in this study highlight associations, but cannot speak to causality (Morgenstern 1995). Last, we did not identify Métis, non-registered First Nations and non-Indigenous peoples living on-reserve. It is however known that approximately 96.6% of the total on-reserve populations are registered First Nations. Others are likely to experience the same patterns of referral when receiving care.
The increased use of hospital admissions to treat First Nations mental health needs raises issues of questionable effectiveness, cultural inappropriateness, poorer responsiveness, and racism (Billie and Smylie 2015; Bourassa et al. 2004; Browne 2017; Browne et al. 2016). Anecdotal evidence suggests that those who are admitted often do not benefit from the treatments provided and are discharged after having been stabilized but showing little progress in terms of managing their condition. The First Nation communities we partnered with suggested that more community-based support would alleviate the need for hospitalization and would be more effective at supporting First Nation individuals who have mental healthcare needs (Kyoon-Achan et al. 2018b). Given the young age at which First Nations are hospitalized for mental health ACSC and gender-based differences, there is a clear need to invest in alternative approaches. Land-based healing and cultural approaches are showing some promise and have been widely identified as effective if designed and delivered by First Nations themselves (Baskin 2016; Dorman et al. 2018). Attention to gender is essential. Here, the legacy of the Aboriginal Healing Foundation (AHF) might offer avenues for community-based interventions. These will however require investments to be realized, as most AHF or other initiatives even when shown to be effective rarely go beyond the stage of a pilot project, because of a lack of sustainable funding for community-based innovations. The lack of political goodwill to support community healing remains the main structural barrier.
Conclusions
Findings from this study show increased rates of hospitalization for mental health conditions, which partners in this study linked to the limited mental health services accessible on-reserve, levels of social distress associated with ongoing oppression through colonization (evidenced by continued decision-making by outsiders), and lack of infrastructure. It is our reflection, which is supported by work reported in other publications (Kyoon-Achan et al. 2018a; Kyoon-Achan et al. 2018b), that mental health conditions might be more effectively treated at the community level through upstream interventions aimed at supporting community members in managing their mental health needs when a crisis develops. The results of our study support the need to invest in innovative approaches in community-based mental health services.
References
Aboriginal Healing Foundation. (2014). Annual report 2009 aboriginal Healing Foundation. Retrieved from Ottawa: http://www.ahf.ca/assets/pdf/english/annual_report_2004.pdf
Baskin, C. (2016). Spirituality: the core of healing and social justice from an indigenous perspective. New Directions for Adult and Continuing Education, 152, 51–60.
Billie, A., & Smylie, J. (2015). First Peoples, second class treatment: the role of racism in the health and well-being of Indigenous peoples in Canada. Retrieved from Toronto:
Boksa, P., Joober, R., & Kirmayer, L. (2015). Mental wellness in Canada's aboriginal communities: Striving toward reconciliation. Journal of Psychiatry and Neuroscience, 40(6), 363–365. https://doi.org/10.1503/jpn.150309.
Bombay, A. (2015). A call to end mental health disparities for indigenous people. Lancet Psychiatry, 2(10), 861–862.
Bombay, A., Matheson, K., & Anisman, H. (2009). Intergenerational trauma: convergence of multiple processes among First Nations peoples in Canada. International Journal of Indigenous Health, 5(3), 6–47.
Bourassa, C., McKay-McNabb, K., & Hampton, M. (2004). Racism, sexism and colonialism: the impact on the health of Aboriginal women in Canada. Canadian Women Studies, 24(1), 23–29.
British Columbia Provincial Health Officer. (2009). Pathways to health and healing – 2nd Report on the Health and Well-being of Aboriginal People in British Columbia. Provincial Health Officer’s Annual Report 2007. Retrieved from Victoria:
Browne, A. J. (2017). Moving beyond description: closing the health equity gap by redressing racism impacting Indigenous populations. Soc Sci Med, 184, 23–26. https://doi.org/10.1016/j.socscimed.2017.04.045.
