Abstract
In vitro dissolution generally involves sink conditions, so dissolution equations generally do not need to accommodate non-sink conditions. Greater use of biorelevant media, which are typically less able to provide sink conditions than pharmaceutical surfactants, necessitates equations that accommodate non-sink conditions. One objective was to derive an integrated, one-parameter dissolution equation for percent dissolved versus time that accommodates non-sink effects via drug solubility and dissolution volume parameters, including incomplete solubility. A second objective was to characterize the novel equation by fitting it to biorelevant dissolution profiles of tablets of two poorly water-soluble drugs, as well as by conducting simulations of the effect of dose on dissolution profile. The Polli dissolution equation was derived, \(\% \;dissolved=100\%\left[1-\frac{\left({{M}_{0}-c}_{s}V\right)}{{M}_{0}-{{c}_{s}Ve}^{{-k}_{d}\left(\frac{{{M}_{0}-c}_{s}V}{V}\right)t}}\right]\), where M0 is the drug dose (mg), cs is drug solubility (mg/ml), V is dissolution volume (ml), and kd is dissolution rate coefficient (ml/mg per min). Maximum allowable percent dissolved was determined by drug solubility and not a fitted extent of dissolution parameter. The equation fit tablet profiles in the presence and absence of sink conditions, using a single fitted parameter, kd, and where solubility ranged over a 1000-fold range. kd was generally smaller when cs was larger. FeSSGF provided relatively small kd values, reflecting FeSSGF colloids are large and slowly diffusing. Simulations showed impact of non-sink conditions, as well as plausible kd values for various cs scenarios, in agreement with observed kd values. The equation has advantages over first-order and z-factor dissolution rate equations. An Excel file for regression is provided.
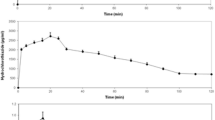
Graphical Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Immediate-release (IR) in vitro dissolution media generally provide sink conditions, or at least 85% dissolution in 60 min (1). For example, United States Pharmacopeia (USP) dissolution of capsules of the poorly water-soluble drug aprepitant employs 2.2% sodium lauryl sulfate (SLS) and a time specification at either 20 or 30 min, depending on the test (i.e., test 1, 2, or 3) (2). Aprepitant solubility without surfactant is only 3–7 µg/ml between pH 2–10 (3).
Because of this general practice of dissolution being designed to allow 85% or more dissolution, dissolution equations that are applied to percent dissolved versus time profiles often do not accommodate sink conditions (4,5,6,7,8,9,10,11). These equations are generally designed for 100% dissolution, like the in vitro test. Of course, these dissolution equations, particularly those in the simple analytical form percent dissolved as a function of time, have also been modified to allow for fitting of an extent of dissolution parameter when dissolution is incomplete (5, 6, 12, 13). Dissolution equations that are only available in differential equation (i.e., not in analytical or integrated form, such as z-factor dissolution rate equation for potential non-sink conditions) are not simple in that they cannot employ regression to fit to dissolution data, but rather require numerical integration (e.g., Runge–Kutta method using STELLA software) (14,15,16,17).
With the greater utilization of biorelevant media, there is a need for simple in vitro dissolution equations that accommodate and consider non-sink conditions, including incomplete dissolution due to insufficient solubility of all drug dose. Biorelevant media, with a composition that is intended to mimic luminal chyme properties, often provides a lower drug solubility than do pharmaceutical surfactants or a pH selection in routine in vitro dissolution. For example, the solubility of each of the weakly acidic, poorly soluble drugs indomethacin, sulindac, ibuprofen, and naproxen was enhanced less than twofold in Fasted State Simulated Intestinal Fluid-Version 2 (FaSSIF-V2, pH 6.5), compared to buffer (18). Meanwhile, the USP medium for indomethacin capsules, sulindac tablets, ibuprofen tablets, and naproxen tablets is pH 7.2 or 7.4 phosphate buffer (2). Similarly, celecoxib is a poorly water-soluble weak acid where only about 5–15% of a 200 mg celecoxib dose dissolves in pH 6.8 phosphate buffer (19) or FaSSIF-V2 (20). Meanwhile, tier 1 regulatory dissolution of celecoxib capsules employs pH 12 sodium phosphate with 1% SLS (21).
More frequent use of biorelevant media will require dissolution equations, preferably simple equations without the need for numerical integration, that can accommodate non-sink conditions. Consistent with this perspective is that, for poorly water-soluble drugs, drug permeation across the gastrointestinal tract occurs even when drug is incompletely dissolved, allowing for subsequent additional drug dissolution (22). I am unaware of a simple (i.e., non-differential) dissolution equation for percent dissolved versus time that accommodates non-sink conditions via drug solubility and dissolution volume. For example, no such equation is listed in Polli et al. or Costa and Lobo (5, 6).
One objective was to derive an integrated (i.e., not differential), one-parameter dissolution equation for percent dissolved versus time that considered non-sink effects. Here, a one-parameter dissolution equation means that only one parameter (denoted the dissolution rate coefficient, kd) is fitted in regressing the equation to the dissolution data, without the need for a fitted extent of dissolution parameter. A second objective was to characterize the novel dissolution equation by fitting the equation to biorelevant dissolution profiles of tablets of two poorly water-soluble drugs with the same 200 mg strength, as well as by conducting simulations of the effect of dose. The two drugs were ibuprofen and ketoconazole, which are a weak acid and weak base, respectively. Biorelevant media were Fasted State Simulated Gastric Fluid (FaSSGF), FaSSIF-V2, Fed State Simulated Gastric Fluid (FeSSGF), and Fed State Simulated Intestinal Fluid-Version 2 (FeSSIF-V2), where drug solubility ranged over 1000-fold.
