Abstract
White matter (WM) abnormalities have long been suspected in major depressive disorder (MDD). Tract-based spatial statistics (TBSS) studies have detected abnormalities in fractional anisotropy (FA) in MDD, but the available evidence has been inconsistent. We performed a quantitative meta-analysis of TBSS studies contrasting MDD patients with healthy control subjects (HCS). A total of 17 studies with 18 datasets that included 641 MDD patients and 581 HCS were identified. Anisotropic effect size-signed differential mapping (AES-SDM) meta-analysis was performed to assess FA alterations in MDD patients compared to HCS. FA reductions were identified in the genu of the corpus callosum (CC) extending to the body of the CC and left anterior limb of the internal capsule (ALIC) in MDD patients relative to HCS. Descriptive analysis of quartiles, sensitivity analysis and subgroup analysis further confirmed these findings. Meta-regression analysis revealed that individuals with more severe MDD were significantly more likely to have FA reductions in the genu of the CC. This study provides a thorough profile of WM abnormalities in MDD and evidence that interhemispheric connections and frontal-striatal-thalamic pathways are the most convergent circuits affected in MDD.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Introduction
Major depressive disorder (MDD) is a common chronically debilitating psychiatric disorder with an estimated prevalence of 13% to 16% in the general population1,2. MDD is characterized by the profound dysregulation of mood as well as additional abnormalities including cognitive dysfunction, insomnia, fatigue and appetite disturbance3. Despite psychopharmacologic and psychotherapeutic treatments, MDD remains a costly mental health illness in terms of total health care expenditures and lost productivity4. Consequently, a greater understanding of the neural correlates underlying MDD is of great significance to identify biologically based targets to improve the specificity and efficacy of diagnostic and treatment strategies for MDD.
Over the last few decades, modern imaging techniques have greatly increased our knowledge of MDD, particularly its neural bases. Previous studies of structural and functional magnetic resonance imaging (MRI) have reported various grey matter (GM) abnormalities in MDD patients, including abnormalities in the prefrontal cortex5,6,7, anterior cingulate cortex8,9, hippocampus10,11 and thalamus12,13. These observations suggest that a dysfunctional prefrontal-limbic circuit instead of a deficit in distinct regions plays an important role in the pathophysiology of MDD. As the infrastructure connecting those cortical and subcortical regions and the basis for structure connectivity, white matter (WM) warrants more exploration.
In contrast to conventional T1-weighted structural images of WM in the brain, diffusion tensor imaging (DTI), a noninvasive magnetic resonance method based on the diffusion characteristics of water, can be used to quantify the fibre orientation and integrity of WM pathways within neural networks14,15. One commonly used parameter for measuring WM integrity is fractional anisotropy (FA), an invariant property of DTI that reflects a nonspherical diffusion tensor with a preferential orientation16,17,18. FA can be measured using two techniques: the region of interest (ROI) approach, which manually preselects limited and potentially biased parts of the brain for analysis, and whole-brain study including voxel-based analysis (VBA) and tract-based spatial statistics (TBSS), which generally report the three-dimensional coordinates for which there are maximal FA differences in patients compared with healthy control subjects (HCS).
FA reduction is related to depression severity and illness duration in MDD patients19, which indicates that DTI may be of clinical value in measuring and tracking disability in MDD. However, many studies have reported inconsistent and controversial results due to small and heterogeneous samples and substantial methodological differences between studies. For example, several studies have reported FA reductions in the right frontal WM, left lateral occipital WM, left superior longitudinal fasciculus, and left anterior limb of the internal capsule (ALIC)20,21,22,23. However, another study with a large sample size observed no significant differences in FA between MDD patients and HCS24. Thus, there has been increasing interest in meta-analysis to identify consistent results for DTI studies in MDD and provide more insight into the neural-anatomical basis for structural connections in this disorder.
However, a major shortcoming of published voxel-wise meta-analyses of DTI studies of MDD is the use of both VBA and TBSS studies25,26,27. VBA is relatively straightforward and involves the spatial normalization of high-resolution images from all of the subjects in the study to the same stereotactic space28. TBSS is a statistical method in which each subject’s FA data are projected onto the mean FA skeleton such that each skeleton voxel takes the FA value from the local centre of the nearest relevant tract, thus alleviating the misalignment problems that can arise in regular VBA studies due to anatomical difference between groups29. Furthermore, Wise et al. published a meta-analysis integrating both TBSS and VBA studies to investigate the structural disconnectivity in MDD and they demonstrated that TBSS might be a more sensitive technique for the detection of WM abnormalities and provide a more accurate estimate compared with VBA27. However, in the study conducted by Wise et al.27, only 10 DTI studies with TBSS were included, and other confounding factors, such as medication status, were not considered. Furthermore, they did not find the association between the symptom severity evaluated by Hamilton Depression Rating Scale (HAMD) and neuroimaging alterations because only 7 TBSS datasets reporting HAMD scores were included in Wise's research while according to Radua et al.30, the meta-regression analysis is invalid if data is available for fewer than 9 datasets. Since more original TBSS studies regarding MDD have been published in recent years, it is worthwhile to conduct an updated tract-based spatial meta-analysis to explore the WM microstructure abnormalities and investigate the effects of symptom severity and other clinical profiles on regional WM alterations.
