Abstract
Under the influence of external and internal factors, various changed proteins inevitably arise in cells. With age, the activity of chaperones and other components of cellular control over protein quality decreases. This is accompanied by the accumulation of misfolded proteins with altered conformations. The most dramatic event for the cell is the transformation of an active soluble protein into an amyloid insoluble and inactive state. It is believed that this change in protein conformation underlies the process of neurodegeneration. Although this process is being intensively studied, many details of neurodegeneration remain unclear. In this review, we present the currently most accepted molecular mechanisms of the pathogenesis of the most common neurodegenerative diseases, Alzheimer’s and Parkinson’s. They include sequential reactions β-amyloid and α-synuclein with membrane receptors and are modulated by phase separation and cross-seeding with other cellular prions. Particular attention is paid to natural polyfunctional compounds as the most therapeutically promising.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Neurodegeneration caused by a conformational change in a protein, despite many years of intensive study, remains one of the most pressing problems in molecular cell biology and medicine. In this review, we have tried to present generally accepted concepts of the pathogenesis of the most common neurodegenerative diseases, Alzheimer’s (AD) and Parkinson’s (PD), as well as modern approaches to the search for substances to combat them.
PROTEIN ISOFORM GENERATION
Under the action of external and internal factors at the level of transcription, translation, or post-translational modifications, various protein forms, or proteoforms, inevitably arise in the cell. The most cardinal of them is the conversion of the active soluble state to the amyloid, insoluble and inactive state. It is widely believed that the ability to form amyloid fibrils is inherent in all polypeptide chains. In other words, even typically nonamyloid proteins, under certain circumstances, are transformed into either an amyloid or an amyloid-like state (Stefani and Dobson, 2003). The cause of this is usually an imbalance between native folding and protein aggregation. The main components of the control system, proteostasis, ensure either the correction of the nonfunctional form of the protein or its proteolysis (Franic et al., 2021). An imbalance most often leads to a decrease in the activity of either lysosomal (Desplats et al., 2009; Hamano et al., 2018), or a dynein–dynactin complex delivering the defective protein to the autophagosome (Kieran et al., 2005). Short-lived proteins involved in the regulation of cell signaling systems are usually degraded by ubiquitin-proteasome parthway. Long-lived cellular components, organelles and protein aggregates, are destroyed by the cell with the help of lysosomal systems. Delivery of these components to lysosomes is carried out in the process of autophagy, including chaperone-mediated autophagy. With aging, the activity of chaperones and cellular control proteins decreases, resulting in the accumulation of misfolded proteins with altered secondary and tertiary structures.
PATHOGENESIS OF ALZHEIMER’S DISEASE
Conformational neurodegenerative diseases (chronic and progressive forms of proteinopathies) have common features: death of neurons in specific areas of the brain, damage to synapses, and accumulation of misfolded protein aggregates, leading to impaired cognitive and a number of other neuronal functions. The common cause of these diseases is that soluble, correctly folded proteins that perform regulatory functions in nerve cells and synapses undergo amyloidization, turning into nonfunctional insoluble aggregates or polymers, the monomers of which are the proteins themselves with a changed conformation. Amyloid aggregation is based on the ability of proteins to self-assemble, which results in the formation of β-pleated secondary structures stabilized by intermolecular hydrogen bonds. Short polymers containing β-layers are called “seeds” or “propagons,” since they significantly accelerate the self-assembly process through the templated mechanism of amyloid reproduction.
Huge clinical and experimental material obtained at the cellular and organismal levels has been intensively studied over the past decades (more than 3). The most common neurodegenerative disease, AD, is associated with damage to synapses and neurons, mainly cholinergic, related to the hippocampus and cerebral cortex (Braak et al., 2006). It is symptomatic of confusion and memory loss. In the brain of patients, in the intercellular space, deposits (plaques) are found, consisting of β-amyloid fibrils (βA) and networks of neurofibrillary strands of τ protein. The deposits of these proteins serve as the main diagnostic marker of AD. Although βA is formed outside the cell, and the τ protein is within, the aggregation of these proteins has an interdependent character (Bennett et al., 2017; Jacobs et al., 2018).
Functionally active βA results from the cleavage of the soluble APP precursor protein by three secretases: α, β, and γ. The main pathway of proteolysis begins with the action of α-secretase and leads to the formation of the soluble sAPP-α protein and the 83-amino-acid nonamyloidogenic protein. Minor amyloidogenic proteolysis at the first stage is carried out by β-secretase. It leads to the soluble protein sAPP-β, from which α-secretase cleaves the protein βA, which contains from 37 to 42 amino acids. Functional proteins, including the APP precursor protein, play a positive regulatory role in normal brain development and synapse activity, as well as neuroprotection (Hillen, 2019; Penke et al., 2019). In particular, βA not only ensures the normal functioning of synapses, but is also needed by nerve cells for regeneration and to maintain the blood–brain barrier. Its antimicrobial and antiviral activity has also been shown. However, the protein structure of βA provides its ability to, first, assemble into soluble intermediates and, then, turn into insoluble fibrils.
On the way to the formation of mature amyloid fibrils, intermediates appear, which are usually divided into three main groups: oligomers, protofibrils, and fibrils that differ in basic parameters. Thus, the oligomers formed at the early stages of fibrillation have a structure with antiparallel β-layers and are not stained with amyloid-specific dyes (thioflavins and Congo red). They are soluble, highly variable in their morphology, and react with antibodies to oligomers.
The class of protofibrils is distinguished by the parallel arrangement of β-layers and binding to amyloid-specific dyes, as well as the reaction to antibodies against amyloid fibrils. However, like oligomers, they remain soluble and retain great morphological diversity. The class of fibrils is characterized by a parallel direction of β-layers, binding to dyes typical of amyloids, reacts to fibrillar antibodies, but, unlike the two previous intermediates, consists of linear insoluble filaments, twisting into strands as they mature (Fig. 1) (Penke et al., 2020). Mature fibrils are usually slightly toxic, and under certain conditions they can even perform a certain function, most often a protective one.
Assembly of units β-amyloid (βA) and their possible transformations. (1) Ribosome, (2) unfolded native monomer, (3) disordered aggregates, (4) chaperones, (5) folded protein containing α- helices and β- layers, (6) oligomer with α- helical structure,(7) oligomer consisting of β -layers, (8) soluble protofibrils with parallel β- layers, (9) proteasome in which aggregates undergo hydrolysis, (10) amino acids, (11) insoluble fibrils, and (12) deposits consisting of large amyloid aggregates and a network of strands of τ protein (plaques).
Numerous evidence has been obtained that oligomers, rather than mature fibrils, are the most toxic intermediates (see review Dujardin et al., 2014). It is believed that small-sized oligomers that appear at the earliest stages of aggregation have a primary pronounced toxic effect (Chernova et al., 2019). At the same time, the ends of the polymer, penetrating into the membrane of the nerve cell and destroying it, serve as one of the main causes of βA toxicity (Wells et al., 2021). Therefore, oligomers, as smaller polymers, are more dangerous for the cell than fibrils. Model experiments with growing different amyloids clearly show that the longer the fibrils, the less their toxicity (Xue et al., 2010).
Recent studies have revealed an interesting fact that is important for the search for effective AD therapy. It turned out that not all oligomers have a pathological effect in vitro and in vivo. In a number of studies, oligomers are divided into toxic and nontoxic subpopulations (Lorenzen et al.,2014; Paslavski et al., 2014; Alam et al., 2019; Penke et al., 2020). Toxic oligomers of the first type have a relatively high molecular weight of more than 50 kDa, are rich in β-layers, do not bind to plaques, do not react with antibodies to fibrils, and impair memory when injected into mice. Oligomers of the second type have a molecular weight of less than 50 kDa, are rich in α helices, and do not lose the functions that monomers carry. They do not form fibrils, they bind to plaques, they react to antibodies to fibrils, and, being nontoxic, they do not impair memory.
The pathogenesis of AD is a long multistage process in which toxic βA oligomers act as triggers after the hydrophobic areas on their surface interact with the lipid layer of the cell membrane of the neuron. The key role in the pathogenesis of AD is presumably played by βA oligomers and modified forms of the membrane τ protein, primarily oligomers and hyperphosphorylated τ fibrils (Penke et al., 2020; Niewiadomska et al., 2021).
In the first pathological process, βA oligomers form complexes with specific receptor proteins. A special role is assigned to the cellular prion protein PrP. It is a glycosylated protein localized (anchored) in the lipid layers of the membrane. The toxic effect of PrP binding to βA, is shown in Drosophila (Younan et al., 2018). In its intact monomeric form, PrP is involved in signal transmission, and altered forms of this protein significantly affect the development of AD (Hachiya et al., 2021; Konig et al., 2021). In addition, the prion form of PrP–Sc changes the structure and expression of the τ protein, which is also associated with the cell membrane. Normally, phosphorylated τ protein binds to microtubulins, ensuring the stability of the genetic material of neurons, and by binding to actin, it participates in the work of the cytoskeleton, protecting the ends of microtubulins from depolymerization. Due to alternative splicing, varying degrees of phosphorylation and fibrillation in neurons, there is a wide variety of τ protein isoforms. In AD, due to interaction with amyloid βA, oligomerization of the τ protein occurs, which reduces its ability to bind to microtubulins and perform its functions (Barbier et al., 2019).
A change in signaling under the action of βA oligomers leads to the appearance of toxic hyperphosphorylated forms of the τ protein, both monomeric and oligomeric proteoforms. At the same time, it turns into strands that prevent the formation of stress granules, and in this state becomes highly toxic. Hyperphosphorylation is accompanied by the transformation of protein molecules into bundles of tangled filaments or a network of neurofibrillary strands (NETs), which is always found in the brain of AD patients. But although these strands are composed of toxic isoforms, they do not necessarily lead to neuronal dysfunction. The key role in the induction and development of toxicity belongs to the oligomers of the τ protein, regardless of the degree of their phosphorylation. They have a developed β-structure and the mechanism of their pathological action on neurons differs from βA. They cause multiple disorders due to exocytosis and the ability to spread to surrounding nerve cells due to endocytosis. Pathological processes triggered by oligomers βA in the intercellular space and τ protein inside the cell are very diverse (Nygaard et al., 2014; Zhang et al., 2019a). These are violations of genomic stability, energy and ion exchange, mitochondrial functions, cell signaling, synaptic conduction, microtubulin assembly, damage to the neuronal cytoskeleton, axonal transport, and the proteolytic system. It should be noted that an increase in βA in the cerebrospinal fluid of patients is detected before the appearance of increased levels of toxic forms of τ protein; therefore, it is believed that βA toxic oligomers is the main primary trigger of AD.
