Abstract
Lanifibranor, a pan-PPAR agonist, improves liver histology in patients with metabolic dysfunction-associated steatohepatitis (MASH), who have poor cardiometabolic health (CMH) and cardiovascular events as major mortality cause. NATIVE trial secondary and exploratory outcomes (ClinicalTrials.gov NCT03008070) were analyzed for the effect of lanifibranor on IR, lipid and glucose metabolism, systemic inflammation, blood pressure (BP), hepatic steatosis (imaging and histological grading) for all patients of the original analysis. With lanifibranor, triglycerides, HDL-C, apolipoproteins, insulin, HOMA-IR, HbA1c, fasting glucose (FG), hs-CRP, ferritin, diastolic BP and steatosis improved significantly, independent of diabetes status: most patients with prediabetes returned to normal FG levels. Significant adiponectin increases correlated with hepatic and CMH marker improvement; patients had an average weight gain of 2.5 kg, with 49% gaining ≥2.5% weight. Therapeutic benefits were similar regardless of weight change. Here, we show that effects of lanifibranor on liver histology in MASH are accompanied with CMH improvement, indicative of potential cardiovascular clinical benefits.
Similar content being viewed by others
Introduction
Metabolic-dysfunction associated steatotic liver disease (MASLD, also known as non-alcoholic fatty liver disease [NAFLD]), the accumulation of lipid-laden vacuoles in hepatocellular cytoplasm, is referred to as the hepatic manifestation of metabolic syndrome (MetS), a cluster of conditions encompassing insulin resistance (IR), dyslipidemia, altered glycemic control, (visceral) adiposity and arterial hypertension1. Metabolic-dysfunction associated steatohepatitis (MASH, also known as NASH), its progressive form, is characterized by histological steatohepatitis, i.e., lobular inflammation and hepatocyte injury2. MASLD global prevalence is 30% and increasing while MASH prevalence is estimated at 5.27%3. With no fully approved pharmacological therapy, MASH remains a major medical need and public health burden4,5.
The pathophysiology of MASH is a complex network of IR, dyslipidemia, altered carbohydrate metabolism, inflammation, hepatocellular injury and, subsequently, fibrogenesis2,6. Increased influx of fatty acids (FA) into hepatocytes from IR-related adipose tissue dysfunction represents a major upstream mechanism of steatohepatitis2,7. Hepatocellular mitochondrial dysfunction, i.e., compromised β-oxidation and electron transport chain activity, induce lipotoxicity by generating reactive lipid intermediaries such as diacylglycerol and ceramides, that reinforce IR and damage cellular structures including endoplasmic reticulum and mitochondria. Cellular injury and resulting inflammation, described as “disease activity”, drive fibrogenesis, a downstream phenomenon in the disease biology8,9.
Without management, liver fibrosis can progress to cirrhosis and ultimately end-stage liver disease10. The histological fibrosis stage, expressed categorically on a 0−4 scale, predicts liver-related mortality. Patients who progressed to cirrhosis, histological F4 per NASH Clinical Research Network (NASH-CRN) staging11, have significantly increased mortality from complications of decompensated cirrhosis, versus patients with pre-cirrhotic fibrosis12,13,14.
The long natural history of MASLD/MASH is typically accompanied by impaired cardiometabolic health (CMH) with increased risk for cardiovascular (CV) disease (CVD) and type-2 diabetes (T2D), including IR, atherogenic lipid profile, poor glycemic control, systemic inflammation and arterial hypertension15. A large body of evidence shows that patients with MASLD are at increased risk for subclinical CVD as well as for clinical CV events and death, to a considerable extent explained by the same underlying disease biology that drives MASLD progression16. Steatosis in itself adds to the CVD risk and is pathogenetically linked to atherosclerosis as a source of atherogenic lipids17,18,19. The risk increases further in patients with MASH and MASH with fibrosis compared to steatosis only20,21. Other mechanisms add to the link between MASH and atherosclerosis, including prothrombotic and inflammatory mediators and angiogenetic factors22.