Therefore, the goals of this study were threefold: first, we conducted an updated quantitative summary of 17 TBSS studies (14 TBSS datasets reported HAMD scores) concerning FA abnormalities in MDD using anisotropic effect size-signed differential mapping (AES-SDM), a newly developed meta-analytic technique with the potential to quantify the reproducibility of neuroimaging findings and to generate insights that are difficult to obtain from an individual study; second, we performed subgroup meta-analyses to compare first-episode, treatment-naive/medication-free MDD patients with HCS to avoid the potential confounding effects of medication; third, we used a meta-regression method to examine the potentially moderating effects of symptom severity and other relevant variables on the reported WM abnormalities.
Results
Included studies and sample characteristics
The search strategy yielded a total of 123 studies, of which 17 TBSS studies20,21,22,23,24,31,32,33,34,35,36,37,38,39,40,41,42 with 18 datasets met the inclusion criteria. The included studies reported FA alterations in WM in 641 individuals with MDD (255 male and 386 female; mean age 37.4 years) relative to 581 HCS (263 male and 318 female; mean age 33.4 years). In one study37, suicide attempters and non-attempters with MDD were compared with the same healthy participants. Thus, we treated this study as two unique and independent datasets in the meta-analysis. The flow diagram of the identification and exclusion of studies is presented in Fig. 1. Table 1 summarizes the characteristics of these studies included in the meta-analysis.
Regional difference in FA in all included studies
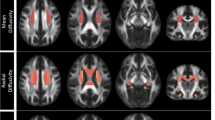
Coordinates for the AES-SDM analysis were obtained from all 18 datasets representing 641 patients with MDD and 581 HCS. As shown in Fig. 2 and Table 2, patients with MDD had significant FA reductions in 2 clusters relative to HCS. The largest cluster exhibited a peak in the genu of the corpus callosum (CC) extending to the body of the CC. The main tracts passing through this region were the interhemispheric fibres connecting the prefrontal and orbitofrontal cortices, shown as yellow tracts in Fig. 3. The other cluster exhibited FA reduction in the left ALIC. The main tracts passing through this region were the anterior thalamic radiation connecting the medial dorsal thalamic nuclei with the prefrontal cortices, shown as the green tracts in Fig. 3. No FA increases in any of the regions were reported in the analysis. The results from Egger’s test revealed no strong evidence for publication bias in the genu of the CC (P = 0.198) and left ALIC (P = 0.123).
Left image (A) observed from the left side of the brain, right image (B) observed from above. Tracts include the interhemispheric fibres running through the genu of the CC (yellow) and the anterior thalamic radiation running through the left ALIC (green). Sagittal and axial slices mapping the FA values are shown in the background for illustrative purposes. Abbreviations: CC, corpus callosum; ALIC, anterior limb of internal capsule; FA, fractional anisotropy.
Jack-knife sensitivity analysis
As shown in Table 3, whole-brain jack-knife sensitivity analysis of the pooled meta-analysis indicated that the FA reduction in patients with MDD in the genu of the CC was highly replicable; this finding was preserved throughout all 18 combinations of the datasets. The FA reduction in the left ALIC remained significant in all but three combinations of the datasets.
Descriptive analysis of quartiles
The descriptive analysis of quartiles demonstrated that the FA reduction in the genu of the CC was detected in the median analysis, indicating that at least 50% of the included datasets detected a significant FA reduction in this region. The left ALIC was not detected in this analysis, indicating that less than 25% of the datasets detected significant FA reduction in this region (Table 3).
Subgroup analysis of first-episode, treatment-naive and medication-free datasets
The subgroup analysis revealed that the above findings remained largely unchanged when only the 7 datasets with first-episode, treatment-naive MDD or only the 14 datasets with medication-free MDD were analysed. However, the above-mentioned analysis revealed no significant differences in the FA in the genu of the CC between patients and HCS when only the 7 datasets with first-episode, treatment-naive MDD were analysed (Table 3).
Meta-regression analysis
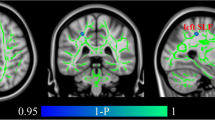
The symptom severity evaluated by HAMD scores was negatively associated with FA reduction in the genu of the CC (Montreal Neurological Institute coordinate: x = 12, y = 30, z = 8; AES-SDM value = −0.102, p = 0.00012; 129 voxels), as shown in Fig. 4. The mean age, illness duration, and drug status of MDD participants were not associated with MDD-related FA reductions in the genu of the CC, at least linearly. However, there was no significant correlation between FA reduction in the left ALIC and symptom severity or other variables.