PATHOGENESIS OF PARKINSON’S DISEASE
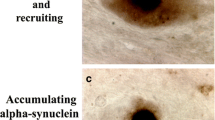
PD is the second-most-common neurodegenerative disease after AD. Its external symptoms are akinesia, decreased tone of the skeletal and internal muscles, tremor at rest, impaired coordination of movements, and in some cases damage to the cognitive sphere. These pathological changes are based on the loss of dopaminergic neurons in an area of the brain called the “substantia nigra.” Surviving neurons contain cytoplasmic inclusions, so-called “Lewy bodies,” which consist of α-synuclein (AS) protein in amyloid form in the state of fibrillar structures (Baba et al., 1998).
α-Synuclein monomers consist of 140 amino acids and control neuronal transmission, i.e., the transmission of a nerve impulse in the synapses of dopaminergic neurons. α-Synuclein aggregation blocks these vital functions. Of the intermediates on the aggregation pathway, oligomers are considered the most toxic, but mature fibrils, preventing neuronal transmission in axons, also contribute to synuclein toxicity (Stephanis, 2012).
There are many processes involved in neuronal death caused by α-synuclein amyloidization. They are based on the ability of certain forms of amyloid to integrate into the lipid layers of the cell membrane, violating its integrity.
At the initial stages of fibrillation, the structure of oligomers is rich in α helices, but as the fibril grows, the proportion of β-layers in them increases sharply. Paslavsky et al. discovered two types of oligomers: one incapable of monomer reverse dissociation, but capable of transforming into fibrils during elongation, and another that is not involved in either fibril formation or synuclein-induced pathogenesis (Paslawski et al., 2014). Later, three classes of oligomers were proposed (Cascella et al., 2022). The first includes tetrameric or more complex oligomers that are rich in α helices, are short lived, and do not differ from monomers in biological function. They are not capable of producing aggregated amyloid forms and are not toxic. The second one is oligomers with disordered structure, short lifetime, sensitive to proteinase K and biologically inert (OA). The third is oligomers of 15–30 monomers rich in β-structure. They are long-lived, resistant to proteinase K, and do not function as monomeric α‑synuclein (OB).
Although the OA and OB classes are able to bind to the cell membrane, it has been shown that nontoxic OA oligomers and toxic OB differently disrupt the integrity of the lipid bilayer membrane (Fusco et al., 2017). The authors used recombinant human amyloid AS expressed in E. coli. The isolated and purified AS fractions were added to calcein–AM-containing model vesicles with an intact lipid membrane. Membrane damage was identified from an increase in the fluorescence of calcein released from vesicles. Incubation of vesicles with OA induced a small amount of calcein released from them comparable to that caused by α-synuclein monomers and mature fibrils. At the same time, incubation of vesicles with OB resulted in a release of calcein that was ten times more intense, which indicates that OB causes significant damage to the lipid layers. These results coincided with data obtained on cell lines of human neuroblastoma and rat cortical neurons: only the OB fraction induced a high level of free calcein luminescence. It also significantly increased the amount of ROS and cell death.
The interaction of α-synuclein oligomers with the bilayer lipid membrane of the cell was studied by confocal scanning microscopy. It has been shown that OAs have a mostly disordered structure and bind exclusively to the membrane surface. Toxic OB oligomers bind to the membrane surface by folding the mobile N-terminal region into amphipathic α-helixes and penetrate into the lipid layers due to core regions rich in β-structures. In this case, the integrity of the two-layer cell membrane is violated, accompanied by significant damage to it. OB oligomers induce the entry of calcium ions into the cytoplasm from the endoplasmic reticulum or from the intercellular space. Since α-synuclein is a lipophilic protein co-localized with mitochondria, (Volles et al., 2001), excess calcium stored in mitochondria disrupts the transport of electrons in the respiratory chain and dysfunction of mitochondria triggers mitophagy (Zubova, 2019). Mitochondria are fragmented, oxidative stress occurs, and ROSs accumulate, disrupting the functions of other cellular structures. In particular, transition takes place of dopamine from vesicles to the cytoplasm, where it is highly toxic (Luth et al., 2014; Vivoli Vega et al., 2019). The accumulation of oligomers causes endoplasmic stress (Colla et al., 2012) and dysfunction of the proteostasis system, disrupting processes in the proteasome system and in the lysosomal degradation system during autophagy (Lindersson et al., 2004; Scudamore and Ciossek, 2018). The suppression of autophagy, in turn, leads to the accumulation of misfolded proteins and increases oxidative stress, with subsequent additional accumulation of ROS.
Cascella et al. (2021) showed that fibrils become sources of toxic oligomers, while long fibrils are less toxic than short ones. The authors explain this by saying that a larger proportion of them consists of small fibrils, since the “cleavage” of oligomers comes from the ends of the fibrils. Small-sized fibrils, like OB oligomers, interact with the surface of the cell membrane due to the special structure of their N-terminal region, but do not penetrate deeply into the membrane and therefore do not cause significant damage in it.
The main mechanism of α-synuclein toxicity is, thus, predominantly associated with OB oligomers that are rich in β-structures and hydrophobic regions oriented towards the lipid layers of the cell membrane, while the main role of fibrils in the pathogenesis of PD is not in damage to cell membranes, but in the fact that they serve as a source of toxic oligomers, and are also necessary for the reproduction and spreading of PD by the prion type. That is, α-synuclein aggregates act as primers, causing amyloid conversion of monomers even with the correct conformation and, thus, triggering pathological changes in recipient neurons. Distribution of α-synuclein is carried out due to exo- and endocytosis. Neurons secrete α-synuclein monomers, oligomers, and fibrils from vesicles and exosomes through calcium-dependent exocytosis (Emmanouilidou et al., 2010), and, with the help of membrane receptors or endocytosis, free fibrils bind to the plasma membrane and penetrate into the cytosol of nerve cells (Hijaz and Volpicelli_Daley., 2020).
THE ROLE OF METALS IN AMYLOIDIZATION
In a number of neurodegenerative diseases, a violation of the homeostasis of metal ions has been noted: the number of metal ions in brain cells increases up to ten times. Normally, the protective function in the cell is performed by neutral endopeptidase (NEP–Zn–metallothionein), which breaks down toxic βA oligomers, regulating the balance between them and monomers (Russo et al., 2005), while increasing the concentration of βA–metalloprotein, and copper, iron, and zinc ions act as a factor in initiating AD (Opazo et al., 2002; Li et al., 2004). A correlation was found between the concentrations of these ions in the brain, the formation of βA plaques, and an increase in oxidative stress associated with an imbalance in redox reactions in mitochondria: an increase in the concentration of metal ions in neurons causes oxidative stress, followed by accumulation of ROS, which is detrimental to the cell (Bush, 2003; Jomova et al., 2010).
One effective way to combat metal-induced toxicity can be the search for chelate ligands, which, when bound to metals, have a higher affinity for the cell membrane compared to that of the metal complex with amyloid-protein molecules. Some purine nucleotide analogs, being natural chelators, may be useful in the treatment of AD, causing disaggregation of βA and, at the same time, acting as antioxidants (Hevroni et al., 2016). Villar-Piqué et al. (2016) showed that the mutant H50-Q protein, binding to Cu2+, causes the displacement of the H50 complex with copper in the amyloid synuclein molecule. In this case, the conversion of toxic forms of the OB protein into nontoxic α-synuclein aggregates of the OA type occurs. The resulting oligomers were amorphous, did not bind to thioflavin T, and were unable to act as a seed. The structure and chelate action of some metal-containing complexes are described in detail (see review Gomes et al., 2020).
CROSS-SEEDING AND HETEROTYPIC INTERACTIONS BETWEEN AMYLOIDS
Although the mechanisms of toxicity are now largely elucidated, it remains unclear what triggers self-assembly, i.e., amyloid aggregation of proteins prone to proteinopathy, in particular, βA and α-synuclein. It is assumed most likely that it is triggered either by stress or by the concentration of monomers that has reached a critical value. It has been shown that a high concentration of monomers causes the conversion of the native protein into a protein with a disturbed conformation prone to aggregation. As a result, seeding occurs. The initial process of self-assembly is called “primary nucleation.” It occurs in the absence of formed amyloid aggregates and leads to the formation of a metastable oligomeric core, from which fibrils are then formed during elongation. The first stage of nucleation can take a long time, but, after its completion, the next stage of secondary nucleation passes quickly (Habchi et al., 2018). Secondary nucleation is a process in which mature fibrils catalyze the formation of new oligomers that act as seeds. The latter not only provide enhanced growth of fibrils, but, due to endocytosis, spread pathology among nerve cells through synapses (Wells et al., 2019).
With many neurodegenerative diseases, including AD and PD, cross-seeding plays an important role in aggregation. Seeds of one protein stimulate the nucleation of others. In recent years, heterotypic interactions between amyloids have been found to be quite common in neurodegenerative diseases, and fundamental processes such as aggregation, nucleation, and toxicity depend on them (Konstantoulea et al., 2021; Subedi et al., 2022). Recent studies have shown that heterotypic protein interactions in AD are not limited to βA with τ and PrP, but also extend to the IAPP polypeptide that causes type 2 diabetes in humans (Wang, Westermark, 2021). In patients with this disease, the chance of getting AD increases several times. In experiments in vitro in various mammalian cell lines, IAPP injections have been shown to increase aggregation βA (Bharadwaj et al., 2020) and injections of βA fibrils in type 2 diabetic transgenic mice have been shown to induce IAPP aggregation (Jackson et al., 2013).
