Abstract
Streptococcus pneumoniae meningitis is an intractable disease of the central nervous system (CNS). Brain-derived neurotrophic factor (BDNF) is a member of the neurotrophic family and found to participate in the immune inflammatory response. In this study, we investigated if activation of the classical inflammatory signaling pathway, myeloid differentiation factor 88 (MyD88)/nuclear factor-kappa B (NF-κB), regulates BDNF expression in experimental S. pneumoniae meningitis. MyD88 knockout (myd88−/−) mice and wild-type littermates were infected intracisternally with S. pneumoniae suspension. Twenty-four hours after inoculation, histopathology of brains was evaluated. Cytokine and chemokine in brains and spleens was analyzed using ELISA. NF-κB activation was evaluated using EMSA. Cortical and hippocampal BDNF was assessed using RT-PCR and ELISA, respectively. BDNF promoter activity was evaluated using ChIP-PCR. myd88−/− mice showed an obviously weakened inflammatory host response. This diminished inflammation was consistent with worse clinical parameters, neuron injury, and apoptosis. Deficiency in MyD88 was associated with decreased BDNF expression. Furthermore, we identified a valid κB-binding site in the BDNF promoter, consistent with activation of NF-κB induced by inflammation. To sum up, MyD88/NF-κB signaling has a crucial role in up-regulating BDNF, which might provide potential therapeutic targets for S. pneumoniae meningitis.
Similar content being viewed by others
Introduction
Streptococcus pneumoniae meningitis is an invasive and often intractable disease of the central nervous system (CNS). Despite effective antibiotics and application of vaccinations, such infection is still associated with an unacceptably high morbidity and mortality1. The main limitation to advance in prevention and treatment of the disease is incomplete knowledge of its pathogenesis and pathophysiology. Generally, the host immune response, such as the activation of macrophages, production of cytokines and chemokines, and migration of leukocytes, is believed to be the first line of defense in response to bacterial invasion during the process of S. pneumoniae meningitis2. Toll-like receptors (TLRs), which are widely expressed in central resident macrophages, sense antigens from microorganisms, leading to the recruitment of myeloid differentiation factor 88 (MyD88) and the activation of downstream signaling pathways3, 4. MyD88 is crucial for the induction of a full innate inflammation response to most TLRs ligands, with the exception of TLR35. Furthermore, the MyD88-dependent pathway elicits nuclear factor-kappa B (NF-κB) and mitogen-activated protein kinase (MAPK) activation, which drives robust gene expression of cytokines and pro-inflammatory mediators6. However, increasing evidence has demonstrated that activation of NF-κB can lead to uncontrolled expression of those pro-inflammatory mediators, which contributes to the pathogenesis of disease processes7. Innate immune response is now widely recognized as a double-edged blade possessing both protective and damaging properties8. There is now solid evidence that intense inflammatory host response causes important damage to the brain, thus inducing unfavorable outcomes of meningitis9, 10.
Brain-derived neurotrophic factor (BDNF) is a member of the neurotrophic family and is widely expressed in the adult brain. In CNS, multiple cell types express BDNF including neurons and glia11. BDNF promotes neuronal survival, maturation, and growth by binding to its high-affinity tropomyosin-related kinase receptor, type B (TrkB)12, 13. Dysfunction in the regulation of BDNF is associated with numerous disorders of CNS, including Alzheimer’s disease (AD), multiple sclerosis (MS), depression, and unacceptable outcomes of bacterial meningitis14,15,16,17. Our previous study showed that increased expression of BDNF following the acute S. pneumonia meningitis was alleviated after antibiotic treatment18. Furthermore, Barichello et al.19 demonstrated that down-regulated BDNF expression in the hippocampus was associated with cognition and memory deficiency in experimental S. pneumoniae meningitis. Interestingly, administration of exogenous BDNF increased the neuronal population in both the cortex and hippocampus, and reversed brain damage20. These findings indicate that regulatory expression of BDNF may be a part of the host inflammatory response in S. pneumoniae meningitis. However, the underlying regulatory mechanism is still not clear.
A recent report has shown that TLR agonists up-regulate nerve growth factor (NGF) in human intervertebral discs by activating and translocating NF-κB into the nucleus21. A tissue engineering study showed that hyaluronic acid-based hydrogels could attenuate inflammatory receptor activity in an interleukin (IL)-1β-induced inflammation model of nucleus pulposus cells, with down-regulation of NGF and BDNF22. Pro-inflammatory factors including endotoxins, cytokines, and oxidative stress have been reported to up-regulate BDNF in immune cells in vitro. In particular, tumor necrosis factor-alpha (TNF-α) has been demonstrated to increase BDNF expression via the extracellular signal-regulated kinase (ERK)/mitogen-activated protein kinase (MAPK) pathway in primary astrocytes23.
In this study, we aimed to investigate if activation of the classical inflammatory signaling pathway, namely the MyD88/NF-κB signaling pathway, regulates BDNF expression in experimental S. pneumoniae meningitis.