CV events are the most frequent cause of mortality in MASH and begin to occur before advanced liver disease manifests17,23,24,25,26,27. Therefore, an investigational compound for MASH ideally shows efficacy on both hepatic and CV health and its effects on CMH markers may inform on its potential to improve CV outcomes.
Peroxisome proliferator-activated receptors (PPAR) are nuclear transcription factors regulating lipid and carbohydrate metabolism, inflammation and fibrosis in liver, adipose tissue, skeletal muscle, and other tissues through programmatic regulation of gene expression. PPARs exist in three isoforms, α, β/δ, and γ. PPARs have distinct yet overlapping tissue distribution and functions, including FA transport and mitochondrial β-oxidation; apolipoprotein (APO) production (mainly PPARα); immune and skeletal muscle homeostasis (mainly PPARβ/δ); insulin sensitivity (IS) in adipose tissue, liver and skeletal muscle; and inhibiting fibrogenesis (mainly PPARγ)2. PPAR transcription factors are thus master regulators of the spectrum of MASH disease biology, from IR and metabolic-immune pathways to fibrosis28.
Lanifibranor is a pan-PPAR agonist with balanced α, β/δ, and γ activity29. It has a distinct chemical structure from other PPAR agonists and a unique pattern of co-activator or -repressor recruitment upon ligand binding30. These characteristics comprehensively address MASH biology and make lanifibranor a promising investigational compound for this indication. Efficacy and safety of lanifibranor in patients with pre-cirrhotic MASH was demonstrated in the phase 2b study NATIVE. Results focused on hepatic endpoints, including both MASH resolution and fibrosis improvement, as well as safety, were recently published31. Here we show that lanifibranor improves CMH in patients with MASH.
Results
Baseline characteristics
Of 247 patients enrolled, 228 completed the study; mean age was 54 years, 58% were female, 94% were Caucasian, mean body mass index (BMI) was 33 kg/m2; 42% (n = 103) had T2D. Of these, 83% received metformin (alone or in combination anti-diabetic treatment), 22%, sulphonylurea; 11%, dipeptidyl peptidase-4 inhibitor; 7% sodium-glucose cotransporter-2 inhibitor medication; 13% had no antidiabetic treatment.
Among 144 patients without T2D, 47 (33%) had prediabetes. Overall, 20% of patients took statins (22%, 22%, 16% with lanifibranor 1200 mg, 800 mg, and placebo respectively). Baseline fasting low density lipoprotein cholesterol (LDL-C) levels were lower in patients on statins (mean close to 2.3 mmol/L) than without (3.0 mmol/L). The cardiometabolic profile and characteristic of MetS were similar in all treatment groups (Supplementary Table 2).
Insulin resistance and glycemic control
Fasting insulin levels (FIL) significantly decreased with lanifibranor in the overall population; adjusted mean difference versus placebo [AMD] at end of treatment [EOT] was −79 pmol/L (95% confidence interval [CI]: −112 to −47, p < 0.001) with lanifibranor 1200 mg; −83 pmol/L (95%CI: −115 to −51, p < 0.001) with 800 mg. In patients with T2D, AMD was −68 pmol/L (95%CI: −125 to −12, p = 0.018) with 1200 mg; −106 pmol/L (95%CI: −163 to −49, p < 0.001) with 800 mg; In non-T2D patients, AMD was −86 pmol/L (95%CI: −122 to −50, p < 0.001) with 1200 mg; −70 pmol/L (95%CI: −105 to −34, p < 0.001) with 800 mg. Similarly, lanifibranor significantly reduced homeostatic model assessment of IR (HOMA-IR) overall (AMD of −4.1 [95%CI: −5.8 to −2.4] with 1200 mg; −4.0 [95%CI: −5.7; −2.3] with 800 mg, both p < 0.001), with improvements in the T2D population (AMD of −4.5 [95%CI: −7.8 to −1.2], p = 0.008 with 1200 mg; −6.3 [95%CI: −9.7 to −2.8], p < 0.001 with 800 mg) and the non-T2D population (Table 1).