Cross seeding, aggregation interdependence, and physical interaction of IAPP with βA on the molecular level were shown by Young et al. (2015). Using ion-mobile mass spectrometry, these authors showed the formation of heterogeneous prefibrillar structures—hetero-oligomers. A possible explanation for the heterotypic relationships of these proteins lies in the significant similarity of their primary amino-acid sequence, which is 47%, while, in certain short sections in hydrophobic regions, which are especially important for amyloid self-assembly, this similarity is even greater. The steric “zipper” effect that emerges between the β-layers of different amyloid peptides makes possible the effective cross-seeding. A short fragment -GNINQQNU- was found in the yeast prion Sup35, stimulating cross seeding both with amyloid βA and with IAPP amyloid and causing co-expression of both amyloids (Zhang Y. et al., 2021 b). The impact of cross- seeding between βA and and enhancer protein of viral immunodeficiency displaying typical features of a prion (HIV/AIDS-SEVI) was demonstrated in experiments in vivo and in vitro. Cross -seeding resulted in an inhibitory effect of SEVI on the aggregation and toxicity of βA (Tang et al., 2022b).
Much information has been accumulated on the heterotypic association of amyloids in AD and PD: Lewy bodies have been found in the brains of many patients with AD (Hashimoto and Masliah, 1999) and βA plaques have been found in the brain of patients with PD (Kalaitzakis et al., 2008). Data in vivo on human brain tissues and transgenic mice indicate greater neuronal degeneration and large defects in both cognitive and motor activity with the simultaneous presence of both amyloids (Masliah, 2001). At the same time, amyloids of different proteins interact both in cells and in the extracellular matrix, which proves the possibility of α-synuclein to be excreted from the cell and that βA can penetrate into neurons (LaFerla et al., 2007). The particular characteristic of interactions βA and α synuclein is that fibrillation βA is suppressed by monomers and oligomers of α-synuclein, although oligomerization of βA, on the contrary, stimulates them (Candreva et al., 2020).
Different cell models show co-expression of α‑synuclein and τ protein, which changes the aggregation kinetics and amyloid polymorphism of α-synuclein (Badiola et al., 2011). An interesting result was obtained by cross seeding TKEQVTNU octopeptide isolated from α-synuclein and IAPP amyloid: as a result, apoptosis of pancreatic cells was significantly reduced (Tang et al., 2022a) . The in vitro data demonstrate that if amyloid α-synuclein and PrP are in the state of co-acervates in nonmembrane organelles (NMOs), their heterologous interaction during the liquid–solid-phase transition is greatly accelerated (Agarwal et al., 2022).
A STRATEGY TO COMBAT NEURODEGENERATIVE DISEASES
To form an effective strategy to combat neurodegenerative diseases, it is important to know which molecules and processes in the cell can resist the misfolding and distribution of the amyloid protein. The cellular-protein quality-control (PQC) system solves several problems. The main one is the control of folding, refolding, and degradation with the help, first of all, of molecular chaperones, mainly Hsp70 and Hsp90, often acting together with co-chaperones (Margulis et al., 2020). It has been shown that some chaperones are involved in the processes of fibrillation and secondary nucleation. So, the heat-shock protein HSP104, binding to oligomers, protofibrils and small fibrils of βA, also suppresses their further fibrillation. Similarly, the introduction of Hsp40 and Hsp70 chaperones suppresses the maturation of fibrils required for secondary nucleation in AD and PD. A number of amyloidogenic proteins contain about 100 amino-acid domains that function as chaperones, limiting the formation of oligomers (Cohen et al., 2015). The endogenous amphipathic antimicrobial peptide LL-37 binds to the C-terminal region of α-synuclein and exhibits chaperone activity, blocking it and, thereby, preventing its penetration into the cell membrane (Santos et al., 2022). A yeast model shows the chaperone-mediated action of factors sorting misfolded inactive proteins into different intracellular deposits (Barbitoff et al., 2017).
The suppression of oligomer-induced toxicity is often associated with oligomer clusters. Clusterin binds prefibrillar forms of various proteins, including βA and α-synuclein, thereby limiting their toxicity and nucleation (Beeg et al., 2016). In some cases, the binding of the chaperone to hydrophobic sites of βA and with the surface of the neuron is more important than reducing the level of aggregation of βA (Fernandez-Funez et al., 2016). Thus, the action of some chaperones of the Hsp family consists in the fact that, when combined with the corresponding site on the amyloid molecule, they strongly change its conformation. This prevents the binding of amyloid to cellular receptor proteins and, thus, blocks the launch of further pathological processes (Wentink et al., 2019).
In addition, small molecules have been found and characterized, which, like dopamine, contain one aromatic ring (Pena-Diaz and Ventura, 2022). Unlike dopamine, which, while temporarily alleviating symptoms, does not affect the mechanisms of PD, these substances act as molecular chaperones. They effectively block aggregation, remodulating this process by the conversion of toxic oligomers into nontoxic, so-called “off-pathway aggregates.”
However, the use of chaperones can in some cases lead to negative results due to the fact that a balance between Hsp90, Hsp70, and Hsp40 is necessary for the normal activity of proteins. In addition, an excess of the concentration of chaperones, which cause fibril dissociation, can lead to the opposite result due to the formation of seeds and an increase in secondary nucleation.
A special approach to the suppression of toxicity βA is the use of monoclonal antibodies to the conformational epitope inherent in β-rich oligomers and fibrils, but not monomers. The same antibodies blocked the increase in the amount of phosphorylated τ protein (Lambert et al., 2007). A similar result was obtained when mice expressing human α-synuclein were vaccinated with monoclonal antibodies against protofibrils. Not only antibodies specific for oligomers were effective, but also peptidomimetics, which reassemble toxic oligomers, converting them into nontoxic forms (Liang et al., 2019).
In some cases, a more indirect effect on cells can lead to a decrease in toxicity. Thus, it has been shown that fatty-acid-associated cellular proteins FABP3 and FABP7 can serve as triggers for amyloidization in the case of PD (Cheng et al., 2022). They are co-localized with α-synuclein, forming complexes with it, and their induction stimulates oxidative stress, which, in turn, activates oligomerization. When cells are exposed to the ligand-modified FABP7 protein, oligomerization and cell death are dramatically reduced.
In yeast, under stress conditions, the Lsb2 protein, taking the prion form, promotes the assembly of other cellular proteins and their conversion to an aggregated state at sites associated with the cytoskeleton. In the form of such temporary deposits, proteins are stored until the stress ends and the Lsb2 prion is lost during cell division (Chernova et al., 2019).
A representative of the imidazolquinolines—imiquimod acting on certain cell receptors, has an anti-amyloid effect on yeast and higher cell cultures, specifically inhibiting the participation of ribosomes in protein assembly (Banerjee and Sanyal, 2014; Blondel et al., 2016).
In addition, nonselective degradation of protein aggregates during proteolysis during autophagy has been shown (Thellung et al., 2019). Spermidine is a semi-amine that stimulates autophagy; in yeast, it eliminates PSI+ and PIN+prions. Dimebon, blocking histamine serotonin and choline receptors, regulates lysosomal activity and ensures degradation of βA in the process of autophagy. The yeast model shows a decrease in the level of aggregated βA under the action of dimebon if the cell does not carry a mutation in the gene ATG8 necessary for the process of formation of the phagotophore (Doody et al., 2008).
The mechanisms of apoptosis, autophagy, and protein quality control are highly conserved; therefore, rapidly dividing and genetically well-studied yeast cells are a very convenient object for modeling neurodegenerative diseases (Botstein, Fink, 2011; Tenreiro et al., 2013; Chernoff et al., 2020). Most of the key chaperones that modulate protein aggregation are the same in yeast as in human beings; therefore, humanized yeast is an extremely successful model for the search for protective substances that affect different stages of pathogenesis. Many effective and simple approaches have been worked out on them, with the help of which a large number of potentially promising substances have been identified (Su et al., 2010; Faria et al., 2013; Tardiff et al., 2013; Fernandes et al., 2014).
We will present one of them that is used in several laboratories. Variants of human βA fused with a fluorescent protein (GFP, YFP, or CFP) were obtained, which, during accumulation and aggregation, provides fluorescence of intracellular inclusions. Fluorescence suppression caused by a test substance indicates that it suppresses aggregation βA. In this way, a direct effect was shown on fibrillogenesis of folic acid (the oxidized form of vitamin B9)—a substance with good anti-inflammatory activity, as well as a number of peptidomimetics obtained for the amyloidogenic site of βA (Fig.2) (Macreadie et al., 2008; Rajasekhar et al., 2015). A detailed analysis of the results obtained on yeast models is contained in a number of works (Chernova et al., 2019; Tuite, 2019). Particular promise (at least for the treatment of synucleinopathies) may be presented by the use of yeast with a sensitivity mutation to synuclein-induced toxicity (Sangkaew et al., 2022).
Yeast model for the search for substances that inhibit amyloidization. Suppression of the fluorescence of cytoplasmic inclusions caused by the test substance manifests in the absence of aggregated GFP-containing β-amyloid molecules in the cells and, thus, serves as an indicator of its anti-amyloid activity.
Among patients with PD, about 15% of cases are related to familial or hereditary forms of the disease caused by mutations in the α-synuclein gene. Thus, the S129 mutation, causing phosphorylation and providing better binding of fibrillar synuclein to the cell membrane, significantly increases the distribution of aberrant synuclein and its pathological consequences (Zhang S. et al., 2021a). Similar mechanisms of aggregation and nucleation in the A30 and A50 mutants and the manifestations of toxicity caused by them are effectively studied in animal models—nematode C. elegans (A30 and A50) and fruit fly D. melanogaster (Mizuno et al., 2010; Perni et al., 2021). Models created using mutant lines are promising for finding remedies for hereditary PD variants.
NMOs (which are also biological condensates) often serve as the center for the formation of amyloid and amyloid-like fibrils (Li and Liu, 2022; Simonsen and Wollert, 2022). NMOs consist of a triacylglycerol core (TAG) and esters of sterol (ESs) surrounded by a phospholipid layer and form as temporary structures between the membranes of the endoplasmic reticulum (Choudhary et al., 2015). In these organelles, phase separation or liquid-to-liquid phase transition occurs. As a result, due to dehydration, the interactions between the solvent and dissolved molecules within a homogeneous system change, i.e., the interaction between the macromolecule and water is replaced by the interaction between the macromolecules themselves (Koopman et al., 2022). A number of studies have shown that 40% of proteins undergo phase separation and such proteins often contain domains with a disordered structure (intrinsically disordered regions, IDRs) (Vernon et al., 2018; Hardenberg et al., 2020). The links of these domains through short sites with a certain set of amino acids form NMOs.