Results
Effect of MyD88 deficiency on characteristics of the meningitis and histopathology
As a result of disease progression following inoculation with S. pneumoniae, all infected mice began to exhibit clinical symptoms of meningitis around 18 h after intracisternal injection, with loss of weight, hypothermia, lags in response and lethargy. Furthermore, the mortality rate was high during the acute disease phase, between 18 and 24 h after infection (Fig. 1). Of the 12 infected wild-type mice, 2 (16.70%) died within 24 h after inoculation, while 4 of 12 (33.3%) infected myd88−/− mice died during the same period. The survival rate of infected myd88−/− mice tended to be lower than infected wild-type mice; however, there was no significant variance (p > 0.05; log rank test). Data from two-way ANOVA indicated significant interactions between the variables (MyD88 and meningitis) on weight loss [F (1,30) = 8.687, p < 0.01] and clinical scores [F (1,36) = 5.345, p = 0.027]. In addition, infected myd88−/− mice lost more weight and had markedly enhanced clinical scores for severity of the disease compared to the infected wild-type mice (Table 1). None of the control mice induced with pyrogen-free saline showed symptoms of infection within the same observation period. All of the infected mice had positive bacterial cultures of the cerebellar homogenates but no pneumococci grew from the brains of uninfected mice.
Representative examples of H&E-stained brain sections of each group are shown in Fig. 2A. Infected wild-type mice showed vast inflammatory exudate in the subarachnoid cavity and ventricle, with hemorrhage-like spots in the parenchyma. However, the brains of infected myd88−/− mice showed obviously weak inflammatory response in the subarachnoid space. This finding corroborated with the dramatic weak antibacterial properties of myd88−/− mice to intracerebral S. pneumoniae infection.
Effect of MyD88 deficiency on histological changes of mouse brains at 24 h after inoculation with S. pneumoniae. (A) H&E staining: Infected myd88−/− mice showed slight neutrophile granulocyte exudate in the subarachnoid cavity, while infected wild-type mice showed vast inflammatory exudate in the subarachnoid cavity and ventricle, with hemorrhage-like spots in the parenchyma. Control groups had no pathological changes of meningitis, with a smooth meninx. (B) Nissl staining: In infected myd88−/− mice group, the structure of most neurons in the hippocampus is incomplete, and Nissl staining is not uniform in the cytoplasm. In infected wild-type mice group, neuron loss is less severe than in infected myd88−/− mice. Nissl staining in control groups had no difference. (C) TUNEL immunofluorescence: There are more TUNEL-positive cells in infected myd88−/− mice than in infected wild-type mice. Few TUNEL-positive cells were observed in both control groups. (D) Quantitative analysis of the TUNEL results, *p < 0.05, **p < 0.01. KO: knockout, PM: pneumoniae meningitis, WT: wild-type, NS: normal saline.
In addition, neuronal injury in hippocampus was analyzed by using Nissl staining. As shown in Fig. 2B, neuron loss was more remarkable in the hippocampus of infected myd88−/− mice than in infected wild-type mice, with a more severely incomplete structure of neurons induced by intracerebral S. pneumoniae infection.
Furthermore, hippocampal apoptosis was investigated by TUNEL staining. Two-way ANOVA indicated significant interactions between the variables (MyD88 and meningitis) on hippocampal apoptosis [F (1,12) = 8.089, p = 0.015]. S. pneumoniae infection caused obvious apoptosis in the hippocampal dentate gyrus as compared with the control groups (Fig. 2C), and the number of TUNEL-positive cells was significantly higher in infected myd88−/− mice than in infected wild-type mice (Fig. 2D).
Effect of MyD88 deficiency on inflammatory mediator production in brains and spleens
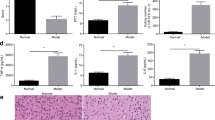
At 24 h after infection, the expression of cytokines and chemokines (i.e., TNF-α, IL-1β, IL-6, and IL-10) was evaluated by using ELISA. Two-way ANOVA indicated interactions significant between the variables (MyD88 and meningitis) on these inflammatory mediator productions (except expression of IL-10 in cortex). Data from two-way ANOVA for interaction on TNF-α in cortex and spleens is [F (1,22) = 29.185, p < 0.01] and [F (1,27) = 38.852, p < 0.01], respectively. Interactions between the variables on IL-1β is [F (1,20) = 11.845, p < 0.01] and [F (1,24) = 36.218, p < 0.01], respectively in cortex and spleens. Data of interactions on IL-6 is [F (1,20) = 115.165, p < 0.01] and [F (1,28) = 13.383, p < 0.01]. In the cortex, a two-way ANOVA of IL-10 expression indicated that there was no significant effect of the MyD88 group [F (1,18) = 2.244, p = 0.151], and there was no significant effect of the meningitis group [F (1,18) = 0.669, p = 0.424] with no significant interaction [F (1,18) = 0.149, p = 0.704]. However, in the spleens, interactions were identified between MyD88 and meningitis [F (1,25) = 35.366, p < 0.01]. Streptococcus pneumoniae infection led to massive cytokine and chemokine increase in both the cerebral cortex and spleen homogenates of wild-type mice (Fig. 3, except expression of IL-10 in cortex). In contrast, the expression of TNF-α, IL1-β, IL-6, and IL-10 was significantly attenuated in infected myd88−/− mice at the same time point, reflecting impaired immune activation.
