Abstract
Studies on the muscular-deep fascial system which connects the upper eyelid, brow, and glabella, are lacking. This study aimed to explore the fine anatomy of the muscular-deep fascial system in the region between the eyebrow and the superior orbital margin. We included eight formalin–phenol-embalmed cadavers (16 sides of specimens), and categorized them into anatomical dissections and histological sections. Five cadavers (10 sides) were dissected for gross anatomical observation, whereas all soft tissues of the other three cadavers (6 sides) were dissected for tissue sectioning and histological analysis. Three tissue blocks and 16 strips in each block were trimmed, numbered, and sliced into these specimens. Hematoxylin–Eosin and Masson’s Trichrome staining were performed. In the region between the eyebrow and the superior orbital margin, the frontalis was covered by the orbicularis oculi. Fibers of the frontalis muscle penetrated into the orbicularis oculi muscle bundles, and crosslinked around the eyebrow level. Both the frontalis and the orbicularis oculi were attached to the thickened multilayered deep fascia in this region, which could be regarded as the muscular-deep fascial system. The muscular-deep fascial system connects the frontalis deep fascia and deep forehead compartments down to the orbicularis-supporting ligament. The precise anatomy of the muscular-deep fascial system in the region between the eyebrow and the superior orbital margin may provide a valuable reference for soft-tissue fixation and suspension in facial surgery.
Similar content being viewed by others
Introduction
The fine anatomical structure of the upper face and periorbital region gives it complex and dynamic characteristics1,2,3. It provides not only the greatest amount of emotional information per area, but also the region where facial aging signals are most obviously and easily detected4,5,6. Signs of aging in this area, including forehead and brow wrinkles, periocular wrinkles, ptosis, and upper eyelid skin laxity, are the result of the combined action of the overlying skin, muscle, aponeurosis, fascial system and bone7,8. Several plastic and aesthetic procedures, including autologous fat grafting, injection of hyaluronic acid or botulinum toxin, endoscopic eyebrow lifting, browpexy, blepharoplasty and so forth are available for the rejuvenation of the upper facial and periorbital rejuvenation9,10,11,12. The effects of these aesthetic procedures are achieved by adjusting the function and/or morphology of the anatomical structure in this region. Thus, the fine anatomy of the periorbital and upper facial regions is of important value, which can provide an important theoretical basis for the optimization of these surgical rejuvenation techniques for the upper facial and periorbital regions mentioned above.
Recent research has explored the fine anatomy of fat compartments, muscles, and fascia in the periorbital, glabellar and brow regions13,14,15,16. However, the muscular-deep fascial system in the region between the eyebrow and the superior orbital margin, which connects the upper eyelid, brow and glabella muscles, has not been described in detail thus far. Considering the lack of satisfactory anatomical descriptions of this muscular-deep fascial system in the previous literature, the present study attempts to clarify the anatomy of the muscles and deep fascial system in the region between the eyebrow and the superior orbital margin, and evaluate their relationship with neighboring vital structures via cadaveric dissection, so as to provide a concise foundation for safer and more effective brow-lifting and upper facial rejuvenation procedures.
Materials and methods
Cadaveric study sample
A total of 8 (16 sides of specimens) formalin–phenol-embalmed cadavers from individuals of Han Chinese ethnicity were acquired from the voluntary cadaver donation program at Peking University Health Science Center (Beijing, People’s Republic of China). This study followed the principles outlined in the Declaration of Helsinki, and conformed ethically to the Cadaver Dissection Regulations of the Peking University Health Science Center (number IRB00001052-21101; August 17, 2021). The informed consent of all body donors was obtained from the body subjects/and or their legal guardians/next of kin. Specimens were excluded if there was a history of previous upper facial and/or periorbital dissection or any signs of facial trauma. In total, 8 (16 sides of specimens) cadaver heads were dissected in this study. The same surgeon (Zhao) conducted all dissection procedures.