In the graphs, AES-SDM values needed to create this plot were extracted from the peak of maximum slope significance, and each study is represented as a dot; the dot size reflects the sample size. The regression line (meta-regression signed differential mapping slope) is presented as a straight line. Abbreviations: FA, fractional anisotropy; CC, corpus callosum; MDD, major depressive disorder; HAMD, Hamilton Depression Rating Scale; AES-SDM, anisotropic effect size-signed differential mapping.
Discussion
This study pooled the largest number of DTI studies using TBSS to date for a meta-analysis of the difference in FA between patients with MDD and HCS. The present voxel-wise meta-analysis using AES-SDM primarily revealed that patients with MDD have FA reductions in the genu of the CC extending to the body of the CC and left ALIC. The results remained largely unchanged when each dataset was discarded individually (jack-knife sensitivity analysis). Descriptive analysis of quartiles further revealed that most of the datasets detected some degree of FA reduction in the genu of the CC and that less than 25% of the datasets detected some degree of FA reduction in the left ALIC.
Our observation of FA reduction in the genu of the CC is consistent with a previous meta-analysis of MDD that included VBA and TBSS studies27. However, other meta-analyses identified decreased FA values in the left superior longitudinal fasciculus, increased FA values in the right inferior fronto-occipital fasciculus25 and decreased FA values in the right frontal lobe, right fusiform gyrus, left frontal lobe and right occipital lobe26. These inconsistencies are attributable to distinct factors. First, the present meta-analysis only included DTI studies using TBSS and excluded studies using VBA, thus eliminating the potential for bias due to methodological differences in MRI data processing. Second, several studies that did not detect significant differences in FA between patients with MDD and HCS were included in the present study, whereas prior meta-analysis excluded these studies because the activation likelihood estimation (ALE) method cannot be used for the studies with no significant group differences26. Finally, the patient sample characteristics (e.g., age, gender, illness duration, age at onset, subtype and severity) of the included studies differ among the meta-analyses.
The CC is the largest WM tract connecting corresponding regions of the cerebral cortex in the two cerebral hemispheres to integrate the motor, sensory, and cognitive functions of the brain43. In neuroimaging studies, the abnormalities of the CC have been increasingly implicated in MDD44,45,46. Structural MRI revealed that the genu region of the CC is smaller in early onset adult MDD47. Selected ROI analyses of DTI have also demonstrated that adult patients with MDD have reduced FA in the genu of the CC48, suggesting decreased structural integrity of its related WM commissural fibres. In addition, magnetization transfer ratio (MTR) imaging has also revealed a lower MTR in the genu of the CC in patients with MDD compared with non-depressed controls49.
The WM fibres passing through the genu of the CC connect the bilateral prefrontal and orbitofrontal cortices, which are related to decision-making, attention, reward processing, and emotion regulation. Specific WM pathologies contributing to low FA could include myelin and/or axonal damage and gliosis50. The genu of the CC and prefrontal WM are both late-myelinating and are therefore more vulnerable to damage than the early myelinating splenium. The reduction of myelination in the genu of the CC could lead to decreased speed or quantity of interhemispheric communications51. The disturbed connectivity between these brain regions may negatively affect the normal process of interhemispheric information transfer in MDD patients, which may subsequently lead to deficits in memory, executive functioning and emotional regulation with predisposition toward more severe depressive symptoms33,52. Deficits in neuropsychological functioning can influence the daily functioning and worsen the quality of life of these patients. Our findings, together with those of previous studies, further support the assertion that MDD is associated with the disorganization of WM architecture in the genu of the CC, which connects prefrontal and orbitofrontal cortices in the two cerebral hemispheres.
Interestingly, the subgroup analysis of first-episode, treatment-naive datasets revealed no significant differences in FA in the genu of the CC, which indicated that the FA reduction in this area might be due to medication. Indeed, only one study in the included first-episode, treatment-naive datasets reported the FA reduction in the genu of the CC in patients with MDD. Another possible explanation of this negative finding in first episode cases is that FA reduction in the genu of the CC might be a “scar” caused by depressive illness duration. This speculation was supported by a previous DTI study, which demonstrated that illness duration of MDD was the predictor of whole-brain mean FA, with a significant negative linear relationship53. However, the results of subgroup analysis should be interpreted with caution because only 7 datasets of small sample size were recruited. Further investigations with longitudinal design are needed for a more comprehensive understanding of the WM abnormalities in different phases of MDD.