Results indicate that an equation for percent dissolved versus time was derived, where the maximum allowable percent dissolved was determined by drug dose, drug solubility, and dissolution volume. The equation was able to fit ibuprofen and ketoconazole tablet dissolution profiles. As perhaps expected, the dissolution rate coefficient kd was generally smaller when drug solubility (cs) was larger. However, FeSSGF provided relatively small kd values, reflecting that FeSSGF colloids are large and slowly diffusing. Simulations of the effect of dose on dissolution profile revealed the expected impact of non-sink conditions, as well as plausible kd values for various cs scenarios, in agreement with observed kd values. The derived equation, with only a one fitted parameter, will have practical utility in fitting percent dissolved versus time profiles, including when non-sink conditions prevail. The derived equation is simple, in that it is an integrated form and is not a differential equation, such that only non-linear regression and not numerical integration is needed to fit the equation to dissolution data. An Excel file for regression is provided.
Theoretical
Derivation of Polli Dissolution Equation
A novel equation is derived for drug dissolution. The equation (i.e., Eq. 21 below) is an applied equation, in that the equation is anticipated to be practically applied to percent dissolved versus time profiles.
Drug dissolution rate is assumed to proceed, in part, due to the amount of drug that is not dissolved, i.e.:
where M is the mass undissolved. The familiar first-order dissolution equation also considers undissolved mass as the driving force of dissolution.
A potential barrier to the rate of dissolution is lack of sink conditions. M0 is the drug dose (i.e., M = M0 at t = 0), not all of which may potentially dissolved if drug solubility (cs) and/or dissolution volume (V) is too low. That is, if cs and/or V is excessively low, M0 may not completely dissolve at even infinite time. Hence, an additional familiar impact on drug dissolution rate is the gradient between drug solubility and drug bulk concentration, i.e.:
Non-sink conditions are not explicitly defined here, although non-sink conditions is a familiar concept where bulk drug concentration becomes sufficiently high relative to cs (e.g., over 33%), such that dissolution rate is hindered.
Considering these two factors (i.e., Eqs. 1 and 2), drug dissolution rate is:
Interestingly, while the above two factors are familiar factors in dissolution equation, I am unaware of Eq. 3 as an expression for dissolution rate, or the availability of its solution (e.g., Eqs. 18 or 21 below). Equation 3 differs from the well known, and certainly more fundamental, film equation (i.e., Fick’s first law):
where A, D, h, and cb are area, diffusivity, film thickness, and drug bulk concentration, respectively. While this difference between Eq. 3 and Fick’s first law may appear modest, Fick’s first law is certainly more fundamental, while Eq. 3, per below, has novel practical application in fitting dissolution profiles.
In order to solve Eq. 3:
Integrating yields:
Substituting M = M0 at t = 0 yields:
With a view to simplify where M = M0 at t = 0:
Hence, M = M0 at t = 0, and M = M0 − csV at t = infinite time.
As M is the mass undissolved, expressing dissolution in terms of mass dissolved (Md) and percent dissolved (% dissolved):
Of note, Eqs. 11–21 are solutions to Eq. 3, the differential form of this Polli dissolution equation. Equation 21 is the solution form of Eq. 3 that directly reflects percent dissolved versus time and denoted the Polli dissolution equation. kd is the only fitted parameter, with the expectation that M0, cs, and V are known.
The Polli Dissolution Equation Under Sink Condition: Collinearity of k d and c s
Under sink conditions (i.e., cs >> \(\frac{{M}_{0}-M}{V}\)), Eq. 3 yields:
Similarly, under sink conditions (i.e., M0 << csV), Eq. 21 yields:
Hence, when sink conditions prevail (e.g., during at least initial dissolution), the value of kd will be impacted by the value of cs, as the two parameters are collinear.
Methods
Application to Ibuprofen 200 mg and Ketoconazole 200 mg Tablet Dissolution Profiles
Ibuprofen and ketoconazole IR tablets were selected as model drug products since they have the same dose (i.e., 200 mg) but differ in solubility profile, in part since ibuprofen is a weak acid and ketoconazole is a weak base. IR tablets were selected to maximize the impact of drug dose and drug solubility on dissolution profile (i.e., IR tablets were selected to minimize the impact of formulation on dissolution profile). That said, it is recognized that IR formulation (e.g., excipients, process) can impact dissolution, and that ibuprofen 200 mg (Major Pharmaceuticals, Livonia, MI) and ketoconazole 200 mg tablets (Teva Generics, Pomona, NY) differ in formulation, such their differing dissolution profiles may reflect differing formulation, in addition to differing drug solubilities. Ibuprofen tablets include excipients colloidal silicon dioxide, corn starch, croscarmellose sodium, hypromellose, iron oxide red, iron oxide yellow, microcrystalline cellulose, polyethylene glycol, polysorbate 80, stearic acid, and titanium oxide (23). Ketoconazole tablets include excipients colloidal silicon dioxide, corn starch, lactose monohydrate, magnesium stearate, microcrystalline cellulose, and povidone (24).
Dissolution and solubility data in FaSSGF, FaSSIF-V2, FeSSGF, and FeSSIF-V2 from location A was previously reported (25). Dissolution of each tablet (n = 12) in 500 ml of “from scratch” biorelevant media had been performed. For each individual profile, Eq. 21 was fitted to percent dissolved versus time data, using Excel Solver (Microsoft, Redmond, WA; version 2206). Solver is a free Microsoft Excel add-in program from Microsoft and is intrinsic to Excel, although may need to be initially loaded into Excel. In Eq. 21, regression fit kd, while dose (M0) was 200 mg, volume (V) was 500 ml, and solubility (cs) was assigned from solubility measurement. Profiles reached terminal dissolution value at differing times. Hence, fits to profiles employed dissolution data up to and including 30 min (for ibuprofen/FaSSIF-V2, ibuprofen/FeSSIF-V2, ketoconazole/FaSSGF, and ketoconazole/FaSSIF-V2) or 60 min (for ibuprofen/FaSSGF, ibuprofen/FeSSGF, ketoconazole/FeSSGF, and ketoconazole/FeSSIF-V2).
