Abstract
Solid tumours are infiltrated by effector T cells with the potential to control or reject them, as well as by regulatory T (Treg) cells that restrict the function of effector T cells and thereby promote tumour growth1. The anti-tumour activity of effector T cells can be therapeutically unleashed, and is now being exploited for the treatment of some forms of human cancer. However, weak tumour-associated inflammatory responses and the immune-suppressive function of Treg cells remain major hurdles to broader effectiveness of tumour immunotherapy2. Here we show that, after disruption of the CARMA1–BCL10–MALT1 (CBM) signalosome complex, most tumour-infiltrating Treg cells produce IFNγ, resulting in stunted tumour growth. Notably, genetic deletion of both or even just one allele of CARMA1 (also known as Card11) in only a fraction of Treg cells—which avoided systemic autoimmunity—was sufficient to produce this anti-tumour effect, showing that it is not the mere loss of suppressive function but the gain of effector activity by Treg cells that initiates tumour control. The production of IFNγ by Treg cells was accompanied by activation of macrophages and upregulation of class I molecules of the major histocompatibility complex on tumour cells. However, tumour cells also upregulated the expression of PD-L1, which indicates activation of adaptive immune resistance3. Consequently, blockade of PD-1 together with CARMA1 deletion caused rejection of tumours that otherwise do not respond to anti-PD-1 monotherapy. This effect was reproduced by pharmacological inhibition of the CBM protein MALT1. Our results demonstrate that partial disruption of the CBM complex and induction of IFNγ secretion in the preferentially self-reactive Treg cell pool does not cause systemic autoimmunity but is sufficient to prime the tumour environment for successful immune checkpoint therapy.
Similar content being viewed by others
Main
Local exposure of tumour-infiltrating Treg cells to their cognate antigens sustains their tumour-promoting immunosuppressive functions4. We therefore explored which T-cell-receptor (TCR)-dependent signalling pathways could be targeted to disable tumour-reactive Treg cells. The scaffold protein CARMA1 nucleates assembly of the CBM complex in T cells in response to TCR-dependent PKCθ activity and promotes several functions, including activation of the AP-1, mTOR and classical NF-κB pathways, as well as stabilization of mRNA5. Constitutive genetic deletion of CARMA1, BCL10 or MALT1 abrogates thymic development of Treg cells6,7,8,9,10, but their role in mature Treg cells is unknown.
When we conditionally deleted either one or both alleles of CARMA1 in mature Treg cells by crossing Foxp3YFP-cre to CARMA1flox/flox mice (hereafter referred to as Fcre × C1f/+ or Fcre × C1f/f mice), levels of CARMA1 protein were proportionally reduced in CD4+FOXP3+ Treg cells from lymph nodes (LNs) (Extended Data Fig. 1a). Fcre × C1f/f, but not Fcre × C1f/+ or C1+/+ control mice, stopped thriving at 17 days; most died before 4 weeks of age after a T-helper-1 (TH1)-dominated multiorgan inflammatory disease characterized by splenomegaly, lymphadenopathy, effector differentiation and inflammatory cytokine secretion by conventional T (Tconv) cells, production of autoreactive IgG, and activation of the myeloid compartment (Fig. 1a, Extended Data Figs. 1b–f, 2a–f). Hence, CARMA1 is essential for Treg cells to maintain immune homeostasis, but a reduction in its expression at least up to 50% is tolerated.
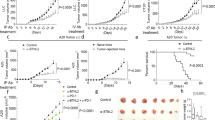
a, Survival of Fcre × C1+/+, C1f/+ and C1f/f mice (n = 8, 10 and 20 per group, respectively). b, Frequency of Treg cells among CD4+ T cells and of eTreg cells among total Treg cells in LNs. c, d, Expression of cytokines (c) and transcription factors (TF) (d) in LN Treg cells after ex vivo stimulation. e, Survival of Fcre × C1f/f mice treated with anti-IFNγ antibodies from day 14 of life, compared with Fcre × C1+/+ and scurfy mice. f, Cytokine expression of YFP+ Treg cells from LNs of nine-week-old female heterozygous Fcre/+ × C1+/+, C1f/+ and C1f/f mice after ex vivo stimulation. g, Frequency of YFP+ Treg cells among CD4+ T cells and of YFP+ eTreg cells among total YFP+ Treg cells in LNs. h, Expression of indicated proteins in YFP+ eTreg cells from 9-week-old mice. Data in b–h represent two independent experiments with similar results. Data are mean and individual replicates. In a and e, *P < 0.05 versus wild type (+/+), &P < 0.05 versus scurfy, and #P < 0.05 versus anti-IFNγ (log-rank (Mantel–Cox) test). In all other panels, *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001 (one-way analysis of variance (ANOVA) with Tukey post hoc test). i, j, Bulk RNA sequencing analysis of YFP+ cTreg and eTreg cells from LNs of Fcre/+ × C1+/+, C1f/+ and C1f/f mice. i, Principal component (PC) analysis of transcriptomes. j, Scaled expression of eTreg signature genes by eTreg cells (defined by fold change > 2 and Padj < 0.01 between C1+/+ cTreg and C1+/+ eTreg cells). Selected eTreg cell genes are annotated.
Absolute numbers of Treg cells were increased in LNs of Fcre × C1f/f mice, concomitant with an increase in overall LN cellularity (Extended Data Fig. 2g, h). However, the overall frequency of Treg cells among CD4+ T cells did not vary with CARMA1 expression, whereas the proportion of CD44highCD62L– effector Treg (eTreg) was strongly reduced in its absence (Fig. 1b). Notably, CARMA1-deficient Treg cells, while retaining expression of FOXP3, almost uniformly secreted IFNγ and—at lower frequencies—secreted IL-4, IL-17 and TNF (Fig. 1c). Although nearly all CARMA1-deficient Treg cells secreted the TH1-cytokine IFNγ, far fewer—and only eTreg cells—expressed the TH1 lineage-defining transcription factor T-bet along with RORγt and, to a lesser degree, GATA-3 (Fig. 1d and Extended Data Fig. 2i, j). Hence, complete—but not partial—deletion of CARMA1 in Treg cells markedly dysregulates their cytokine expression that (in the case of IFNγ) is dissociated from expression of T-bet, and may contribute to the pathogenesis of inflammatory disease. Indeed, Fcre × C1f/f mice died more rapidly than Treg cell-deficient scurfy mice, but their lifespans were similar when IFNγ was neutralized (Fig. 1e). Thus, under inflammatory conditions, CARMA1-deficient Treg cells convert from an immunoregulatory cell type into an IFNγ-secreting pathogenic cell type.
In heterozygous female Fcre/+ × C1f/f mice, random inactivation of the X chromosome causes the yellow fluorescent protein–Cre recombinase (YFP–Cre) fusion protein to be expressed and CARMA1 to be deleted in only half of the Treg cells, whereas the other half maintains immune homeostasis (Extended Data Fig. 3a–c). Under such non-inflammatory conditions, CARMA1-deficient Treg cells did not secrete effector cytokines (Fig. 1f). However, in competition with CARMA1-sufficient Treg cells for niche space, we observed a proportional decline specifically in the frequency of eTreg cells—but not of central Treg (cTreg) cells—that lacked one or both alleles of CARMA1 (Fig. 1g and Extended Data Fig. 3e). The remaining YFP+ eTreg cells expressed less FOXP3 and other proteins that are characteristically increased in expression during the differentiation of cTreg cells into eTreg cells (Fig. 1h). They expressed more of the pro-apoptotic protein BIM, but also more of the anti-apoptotic protein BCL2, which probably reflects impaired differentiation of eTreg cells, as control eTreg cells strongly downregulated both BCL2 and BIM relative to cTreg cells (Extended Data Fig. 3d–h). The in vitro suppressive function of CARMA1-deficient Treg cells was reduced, but not abrogated (Extended Data Fig. 4a, b), and they failed to persist and did not suppress lymphopenia-induced expansion of effector T cells after transfer into RAG1-deficient hosts (Extended Data Fig. 4c). Failure to persist in vivo did not seem to result from accelerated apoptosis, because the previously described high apoptotic rate of eTreg cells11 was not further enhanced in the absence of CARMA1 (Extended Data Fig. 4d). Lack of CARMA1 did not lead to an increase in the formation of FOXP3-negative ‘exTreg’ cells (Extended Data Fig. 4e).
On the basis of global gene expression analyses, CARMA1-deficient eTreg cells were equally dissimilar to control eTreg cells as they were to control cTreg cells, whereas CARMA1-deficient cTreg cells were only moderately dissimilar to control cTreg cells (Fig. 1i). In the latter, only 96 genes were differentially expressed, compared with 344 genes in eTreg cells (Extended Data Fig. 5a and Supplementary Table 1). Based on differences between control cTreg and eTreg cells, we defined an ‘eTreg signature’, which largely overlapped with a previously reported gene set12,13. When examining these 689 genes, hemizygous CARMA1-deletion had only a moderate effect, whereas homozygous deletion induced major changes specifically in the eTreg cell gene expression program (Fig. 1j and Extended Data Fig. 5b). Minor changes in the expression of the Bcl2 family of apoptotic regulator genes occurred during eTreg cell differentiation, but CARMA1-deficient eTreg cells did not deviate from this pattern apart from having less pronounced downregulation of BCL2 and BIM, confirming our observations on protein expression (Extended Data Fig. 6). Thus, a complete—and even a partial—loss of CARMA1 expression impairs eTreg cell differentiation and persistence, but does not induce the cells to become pathogenic or convert to exTreg cells under non-inflammatory conditions. However, in the context of incipient inflammation trigged by a global loss of the suppressive function of Treg cells, CARMA1-deficient Treg cells secrete IFNγ, which further accelerates inflammatory disease.