Anatomical dissection
The periorbital and upper face regions of 5 cadavers (10 sides of specimens) were carefully dissected for the evaluation of their anatomical structure. The incisions were made along the median line of the upper face, frontotemporal hairline, and ipsilateral palpebral margin, and the skin and subcutaneous adipose tissue were carefully peeled back to expose the frontalis and orbicularis oculi muscles. The frontalis muscle was then carefully dissected from the orbicularis oculi. For six of the specimens, the surgeon carefully dissected the frontalis muscle and the deep fascia from the hairline to the periorbital area. Then, the deep fascia was dissected from the periosteum carefully and separated obtusely from the hairline to the periorbital area. For each of the remaining four specimens, an additional vertical incision was made at the median line of each eyelid and across the forehead, eyebrow, and upper eyelid, to explore the anatomical relationships among the frontalis muscle, orbicularis oculi and deep fascia in this area more directly.
Histologic sections and analysis
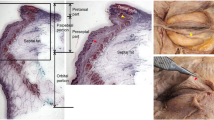
In the remaining three cadavers (6 sides), full-layer soft tissues were dissected in the following order to obtain square like full-layer soft tissue specimens. First, the frontal hairline was dissected from the midpoint of the frontal hairline to the temporal edge, then dissected down to the edge of the upper eyelid, cut inward to reach the median line of the face, and finally turned up to the hairline level. The full-layer soft tissue specimens were trimmed into 12-cm high and 6.4-cm wide blocks, with care to ensure that the major part of the upper eyelid, entire eyebrow and area from the brow to the frontal tubercle were all located within the trimmed soft-tissue specimen. Each specimen was then equally divided into three tissue blocks from the forehead region to the upper eyelid region (height 4 cm; length 6.4 cm), and the lower, middle, and upper parts were marked as blocks A, B, and C, respectively. In each tissue block, the soft tissue was cut vertically into strips from the brow side to the temporal side at every 4-mm stretch, and sequentially numbered from 1 to 16 (Fig. 1). All 48 soft-tissue strips were embedded in paraffin, and then, two 5-μm-thick slices were obtained from cross-sections through the middle of each strip via a Leica RM2255 slicer, and stained with hematoxylin–eosin (H&E) and Masson´s trichrome staining, respectively.
All the slices were scanned with a Hamamatsu Nano Zoomed slice scanner, and recorded by their strip number. For example, the first strip of Tissue Block A was named A-01, and the second strip was named A-02. The same number of strips from different tissue blocks were placed in the same vertical position.
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Cadaver Dissection Regulations of the Peking University Health Science Center (number IRB00001052-21101; August 17, 2021). The informed consent for publication of identifying information/images in an online open-access publication of all body donors was obtained from the body subjects/and or their legal guardians/next of kin.
Results
Gross anatomical observation
Anatomical dissections revealed the existence of a deep fascial system in the periorbital and upper face region, which was located between the frontalis and the periosteum. In the region between the eyebrow and the superior orbital margin, the deep fascia significantly thickened, the frontalis muscle was partially covered by the upper orbital part of the orbicularis oculi in this region, and the frontalis and the orbital part of the orbicularis oculi were both attached to the deep fascia (Fig. 2a and b).
A photo of the gross anatomy of Cadaver A. (a) and (b) shows the anatomical relationship between the frontalis muscle, orbicularis oculi and deep fascia in the region between the eyebrow and the superior orbital margin. (b) shows the tight connection between the frontal muscle and the orbicularis oculi muscle in this region. The black, blue, and red arrows indicate the frontalis muscle, orbicularis oculi, and thickened deep fascia, respectively.
The anatomic relationships among the frontalis muscle, the upper orbital part of the orbicularis oculi, and the deep fascia were more clearly observed through vertical incisions across the forehead, eyebrow and upper eyelid. The fasciculus of the frontalis muscle penetrated into the deep surface of the upper orbital part of the orbicularis oculi, and was attached to the deep fascia beneath it. The deep fascia begins to thicken significantly at the eyebrow level, and this thickening tends to extend to the superior orbital margin (Fig. 3).
A photo of the gross anatomy of Cadaver B showing the anatomical relationships among the frontalis muscle, orbicularis oculi and deep fascia in the region between the eyebrow and the superior orbital margin. The black, blue, white, and red arrows indicate the frontalis muscle, orbicularis oculi, preseptal fat pad, and thickened deep fascia, respectively.