Simulations of the Effect of Dose on Dissolution Profile
In order to complement fits to ibuprofen 200 mg and ketoconazole 200 mg tablet dissolution profiles, simulations in each 900 ml and 250 ml were performed to assess the effect of dose on dissolution profile. Using Eq. 21, simulations varied dose (i.e., 1, 10, 100, and 1000 mg) and drug solubility (i.e., 0.01, 0.1, 1, and 10 mg/ml). Simulations employed a kd range of 0.01 to 10 ml/mg per min, as fits to observed data below show kd ranged from 0.0154 to 4.59 ml/mg per min.
Results
Ibuprofen 200 mg and Ketoconazole 200 mg Tablet Dissolution Profiles: Profile Fits
Figures 1, 2, 3, and 4 plot the observed and fitted dissolution profiles into FaSSGF, FaSSIF-V2, FeSSGF, and FeSSIF-V2, respectively. As noted in Table I, ibuprofen/FaSSGF (Fig. 1), ketoconazole/FaSSIF-V2 (Fig. 2), and ketoconazole/FeSSIF-V2 (Fig. 4) showed incomplete dissolution due to inability of 500 ml of media to completely solubilize drug dose of 200 mg. Nevertheless, the Polli dissolution equation (i.e., Eq. 21) was able to adequately fit profiles. The median r2 (from n = 12 profiles) for ibuprofen in FaSSGF, FaSSIF-V2, FeSSGF, and FeSSIF-V2 was 0.98, 0.98, 0.88, and 0.98, respectively, and median r2 (from n = 12 profiles) for ketoconazole in FaSSGF, FaSSIF-V2, FeSSGF, and FeSSIF-V2 was 0.99, 0.69, 0.95, and 0.96, respectively.
Observed and fitted dissolution profiles into FeSSGF. Both profiles reflect that FeSSGF colloids are large and slowly diffusing, such that drug dissolution was slow. For each drug, kd was the slowest in FeSSGF than any other biorelevant media. Dissolution was also slowed, particularly for ketoconazole, since non-sink conditions prevailed (i.e., ibuprofen and ketoconazole required 169 ml and 359 ml FeSSGF to completely dissolve)
In Fig. 2, the fit of ketoconazole in FaSSIF-V2 was dominated by cs, where cs anticipated only 1.3% of dose to dissolve, although 2.1% dissolved (Table I), resulting in a relatively low r2 (median r2 = 0.69); however, observed and fitted profiles were close (Fig. 2). The fit with the largest difference between observed and fitted profiles was ibuprofen/FeSSGF, reflecting the shape of Eq. 21 was less able to accommodate the more linear observed dissolution profile (Fig. 3). Overall, Eq. 21 was able to adequately fit profiles.
Ibuprofen 200 mg and Ketoconazole 200 mg Tablet Dissolution Profiles: Impact of c s on k d
Table I lists mean kd values from fits, where drug/medium are listed in Table I in order of solubility, from highest to lowest. As perhaps expected, kd was generally smaller when cs was larger, as the two parameters are collinear.
Drug solubility ranged over 1000-fold, from 11.2 mg/ml for ketoconazole in FaSSGF to 0.00518 mg/ml for ketoconazole in FaSSIF-V2. Per Eq. 3, dissolution rate is determined by the product of kd, mass undissolved, and drug solubility, at least initially. Similarly, under sink conditions, the fitted value of kd will be impacted by the value of cs. In Table I, the two highest solubility scenarios are ketoconazole/FaSSGF (cs = 11.2 mg/ml) and ibuprofen/FeSSIF-V2 (cs = 1.76 mg/ml). Sink conditions prevailed in each scenario (e.g., only 114 ml FeSSIF-V2 needed to dissolve dose). For this comparison, kd was smaller when cs was larger (i.e., ketoconazole/FaSSGF kd = 0.0154 ml/mg per min was smaller than ibuprofen/FeSSIF-V2 kd = 0.0780 ml/mg per min).
This trend was generally observed across Table I. The smallest kd was for the scenario with the highest solubility, ketoconazole/FaSSGF; the largest kd was as for the scenario with the lowest solubility, ketoconazole/FaSSIF-V2. Of note, individual estimates for ketoconazole/FaSSIF-V2 kd varied widely, reflecting rapid achievement of the low terminal extent of dissolution, but were at least 0.420 ml/mg per min for any individual profile.
An exception to this trend were both drugs in FeSSGF, where ibuprofen/FeSSGF yielded a relatively low kd = 0.0303 ml/mg per min and ketoconazole/FeSSGF yielded a relatively low kd = 0.0550 ml/mg per min. Here, drug dissolution rate is assumed to be limited by diffusion of drug-loaded FeSSGF colloid from drug particle to bulk solution. But, FeSSGF colloids are large and slowly diffusing relative to other biorelevant media colloids (26). In the context of results in Table I, a relatively low kd for dissolution in FeSSGF is consistent with FeSSGF colloid being large and slowly diffusing.
The other exception to the trend was ibuprofen/FaSSGF, where limited solubility anticipates that only 16.2% of dose can dissolve. Fitted kd was only 0.0668 ml/mg per min. The reason for this exception to the observed trend is unknown. However, this perhaps slower than expected dissolution kd for ibuprofen/FaSSGF is a reminder of the simplified dissolution model underpinning this analysis (i.e., Eq. 3). That is, other potential considerations were not explicitly considered (e.g., effect of excipients and tablet manufacturing process). For example, relative to other biorelevant media, FaSSGF has a very low pH of 1.6, which could result in excipients in ibuprofen tablets, or the tablet structure of ibuprofen tablets, to slow drug dissolution, beyond the pH effect on ibuprofen cs.
