Abstract
The appropriate timing for initiating renal replacement therapy (RRT) in critically ill patients with acute kidney injury (AKI) remains unknown. This meta-analysis aims to assess the efficacy of early initiation of RRT in critically ill patients with AKI. The Pubmed, Embase and Cochrane databases were searched up to August 13, 2019. Only randomized controlled trials (RCTs) comparing the effects of early and late RRT on AKI patients were included. The primary outcome was 28-day mortality. Eleven RCTs including 1131 and 1111 AKI patients assigned to early and late RRT strategies, respectively, were enrolled in this meta-analysis. The pooled 28-day mortality was 38.1% (431/1131) and 40.7% (453/1111) in the patients assigned to early and late RRT, respectively, with no significant difference between groups (risk ratio (RR), 0.95; 95% CI, 0.78–1.15, I2 = 63%). No significant difference was found between groups in terms of RRT dependence in survivors on day 28 (RR, 0.90; 95% CI, 0.67–1.25, I2 = 0%), and recovery of renal function (RR, 1.03; 95% CI, 0.89–1.19, I2 = 56%). The early RRT group had higher risks of catheter-related infection (RR, 1.7, 95% CI, 1.01–2.97, I2 = 0%) and hypophosphatemia (RR, 2.5, 95% CI, 1.25–4.99, I2 = 77%) than the late RRT group. In conclusion, an early RRT strategy does not improve survival, RRT dependence, or renal function recovery in critically ill patients with AKI in comparison with a late RRT strategy. However, clinicians should be vigilant because early RRT can carry higher risks of catheter-related infection and hypophosphatemia during dialysis than late RRT.
Similar content being viewed by others
Introduction
Acute kidney injury (AKI) is a common complication in critically ill patients, and the incidence of AKI patients requiring dialysis has also increased recently1,2,3. The development of AKI can be associated with increased morbidity, mortality and health-care costs1,4,5. Renal replacement therapy (RRT) remains the primary supportive strategy in the management of critically ill patients with severe AKI. However, in spite of improvements in RRT technology, such as the advent of continuous renal replacement therapy (CRRT) for patients with unstable hemodynamics, the mortality of patients with AKI requiring RRT remains high6,7,8. Several issues need to be addressed to improve the outcomes of these critically ill patients, such as the appropriate time to initiate RRT, the optimal intensity, and the choice of modality for RRT.
In common practice, RRT is usually initiated for acute management of life-threatening complications of AKI such as severe hyperkalemia, pulmonary edema, refractory metabolic acidosis, uremic pericarditis, and uremic encephalopathy9. Beyond these indications however, the appropriate timing for initiating RRT in critically ill patients is unknown. Early initiation of RRT is supposed to achieve better fluid and electrolyte balance, superior acid-base homeostasis, and more efficient removal of uremia toxins than standard therapy. Through these mechanisms, early RRT may help prevent AKI -associated kidney-specific or other vital organ injuries10,11,12,13. However, early RRT carries risks of several adverse events including vascular access placement-associated complications, catheter-related infections, bleeding due to the use of anticoagulants, too rapid changes in electrolytes, unnecessary clearance of important medications, delayed recovery of renal function and increased costs13,14. Several randomized controlled trials15,16,17,18,19,20,21,22,23 (RCTs) were conducted to find the optimal timing of RRT for critically ill AKI patients, but no consistent results were found. In 2018, one large RCT24 focused on patients with septic shock and severe AKI in the IDEAL-ICU trial found no significant difference in 90-day mortality between patients with early and delayed initiation of RRT. Their findings were consistent with those in another multicenter RCT by the AKIKI study group22, but were contrary to the findings of a recent single-center RCT in the ELAIN trial23. All of these findings indicate uncertainty about the usefulness of early RRT in critically ill patients. Although this issue had been discussed in one meta-analyses25 recently, we aimed to conduct an updated systematic review and meta-analysis of RCTs to assess the efficacy of early initiation of RRT in critically ill AKI patients.
Materials and Methods
Study search and selection
This systematic review and meta-analysis were conducted according to the preferred reporting items for systematic reviews and meta-analyses (PRISMA) statement (Supplemental Table 1). All clinical studies were identified by a systematic review of the literature in the PubMed, Embase, and Cochrane databases until August 13, 2019 using the following Mesh terms – “earl*”, “accelerat*”, “acute kidney”, “acute renal”, “anuria”, “oliguria”, “acute renal failure”, “anuria”, “oliguria”, “organ failure”, “dialy*”, “renal replacement”, “hemodialysis”, “hemofiltration”, “hemodiafiltration”, “RCT*” and “random*”. We excluded observation studies, case reports or case series, studies enrolling pediatric patients, and conference abstracts, and therefore, only RCTs that compared the clinical efficacy of early RRT and late RRT for critically ill adult patients with AKI were included. In addition, we searched all references in the relevant articles and reviews for additional eligible studies. Two reviewers (Chang & Wang) searched and examined publications independently to avoid bias. When they disagreed, another author (Lai) resolved the issue. The data included authors, year of publication, study design and duration, study population, sites of study, disease severity, indications for early RRT, and outcomes. Ethics board approval and patient consent were not required due to the nature of a systematic review. This meta-analysis was performed according the guidelines of Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA).