Histological findings
Relationship between the frontalis and the orbicularis oculi
The anatomic relationship between the frontalis and the orbital part of the orbicularis oculi was observed in paraffin sections of strips A1–A16 of all specimens. In these sections, the frontalis showed cord-like longitudinal fibers, and the orbicularis oculi presented dot-like circular fibers. We observed that, in general, the frontalis was located deep to the orbicularis oculi; however, at the level of the eyebrow, the cord-like fibers of the frontalis started penetrating into the orbicularis oculi muscle bundles, and were interlaced and closely linked (Fig. 4a–d). And, some of the frontalis muscle fibers extend deep into the subdermal layer and closely connect with the septum of fat compartments. In addition, few frontalis muscle fibers were also found extending into the dermis (Fig. 5a and b).
The histological sections of strips A-03 (a), A-05 (b), A-07 (c), and A-11 (d) were 2.5 mm in scale. The left side of the section is near the orbit, and the right side is near the brow; the red arrow represents the level of the eyebrow. In all these sections, at the level of the eyebrow, the cord-like fibers of the frontalis penetrated into the orbicularis oculi muscle bundles, and they were interlaced and closely linked.
Characteristics of the deep fascial system
Through the continuous observation of tissue blocks C → B → A, we found that the deep multilayered fascial structure originated from the epicranial aponeurosis. In the frontal area, fat compartments existed between the fascial layers; however, at approximately 2 cm above the eyebrow, the fascia became denser as the fat compartments gradually disappeared. And, at the eyebrow level, the fat compartments were again found to exist between the fascial layers.
The deep fascia is composed of multiple layers of longitudinal fibers. In the region above the eyebrow, these multiple layers of fascia were densely distributed; however, at the level of the eyebrows to the level of the orbital margin, fat compartments were distributed between the fascial layers, and their location was consistent with the fascia thickening observed on gross anatomy (Fig. 6). In 2008, Ghavami17 proposed the existence of an orbicularis-supporting ligament located deep to the orbicularis oculi and preseptal fat pad. In the present study, we observed this orbicularis-supporting ligament, which isolated the preseptal fat pad from the thickened area of the sub-brow deep fascia. Despite being frequently referred to as the “ROOF (retro-orbicularis oculi fat)” system as a whole in the previous literature18, we found obvious histological differences between the multilayered deep fascial structure and the preseptal fat pad. The multilayered fascia was relatively dense and it thickened at the region between the brow and the superior orbital margin, whereas the septae of the fat compartment were interspersed between the fascia. However, the septal walls within the preseptal fat were thin, and the compartments were clustered (Fig. 6).
Relationship and histological characteristics of the preseptal fat, orbicularis-retaining ligament, and multilayer deep fascia. The red arrow represents the level of the eyebrow. The area within the green solid circle is the preseptal fat, the area between the blue-dotted lines is the orbicularis-retaining ligament, and the area within the black-dotted circle is the multilayer deep fascia.
Discussion
In the present study, we examined the gross anatomy and histological structures of paraffin sections of the muscular-deep fascial system in the region between the eyebrow and the superior orbital margin, and elucidated three primary findings.
First, a muscular-multilayered deep fascial system was found in the region between the eyebrow and the superior orbital margin. In this region, the frontalis penetrats into the orbicularis oculi muscle bundles, and both the muscles are interlaced and closely linked, and attached to the multilayered fascia on the deep side. This finding may suggest a new possible suspension level for ptosis correction procedures. In surgery for severe ptosis correction, the area above the eyebrow level is usually dissected to expose the frontalis muscle for the suspension of the levator palpabrae muscle19. The frontalis muscle fibers located in the area between the eyebrow and the superior orbital margin may serve as an alternative suspension point. Suspension of the levator palpabrae muscle in this area can reduce the dissection step of the area above the eyebrow, thus simplifying the surgical procedure and reducing surgical trauma.