Failed thymic development of Treg cells in the absence of CARMA1 results from disabled NF-κB signalling and is restored through the expression of a constitutively active form of IκB kinase 2 (referred to as IKK2ca)12. Furthermore, the NF-κB proteins REL (also known as c-Rel) and RELA (p65) have important roles in Treg cell function13,14,15, which suggests that failed activation of NF-κB may primarily account for the effects of CARMA1-deletion in Treg cells. However, the expression of IKK2ca in Treg cells neither prolonged the lifespan of Fcre × C1f/f mice, nor reduced the differentiation of effector Tconv cells (Extended Data Fig. 7a, b). Restoring NF-κB activation did not restore differentiation of eTreg cells, and did not limit the secretion of IFNγ, but only of TNF (Extended Data Fig. 7c, d). Therefore, although NF-κB activation is evidently essential13,16, additional CBM-complex effector functions are also crucial for maintaining Treg cell function. The relevance of these additional functions will need to be investigated, but an initial examination of CARMA1-deficient Treg cells from healthy Fcre/+ × C1f/f mice already revealed decreased expression and TCR-induced phosphorylation of the AP-1 family protein JUN, as well as changes to phosphorylation of FOXO1, possibly reflecting CARMA1- and TBK1-driven regulation of AKT activity17 (Extended Data Fig. 7e, f).
Considering the pro-inflammatory potential of CARMA1-deficient Treg cells, we examined their tumour response. Subcutaneous implantation of the poorly immunogenic BrafV600E × Pten−/− melanoma D4M.3A18 into female Fcre/+ × C1f/f hosts amplified the effects of CARMA1-deficiency on Treg cells, because the frequency not only of eTreg cells but also of total Treg cells was reduced in tumours and tumour-draining LNs (tdLNs) as a function of decreasing CARMA1 expression, accompanied also by a more pronounced reduction in FOXP3 expression (Extended Data Fig. 8a–d). Notably, we observed growth deceleration of D4M.3A melanoma, and of MC38 colon carcinoma, when half of the Treg cells lacked one or both alleles of CARMA1 (Fig. 2a and Extended Data Fig. 8e). Because a mere loss of function in only half of the Treg cells is not predicted to cause loss of tumour tolerance19, this suggested active Treg-cell-mediated anti-tumour activity. Indeed, a large fraction of completely or even partially CARMA1-deficient Treg cells secreted both TNF and IFNγ in situ, whereas these effector cytokines were undetectable in tumour-infiltrating CD4+ and CD8+ Tconv cells (Fig. 2b, c). Importantly, no increase in cytokine secretion by Treg cells was observed in tdLNs or in non-lymphoid tissues, such as skin or lung (Fig. 2d and Extended Data Fig. 8f, g). IFNγ expression in tumour tissue correlated with downregulation, but not loss of FOXP3 in both partially and fully CARMA1-deficient Treg cells (Extended Data Fig. 8h). Notably, destabilization of control Treg cells by IFNγ-producing Treg cells, as described in other settings20, did not occur because no increase in cytokine expression was detectable in YFP− CARMA1-sufficient Treg cells in the same tumours (not shown). Neutralization of IFNγ fully restored tumour growth in Fcre/+ × C1f/f mice (Extended Data Fig. 8i), which suggests a crucial role for this cytokine in Treg-cell-mediated anti-tumour immunity. However, IFNγ may also derive from other cellular sources after Treg cell destabilization. To test the role of Treg-cell-produced IFNγ specifically, we transferred Treg cells with reduced expression of CARMA1 into tumour-bearing C57BL/6 or Ifng–/– mice. In both hosts, Treg cells stunted tumour growth similarly, but not when IFNγ was neutralized, which indicates that Treg-cell-derived IFNγ is both necessary and sufficient for anti-tumour effects (Fig. 2e, f and Extended Data Fig. 8j–m). Therefore, although neither partially nor fully CARMA1-deficient Treg cells cause inflammation in healthy mice, both are selectively destabilized in tumour tissue and secrete IFNγ to decelerate tumour growth.
a, Female Fcre/+ × C1+/+, C1f/+ and C1f/f mice were implanted with D4M.3A melanoma, and tumour growth was recorded. b–d, In situ expression in tumour tissue (b, c) or tdLNs (d) of effector cytokines in YFP+ Treg cells lacking one or both alleles of CARMA1 as well as in CD4+ and CD8+ Tconv cells 18 days after tumour implantation. e, f, One million YFP+ Treg cells from Fcre/+ × C1f/+ or C1+/+ mice were injected intravenously (i.v.) into either C57BL/6 (e) or IFNγ-deficient (f) hosts, which were implanted with D4M.3A melanoma the next day, and tumour growth was recorded. Some IFNγ-deficient hosts were treated with neutralizing anti-IFNγ antibody. Data represent two independent replicates with similar results. Data are mean and either individual replicates (c, d) or s.e.m. (a, e, f). *P < 0.05, **P < 0.01, ****P < 0.0001 (two-way ANOVA with Bonferroni post hoc test in a, f; one-way ANOVA with Tukey post hoc test in c, d; two-tailed Student’s t-test in e).
Expression of IKK2ca restored the frequencies of total Treg and eTreg cells in tdLNs, but not in tumour tissue (Extended Data Fig. 9a). It did not restore FOXP3 expression, only partially reduced TNF and IFNγ co-expression by tumour-infiltrating CARMA1-deficient Treg cells, and did not prevent their anti-tumour activity (Extended Data Fig. 9b–d), which emphasizes the importance of CBM-complex effector functions other than NF-κB activation16 in stabilizing tumour-reactive Treg cells.
To examine whether CARMA1 deletion acutely destabilizes intratumoral Treg cells, we generated Foxp3GFP-creERT2 × CARMA1f/f (hereafter termed FcreERT2 × C1f/f) mice and treated these with tamoxifen to trigger Cre-mediated CARMA1 deletion when tumours were already established (Fig. 3a and Extended Data Fig. 9e). To prevent subsequent recruitment of additional Treg cells from tdLNs, we concurrently blocked lymphocyte tissue egress using the functional S1P receptor antagonist FTY720, as previously described4. Within two days of treatment, tumour growth decelerated (Fig. 3b). A similarly rapid, albeit slightly less pronounced, growth effect as well as increased secretion of effector cytokines by Treg cells resulted from deletion of CARMA1 in only half of the Treg cells (Extended Data Fig. 9f, g). Intratumoral destabilization of Treg cells was accompanied by pronounced induction of macrophage expression of cell-surface major histocompatibility complex class II (MHC-II) molecules, both after constitutive or acute deletion of one or both alleles of CARMA1 in Treg cells (Fig. 3c and Extended Data Fig. 9h). Furthermore, the expression of MHC-I molecules on tumour cells increased, predictably sensitizing them to cytotoxic-T-lymphocyte (CTL)-mediated lysis (Fig. 3d). Although Treg cell-derived IFNγ thus caused widespread tumour inflammation, it also triggered tumour cell-expression of PD-L1, a ligand for the T cell inhibitory receptor PD-1, which suggests that concurrent induction of adaptive immune resistance3 limited improved tumour control resulting from enhanced anti-tumour immune effector functions (Fig. 3d).
a, b, D4M.3A melanoma growth in FcreERT2 × C1+/+ and C1f/f mice treated with tamoxifen from days 8–12 as well as with FTY720 starting the same day until the end of the experiment. Arrow in b indicates the start of treatment. c, d, MHC-II surface expression on F4/80+ tumour macrophages (c), and MHC-I and PD-L1 expression on D4M.3A tumour cells (expressing blue-fluorescent H2B-Cerulean) (d) three days after the initiation of tamoxifen treatment. MFI, mean fluorescence intensity. Data represent two independent replicates with similar results. Data are mean and individual replicates (c, d) or s.e.m. (b). *P < 0.05 (two-tailed Student’s t-test).
