Abstract
Background
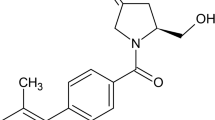
OBE001 is a novel, orally active nonpeptide oxytocin receptor antagonist under development for the treatment of preterm labor and improvement in embryo implantation and pregnancy rate in assisted reproductive technology (ART). The reproductive safety of OBE001 was evaluated in customized fertility embryonic development (FER)/early embryonic development (EED) and fetal development (FD) and pre/postnatal development (PPN) studies mimicking clinical exposure scenarios.
Methods
Oral OBE001 was evaluated at doses of 37.5, 75, and 125 mg/kg/d in female rats during a FER/EED study (from premating to implantation) and throughout FD during a FD/PPN study.
Results
No OBE001 effects were observed during the FER/EED study. The FD/PPN study did not result in adverse OBE001 effects in females allowed to litter, their offspring, and second-generation fetuses. Females at 125 mg/kg/d who underwent cesarean section before term had slight reductions in body weights and food consumption, and associated fetuses had slightly delayed ossification of skull bones, which was not adverse in the absence of effects on live offspring.
Conclusion
OBE001 at up to 125 mg/kg/d had no effects on EED and no adverse effects on FD and postnatal development of rats. These results constitute an important step toward the development of OBE001 in preterm labor and ART indications.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
http://ClinicalTrials.gov. OBE001 Phase 2 Dose-finding Study Versus Placebo in Women Undergoing Embryo Transfer in the Context of IVF-ICSI (IMPLANT). 2015. http://climcaltrials.gov/ct2/show/NCT02310802?term=obseva&rank=1/ct2/show/NCT02310802?term=obseva&rank=l. Accessed September 15, 2015.
http://ClinicalTrials.govA Phase 2 Study of OBE001 Versus Placebo in the Delay of Preterm Birth (TERM). 2015. https://clinicaltrials.gov/ct2/show?term=obseva&rank=2/ct2/show?term=obseva&rank=2. Accessed September 15, 2015.
Howson CP, Kinney MV, McDougall L, Lawn JE. Bom too soon:preterm birth matters. Reprod Health. 2013; 10(suppl 1):S1.
Vrachnis N, Malamas FM, Sifakis S, Deligeoroglou E, Iliodromiti Z. The oxytocin-oxytocin receptor system and its antagonists as tocolytic agents. Int J Endocrinol. 2011; 2011:350546.
Cirillo R, Gillio Tos E, Schwarz MK, et al. Pharmacology of (2S,4Z)-N-[(2S)-2-hydroxy-2-phenylethyl]-4-(methoxyimino)-l-[(2’-methyl[l,l’-biphenyl]-4-yl)carbonyl]-2-pyrrolidinecarboxamide, a new potent and selective nonpeptide antagonist of the oxytocin receptor. J Pharmacol Exp Ther. 2003 Jul; 306(1):253–261.
Romero R, Sibai BM, Sanchez-Ramos L, et al. An oxytocin receptor antagonist (atosiban) in the treatment of preterm labor:a randomized, double-blind, placebo-controlled trial with tocolytic rescue. Am J Obstet Gynecol. 2000; 182(5):1173–1183.
Thornton S, Vatish M, Slater D. Oxytocin antagonists:clinical and scientific considerations. Exp Physiol. 2001; 86(2):297–302.
Ayoubi JM, Epiney M, Brioschi PA, Fanchin R, Chardonnens D, de Ziegler D. Comparison of changes in uterine contraction frequency after ovulation in the menstrual cycle and in in vitro fertilization cycles. Fertil Steril. 2003; 79(5):1101–1105.
Fanchin R, Righini C, Olivennes F, Taylor S, de Ziegler D, Fryd-man R. Uterine contractions at the time of embryo transfer alter pregnancy rates after in-vitro fertilization. Hum Reprod. 1998; 13(7):1968–1974.
Zhu L, Che HS, Xiao L, Li YP. Uterine peristalsis before embryo transfer affects the chance of clinical pregnancy in fresh and frozen-thawed embryo transfer cycles. Hum Reprod. 2014; 29(6):1238–1243.
Moraloglu O, Tonguc E, Var T, Zeyrek T, Batioglu S. Treatment with oxytocin antagonists before embryo transfer may increase implantation rates after IVF. Reprod Biomed Online. 2010; 21(3):338–343.