Furthermore, the multilayered fascial structure may not simply be summarized as a continuation of the orbital septum. We found that the multilayered fascial structure extended along the deep galea to the orbital septum, which is more complex than a mere septum. In the upper facial area, thin plate-like fat layers are distributed among these multilayered fascial structures to form the thickened fascial structure between the eyebrow and the superior orbital margin area and the deep forehead compartment, respectively. The complex of dense fibers and thin fat layers of the multilayered fascial structure was especially thickened below the intersection of the orbicularis oculi and frontalis muscles. At 1–2 cm above the level of intersection, the fat layers gradually disappeared to form a firm deep fascia. In anatomical research of brow compartments through images from CT scans taken by Cotofana20, the researcher reported that the inferior boundary of the deep lateral brow compartments was formed by a septum that was an average distance from the supraorbital rim of 1.5 cm in the midline and 3.0 cm at its lateral end. This finding is consistent with the location of the firm deep fascia that we observed in the present study. According to its multilayered and dense anatomical characteristics, we believe that the thickened fascia in the region between the eyebrow and the superior orbital margin might be a fine fixation point of soft-tissue suspension for upper facial rejuvenation surgery. Transpalpebral browpexy is a brow-lifting technique that has been increasingly applied in recent years for upper face rejuvenation21,22. After blepharoplasty, dissection continues in the suborbicularis oculi plane between the middle and lateral thirds of the eyebrow to the supraorbital rim. A suspension suture is inserted into the overlying muscle/subcutis tissue underneath the eyebrow affixed to the periosteum of the frontal bone sufficiently high to achieve the desired form and elevation21. In this procedure, the multilayered-deep fascial system we found in this study may have served together with the periosteum as a fixed suspension structure. Infra-eyebrow blepharoplasty is another popular surgical technique for upper eyelid rejuvenation, especially for Asian populations. In this procedure, the excision was usually fusiform shaped from near the inner lateral tip of the eyebrow to the lateral tip of the eyebrow or slightly beyond the lateral tip, and the upper excision line should be made along the lower edge of the eyebrow. The skin and redundant orbicularis oculi muscle were excised, and the skin and subcutaneous tissue of the upper and lower excision lines were sutured23,24. However, after simply suturing the skin and subcutaneous tissue without suspension, droopy eyebrows may appear postoperatively. In 2013, Fang et al.23 reported an improved technique for this classical surgery. Aftera fusiform-shaped excision of the skin and subcutaneous tissue was made, the orbicularis oculi were partially excised and the retro-orbicularis oculi fat was dissected and trimmed; then, the periorbital septum was partly released. The undersurface of the orbicularis muscle was fixed to the periosteum and connective tissue above the supraorbital rim. While, Shu et al.24 elevated and sutured the orbicularis oculi in the inferior flap to the frontalis. These classic upper facial rejuvenation procedures mentioned above may both involve the multilayered fascial structures when soft tissue suspension is performed. The fine anatomy of the multilayered facial structure that weelaborated on in the present study may provide valuable consideration for soft-tissue fixation and the suspensory position of the blepharoplasty and browpexy techniques.
We also found that, the thickened fascial structure in the area between the eyebrow and the superior orbital margin could not be simply considered a part of the “ROOF” system together with the preseptal fat pad, as they have different structural characteristics, and may require different surgical approaches. The fat compartment between the muscles (the orbicularis oculi and frontalis muscles) and the orbital septum/frontalis fascia have been collectively referred to as the “ROOF” system in recent literatures18,25,26. In 2008, Ghavami et al.17 reported a ligamentous system that arises from the inferior orbital rim, and called it the orbicularis retaining ligament. This ligament spans the entire circumference of the orbit from the medial to the lateral canthi, and arises from the orbital rim several centimeters above the inferior edge. In the present study, we observed the existence of this retaining ligament, which clearly separates the so-called “ROOF” system. And, there are obvious differences in the distributions of fat and fibers between the preseptal fat pad, located infra-anterior to the retaining ligament, and the sub-brow fat pad, located supero-posterior to the retaining ligament. In the area between the eyebrow and the superior orbital margin, we noted the distribution of multiple, dense longitudinal fibers and thin plate-like fat layers among the fascia. However, in the preseptal fat pad, the fat compartments are clustered and the septal fibers are obviously thinner, which canbe clearly differentiated on histological sections. The dense facia system may provide good attachment points for “ROOF” suspension in upper eyelid plastic surgery. When performing surgery in this area, careful operation should be taken to distinguish between the “ROOF” and the fascial system to avoid additional damage tothis deep multilayered fascial structure.