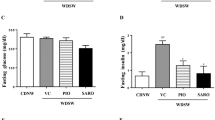
Fasting glucose (FG) levels significantly decreased with lanifibranor in the overall population (Fig. 1E). In T2D, the AMD at EOT was −1.2 mmol/L (95%CI: −1.9 to −0.5, p < 0.001) with 1200 mg and −1.7 mmol/L (95%CI: −2.4 to −1.0, p < 0.001) with 800 mg. Overall, AMD was −0.8 mmol/L (95%CI: −1.2 to −0.5, p < 0.001) with 1200 mg and −1.0 mmol/L (95%CI: −1.4 to −0.7, p < 0.001) with 800 mg. With T2D, AMD in hemoglobin A1c (HbA1c) at EOT was −0.7% (95%CI: −1.0 to −0.4, p < 0.001) in both active arms. Overall, HbA1c was −0.5% (95%CI: −0.6 to −0.3, p < 0.001) with both lanifibranor 1200 mg and 800 mg (Table 1, Fig. 1F).
A Triglycerides (n = 242 patients at W4, 231 at W14 and 217 at EOT), B HDL-C (n = 243 patients at W4, 232 at W14 and 218 at EOT), C LDL-C (n = 239 patients at W4, 227 at W14 and 213 at EOT), D APO-B (n = 208 patients), E fasting glucose (n = 242 patients at W4, 232 at W14 and 216 at EOT), F HbA1c (n = 243 patients at W4, 233 at W14 and 218 at EOT), G hs-CRP (n = 218 patients), H ferritin (n = 218 patients), I diastolic blood pressure (n = 243 patients at W4, 233 at W14 and 218 at EOT) and J NT-proBNP (n = 212 patients). Data are plotted as mean ± 95%CI. Treatment groups are indicated as follows: placebo, blue circle and solid line; lanifibranor 800 mg, red plus and dash line; lanifibranor 1200 mg, green cross and mixed line. *p < 0.01, **p < 0.001, from two-sided Mixed Model for Repeated Measures using change from baseline as endpoint, the time, treatment, the diabetic status, the interaction (treatment*time) and the baseline value as fixed effects, a time repeated measure within each subject and an unstructured variance covariance matrix. No adjustment for multiple comparisons was performed. Source data are provided as a Source Data file. APO apolipoprotein, CI confidence interval, EOT end of treatment, HbA1c hemoglobin A1c, HDL high density lipoprotein, hs-CRP high-sensitivity C-reactive protein, LDL low density lipoprotein, p = p value, NT-proBNP N-terminal pro b-type natriuretic peptide, W week.
Glycemic control in patients with prediabetes
With prediabetes, FG decreased at EOT to <5.6 mmol/L in 71% (95%CI: 48 to 95, p = 0.009) of patients on lanifibranor 1200 mg, 67% (95%CI: 45 to 88, p = 0.013) on 800 mg versus 11% (95%CI: 0 to 32) on placebo, indicating return to normoglycemia in the majority of lanifibranor-treated patients. At EOT, 86% (95%CI: 67 to 100, p = 0.05) of patients on lanifibranor 1200 mg and 78% (95%CI: 59 to 97, p = 0.08) on 800 mg returned to normal FIL (≤173 pmol/L) versus 37% (95%CI: 4 to 71) on placebo. HOMA-IR normalized (≤3) in 21% (95%CI: 0 to 43) and 23% (95%CI: 3 to 44) with lanifibranor 1200 mg and 800 mg, respectively, versus none on placebo (n = 8) (Supplementary Table 3).