Effect of MyD88 deficiency on inflammatory mediator production in brains and spleens. myd88−/− and wild-type mice received intracisternal injection of S. pneumoniae, and cytokine/chemokine expression in brains and spleens were evaluated using ELISA kits for (A) TNF-α, (B) IL-1β, (C) IL-6, and (D) IL-10. In cortex and spleen homogenates from infected myd88−/− mice, no significantly increased expression of TNF-α, IL-1β, and IL-6 was detected. Inoculation with S. pneumoniae caused a significant increase in the expression of these inflammatory mediators in brains and spleens obtained from infected wild-type mice at 24 h after inoculation. Inoculation with S. pneumoniae led to increase of IL-10 in spleens both from infected myd88−/− mice and infected wild-type mice at 24 h after inoculation. Moreover, the expression of this anti-inflammatory mediator was much higher in infected wild-type mice than in infected myd88−/− mice. *p < 0.05, **p < 0.01. KO: knockout, PM: pneumoniae meningitis, WT: wild-type, NS: normal saline.
MyD88 is a major contributor to activation of NF-κB following S. pneumoniae administration
To further determine the role played by MyD88 in S. pneumoniae-induced activation of NF-κB, EMSA was performed in nuclear extracts from brains derived from both myd88−/− and wild-type mice. NF-κB binding activation was significantly enhanced in infected wild-type mice compared with wild-type control mice (Fig. 4). However, this bacteria-induced NF-κB binding activation was markedly attenuated in myd88−/− mice. These data are in agreement with published studies24, 25 and indicate that MyD88 is required for S. pneumoniae-induced NF-κB binding activation in the CNS.
Effect of MyD88 deficiency on activation of NF-κB after inoculation with S. pneumoniae. NF-κB binding activity in the cortex in different groups was assessed by EMSA. Bacteria-induced NF-κB binding was markedly enhanced in infected wild-type mice compared to infected myd88−/− mice. KO: knockout, PM: pneumoniae meningitis, WT: wild-type, NS: normal saline.
MyD88 is required for S. pneumoniae-mediated increase in BDNF expression
Our previous studies have demonstrated that BDNF increases both in the cortex and hippocampus during the acute phase of S. pneumoniae meningitis, but decreases after antibiotics treatment18. In the present study, we further explored if MyD88 activation could induce the expression of BDNF in S. pneumoniae meningitis. At 24 h following inoculation, cortical cortex and hippocampus homogenates were collected and analyzed for expression of BDNF at the transcriptional and translational level. Data from two-way ANOVA indicated significant interactions between MyD88 and meningitis on BDNF expression. For BDNF mRNA [F (1,14) = 64.356, p < 0.01] and [F (1,20) = 9.731, p < 0.01], respectively in cortex and hippocampus. For BDNF protein [F (1,21) = 48.726, p < 0.01] and [F (1,17) = 6.902, p = 0.018], respectively in cortex and hippocampus. Infected wild-type mice promoted a strong trend of increased BDNF mRNA expression compared to saline controls (Fig. 5). Importantly, this bacteria-induced BDNF mRNA elevation was markedly attenuated in the cortical cortex and hippocampus isolated from myd88−/− mice. Next, we analyzed the protein level of BDNF in the cortical cortex and hippocampus. Similarly, we found that increases in levels of BDNF protein observed at 24 h following S. pneumoniae administration were absent in myd88−/− mice (Fig. 6).
BDNF mRNA expression in the cortex and hippocampus at 24 h after inoculation with S. pneumoniae. BDNF mRNA expression in (A) the cortex and (B) hippocampus was significantly higher in infected wild-type mice than in control wild-type mice and infected myd88−/− mice. However, BDNF mRNA expression was similar between infected myd88−/− mice and control mice. *p < 0.05, **p < 0.01. BDNF: brain-derived neurotrophic factor, KO: knockout, PM: pneumoniae meningitis, WT: wild-type, NS: normal saline.
BDNF protein levels in the cortex and hippocampus at 24 h after inoculation with S. pneumoniae. BDNF in the cortex (A) and hippocampus (B) were significantly higher in infected wild-type mice than in control wild-type mice and infected myd88−/− mice. *p < 0.05, **p < 0.01. BDNF: brain-derived neurotrophic factor, KO: knockout, PM: pneumoniae meningitis, WT: wild-type, NS: normal saline.
NF-κB directly acts with BDNF promoter expression in BV-2 strain
As shown in Fig. 7, the binding site of NF-κB to the BDNF promoter was found by ChIP-PCR assay. Mouse GAPDH prime sets amplified mouse gapdh gene only in Input and RNA pol II group, examining validity of ChIP-PCR experiment (Fig. 7A). Then, one pair of primers could amplify the ChIP products to mouse bdnf gene (about 300 bp) in NF-κB group (Fig. 7B). Thus, there is a consensus NF-κB binding site present in the BDNF promoter region.