Simulations of the Effect of Dose on Dissolution Profile
Table II summarizes results from simulations in 900 ml using Eq. 21 where dose was varied across four levels (i.e., 1, 10, 100, and 1000 mg), cs was varied across four levels, and kd was varied across four levels. Given the above potential collinearity of cs and kd, dose effect was inspected in Table II across the range of kd values, for each drug solubility level. As expected, qualitatively, dose effect ranged from essentially no effect at high solubility to pronounced effect at low solubility. For example, in Table II, there was essentially no dose effect when cs = 10 mg/ml, since that high solubility resulted in rapid (i.e., 85% in 30 min) and complete dissolution for even the most dissolution adverse condition of 1000 mg and kd = 0.01 ml/mg per min.
Figures S1-4 in Supplementary Materials plots all 900 ml simulation results. Selected simulations in each 900 ml and 250 ml are discussed immediately below, which employed doses (M0) of 1, 10, 100, and 1000 mg.
Figure 5 plots the impact of dose on dissolution profile into 900 ml (panel A) and 250 ml (panel B) when drug solubility cs = 1 mg/ml and kd = 0.1 ml/mg per min. For 900 ml simulations, there was essentially no dose effect, other than slightly incomplete dissolution for 1000 mg. One milligram, 10 mg, and 100 mg were rapidly dissolving. From Fig S2, simulation in 900 ml implicates that kd = 0.01 ml/mg per min is probably too low for most IR applications when cs = 1 mg/ml. Compared to 900 ml, the dose most impacted by a lower dissolution profile in 250 ml was 1000 mg (panel B of Fig. 5).
Impact of dose on dissolution profile into 900 ml and 250 ml when drug solubility cs = 1 mg/ml and kd = 0.1 ml/mg per min. Simulations employed dose (M0) of 1, 10, 100, and 1000 mg. A and B are 900 ml and 250 ml, respectively. Compared to 900 ml, the dose most impacted by a lower dissolution profile in 250 ml was 1000 mg
Figure 6 plots the impact of dose on dissolution profile into 900 ml (panel A) and 250 ml (panel B) when drug solubility cs = 0.1 mg/ml and kd = 1 ml/mg per min. Figure 7 uses the same simulation parameters as Fig. 6, except kd = 0.1 ml/mg per min. In each Figs. 6 and 7, there was a dose effect for 900 ml simulations. With progressively slower kd, each profile progressively slowed (Fig S3). This sensitivity to kd contrasts with the relative insensitivity of dissolution to kd when cs was 10 mg/ml (Fig S1) or 1 mg/ml (Fig S2). Overall, simulations in 900 ml implicate that a kd value of 0.1 ml/mg per min is low but plausible when cs = 0.1 mg/ml. Compared to 900 ml, the dose most impacted by a lower dissolution profile in 250 ml when cs = 0.1 mg/ml was the 100 mg dose for each kd = 1 ml/mg per min and kd = 0.1 ml/mg per min (panel B of Fig. 6 and panel B of Fig. 7, respectively).
Figure 8 plots the impact of dose on dissolution profile into 900 ml (panel A) and 250 ml (panel B) when drug solubility cs = 0.01 mg/ml and kd = 10 ml/mg per min. For 900 ml simulations, there was a large dose effect, and sink conditions prevailed only for the 1 mg dose. With the low cs value, dissolution of the 1 mg dose with kd of 10 ml/mg per min was rapid, but just minimally. Simulations in 900 ml implicate that kd = 1 ml/mg per min is low but plausible value when cs = 0.01 mg/ml (Fig S4). Compared to 900 ml, the dose most impacted by a lower dissolution profile in 250 ml was 10 mg (panel B of Fig. 8).
Agreement Between Observed Dissolution Profiles and Simulations: Implications About k d
A general trend from observed dissolution profile fits in Table I is that kd was generally smaller when cs was larger. kd ranged from 0.0154 to 4.59 ml/mg per min from the highest to lowest drug solubility scenarios, respectively. Hence, simulations employed a kd range of 0.01 to 10 ml/mg per min. Four observations about kd are described in Table I and discussed below relative to fits of observed dissolution profiles.
From cs = 10 mg/ml simulations in 900 ml, it was concluded that the high solubility of 10 mg/ml results in rapid and complete dissolution, even for kd = 0.01 ml/mg per min. Only ketoconazole/FaSSGF had a solubility over 10 mg/ml, where immediate and complete dissolution was characterized by a fitted kd of 0.0154 ml/mg per min. Hence, observed dissolution profile was supportive of simulations.
From cs = 1 mg/ml simulations in 900 ml, it was concluded that kd = 0.01 ml/mg per min is probably too low for most IR applications when cs = 1 mg/ml. Although cs exceeded 1 mg/ml for several drug/media scenarios, no fitted kd was less 0.0154 ml/mg per min, supporting this simulation conclusion.
From cs = 0.1 mg/ml simulations in 900 ml, it was concluded that kd = 0.1 ml/mg per min is low but plausible value when cs = 0.1 mg/ml. Ketoconazole/FeSSIF-V2 and ibuprofen/FaSSGF were scenarios with cs of about 0.1 mg/ml, and their fitted kd were 0.247 and 0.0668 ml/mg per min, respectively. There was general support from dissolution data of this conclusion from simulations, although dissolution data suggest that kd < 0.1 ml/mg per min when cs = 0.1 mg/ml is possible. These results remind that, even for IR tablets, several factors can slow dissolution, such as excipients and tablet processing effects.
From cs = 0.01 mg/ml simulations in 900 ml, it was concluded that kd value of 1 ml/mg per min is a low but plausible value for 0.01 mg/ml solubility. Ketoconazole/FaSSIF-V2 scenario had a cs of about 0.01 mg/ml. Its fitted kd was 4.59 ml/mg per min, in support of the conclusion from simulations.
Overall, there was good agreement between observed dissolution profiles and simulations about the expected range of kd values of IR products, including kd trending smaller when cs is high.
