Abstract
We report subpopulations of airway parasympathetic neurons expressing substance P, neuronal nitric oxide synthase, and tyrosine hydroxylase, highlighting unexplored heterogeneity in this population. These neurotransmitter-specific subpopulations did not form intraganglionic interneurons, but rather, extended outside the ganglia, into the airways, to distant innervation targets. Our experiments demonstrate the utility of multicolor labeling to characterize airway innervation, allowing us to confirm the extensive heterogeneity of postganglionic parasympathetic neurons. These methods will facilitate future investigations of neurophysiology and neural contributions to airway disease.
Similar content being viewed by others
Introduction
Airway parasympathetic neurons are primarily cholinergic, releasing acetylcholine onto muscarinic receptors on airway smooth muscle to elicit bronchoconstriction and mucus secretion. However, immunostaining in human and ferret airways has also identified subsets of airway neurons that express substance P (SP)1,2,3, neuronal nitric oxide synthase (nNOS)2,4, and tyrosine hydroxylase (TH)5. The functions and innervation targets of these neuronal subpopulations remain unknown. Intriguingly, the prevalence of these unique neuronal subpopulations is increased in disease states, including increases in substance P-expressing neurons in ozone-mediated airway hyperreactivity6 and increases in tyrosine hydroxylase-expressing neurons post-lung transplant5. Understanding the connectivity of these subpopulations will provide new insights into their function and role in airway pathophysiology.
Multicolor labeling of nerves, such as in Brainbow mice7, allows distinct nerve processes in close proximity to be distinguished and traced to their target destinations. This technique generates fluorescent labeling over a wide spectrum of colors in Thy1 + neurons by using random combinations of three fluorophores. Notably, the original Brainbow technique cannot be applied to the study of airway nerves because it utilizes a Thy1 promoter to drive fluorophore expression, and the Thy1 promoter is not expressed in postganglionic parasympathetic nerves8. Thus, we employed a combinatorial multicolor viral vector labeling strategy, as has been employed in other organs9. In this approach, mice are simultaneously injected with three adeno-associated virus (AAV) vectors, each of which expresses a different fluorophore. Transduction produces a stochastic distribution of vector genome copies encoding fluorophores within each target cell and results in a wide variety of colors across neurons that can be distinguished and traced. Here, we first established the tropism of AAV9 vectors for parasympathetic nerves in the airways. We subsequently used immunohistochemistry to identify the cell bodies of SP-, nNOS-, and TH-expressing neurons within murine parasympathetic ganglia and applied AAV9-mediated combinatorial multicolor viral vector nerve labeling to trace individual neuronal processes and determine whether these cells represented intra-ganglionic interneurons or projected to more distant targets.
Materials and methods
Animals
Experiments used 8-week-old C57BL/6 mice or offspring from a cross between CHAT-Cre (#028861) and CH2-EYFP (#024109) mice from Jackson Labs. All mice were housed communally with unlimited access to food and water and 12 h light/dark cycle. Male and female mice were used for quantification of neurons expressing SP, nNOS, and TH, male mice were used for viral vector and tracing studies.
Plasmids
AAV vector genome plasmids harboring CAG-driven mNeonGreen, mRuby2, and mTurquoise2 transgene cassettes were purchased from Addgene. pAAV-CAG-mNeonGreen was a gift from Pantelis Tsoulfas (RRID:Addgene_124101). pAAV-CAG-mTurquoise2 (RRID:Addgene_99122) and pAAV-CAG-mRuby2 (RRID:Addgene_99123) were a gift from Viviana Gradinaru (Fig. 1a).
Multicolor nerve labeling approach and identification of parasympathetic subpopulations. (a,b) Schematic of multicolor AAV vector approach and AAV vector genome plasmids. Mouse airways before (c) and after (d) passive clearing in Ce3D. (e) Whole mouse trachea and lungs showing multicolor parasympathetic ganglia.
Cell culture conditions and experiments
HEK293 cells were maintained in Dulbecco’s Modified Eagle’s Medium (Lonza) supplemented with 10% fetal bovine serum (Sigma-Aldrich), 1% L-glutamine (Lonza), and 1% penicillin–streptomycin (Lonza). mNeonGreen, mRuby2, and mTurquoise2 plasmids were independently transfected into HEK293 cells using Lipofectamine 2000 (Thermo Fisher) with 400 ng plasmid per well on an 8-well slide. Cells were imaged using confocal microscopy after 48 h. Microscope settings were optimized to limit bleed-through (Supplementary Fig. 1).