Phase transitions can lead to abnormal protein aggregation underlying many neurodegenerative pathologies such as PD, amyotrophic lateral sclerosis, frontal temporal dementia, and a number of tauopathies (Li and Liu, 2022). However, NMOs are also used by the cell to control proteostasis, namely, selective autophagy responsible for the degradation of misfolded proteins. Which process will prevail—aggregation of fibrils or their degradation during autophagy—depends on the state of autophagy receptors or other proteins involved in the synthesis of NMO and TAG components, as well as on the molecular chaperones incorporated into NMOs (Schepers and Behl, 2021).
Ubiquitin-dependent and -independent receptors are membrane proteins activated by stress or dysfunction of cell organelles. They contain an interactive site with a disordered structure, due to which they are associated with the Atg8 protein. Receiving energy from NMOs, Atg8 triggers the formation of an autophagophore. After elongation, the mature autophagosome, together with cargo (spoiled protein), is delivered to the lysosome, fuses with it, and undergoes degradation (Jacquier et al., 2011;). In the process of selective autophagy, the interaction of autophagic receptors with the central (core) regions of autophagy-controlling proteins ensures the synthesis of autophagosomal membranes (Simonsen and Wollert, 2022).
Synthesis of ESs is carried out with the help of two membrane proteins of the endoplasmic reticulum—Are1 and Are2. The yeast model showed that their absence leads to a reduction in autophagic degradation activity. The presence of ergosterol in the membranes of the endoplasmic reticulum restored vacuolar activity (Hurst and Fratti, 2020). Some NMO-localized lipases degrade TAG and ES, while others play an essential role in autophagy (Tanguy et al., 2019).
NMOs arise as temporary formations in response to the actions of various exogenous and endogenous factors. Molecular chaperones intercalating into NMOs regulate their dynamic assembly and stability. Some chaperones switch their activity and, through post-translational modifications, prevent or stimulate phase transitions (Li and Liu, 2022). In addition to chaperones, single- and double-stranded DNA, RNA, and small RNAs act. They modulate phase separation and phase transition by inducing, for example, the conversion of PrP to the prion form. At the same time, antisense oligonucleotides acting on PrP protein RNA increase the lifespan of an infected animal and, thus, can serve as a potential remedy for prion diseases (Silva et al., 2022).
THE MOST PROMISING ANTIAMYLOID SUBSTANCES NATURAL AND MULTIDIRECTIONAL IN THEIR ACTION
Particular interest from the point of view of therapy is presented by natural products—naturally occurring organic molecules that can effectively modulate protein aggregation (Ashrafian et al., 2021). Two natural products belonging to the class of aminosterols—squalamine and troduskvemin—can modulate aggregation of βA and α-synuclein, changing the physicochemical properties of oligomers and suppressing toxicity in neuroblastoma cells. The mechanism of toxicity suppression is associated with the chelate displacement of amyloid aggregates from the cell membrane in the presence of zinc ions (Perni et al., 2018; Limbocker et al., 2021).
Natural compounds whose structure includes one or more phenolic rings actively inhibit aggregation of βA, and some of them also inhibit aggregation of α‑synuclein. Due to the peculiarity of the structure of the phenol ring, they form noncovalent bonds with β‑layers that are common to all amyloidogenic structures.
The original two-step system for searching for inhibitors of α-synuclein aggregation is given by Hideshima et al. (2022). At the first stage, these authors transformed HeLa cells with a prefibrillar α-synuclein isoform labeled with a fluorescent protein. Cells were stained with thioflavin T, which made it possible to judge the degree of amyloidization, and cell-based assays were performed at the second stage. As a result of this screening, the substances were evaluated for their ability to inhibit fibrillation without inhibiting cell survival. Out of the 1262 low-molecular-weight substances approved for use in medicine, the authors selected seven compounds, among which thiamic acid containing a phenol ring turned out to be the most promising. Testing of thiamic acid was successfully carried out in experiments in vitro on widely used models—mouse neurons and nematode C. elegans muscle cells (Hideshima et al., 2022).
On the whole, polyphenol rings effectively suppress the nucleation and elongation of aggregates by interacting with aromatic amino-acid residues. These substances are found in berries, nuts, red wine, and green tea. A wide range of polyphenols reduce oxidative stress by binding metal ions. The antioxidant activity of polyphenols such as queritin, cathetin, and rutin is due to the chelation of Fe3+, Cu2+, and Zn2+ ions, which, in associating with the aggregated form of βA, induce the formation of free radicals. Resveratrol, which is found in grapes and red wine, binds to the N-terminus of βA, preventing further oligomerization. Its effect on proteasome activity has also been shown (Beldona et al., 2022). Polyphenols carry out enhanced positive regulation of such cellular antioxidant enzymes as catalase, glutathione peroxidase, and superoxide dismutase.
Among natural polyphenols, catechins are worth noting. They effectively suppress the formation of the PrP prion, and also change the way the APP precursor is cleaved by the type of nonamyloidogenic hydrolysis. Among them, a unique compound isolated from green tea, epigalocatechin gallate (EGCG), was found, which has multiple neuroprotective effects well studied on amyloid βA (Youn et al., 2022). EGCG directs precursor proteolysis of βA along the nonamyloidogenic pathway, thereby blocking the formation of toxic oligomers. In addition, EGCG binds directly to mature fibrils and transforms them into amorphous nontoxic aggregates. In this case, the dissociation of fibrils into monomers and oligomers does not occur (Gauci et al., 2011; Grelle et al., 2011; Palhano et al., 2013). EGCG also stimulates monomer aggregation of βA, turning it into a nonstructurable and nontoxic oligomer (Ehrnhoefer et al., 2008).
It has been shown that EGCG can transform dense fibrillar structures of βA–Cu2+complexes, turning them into globular aggregates with inaccessible free ends (Tavanti et al., 2020). In this case, EGCG has a chelating effect due to the fact that the central (core) region βA possesses higher affinity to it than the complex with copper. EGCG acts as a molecular chaperone and, in the case of PD, directs the formation of oligomers along a nontoxic pathway (Hardenberg et al., 2021). Cellular models have shown that EGCG forms intermolecular hydrogen bonds with IAPP and βA, and it turns out to be highly effective in suppressing IAPP–βA heteroaggregates, reducing their co-aggregation and cytotoxicity (Adem et al., 2022).
In a previous review, we presented our own data on the multidirectional anti-amyloid action of another natural compound, red pigment (RP), produced by Saccharomycetes yeasts mutated in genes ADE1and ADE2 (Nevzglyadova et al., 2022). This substance, a polymerization product of aminoimidazole ribotide, was studied by us in experiments in vitro and in vivo. RP significantly reduces the amount of both native yeast amyloids themselves, which increases with age, and aggregated proteins of βA and human α-synuclein expressed in yeast. In model experiments with the growth of fibrils of insulin, lysozyme, and βA, RP almost completely suppresses their growth at the prefibrillar stage, contributing to the formation of stable conglomerates. In RP-accumulating yeasts, the aggregated fraction of lysates did not contain prion-dependent proteins, which include some chaperones involved in seeding induction and distribution. We demonstrated the ability of RP to change the structure of toxic aggregates using FRAP analysis of yeast cells expressing α-synuclein–GFP (Nevzglyadova et al., 2022). In cells grown in the presence of RP, the survival rate increased and the proportion of cell inclusions with high diffusion, the ones most mobile and fully restored after laser irradiation, decreased, and a new fraction of inclusions appeared, which practically did not restore luminescence. This composition of cytoplasmic inclusions can be explained by the fact that, under the action of RP, dense β-layers of toxic oligomers are transformed into a disordered structure, and the emerging nontoxic aggregates form stable conglomerates similar to those that arise under the action of EGCG.
It is generally accepted that neuronal death in AD and PD occurs due to oxidative stress and accumulation of ROS. We have shown that, in the presence of RP, ROS accumulation practically does not occur. The protective effect of RP was confirmed in experiments on transgenic Drosophila lines expressing βA proteins and human α-synuclein. These models made it possible to see the relationship between changes caused by RP in brain cells and improvement in behavioral indicators: memory in AD and motor activity in PD.
It should be noted that the difficulty in finding an effective therapy for neuronal degradation is that it occurs as a result of a whole cascade of processes occurring both inside and outside the cell. Strategies for the treatment of neurodegenerative diseases associated with the modulation of the mechanisms of fibrillogenesis can lead to significant complications in the medium and long-term stages of treatment. For example, attempts at therapy with fibril-growth inhibitors do not lead to the desired result in medium-term studies, because a small amount of toxic oligomers are enough to trigger further pathological processes. In addition, direct destruction of amyloid deposits (for example, when using specific antibodies) can cause serious complications, because as a result of fibril decay, toxic oligomers are formed that act as a seed for secondary nucleation. Therefore, we believe that a further search for compounds with a multifunctional effect, as well as substances that suppress aggregation at the earliest stage and/or transform oligomers into a nontoxic state, has the greatest chance of leading to positive results.
CONCLUSIONS
In works of recent years, the most significant issue is the decoding of the cascade mechanism underlying neurodegeneration, including such widespread diseases as Alzheimer’s and Parkinson’s diseases. The links of this cascade include the reactions of βA and α‑synuclein with membrane receptors, as well as modifications of aggregation by phase separation and heterotypic interactions with other cellular amyloids. It is noteworthy that nontoxic variants incapable of aggregation were found among the class of soluble oligomers considered to be triggers of the neurodegeneration process. It has been shown that natural polyfunctional substances that support the selection of nontoxic oligomers are especially promising for therapy.