Pohl O, Homery MC, Lemaux F, Patat A, Chollet A. Pharmacokinetic interactions of OBEOOl and betamethasone in healthy female volunteers. J Clin Pharm Ther. 2015; 40(3):328–332.
International Conference on Harmonisation of Technical Requirements for Registration of Pharmaceuticals for Human Use. ICH M3 (R2)—Guideline on Nonclinical Safety Studies for the Conduct of Human Clinical Trials and Marketing Authorization for Pharmaceuticals. 2009. http://www.ich.org/fileadmin/Public_Web_Site/ICH_Products/Guidelines/Multidisciplinary/ M3_R2/Step4/M3_R2_Guideline.pdf/fileadmin/Public_Web_Site/ICH_Products/Guidelines/Multidisciplinary/ M3_R2/Step4/M3_R2_Guideline.pdf. Accessed September 15, 2015.
ICH Harmonised Tripartite Guideline. Part I:Detection of Toxicity to Reproduction for Medicinal Products (24 June 1993). In:International Conference on Harmonisation of Technical Requirements for Registration of Pharmaceuticals for Human Use. ICH S5(R2)—Detection of Toxicity to Reproduction for Medicinal Products and Toxicity to Male Fertility. 2005. http://www.ich.org/fileadmin/Public_Web_Site/ICH_Products/Guide-lines/Safety/S5/Step4/S5_R2__Guideline.pdf/fileadmin/Public_Web_Site/ICH_Products/Guide-lines/Safety/S5/Step4/S5_R2__Guideline.pdf Accessed September 15, 2015.
Staples RE. Teratogens and the delaney clause. Science. 1974; 185(4154):813–814.
Wilson JG. Embryological considerations in teratology. Ann N Y Acad Sci. 1965; 123:219–227.
Shaima S, Lee J, Gao P, Steele VE. Toxicity profile of solvents by aspiration approach for topical agent delivery to respiratory tract epithelium. Int J Toxicol. 2011; 30(3):358–366.
Delongeas JL, de Conchard GV, Beamonte A, et al. Assessment of Labrasol/Labrafil/Transcutol (4/4/2, v/v/v) as a non-clinical vehicle for poorly water-soluble compounds after 4-week oral toxicity study in Wistar rats. Regul Toxicol Pharmacol. 2010; 57(2–3):284–290.
Healing G, Sulemann T, Cotton P, et al. Safety data on 19 vehicles for use in I month oral rodent pre-clinical studies:administration of hydroxypropy1-β-cyclodextrin causes renal toxicity [published online May 10, 2015]. J Appl Toxicol. 2015. doi:10.1002/jat.3155.
Bailey GP, Wise LD, Buschmann J, Hurtt M, Fisher JE. Pre-and postnatal developmental toxicity study design for pharmaceuticals. Birth Defects Res B Dev Reprod Toxicol. 2009; 86(6):437–445.
Aliverti V, Bonanomi L, Giavini E, Leone VG, Mariani L. The extent of fetal ossification as an index of delayed development in teratogenic studies on the rat. Teratology. 1979; 20(2):237–242.
Destexhe E, Stannard D, Wilby OK, et al. Nonclinical reproductive and developmental safety evaluation of the MAGE-A3 Cancer Immunotherapeutic, a therapeutic vaccine for cancer treatment. Reprod Toxicol. 2015; 51:90–105.
McAnulty PA, Bums LM. Evaluation of the maternal and neonatal effects of the oxytocin antagonist, atosiban, in a cross-fostering study in rats. Reprod Toxicol. 2004; 19(1):65–70.
EMEA. Tractocile:EPAR. 2004. http://viww.ema.europa.eu/docs/en_GB/document_library/EPAR_-_Scientific_ Discussion/human/000253/WC500040491.pdf/docs/en_GB/document_library/EPAR_-_Scientific_ Discussion/human/000253/WC500040491.pdf Accessed June 06, 2015.
McGovem PG, Llorens AJ, Skumick JH, Weiss G, Goldsmith LT. Increased risk of preterm birth in singleton pregnancies resulting from in vitro fertilization-embryo transfer or gamete intrafallopian transfer:a meta-analysis. Fertil Steril. 2004; 82(6):1514–1520.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pohl, O., Perks, D., Rhodes, J. et al. Effects of the Oral Oxytocin Receptor Antagonist Tocolytic OBE001 on Reproduction in Rats. Reprod. Sci. 23, 439–447 (2016). https://doi.org/10.1177/1933719115607979
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719115607979