AAV9 vector production, purification, titration, and administration
We produced AAV9 vectors in HEK293 cells (AAV-293, Agilent) using an adenovirus-free triple transfection method followed by polyethylene glycol 8000 precipitation and purification by two rounds of cesium chloride ultracentrifugation10. The final vector excipient was 5% sorbitol in PBS supplemented with 0.001% Pluronic-F68. Vectors were titered by radioactive dot blot assay11 and an equimolar mixture of mNeonGreen, mRuby2, and mTurquoise2 AAV9 vectors was administered intravenously via lateral tail vein without sedation at a total dose of 3 × 1011 to 3 × 1012 vg per mouse (Fig. 1b). For initial tests of viral dosage, AAV9 vectors expressing GFP were administered at doses of 5 × 1010 to 5 × 1012. Animals were euthanized 21 days after viral injection.
Tissue immunohistochemistry, optical clearing and imaging of airway nerves
Mice were euthanized with pentobarbital (150 mg/kg i.p.) and perfused with PBS. Tracheas were excised and stored at 4 °C in Zamboni fixative (Newcomer Supply) overnight. For investigation of vector uptake into other neural types, DRGs, vagal ganglia, and superior cervical ganglia were also excited, and tissues were processed in the same manner. To image fluorescent nerves, tissues were washed with TBS and passively cleared in N-methylacetamide/Histodenz (Ce3D)12 overnight (Fig. 1c,d). For immunohistochemistry experiments, tracheas were blocked overnight with 4% goat serum, 1% Triton X-100, and 5% powdered milk, then incubated for 4 h at 4 °C with antibodies against PGP9.5 (rabbit anti-human PGP9.5, 1:500; Millipore AB1761-I), substance P (rat anti-SP, 1:500; BD Pharmigen 556312), neuronal nitric oxide synthase (rabbit anti-nNOS, 1:100; Cell Signal C7D7), or tyrosine hydroxylase (rabbit anti-TH, 1:500, Pel Freez P40101). Tracheas were washed and incubated overnight with secondary antibodies (Alexa goat anti-rat 647, 1:1,000; Alexa goat anti-rabbit 647, 1:1,000; Alexa goat anti-chicken 488, 1:1,000; Invitrogen) before clearing overnight in Ce3D. Tissues were mounted in Ce3D on slides in silicon wells (Grace Labs) and imaged using an LSM 900 confocal microscope with four separate lasers and acquisition tracks: 405 nm (detection wavelengths 467–503), 488 nm (516–526), 561 nm (576–619) and 640 nm (645–700). Images were acquired as z-stacks, with single plane and maximum intensity projections used for visualization. Imaris and Imaris Stitcher software were used for 3D visualization.
nTracer analysis of parasympathetic nerve morphology
Tracing studies were performed on 8-bit images using FIJI software with the nTracer plugin13. Cell bodies for SP, nNOS, and TH neurons were identified with immunofluorescent labeling. Traces were created around the cell bodies of neurons and followed axons through each image. User inputs for points along the axon were verified through three-channel color intensity analysis in nTracer. Final traces represent a path of pixels with matching intensity in each color channel between user-identified points.
Statistical analysis
Fluorescence intensity data for multicolor cell bodies was not normally distributed (D’Agostino and Pearson test), and were analyzed using a Kruskal–Wallis test with Dunn’s post-hoc using GraphPad Prism software. The study was carried out in compliance with ARRIVE guidelines14.
Regulatory
All methods were approved by the Oregon Health & Science University’s Institutional Animal Care and Use Committee and Institutional Biosafety Committee and were performed in accordance with the relevant guidelines and regulations.
Results
Airway postganglionic parasympathetic neurons express substance P, neuronal nitric oxide synthase, and tyrosine hydroxylase
Trachea and primary bronchi from wild type C57BL/6 mice were labeled with antibodies against PGP9.5 and either SP, nNOS, or TH. Small numbers of postganglionic parasympathetic cell bodies, identified based on morphology and location within tissue, stained positively for each of these neurotransmitter markers (Fig. 2). The number of positive neurons varied between mice, with SP positive neurons representing (7 ± 2.0, n = 24 mice), nNOS (19.1 ± 6.6, n = 10), and TH (7.2 ± 3.1, n = 10) neurons per mouse (Fig. 2d).
AAV9 transduces airway parasympathetic neurons
We investigated the efficacy of using AAV9 viral capsids to transduce airway parasympathetic neurons. AAV9 viral capsids containing GFP driven by a CAG promoter were injected intravenously into 8 week old C57BL/6 mice at variable doses. AAV9-mediated transduction efficiency of airway parasympathetic neurons was low when a systemic dose of 5 × 1010 vg was used, but increased to nearly one hundred percent transduction efficiency at a dose of 5 × 1012 vg (Fig. 3).