Discussion
Need for Applied Dissolution Equations that Can Accommodate Non-sink Conditions
IR in vitro dissolution media generally provide sink conditions, or at least 85% dissolution in 60 min (1). With the greater utilization of biorelevant media, there is a need for in vitro dissolution equations that accommodate and consider non-sink conditions, including incomplete dissolution due to insufficient solubility of all drug dose. Biorelevant media often provides a lower drug solubility than pharmaceutical surfactants.
For example, FaSSIF (pH = 6.5) increased carvedilol solubility only about 1.2-fold, compared to buffer, to 55.9 µg/ml (27). Meanwhile, 1% SLS (pH = 6.8) increased carvedilol solubility about 70-fold, compared to buffer, to about 1400 µg/ml (28). FaSSIF increased griseofulvin solubility only about 3%, compared to buffer, to about 12 µg/ml (29). Meanwhile, 1% SLS increased griseofulvin solubility about 85-fold to about 941 µg/ml (30). Posaconazole solubility at pH 6.5 is 0.27 µg/ml (31). FaSSIF and 0.3% SLS increased posaconazole solubility to 1.7 µg/ml and 31.2 µg/ml, respectively (32). Cinnarizine solubility at pH 6.5 is 0.16 µg/ml (33). FaSSIF-V2 and 2% SLS increased cinnarizine solubility to 2.82 µg/ml and 120 µg/ml, respectively (34).
Utility and Advantages of Polli Dissolution Equation
In general, one major application of equation fitting is to summarize data (i.e., data reduction) (35). Dissolution data is frequently subjected to equation fitting, with subsequent analysis such predicting absorption, physiologically based biopharmaceutics modeling (PBBM), in vitro-in vivo correlation, or comparison of dissolution profiles (36,37,38,39,40). For example, the FDA guidance on IR dissolution testing recognizes model-depended approaches compare profiles (1). The Hixson-Crowell equation has been used to compare profiles (5). In forecasting the in vivo impact of roller compaction scale up, dissolution data was fit to several dissolution equations, including a modified Higuchi equation (41, 42). Carducci has described the development of a real-time-release testing strategy that involves curve fitting to dissolution profiles, followed by regression of the curve fit parameters against the critical material attributes, critical processing parameters, and/or near-infrared (NIR) data (43). In similar cases, the Polli dissolution equation (i.e., Eq. 21, or Eq. 3) has potential application. Figure S5 shows the impact of kd value on potential “safe space” dissolution profiles into 900 ml when drug solubility cs = 0.1 mg/ml and dose = 10 mg.
Also, a shown here, the Polli dissolution equation has utility in fitting and summarizing dissolution data with a single parameter, when cs is known and regardless of sink condition prevailing or not prevailing. With only a fit single parameter, potential for model over-parameterization or poor model identifiability is low. Some other dissolution equations, such as Weibull equation, have at least two fitted parameters, which can be a disadvantage in data reduction, particularly if such data summarization is intended to be used in subsequent analysis (e.g., profile comparisons, a real-time-release testing strategy, parameter sensitivity assessment). The Polli dissolution equation is a relatively simple, non-differential equation. Excel software was used here to fit dissolution data. Included is an Excel file with instructions for the non-linear regression of the Polli dissolution equation to conventional dissolution data (i.e., percent dissolved versus time data). The Excel file requires the free and simple Excel Solver add-in. Since Eq. 21 is the solution to the differential form of the equation (i.e., Eq. 3), software that performs numerical integration is not needed.
Dissolution equations that are applied to percent dissolved versus time profiles often do not accommodate sink conditions, since sink conditions are commonplace (4,5,6,7,8,9,10,11). These dissolution equations have also been modified to allow for fitting of an extent of dissolution parameter when dissolution is incomplete (12, 13). Equation 21 intrinsically considers non-sink conditions. No extent of dissolution parameter was needed, although cs was needed.
Comparison of Polli Equation to the First-Order Dissolution Equation
A common equation for fitting percent dissolved versus time profiles is the familiar first-order Eq. (44, 45), whose differential and solution forms are, respectively:
Equation 3, the differential form of the Polli question, has similarity to the above differential first-order dissolution equation (i.e., Eq. 25). Both are more applied equations than mechanistic equations, although both employ undissolved mass as the driving force for dissolution rate, which is often an acknowledgeable factor of dissolution rate. Under sink conditions, Eq. 3 yields Eq. 22 above, which is practically indistinguishable from the differential first-order equation. However, relative to Eq. 21, a limitation of the first-order equation is that its solution does not accommodate a solubility limit impact on percent dissolved. Of course, such a solubility limit impact can be added to the first-order equation if an impact of solubility on extent of dissolution had been observed or expected, yielding:
But, this decision-making is undesirable. Equation 21 has the advantage of not needing to conduct such decision-making, since potential non-sink condition effects are intrinsic to Eq. 21. Equation 21 can be employed in the presence and absence of sink conditions.
Of course, Eq. 21 will not be able to fit many dissolution profile shapes, such as sigmoidal profiles due to slow disintegration. kd is constant, although could be modified to be a function of time to accommodate other shapes. The Weibull equation is generally recognized as a function that has broad success in fitting a range of dissolution profile shapes. This advantage is in part due to it containing two fitted parameters (i.e., time factor τ and shape factor β), a potential disadvantage, particularly if such data reduction is intended to be used in subsequent analysis (e.g., dissolution profile comparisons, a real-time-release testing strategy, parameter sensitivity assessment). Additionally, like above for the first-order equation, the Weibull equation does not a priori accommodate non-sink condition effects.