REFERENCES
Adem, K., Shanti, A., Srivastava, A., Homouz, D., Thomas, S.A., Khair, M., Stefanini, C., Chan, V., Kim, T.Y., and Lee, S., Linking Alzheimer’s disease and type 2 diabetes: characterization and inhibition of cytotoxic Aβ and IAPP hetero-aggregates, Front. Mol. Biosci., 2022, vol. 9, p. 842582. https://doi.org/10.3389/fmolb.2022.842582
Agarwal, A., Arora, L., Rai, S.K., Avni, A., and Mukhopadhyay, S., Spatiotemporal modulations in heterotypic condensates of prion and α-synuclein control phase transitions and amyloid conversion, Nat. Commun., 2022, vol. 13, p. 1. https://doi.org/10.1038/s41467-022-28797-5
Alam, P., Bousset, L., Melki, R., and Otzen, D.E., α-Synuclein oligomers and fibrils: a spectrum of species, a spectrum of toxicities, J. Neurochem., 2019, vol. 150, p. 522. https://doi.org/10.1111/jnc.14808
Ashrafian, H., Zadeh, E.H., and Khan, R.H.,Review on Alzheimer’s disease: inhibition of amyloid beta and tau tangle formation, Int. J. Biol. Macromol., 2021, vol. 167, p. 382. https://doi.org/10.1016/j.ijbiomac.2020.11.192
Baba, M., Nakajo, S., Tu, P.H., Tomita, T., Nakaya, K., Lee, V.M., Trojanowski, J.Q., and Iwatsubo, T., Aggregation of alpha-synuclein in Lewy bodies of sporadic Parkinson’s disease and dementia with Lewy bodies, Am. J. Pathol., 1998, vol. 152, p. 879.
Badiola, N., de Oliveira, R.M., Herrera, F., Guardia-Laguarta, C., Gonçalves, S.A., Pera, M., Suárez-Calvet, M., Clarimon, J., Outeiro, T.F., and Lleó, A., Tau enhances α-synuclein aggregation and toxicity in cellular models of synucleinopathy, PLoS One, 2011, vol. 6, p. e26609. https://doi.org/10.1371/journal.pone.0026609
Banerjee, D. and Sanyal, S., Protein folding activity of the ribosome (PFAR)—a target for antiprion compounds, Viruses, 2014, vol. 6, p. 3907. https://doi.org/10.3390/v6103907
Barbier, P., Zejneli, O., Martinho, M., Lasorsa, A., Belle, V., Smet-Nocca, C., Tsvetkov, P.O., Devred, F., and Landrieu, I., Role of Tau as a microtubule-associated protein: structural and functional aspects, Front. Aging Neurosci., 2019, vol. 11, p. 204. https://doi.org/10.3389/fnagi.2019.00204
Barbitoff, Y.A., Matveenko, A.G., Moskalenko, S.E., Zemlyanko, O.M., Newnam, G.P., Patel, A., Chernova, T.A., Chernoff, Y.O., and Zhouravleva, G.A., To CURe or not to CURe? Differential effects of the chaperone sorting factor Cur1 on yeast prions are mediated by the chaperone Sis1, Mol. Microbiol., 2017, vol. 105, p. 242. https://doi.org/10.1111/mmi.13697
Beeg, M., Stravalaci, M., Romeo, M., Carrá, A.D., Cagnotto, A., Rossi, A., Diomede, L., Salmona, M., and Gobbi, M.,Clusterin binds to Aβ1-42 oligomers with high affinity and interferes with peptide aggregation by inhibiting primary and secondary nucleation, J. Biol. Chem., 2016, vol. 291, p. 6958. https://doi.org/10.1074/jbc.M115.689539
Beldona, V., Patel, A., Patel, K., Abraham, N., Halvor-sen, A., Liu, A., Mannem, N., and Renganathan, G.,Natural product polyphenol inhibition of amyloid-β aggregation, J. High School Sci., 2022, vol. 32281. http://jhss.scholasticahq.com.
Bennett, R.E., DeVos, S.L., Dujardin, S., Corjuc, B., Gor, R., Gonzalez, J., Roe, A.D., Frosch, M.P., Pitstick, R., Carlson, G.A., and Hyman, B.T., Enhanced tau aggregation in the presence of amyloid β, Am. J. Pathol., 2017, vol. 187, p. 1601. https://doi.org/10.1016/j.ajpath.2017.03.011
Bharadwaj,P., Solomon, T., Sahoo, B.R., Ignasiak, K., Gaskin, S., Rowles, J., Verdile, G., Howard, M.J., Bond, C.S., Ramamoorthy, A., Martins, R.N., and Newsholme, P., Amylin and beta amyloid proteins interact to form amorphous heterocomplexes with enhanced toxicity in neuronal cells, Sci. Rep., 2020, vol. 10, p. 10356. https://doi.org/10.1038/s41598-020-66602-9
Blondel, M., Soubigou, F., Evrard, J., Nguyen, P.H., Hasin, N., Chédin, S., Gillet, R., Contesse, M.A., Friocourt, G., Stahl, G., Jones, G.W., and Voisset, C., Protein folding activity of the ribosome is involved in yeast prion propagation, Sci. Rep., 2016, vol. 6, p. 32117. https://doi.org/10.1038/srep32117
Botstein, D. and Fink, G.R., Yeast: an experimental organism for 21st century biology, Genetics, 2011, vol. 189, p. 695. https://doi.org/10.1534/genetics.111.130765
Braak, H., Alafuzoff, I., Arzberger, T., Kretzschmar, H., and Del Tredici, K.,Staging of Alzheimer disease-associated neurofibrillary pathology using paraffin sections and immunocytochemistry, Acta Neuropathol., 2006, vol. 112, p. 389. https://doi.org/10.1007/s00401-006-0127-z
Bush, A.I., The metallobiology of Alzheimer’s disease, Trends Neurosci., 2003, vol. 26, p. 207. https://doi.org/10.1016/S0166-2236(03)00067-5
Candreva, J., Chau, E., Rice, M.E., and Kim, J.R., Interactions between soluble species of β-Amyloid and α-Synuclein promote oligomerization while inhibiting fibrillization, Biochemistry, 2020, vol. 59, p. 425. https://doi.org/10.1021/acs.biochem.9b00655
Cascella, R., Chen, S.W., Bigi, A., Camino, J.D., Xu, C.K., Dobson, C.M., Chiti, F., Cremades, N., and Cecchi, C., The release of toxic oligomers from α-synuclein fibrils induces dysfunction in neuronal cells, Nat. Commun., 2021, vol. 12, p. 1814. https://doi.org/10.1038/s41467-021-21937-3
Cascella, R., Bigi, A., Cremades, N., and Cecchi, C., Effects of oligomer toxicity, fibril toxicity and fibril spreading in synucleinopathies, Cell Mol. Life Sci., 2022, vol. 79, p. 174. https://doi.org/10.1007/s00018-022-04166-9
Cheng, A., Wang, Y.F., Shinoda, Y., Kawahata, I., Yamamoto, T., Jia, W.B., Yamamoto, H., Mizobata, T., Kawata, Y., and Fukunaga, K.,Fatty acid-binding protein 7 triggers α-synuclein oligomerization in glial cells and oligodendrocytes associated with oxidative stress, Acta Pharmacol. Sin., 2022, vol. 43, p. 552. https://doi.org/10.1038/s41401-021-00675-8
Chernova, T.A., Chernoff, Y.O., and Wilkinson, K.D., Yeast models for amyloids and prions: environmental modulation and drug discovery, Molecules, 2019, vol. 24, p. 3388. https://doi.org/10.3390/molecules24183388
Chernoff, Y.O., Grizel, A.V., Rubel, A.A., Zelinsky, A.A., Chandramowlishwaran, P., and Chernova, T.A., Application of yeast to studying amyloid and prion diseases, Adv. Genet., 2020, vol. 105, p. 293. https://doi.org/10.1016/bs.adgen.2020.01.002
Choudhary, V., Ojha, N., Golden, A., and Prinz, W.A., A conserved family of proteins facilitates nascent lipid droplet budding from the ER, J. Cell Biol., 2015, vol. 211, p. 261. https://doi.org/10.1083/jcb.201505067
Cohen, S.I.A., Arosio, P., Presto, J., Kurudenkandy, F.R., Biverstal, H., Dolfe, L., Dunning, C., Yang, X., Frohm, B., Vendruscolo, M., Johansson, J., Dobson, C.M., Fisahn, A., Knowles, T.P.J., and Linse, S., A molecular chaperone breaks the catalytic cycle that generates toxic Aβ-oligomers, Nat. Struct. Mol. Biol., 2015, vol. 22, p. 207. https://doi.org/10.1038/nsmb.2971
Colla, E., Coune, P., Liu, Y., Pletnikova, O., Tronco-so, J.C., Iwatsubo, T., Schneider, B.L., and Lee, M.K., Endoplasmic reticulum stress is important for the manifestations of α-synucleinopathy in vivo, J. Neurosci., 2012, vol. 32, p. 3306. https://doi.org/10.1523/JNEUROSCI.2617-07.2007
Desplats, P., Lee, H.J., Bae, E.J., Patrick, C., Rockenstein, E., Crews, L., Spencer, B., Masliah, E., and Lee, S.J., Inclusion formation and neuronal cell death through neuron-to-neuron transmission of alpha-synuclein, Proc. Natl. Acad. Sci. U. S. A., 2009, vol. 106, p. 13010. https://doi.org/10.1073/pnas.0903691106
Doody, R.S., Gavrilova, S.I., Sano, M., Thomas, R.G., Aisen, P.S., Bachurin, S.O., Seely, L., Hung, D., and Dimebon, I., Effect of dimebon on cognition, activities of daily living, behaviour, and global function in patients with mild-to-moderate Alzheimer’s disease: a randomised, double-blind, placebo-controlled study, Lancet, 2008, vol. 372, p. 207. https://doi.org/10.1016/S0140-6736(08)61074-0
Dujardin, S., Bégard, S., Caillierez, R., Lachaud, C., Delattre, L., Carrier, S., Loyens, A., Galas, M.-C., Bousset, L., Melki, R., Auregan, G., Hantraye, P., Brouillet, E., Buee, L., and Colin, M., Ectosomes: a new mechanism for non-exosomal secretion of Tau protein, PLoS One, 2014, vol. 9, p. e100760. https://doi.org/10.1371/journal.pone.0100760
Ehrnhoefer, D.E., Bieschke, J., Boeddrich, A., Herbst, M., Masino, L., Lurz, R., Engemann, S., Pastore, A., and Wanker, E.E.,EGCG redirects amyloidogenic polypeptides into unstructured, off-pathway oligomers, Nat. Struct. Mol. Biol., 2008, vol. 15, p. 558. https://doi.org/10.1038/nsmb.1437
Emmanouilidou, E., Melachroinou, K., Roumeliotis, T., Garbis, S.D., Ntzouni, M., Margaritis, L.H., Stefanis, L., and Vekrellis, K., Cell-produced alpha-synuclein is secreted in a calcium-dependent manner by exosomes and impacts neuronal survival, J. Neurosci., 2010, vol. 30, p. 6838. https://doi.org/10.1523/JNEUROSCI.5699-09.2010
Faria, C., Jorge, C.D., Borges, N., Tenreiro, S., Outeiro, T.F., and Santos, H., Inhibition of formation of α-synuclein inclusions by mannosyl glycerate in a yeast model of Parkinson’s disease, Biochim. Biophys. Acta, 2013, vol. 1830, p. 4065. https://doi.org/10.1016/j.bbagen.2013.04.015