Multicolor labeling identifies individual airway parasympathetic neuronal cell bodies and their processes
Three AAV plasmids from Addgene expressing the fluorescent proteins mNeonGreen, mRuby2, and mTurquoise2 were packaged into AAV9 viral capsids and injected intravenously into mice. Tissues were passively cleared by immersion in Ce3D solution to preserve endogenous fluorescence. Imaging revealed multicolor labeling of parasympathetic neurons, as identified by anatomical location (Fig. 1e). Sensory and sympathetic neurons also showed vector uptake, although these populations were not used for further tracing studies (Fig. 4). Increased viral doses increased the range of fluorescence colors as well as the intensity, although a total dose of 1 × 1012 vg showed the greatest color spread (Fig. 5). We used the nTracer plugin for FIJI to semi-manually trace axons (Fig. 6).
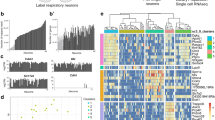
Fluorescence intensity of parasympathetic neurons dependent on viral dose. (a) Representative images of ganglia from three viral doses. (b) Fluorescence intensity represents the average intensity in a single nerve soma with the three color channels added together. Doses compared using a Kruskal–Wallis test with Dunn’s post-hoc test. *p < 0.01, ****p < 0.0001. n = 41–139. (c) Ternary plots for each dose were used to assess color spread, with the normalized fluorescent intensity of each neuron cell body plotted as a proportion of the three possible colors. Color variation was smaller (points clustering towards the center of the chart) in the high dose, was skewed toward the Turquoise vector in the low dose, and was most evenly distributed in the middle dose.
Substance P, nNOS, and tyrosine hydroxylase do not represent intra-ganglionic interneurons
We co-stained AAV9-labeled tracheas with antibodies against SP, nNOS, or TH using secondary antibodies in the far-red spectrum. We identified a single SP-positive parasympathetic neuron (Fig. 7a), plus two neurons labeled with nNOS, and two with TH. The SP-positive neuron was not part of a ganglion. Neurites of nNOS and TH-positive nerves exited their respective ganglia, rather than terminating within the ganglia as interneurons (Fig. 7b,c). Co-staining for substance P in mice with GFP driven by the choline acetyltransferase (CHAT) promoter was used in addition to anatomical location around the airways to confirm the parasympathetic nature of these neurons (Fig. 8).
Tracheas immunolabeled for substance P (a), neuronal nitric oxide synthase (b), and tyrosine hydroxylase (c). Left column shows immunolabeling in a single plane. Middle column shows multicolor labeling of neurons in a maximum intensity projection. Right column shows traces of cell bodies and axons of labeled neurons. Two axons of very similar color are present in the substance P image, however only one originates from the cell body that is shown, as can be seen more clearly in a 3D/orthogonal view (see supplementary Fig. 2).
Examples of substance P (blue) nerves in parasympathetic ganglia in mice with CHAT driving expression of EYFP (green) co-stained with PGP9.5 (red). (a) A parasympathetic ganglion with three cell bodies and a single substance P neuron both expressing EYFP. (b) A densely innervated parasympathetic ganglion with one of its neurons expressing substance P and all expressing EYFP.
Discussion
This study is the first demonstration of nNOS- and TH-expressing neurons in airway parasympathetic ganglia of mouse airways, and confirms reports of mouse parasympathetic SP expression. Our technique has exciting potential for studying the role of these neurons in airway disease.
Increased substance P in parasympathetic neurons, with pro-inflammatory and neurotransmitter roles, may have a role in airway hyperreactivity6. Nitric oxide is a bronchodilator, usually produced by a population of neurons with cell bodies located in the esophagus15. Tyrosine hydroxylase produces dopamine, epinephrine, and norepinephrine, and is usually found in sympathetic nerves, which can suppress airway parasympathetic nerves, and inhibit bronchoconstriction. While one possibility for the physiologic effects of these neurons is that they function as interneurons within ganglia, our studies show that processes from these neurons predominantly project outside their ganglia of origin to innervate distant targets.
Previous studies have seen parasympathetic neurons synapsing onto one another between ganglia16, but did not identify whether those nerves expressed neurotransmitters other than acetylcholine. While none of the SP, TH or nNOS neurons we identified projected to other parasympathetic neurons within their own ganglia, projection to parasympathetic neurons in other ganglia cannot be ruled out. Other neuropeptides, such as VIP and NPY, have also been identified in rodent and human parasympathetic ganglia2,4,17, and would be interesting to investigate with this method in future studies.
Our results indicate, for the first time, that AAV9 is capable of driving expression of fluorescent proteins in airway nerves after intravenous injection. Multicolor labeling of airway neurons using viral vectors represents a significant step forward in airway innervation research, especially given its versatility and applicability in larger animal models.
References
Dey, R. D., Hoffpauir, J. & Said, S. I. Co-localization of vasoactive intestinal peptide- and substance P-containing nerves in cat bronchi. Neuroscience 24, 275–281 (1988).