MyD88 up-regulates BDNF expression during S. pneumoniae meningitis by direct binding of NF-κB to the BDNF promoter. ChIP experiments were carried out in the mouse BV-2 cell strain. Nuclear extracts were analyzed by ChIP-PCR. IgG and RNA pol II antibody was used as negative and positive control. (A) GAPDH prime sets were performed to examine the validity. (B) One pair of BDNF primes amplified the ChIP products in NF-κB group.
Discussion
The present results demonstrate that S. pneumoniae infection drives robust gene expression of cytokines and chemokines in the CNS and peripheral immune organs, along with BDNF gene and protein expression in the cortex and hippocampus. The activity of MyD88/NF-κB signaling is not only crucial to innate immune response, but it is also required for BDNF expression. These results identify a new insight into the regulatory mechanism mediating BDNF expression during S. pneumoniae meningitis, thus contributing to a deep understanding of pathogenesis and pathophysiology of this disease.
Streptococcus pneumoniae is still the most common cause of community-acquired meningitis in developing countries26. Current viewpoints are that when bacteria enter the CNS, innate immune response is activated initially to limit bacteria diffusion as well as eliminate its components27. Although the inflammatory response can exert its defensive role, it can also induce neurotoxic effects, which are associated with cell death and neurological sequelae8, 28. The inefficiency of the host immune response is assumed to be associated with higher mortality of meningitis. Modulating inflammatory response and reducing side effects associated with excessive immune response have long been a hot-spot therapeutic target during bacterial meningitis. In the past decades, numerous researchers have tried different adjuvant treatments involving dexamethasone, IL-1β receptor antagonist, and mood-stabilizer lithium, among others, to improve the outcomes of S. pneumoniae meningitis. However, the clinical efficacy remains barely satisfactory29,30,31. Better knowledge of the pathogenesis and pathophysiology of this disease may be the sally port. Our previous results have demonstrated that BDNF increases during acute stage of S. pneumoniae meningitis but decreases with time18, 32. Similarly, BDNF concentration in the peripheral blood and injured brain increases in humans and animals suffering from trauma and ischemic insult33, 34. These prior studies indicated that besides its normal physiological functions, increased expression of BDNF in the CNS after a variety of insults indicates a neuro-restorative and neuroprotective role for this neurotrophic factor. Clinically, BDNF has been suggested to increase neurogenesis of neural stem cells (NSCs) and has been potentially to reduce neurological sequelae associated with meningitis and focal cerebral ischemia32, 35. It is estimated that there is not only the destruction of inflammatory factors but also a protective effect of neurotrophic factors. The two systems combine to the pathophysiologic process of S. pneumoniae meningitis.
MyD88 has been identified as TLRs adapter molecule that plays a crucial role in initiating inflammatory host immune responses to bacterial challenge mainly via TLRs engagement28. As it behaves dually in host immune defense, it is now widely recognized as a doubled-edged blade. MyD88-deficient mice have been demonstrated to be highly susceptible to intracerebral infection with Escherichia coli strain K136 and have a high mortality and severe bacteremia in infectious diseases37, 38. In present study, we showed that absence of MyD88 decreased the resistance of mice to S. pneumoniae meningitis, including more weight loss and worse clinical manifestations, with diminishing neutrophil infiltration and subarachnoid hemorrhage, attenuated production of cytokines (TNF-α, IL-1β, and IL-6) and anti-inflammatory factor (IL-10) in both CNS and peripheral regions. Although significant difference in mortality between two infectious groups has not been observed in our study, there was a tendency that infected myd88−/− mice had a lower survival rate than infected wild-type mice. We speculate that the mortality difference would reach the level of statistical significance if we enlarge the number of animals. These results are in accordance with previous studies regarding the key role for MyD88 in immune defense but also neurons injure in both Gram-positive and Gram-negative bacterial meningitis37, 38. Moreover, the population of survival neurons significantly decreased and apoptosis body increased in hippocampus of infected myd88−/− mice compared with infected wild-type mice. Here, we also found that MyD88 underlies the ability for immune response to enhance neurotrophic expression, as myd88−/− mice express significantly lower BDNF production after infected with bacteria when compared with infected wild-type mice. Accordingly, this signaling adaptor molecule not only has a critical role in producing inflammatory factors during S. pneumoniae meningitis, but also is essential to induce neuroprotective agent. Therefore, this signal point may potentially exert the ability to protect from neuronal injury and death via balancing extent of inflammatory response and expression of neurotrophic elements.