Considering the induction of PD-L1 on tumour cells, we hypothesized that antibody-mediated blockade of PD-1 may synergize with the anti-tumour effects of IFNγ-secreting Treg cells. Indeed, treatment with anti-PD-1 antibody simultaneously with CARMA1 deletion in Treg cells enabled much more rapid and consistent control of D4M.3A melanoma than either treatment alone (Fig. 4a). Targeting the CBM complex in Treg cells may thus be highly effective at enhancing the potency of immune checkpoint therapy (ICT) in patients with cancer.
a, Female FcreERT2 × C1+/+ and C1f/f mice were implanted with D4M.3A melanoma, and treated with tamoxifen starting on day 9 until the end of the experiment, as well as with three doses of the anti-PD-1-antibody 29F.1A12 or isotype control, and tumour growth was recorded. b, CBM complex effector pathways and predicted effects (red arrows) of the MALT1 protease inhibitors mepazine and MI-2. c, d, D4M.3A tumour growth in C57BL/6 (c) or RAG1-deficient (d) hosts treated with MALT1 inhibitors (MI-2 or mepazine). Dimethylsulfoxide (DMSO) was used as a vehicle control. e, f, Effects of mepazine treatment for three days on intratumoral Treg cell frequency and their in situ expression of effector cytokines (e), and on the expression of MHC-I and PD-L1 on tumour cells (f). g, h, Synergistic control of tumours by combined anti-PD-1 and mepazine treatment of poorly immunogenic D4M.3A (g) and immunogenic D4M.3A-SIINFEKL (h) tumours in male C57BL/6 hosts. Numbers in parentheses indicate fraction of mice without relapse for more than 12 months after discontinuation of treatment. Data in a, c–f represent two independent replicates with similar results. Data are mean and individual replicates (e, f) or s.e.m. (a, c, d, g, h). Arrows in tumour growth charts indicate the start of treatment. In a, *P < 0.05 versus C1+/+, #P < 0.05 versus C1+/+ + anti-PD-1, and &P < 0.05 versus C1f/f. In g and h, *P < 0.05 versus vehicle (DMSO), #P < 0.05 versus anti-PD-1, and &P < 0.05 versus and mepazine, respectively. In e, *P < 0.05 (two-way ANOVA with Bonferroni post hoc test in a, c, g, h; two-tailed Student’s t-test in d–f).
Although pharmacological inhibitors of the scaffold protein CARMA1 are, to our knowledge, currently not available, inhibitors of MALT1 paracaspase are predicted to attenuate the majority of CBM-complex-dependent effector pathways (Fig. 4b). Indeed, similar to CARMA1-deficient mice, Treg cells are virtually absent in mice that express mutant MALT1 proteins that lack paracaspase activity (replicating continual and complete pharmacological inhibition)21,22,23. We therefore tested the allosteric MALT1 inhibitor mepazine24,25 and the catalytic site binder MI-226 for activity against solid tumours. Both inhibitors produced a similar deceleration in melanoma growth to that observed after deletion of CARMA1 in Treg cells (Fig. 4c), even when CD8+ T cells were depleted (Extended Data Fig. 9i). Systemic inhibition of MALT1 will also target cells other than Treg cells, including melanoma cells27. However, no effect on tumour growth occurred in RAG1-deficient mice that lack lymphocytes (Fig. 4d). Inhibition of MALT1 did not synergize with deletion of CARMA1 in Treg cells, which suggests that the anti-tumour activity of MALT1 does not result from effects other than attenuated CBM complex function in Treg cells (Extended Data Fig. 9j). Because MALT1 inhibition is predicted to attenuate, and not enhance lymphocyte effector functions28, we conclude that its effect on tumour growth is probably mediated through destabilization of Treg cells. Similar to Treg-cell-specific deletion of CARMA1, treatment with mepazine caused a rapid, albeit less pronounced, induction of TNF and IFNγ expression by tumour-infiltrating Treg cells (Fig. 4e). Short-term in vitro treatment of Treg cells triggered only a minor reduction of FOXP3, GITR and CTLA-4 expression (Extended Data Fig. 10a) and did not induce IFNγ secretion (data not shown), which indicates that the latter occurs only under the conditions of the tumour microenvironment. Accordingly, mepazine caused upregulation of the expression of PD-L1 and MHC-I molecules on tumour cells in vivo (Fig. 4f) and induction of Ifng and a wide range of IFNγ-regulated genes indicative of both TH1 inflammation and adaptive immune resistance in tumour tissue (Extended Data Fig. 10b). In contrast to constitutive deletion of CARMA1, short-term inhibition of MALT1 did not reduce the frequency of Treg cells, and the expression of Treg-cell-associated genes in tumour tissue was not reduced (Fig. 4e and Extended Data Fig. 10c). Nevertheless, in addition to overall enhanced infiltration of immune cells, treatment with mepazine specifically increased the frequencies of CTL and natural killer cells in tumour tissue (Extended Data Fig. 10d–h).
A high tumour mutational load favours response to ICT in patients with cancer29,30, and a low mutational burden remains a major challenge that limits the success of this form of immunotherapy to some cancer types and to a minority of patients. Accordingly, D4M.3A melanoma, which carries a negligible mutational load relative to the C57BL/6J reference exome (D. E. Fisher, personal communication), is completely resistant to anti-PD-1 monotherapy in male hosts (Fig. 4g), in contrast to female hosts, in which Y-antigen-expressing male D4M.3A tumours showed a partial response (Fig. 4a). Concurrent MALT1 inhibition, however, synergized with anti-PD-1 treatment, and arrested tumour growth even in male hosts (Fig. 4g). Anti-PD-1 treatment did not further increase Treg cell expression of IFNγ, indicating that PD-1 did not restrict the pro-inflammatory function of destabilized Treg cells (Extended Data Fig. 10i). Furthermore, when we raised the immunogenicity of D4M.3A tumours by expressing the chicken ovalbumin-derived SIINFEKL epitope as a surrogate mutational neoantigen, we observed an initial response to anti-PD-1 monotherapy, but 40% of tumours relapsed. A combination of anti-PD-1 antibodies with mepazine, however, produced accelerated rejection and prevented relapse (Fig. 4h). Finally, to explore the effects of MALT1 inhibition on other cancer types, we treated mice implanted with MC38 colon carcinoma. Although anti-PD-1 monotherapy had only a moderate effect on late-stage tumours, combination with mepazine enabled profound tumour control and relapse-free rejection in most mice (Extended Data Fig. 10j). Hence, systemic inhibition of MALT1 inflames the tumour environment and renders poorly immunogenic tumours responsive to anti-PD-1 therapy while enhancing responses of immunogenic tumours and minimizing the frequency of relapse, a common problem in clinical ICT31.
We propose that inhibition of MALT1 protease or of other CBM complex functions could be a useful therapeutic strategy to elicit an intratumoral TH1 autoimmune reaction mediated by locally destabilized, preferentially self-reactive Treg cells. Pro-inflammatory effects of destabilized Treg cells seem to outweigh any potential attenuation of immune effector cell activities through MALT1 inhibition. Owing to its selectivity for intratumoral Treg cells, this treatment may increase the fraction of patients with cancer who respond to PD-1/PD-L1-targeted ICT or other forms of immunotherapy, without inducing systemic autoimmune toxicity.
Methods
Mice
Foxp3YFP-cre (ref. 32), Foxp3GFP-creERT2 (ref. 33), ROSA26-stopf/f-YFP (ref. 34), ROSA26-stopf/f-IKK2ca (ref. 35), Ifng−/−36, B6-scurfy (ref. 37) and C57BL/6/J mice were purchased from Jackson Laboratories. R. J. Xavier and J. J. Moon provided CARMA1f/f (ref. 38) and Rag1−/− mice, respectively. Animals were housed in specific-pathogen-free facilities at the Massachusetts General Hospital (MGH) and all experimental studies were approved and performed in accordance with guidelines and regulations implemented by the MGH Institutional Animal Care and Use Committee (IACUC). For survival studies, the age of mice at euthanasia mandated by a moribund state of health was recorded in Kaplan–Meyer plots.
Tumour cell lines
The BrafV600E × Pten−/− melanoma cell line D4M.3A (ref. 18) was provided by D. E. Fisher. For some experiments, D4M.3A cells were lentivirally transduced to express a blue fluorescent histone H2B-Cerulean fusion protein (D4M.3A-H2B-Cerulean), as previously described39, to facilitate detection by flow cytometry. To generate D4M.3A-SIINFEKL tumours expressing the chicken ovalbumin-derived H-2Kb-restricted SIINFEKL peptide, we transduced D4M.3A cells with a VSV-G pseudotyped pHAGE-EF1α lentiviral vector engineered to express a fusion of histone H2B and Cerulean separated by two copies of the SIINFEKL minigene and its native flanking sequences in the ovalbumin protein to facilitate processing for antigen presentation. The colon adenocarcinoma cell line MC3840 was obtained from A. D. Luster. All tumour lines were grown in DMEM with 10% fetal calf serum (FCS) and used for experiments when in exponential growth phase.
Tumour growth studies and treatments
One million D4M.3A, D4M.3A-H2B-Cerulean, D4M.3A-SIINFEKL or MC38 tumour cells were injected subcutaneously in 100 μl HBSS without Ca2+ into the flanks of mice. Wherever possible, animals were randomized into treatment groups. Tumour volumes were measured every second to third day after the start of treatments and calculated as V = (length × width2)/2.
Tamoxifen (1 mg per mouse in 100 μl of a 9:1 mixture of olive oil and ethanol) was injected intraperitoneally daily as indicated. FTY720 (1 mg kg−1 bodyweight) in 150 μl H2O was injected intraperitoneally every other day until the end of the experiment. Anti-IFNγ antibody (500 μg per mouse; clone XMG1.2) was injected intraperitoneally on day 14 after birth or on the day of tumour implantation and then every other day thereafter until the end of the experiment. Anti-PD-1 (200 μg; clone 29F.1A12) or rat IgG2a isotype control (200 μg; clone 2A3) was injected intraperitoneally three times in 100 μl PBS every other day at the indicated time points. Anti-CD8α (150 μg; clone YTS169.4) was injected in 100 μl PBS every other day from the indicated time point until the end of the experiment. Mepazine (16 mg kg−1 bodyweight in 5% dimethylsulfoxide (DMSO)) or MI-2 (20 mg kg−1 in 5% DMSO in purfied H2O) was injected intraperitoneally daily starting at the indicated time points until the end of the experiment, unless indicated otherwise. For adoptive Treg cell transfer studies, CD4+ YFP+ Treg cells were purified to more than 95% purity through magnetic-activated cell sorting (Miltenyi) from LNs and spleen of Fcre × C1f/+ or C1+/+ mice and 106 cells per mouse were injected intravenously into the tail vein the day before tumour implantation.