Conversely, among 83 patients with normoglycemia at baseline, 0% with lanifibranor 1200 mg and 800 mg progressed to prediabetes at EOT, versus 26% (95%CI: 10 to 41, both p < 0.01) in the placebo arm (Supplementary Table 3).
Lipid metabolism
Fasting total serum triglycerides (TG) levels decreased significantly with lanifibranor compared to placebo, with an AMD at EOT of −0.5 mmol/L (95%CI: −0.8 to −0.3, equivalent to −44.3 mg/dL, p < 0.001) with both lanifibranor 1200 mg and 800 mg groups (Table 1). Among the 109 patients with high baseline TG values (>1.7 mmol/L, 150.5 mg/dL), 60% and 70% on lanifibranor 1200 mg and 800 mg, respectively, improved to low-risk TG levels of ≤1.7 mmol/L at EOT, versus 27% on placebo (Supplementary Fig. 1).
Fasting high density lipoprotein cholesterol (HDL-C) increased significantly at treatment week 4 (TW4), maintained until EOT: patients receiving lanifibranor 1200 mg and 800 mg had an AMD at EOT of 0.10 mmol/L (95%CI: 0.03 to 0.16, p = 0.003, equivalent to 3.9 mg/dL) and 0.16 mmol/L (95%CI: 0.09 to 0.22, p < 0.001, equivalent to 6.2 mg/dL), respectively (Table 1). TG and HDL-C changes with lanifibranor were consistent over time (Fig. 1A, B). No significant LDL-C change was observed with either lanifibranor dose versus placebo (Table 1, Fig. 1C).
Lanifibranor significantly reduced APO-B with an AMD at EOT of −10 mg/dL (95%CI: −15 to −4, p < 0.001) with both doses (Table 1, Fig. 1D), as well as the APO-B/APO-A1 ratio with an AMD at EOT of −0.06 (95%CI: −0.11 to −0.01, p = 0.013) with 1200 mg and −0.08 (95%CI: −0.13 to −0.03, p = 0.002) with 800 mg (Table 1). APO-A1 levels did not change significantly at EOT.
Systemic inflammation
Baseline high-sensitivity C-reactive protein (hs-CRP) levels were elevated in most patients: mean 5.4, 5.1 and 4.0 mg/dL in lanifibranor 1200 mg, 800 mg, and placebo arms, respectively (Supplementary Table 2). Values decreased at EOT in both lanifibranor arms but remained stable under placebo (Fig. 1G). With lanifibranor 1200 mg and 800 mg respectively, AMD at EOT was −1.5 mg/L (95%CI: −2.8 to −0.2, p = 0.026) and −2.2 mg/L (95%CI: −3.5 to −0.9, p = 0.001); (Table 1); 38% (95%CI: 22 to 53) and 44% (95%CI: 28 to 61) of patients at high CV risk improved to intermediate or low risk and 44% (95%CI: 25 to 63) and 35% (95%CI: 16 to 53) of those at intermediate risk improved to low risk, respectively (Supplementary Table 4). Only 26% (95%CI: 12 to 40) of patients on placebo at high risk improved to intermediate risk and 13% (95%CI: 0 to 27) improved from intermediate to low risk.
Mean baseline ferritin levels were comparably elevated: 237.5 (standard deviation [SD]: 238.2) µg/L, 230.9 (SD: 229.0) µg/L and 254.6 (SD: 233.3) µg/L with lanifibranor 800 mg, 1200 mg and placebo, respectively (Supplementary Table 2). At EOT, levels decreased significantly with lanifibranor (AMD at EOT: −84.2 µg/L [95%CI: −125.2 to –43.3], −71.8 µg/L [95%CI: −112.6 to −31.0] for lanifibranor 800 mg and 1200 mg, respectively, both p < 0.001), but were unchanged with placebo (Table 1, Fig. 1H).