In addition to emphasizing the ability of MyD88 in up-regulation of BDNF during S. pneumoniae meningitis, the present study also verified the effect of the downstream transcription factor NF-κB involved in the process. The activation of MyD88 activates downstream signal pathways, thus inducing a variety of transcription factors to translocate to the nucleus. NF-κB is one of the most major transcription factors, acting as a gate for immune response. As expected, our EMSA results confirmed previous findings that MyD88 activation increased NF-κB activation and induced p65 translocation. Potential roles for NF-κB have long been suggested in inflammation and immune response39 and recently in neuron survival. For example, blockade of NF-κB activity by pharmacological inhibitors attenuates CNS complications and provides protective effects for brain in bacterial meningitis40, 41. A recent study found that activation of NF-κB increases expression of NGF in disc cells during disc degeneration21. Therefore, we presume that NF-κB may be required for MyD88 to increase BDNF expression. To confirm this speculation, we performed ChIP-PCR to search for probable NF-κB binding sites with the promoter region of murine BDNF. Excitingly, this search revealed a consensus NF-κB binding site present in the BDNF promoter region, confirming a direct proof for this transcription factor in regulating BDNF. Therefore, we hypothesize that there is target point of NF-κB to both inflammation-related genes and neurotrophic elements.
In conclusion, the present findings suggested that S. pneumoniae meningitis induces neurotoxic cytokines and chemokines, but also neuroprotective elements. The activity of MyD88/NF-κB signaling induced innate immune response, and this pathway is also required for BDNF expression. However, how to modulate this key signal pathway to balance the effect of excessive inflammatory injury and neuroprotective survival need further investigation. BDNF undoubtedly plays a neuroprotective effect during the process of S. pneumoniae meningitis. Better understanding of how BDNF is regulated can be helpful to find a therapeutic target in bacterial meningitis.
Methods
Mouse strains and experimental design
Six-week old MyD88 knockout (myd88−/−) mice that have been backcrossed with C57BL/6 mice for over 10 generations, as well as wild-type littermates, were purchased from Jackson Laboratory (Bar Harbor, ME). We divided the mice into the following groups: (1) myd88−/− mice injected intracisternally with S. pneumoniae suspension (n = 12); (2) myd88−/− mice injected intracisternally with sterile saline (n = 8); (3) wild-type mice injected intracisternally with S. pneumoniae suspension (n = 12); and (4) wild-type mice injected intracisternally with sterile saline (n = 8). The animal experiments were approved by the Animal Ethical and Welfare Committee of Xinhua Hospital Affiliated to Shanghai Jiaotong University School of Medicine. All methods were performed in accordance with the relevant guidelines and regulations. We made efforts to minimize the number of animals used and their suffering.
Infecting organisms
We used the serotype III S. pneumoniae strain, which was obtained from ATCC. To obtain the appropriate concentrations of bacteria, serotype III S. pneumoniae was cultured on a blood-agar plate for 18 h and then inoculated into Vital Aer Broth overnight at 37 °C in air with 5% CO2 for another 18 h to reach the logarithmic phase. The bacteria were then centrifuged and washed twice with sterile saline. We used a nephelometer to achieve a concentration of approximately 1 × 104 colony forming units (cfu)/ml by re-suspending the bacteria with sterile saline.
Animal model of meningitis
All mice (n = 40) were anesthetized with 1–1.5 ml/100 g 5% chloral hydrate by intraperitoneal injection. A 10-μl volume containing either 1 × 104 cfu/ml S. pneumoniae or sterile saline was injected intracisternally into each mouse. At 24 h after infection with S. pneumoniae or saline, the health status of the mice were assessed by weighting and by a clinical score: 0 = no apparent behavioral abnormality; 1 = moderate lethargy (apparent decrease of spontaneous activity); 2 = severe lethargy (rare spontaneous movements, but walking after stimulation by the investigator); 3 = unable to walk; and 4 = dead42. After clinical evaluation, mice from all groups were sacrificed at 24 h after inoculation to harvest brains and spleens. In order to document the development of bacterial meningitis, cerebellum homogenates were plated and cultured on blood-agar plates.
Histopathological evaluation of murine brain sections
At 24 h after inoculation, all surviving animals were anesthetized and perfused through the left ventricular with 50 ml normal saline. Then, the animals were decapitated, the brains were removed, followed by segmentation of the brains into 2 hemispheres. The left hemispheres were fixed in 4% paraformaldehyde overnight at 4 °C, embedded in paraffin, and cut into 4-μm-thick coronal sections through the hippocampus. The sections were stained with hematoxylin & eosin (H&E) (Beyotime Biotechnology, China) and cresyl violet (Sigma-Aldrich, USA) according to a standard protocol. Apoptosis-like cell death was determined by terminal deoxynucleotidyl transferase dUTP nick end labeling (TUNEL) immunofluorescence staining using the In-Situ Cell Death Detection Kit (Roche, USA) according to the manufacturer’s instructions.
Quantification of cytokine and chemokine secretion
Brains and spleens were sonicated in PBS buffer containing a proteinase inhibitor cocktail and centrifuged at 12000 g for 15 min to remove cellular debris. The concentrations of TNF-α, IL-1β, IL-6, and IL-10 in supernatant were determined using commercial enzyme-linked immunosorbent assay (ELISA) kits (eBioscience, USA). Cytokine and chemokine levels in brain homogenates were normalized to total brain weight and reported as picograms per milliliter.