The ALIC is the WM tract between the head of the caudate nucleus and the lenticular nucleus, which is heavily involved in motivation, decision-making, and evaluating the saliency of emotional and rewarding stimuli54. The observed FA reduction in the ALIC implicates an impairment of the integrity of WM fibre tracts, which is particularly important in understanding the pathophysiology of MDD and is a useful addition to the findings obtained in the previous meta-analysis by Wise et al. (2015). Subgroup analysis of first-episode, treatment-naive MDD or medication-free MDD revealed that the FA reduction in the left ALIC remained unchanged. In the present meta-analysis, the fibre tract passing through the left ALIC with decreased FA, as identified by DTIquery software, was the anterior thalamic radiation connecting the medial dorsal thalamic nuclei with the prefrontal cortices, which is the main WM fibre tract passing from the ALIC and the large number of horizontally cut fibres in the ALIC55.
Disrupted or decreased demyelination or decreased fibre density or coherence in the region may be the biological mechanism underlying the decrease in FA in MDD. Abnormalities of the ALIC have been reported in patients with depression. A DTI study of adult depression using the VBA method revealed significantly decreased FA in the left ALIC19. Other DTI studies using the VBA method have also indicated decreased FA in the left ALIC in suicide attempters compared to both non attempters and HCS56 and reduced fibre projections through the ALIC to the left medial frontal cortex, orbitofrontal cortex and thalamus in depressed patients57. Furthermore, the ALIC is the most frequent therapeutic target for deep brain stimulation in treatment-resistant depression58,59. The FA reduction in the left ALIC may reflect a disconnection of frontal-striatal-thalamic neuronal circuits, which may cause damage to executive function and emotional lability in MDD patients60. Because the frontal-striatal-thalamic neuronal circuits consist of massive bundles of fibres passing through the ALIC, this disorganization of WM architecture in the ALIC further indicates an important role of frontal-striatal-thalamic pathways in MDD pathogenesis.
Meta-regression analysis demonstrated that the severity of depressive symptoms (HAMD scores) was negatively correlated with FA reduction in the genu of the CC, which indicates that the symptom severity of patients with MDD influences the degree of WM disruption to some extent. This finding is consistent with a previous DTI study that correlated greater depression severity with reduced WM integrity in the genu of the CC54. These converging lines of evidence further demonstrate that abnormalities in structural connectivity are associated with the pathophysiology of MDD. However, there was no significant correlation between FA reduction in the left ALIC and symptom severity, consistent with the findings of previous DTI studies that used the VBA method56. Conversely, another DTI study observed that FA reduction in the left ALIC is negatively related to the severity of depressive symptoms19. These discrepancies are likely due to variations of age, gender, illness duration, age at onset, subtype and medication status in patients with MDD.
The present study has several limitations. First, the number of DTI studies with TBSS in adolescent or late-life depression was small. Thus, we only included studies of adult depression and were not able to compare differences in FA in various age ranges. Second, the heterogeneity of the MRI data acquisition, including voxel size, diffusion direction, and slice thickness, may decrease the accuracy of the results of the present meta-analysis. Third, the included studies varied in terms of patient characteristics and clinical variables. For example, the patients with MDD included in the present study had either first-episode or recurrent MDD. Although we performed a subgroup meta-analysis for the first-episode, treatment-naive and medication-free datasets, the results should be interpreted with caution. There are only 7 first-episode, treatment-naive datasets, and the small sample size of the subgroup meta-analysis limits the generalizability of the results. These first-episode MDD patients could potentially experience manic or hypomanic episodes in the future and may be diagnosed with bipolar disorder. Compared with unipolar depression, bipolar disorder has more widespread abnormalities in WM connectivity and WM hyperintensities61. In addition, the washout period prior to MRI scanning varied among the included studies and was as short as only 2 days. Therefore, the subgroup meta-analysis of medication-free datasets may not completely exclude the effects of medication. Fourth, while it is true that TBSS appears to be a more sensitive method than VBA, omitting these studies using VBA reduces the number of the included studies and gives a somewhat incomplete picture of the literature. Finally, we only focused on FA and did not consider other measures of diffusivity, such as mean, radial or axial diffusivity, which may provide insights on the nature of the underlying WM changes contributing to alterations in FA.
In summary, this meta-analysis of DTI studies with TBSS identified two consistent locations of FA reduction in patients with MDD. The largest cluster, located in the genu of the CC and extending to the body of the CC, represents the interhemispheric fibres connecting the prefrontal and orbitofrontal cortices. The other cluster of FA reduction, located in the left ALIC, is the anterior thalamic radiation connecting the medial dorsal thalamic nuclei with the prefrontal cortices. These findings integrate previous inconsistencies in the DTI studies of MDD and provide a coherent picture of the most prominent and replicable abnormalities of WM in patients with MDD. Furthermore, our meta-regression analysis provides evidence suggesting that the symptom severity of patients with MDD is negatively associated with FA reduction in the genu of the CC. Our results demonstrate that the abnormalities of interhemispheric connections and frontal-striatal-thalamic pathways may play an important role in MDD pathogenesis.