Blood pressure (BP)
From TW4 and maintained during treatment, diastolic BP (DBP) decreased with both lanifibranor doses (AMD at EOT was −2.5 mmHg [95%CI: −5.5 to 0.6, p = 0.110] with lanifibranor 1200 mg and −3.9 mmHg [95%CI: −6.9 to −0.9, p = 0.012] with 800 mg, [Table 1, Fig. 1I]). Systolic BP did not change significantly.
Hepatic steatosis
Histological steatosis improved significantly at EOT with lanifibranor versus placebo, with more than 35% of patients improving by at least 2 grades with lanifibranor versus 5% with placebo (Fig. 2A). Controlled attenuation parameter (CAP™) similarly decreased significantly at EOT with lanifibranor (AMD at EOT was −23 dB/m [95%CI: −41 to −5, p = 0.012] with 1200 mg and −16 dB/m [95%CI: −33 to 1, p = 0.070] with 800 mg [Table 1]) but not with placebo (Fig. 2C). Baseline CAP™ category distribution was comparable between treatment groups; at EOT, a significantly higher proportion of patients had CAP™ ≤302 dB/m, corresponding to S ≤ S1, with lanifibranor 1200 mg (50%, 95%CI: 36 to 64, p = 0.009) and 800 mg (46%, 95%CI: 33 to 60, p = 0.019) versus placebo (25%, 95%CI: 13 to 37) (Fig. 2D). There was a significant relationship (Spearman coefficient [Rs]: 0.37, p < 0.001) between CAP™ and histological steatosis grade at screening and EOT (Fig. 2B). CAP™ steatosis decrease correlated with TG and HbA1c lowering at EOT (Supplementary Fig. 2C, D).
A CRN-S improvement, defined as at least one-point improvement of CRN-S at EOT compared to screening (n = 207 patients). Point-improvement groups are indicated as follows: 1 point, blue; 2 points, red; 3 points, green. p-values from two-sided Cochran-Mantel-Haenszel test, stratified on the diabetic status at Baseline. B Correlation between CAP™ and CRN-S (n = 294 pooled pre- and post-treatment biopsies). The box’s length represents the IQR, the diamond inside the box represents the mean, the horizontal line inside the box represents the median, the whiskers extend to the minimum and maximum values included in [Q1-1.5*IQR; Q3 + 1.5IQR], the circles outside the whiskers represent the outliers. P value from two-sided Spearman correlation test. C CAP™ at screening and EOT, by treatment group (n = 153 patients). Data are plotted as mean ± 95%CI. Treatment groups are indicated as follows: placebo, blue circle and solid line; lanifibranor 800 mg, red plus and dash line; lanifibranor 1200 mg, green cross and mixed line. *p < 0.05, from two-sided Wilcoxon-Mann-Whitney test. D CAP™ ≤302a dB/m at screening and EOT (n = 153 patients). P values from two-sided Chi² test a Youden optimal cutoff of the CAP™ as a diagnosis marker of steatosis ≥S1 versus S0. No adjustment for multiple comparisons was performed. Source data are provided as a Source Data file. CAP™ controlled attenuation parameter, CI confidence interval, Coef. coefficient, CRN Clinical Research Network, EOT end of treatment, IQR interquartile range.