Electrophoretic mobility shift assay for NF-κB activation
Nuclear extract preparation and electrophoretic mobility shift assay (EMSA) were performed using the EMSA kit (Thermofisher, USA) as described previously, with some modifications34. Briefly, nuclear extract (20 ug) was incubated with binding buffer and nonspecific oligonucleotides for 15 min, and then incubated with NF-κB biotin-labeled oligonucleotide probes (forward: 5′-AGT TGA GGG GAC TTT CCC AGG C-3′; reverse: 5′-G CCT GGG AAA GTC CCC TCA ACT-3′) for another 15 min. For super shift assays, NF-κB antibody was added along with the binding buffer. Subsequently, samples were separated by electrophoresis in a 5.5% polyacrylamide gel with 0.25 × Tris-borate-EDTA buffer. The retarded bands were detected by chemiluminescence.
Analyses of BDNF at transcriptional and translational level
Reverse transcription polymerase chain reaction (RT-PCR) was performed as previously described43. Briefly, total RNA from brain tissues (cerebral cortex and hippocampus) were extracted using Trizol reagent (TaKaRa, Japan) and isolated using chloroform following the manufacturer’s instructions. RNA was converted to cDNA by using the Primer-Script One-Step RT-PCR kit (TaKaRa). Real-time PCR was performed using the ABI7500 system (Applied Biosystems, Carlsbad, CA) using the SYBR Premix Dimmer Eraser kit (TaKaRa) to amplify the cDNA template. The forward and reverse strand primers that were used to amplify the mRNA encoding mouse BDNF were ATTAGCGAGTGGGTCACAGC and TCAGTTGGCCTTTGGATACC, respectively. The primers were synthesized by Shanghai Sangon Biological Engineering Technology Company Limited. BDNF gene expression in each sample was normalized to β-actin expression. The relative expression level of mRNAs was calculated by the 2−ΔΔCt method.
To assay BDNF synthesis, BDNF ELISA kit (Cusabio, China) was used to quantify protein concentration in cerebral cortex and hippocampus according to the manufacturer’s instruction.
Chromatin immunoprecipitation assay
Chromatin immunoprecipitation (ChIP) were performed with the BV-2 cell strain (a standard microglia cell stain). Cellular protein-DNA complexes were cross-linked, isolated and fragmented. Immunoprecipitation was performed with NF-κB antibody (Millipore, USA) to enrich specific chromatin fragments. RNA pol II antibody (Santa Cruz, USA) was added as positive control, and goat IgG was used as negative control. Antibody complexes were collected and washed, then reversed the cross-links. The amounts of immunoprecipitated DNA were calculated by comparison to input DNA. The ChIP products were also analyzed by PCR. The primer sets used to amplify mouse bdnf gene are listed in supplementary data.
Statistical analysis
The Shapiro-Wilk test and Levene test were used to distinguish between parametric and nonparametric values. Differences among groups were analyzed using two-way ANOVA (MyD88 and meningitis) for parametric data, followed by Tukey’s post-hoc test; otherwise, the Mann-Whitney test was used, the intergroup comparisons were performed using Wilcoxon’s tests. If not stated otherwise, the data was reported as the mean ± SD. Survival rates were compared by the log rank test. Differences were considered significant at p < 0.05. All graphs were generated using Graph Pad Prism 5.0. Statistical analyses were performed using SPSS software version 18.0.
References
Backhaus, E. et al. Epidemiology of invasive pneumococcal infections: manifestations, incidence and case fatality rate correlated to age, gender and risk factors. BMC Infect Dis 16, 367, doi:10.1186/s12879-016-1648-2 (2016).
Scheld, W. M., Koedel, U., Nathan, B. & Pfister, H. W. Pathophysiology of bacterial meningitis: mechanism(s) of neuronal injury. J Infect Dis 186 Suppl 2, S225–233, doi:JID020578 (2002).
Kawai, T. & Akira, S. The role of pattern-recognition receptors in innate immunity: update on Toll-like receptors. Nat Immunol 11, 373–384, doi:10.1038/ni.1863 (2010).
Carpentier, P. A., Duncan, D. S. & Miller, S. D. Glial toll-like receptor signaling in central nervous system infection and autoimmunity. Brain Behav Immun 22, 140–147, doi:S0889-1591(07)00211-5 (2008).
Takeuchi, O. & Akira, S. Pattern recognition receptors and inflammation. Cell 140, 805–820, doi:10.1016/j.cell.2010.01.022 (2010).
Mitchell, J. A., Paul-Clark, M. J., Clarke, G. W., McMaster, S. K. & Cartwright, N. Critical role of toll-like receptors and nucleotide oligomerisation domain in the regulation of health and disease. J Endocrinol 193, 323–330, doi:193/3/323 (2007).
Bondeson, J., Foxwell, B., Brennan, F. & Feldmann, M. Defining therapeutic targets by using adenovirus: blocking NF-kappaB inhibits both inflammatory and destructive mechanisms in rheumatoid synovium but spares anti-inflammatory mediators. Proc Natl Acad Sci USA 96, 5668–5673 (1999).