Browne, A. J., Varcoe, C., Lavoie, J. G., Smye, V. L., Wong, S. T., Krause, M., et al. (2016). Enhancing health care equity with Indigenous populations: evidence-based strategies from an ethnographic study. BMC Health Serv Res, 16(544), 1–17. https://doi.org/10.1186/s12913-016-1707-9.
Caminal, J., Starfield, B., Sánchez, E., Casanova, C., & Morales, M. (2004). The role of primary care in preventing ambulatory care sensitive conditions. The European Journal of Public Health, 14(3), 246–251.
Canadian Institute for Health Information. (2007). Health indicators 2007. Retrieved from Ottawa: http://secure.cihi.ca/cihiweb/dispPage.jsp?cw_page=indicators_definitions_health_system_e
Dorman, K., Biedermann, B., Linklater, C., & Jaffer, Z. (2018). Community strengths in addressing opioid use in northeastern Ontario. Canadian Journal of Public Health, 109(2), 219–222.
Elias, B., Mignone, J., Hall, M., Hong, S. P., Hart, L., & Sareen, J. (2012). Trauma and suicide behaviour histories among a Canadian indigenous population: an empirical exploration of the potential role of Canada's residential school system. Soc Sci Med, 74(10), 1560–1569.
Firestone, M., Smylie, J., Maracle, S., McKnight, C., Spiller, M., & O'Campo, P. (2015). Mental health and substance use in an urban First Nations population in Hamilton, Ontario. Canadian Journal of Public Health, 106(6), e375–e381. https://doi.org/10.17269/cjph.106.4923.
Health Canada First Nations and Inuit Health Branch. (2012). First Nations and Inuit Health Program Compendium 2011/2012. Retrieved from Ottawa: https://www.homelesshub.ca/resource/first-nations-and-inuit-health-program-compendium-20112012.
Health Canada First Nations and Inuit Health Branch. (2015). Non-insured health benefits program short-term crisis intervention mental health Counselling National Benefit Profile. Retrieved from Ottawa: www.afn.ca/uploads/files/.../fnihb_stcimhc_national_benefit_profile_oct_2015.pdf
Indigenous and Northern Affairs Canada. (2017). Reserves/Settlements/Villages. Retrieved from Ottawa: http://fnp-ppn.aandc-aadnc.gc.ca/fnp/main/Definitions.aspx?lang=eng#Reserves/Settlements/Villages
Kirmayer, L. J., Brass, G. M., & Tait, C. L. (2000). The mental health of Aboriginal peoples: transformations of identity and community. Can J Psychiatr, 45(7), 607–616. https://doi.org/10.1177/070674370004500702.
Kyoon-Achan, G., Lavoie, J. G., Avery Kinew, K., Philips-Beck, W., Ibrahim, N., Sinclair, S., & Katz, A. (2018). Innovating for transformation in First Nations health using community-based participatory research. Qual Health Res, 28(7), 1036–1049. https://doi.org/10.1177/1049732318756056.
Kyoon-Achan, G., Philips-Beck, W., Lavoie, J. G., Eni, R., Sinclair, S., Avery Kinew, K., . . . Katz, A. (2018a). Defining primary healthcare as a first step towards transforming the health of Manitoba First Nations. Healthcare policy, In review.
Kyoon-Achan, G., Philips-Beck, W., Lavoie, J. G., Eni, R., Sinclair, S., Avery Kinew, K., et al. (2018b). Looking back, moving forward: a First Nations framework for mental wellness. Int J Cult Ment Health, 11(4), 679–692. https://doi.org/10.1080/17542863.2018.1556714.
Lavoie, J. G., Forget, E. L., Prakash, T., Dahl, M., Martens, P. J., & O'Neil, J. D. (2010). Have investments in on-reserve health services and initiatives promoting community control improved First Nations’ health in Manitoba? Soc Sci Med, 71(4), 717–724. https://doi.org/10.1016/j.socscimed.2010.04.037.