Methods
Literature search strategy
Systematic and comprehensive searches of the PubMed, Web of Science, PsycINFO, Cochrane Library, and EMBASE databases were performed for studies published between January 1994 and July 2015 and “in press” articles. The search keywords were (“unipolar disorder” or “depressive disorder” or “depression”) and (“tract-based spatial statistics” or “TBSS”) and (“diffusion tensor” or “DTI”). The reference lists of the identified articles and review articles were also manually reviewed to identify additional papers.
Study eligibility criteria
All DTI studies using a TBSS approach yielded by our search were assessed for potential suitability, and the articles that met the following inclusion criteria were adopted for the meta-analysis: (i) published in a peer-reviewed English language journal; (ii) included adult patients with MDD to minimize the influence of neurodevelopment and neurodegeneration on WM diffusion; (iii) compared a group of MDD patients according to the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV) criteria with a group of HCS; (iv) utilized TBSS to investigate FA alterations between MDD patients and HCS; (v) used thresholds for significance corrected for multiple comparisons or uncorrected with spatial extent thresholds; and (vi) reported whole-brain three-dimensional coordinates (Talairach or Montreal Neurological Institute) of FA alterations in a stereotactic space to enable voxel-level quantitative meta-analysis. For publications that were otherwise suitable for meta-analysis but did not report whole-brain coordinates, the corresponding authors were contacted for additional information.
The studies were excluded if they had at least one of the following deficiencies: (i) the studies were case reports or reviews; (ii) the studies included adolescent patients with depression or patients with late-life depression; (iii) the three -dimensional coordinates in stereotactic space could not be obtained; (iv) the data were entered twice from a study population that had been analysed in more than one publication; (v) participants with multiple combined Axis I diagnoses were explicitly recruited; and (vi) fewer than ten subjects in either the MDD group or the HCS group were studied. The method used in the current study was in accordance with the Meta-analysis Of Observational Studies in Epidemiology (MOOSE) guidelines for meta-analyses of observational studies62.
Quality assessment and data extraction
Two authors (G.X.C. and X.Y.H.) independently searched the literature, examined the retrieved articles, and extracted and cross-checked data. The quality of the included studies were also independently assessed by the two authors using a 12-point checklist (see the Supplementary Information, Table S1) that focused on both the clinical and demographic aspects of individual study samples and on the imaging-specific methodology63. If agreement was not obtained, one of the authors (L.L.) mediated. The quality scores for each study are provided in Table 1. For each included study, the following data were extracted: demographic information including participant characteristics (sample size, age, and gender), age at onset, illness duration, symptom severity, diagnosis, statistical threshold and drug status; the three-dimensional coordinates in each study were also extracted for the meta-analysis according to the AES-SDM method64, the main features of which are the possibility of combining peak coordinates and statistical parametric maps, as well as the use of well-established statistics accounting for within- and between-study variance65.
Voxel-wise meta-analysis
Voxel-wise meta-analysis was performed on the selected studies using AES-SDM software in a standard process to compare FA changes between the MDD group and HCS group. Descriptive analysis of quartiles was also performed to check the actual proportion of the studies reporting results in a particular brain region. Systematic whole-brain voxel-based jack-knife sensitivity analysis was performed to test the replicability of the results. To control for any possible influence of drug status between studies, subgroup meta-analyses of the first-episode, treatment-naive and medication-free datasets were conducted. The AES-SDM software editor was also contacted via email when necessary. These analytical processes refer to the AES-SDM tutorial (http://sdmproject.com/software/Tutorial.pdf) and related publications64,66. The analytical parameters of the AES-SDM were as follows: anisotropy = 1.0; isotropic full-width at half-maximum (FWHM) = 20 mm; voxel p = 0.005; peak height threshold = 1; cluster extent = 10 voxels with 10 repetitions of standard randomization tests. Moreover, we used MRIcron software (http://www.cabiatl.com/mricro/mricron/) to visualize AES-SDM maps overlaid onto a high-resolution brain template generated by the International Consortium for Brain Mapping. DTIquery software (http://graphics.stanford.edu/projects/dti/) and an atlas of human WM anatomy67 was applied to help identify the fascicles involved in each region. We used the sample data of a healthy 35-year-old male provided by DTIquery software. The possible existence of publication bias for the brain regions with FA alterations was assessed by Egger’s test using Stata software (version12.0).
Meta-regression analysis
The potential effects of the mean age, illness duration, symptom severity (HAMD scores) and drug status of the MDD participants were examined by simple linear regression, weighted by the square root of the sample size and restricted to predict only possible AES-SDM values (i.e., from −1 to 1) in the observed range of values of the variable. The main output for each variable was a map of the regression slope30. As described in previous meta-analyses, to minimize the detection of spurious relationships, we decreased the probability threshold to 0.0005 required abnormalities to be detected both in the slope and in one of the extremes of the regressor and discarded findings in regions other than those detected in the main analyses. Regression plots were visually inspected to discard fittings driven by too few studies68.