Fernandes, J.T., Tenreiro, S., Gameiro, A., Chu, V., Outeiro, T.F., and Conde, J.P., Modulation of α-synuclein toxicity in yeast using a novel microfluidic-based gradient generator, Lab. Chip, 2014, vol. 14, p. 3949. https://doi.org/10.1039/C4LC00756E
Fernandez-Funez, P., Sanchez-Garcia, J., de Mena, L., Zhang, Y., Levites, Y., Khare, S., Golde, T.E., and Rincon-Limas, D.E.,Holdase activity of secreted Hsp70 masks amyloid-β42 neurotoxicity in Drosophila, Proc. Natl. Acad. Sci. U. S. A., 2016, vol. 113, p. E5212. https://doi.org/10.1073/pnas.1608045113
Franić, D., Zubčić, K., and Boban, M., Nuclear ubiquitin-proteasome pathways in proteostasis maintenance, Biomolecules, 2021, vol. 4, p. 54. https://doi.org/10.3390/biom11010054
Fusco, G., Chen, S.W., Williamson, P.T.F., Cascella, R., Perni, M., Jarvis, J.A., Cecchi, C., Vendruscolo, M., Chiti, F., Cremades, N., Ying, L., Dobson, C.M., and De Simone, A., Structural basis of membrane disruption and cellular toxicity by α-synuclein oligomers, Science, 2017, vol. 358, p. 1440. https://doi.org/10.1126/science.aan6160
Gauci, A.J., Caruana, M., Giese, A., Scerri, C., and Vassallo, N.,Identification of polyphenolic compounds and black tea extract as potent inhibitors of lipid membrane destabilization by Aβ42 aggregates, J. Alzheimers Dis., 2011, vol. 27, p. 767. https://doi.org/10.3233/JAD-2011-111061
Gomes, L.M.F., Bataglioli, J.C., and Storr, T.,Metal complexes that bind to the amyloid-β peptide of relevance to Alzheimer’s disease, Coordinat. Chem. Rev., 2020, vol. 412, p. 213255. https://doi.org/10.1016/j.ccr.2020.213255
Grelle, G., Otto, A., Lorenz, M., Frank, R.F., Wanker, E.E., and Bieschke, J.,Black tea theaflavins inhibit formation of toxic amyloid-beta and alpha-synuclein fibrils, Biochemistry, 2011, vol. 50, p. 10624. https://doi.org/10.1021/bi2012383
Habchi, J., Chia, S., Galvagnion, C., Michaels, T.C.T., Bellaiche, M.M.J., Ruggeri, F.S., Sanguanini, M., Idini, I., Kumita, J.R., Sparr, E., Linse, S., Dobson, C.M., Knowles, T.P.J., and Vendruscolo, M., Cholesterol catalyses Aβ42 aggregation through a heterogeneous nucleation pathway in the presence of lipid membranes, Nat. Chem., 2018, vol. 10, p. 673. https://doi.org/10.1038/s41557-018-0031-x
Hachiya N., Fułek M., Zajączkowska K., Kurpas D., Trypka E., Leszek J. 2021. Cellular prion protein and amyloid-β oligomers in Alzheimer’s disease – there are connections? Preprints. 2021050032. https://doi.org/10.20944/preprints202105.0032.v1
Hamano, T., Hayashi, K., Shirafuji, N., and Nakamoto, Y., The implications of autophagy in Alzheimer’s disease, Curr. Alzheimer Res., 2018, vol. 15, p. 1283. https://doi.org/10.2174/1567205015666181004143432
Hardenberg,M., Horvath, A., Ambrus, V., Fuxreiter, M., and Vendruscolo, M.,Widespread occurrence of the droplet state of proteins in the human proteome, Proc. Natl. Acad. Sci. U. S. A., 2020, vol. 117, p. 33254. https://doi.org/10.1073/pnas.2007670117
Hardenberg, M.C., Sinnige, T., Casford, S., Dada, S.T., Poudel, C., Robinson, E.A., Fuxreiter, M., Kaminksi, C.F., Kaminski Schierle, G.S., Nollen, E.A.A., Dobson, C.M., and Vendruscolo, M., Observation of an α-synuclein liquid droplet state and its maturation into Lewy body-like assemblies, J. Mol. Cell Biol., 2021, vol. 13, p. 282. https://doi.org/10.1093/jmcb/mjaa075
Hashimoto, M. and Masliah, E., Alpha-synuclein in Lewy body disease and Alzheimer’s disease, Brain Pathol., 1999, vol. 9, p. 707. https://doi.org/10.1111/j.1750-3639.1999.tb00552.x
Hevroni, B.L., Major, D.T., Dixit, M., Mhashal, A.R., Das, S., and Fischer, B., Nucleoside-2′, 3′/3′, 5′-bis (thio) phosphate antioxidants are also capable of disassembly of amyloid beta 42-Zn (ii)/Cu (ii) aggregates via Zn (ii)/Cu (ii)-chelation, Org. Biomol. Chem., 2016, vol. 14, p. 4640. http://goi.org/10/1039/C6OB00613B
Hideshima, M., Kimura, Y., Aguirre, C., Kakuda, K., Takeuchi, T., Choong, C.J., Doi, J., Nabekura, K., Yamaguchi, K., Nakajima, K., Baba, K., Nagano, S., Goto, Y., Nagai, Y., Mochizuki, H., and Ikenaka, K., Two-step screening method to identify α-synuclein aggregation inhibitors for Parkinson’s disease, Sci. Rep., 2022, vol. 12, p. 351. https://doi.org/10.1038/s41598-021-04131-9
Hijaz, B.A. and Volpicelli-Daley, L.A.,Initiation and propagation of α-synuclein aggregation in the nervous system, Mol.Neurodegener., 2020, vol. 15, p. 19. https://doi.org/10.1186/s13024-020-00368-6
Hillen, H.,The beta amyloid dysfunction (BAD) hypothesis for Alzheimer’s disease, Front. Neurosci., 2019, vol. 13, p. 1154. https://doi.org/10.3389/fnins.2019.01154
Hurst, L.R. and Fratti, R.A.,Lipid rafts, sphingolipids, and ergosterol in yeast vacuole fusion and maturation, Front. Cell Dev. Biol., 2020, vol. 8, p. 539. https://doi.org/10.3389/fcell.2020.00539
Jackson, K., Barisone, G.A., Diaz, E., Jin, L.W., DeCarli, C., and Despa, F.,Amylin deposition in the brain: a second amyloid in Alzheimer disease?,Ann. Neurol., 2013, vol. 74, p. 517. https://doi.org/10.1002/ana.23956
Jacobs, H.I.L., Hedden, T., Schultz, A.P., Sepulcre, J., Perea, R.D., Amariglio, R.E., Papp, K.V., Rentz, D.M., Sperling, R.A., and Johnson, K.A., Structural tract alterations predict downstream tau accumulation in amyloid-positive older individuals, Nat.Neurosci., 2018, vol. 21, p. 424. https://doi.org/10.1038/s41593-018-0070-z
Jacquier, N., Choudhary, V., Mari, M., Toulmay, A., Reggiori, F., and Schneiter, R.,Lipid droplets are functionally connected to the endoplasmic reticulum in Saccharomyces cerevisiae, J. Cell Sci., 2011, vol. 124, p. 2424. https://doi.org/10.1242/jcs.076836
Jomova, K., Vondrakova, D., Lawson, M., and Valko, M., Metals, oxidative stress and neurodegenerative disorders, Mol. Cell Biochem., 2010, vol. 345, p. 91. https://doi.org/10.1007/s11010-010-0563-x
Kalaitzakis, M.E., Graeber, M.B., Gentleman, S.M., and Pearce, R.K., Striatal beta-amyloid deposition in Parkinson disease with dementia, J. Neuropathol. Exp. Neurol., 2008, vol. 67, p. 155. https://doi.org/10.1097/NEN.0b013e31816362aa
Kieran, D., Hafezparast, M., Bohnert, S., Dick, J.R., Martin, J., Schiavo, G., Fisher, E.M., and Greensmith, L.,A mutation in dynein rescues axonal transport defects and extends the life span of ALS mice, J. Cell Biol., 2005, vol. 169, p. 561. https://doi.org/10.1083/jcb.200501085
König, A.S., Rösener, N.S., Gremer, L., Tusche, M., Flender, D., Reinartz, E., Hoyer, W., Neudecker, P., Willbold, D., and Heise, H.,Structural details of amyloid β oligomers in complex with human prion protein as revealed by solid-state MAS NMR spectroscopy, J. Biol. Chem., 2021, vol. 296, p. 100499. https://doi.org/10.1016/j.jbc.2021.100499
Konstantoulea, K., Louros, N., Rousseau, F., and Schymkowitz, J., Heterotypic interactions in amyloid function and disease, FEBS J., 2021, vol. 289, p. 2025. https://doi.org/10.1111/febs.15719
Koopman, M.B., Ferrari, L., and Rüdiger, S.G.D., How do protein aggregates escape quality control in neurodegeneration?,Trends Neurosci., 2022, vol. 45, p. 257. https://doi.org/10.1016/j.tins.2022.01.006
LaFerla, F.M., Green, K.N., and Oddo, S., Intracellular amyloid-beta in Alzheimer’s disease, Nat. Rev. Neurosci., 2007, vol. 8, p. 499. https://doi.org/10.1038/nrn2168
Lambert, M.P., Velasco, P.T., Chang, L., Viola, K.L., Fernandez, S., Lacor, P.N., Khuon, D., Gong, Y., Bigio, E.H., Shaw, P., De Felice, F.G., Krafft, G.A., and Klein, W.L., Monoclonal antibodies that target pathological assemblies of Abeta, J. Neurochem., 2007, vol. 100, p. 23. https://doi.org/10.1111/j.1471-4159.2006.04157.x
Li, D. and Liu, C.,Spatiotemporal dynamic regulation of membraneless organelles by chaperone networks, Trends Cell. Biol., 2022, vol. 32, p. 1. https://doi.org/10.1016/j.tcb.2021.08.004
Li, F., Calingasan, N.Y., Yu, F., Mauck, W.M., Toidze, M., Almeida, C.G., Takahashi, R.H., Carlson, G.A., Flint Beal, M., Lin, M.T., and Gouras, G.K., Increased plaque burden in brains of APP mutant MnSOD heterozygous knockout mice, J. Neurochem., 2004, vol. 89, p. 1308. https://doi.org/10.1111/j.1471-4159.2004.02455.x
Liang, C., Savinov, S.N., Fejzo, J., Eyles, S.J., and Chen, J., Modulation of amyloid-β42 conformation by small molecules through nonspecific binding, J. Chem. Theory Comput., 2019, vol. 15, p. 5169. https://doi.org/10.1021/acs.jctc.9b00599
Limbocker, R., Staats, R., Chia, S., Ruggeri, F.S., Mannini, B., Xu, C.K., Perni, M., Cascella, R., Bigi, A., Sasser, L.R., Block, N.R., Wright, A.K., Kreiser, R.P., Custy, E.T., Meisl, G., et al., Squalamine and its derivatives modulate the aggregation of amyloid-β and α-synuclein and suppress the toxicity of their oligomers, Front. Neurosci., 2021, vol. 15, p. 680026. https://doi.org/10.3389/fnins.2021.680026
Lindersson, E., Beedholm, R., Højrup, P., Moos, T., Gai, W., Hendil, K.B., and Jensen, P.H., Proteasomal inhibition by alpha-synuclein filaments and oligomers, J. Biol. Chem., 2004, vol. 279, p. 12924.