Sellner, J., Tauber, M. G. & Leib, S. L. Pathogenesis and pathophysiology of bacterial CNS infections. Handb Clin Neurol 96, 1–16, doi:10.1016/S0072-9752(09)96001-8 (2010).
Meli, D. N., Christen, S., Leib, S. L. & Tauber, M. G. Current concepts in the pathogenesis of meningitis caused by Streptococcus pneumoniae. Curr Opin Infect Dis 15, 253–257 (2002).
Kim, K. S. Pathogenesis of bacterial meningitis: from bacteraemia to neuronal injury. Nat Rev Neurosci 4, 376–385, doi:10.1038/nrn1103 (2003).
Riley, C. P., Cope, T. C. & Buck, C. R. CNS neurotrophins are biologically active and expressed by multiple cell types. J Mol Histol 35, 771–783, doi:10.1007/s10735-004-0778-9 (2004).
McAllister, A. K., Katz, L. C. & Lo, D. C. Neurotrophins and synaptic plasticity. Annu Rev Neurosci 22, 295–318, doi:10.1146/annurev.neuro.22.1.295 (1999).
Binder, D. K. & Scharfman, H. E. Brain-derived neurotrophic factor. Growth Factors 22, 123–131 (2004).
Tanila, H. The role of BDNF in Alzheimer’s disease. Neurobiol Dis, doi:S0969-9961(16)30102-4 (2016).
Makar, T. K. et al. TrkB agonist, 7,8-dihydroxyflavone, reduces the clinical and pathological severity of a murine model of multiple sclerosis. J Neuroimmunol 292, 9–20, doi:10.1016/j.jneuroim.2016.01.002 (2016).
Kozisek, M. E., Middlemas, D. & Bylund, D. B. Brain-derived neurotrophic factor and its receptor tropomyosin-related kinase B in the mechanism of action of antidepressant therapies. Pharmacol Ther 117, 30–51, doi:S0163-7258(07)00152-0 (2008).
Li, L. et al. [Expression of brain-derived neurotrophic factor at acute inflammatory injury of the brain]. Zhejiang Da Xue Xue Bao Yi Xue Ban 32, 433–436 (2003).
Li, L., Shui, Q. X. & Zhao, Z. Y. Regulation of brain-derived neurotrophic factor (BDNF) expression following antibiotic treatment of experimental bacterial meningitis. J Child Neurol 18, 828–834 (2003).
Barichello, T. et al. Correlation between behavioral deficits and decreased brain-derived neurotrophic [correction of neurotrofic] factor in neonatal meningitis. J Neuroimmunol 223, 73–76, doi:10.1016/j.jneuroim.2010.04.004 (2010).
Li, L., Shui, Q. X., Liang, K. & Ren, H. Brain-derived neurotrophic factor rescues neurons from bacterial meningitis. Pediatr Neurol 36, 324–329, doi:S0887-8994(07)00042-2 (2007).
Krock, E. et al. Nerve Growth Factor Is Regulated by Toll-Like Receptor 2 in Human Intervertebral Discs. J Biol Chem 291, 3541–3551, doi:10.1074/jbc.M115.675900 (2016).
Isa, I. L. et al. Hyaluronic Acid Based Hydrogels Attenuate Inflammatory Receptors and Neurotrophins in Interleukin-1beta Induced Inflammation Model of Nucleus Pulposus Cells. Biomacromolecules 16, 1714–1725, doi:10.1021/acs.biomac.5b00168 (2015).
Saha, R. N., Liu, X. & Pahan, K. Up-regulation of BDNF in astrocytes by TNF-alpha: a case for the neuroprotective role of cytokine. J Neuroimmune Pharmacol 1, 212–222, doi:10.1007/s11481-006-9020-8 (2006).
Gaikwad, S. M., Thakur, B., Sakpal, A., Singh, R. K. & Ray, P. Differential activation of NF-kappaB signaling is associated with platinum and taxane resistance in MyD88 deficient epithelial ovarian cancer cells. Int J Biochem Cell Biol 61, 90–102, doi:10.1016/j.biocel.2015.02.001 (2015).
Wu, Y. et al. Inhibiting the TLR4-MyD88 signalling cascade by genetic or pharmacological strategies reduces acute alcohol-induced sedation and motor impairment in mice. Br J Pharmacol 165, 1319–1329, doi:10.1111/j.1476-5381.2011.01572.x (2012).
Kuti, B. P., Bello, E. O., Jegede, T. O. & Olubosede, O. Epidemiological, clinical and prognostic profile of childhood acute bacterial meningitis in a resource poor setting. J Neurosci Rural Pract 6, 549–557, doi:10.4103/0976-3147.165424 (2015).
Barichello, T. et al. Targets for adjunctive therapy in pneumococcal meningitis. J Neuroimmunol 278, 262–270, doi:10.1016/j.jneuroim.2014.11.015 (2015).