Preparation of single-cell suspensions, antibody staining and flow cytometry
Heparinized peripheral blood collected through sub-mandibular vein puncture was treated with ACK red blood cell lysis buffer. LNs and spleens were passed through 40-μm cell strainers, followed by red blood cell lysis (spleens only). Tumours and lung tissue were minced into small fragments and treated with 1.5 mg ml−1 collagenase IV and 50 U ml−1 DNase I for 30 min at 37 °C under agitation. Skin tissue was digested in medium containing 2% FCS, 10 mM HEPES, 0.5 mg ml−1 hyaluronidase, 1.5 mg ml−1 collagenase IV, and 50 U ml−1 DNase I for 45 min at 37 °C under agitation. Residual tissue fragments were mechanically dissociated.
Cell surface proteins were stained for 20 min at 4 °C with the following antibodies against: CD11b (M1/70), CD120b/TNFR2 (polyclonal Armenian hamster IgG), CD274/PD-L1 (10F.9G2), CD357/GITR (DTA-1), CD4 (GK1.5), CD45 (30-F11), CD62L (MEL-14), CD73 (TY/11.8), CD8α (53-6.7), CD90.2 (30-H12), F4/80 (BM8), H-2Kb (AF6-88.5), -I-A/I-E (M5/114.15.2), Ly-6C (HK1.4), Ly-6G (1A8), CD45R/B220 (RA3-6B2), CD64 (FcγRI) (X54-5/7.1), CD11c (N418), CD103 (2E7), NK-1.1 (PK136), CD335 (NKp46) (29A1.4), CD3 (17A2), CD19 (1D3/CD19), CD45RB (16A), and CD44 (IM7) (BioLegend), CD11c (HL3) and CD25 (PC61.5) (eBIoscience).
Intracellular and nuclear proteins were stained for 60 min at room temperature after permeabilization and fixation (Mouse regulatory T cell staining Kit; eBioscience) using antibodies against: CD152/CTLA-4-(UC10-4B9), TNF (MP6-XT22), IL-4 (11B11), IL-17A (TC11-18H10.1), IFNγ (XMG1.2), T-bet (4B10), and Ki67 (16A8) (BioLegend), BIM (C34C5), CARD11/CARMA1 (1D12) (Cell Signaling), FOXP3 (FJK-16 s, eBioscience), GATA-3 (L50-823) and Ki67 (B56) (BD Biosciences), RORγt (AFKJS-9) and GFP (rabbit polyclonal) (Invitrogen). Polyclonal goat anti-rabbit Ig (H+L) secondary antibody (Life Technologies) was used to reveal primary anti-CARMA1 staining.
Preceding antibody staining, dead cells were stained using the fixable viability violet dye Zombie Red (Biolegend) for 15 min at room temperature, followed by blocking of Fc receptors with TruStain FcX (Biolegend) for 20 min at 4 °C. Cells were analysed on LSR II, LSRFortessa or LSRFortessa X-20 flow cytometers (BD Biosciences), and data were analysed with FlowJo software v.9.9.5.
Phospho-protein analysis
LN single-cell suspensions were stained using the fixable viability dye ZombieRed (Biolegend) for 15 min at room temperature, and added for 30 min at 37 °C to tissue culture plates pre-coated overnight with anti-CD3ε (clone 145-2C11) and anti-CD28 (clone 37.51) antibodies (at 10 μg ml−1 of each antibody), or to uncoated control plates. Samples were then fixed in 4% paraformaldehyde (PFA) for 10 min at room temperature, and permeabilized for 20 min through dropwise addition of 1 ml ice-cold methanol. Cells were then stained for CD90.2 (30-H12), CD4 (GK1.5), CD8α (53-6.7), CD44 (IM7) (BioLegend), Foxp3 (FJK-16 s, eBioscience), pFoxo1 (Thr24)/Foxo3a (Thr32), p-c-Jun (Ser73) (D47G9) (Cell Signaling) and GFP (rabbit polyclonal Ab) (Invitrogen).
Analysis of in situ and ex vivo stimulated cytokine secretion
To detect in situ cytokine secretion, mice were slowly injected intravenously with 500 μg of brefeldin A in 250 μl PBS 6 h before euthanization and intracellular cytokine staining.
To detect cytokine secretion in T cells upon ex vivo re-stimulation, single-cell suspensions from tumours and LNs were resuspended in RPMI 1640 with 10% FCS and added to anti-CD3 (clone 145-2C11)/anti-CD28 (clone 37.51) antibody-coated (overnight at 10 μg ml−1 antibody) tissue culture plates for 8 h at 37 °C in the presence of 1 μg ml−1 Golgiplug and Monensin (both from Biolegend) and cells processed for intracellular cytokine staining.
Analysis of exTreg cells
CD4+ YFPbright cells were first purified by FACS from LNs and spleens of Foxp3YFP-cre/+ × CARMA1f/f (or f/+ or +/+) × ROSA26YFP mice and stained for FOXP3 expression for flow cytometry analysis, as described above.
In vivo and in vitro suppression
For in vivo suppression studies, 3 × 105 Miltenyi (negative selection) enriched CD4+ and FACS sorted (>98% purity) CD45RBhigh YFP− cells from LNs and spleens of Foxp3YFP-cre/cre mice were intravenously injected into the tail vein of Rag1−/− mice with or without 1 × 105 Miltenyi (negative selection) enriched CD4+ and FACS sorted (>98% purity) YFPbright Treg cells from LNs and spleens of Foxp3YFP-cre/+ × CARMA1f/f (or CARMA1f/+ or CARMA1+/+) × ROSA26YFP mice.
For in vitro suppression studies, 1 × 104 FACS-sorted (>98% purity) CD4+ YFP− conventional T cells from LNs and spleens of Foxp3YFP-cre/cre mice were labelled with 5 μM CellTrace Violet and stimulated with 250 ng ml−1 of anti-CD3 monoclonal antibody (145-2c11, Biolegend) in presence of 2.5 × 104 T-cell depleted splenocytes and different concentrations (from 1:1 to 1:16) of Miltenyi (negative selection) enriched CD4+ and FACS sorted (>98% purity) YFPbright Treg cells from LNs and spleens of Foxp3YFP-cre/+ × CARMA1f/f (or CARMA1f/+ or CARMA1+/+) × ROSA26-stopf/f-YFP mice. CD4+ YFP– conventional T cell proliferation was read out after 72 h, as previously described41. In brief, percentage of suppression was scaled from 0 (proliferation of conventional T cell in absence of Treg cells) to 100 (complete absence of proliferation).
In vitro apoptosis
Enriched CD4+ and FACS-purified (>99% purity) YFPbright Treg cells from LNs of Foxp3YFP-cre/+ × CARMA1f/f (or CARMA1+/+) × ROSA26-stopf/f-YFP mice were added for 6 and 18 h at 37 °C to tissue culture plates pre-coated overnight with anti-CD3ε (clone 145-2C11) and anti-CD28 (clone 37.51) antibodies (at 10 μg ml−1 of each antibody). Viability of CD44lowCD62L+ cTreg and CD44highCD62L– eTreg cells was then read out by annexin V and Zombie Red staining (Biolegend).
RNA sequencing studies: sample collection
CD4+ T cells from LNs and spleens of Fcre/+ × C1+/+, C1 f/+ or C1 f/f mice were pre-enriched by immunomagnetic cell sorting (Miltenyi negative selection) and then 5 × 103 YFP+CD4+CD44lowCD62L+ cTreg cells per animal and the same number of YFP+CD4+CD44highCD62L– eTreg cells were sorted to >99% purity directly into 10 μl lysis buffer consisting of TCL buffer (Qiagen) and 1% of β-mercaptoethanol. Samples were then flash-frozen and kept at −80 °C before further processing following a modified version of the Smart-Seq2 protocol11,12,14, as described below. A total of 18 samples was collected, but 2 samples were discarded for technical reasons.
Reverse transcription
Samples were thawed on ice for 2 min, and then centrifuged at 2,500 rpm at 4 °C for 1 min and the RNA concentration normalized. RNA (1.9 μl per sample) was moved to a full-skirt 96-well plate (Eppendorf). Each sample was then mixed with 1 μl 10 μM RT primer 5′-AAGCAGTGGTATCAACGCAGAGTACTTTTTTTTTTTTTTTTTTTTTTTTTTTTTTVN-3′ (IDT), 1 μl 10 mM dNTP (Life Technologies/Thermo Fisher Scientific), and 0.1 μl SUPERase·In RNase-Inhibitor (20 U μl−1, Life Technologies/Thermo Fisher Scientific). Samples were denatured at 72 °C for 3 min using an Eppendorf Mastercycler and placed immediately on ice afterwards. The Reverse Transcription Mix (7 μl) was subsequently added to every well, consisting of: 2 μl 5× RT buffer (Thermo Fisher Scientific), 2 μl 5 M betaine (Sigma-Aldrich), 0.9 μl 100 mM MgCl2 (Sigma-Aldrich), 1 μl 10 μM TSO (5′-AAGCAGTGGTATCAACGCAGAGTACATrGrG+G-3′, Exiqon), 0.25 μl SUPERase·In RNase-Inhibitor (20 U μl−1, Life Technologies/Thermo Fisher Scientific), 0.1 μl Maxima H Minus Reverse Transcriptase (200 U μl−1, Thermo Fisher Scientific) and 0.75 μl nuclease-free water. Reverse transcription was carried out by incubating the plate at 50 °C for 90 min, followed by heat inactivation at 85 °C for 5 min.