Moreover, this study provides a reference for the extent of dissection of the infra-eyebrow multilayer fascia in plastic surgery. Because the multilayered thickened fascia connects the preseptal fat pad and deep forehead compartment, we suggest that surgeons may need to avoid damage to this area to prevent periorbital soft-tissue ptosis. Endoscopic brow lift with minimally invasive and hidden incision characteristics is a popular procedure for brow and eyebrow rejuvenation. Dissection is commonly performed along the periosteal subgaleal plane. After complete dissection, the brow soft tissue is integrally suspended to achieve relief from wrinkles and ensure eyebrow lifting27,28. Some surgeons choose to cut the frontalis in a linear, strip, or reticular manner to further relieve the transverse wrinkles of the forehead29. However, a shallow eye socket is one of the postprocedural complications. Considering the anatomical findings of this study, a possible reason for the shallow eye socket could be that the sub-brow multilayer deep fascia is severed during the dissection of the frontalis muscle through the periosteal approach. The soft tissue beneath the incision loses the mechanical support of the dense fascia; therefore, the upper eyelid sags, which results in a shallow eye socket. Thus, on the basis of our findings in the present study, reaffixation and resuspension of the deep multilayered fascial structure after dissection of the frontalis may be a way to prevent this complication.
This study has limitations because fresh specimens were not used. The actual thickness of fat, muscles, and fascia in the specimens treated with formalin–phenol may differ from those in the fresh cadaveric specimens. However, a strength of the present study was that the fine anatomy of the region between the eyebrow and the superior orbital margin was revealed. We found a compound thickened structure composed of multilayered fibers and fat compartments deep to the intersection of the orbicularis oculi and frontalis muscles. This structure, which could be regarded as the multilayered muscular-deep fascial system, connects to the frontalis deep fascia and the deep forehead compartments, and down to the orbicularis supporting ligament. This precise anatomy may provide a valuable clinical basis for soft-tissue fixation and suspension of upper face rejuvenation techniques.
Data availability
The corresponding author should be contacted if someone wants to request the data from this study.
References
Cotofana, S. et al. The anatomy behind eyebrow positioning: A clinical guide based on current anatomic concepts. Plast. Reconstr. Surg. 149, 869–879 (2022).
Packiriswamy, V., Kumar, P. & Bashour, M. Anthropometric and anthroposcopic analysis of periorbital features in Malaysian population: An inter-racial study. Facial Plast. Surg. 34, 400–406 (2018).
Langelier, N., Beleznay, K. & Woodward, J. Rejuvenation of the upper face and periocular region: Combining neuromodulator, facial filler, laser, light, and energy-based therapies for optimal results. Dermatol. Surg. 42(Suppl 2), S77–S82 (2016).
Caldara, R., Zhou, X. & Miellet, S. Putting culture under the “spotlight” reveals universal information use for face recognition. PLoS ONE. 5, e9708 (2010).
Gosselin, F. & Schyns, P. G. Bubbles: A technique to reveal the use of information in recognition tasks. Vis. Res. 41, 2261–2271 (2001).
Boonipat, T. et al. Impact of surgical rejuvenation on visual processing and character attribution of periorbital aging. Plast. Reconstr. Surg. 150, 539–548 (2022).
Lambros, V. Observations on periorbital and midface aging. Plast. Reconstr. Surg. 120, 1367–1376 (2007).
Wang, J. et al. A Randomized, controlled study comparing subbrow blepharoplasty and subbrow blepharoplasty combined with periorbital muscle manipulation for periorbital aging rejuvenation in Asians. Aesthet. Plast. Surg. 44, 788–796 (2020).
Kane, M. A. C. Nonsurgical periorbital and brow rejuvenation. Plast. Reconstr. Surg. 135, 63–71 (2015).
Xu, L. et al. Aesthetic analysis of alteration of eyebrow and forehead position after endoscopic eyebrow lift. Aesthet. Plast. Surg. 46, 2258–2265 (2022).
Huang, P. J. et al. Objective comparison of eyebrow position after internal and external browpexy. Plast. Reconstr. Surg. 152, 414e–423e (2023).