Comparison of Polli Equation to the z-Factor Dissolution Rate Equation
The z-factor dissolution rate equation with sink conditions is (14, 15):
where \(z=\frac{3D}{h\rho {r}_{0}}\), where z is the particle dissolution z-factor, D is drug diffusion coefficient in the media, h is diffusion layer thickness, ρ is the particle density, and r0 is the initial particle radius. Although the units of kd and the particle dissolution z-factor can be considered the same (i.e., ml/mg per min), kd and z are not identical, by inspection of Eq. 3versus Eq. 28. Equations 3 and 28 differ from one another in that Eq. 3 includes \({k}_{d}M\) term, while Eq. 28 includes \(z{M}_{0}^{1/3}{M}^{2/3}\) term. In general, in fitting profiles, fitted kd values can be expected to be greater than fitted z values, since M < \({M}_{0}^{1/3}{M}^{2/3}\) when t > 0.
Although Eq. 28 was derived by considering spherical, uniform-sized particle dissolution, it is in practice an applied equation (14,16). For example, Hofsass and Dressman describe z-factor (i.e., z) as a hybrid parameter with potential pitfalls (16), particularly in application to solid oral dosage forms, where particles are typically neither spherical and uniform-sized, nor immediately available for dissolution.
Furthermore, particle size of drug in the formulation is often not available, such that applications of the z-factor dissolution rate equation often do not employ particle size, but rather utilize Eq. 28 for data reduction and simulation (46, 47). For example, Heimbach et al. determined the safe space for etoricoxib tablets by employing a PBBM model that used the z-factor dissolution rate equation for data reduction (46). Without regard to particle size, simulations at each pH 6.8 and 2.0 were conducted where z-factor was varied in a in stepwise fashion until the simulated Cmax was at least 20% reduced, to define the safe space. Similarly, the z-factor dissolution rate equation was used to fit in vitro dissolution data of lesinurad IR tablets, for subsequent pharmacokinetic modeling (47). However, particle distribution was not an input parameter set, but rather a fitted parameter set.
A limitation of Eq. 28 is that the equation is practically only available in the differential form, necessitating the need for software such as GastroPlus, SAAM II, or STELLA that can perform numerical integration (14,15,16,17). Compared to z-factor, the Polli equation has the advantage of not needing such software to fit dissolution profiles, as it is an analytical solution and hence does not need numerical integration methods but only regression. Of note, Pepin et al. have provided an Excel file with macros to perform numerical integration to fit the z-factor dissolution rate equation, in the context of an approach employing a certain input parameter set (47).
Table III compares characteristics of the Polli equation to the z-factor dissolution rate equation under non-sink conditions, and points towards the simplicity of the Polli equation as a strength. Other particle dissolution rate equations are the Johnson equation and the Wang-Flanagan equation (11,17). Like the z-factor dissolution rate equation, a well-appreciated strength of these equations is ability to simulate particle size effects on dissolution. However, they also require numerical integration to fit dissolution data (14,15,16,17). Most particle dissolution models assume spherical shape, which is typically not the case. Drug particle size distribution and shape are often not known in formulated tablets, attenuating the potential advantage of such particle dissolution models, and perhaps creating opportunity for model over-parameterization. Meanwhile, with only a single fitted parameter, Eq. 21 does not assume any particular particle distribution or shape, but only that drug mass is a driving force for dissolution, with drug solubility (i.e., non-sink conditions) potentially reducing dissolution. Likewise, while z in Eq. 28 can be considered an explicit function of drug diffusion coefficient, which may or may not be known (26, 29), Eq. 21 does not assume any particular drug transport phenomena beyond drug mass as a driving force for dissolution, with potential non-sink effects. Interesting, as noted above, FeSSGF here provided relatively small kd values, reflecting that FeSSGF colloids are large and slowly diffusing.
Conclusion
The main objective was to derive a dissolution equation for percent dissolved versus time that considered non-sink effects, including incomplete solubility in dissolution media. Equation 21 was derived, where the maximum allowable percent dissolved was determined by drug solubility, and without a fitted extent of dissolution parameter. The equation, denoted the Polli dissolution equation, was able to fit ibuprofen and ketoconazole dissolution profiles in biorelevant media, using a single fitted parameter, kd. Equation 21 was fit to dissolution profiles without regard to sink conditions, and where solubility ranged over a 1000-fold range. kd was generally smaller when cs was larger. FeSSGF provided relatively small kd values, reflecting that FeSSGF colloids are large and slowly diffusing. Simulations showed the impact of non-sink conditions, as well as plausible kd values for various cs scenarios, in agreement with observed kd values. The Polli equation accommodated non-sink condition effects, including whether or not solubility limits dissolution to less than 100%. This accommodate is intrinsic to the equation. The equation has advantages over the use of the first-order and z-factor dissolution rate equations. An Excel file for regression is provided.
Change history
14 January 2023
The original article has been updated to include the missing supplemental file.
References
Food and Drug Administration. Dissolution testing of immediate release solid oral dosage forms. 1997. https://www.fda.gov/media/70936/download. Accessed 18 Aug 2022.
United States Pharmacopeial Convention Committee of Revision. United States pharmacopeia - national formulary 2022. Rockville, MD: United States Pharmacopeial Convention; 2022.
Wu Y, Loper A, Landis E, Hettrick L, Novak L, Lynn K, et al. The role of biopharmaceutics in the development of a clinical nanoparticle formulation of MK-0869: a Beagle dog model predicts improved bioavailability and diminished food effect on absorption in human. Int J Pharm. 2004;285:135–46. https://doi.org/10.1016/j.ijpharm.2004.08.001.
Siepmann J, Siepmann F. Mathematical modeling of drug dissolution. Int J Pharm. 2013;453:12–24. https://doi.org/10.1016/j.ijpharm.2013.04.044.
Polli JE, Rekhi GS, Augsburger LL, Shah VP. Methods to compare dissolution profiles and a rationale for wide dissolution specifications for metoprolol tartrate tablets. J Pharm Sci. 1997;86:690–700. https://doi.org/10.1021/js960473x.
Costa P, Sousa Lobo JM. Modeling and comparison of dissolution profiles. Eur J Pharm Sci. 2001;13:123–33. https://doi.org/10.1016/s0928-0987(01)00095-1.