PCR pre-amplification and cDNA purification
PCR Mix (14 μl, consisting of 0.5 μl 10 μM PCR primer 5′-AAGCAGTGGTATCAACGCAGAGT-3′ (IDT), 12.5 μl 2× KAPA HiFi HotStart ReadyMix (KAPA Biosystems) and 1 μl nuclease-free water) was added to each well for a final PCR reaction volume of 25 μl. The reaction was carried out with an initial incubation at 98 °C for 3 min, followed by 16 cycles at 98 °C for 15 s, 67 °C for 20 s, and 72 °C for 6 min, and a final extension at 72 °C for 5 min. PCR products were purified by mixing them with 20 μl (0.8×) of Agencourt AMPureXP SPRI beads (Beckman-Coulter), followed by a 6-min incubation period at room temperature. The plate was then placed onto a magnet for 6 min before removing the supernatant. SPRI beads were washed twice with 100 μl of freshly prepared 70% ethanol, with care being taken to avoid loss of beads during the washes. After removing all residual ethanol traces, SPRI beads were left to dry at room temperature for 10 min. The beads were then resuspended in 20 μl of TE buffer (Teknova) and incubated at room temperature for 5 min. The plate was placed on the magnet for 5 min before transferring the supernatant containing the amplified cDNA to a new 96-well plate. This cDNA SPRI clean-up procedure was repeated a second time to remove all residual primer dimers. The concentration of amplified cDNA was measured on the Synergy H1 Hybrid Microplate Reader (BioTek) using the Qubit dsDNA High Sensitivity Assay Kit (Life Technologies/Thermo Fisher Scientific). The cDNA size distribution of few selected wells was assessed on a High-Sensitivity Bioanalyzer Chip (Agilent), and the expected size distribution sharply peaked around 2 kb.
Sequencing library preparation
Library preparation was carried out using the Nextera XT DNA Sample Kit (Illumina) with custom indexing adapters, allowing the 18 libraries to be simultaneously generated in a 384-well PCR plate (Eppendorf). For each library, the amplified cDNA was normalized to a 0.15–0.20 ng μl−1 concentration range. The tagmentation reaction consisted of mixing 0.625 μl of normalized cDNA with 1.25 μl of Tagmentation DNA (TD) buffer and 0.625 μl of Amplicon Tagment enzyme Mix (ATM). The 2.5-μl reaction was incubated at 55 °C for 10 min and then immediately placed on ice upon completing this incubation step. The reaction was quenched with 0.625 μl of Neutralize Tagment (NT) buffer and incubated at room temperature for 10 min. The libraries were amplified by adding 1.875 μl of Nexstera PCR Master (NPM) Mix, 0.625 μl of 10 μM i5 adaptor 5′-AATGATACGGCGACCACCGAGATCTACAC[i5]TCGTCGGCAGCGTC-3′ (IDT), in which [i5] signifies the 8-bp i5 barcode sequence (see below for sequences), and 0.625 μl of 10 μM i7 adaptor 5′CAAGCAGAAGACGGCATACGAGAT[i7]GTGACTGGAGTTCAGACGTGTGCTCTTCCGATCTGGG-3′ (IDT), in which [i7] represents the reverse-complement of the 8-bp i7 barcode sequence (see below for sequences used). The PCR was carried out at an initial incubation at 72 °C for 3 min, 95 °C for 30 s, followed by 12 cycles of (95 °C for 10 s, 55 °C for 30 s, 72 °C for 1 min), and a final extension at 72 °C for 5 min. Following PCR amplification, 2.5 μl of each library were pooled together in a 1.5-ml Eppendorf tube. The pool was mixed with 67.5 μl (0.9× ratio for 2.5 μl of 30 samples pooled together) of Agencourt AMPureXP SPRI beads (Beckman-Coulter) and incubated at room temperature for 5 min. The pool was then placed on a magnet (DynaMag-2, Life Technologies) and incubated for 5 min. The supernatant was removed and the SPRI beads were washed twice with 1 ml of freshly prepared 70% ethanol. After removing all residual ethanol traces, the SPRI beads were left to dry at room temperature for 10 min. The beads were resuspended in 100 μl of nuclease-free water and incubated at room temperature for 5 min. The tube was then placed back on the magnet for 3 min before transferring the supernatant to a new 1.5-ml Eppendorf tube. This SPRI clean-up procedure of the library was repeated a second time to remove all residual primer dimers, using the same approach. The concentration of the pooled libraries was measured using the Qubit dsDNA High Sensitivity Assay Kit (Life Technologies/Thermo Fisher Scientific), and the library size distribution measured on a High-Sensitivity Bioanalyzer Chip (Agilent), showing the expected size distribution of 300–500 bp. The 18 pooled samples were sequenced as paired-end on an Illumina NextSeq 500 instrument using the NextSeq 500/550 High Output v2 kit (75 cycles).
i5 barcodes: AAGTAGAG, ACACGATC, TGTTCCGA. i7 barcodes: GAATTGCT, GTCAAGTT, ATCCGACA, CAAGGCGA, AGTGTCTT, GACCGAGA.
RNA sequencing analysis
Raw sequencing reads were demultiplexed and converted to FASTQ files using Illumina bcl2fastq2 Illumina software (version 2.17.1.14). FASTQ sequencing reads were then aligned to mm10 reference genome using the STAR aligner with default parameters42. RSEM (v.1.2.8) was used to quantify gene expression level from aligned reads and generate count expression matrices for each experimental condition43. We filtered out lowly expressed genes with a count per million (CPM) < 0.5 in more than two conditions, leaving a total of 14,168 genes for further analysis. The distribution of log2 normalized CPM data was visualized to assess for coverage, and all conditions had similar distributions.
Gene expression analysis
Gene expression matrices were analysed using the limma package in R44. The global topology of quantile normalized data was visualized using the multidimensional scaling (plotMDS) function in limma after removing batch effects using the removebatchEffect function in limma with default parameters taking into account design and batch matrices. Differential gene expression was performed using empirical Bayesian statistics (eBayes) function in limma simultaneously correcting for batch using blocking terms for batch covariates. Differentially expressed genes with log fold change greater than 1 and a P value below cut-off were visualized using the heatmap.2 function in gplots. All P values were corrected for multiple hypothesis testing using Benjamini–Hochberg correction. For R scripts used to perform the gene expression analyses see Supplementary Methods. The same differential expression steps were used to re-analyse the gene expression data from GEO accession GSE82008 to obtain the list of differentially expressed genes between c-Rel and p65 knockout versus wild-type resting and activated Treg cells. A list of 831 ‘eTreg signature’ genes from ref. 16 was obtained by direct correspondence with the authors. Overlap between differentially expressed genes, including the list of eTreg cell signatures from the current study and ref. 16, was visualized using the vennDiagram function in limma.
Quantitative RT–PCR
For analysis of gene expression, RNA was isolated (AllPrep, DNA/RNA Mini kit; Qiagen) from CD4+ GFP+ Treg cells sorted to >99% purity from tdLNs and tumours, or from homogenized tumour tissue, and reverse transcribed using iScript cDNA Synthesis Kit (Bio-RAD). Quantitative reverse transcription (RT–PCR) was performed using iQ SYBR green supermix (Bio-RAD) and primers: CARMA1 Fwd 5′-ACATGCTGAGCCGTTACATCA-3′, CARMA1 Rev 5′-CCACATAGCCCCTTTGTCCC-3′, Ifng Fwd 5′-CGGCACAGT CATTGAAAGCCTA-3′, Ifng Rev 5′-GTTG CTGATGGCC TGATTGTC-3′, Ctla4 Fwd 5′-GCTTCCTAGATTACCCCTTCTGC-3′, Ctla4 Rev 5′-CGGGCATGG TTCTGGATCA-3′, CD25-Fwd 5′-CCACATTCAAAGCC CTCTCCTA-3′, CD25-Rev 5′-GTTTTCCCACACTTCATCTTGC-3′, Foxp3 Fwd 5′-TTGG CCAGCGCCA TCTT-3′, Foxp3 Rev 5′-TGCCTCCTCCAGAGAGAAGTG-3′, GITR (also known as Tnfrsf18) Fwd 5′-AAGGTTCAGAACGGAAGTG-3′, GITR Rev 5′-GGGTCTCCACAGTGGTACT-3′, CD73 (also known as Nt5e) Fwd 5′-CAA ATCCCACACAACCACTG-3′, CD73 Rev 5′-TGCTCACTTGGTCACA GGAC-3′, Gzmb Fwd 5′-CATGTAGGGTCGAGAGTGGG-3′, Gzmb Rev 5′-CCTCCTGC TACTGCTGAC CT-3′, Pdl1 (also known as Cd274) Fwd 5′-TGCTGCATAATCAGCTACGG-3′, Pdl1 Rev 5′-GCTGGTCACATT GAGAAGCA-3′, Socs1-Fwd 5′-ACAAGCTGCTACAACCAGG G-3′, Socs1 Rev 5′-ACT TCTGGCTGGAGACCTCA-3′, Tap1 Fwd 5′-GTGGCCGCAGTG GGA CAAGAG-3′, Tap1 Rev 5′-AGGGCACTGGTGGCATCATC-3′, Stat1 Fwd 5′-TGGTGAAATTGCAAG AGCTG-3′, Stat1 Rev 5′-CAGACTTCCG TTGGTGGATT-3′, Irf1 Fwd 5′-CAG AGGAAAG AGAGAAAGTCC-3′, Irf1 Rev 5′-CACACGGTGACAGTGCTGG, Cxcl10 Fwd 5′-CATC CTGCTGGGT CTGAGTG-3′, Cxcl10-Rev 5′-ATTCTCACTGGCCCGTCATC, Nos2 Fwd 5′-CAAGAGAGTGCTGTTCCAGGT-3′ and Nos2 Rev 5′-GAGCACGCTGAGT ACC TCATT-3′, Gapdh Fwd 5′-TGGTGAAGGTCGGTGAAC-3′ and Gapdh Rev 5′-CC ATGTAGTTGAGGTCAATGAAGG-3′. Results were expressed as 2−ΔCt relative to the house keeping gene Gapdh.