Weight change in relation to CMH and hepatic markers
Mean absolute (resp. relative) weight increase at EOT was 2.7 (3.1%) and 2.4 (2.6%) kg for lanifibranor 1200 mg and 800 mg, respectively. Weight change showed considerable interindividual variability: at EOT, 51% of patients in pooled lanifibranor arms had stable weight (≤2.5% increase), 16% had moderate increase (2.5−5%), and 33% had ≥5% increase from baseline; with placebo 84% had stable weight, but 16% had >2.5% weight increase (Supplementary Fig. 3). In pooled lanifibranor arms, all CMH markers, i.e., steatosis, HOMA-IR, FIL, lipids (HDL-C, TG, APO-B, APO-C3, APO-B/APO-A), FG, hs-CRP, ferritin and DBP, as well as liver tests (ALT, AST, gamma-glutamyl transferase [GGT]), improved to the same degree in the three weight-change groups. In contrast, placebo-treated patients with increased weight at EOT had unchanged or worsening values of these markers. (Supplementary Table 5, Fig. 3A, B, C, E, F). N-terminal pro b-type natriuretic peptide (NT-proBNP) increased with both lanifibranor doses; AMD at EOT was 8.4 pmol/L (71 pg/mL) with lanifibranor 1200 mg and 4.0 pmol/L (34 pg/mL) with 800 mg (Table 1, Fig. 1J), this increase being correlated with weight increase (Supplementary Table 4, Fig. 3G).
A HOMA-IR (n = 169 patients), B ferritin (n = 217 patients), C ALT (n = 217 patients at W4 and W14, 216 at EOT), D adiponectin (n = 217 patients), E CAP™ (n = 142 patients), F diastolic blood pressure (n = 217 patients at W4, W14 and EOT) and G NT-pro-BNP (n = 210 patients). Data are plotted as mean ± 95%CI. Weight-change groups are indicated as follows: stable (≤2.5%), blue circle and solid line; moderate (within 2.5% and 5%), red plus and dash line; increase (≥5%), green cross and mixed line for lanifibranor-treated patients, and stable (≤2.5%), blue circle and solid line; increase (>2.5%), red plus and dash line for placebo-treated patients. Only two weight relative change groups defined for placebo due to few patients ≥5% (n = 4). For HOMA-IR related figures, patients treated with sulphonylureas were removed from the analyses. Source data are provided as a Source Data file. ALT alanine aminotransferase, BL Baseline, CAP™ controlled attenuation parameter, CI confidence interval, EOT end of treatment, HOMA-IR homeostatic model assessment of insulin resistance, NT-proBNP N-terminal pro b-type natriuretic peptide, W week.
Adiponectin, a cardiometabolic and hepatic efficacy marker
Mean baseline adiponectin levels were low at 5.1 μg/mL with high variation (range 0.8−30.8 μg/mL); 60% of patients had low, 32% medium and 8% high values (Supplementary Table 6). Higher increase of adiponectin levels was observed in the lanifibranor 1200 mg (mean fold 4.5) compared to lanifibranor 800 mg (3.8) at EOT, 86% of patients on lanifibranor 800 mg had moderate (58%) or high (29%) increase and 95% of those on 1200 mg had moderate (52%) or high (42%) increase. With placebo only 10% had moderate, and none high increase (Supplementary Table 6). In the pooled lanifibranor arms, adiponectin increased in all three weight-change groups, with a higher increase in the “>2.5% weight increase” groups, versus the “≤2.5% weight stable” group (Fig. 3D).
Adiponectin increase at EOT correlated with improvement in IR (FIL, HOMA-IR), glycemic control (FG, Hb1Ac), lipid metabolism (TG and APO-B decrease, HDL-C increase), hs-CRP, aminotransferases, steatosis markers (GGT, CAP™), with a larger effect size for high than for moderate increase (Supplementary Table 7, Fig. 4A–E). Mean CAP™ values improved from 317 at baseline to 280 dB/m at EOT in patients with >4-fold adiponectin increase, 73% of them to values < 302 dB/m (corresponding to steatosis grade ≤1) (Fig. 4E).
Absolute changes in levels of A HDL-C, B HbA1c, D ALT, (n = 139 patients at W4, W14, EOT) and levels of C AST (n = 139 patients at baseline, W4, W14, EOT), E CAPTM (n = 90 patients at screening and EOT). Data are plotted as mean ± 95%CI. Adiponectin increase groups are indicated as follows: unchanged (<1.5-fold), blue circle and solid line; moderate (within 1.5- and 4-fold), red plus and dash line; high (>4-fold), green cross and mixed line. Source data are provided as a Source Data file. AST aspartate aminotransferase, ALT alanine aminotransferase, CAP™ controlled attenuation parameter, CI confidence interval, EOT end of treatment, HbA1c hemoglobin A1c, HDL high density lipoprotein.