Definitions and outcome
The primary outcome was 28-day mortality and secondary outcomes included recovery of renal function, RRT dependence among survivors and adverse events.
Data analysis
We used the Cochrane Risk of Bias tool to evaluate the quality of enrolled studies and the risk of bias26. The statistical analysis was conducted using the software Review Manager, version 5.3. The degree of heterogeneity was evaluated with the Q statistic generated from the χ2 test. The proportion of statistical heterogeneity was assessed by the I2 measure. Heterogeneity was considered significant when the p-value was less than 0.10 or the I2 more than 50%. The fixed effects model and the random effects model were applied when the data was homogenous and heterogeneous, respectively. Pooled risk ratios (RR) and 95% confidence intervals (CI) were calculated for outcome analyses. Funnel plot was used to probe for publication bias. A p-value <0.05 was set as the threshold of statistical significance. Sensitivity analyses were conducted by excluding or subgrouping studies to reduce the potential confounding effects of patient population, RRT modality, study design, and study sample size.
Results
Study selection and characteristics
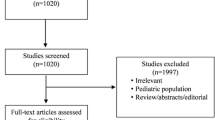
The search program yielded 807 references, including 207 from Pubmed, 325 from Embase, and 274 from the Cochrane database. Then, 425 articles were screened for title and abstract after excluding 382 duplicated articles. Finally, a total of eleven RCTs15,16,17,18,19,20,21,22,23,24,27 fulfilling the inclusion criteria were included in this meta-analysis (Fig. 1, Supplemental Table 2). All the studies15,16,17,18,19,20,21,22,23,24 were designed to compare the clinical efficacy of early and late RRT for critically ill patients with AKI (Table 1). During the initial enrollment, early and late RRT was applied for 1131 and 1111 patients, respectively. Four studies17,18,20,23 were conducted in a single center, and other seven were multicenter studies15,16,19,21,22,24,27. Six studies were performed in Europe15,16,19,22,23,24, four studies were conducted in Asia17,18,20,27, and one study21 was done in North America. The modalities of RRT varied, including mixed intermittent hemodialysis (IHD)/CRRT in three studies21,22,24, CRRT only in six studies15,16,19,20,23,27, and IHD only in two studies17,18. Two studies19,24 only enrolled patients with sepsis, and more than half of enrolled patients had sepsis in another three studies21,22,27. Figure 2 show the analyses of risk of bias. The risk of allocation concealment, the risk of blinding of participants and personnel, and the risk of blinding of outcome assessment were classified as high or unclear.
Primary outcomes
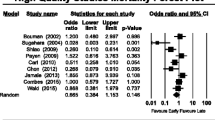
In the eleven enrolled trials, the pooled 28-day mortality was 38.1% (431/1131) and 40.7% (453/1111) in the groups of patients assigned to early and late RRT, respectively, with no significant difference between groups (RR, 0.95; 95% CI, 0.78–1.15, I2 = 63%, Fig. 3). Sensitivity analysis after deleting an individual study each time to reflect the influence of the single dataset on the pooled RR showed similar findings. The publication bias was shown in funnel plot (Fig. 4). We found no differences between early and late RRT in terms of 60-day mortality RR, 0.96; 95% CI, 0.75–1.23, I2 = 31%) in four studies16,22,23,24, and 90-day mortality (RR, 0.97 95% CI, 0.64–1.45, I2 = 0%) in four studies16,21,23,24. Four studies reported the ICU mortality15,16,21,24 and five studies15,16,17,18,21 showed in-hospital mortality. The pooled ICU mortality (RR, 1.16; 95% CI, 0.88–1.52, I2 = 0%) and in hospital-mortality (RR, 1.25; 95% CI, 0.74–2.11, I2 = 49%) were similar between groups.
In the four studies16,17,20,23 that only enrolled surgical patients, the early RRT group had a lower risk of mortality than the late RRT group (RR, 0.52; 95% CI, 0.27–0.99, I2 = 77%). There were no significant differences in terms of mortality between groups in the analysis of other subgroups, including mixed study populations, study sites, study designs, portion of patients with sepsis and RRT modality (Table 2).