Lavoie, J. G., Wong, S. T., Ibrahim, N., O’Neil, J. D., Green, M., & Ward, A. (2019). Underutilized and undertheorized: the use of hospitalization for ambulatory care sensitive conditions for assessing the extent to which primary healthcare services are meeting needs in British Columbia First Nation communities. BMC Health Serv Res, 19(1), 50. https://doi.org/10.1186/s12913-018-3850-y.
Loppie Reading, C., & Wien, F. (2009). Health inequalities and the social determinants of Aboriginal peoples' health. Retrieved from Prince George:
McQuaid, R., Bombay, A., McInnis, O., Humeny, C., Matheson, K., & Anisman, H. (2017). Suicide ideation and attempts among First Nations peoples living on-reserve in Canada: the intergenerational and cumulative effects of Indian residential schools. Can J Psychiatry, 62(6), 422–430.
Morgenstern, H. (1995). Ecologic studies in epidemiology: concepts, principles, and methods. Annual Review of Public Health, 16, 61–81.
Pollock, N. J., Healey, G. K., Jong, M., Valcour, J. E., & Mulay, S. (2018). Tracking progress in suicide prevention in Indigenous communities: a challenge for public health surveillance in Canada. BMC Public Health, 18(1), 1320. https://doi.org/10.1186/s12889-018-6224-9.
Roos, N. P. (1992). Hospitalization style of physicians in Manitoba: the disturbing lack of logic in medical practice. Health Serv Res, 27(3), 361–384.
Royal Commission on Aboriginal Peoples. (1996). Volume 5 - a twenty year commitment. Retrieved from Ottawa: http://www.indigenous.bc.ca/tableofcontents/Vol3TableofContents.asp
Truth and Reconciliation Commission of Canada. (2015). Honouring the truth, reconciling for the future summary of the final report of the truth and reconciliation commission of Canada. Retrieved from Ottawa: http://www.myrobust.com/websites/trcinstitution/File/Reports/Executive_Summary_English_Web.pdf
Watson, D. E., Heppner, P., Roos, N. P., Reid, R. J., & Katz, A. (2005). Population-based use of mental health services and patterns of delivery among family physicians, 1992 to 2001. Can J Psychiatr, 50(7), 398–406.
Wesley-Esquimaux, C. C., & Smolewski, M. (2004). Historic trauma and Aboriginal healing. Retrieved from Ottawa:
Acknowledgements
We would like to acknowledge the unique and invaluable contribution of our community partners: Birdtail Sioux Dakota Nation, Berens River First Nation, Cross Lake Band of Indians Pimicikamak Cree Nation, Ebb and Flow First Nation, Northlands Denesuline First Nation, Pinaymootang First Nation and Fisher River Cree Nation. Also, we thank Mr. Matthew Dahl, data analyst at the Manitoba Centre for Health Policy, for running the analysis.
Funding
This study was funded by the Canadian Institutes of Health Research (Study 292821; grant no. TT1-128267).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval was received from the University of Manitoba Health Research Ethics Board. Approval for data access was received from the Government of Manitoba Health Information Privacy Committee and the Manitoba First Nations Health Information Research Governance Committee.
Conflict of interest
The authors declare that they have no competing interests.
Disclaimer
The funder played no role in the design of the study, the collection, analysis and interpretation of data, or the writing of the manuscript.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lavoie, J.G., Phillips-Beck, W., Kinew, K.A. et al. Manitoba First Nation peoples’ use of hospital-based mental health services: trends and solutions. Can J Public Health 112, 231–239 (2021). https://doi.org/10.17269/s41997-020-00328-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.17269/s41997-020-00328-z
Keywords
- Indians, North American
- Canada
- Social marginalization
- Health equity
- Access to health care
- Primary health care