Yuksel N, Kanik AE, Baykara T. Comparison of in vitro dissolution profiles by ANOVA-based, model-dependent and -independent methods. Int J Pharm. 2000;209:57–67. https://doi.org/10.1016/s0378-5173(00)00554-8.
Lansky P, Weiss M. Does the dose-solubility ratio affect the mean dissolution time of drugs? Pharm Res. 1999;16:1470–6. https://doi.org/10.1023/a:1018923714107.
Macheras P, Dokoumetzidis A. On the heterogeneity of drug dissolution and release. Pharm Res. 2000;17:108–12. https://doi.org/10.1023/a:1007596709657.
Shekunov B, Montgomery ER. Theoretical analysis of drug dissolution: I. Solubility and intrinsic dissolution rate. J Pharm Sci. 2016;105:2685–2697. https://doi.org/10.1016/j.xphs.2015.12.006.
Wang J, Flanagan DR. General solution for diffusion-controlled dissolution of spherical particles. 1. Theory. J Pharm Sci. 1999;88:731–8. https://doi.org/10.1021/js980236p.
Usta DY, Incecayir T. Modeling of in vitro dissolution profiles of carvedilol immediate-release tablets in different dissolution media. AAPS PharmSciTech. 2022;23:201. https://doi.org/10.1208/s12249-022-02355-0.
Lee H, Park S, Sah H. Surfactant effects upon dissolution patterns of carbamazepine immediate release tablet. Arch Pharm Res. 2005;28:120–6. https://doi.org/10.1007/BF02975147.
Nicolaides E, Symillides M, Dressman, Reppas C. Biorelevant dissolution testing to predict the plasma profile of lipophilic drugs after oral administration. Pharm Res. 2001;18:380–8. https://doi.org/10.1023/a:1011071401306.
Takano R, Sugano K, Higashida A, Hayashi Y, Machida M, Aso Y, Yamashita S. Oral absorption of poorly water-soluble drugs: computer simulation of fraction absorbed in humans from a miniscale dissolution test. Pharm Res. 2006;23:1144–56. https://doi.org/10.1007/s11095-006-0162-4.
Hofsass MA, Dressman J. Suitability of the z-factor for dissolution simulation of solid oral dosage forms: potential pitfalls and refinements. J Pharm Sci. 2020;109:2735–45. https://doi.org/10.1016/j.xphs.2020.05.019.
Johnson KC. Comparison of methods for predicting dissolution and the theoretical implications of particle-size-dependent solubility. J Pharm Sci. 2012;101:681–9. https://doi.org/10.1002/jps.22778.
Bou-Chacra N, Melo KJC, Morales IAC, Stippler ES, Kesisoglou F, Yazdanian M, et al. Evolution of choice of solubility and dissolution media after two decades of biopharmaceutical classification system. AAPS J. 2017;19:989–1001. https://doi.org/10.1208/s12248-017-0085-5.
Rawat S, Jain SK. Solubility enhancement of celecoxib using beta-cyclodextrin inclusion complexes. Eur J Pharm Biopharm. 2004;57(2):263–7. https://doi.org/10.1016/j.ejpb.2003.10.020.
Shono Y, Jantratid E, Janssen N, Kesisoglou F, Mao Y, Vertzoni M, et al. Prediction of food effects on the absorption of celecoxib based on biorelevant dissolution testing coupled with physiologically based pharmacokinetic modeling. Eur J Pharm Biopharm. 2009;73:107–14. https://doi.org/10.1016/j.ejpb.2009.05.009.
Dissolution Methods Database. Food and Drug Administration, White Oak, MD. 2022. https://www.accessdata.fda.gov/scripts/cder/dissolution/index.cfm. Accessed 18 Aug 2022.
Mudie DM, Shi Y, Ping H, Gao P, Amidon GL, Amidon GE. Mechanistic analysis of solute transport in an in vitro physiological two-phase dissolution apparatus. Biopharm Drug Dispos. 2012;33:378–402. https://doi.org/10.1002/bdd.1803.
Major Pharmaceuticals. Ibuprofen tablets 200mg label. Livonia, MI: Major Pharmaceuticals; 2017.
Teva Generics. Ketoconazole tablets 200mg label. Pomona, NY: Teva Generics; 2013.
Jamil R, Xu T, Shah HS, Adhikari A, Sardhara R, Nahar K, et al. Similarity of dissolution profiles from biorelevant media: assessment of interday repeatability, interanalyst repeatability, and interlaboratory reproducibility using ibuprofen and ketoconazole tablets. Eur J Pharm Sci. 2021;156: 105573. https://doi.org/10.1016/j.ejps.2020.105573.
Jamil R, Polli JE. Prediction of in vitro drug dissolution into fed-state biorelevant media: contributions of solubility enhancement and relatively low colloid diffusivity. Eur J Pharm Sci. 2022;173: 106179. https://doi.org/10.1016/j.ejps.2022.106179.
Fagerberg JH, Tsinman O, Sun N, Tsinman K, Avdeef A, Bergström CA. Dissolution rate and apparent solubility of poorly soluble drugs in biorelevant dissolution media. Mol Pharm. 2010;7:1419–30. https://doi.org/10.1021/mp100049m.
Incecayir T. The effects of surfactants on the solubility and dissolution profiles of a poorly water-soluble basic drug, carvedilol. Pharmazie. 2015;70:784–90.
Jamil R, Polli JE. Prediction of in vitro drug dissolution into fasted-state biorelevant media: contributions of solubility enhancement and relatively low colloid diffusivity. Eur J Pharm Sci. 2022;174: 106210. https://doi.org/10.1016/j.ejps.2022.106210.
Sjokvist E, Nystrom C, Alden M, Caram-Lelham N. Physicochemical aspects of drug release. XIV. The effects of some ionic and non-ionic surfactants on properties of a sparingly soluble drug in solid dispersions. Int J Pharm. 1992;79:123–133.