Histology
Tissue samples obtained from all organs were fixed in 10% buffered formalin for 48 h, trimmed and placed into microcassettes, and embedded in paraffin wax. Sections of 5 μm were stained with haematoxylin and eosin according to standard procedures.
Immunofluorescence
Kidney, liver, and stomach from a Rag1−/− mouse were embedded in OCT and flash-frozen in cold methylbutane equilibrated on dry ice. Sections of 10 μm were permeabilized with pre-cooled 90% methanol for 10 min at −20 °C, blocked in TruStain FcX (93, Biolegend) with 1% goat serum and 0.25% BSA in PBS for 60 min, incubated with sera (1:100 dilution) from Foxp3YFP-cre × CARMA1f/f (or CARMA1 f/+ or CARMA1+/+) mice for 120 min and stained with anti-mouse IgG (H+L)-Alexa Fluor 647 (1:500) (A-21235, Thermo Fisher) and DAPI (Sigma) for 120 min. Sections were mounted on coverslips in Prolong (Thermo Fisher) and imaged with LSM 780 AxioObserver confocal microscope (Carl Zeiss) using a 20× lens (Apochromat, 0.8 W).
Statistical analysis
A two-tailed Student’s t-test was used for comparisons between two groups, and a two-way ANOVA with Bonferroni post hoc test (multiple time points) or one-way ANOVA with Tukey post hoc test (single time points) was used for comparisons across multiple groups, unless otherwise indicated. A log-rank (Mantel–Cox) test was used to compare survival curves. All statistical tests were performed with GraphPad Prism software, and P < 0.05 was considered statistically significant. No statistical methods were used to predetermine sample size. Investigators were not blinded to allocation during experiments and outcome assessment.
Reporting summary
Further information on research design is available in the Nature Research Reporting Summary linked to this paper.
Data availability
All datasets generated during the current study are available from the corresponding authors upon reasonable request. RNA sequencing data have been deposited at the Gene Expression Omnibus (GEO) under accession number GSE129480.
References
Savage, P. A., Leventhal, D. S. & Malchow, S. Shaping the repertoire of tumor-infiltrating effector and regulatory T cells. Immunol. Rev. 259, 245–258 (2014).
Mellman, I., Coukos, G. & Dranoff, G. Cancer immunotherapy comes of age. Nature 480, 480–489 (2011).
Spranger, S. et al. Up-regulation of PD-L1, IDO, and Tregs in the melanoma tumor microenvironment is driven by CD8+ T cells. Sci. Transl. Med. 5, 200ra116 (2013).
Bauer, C. A. et al. Dynamic Treg interactions with intratumoral APCs promote local CTL dysfunction. J. Clin. Invest. 124, 2425–2440 (2014).
Meininger, I. & Krappmann, D. Lymphocyte signaling and activation by the CARMA1-BCL10-MALT1 signalosome. Biol. Chem. 397, 1315–1333 (2016).
Medoff, B. D. et al. Differential requirement for CARMA1 in agonist-selected T-cell development. Eur. J. Immunol. 39, 78–84 (2009).
Molinero, L. L. et al. CARMA1 controls an early checkpoint in the thymic development of FoxP3+ regulatory T cells. J. Immunol. 182, 6736–6743 (2009).
Barnes, M. J. et al. Commitment to the regulatory T cell lineage requires CARMA1 in the thymus but not in the periphery. PLoS Biol. 7, e1000051 (2009).
Brüstle, A. et al. MALT1 is an intrinsic regulator of regulatory T cells. Cell Death Differ. 24, 1214–1223 (2017).
Schmidt-Supprian, M. et al. Differential dependence of CD4+CD25+ regulatory and natural killer-like T cells on signals leading to NF-κB activation. Proc. Natl Acad. Sci. USA 101, 4566–4571 (2004).
Smigiel, K. S. et al. CCR7 provides localized access to IL-2 and defines homeostatically distinct regulatory T cell subsets. J. Exp. Med. 211, 121–136 (2014).
Long, M., Park, S.-G., Strickland, I., Hayden, M. S. & Ghosh, S. Nuclear factor-κB modulates regulatory T cell development by directly regulating expression of Foxp3 transcription factor. Immunity 31, 921–931 (2009).
Oh, H. et al. An NF-κB transcription-factor-dependent lineage-specific transcriptional program promotes regulatory T cell identity and function. Immunity 47, 450–465.e5 (2017).
Vasanthakumar, A. et al. The TNF receptor superfamily-NF-κB axis is critical to maintain effector regulatory T cells in lymphoid and non-lymphoid tissues. Cell Rep. 20, 2906–2920 (2017).
Messina, N. et al. The NF-κB transcription factor RelA is required for the tolerogenic function of Foxp3+ regulatory T cells. J. Autoimmun. 70, 52–62 (2016).
Grinberg-Bleyer, Y. et al. NF-κB c-Rel is crucial for the regulatory T cell immune checkpoint in cancer. Cell 170, 1096–1108.e13 (2017).
Yu, J. et al. Regulation of T-cell activation and migration by the kinase TBK1 during neuroinflammation. Nat. Commun. 6, 6074 (2015).
Jenkins, M. H. et al. Multiple murine BRafV600E melanoma cell lines with sensitivity to PLX4032. Pigment Cell Melanoma Res. 27, 495–501 (2014).
Pierson, W. et al. Antiapoptotic Mcl-1 is critical for the survival and niche-filling capacity of Foxp3+ regulatory T cells. Nat. Immunol. 14, 959–965 (2013).
Overacre-Delgoffe, A. E. et al. Interferon-γ drives Treg fragility to promote anti-tumor immunity. Cell 169, 1130–1141.e11 (2017).
Gewies, A. et al. Uncoupling Malt1 threshold function from paracaspase activity results in destructive autoimmune inflammation. Cell Reports 9, 1292–1305 (2014).
Jaworski, M. et al. Malt1 protease inactivation efficiently dampens immune responses but causes spontaneous autoimmunity. EMBO J. 33, 2765–2781 (2014).
Bornancin, F. et al. Deficiency of MALT1 paracaspase activity results in unbalanced regulatory and effector T and B cell responses leading to multiorgan inflammation. J. Immunol. 194, 3723–3734 (2015).
Nagel, D. et al. Pharmacologic inhibition of MALT1 protease by phenothiazines as a therapeutic approach for the treatment of aggressive ABC-DLBCL. Cancer Cell 22, 825–837 (2012).
Schlauderer, F. et al. Structural analysis of phenothiazine derivatives as allosteric inhibitors of the MALT1 paracaspase. Angew. Chem. Int. Edn Engl. 52, 10384–10387 (2013).
Fontan, L. et al. MALT1 small molecule inhibitors specifically suppress ABC-DLBCL in vitro and in vivo. Cancer Cell 22, 812–824 (2012).
Wang, Y. et al. MALT1 promotes melanoma progression through JNK/c-Jun signaling. Oncogenesis 6, e365 (2017).
Thome, M., Charton, J. E., Pelzer, C. & Hailfinger, S. Antigen receptor signaling to NF-κB via CARMA1, BCL10, and MALT1. Cold Spring Harb. Perspect. Biol. 2, a003004–a003004 (2010).
Le, D. T. et al. PD-1 blockade in tumors with mismatch-repair deficiency. N. Engl. J. Med. 372, 2509–2520 (2015).
Rizvi, N. A. et al. Cancer immunology. Mutational landscape determines sensitivity to PD-1 blockade in non-small cell lung cancer. Science 348, 124–128 (2015).
Zaretsky, J. M. et al. Mutations associated with acquired resistance to PD-1 blockade in melanoma. N. Engl. J. Med. 375, 819–829 (2016).
Rubtsov, Y. P. et al. Regulatory T cell-derived interleukin-10 limits inflammation at environmental interfaces. Immunity 28, 546–558 (2008).
Rubtsov, Y. P. et al. Stability of the regulatory T cell lineage in vivo. Science 329, 1667–1671 (2010).