Lorenzen, N., Nielsen, S.B., Yoshimura, Y., Vad, B.S., Andersen, C.B., Betzer, C., Kaspersen, J.D., Christian-sen, G., Pedersen, J.S., Jensen, P.H., Mulder, F.A., and Otzen, D.E., How epigallocatechin gallate can inhibit α-synuclein oligomer toxicity in vitro, J. Biol. Chem., 2014, vol. 289, p. 21299. https://doi.org/10.1074/jbc.M114.554667
Luth, E.S., Stavrovskaya, I.G., Bartels, T., Kristal, B.S., and Selkoe, D.J., Soluble, prefibrillar α-synuclein oligomers promote complex I-dependent, Ca2(+)-induced mitochondrial dysfunction, J. Biol. Chem., 2014, vol. 289, p. 21490. https://doi.org/10.1074/jbc.M113.545749
Macreadie, I., Lotfi-Miri, M., Mohotti, S., Shapira, D., Bennett, L., and Varghese, J., Validation of folate in a convenient yeast assay suited for identification of inhibitors of Alzheimer’s amyloid-β aggregation, J. Alzheimers Dis., 2008, vol. 15, p. 391. https://doi.org/10.3233/JAD-2008-15305
Margulis, B., Tsimokha, A., Zubova, S., and Guzhova, I., Molecular chaperones and proteolytic machineries regulate protein homeostasis in aging cells, Cells, 2020, vol. 9, p. 1308. https://doi.org/10.3390/cells9051308
Masliah, E., Recent advances in the understanding of the role of synaptic proteins in Alzheimer’s disease and other neurodegenerative disorders, J. Alzheimers Dis., 2001, vol. 3, p. 121. https://doi.org/10.3233/jad-2001-3117
Mizuno, H., Fujikake, N., Wada, K., and Nagai, Y., α-Synuclein transgenic Drosophila as a model of Parkinson’s disease and related synucleinopathies, Parkinsons Dis., 2010, vol. 2011, p. 212706. https://doi.org/10.4061/2011/212706
Nevzglyadova, O.V., Mikhailova, E.V., and Soidla, T.R., Yeast red pigment, protein aggregates, and amyloidoses: a review, Cell Tissue Res., 2022, vol. 388, p. 211. https://doi.org/10.1007/s00441-022-03609-w
Niewiadomska, G., Niewiadomski, W., Steczkowska, M., and Gasiorowska, A., Tau oligomers neurotoxicity, Life (Basel), 2021, vol. 11, p. 28. https://doi.org/10.3390/life11010028
Nygaard, H.B., van Dyck, C.H., and Strittmatter, S.M., Fyn kinase inhibition as a novel therapy for Alzheimer’s disease, Alzheimers Res. Ther., 2014, vol. 6, p. 8. https://doi.org/10.1186/alzrt238
Opazo, C., Huang, X., Cherny, R.A., Moir, R.D., Roher, A.E., White, A.R., Cappai, R., Masters, C.L., Tanzi, R.E., Inestrosa, N.C., and Bush, A.I., Metalloenzyme-like activity of Alzheimer’s disease beta-amyloid. Cu-dependent catalytic conversion of dopamine, cholesterol, and biological reducing agents to neurotoxic H(2)O(2), J. Biol. Chem., 2002, vol. 277, p. 40302. https://doi.org/10.1074/jbc.M206428200
Palhano, F.L., Lee, J., Grimster, N.P., and Kelly, J.W.,Toward the molecular mechanism(s) by which EGCG treatment remodels mature amyloid fibrils, J. Am. Chem. Soc., 2013, vol. 135, p. 7503. https://doi.org/10.1021/ja3115696
Paslawski, W., Mysling, S., Thomsen, K., Jørgensen, T.J., and Otzen, D.E., Co-existence of two different α-synuclein oligomers with different core structures determined by hydrogen/deuterium exchange mass spectrometry, Angew. Chem. Int. Ed. Engl., 2014, vol. 53, p. 7560. https://doi.org/10.1002/anie.201400491
Pena-Diaz, S. and Ventura, S., One ring is sufficient to inhibit α-synuclein aggregation, Neural Regen. Res., 2022, vol. 17, p. 508. https://doi.org/10.4103/1673-5374.320973
Penke, B., Bogár, F., Paragi, G., Gera, J., and Fülöp, L.,Key peptides and proteins in Alzheimer’s disease, Curr. Protein Pept. Sci., 2019, vol. 20, p. 577. https://doi.org/10.2174/1389203720666190103123434
Penke, B., Szűcs, M., and Bogár, F., Oligomerization and conformationalchange turn monomeric β-Amyloid and tau proteins toxic: their role in Alzheimer’s pathogenesis, Molecules, 2020, vol. 25, p. 1659. https://doi.org/10.3390/molecules25071659
Perni, M., Flagmeier, P., Limbocker, R., Cascella, R., Aprile, F.A., Galvagnion, C., Heller, G.T., Meisl, G., Chen, S.W., Kumita, J.R., Challa, P.K., Kirkegaard, J.B., Cohen, S.I.A., Mannini, B., Barbut, D., et al., Multistep inhibition of α-synuclein aggregation and toxicity in vitro and in vivo by trodusquemine, ACS Chem. Biol., 2018, vol. 13, p. 2308. https://doi.org/10.1021/acschembio.8b00466
Perni, M., van der Goot, A., Limbocker, R., van Ham, T.J., Aprile, F.A., Xu, C.K., Flagmeier, P., Thijssen, K., Sormanni, P., Fusco, G., Chen, S.W., Challa, P.K., Kirkegaard, J.B., Laine, R.F., Ma, K.Y., et al., Comparative studies in the A30P and A53T α-synuclein C. elegans strains to investigate the molecular origins of Parkinson’s disease, Front. Cell Dev. Biol., 2021, vol. 9, p. 552549. https://doi.org/10.3389/fcell.2021.552549
Rajasekhar, K., Suresh, S.N., Manjithaya, R., and Govindaraju, T., Rationally designed peptidomimetic modulators of aβ toxicity in Alzheimer’s disease, Sci. Rep., 2015, vol. 30, p. 8139. https://doi.org/10.1038/srep08139
Russo, R., Borghi, R., Markesbery, W., Tabaton, M., and Piccini, A.,Neprylisin decreases uniformly in Alzheimer’s disease and in normal aging, FEBS Lett., 2005, vol. 579, p. 6027. https://doi.org/10.1016/j.febslet.2005.09.054
Sangkaew, A., Kojornna, T., Tanahashi, R., Takagi, H., and Yompakdee, C., A novel yeast-based screening system for potential compounds that can alleviate human α-synuclein toxicity, J. Appl. Microbiol., 2022, vol. 132, p. 1409. https://doi.org/10.1111/jam.15256
Santos, J., Pallarès, I., and Ventura, S.,Is a cure for Parkinson’s disease hiding inside us?, Trends Biochem. Sci., 2022, vol. 19, p. S0968-0004(22)00025-1. https://doi.org/10.1016/j.tibs.2022.02.001
Schepers, J. and Behl, C., Lipid droplets and autophagy-links and regulations from yeast to humans, J. Cell Biochem., 2021, vol. 122, p. 602. https://doi.org/10.1002/jcb.29889
Scudamore, O. and Ciossek, T.,Increased oxidative stress exacerbates α-synuclein aggregation in vivo, J. Neuropathol. Exp. Neurol., 2018, vol. 77, p. 443. https://doi.org/10.1093/jnen/nly024
Silva, J.L., Vieira, T.C., Cordeiro, Y., and de Oliveira, G.A.P.,Nucleic acid actions on abnormal protein aggregation, phase transitions and phase separation, Curr. Opin. Struct. Biol., 2022, vol. 73, p. 102346. https://doi.org/10.1016/j.sbi.2022.102346
Simonsen, A. and Wollert, T., Don’t forget to be picky—selective autophagy of protein aggregates in neurodegenerative diseases, Curr. Opin. Cell Biol., 2022, vol. 75, p. 102064. https://doi.org/10.1016/j.ceb.2022.01.009
Stefani, M. and Dobson, C.M., Protein aggregation and aggregate toxicity: new insights into protein folding, misfolding diseases and biological evolution, J. Mol. Med. (Berl.), 2003, vol. 81, p. 678. https://doi.org/10.1007/s00109-003-0464-5
Stefanis, L., α-Synuclein in Parkinson's disease, Cold Spring Harb. Perspect. Med., 2012, vol. 2, p. a009399. https://doi.org/10.1101/cshperspect.a009399
Su, L.J., Auluck, P.K., Outeiro, T.F., Yeger-Lotem, E., Kritzer, J.A., Tardiff, D.F., Strathearn, K.E., Liu, F., Cao, S., Hamamichi, S., Hill, K.J., Caldwell, K.A., Bell, G.W., Fraenkel, E., Cooper, A.A., et al., Compounds from an unbiased chemical screen reverse both ER-to-Golgi trafficking defects and mitochondrial dysfunction in Parkinson’s disease models, Dis. Model. Mech., 2010, vol. 3, p. 194. https://doi.org/10.1242/dmm.004267
Subedi, S., Sasidharan, S., Nag, N., Saudagar, P., and Tripathi, T., Amyloid cross-seeding: mechanism, implication, and inhibition, Molecules, 2022, vol. 27, p. 1776. https://doi.org/10.3390/molecules27061776