Dey, R. D. et al. Neurochemical characterization of intrinsic neurons in ferret tracheal plexus. Am. J. Respir. Cell Mol. Biol. 14, 207–216 (1996).
Scott, G. D., Blum, E. D., Fryer, A. D. & Jacoby, D. B. Tissue optical clearing, three-dimensional imaging, and computer morphometry in whole mouse lungs and human airways. Am. J. Respir. Cell Mol. Biol. 51, 43–55 (2014).
Fischer, A., McGregor, G. P., Saria, A., Philippin, B. & Kummer, W. Induction of tachykinin gene and peptide expression in guinea pig nodose primary afferent neurons by allergic airway inflammation. J. Clin. Investig. 98, 2284–2291 (1996).
Springall, D. R. et al. Persistence of intrinsic neurones and possible phenotypic changes after extrinsic denervation of human respiratory tract by heart-lung transplantation. Am. Rev. Respir. Dis. 141, 1538–1546 (1990).
Wu, Z.-X., Satterfield, B. E. & Dey, R. D. Substance P released from intrinsic airway neurons contributes to ozone-enhanced airway hyperresponsiveness in ferret trachea. J. Appl. Physiol. 95, 742–750 (2003).
Livet, J. et al. Transgenic strategies for combinatorial expression of fluorescent proteins in the nervous system. Nature 450, 56–62 (2007).
Tsuriel, S., Gudes, S., Draft, R. W., Binshtok, A. M. & Lichtman, J. W. Multispectral labeling technique to map many neighboring axonal projections in the same tissue. Nat. Methods 12, 547–552 (2015).
Chan, K. Y. et al. Engineered AAVs for efficient noninvasive gene delivery to the central and peripheral nervous systems. Nat. Neurosci. 20, 1172–1179 (2017).
Earley, L. F. et al. Adeno-associated virus (AAV) assembly-activating protein is not an essential requirement for capsid assembly of AAV serotypes 4, 5, and 11. J. Virol. 91, e01980-16 (2017).
Powers, J. M., Chang, X. L., Song, Z. & Nakai, H. A quantitative dot blot assay for AAV titration and its use for functional assessment of the adeno-associated virus assembly-activating proteins. J. Vis. Exp. https://doi.org/10.3791/56766 (2018).
Li, W., Germain, R. N. & Gerner, M. Y. Multiplex, quantitative cellular analysis in large tissue volumes with clearing-enhanced 3D microscopy (Ce3D). Proc. Natl. Acad. Sci. USA. 114, E7321–E7330 (2017).
Roossien, D. H. et al. Multispectral tracing in densely labeled mouse brain with nTracer. Bioinformatics 35, 3544–3546 (2019).
du Sert, N. P. et al. The ARRIVE guidelines 2.0: Updated guidelines for reporting animal research. PLoS Biol. 18, e3000410 (2020).
Canning, B. J. & Undem, B. J. Relaxant innervation of the guinea-pig trachealis: Demonstration of capsaicin-sensitive and -insensitive vagal pathways. J. Physiol. 460, 719–739 (1993).
Coburn, R. F. & Kalia, M. P. Morphological features of spiking and nonspiking cells in the paratracheal ganglion of the ferret. J. Comp. Neurol. 254, 341–351 (1986).
Richardson, R. J., Grkovic, I. & Anderson, C. R. Immunohistochemical analysis of intracardiac ganglia of the rat heart. Cell Tissue Res. 314, 337–350 (2003).
Acknowledgements
We thank the Oregon Health & Science University Advanced Light Microscopy core, especially Stephanie Kaech-Petrie, Brian Jenkins, and Crystal Shaw for their assistance with imaging. Many thanks to Dawen Cai for his guidance and technical support using nTracer software. The distribution of nTracer is partially supported by grant funding from NSF-1707316 Neunex MINT.
Funding
This work was supported by the National Institutes of Health [HL131525, HL144008, AI152498, HL145906].
Author information
Authors and Affiliations
Contributions
A.B.P., S.J.H., K.M.L., M.G.D., H.N., A.D.F., and D.B.J. designed the studies. A.B.P., K.M.L., U.D., and B.J.P. performed immunohistochemistry experiments and analysis. S.J.H. and H.N. produced and administered AAVs. A.B.P. conducted nerve tracing studies. A.B.P. and S.J.H. prepared figures and wrote the manuscript. All authors contributed to the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Pincus, A.B., Huang, S.J., Lebold, K.M. et al. Multicolor labeling of airway neurons and analysis of parasympathetic heterogeneity. Sci Rep 12, 5006 (2022). https://doi.org/10.1038/s41598-022-08655-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-08655-6
- Springer Nature Limited