Additional Information
How to cite this article: Chen, G. et al. Disorganization of white matter architecture in major depressive disorder: a meta-analysis of diffusion tensor imaging with tract-based spatial statistics. Sci. Rep. 6, 21825; doi: 10.1038/srep21825 (2016).
References
Moussavi, S. et al. Depression, chronic diseases, and decrements in health: results from the World Health Surveys. Lancet 370, 851–858 (2007).
Vos, T. et al. Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 380, 2163–2196 (2012).
Fitzgerald, P. J. Gray colored glasses: is major depression partially a sensory perceptual disorder? J Affect Disord 151, 418–422 (2013).
Egede, L. E. Major depression in individuals with chronic medical disorders: prevalence, correlates and association with health resource utilization, lost productivity and functional disability. Gen Hosp Psychiatry 29, 409–416 (2007).
Salvadore, G. et al. Prefrontal cortical abnormalities in currently depressed versus currently remitted patients with major depressive disorder. Neuroimage 54, 2643–2651 (2011).
Scheuerecker, J. et al. Orbitofrontal volume reductions during emotion recognition in patients with major depression. J Psychiatry Neurosci 35, 311–320 (2010).
Rive, M. M. et al. Neural correlates of dysfunctional emotion regulation in major depressive disorder. A systematic review of neuroimaging studies. Neurosci Biobehav Rev 37, 2529–2553 (2013).
Bertocci, M. A. et al. Abnormal anterior cingulate cortical activity during emotional n-back task performance distinguishes bipolar from unipolar depressed females. Psychol Med 42, 1417–1428 (2012).
Wagner, G. et al. Enhanced rostral anterior cingulate cortex activation during cognitive control is related to orbitofrontal volume reduction in unipolar depression. J Psychiatry Neurosci 33, 199–208 (2008).
Arnone, D. et al. State-dependent changes in hippocampal grey matter in depression. Mol Psychiatry 18, 1265–1272 (2013).
Zou, K. et al. Changes of brain morphometry in first-episode, drug-naive, non-late-life adult patients with major depression: an optimized voxel-based morphometry study. Biol Psychiatry 67, 186–188 (2010).
Soriano-Mas, C. et al. Cross-sectional and longitudinal assessment of structural brain alterations in melancholic depression. Biol Psychiatry 69, 318–325 (2011).
Zhang, X. et al. Gray matter volume abnormalities in individuals with cognitive vulnerability to depression: a voxel-based morphometry study. J Affect Disord 136, 443–452 (2012).
Assaf, Y. & Pasternak, O. Diffusion tensor imaging (DTI)-based white matter mapping in brain research: a review. J Mol Neurosci 34, 51–61 (2008).
Taylor, W. D., Hsu, E., Krishnan, K. R. & MacFall, J. R. Diffusion tensor imaging: background, potential, and utility in psychiatric research. Biol Psychiatry 55, 201–207 (2004).
Beaulieu, C. The basis of anisotropic water diffusion in the nervous system - a technical review. NMR Biomed 15, 435–455 (2002).
Mamata, H. et al. High-resolution line scan diffusion tensor MR imaging of white matter fiber tract anatomy. AJNR Am J Neuroradiol 23, 67–75 (2002).
Shimony, J. S. et al. Quantitative diffusion-tensor anisotropy brain MR imaging: normative human data and anatomic analysis. Radiology 212, 770–784 (1999).
Zou, K. et al. Alterations of white matter integrity in adults with major depressive disorder: a magnetic resonance imaging study. J Psychiatry Neurosci 33, 525–530 (2008).
Zuo, N. et al. White matter abnormalities in major depression: a tract-based spatial statistics and rumination study. PLoS One 7, e37561 (2012).
Lai, C. H. & Wu, Y. T. Alterations in white matter micro-integrity of the superior longitudinal fasciculus and anterior thalamic radiation of young adult patients with depression. Psychol Med 44, 2825–2832 (2014).
Zhu, X. et al. Altered white matter integrity in first-episode, treatment-naive young adults with major depressive disorder: a tract-based spatial statistics study. Brain Res 1369, 223–229 (2011).
Versace, A. et al. Right orbitofrontal corticolimbic and left corticocortical white matter connectivity differentiate bipolar and unipolar depression. Biol Psychiatry 68, 560–567 (2010).
Choi, K. S. et al. Reconciling variable findings of white matter integrity in major depressive disorder. Neuropsychopharmacology 39, 1332–1339 (2014).
Murphy, M. L. & Frodl, T. Meta-analysis of diffusion tensor imaging studies shows altered fractional anisotropy occurring in distinct brain areas in association with depression. Biol Mood Anxiety Disord 1, 3 (2011).
Liao, Y. et al. Is depression a disconnection syndrome? Meta-analysis of diffusion tensor imaging studies in patients with MDD. J Psychiatry Neurosci 38, 49–56 (2013).