Secondary outcomes
Six studies15,20,22,23,24,27 reported the rate of RRT dependence in survivors on day 28, and no significant difference was found between early and late RRT groups (RR, 0.90; 95% CI, 0.67–1.25, I2 = 0%, Fig. 5). The five studies16,18,21,23,24 that reported the rate of RRT dependence on day 90, showed similar rates in the two groups (RR, 0.76; 95% CI, 0.30–1.90, I2 = 0%). The recovery of renal function was reported in eight studies15,16,18,20,21,22,23,27, with similar rates in the two groups (RR, 1.03; 95% CI, 0.89–1.19, I2 = 56%, Fig. 6).
Adverse events
We assessed the rates of several common adverse events during RRT including hemorrhage, hypotension, arrhythmia, catheter-related infection, hypokalemia, hyperkalemia, metabolic acidosis and hypophosphatemia. A pooled analysis of five studies15,18,21,22,27 reporting the risk of catheter-related infections showed the early RRT group had a higher risk of this infection than late RRT group (RR, 1.7, 95% CI, 1.01–2.97, I2 = 0%) The early RRT group had a higher risk of hypophosphatemia than the late RRT group in a pooled analysis of 3 studies16,22,27 (RR, 2.5, 95% CI, 1.25–4.99, I2 = 77%). There were no significant differences between early and late groups in terms of hemorrhage (RR, 0.88, 95% CI, 0.68–1.14, I2 = 0%) in seven studies15,16,18,21,22,23,24, hypotension (RR, 1.11, 95% CI, 0.96–1.29, I2 = 0%) in six studies16,18,21,23,24,27, arrhythmia (RR, 1.21, 95% CI, 0.83–1.77, I2 = 36%) in six studies17,21,22,23,24,27, hypokalemia (RR, 1.11, 95% CI, 0.83–1.47, I2 = 24%) in three studies16,22,27, and hyperkalemia (RR, 0.52, 95% CI, 0.17–1.61, I2 = 57%) in three studies16,22,24. Pooled analysis of two studies16,24 showed that the early RRT group had a lower risk of metabolic acidosis than the late RRT group (RR, 0.60, 95% CI, 0.39–0.90, I2 = 0%).
Discussion
This meta-analysis of eleven RCTs with 1131 and 1111 AKI patients receiving early and late RRT, respectively, provided several significant findings. Most importantly, early RRT was not associated with a better outcome for these patients than late RRT. Overall, there was no significant difference in 28-day mortality between groups. There were no differences with different study sites (Europe, Asia or North America), study designs (single or multi-center), portion of patients with sepsis (50–<100%, or 100%) or RRT modality (IHD, CRRT, mixed). The early and late RRT groups had similar ICU-, hospital-, 60 day- and 90 day- mortality rates. All these findings are consistent with previous meta-analyses25,28,29,30, and indicate that early RRT does not provide additional survival benefits for AKI patients compared with late RRT. In addition to mortality, Pasin et al.25 ever showed that early RRT was associated with a significant reduction in length of hospital stay. However, the positive impact of early RRT on the length of hospital stay still need further confirmation in the high-quality studies.
Subgroup analysis of four studies16,17,20,23 that only enrolled surgical patients showed that the early RRT group had a lower risk of mortality than the late RRT group (RR, 0.52; 95% CI, 0.27–0.99, I2 = 77%). This finding is consistent with the result of a previous meta-anlaysis31 of nine retrospective cohort studies and two RCTs showing a lower 28-day mortality rate the early RRT group (OR = 0.29, 95% CI, 0.16–0.52, p < 0.0001) than the late RRT group among critically ill patients with AKI after cardiac surgery. However, both that meta-analysis31 and our findings in surgical patients were based on studies with very high heterogeneity. Further research with a larger number of studies and consistent results is still needed to confirm this finding in surgical patients.
We also found no differences in the recovery of renal function or RRT dependency in the early and late RRT groups. In Karvellas et al.’s meta-analysis32 of 15 studies, early RRT was associated with greater renal recovery than late RRT. However, only two RCTs were enrolled in that meta-analysis32, and the quality of those heterogeneous studies varied. In contrast, the present analysis only enrolled large-scale RCTs, and our findings were consistent with other meta-analyses29,30,33 of RCTs. These results should be more convincing than Karvellas et al.'s meta-analysis32. Therefore, based on current evidence, early RRT was not associated with greater renal recovery and lower dialysis dependence than late RRT for critically ill patients with AKI.