Gerber, J. & Nau, R. Mechanisms of injury in bacterial meningitis. Curr Opin Neurol 23, 312–318, doi:10.1097/WCO.0b013e32833950dd (2010).
Blaser, C., Wittwer, M., Grandgirard, D. & Leib, S. L. Adjunctive dexamethasone affects the expression of genes related to inflammation, neurogenesis and apoptosis in infant rat pneumococcal meningitis. PLoS One 6, e17840, doi:10.1371/journal.pone.0017840 (2011).
Barichello, T. et al. Interleukin-1beta Receptor Antagonism Prevents Cognitive Impairment Following Experimental Bacterial Meningitis. Curr Neurovasc Res 12, 253–261, doi:CNR-EPUB-67917 (2015).
Liechti, F. D. et al. The mood-stabilizer lithium prevents hippocampal apoptosis and improves spatial memory in experimental meningitis. PLoS One 9, e113607, doi:10.1371/journal.pone.0113607 (2014).
Lian, D. et al. Exogenous BDNF increases neurogenesis in the hippocampus in experimental Streptococcus pneumoniae meningitis. J Neuroimmunol 294, 46–55, doi:10.1016/j.jneuroim.2016.03.014 (2016).
Bucker, J. et al. Brain-derived neurotrophic factor and inflammatory markers in school-aged children with early trauma. Acta Psychiatr Scand 131, 360–368, doi:10.1111/acps.12358 (2015).
Jiang, Y. et al. Intranasal brain-derived neurotrophic factor protects brain from ischemic insult via modulating local inflammation in rats. Neuroscience 172, 398–405, doi:10.1016/j.neuroscience.2010.10.054 (2011).
Lu, H. et al. Neuroprotective Effects of Brain-Derived Neurotrophic Factor and Noggin-Modified Bone Mesenchymal Stem Cells in Focal Cerebral Ischemia in Rats. J Stroke Cerebrovasc Dis 25, 410–418, doi:10.1016/j.jstrokecerebrovasdis.2015.10.013 (2016).
Ribes, S. et al. Resistance of the brain to Escherichia coli K1 infection depends on MyD88 signaling and the contribution of neutrophils and monocytes. Infect Immun 81, 1810–1819, doi:10.1128/IAI.01349-12 (2013).
Koedel, U. et al. MyD88 is required for mounting a robust host immune response to Streptococcus pneumoniae in the CNS. Brain 127, 1437–1445, doi:10.1093/brain/awh171 (2004).
Liu, S. & Kielian, T. MyD88 is pivotal for immune recognition of Citrobacter koseri and astrocyte activation during CNS infection. J Neuroinflammation 8, 35, doi:10.1186/1742-2094-8-35 (2011).
Rothwarf, D. M. & Karin, M. The NF-kappa B activation pathway: a paradigm in information transfer from membrane to nucleus. Sci STKE 1999, RE1, doi:10.1126/stke.1999.5.re1 (1999).
Koedel, U., Bayerlein, I., Paul, R., Sporer, B. & Pfister, H. W. Pharmacologic interference with NF-kappaB activation attenuates central nervous system complications in experimental Pneumococcal meningitis. J Infect Dis 182, 1437–1445, doi:JID000589 (2000).
Selvaraj, S. K. & Prasadarao, N. V. Escherichia coli K1 inhibits proinflammatory cytokine induction in monocytes by preventing NF-kappaB activation. J Leukoc Biol 78, 544–554, doi:jlb.0904516 (2005).
Kuhn, P. L. & Wrathall, J. R. A mouse model of graded contusive spinal cord injury. J Neurotrauma 15, 125–140, doi:10.1089/neu.1998.15.125 (1998).
Krock, E. et al. Painful, degenerating intervertebral discs up-regulate neurite sprouting and CGRP through nociceptive factors. J Cell Mol Med 18, 1213–1225, doi:10.1111/jcmm.12268 (2014).
Acknowledgements
This work was supported by National Natural Science Foundation of China [grant numbers 81571180 and 81271337].
Author information
Authors and Affiliations
Contributions
Danfeng Xu wrote the main manuscript text. Di Lian performed the in vivo experiment of the study. Zhijie Zhang helped with the in vitro experiment. Ying Liu cultured the infectious organisms for the study. Jiaming Sun performed the histopathological experiments of the study. Prof. Ling Li provided necessary guidance on the performance of all the experiment. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Xu, D., Lian, D., Zhang, Z. et al. Brain-derived neurotrophic factor is regulated via MyD88/NF-κB signaling in experimental Streptococcus pneumoniae meningitis. Sci Rep 7, 3545 (2017). https://doi.org/10.1038/s41598-017-03861-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-03861-z
- Springer Nature Limited
This article is cited by
-
Interactions Among Brain-Derived Neurotrophic Factor and Neuroimmune Pathways Are Key Components of the Major Psychiatric Disorders
Molecular Neurobiology (2022)
-
Chaihu-Shugan-San (Shihosogansan) alleviates restraint stress-generated anxiety and depression in mice by regulating NF-κB-mediated BDNF expression through the modulation of gut microbiota
Chinese Medicine (2021)