Wise, T. et al. Voxel-Based Meta-Analytical Evidence of Structural Disconnectivity in Major Depression and Bipolar Disorder. Biol Psychiatry [Epub ahead of print], doi: 10.1016/j.biopsych.2015.1003.1004 (2015).
Ashburner, J. & Friston, K. J. Voxel-based morphometry–the methods. Neuroimage 11, 805–821 (2000).
Smith, S. M. et al. Tract-based spatial statistics: voxelwise analysis of multi-subject diffusion data. Neuroimage 31, 1487–1505 (2006).
Radua, J. & Mataix-Cols, D. Voxel-wise meta-analysis of grey matter changes in obsessive-compulsive disorder. Br J Psychiatry 195, 393–402 (2009).
Murphy, M. L. et al. Neurotrophic tyrosine kinase polymorphism impacts white matter connections in patients with major depressive disorder. Biol Psychiatry 72, 663–670 (2012).
Guo, W. B. et al. Altered white matter integrity of forebrain in treatment-resistant depression: a diffusion tensor imaging study with tract-based spatial statistics. Prog Neuropsychopharmacol Biol Psychiatry 38, 201–206 (2012).
Han, K. M. et al. Cortical thickness, cortical and subcortical volume, and white matter integrity in patients with their first episode of major depression. J Affect Disord 155, 42–48 (2014).
Hayashi, K. et al. COMT Val158Met, but not BDNF Val66Met, is associated with white matter abnormalities of the temporal lobe in patients with first-episode, treatment-naive major depressive disorder: a diffusion tensor imaging study. Neuropsychiatr Dis Treat 10, 1183–1190 (2014).
Kieseppa, T. et al. Major depressive disorder and white matter abnormalities: a diffusion tensor imaging study with tract-based spatial statistics. J Affect Disord 120, 240–244 (2010).
Lyden, H. et al. Electroconvulsive therapy mediates neuroplasticity of white matter microstructure in major depression. Transl Psychiatry 4, e380 (2014).
Olvet, D. M. et al. A diffusion tensor imaging study of suicide attempters. J Psychiatr Res 51, 60–67 (2014).
Seok, J. H. et al. Effect of the COMT val158met polymorphism on white matter connectivity in patients with major depressive disorder. Neurosci Lett 545, 35–39 (2013).
Guo, W. B. et al. Altered white matter integrity in young adults with first-episode, treatment-naive, and treatment-responsive depression. Neurosci Lett 522, 139–144 (2012).
Korgaonkar, M. S. et al. Loss of white matter integrity in major depressive disorder: evidence using tract-based spatial statistical analysis of diffusion tensor imaging. Hum Brain Mapp 32, 2161–2171 (2011).
Wang, Y. F. et al. White matter abnormalities in medication-naive adult patients with major depressive disorder: Tract-based spatial statistical analysis. Neuroendocrinology Letters 35, 697–702 (2014).
Xiao, J., He, Y., McWhinnie, C. M. & Yao, S. Altered white matter integrity in individuals with cognitive vulnerability to depression: a tract-based spatial statistics study. Sci Rep 5, 9738 (2015).
Lacerda, A. L. et al. Anatomical MRI study of corpus callosum in unipolar depression. J Psychiatr Res 39, 347–354 (2005).
Sun, J., Maller, J. J., Daskalakis, Z. J., Furtado, C. C. & Fitzgerald, P. B. Morphology of the corpus callosum in treatment-resistant schizophrenia and major depression. Acta Psychiatr Scand 120, 265–273 (2009).
Macmaster, F. P., Carrey, N. & Marie Langevin, L. Corpus callosal morphology in early onset adolescent depression. J Affect Disord 145, 256–259 (2013).
Ballmaier, M. et al. Mapping callosal morphology in early- and late-onset elderly depression: an index of distinct changes in cortical connectivity. Neuropsychopharmacology 33, 1528–1536 (2008).
Kemp, A. et al. Age of onset and corpus callosal morphology in major depression. J Affect Disord 150, 703–706 (2013).
Xu, K. et al. Impaired interhemispheric connectivity in medication-naive patients with major depressive disorder. J Psychiatry Neurosci 38, 43–48 (2013).
Kumar, A. et al. Biophysical changes in normal-appearing white matter and subcortical nuclei in late-life major depression detected using magnetization transfer. Psychiatry Res 130, 131–140 (2004).
Tobias, M. C. et al. White-matter abnormalities in brain during early abstinence from methamphetamine abuse. Psychopharmacology (Berl) 209, 13–24 (2010).
Brambilla, P. M. N., Sassi, R. B., Mallinger, A. G., Frank, E., Keshavan, M. S. & Soares, J. C. Corpus callosum signal intensity in patients with bipolar and unipolar disorder. J Neurol Neurosurg Psychiatry 75, 221–225 (2004).