Tang, Y., Zhang, D., Liu, Y., Zhang, Y., Zhou, Y., Chang, Y., Zheng, B., Xu, A., and Zheng, J., A new strategy to reconcile amyloid cross-seeding and amyloid prevention in a binary system of α-synuclein fragmental peptide and hIAPP, Protein Sci., 2022a, vol. 31, p. 485. https://doi.org/10.1002/pro.4247
Tang, Y., Zhang, D., Zhang, Y., Liu, Y., Miller, Y., Gong, K., and Zheng, J.,Cross-seeding between Aβ and SEVI indicates a pathogenic link and gender difference between Alzheimer diseases and AIDS, Commun. Biol., 2022b, vol. 5, p. 417. https://doi.org/10.1038/s42003-022-03343-7
Tanguy, E., Wang, Q., Moine, H., and Vitale, N., Phosphatidic acid: from pleiotropic functions to neuronal pathology, Front. Cell Neurosci., 2019, vol. 13, p. 2. https://doi.org/10.3389/fncel.2019.00002
Tardiff, D.F., Jui, N.T., Khurana, V., Tambe, M.A., Thompson, M.L., Chung, C.Y., Kamadurai, H.B., Kim, H.T., Lancaster, A.K., Caldwell, K.A., Caldwell, G.A., Rochet, J.C., Buchwald, S.L., and Lindquist, S., Yeast reveal a druggable Rsp5/Nedd4 network that ameliorates α-synuclein toxicity in neurons, Science, 2013, vol. 342, p. 979. https://doi.org/10.1126/science.1245321
Tavanti, F., Pedone, A., and Menziani, M.C.,Insights into the effect of curcumin and (–)-epigallocatechin-3-gallate on the aggregation of Aβ(1–40) monomers by means of molecular dynamics,Int. J. Mol. Sci., 2020, vol. 21, p. 5462. https://doi.org/10.3390/ijms21155462
Tenreiro, S., Munder, M.C., Alberti, S., and Outeiro, T.F.,Harnessing the power of yeast to unravel the molecular basis of neurodegeneration, J. Neurochem., 2013, vol. 127, p. 438. https://doi.org/10.1111/jnc.12271
Thellung, S., Corsaro, A., Nizzari, M., Barbieri, F., and Florio, T.,Autophagy activator drugs: a new opportunity in neuroprotection from misfolded protein toxicity, Int. J. Mol. Sci., 2019, vol. 20, p. 901. https://doi.org/10.3390/ijms20040901
Tuite, M.F., Yeast models of neurodegenerative diseases, Prog. Mol. Biol. Transl. Sci., 2019, vol. 168, p. 351. https://doi.org/10.1016/bs.pmbts.2019.07.001
Vernon, R.M., Chong, P.A., Tsang, B., Kim, T.H., Bah, A., Farber, P., Lin, H., and Forman-Kay, J.D.,Pi-Pi contacts are an overlooked protein feature relevant to phase separation, Elife, 2018, vol. 7, p. e31486. https://doi.org/10.7554/eLife.31486
Villar-Piqué,A., da Fonseca, T.L., Sant’Anna, R., Szegö, É.M., Fonseca-Ornelas,L., Pinho, R., Carija, A.,Gerhardt,E., Masaracchia,C., Abad,G.E., Rossetti,G., Carloni, P., Fernández, C.O., Foguel,D., Milosevic,I., et al., Environmental and genetic factors support the dissociation between α-synuclein aggregation and toxicity, Proc. Natl. Acad. Sci. U. S. A., 2016, vol. 113, p. E6506. https://doi.org/10.1073/pnas.1606791113
Vivoli Vega,M., Cascella, R., Chen, S.W., Fusco, G., De Simone, A.,Dobson, C.M., Cecchi, C., and Chiti, F.,The toxicity of misfolded protein oligomers is independent of their secondary structure, ACS Chem. Biol., 2019, vol. 14, p. 1593. https://doi.org/10.1021/acschembio.9b00324
Volles, M.J., Lee, S.J., Rochet, J.C., Shtilerman, M.D., Ding, T.T., Kessler, J.C., and Lansbury, P.T., Jr., Vesicle permeabilization by protofibrillar alpha-synuclein: implications for the pathogenesis and treatment of Parkinson’s disease, Biochemistry, 2001, vol. 40, p. 7812. https://doi.org/10.1021/bi0102398
Wang, Y. and Westermark, G.T., The amyloid forming peptide islet amyloid polypeptide and amyloid β interact at the molecular level, Int. J. Mol. Sci., 2021, vol. 22, p. 11153. https://doi.org/10.3390/ijms222011153
Wells, C., Brennan, S.E., Keon, M., and Saksena, N.K.,Prionoid proteins in the pathogenesis of neurodegenerative diseases, Front. Mol. Neurosci., 2019, vol. 12, p. 271. https://doi.org/10.3389/fnmol.2019.00271
Wells, C., Brennan, S.E., Keon, M., and Ooi, L., The role of amyloid oligomers in neurodegenerative pathologies, Int. J. Biol. Macromol., 2021, vol. 181, p. 582. https://doi.org/10.1016/j.ijbiomac.2021.03.113
Wentink, A., Nussbaum-Krammer, C., and Bukau, B.,Modulation of amyloid states by molecular chaperones, Cold Spring Harb. Perspect. Biol., 2019, vol. 11, p. a033969. https://doi.org/10.1101/cshperspect.a033969
Xue, W.F., Hellewell, A.L., Hewitt, E.W., and Radford, S.E., Fibril fragmentation in amyloid assembly and cytotoxicity, Prion, 2010, vol. 4, p. 20. https://doi.org/10.4161/pri.4.1.11378
Youn, K., Ho, C., and Jun, M.,Multifaceted neuroprotective effects of (-)-epigallocatechin-3-gallate (EGCG) in Alzheimer’s disease: an overview of pre-clinical studies focused on β-amyloid peptide, Food Sci. Hum. Wellness, 2022, vol. 11, p. 483. https://doi.org/10.1016/j.fshw.2021.12.006
Younan, N.D., Chen, K.F., Rose, R.S., Crowther, D.C., and Viles, J.H., Prion protein stabilizes amyloid-β (βA) oligomers and enhances Aβ neurotoxicity in a Drosophilamodel of Alzheimer’s disease, J. Biol. Chem., 2018, vol. 293, p. 13090. https://doi.org/10.1074/jbc.RA118.003319
Young, L.M., Mahood, R.A., Saunders, J.C., Tu, L.H., Raleigh, D.P., Radford, S.E., and Ashcroft, A.E., Insights into the consequences of co-polymerisation in the early stages of IAPP and Aβ peptide assembly from mass spectrometry, Analyst, 2015, vol. 140, p. 6990. https://doi.org/10.1039/c5an00865d
Zhang, Y., Zhao, Y., Zhang, L., Yu, W., Wang, Y., and Chang, W.,Cellular prion protein as a receptor of toxic amyloid-β 42 oligomers is important for Alzheimer’s disease, Front. Cell Neurosci., 2019, vol. 13, p. 339. https://doi.org/10.3389/fncel.2019.00339
Zhang, S., Liu, Y.Q., Jia, C., Lim, Y.J., Feng, G., Xu, E., Long, H., Kimura, Y., Tao, Y., Zhao, C., Wang, C., Liu, Z., Hu, J.J., Ma, M.R., Liu, Z., et al., Mechanistic basis for receptor-mediated pathological α-synuclein fibril cell-to-cell transmission in Parkinson’s disease, Proc. Natl. Acad. Sci. U. S. A., 2021a, vol. 118, p. e2011196118. https://doi.org/10.1073/pnas.2011196118
Zhang, Y., Zhang, M., Liu, Y., Zhang, D., Tang, Y., Ren, B., and Zheng, J.,Dual amyloid cross-seeding reveals steric zipper-facilitated fibrillization and pathological links between protein misfolding diseases, J. Mat. Chem. B, 2021b, vol. 9, p. 3300. https://doi.org/10.1039/D0TB0295K
Zubova, S.G., The diversity of autophagy and its controversial role in biological processes, Tsitologiya, 2019, vol. 61, no. 12, p. 941. https://doi.org/10.1134/S0041377119120095
Funding
The work was carried out at the expense of the budgetary funds of the Institute of Cytology of the Russian Academy of Sciences, subject no. AAAA-A17-117032350034-7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors declare that they have no conflicts of interest.
The work did not include experiments involving animals or human beings.
Additional information
Publisher’s Note.
Pleiades Publishing remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Abbreviations: βA—β-amyloid; AS—α-synuclein; ROS—reactive oxygen species; AD—Alzheimer’s disease; PD—Parkinson’s disease; RP—red yeast pigment; NMO—nonmembrane organelle; TAG—triacylglycerol; ES—ester of sterol; EGCG—epigalocatechin gallate; calcein–AM—calcein acetoxymethyl.
Rights and permissions
About this article
Cite this article
Nevzglyadova, O.V., Mikhailova, E.V. & Soidla, T.R. Molecular Mechanisms Underlying Alzheimer’s and Parkinson’s Disease and the Possibility of Their Neutralization. Cell Tiss. Biol. 17, 593–607 (2023). https://doi.org/10.1134/S1990519X23060093
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S1990519X23060093