We cannot omit another important issue of RRT – safety. We evaluated the risks of several common complications during RRT. Although the incidence of most adverse events such as hemorrhage, hypotension, arrhythmia, hypokalemia and hyperkalemia were similar between groups, the early RRT group had higher risks of catheter-related infections, and hypophosphatemia than the late RRT group. Overall, our findings should remind clinicians to keep alert concerning the high risks of these two complications in early RRT for patients with AKI.
Although this meta-analysis enrolled several large-scale RCTs with a reasonable quality to enhance the level of evidence, there was one major limitation. There was relatively high heterogeneity with an I2 value of more than 50% in the outcome analysis. These heterogeneities could be caused by significant variations in the study design, population characteristics, disease severity, timing of initiating RRT, modality of RRT, and duration of follow-up in the studies.
Conclusion
This meta-analysis suggested that early RRT does not improve the survival, RRT dependence, or renal function recovery of critically ill patients with AKI in comparison with late RRT. Early RRT was associated with a lower 28-day mortality than late RRT in surgical patients with AKI. However, clinicians should be vigilant as early RRT can carry higher risks of catheter-related infection and hypophosphatemia during dialysis than late RRT.
Data availability
The datasets used and/or analyzed in the current study are available from the corresponding author upon request.
References
Li, P. K., Burdmann, E. A. & Mehta, R. L. Acute kidney injury: global health alert. Kidney international. 83, 372–376 (2013).
Kolhe, N. V., Muirhead, A. W., Wilkes, S. R., Fluck, R. J. & Taal, M. W. National trends in acute kidney injury requiring dialysis in England between 1998 and 2013. Kidney international. 88, 1161–1169 (2015).
Hsu, R. K., McCulloch, C. E., Dudley, R. A., Lo, L. J. & Hsu, C. Y. Temporal changes in incidence of dialysis-requiring AKI. J Am Soc Nephrol. 24, 37–42 (2013).
Pannu, N., James, M., Hemmelgarn, B. & Klarenbach, S. Association between AKI, recovery of renal function, and long-term outcomes after hospital discharge. Clin J Am Soc Nephrol. 8, 194–202 (2013).
Mandelbaum, T. et al. Outcome of critically ill patients with acute kidney injury using the Acute Kidney Injury Network criteria. Crit Care Med. 39, 2659–2664 (2011).
Bagshaw, S. M. et al. Prognosis for long-term survival and renal recovery in critically ill patients with severe acute renal failure: a population-based study. Crit Care. 9, R700–709 (2005).
Uchino, S. et al. Acute renal failure in critically ill patients: a multinational, multicenter study. Jama. 294, 813–818 (2005).
Mehta, R. L. et al. Spectrum of acute renal failure in the intensive care unit: the PICARD experience. Kidney international. 66, 1613–1621 (2004).
Bagshaw, S. M. & Wald, R. Strategies for the optimal timing to start renal replacement therapy in critically ill patients with acute kidney injury. Kidney international. 91, 1022–1032 (2017).
Andres-Hernando, A. et al. Prolonged acute kidney injury exacerbates lung inflammation at 7 days post-acute kidney injury. Physiol Rep. 2 (2014).
Ishii, T. et al. Neutrophil elastase contributes to acute lung injury induced by bilateral nephrectomy. Am J Pathol. 177, 1665–1673 (2010).
Burchill, L. et al. Acute kidney injury in the rat causes cardiac remodelling and increases angiotensin-converting enzyme 2 expression. Exp Physiol. 93, 622–630 (2008).
Gibney, N. et al. Timing of initiation and discontinuation of renal replacement therapy in AKI: unanswered key questions. Clin J Am Soc Nephrol. 3, 876–880 (2008).
Karakala, N. & Tolwani, A. J. Timing of Renal Replacement Therapy for Acute Kidney Injury. J Intensive Care Med. 885066618774257 (2018).
Bouman, C. S., Oudemans-Van Straaten, H. M., Tijssen, J. G., Zandstra, D. F. & Kesecioglu, J. Effects of early high-volume continuous venovenous hemofiltration on survival and recovery of renal function in intensive care patients with acute renal failure: a prospective, randomized trial. Crit Care Med. 30, 2205–2211(2002).
Combes, A. et al. Early High-Volume Hemofiltration versus Standard Care for Post-Cardiac Surgery Shock. The HEROICS Study. Am J Respir Crit Care Med. 192, 1179–1190 (2015).
Durmaz, I. et al. Prophylactic dialysis in patients with renal dysfunction undergoing on-pump coronary artery bypass surgery. Ann Thorac Surg. 75, 859–864 (2003).