Tham, M. W., Woon, P. S., Sum, M. Y., Lee, T. S. & Sim, K. White matter abnormalities in major depression: evidence from post-mortem, neuroimaging and genetic studies. J Affect Disord 132, 26–36 (2011).
de Diego-Adelino, J. et al. Microstructural white-matter abnormalities associated with treatment resistance, severity and duration of illness in major depression. Psychol Med 44, 1171–1182 (2014).
Henderson, S. E. et al. A preliminary study of white matter in adolescent depression: relationships with illness severity, anhedonia, and irritability. Front Psychiatry 4, 152 (2013).
Axer, H. & Keyserlingk, D. G. Mapping of fiber orientation in human internal capsule by means of polarized light and confocal scanning laser microscopy. J Neurosci Methods 94, 165–175 (2000).
Jia, Z. et al. High-field magnetic resonance imaging of suicidality in patients with major depressive disorder. Am J Psychiatry 167, 1381–1390 (2010).
Jia, Z. et al. Impaired frontothalamic circuitry in suicidal patients with depression revealed by diffusion tensor imaging at 3.0 T. J Psychiatry Neurosci 39, 170–177 (2014).
Gutman, D. A., Holtzheimer, P. E., Behrens, T. E. J., Johansen-Berg, H. & Mayberg, H. S. A Tractography Analysis of Two Deep Brain Stimulation White Matter Targets for Depression. Biol Psychiatry 65, 276–282 (2009).
Taghva, A. S., Malone, D. A. & Rezai, A. R. Deep brain stimulation for treatment-resistant depression. World Neurosurg 80, S27 e17–24 (2013).
Tekin, S. & Cummings, J. L. Frontal-subcortical neuronal circuits and clinical neuropsychiatry: an update. J Psychosom Res 53, 647–654 (2002).
Cardoso de Almeida, J. R. & Phillips, M. L. Distinguishing between Unipolar Depression and Bipolar Depression: Current and Future Clinical and Neuroimaging Perspectives. Biol Psychiatry 73, 111–118 (2013).
Stroup, D. F. et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283, 2008–2012 (2000).
Du, M. et al. Brain grey matter volume alterations in late-life depression. J Psychiatry Neurosci 39, 397–406 (2014).
Radua, J. et al. Anisotropic kernels for coordinate-based meta-analyses of neuroimaging studies. Front Psychiatry 5, 13 (2014).
Radua, J. et al. A new meta-analytic method for neuroimaging studies that combines reported peak coordinates and statistical parametric maps. Eur Psychiatry 27, 605–611 (2012).
Lim, L., Radua, J. & Rubia, K. Gray matter abnormalities in childhood maltreatment: a voxel-wise meta-analysis. Am J Psychiatry 171, 854–863 (2014).
Wakana, S., Jiang, H., Nagae-Poetscher, L. M., van Zijl, P. C. & Mori, S. Fiber tract-based atlas of human white matter anatomy. Radiology 230, 77–87 (2004).
Radua, J. et al. Multimodal meta-analysis of structural and functional brain changes in first episode psychosis and the effects of antipsychotic medication. Neurosci Biobehav Rev 36, 2325–2333 (2012).
Acknowledgements
This study was supported by the National Natural Science Foundation (Grant Nos. 81220108013, 81227002 and 81030027) and the Program for Changjiang Scholars and Innovative Research Team in University (PCSIRT, Grant No. IRT1272) of China. Dr. Gong would also like to acknowledge the support from his Changjiang Scholar Professorship Award (Award No. T2014190) of China and the CMB Distinguished Professorship Award (Award No. F510000/G16916411) administered by the Institute of International Education, USA.
Author information
Authors and Affiliations
Contributions
Q.Y.G. conceived the project. G.X.C. and X.Y.H. designed the protocol and wrote the main manuscript. G.X.C., X.Y.H. and L.L. obtained the data. X.Q.H., S.L. and W.H.K. analysed the results. All authors reviewed the manuscript. H.A., F.B., Z.W.G. and Q.Y.G. revised the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Chen, G., Hu, X., Li, L. et al. Disorganization of white matter architecture in major depressive disorder: a meta-analysis of diffusion tensor imaging with tract-based spatial statistics. Sci Rep 6, 21825 (2016). https://doi.org/10.1038/srep21825
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep21825
- Springer Nature Limited
This article is cited by
-
Brain connectivity in major depressive disorder: a precision component of treatment modalities?
Translational Psychiatry (2023)
-
White matter predicts tDCS antidepressant effects in a sham-controlled clinical trial study
European Archives of Psychiatry and Clinical Neuroscience (2023)
-
White matter changes following electroconvulsive therapy for depression: a multicenter ComBat harmonization approach
Translational Psychiatry (2022)
-
Microstructural white matter alterations associated with migraine headaches: a systematic review of diffusion tensor imaging studies
Brain Imaging and Behavior (2022)
-
Concurrent alterations of white matter microstructure and functional activities in medication-free major depressive disorder
Brain Imaging and Behavior (2021)