Absolute and categorical (fold change) adiponectin increase also correlated with improvement of liver histological endpoints for disease activity, i.e., CRN-NAFLD activity score (NAS) and individual activity components (ballooning and inflammation), and with improvement in fibrosis stage (38% versus 57% for adiponectin increase ≤4- versus >4-fold, respectively) (Supplementary Table 8, Fig. 5A−D).
A CRN-NAS score, B CRN-I, C CRN-B and D CRN-F (n = 128 patients). Histological improvement is indicated as follows: improvement of at least one point at EOT compared to screening according to NASH-CRN grading and staging, red; and no improvement otherwise; blue. Adiponectin increase groups are defined as unchanged (<1.5-fold), moderate (within 1.5- and 4-fold) and high (>4-fold). Source data are provided as a Source Data file. B ballooning, CRN Clinical Research Network, EOT end of treatment, F fibrosis, I inflammation, NAS NAFLD activity score.
Correlation between improvement of IR and hepatic markers
Baseline HbA1c levels correlated with baseline histological MASH activity and fibrosis (Spearman Rs: 0.15, p = 0.017, and 0.15, p = 0.021, respectively) (Supplementary Fig. 4). HbA1c improvement correlated with histological response in the lanifibranor arms: HbA1c decrease was larger in histological steatosis “improvers” (−0.46%) versus “non-improvers” (−0.20%, p = 0.048); and ballooning “improvers” (−0.45%) versus “non-improvers” (−0.33%, p = 0.088) (Supplementary Fig. 5). Similarly, HOMA-IR decrease correlated with improvement of liver tests and normal HOMA-IR at EOT was associated with histological improvement (Supplementary Tables 9, 10).
Under lanifibranor, HbA1c decrease also correlated with improvement of FG (Spearman Rs:0.55, p < 0.001), FIL (Rs: 0.36, p < 0.001), HOMA-IR (Rs: 0.51, p < 0.001), ALT (Rs: 0.35, p < 0.001), AST (Rs: 0.28, p < 0.001), GGT (Rs: 0.33, p < 0.001), CAP™ (Rs: 0.17, p = 0.092), HDL-C (Rs: −0.21, p = 0.011), TG (Rs: 0.27, p < 0.001), APO-B (Rs: 0.23, p = 0.008) and APO-B/APO-A1 (Rs: 0.26, p = 0.002) (Supplementary Table 11).
Correlation between steatosis improvement and CMH markers
Baseline CAP™ steatosis ≤302 and >302 dB/m correlated with HOMA‑IR (7.8 and 11.9, p = 0.003), HbA1c (5.7 and 6.2%, p < 0.001), TG (1.72 and 2.04 mmol/L, p = 0.012), DBP, and inversely with HDL‑C (1.30 and 1.18 mmol/L, p = 0.007) and APO‑A1 (151 and 142 mg/dL, p = 0.027), respectively; adiponectin did not differ with steatosis severity (Supplementary Table 12). Improvement of HOMA‑IR with lanifibranor therapy was independent of steatosis reduction; HbA1c improvement was correlated with improvement of both histological steatosis grade and CAP™ change; TG decrease correlated with change in CAP™ categorized as increase (≥+10%), no change (−10%; +10%) and decrease (< −10%); HDL‑C increase also correlated with histological steatosis improvement. Adiponectin levels increased 3.1-, 3.9-, 5.3- and 6.0-fold for no change, 1-, 2- and 3-points reductions of steatosis grade (Spearman Rs: −0.40, p < 0.001) (Supplementary Fig. 2A−F).