Srinivas, S. et al. Cre reporter strains produced by targeted insertion of EYFP and ECFP into the ROSA26 locus. BMC Dev. Biol. 1, 4 (2001).
Sasaki, Y. et al. Canonical NF-κB activity, dispensable for B cell development, replaces BAFF-receptor signals and promotes B cell proliferation upon activation. Immunity 24, 729–739 (2006).
Dalton, D. K. et al. Multiple defects of immune cell function in mice with disrupted interferon-γ genes. Science 259, 1739–1742 (1993).
Godfrey, V. L., Wilkinson, J. E., Rinchik, E. M. & Russell, L. B. Fatal lymphoreticular disease in the scurfy (sf) mouse requires T cells that mature in a sf thymic environment: potential model for thymic education. Proc. Natl Acad. Sci. USA 88, 5528–5532 (1991).
Egawa, T. et al. Requirement for CARMA1 in antigen receptor-induced NF-κB activation and lymphocyte proliferation. Curr. Biol. 13, 1252–1258 (2003).
Marangoni, F. et al. The transcription factor NFAT exhibits signal memory during serial T cell interactions with antigen-presenting cells. Immunity 38, 237–249 (2013).
Spiess, P. J., Yang, J. C. & Rosenberg, S. A. In vivo antitumor activity of tumor-infiltrating lymphocytes expanded in recombinant interleukin-2. J. Natl. Cancer Inst. 79, 1067–1075 (1987).
Marangoni, F. et al. Tumor tolerance-promoting function of regulatory T cells is optimized by CD28, but strictly dependent on calcineurin. J. Immunol. 200, 3647–3661 (2018).
Dobin, A. et al. STAR: ultrafast universal RNA-seq aligner. Bioinformatics 29, 15–21 (2013).
Li, B. & Dewey, C. N. RSEM: accurate transcript quantification from RNA-Seq data with or without a reference genome. BMC Bioinformatics 12, 323 (2011).
Ritchie, M. E. et al. limma powers differential expression analyses for RNA-sequencing and microarray studies. Nucleic Acids Res. 43, e47 (2015).
Acknowledgements
We thank the MGH Pathology Flow Cytometry Core and N. Ali-Akbar for technical assistance. This study was funded by an EMBO fellowship (ALTF534-2015) and a Marie Curie Global Fellowship (750973) (M.D.P.), DFG Fellowships (PR 1652/1-1 to J.N.P and US 116/2-1 to S.M.U), NIH T32 CA207021 (V.M.), a Sara Elizabeth O’Brien Fellowship (F.M.), and Melanoma Research Alliance Senior Investigator Award MRA-348693, NIH AI123349, and the Bob and Laura Reynolds MGH Research Scholar Award (T.R.M.).
Reviewer information
Nature thanks Shimon Sakaguchi and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
M.D.P. initiated, designed, performed and analysed the experiments, and wrote the manuscript. E.Y.K. initiated the project, designed and performed experiments, V.Z. performed histological analyses, S.M.U. performed autoantibody assays, V.M. and F.M. performed Treg cell analyses in lung and skin. F.M. performed in vitro Treg suppression assay. E.C. generated tumour cell lines. M.N.N. and A.-C.V. performed RNA sequencing analyses, B.D.M. provided genetic mouse models, D.S. designed and performed RT–qPCR assay, B.L.C., S.M., J.N.P., R.D.W. and M.L. performed tumour growth studies and survival studies, T.R.M. conceived the study, supervised the project, designed experiments, and wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
M.D.P. and T.R.M. have filed a patent application (PCT/US2018/067856) related to the use of MALT1 inhibitors. T.R.M. is a co-founder of Monopteros Therapeutics. All other authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 Lymphoproliferative disease after Treg-cell-specific deletion of CARMA1.
a, CARMA1 protein in Treg cells and CD4+ Tconv cells from LNs of Fcre × C1+/+, C1f/+ and C1f/f mice. b, Weight curves (n = 5 per group). c, d, Appearance of 21-day-old mice (c), and their spleens and LNs (d). e, Histological appearance of liver, skin and lung at 21 days of age of indicated mice. Scale bars, 150 μm and 50 μm (insets). f, Kidney, liver and stomach tissue sections of healthy C57BL/6 Rag1−/− mice were reacted with serum from 21-day-old mice of the indicated genotypes, and self-tissue-reactive IgG revealed by anti-mouse IgG staining (green). Nuclei were stained with DAPI (red). In b, *P < 0.05 versus C1+/+ and C1f/+ (two-way ANOVA with Bonferroni post hoc test).
Extended Data Fig. 2 Myeloid cell expansion and effector cytokine secretion by Tconv and Treg cells after Treg-cell-specific deletion of CARMA1.
a–c, Size of the CD11b+ splenic myeloid compartment and proportions of Ly6G+ neutrophils, CD11c+MHC IIhigh dendritic cells (DCs), Ly6Chigh monocytes, Lyc6GlowSSChigh eosinophils, and Ly6ClowSSClow macrophages in Fcre × C1+/+, C1f/+ or C1f/f mice. d, Expression of MHC-I, MHC-II and PD-L1 on splenic myeloid subsets. e, Frequency of CD4+ and CD8+ Tconv cells with a CD44highCD62L− effector memory phenotype in LNs of indicated mice at age 12 and 21 days. f, Effector cytokine expression of Tconv cells from 21-day-old mice after 8-h ex vivo stimulation on anti-CD3/CD28-coated plates. g, LN cellularity. h, Absolute numbers of Treg cells in LNs. i, Co-expression of indicated transcription factors by Treg cells from LNs of indicated mice. j, Expression of CD44 and CD62L by Fcre × C1f/f Treg cells expressing T-bet (green dots), GATA-3 (blue dots), or RORγt (red dots), compared to total C1f/f Treg cells (contour plots). *P < 0.05, **P < 0.01, ***P < 0.001, ***P < 0.0001 (one-way ANOVA with Tukey post hoc test).
Extended Data Fig. 3 Role of CARMA1 in eTreg cell differentiation.
a, Female heterozygous Fcre/+ × C1f/f mice express YFP–Cre and delete C1f/f in half of the Treg cells owing to X-chomosomal location of the Foxp3YFP-cre allele and random X chromosome inactivation, whereas the other half of the Treg cells remains functional. b, Frequency of CD4+ and CD8+ Tconv cells with a CD44highCD62L– effector memory phenotype in peripheral blood of ageing Fcre/+ × C1+/+, C1f/+ or C1f/f mice (n = 4 per group). c, Appearance of spleens and LNs of indicated mice at one year of age. d–f, Frequency and absolute numbers (e) of eTreg cells and expression of FOXP3, indicated markers of eTreg cell differentiation, as well as proliferation marker Ki67, pro-apoptotic protein BIM and anti-apoptotic protein BCL2 by YFP+ cTreg and eTreg cells (d, f) from nine-week-old Fcre/+ × C1+/+, C1f/+ or C1f/f mice. Note that some data on eTreg cells in e and f are also shown in Fig. 1g, h and shown here to facilitate the comparison to cTreg and YFP– Treg cells in g and h. g, h, Frequency and absolute numbers of eTreg cells (g) and eTreg cell markers on YFP– cTreg and eTreg cells (h) from the same mice as shown in d and f. *P < 0.05, **P < 0.01, ***P < 0.001, ***P < 0.0001 (one-way ANOVA with Tukey post hoc test).
Extended Data Fig. 4 In vitro and in vivo suppression, apoptotic rate and exTreg cell formation of CARMA1-deficient Treg cells.
a, CD4+CD45RBhighYFP– Tconv cells and CD4+CD45RBlowYFPbright Treg cells were double-sorted to more than 98% purity from LNs and spleens of Fcre × C1+/+ × ROSA26-stopf/f-YFP mice, which allow for clear differentiation of Cre-expressing Treg cells based on high expression of soluble enhanced yellow fluorescent protein (eYFP) in addition to the YFP–Cre fusion protein. b, YFPbright Treg from Fcre × C1+/+ or Fcre/+ × C1f/+ or C1 f/f mice and CellTrace Violet-labelled Tconv cells from Fcre × C1+/+ mice were co-cultured at indicated ratios for three days in the presence of anti-CD3 antibodies and T-cell-depleted splenocytes, and suppression measured as reduction of Tconv cell proliferation. c, Treg cells of various genotypes and Tconv cells were co-adoptively transferred into Rag-deficient hosts and their respective frequency in peripheral blood was determined eight weeks later. d, CD4+YFP+ Treg cells of indicated genotypes were cultured without exogenous IL-2 on anti-CD3/CD28-coated or uncoated plates for 6 or 18 h and examined for reactivity with annexin V and the viability dye ZombieRed. e, CD4+YFPbright cells were sorted from LNs of one-year-old and Fcre/+ × C1+/+ (or C1 f/+, C1 f/f) × ROSA26-stopf/f-YFP mice and subsequently stained for expression of FOXP3 protein to determine the frequency of FOXP3– exTreg cells. *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001 (two-way ANOVA with Sidak post hoc test in b, c; two-tailed Student’s t-test in d).