Wang, J., Su, Y., Zhang, J., Guo, P. & Song, B. Subbrow blepharoplasty combined with periorbital muscle manipulation for periorbital rejuvenation in Asian women. Plast. Reconstr. Surg. 144, 760e–769e (2019).
Sykes, J. M. et al. Upper face: Clinical anatomy and regional approaches with injectable fillers. Plast. Reconstr. Surg. 136, 204S-218S (2015).
Zins, J. E., Grow, J. & Cakmakoglu, C. Brow anatomy and aesthetics of the upper face. Clin. Plast. Surg. 49(3), 339–348 (2022).
Yi, K. H., Lee, J. H., Hu, H. W. & Kim, H. J. Anatomical proposal for botulinum neurotoxin injection for glabellar frown lines. Toxins 14, 268 (2022).
Neves, J. C., Arancibia-Tagle, D., Medel-Jiménez, R. & Vásquez, L. M. Periorbital surgical anatomy. Facial Plast. Surg. 36, 317–328 (2020).
Ghavami, A. et al. The orbicularis retaining ligament of the medial orbit: Closing the circle. Plast. Reconstr. Surg. 121, 994–1001 (2008).
Wang, X. & Wang, H. Anatomical study and clinical observation of retro-orbicularis oculi fat (ROOF). Aesthet. Plast. Surg. 44(1), 89–92 (2020).
Zhang, D., Guo, B. & Cai, W. Effect of frontal muscle aponeurosis flap suspension surgery for severe congenital ptosis in children. Minerva Pediatr. 71(4), 358–361 (2019).
Cotofana, S. et al. An update on the anatomy of the forehead compartments. Plast. Reconstr. Surg. 139(4), 864e–872e (2017).
Iblher, N., Manegold, S., Porzelius, C. & Stark, G. B. Morphometric long-term evaluation and comparison of brow position and shape after endoscopic forehead lift and transpalpebral browpexy. Plast. Reconstr. Surg. 130, 830e–840e (2012).
Nemet, A. Y. Brow ptosis: Is transblepharoplasty internal browpexy suitable for everyone?. J. Craniofac. Surg. 30, 2425–2428 (2019).
Fang, Y. H., Liao, W. C. & Ma, H. Infraeyebrow blepharoplasty incorporated browpexy in an Asian population. Ann. Plast. Surg. 71(Suppl 1), S20–S24 (2013).
Shu, M. et al. A novel supra-brow combined with infra-brow lift approach for Asian women. Aesthet. Plast. Surg. 40, 343–348 (2016).
Zhang, Y. S. et al. Local retro-orbicularis oculus fat (ROOF) resection in upper blepharoplasty: A retrospective evaluation study of 65 bilateral upper blepharoplasties. J. Plast. Reconstr. Aesthet. Surg. 72, 1373–1378 (2019).
Wang, X. & Wang, H. Anatomical study and clinical observation of retro-orbicularis oculi fat (ROOF). Aesthet. Plast. Surg. 44, 89–92 (2020).
Rohrich, R. J. & Cho, M. J. Endoscopic temporal brow lift: Surgical indications, technique, and 10-year outcome analysis. Plast. Reconstr. Surg. 144(6), 1305–1310 (2019).
McKinney, P., Celetti, S. & Sweis, I. An accurate technique for fixation in endoscopic brow lift. Plast. Reconstr. Surg. 97, 824–827 (1996).
Wang, G., Tao, L. & Xie, H. A novel endoscopic forehead lift technique for patients with upper facial wrinkles: Morphometric evaluation and patient-reported outcome using FACE-Q scales. Facial Plast. Surg. 36, 226–234 (2020).
Author information
Authors and Affiliations
Contributions
S.Y. contributed to study design, data collection, data analysis, and manuscript writing. G.W. contributed to data collection, data analysis, anatomical manipulation and specimen collection, and manuscript writing. Z.Z. contributed to study conception, study design, data analysis, and data interpretation. W.Z. contributed to study conception, study design, anatomical manipulation and specimen collection, and data interpretation.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Yin, S., Wang, G., Zhao, Z. et al. The muscular-deep fascial system: new findings on the anatomy of the structure attached to the superior orbital margin. Sci Rep 14, 21530 (2024). https://doi.org/10.1038/s41598-024-72443-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-72443-7
- Springer Nature Limited