Jamale, T. E. et al. Earlier-start versus usual-start dialysis in patients with community-acquired acute kidney injury: a randomized controlled trial. Am J Kidney Dis. 62, 1116–1121 (2013).
Payen, D. et al. Impact of continuous venovenous hemofiltration on organ failure during the early phase of severe sepsis: a randomized controlled trial. Crit Care Med. 37, 803–810 (2009).
Sugahara, S. & Suzuki, H. Early start on continuous hemodialysis therapy improves survival rate in patients with acute renal failure following coronary bypass surgery. Hemodial Int. 8, 320–325 (2004).
Wald, R. et al. Comparison of standard and accelerated initiation of renal replacement therapy in acute kidney injury. Kidney international. 88, 897–904 (2015).
Gaudry, S. et al. Initiation Strategies for Renal-Replacement Therapy in the Intensive Care Unit. N Engl J Med. 375, 122–133 (2016).
Zarbock, A. et al. Effect of Early vs Delayed Initiation of Renal Replacement Therapy on Mortality in Critically Ill Patients With Acute Kidney Injury: The ELAIN Randomized Clinical Trial. Jama. 315, 2190–2199 (2016).
Barbar, S. D. & Clere-Jehl, R. Timing of Renal-Replacement Therapy in Patients with Acute Kidney Injury and Sepsis. 379, 1431–1442 (2018).
Pasin, L., Boraso, S. & Tiberio, I. Early initiation of renal replacement therapy in critically ill patients: a meta-analysis of randomized clinical trials. BMC anesthesiology. 19, 62 (2019).
Higgins, J. P. et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. Bmj. 343, d5928 (2011).
Lumlertgul, N. et al. Early versus standard initiation of renal replacement therapy in furosemide stress test non-responsive acute kidney injury patients (the FST trial). Crit Care. 22, 101 (2018).
Mavrakanas, T. A., Aurian-Blajeni, D. E. & Charytan, D. M. Early versus late initiation of renal replacement therapy in patients with acute kidney injury: a meta-analysis of randomised clinical trials. Swiss Med Wkly. 147, w14507 (2017).
Bhatt, G. C. & Das, R. R. Early versus late initiation of renal replacement therapy in patients with acute kidney injury-a systematic review & meta-analysis of randomized controlled trials. BMC Nephrol. 18, 78 (2017).
Lai, T. S. & Shiao, C. C. Earlier versus later initiation of renal replacement therapy among critically ill patients with acute kidney injury: a systematic review and meta-analysis of randomized controlled trials. 7, 38 (2017).
Liu, Y., Davari-Farid, S., Arora, P., Porhomayon, J. & Nader, N. D. Early versus late initiation of renal replacement therapy in critically ill patients with acute kidney injury after cardiac surgery: a systematic review and meta-analysis. J Cardiothorac Vasc Anesth. 28, 557–563 (2014).
Karvellas, C. J. et al. A comparison of early versus late initiation of renal replacement therapy in critically ill patients with acute kidney injury: a systematic review and meta-analysis. Crit Care. 15, R72 (2011).
Yang, X. M. et al. A comparison of early versus late initiation of renal replacement therapy for acute kidney injury in critically ill patients: an updated systematic review and meta-analysis of randomized controlled trials. BMC Nephrol. 18, 264 (2017).
Acknowledgements
The authors thank Dr. Chien-Ming Chao and Shao-Huan Lan for helping assessment of the articles of meta-analysis. The authors declare that they did not receive any funding for this work.
Author information
Authors and Affiliations
Contributions
W.T., C.C. and J.J. designed the study. C.C. and J.J. designed the search strategy and performed the search. W.T., C.C., S.P. and J.J. performed abstract screening, full text screening, data extraction, and risk of bias assessment. C.C., S.P. and J.J. performed data analysis. W.T., C.C. and J.J. helped in finalizing the full text screening, and in data interpretation. C.C., S.P. and J.J. participated in the statistical analysis, risk of bias assessment, and rating of the certainty of evidence. W.T. and C.C. drafted the manuscript. All authors revised the manuscript and read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lin, WT., Lai, CC., Chang, SP. et al. Effects of early dialysis on the outcomes of critically ill patients with acute kidney injury: a systematic review and meta-analysis of randomized controlled trials. Sci Rep 9, 18283 (2019). https://doi.org/10.1038/s41598-019-54777-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-54777-9
- Springer Nature Limited
This article is cited by
-
Acute Kidney Injury in Acute on Chronic Liver Failure Versus Decompensated Cirrhosis—What Is the Difference?
Current Hepatology Reports (2024)
-
APASL clinical practice guidelines on the management of acute kidney injury in acute-on-chronic liver failure
Hepatology International (2024)