Extended Data Fig. 5 Bulk RNA sequencing analysis of YFP+ cTreg and eTreg cells from LNs of Fcre/+ × C1+/+, C1f/+ and C1f/f mice.
a, Scaled expression in cTreg cells (top) and eTreg cells (bottom) of genes differentially expressed (fold change > 2 and Padj < 0.05) between C1+/+ and C1f/f mice. b, High-resolution, fully annotated heat map of eTreg signature genes as shown in Fig. 1j.
Extended Data Fig. 6 Expression of apoptotic regulator genes.
a, Comparison of normalized, log-transformed mRNA expression levels of anti- and pro-apoptotic Bcl2 family genes in YFP+ cTreg and eTreg from Fcre/+ × C1+/+ mice, based on RNA sequencing analyses. b, Comparison of expression of the same genes in cTreg (top) and eTreg (bottom) cells of the indicated genotypes. *Padj < 0.05.
Extended Data Fig. 7 Restoring NF-κB activation in CARMA1-deficient Treg cells.
a, Survival of Fcre × C1+/+ (or C1f/f) × ROSA26-stopf/f-IKK2ca mice that express one allele of IKK2ca after expression of Foxp3cre. b–d, Frequency of CD4+ and CD8+ Tconv cells with a CD44highCD62L– effector memory phenotype in LNs (b), frequency of Treg among CD4+ T cells and of eTreg cells among total Treg cells in LNs (c), and effector cytokine expression of Tconv cells after 8-h ex vivo stimulation on anti-CD3/CD28-coated plates (d) in indicated mice. e, f, Expression of indicated phospho-proteins by YFP+ Treg cells from Fcre/+ × C1+/+ or × C1f/f mice at baseline and after 30 min. Anti-CD3/CD28 in vitro stimulation. Grey solid histograms show unstained control cells. Tconv cells were used as internal controls, and showed no differences (not shown). *P < 0.05, ***P < 0.001, ****P < 0.0001 (log-rank (Mantel–Cox) test in a; one-way ANOVA with Tukey post hoc test in b–d, f).
Extended Data Fig. 8 Role of IFNγ secretion by FOXP3int unstable Treg cells selectively in tumour tissue.
a–c, Frequencies of total YFP+ Treg cells and of YFP+ eTreg cells among CD4+ T cells (a), absolute YFP+ Treg and eTreg cell numbers (b), and normalized FOXP3 expression in YFP+ Treg and eTreg (c) in tdLN and tumour tissue of 18-day-old D4M.3A tumours in female heterozygous Fcre/+ × C1+/+, C1 f/+ or C1 f/f mice. d, tdLN and tumour cellularities. e, Growth of MC38 tumours in female heterozygous Fcre/+ × C1+/+ or C1 f/+ mice. f, g, Tumour-bearing mice were treated with brefeldin A for 5 h, injected intravenously with 3 μg of anti-THY1.2 monoclonal antibodies, and 3 min later collected for direct ex vivo analysis of IFNγ expression in extravascular YFP+ Treg cells in the lung (f) and skin (g). Gates for IFNγ+ cells drawn based on fluorescence-minus-one (FMO) controls. h, Normalized FOXP3 expression in IFNγ+ and IFNγ– Treg cells from tumour tissue. n.d., not detectable. i, Tumour growth in indicated mice implanted with D4M.3A melanoma and19 treated with or without neutralizing anti-IFNγ antibody. j, Frequency of adoptively transferred, YFP+ Treg cells of indicated genotypes in tdLNs of Ifng−/− hosts at day 18 of tumour growth. k–m, Frequency (k, l) and effector cytokine expression (m) of adoptively transferred, YFP+ Treg cells in tumours in Ifng−/− hosts. *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001 (one-way ANOVA with Tukey post hoc test in a–d, f, g; two-tailed Student’s t-test in e, h, j, l, m; two-way ANOVA with Bonferroni post hoc test in i).
Extended Data Fig. 9 Tumour response of CARMA1-deficient Treg cells after restoration of NF-κB activation.
a–d, D4M.3A melanoma cells were implanted into Fcre/+ × C1+/+ (or C1 f/f) × ROSA26-stopf/f-IKK2ca mice to record frequencies of YFP+ Treg and eTreg cells among CD4+ T cells (a) and their normalized FOXP3 expression (b) in tdLNs and tumour tissue, effector cytokine expression by tumour-infiltrating Treg cells (c), and tumour growth (d). e, YFP+ Treg cells were sorted from D4M.3A melanoma tissue and tdLNs after five days of treatment of FcreERT2 × C1+/+ and C1f/f with tamoxifen and analysed for CARMA1 expression by RT–qPCR. f, Tumour growth in female FcreERT2 or FcreERT2/+ × C1+/+ and C1 f/f mice, in which CARMA1 was deleted in all (FcreERT2) or half (FcreERT2/+) of Treg cells. Arrow indicates tamoxifen treatment start. g, In situ expression in tumour tissue of effector cytokines by YFP+ Treg five days after CARMA1 deletion in half or all Treg cells. h, MHC-II expression on tumour-associated macrophages in D4M.3A-implanted Fcre/+ × C1+/+, C1f/+ or C1f/f mice. i, D4M.3A tumour growth in mice treated with depleting anti-CD8 antibody from day 8 and treated with mepazine or vehicle from day 9. j, D4M.3A tumour growth in Fcre/+ × C1+/+ or C1f/f mice treated with mepazine or vehicle starting on day 9. Data are mean and individual replicates or s.e.m. In a–c, g–i, P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001. In d, *P < 0.05 versus C1+/+, &P < 0.05 versus C1+/+ + IKK2ca. In f, *P < 0.05 versus FcreERT2 × C1+/+, #P < 0.05 versus FcreERT2/+ × C1f/f. In j, *P < 0.05 versus C1+/+, #P < 0.05 versus C1+/+ + mepazine (one-way ANOVA with Tukey post hoc test in a–c, g, h; two-way ANOVA with Bonferroni post hoc test in d, f, j: two-tailed Student’s t-test in i).
Extended Data Fig. 10 Mepazine effects on the tumour microenvironment.
a, YFP+ Treg cells were sorted from Fcre × C1+/+ mice and treated with 10 μM mepazine or vehicle for 8 or 24 h with or without concurrent anti-CD3/28 monoclonal antibody TCR stimulation (8-h time point only). Expression of FOXP3, markers of eTreg cell differentiation, cell viability, and frequency of eTreg cells were recorded. b, c, RT–qPCR analysis of expression of Ifng and genes of adaptive immune resistance (the PD-L1 genes Cd274 and Socs1), antigen presentation (Tap1), IFNγ signalling (Stat1 and Irf1), T-cell recruitment (Cxcl10), M1 macrophage-activation (Nos2) (b) and of Foxp3 and various Treg-cell-associated genes (c) in whole tumour tissue lysate after three days of treatment with mepazine or vehicle control. d–h, Composition of the tumour tissue immune infiltrate and frequencies of CD45+ cells (e) and of various immune cell subsets (f) as well Ki67 expression by Tconv cells (g) and MHC-II expression by macrophages (h) after three days of treatment with mepazine or vehicle control. i, Effector cytokine co-expression by tumour-infiltrating Treg cells after 12 days of treatment with mepazine and anti-PD-1 antibody. j, Synergistic tumour control of MC38 colon carcinoma through anti-PD-1 and mepazine combination treatment in female C57BL/6 hosts. Numbers in parentheses indicate fraction of mice without relapse for more than 12 months after discontinuation of treatment. In j, *P < 0.05 versus vehicle, #P < 0.05 versus anti-PD-1, and &P < 0.05 versus mepazine. In all other panels, *P < 0.05, **P < 0.01, ***P < 0.001 (two-tailed Student’s t-test in a–c, e–h; one-way ANOVA with Tukey post hoc test in i; two-way ANOVA with Bonferroni post hoc test in j).
Supplementary information
Supplementary Information
This file contains Supplementary Materials and Methods: R scripts used in the analyses of RNA-sequencing data.
Supplementary Table
This file contains Supplementary Table 1: Sheets 1, 2: Differentially expressed genes (DEGs, defined by fold change > 2 and padj <0.05) in YFP+ cTreg (sheet 1) or YFP+ eTreg (sheet 2) from Foxp3Cre/+ x CARMA1flox/flow compared to Foxp3Cre x CARMA1+/+ mice. Sheet 3: Differences in eTreg signature genes between YFP+ eTreg from Foxp3Cre/+ x CARMA1flox/flox versus Foxp3Cre x CARMA1+/+ mice.
Rights and permissions
About this article
Cite this article
Di Pilato, M., Kim, E.Y., Cadilha, B.L. et al. Targeting the CBM complex causes Treg cells to prime tumours for immune checkpoint therapy. Nature 570, 112–116 (2019). https://doi.org/10.1038/s41586-019-1215-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-019-1215-2
- Springer Nature Limited
This article is cited by
-
Recent developments in immunotherapy for gastrointestinal tract cancers
Journal of Hematology & Oncology (2024)
-
Infiltrating treg reprogramming in the tumor immune microenvironment and its optimization for immunotherapy
Biomarker Research (2024)
-
Potential anti-tumor effects of regulatory T cells in the tumor microenvironment: a review
Journal of Translational Medicine (2024)
-
Therapeutic and immunomodulatory potentials of mesenchymal stromal/stem cells and immune checkpoints related molecules
Biomarker Research (2024)
-
Functional CRISPR screens in T cells reveal new opportunities for cancer immunotherapies
Molecular Cancer (2024)