Duong TV, Ni Z, Taylor LS. Phase behavior and crystallization kinetics of a poorly water-soluble weakly basic drug as a function of supersaturation and media composition. Mol Pharm. 2022;19:1146–59. https://doi.org/10.1021/acs.molpharmaceut.1c00927.
Chen Y, Wang S, Wang S, Liu C, Su C, Hageman M, et al. Sodium lauryl sulfate competitively interacts with HPMC-AS and consequently reduces oral bioavailability of posaconazole/HPMC-AS amorphous solid dispersion. Mol Pharm. 2016;13:2787–95. https://doi.org/10.1021/acs.molpharmaceut.6b00391.
Berlin M, Przyklenk K, Richtberg A, Baumann W, Dressman JB. Prediction of oral absorption of cinnarizine—a highly supersaturating poorly soluble weak base with borderline permeability. Eur J Pharm Biopharm. 2014;88:795–806. https://doi.org/10.1016/j.ejpb.2014.08.011.
Kayaert P, Van den Mooter G. Is the amorphous fraction of a dried nanosuspension caused by milling or by drying? A case study with naproxen and cinnarizine. Eur J Pharm Biopharm. 2012;81:650–6. https://doi.org/10.1016/j.ejpb.2012.04.020.
Wagner JG. Pharmacokinetics for the pharmaceutical scientist. 1st ed. Lancaster, PA: Technomic Publishing Company; 1993.
Mohamed MF, Winzenborg I, Othman AA, Marroum P. Utility of modeling and simulation approach to support the clinical relevance of dissolution specifications: a case study from upadacitinib development. AAPS J. 2022;24:39. https://doi.org/10.1208/s12248-022-00681-6.
Aburub A, Chen Y, Chung J, Gao P, Good D, Hansmann S, et al. An IQ Consortium perspective on connecting dissolution methods to in vivo performance: analysis of an industrial database and case studies to propose a workflow. AAPS J. 2022;24:49. https://doi.org/10.1208/s12248-022-00699-w.
Mitra A, Parrott N, Miller N, Lloyd R, Tistaert C, Heimbach T, et al. Prediction of pH-dependent drug-drug interactions for basic drugs using physiologically based biopharmaceutics modeling: industry case studies. J Pharm Sci. 2020;109:1380–94. https://doi.org/10.1016/j.xphs.2019.11.017.
Wu F, Shah H, Li M, Duan P, Zhao P, Suarez S, et al. Biopharmaceutics applications of physiologically based pharmacokinetic absorption modeling and simulation in regulatory submissions to the U.S. Food and Drug Administration for new drugs. AAPS J. 2021;23:31. https://doi.org/10.1208/s12248-021-00564-2.
Hens B, Seegobin N, Bermejo M, Tsume Y, Clear N, McAllister M, et al. Dissolution challenges associated with the surface pH of drug particles: integration into mechanistic oral absorption modeling. AAPS J. 2022;24:17. https://doi.org/10.1208/s12248-021-00663-0.
Shesky P, Sackett G, Mahe, L, Lentz KA, Tolle S, and Polli JE. Roll compaction granulation of a controlled-release matrix tablet containing HPMC: effect of process scale-up on robustness of tablets and predicted in vivo performance. Pharm Tech. 1999;23(suppl.): 6–21.
Sheskey P, Pacholke K, Sackett G, Maher L, Polli JE. Roll compaction granulation of a controlled-release matrix tablet containing HPMC: effect of process scale-up on robustness of tablets and predicted in vivo performance. Part II Pharm Tech. 2000;24(11):30–52.
Zaborenko N, Carducci TM, Ryckaert A, Mandula H, Walworth MJ, et al. Predictive dissolution models for real-time release testing: development and implementation – workshop summary report. Dissolution Technolog. 2022;29:150–72. https://doi.org/10.14227/DT290322P150.
Polli JE, Crison JR, Amidon GL. Novel approach to the analysis of in vitro-in vivo relationships. J Pharm Sci. 1996;85:753–60. https://doi.org/10.1021/js9503587.
Yu XL, Amidon GL. A compartmental absorption and transit model for estimating oral drug absorption. Int J Pharm. 1999;186:119–25. https://doi.org/10.1016/s0378-5173(99)00147-7.
Heimbach T, Kesisoglou F, Novakovic J, Tistaert C, Mueller-Zsigmondy M, Kollipara S, et al. Establishing the bioequivalence safe space for immediate-release oral dosage forms using physiologically based biopharmaceutics modeling (PBBM): case studies. J Pharm Sci. 2021;110:3896–906. https://doi.org/10.1016/j.xphs.2021.09.017.
Pepin XJ, Flanagan TR, Holt DJ, Eidelman A, Treacy D, Rowlings CE. Justification of drug product dissolution rate and drug substance particle size specifications based on absorption PBPK modeling for lesinurad immediate release tablets. Mol Pharm. 2016;13:3256–69. https://doi.org/10.1021/acs.molpharmaceut.6b00497.
Funding
This research was supported by the Food and Drug Administration (FDA) of the US Department of Health and Human Services (HHS) as part of a financial assistance award 5U01FD005946-05 totaling $1,577,013 with 100% funded by FDA/HHS. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement, by FDA/HHS, or the US Government.
Author information
Authors and Affiliations
Contributions
The author conducted the analysis, writing, and approval of the version to be published.
Corresponding author
Ethics declarations
Conflict of Interest
JEP is a member of the Scientific Advisory Board of SimulationsPlus.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1
(DOCX 237 kb)
Supplementary file2
(XLSX 25.9 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Polli, J.E. A Simple One-Parameter Percent Dissolved Versus Time Dissolution Equation that Accommodates Sink and Non-sink Conditions via Drug Solubility and Dissolution Volume. AAPS J 25, 1 (2023). https://doi.org/10.1208/s12248-022-00765-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12248-022-00765-3