Cardiometabolic health markers in obese and non-obese patients
Of 247 patients enrolled, 161 (65%) patients were obese (BMI ≥ 30) and 86 (35%) patients had a BMI < 30 at baseline (Supplementary Table 1). Overall, the effects of lanifibranor therapy versus placebo on markers of CMH and on liver tests were similar for obese and non-obese patients (Supplementary Table 13).
Discussion
Patients enrolled in the NATIVE trial had, as expected, poor CMH with increased CV risk, namely IR, atherogenic lipid profile, poor glycemic control, systemic inflammation, elevated BP and hepatic steatosis. The data presented here demonstrate that lanifibranor therapy broadly and significantly improves metabolic-immune markers that are associated with the risk for CVD and T2D in patients with MASH, with similar effect sizes for both doses studied.
Elevated TG at baseline corresponded to different degrees of CV risk; after 4 weeks and throughout the treatment period, most patients on lanifibranor reverted to “low-risk range” levels. Similarly, APO-B, APO-C3 and APO-B/APO-A1 were significantly lowered at EOT, and HDL-C increased from week 4 throughout treatment. Improving proatherogenic lipid levels, including TG and APO-B, may reduce CV events32, and the recognition of APO-C3 as an independent risk factor for atherosclerosis has led to renewed interest in APO-C3 as therapeutic target. The potential aggregate clinical effect from several lipid risk factors moving in the right direction warrants further evaluation of lanifibranor therapy for CV outcomes.
The risk for CVD is further determined by IR, glycemia control, systemic inflammation, BP and steatosis, risk factors that all respond to lanifibranor therapy. Hs-CRP levels decreased significantly with both lanifibranor doses, whereas a mean increase was seen with placebo. Hs-CRP, an acute phase protein produced by hepatocytes, macrophages and vascular smooth muscle cells, is a marker of systemic inflammation associated with formation and rupture of atherosclerotic plaques, promotion of occlusive thrombi, damage of vascular endothelial integrity, activation of the renin-angiotensin system and vascular remodeling33. CRP is an important predictor of adverse coronary events independent of dyslipidemia34,35,36. About 50% of patients had high-risk hs-CRP levels (>3 mg/dL); although mean baseline values were higher in the active arms than in the placebo arm, a significantly larger percentage of patients reached hs-CRP levels of a lower risk category with lanifibranor than with placebo. Similarly, elevated ferritin levels are related to inflammation, IR and CVD parallel to the effects of hs-CRP in MetS37. Both lanifibranor doses significantly reduce ferritin levels.
Poor glycemic control is also associated with severity of MASH; higher HbA1c values correlate with higher degrees of histological steatosis, ballooning hepatocytes and fibrosis38,39,40, a correlation that was also observed in NATIVE. With lanifibranor, HbA1c decrease at EOT correlated with improvement of metabolic and hepatic (IR, TG, HDL-C, APOs, steatosis, aminotransferases) markers. Among patients without overt T2D, a substantial proportion had prediabetes, which is associated with increased risk for atherosclerotic CVD and later T2D development41. Although professional guidelines advocate early management to return FG levels to normal values, effectively preventing T2D development, prediabetes remains underrecognized42. Lanifibranor therapy brought FG within the normal range in the majority of patients with prediabetes, thereby reducing the risk for progressive metabolic disease.
Lanifibranor also significantly reduced steatosis, with half of the patients reaching CAP™ values below the threshold for histological grade S143, an effect that correlated with lowering of TG and HbA1c.
Weight gain observed with PPAR agonist therapy is well defined as metabolically distinct from life-style-related (poor diet and/or lack of physical activity) weight gain. PPARγ activation reduces visceral and hepatic fat, while inducing maturation of insulin sensitive subcutaneous fat, as demonstrated with pioglitazone, a PPARγ agonist approved for T2D; in contrast, weight gain from diet failure increased visceral and hepatic fat44,45. PPARγ activity thereby induces redistribution from metabolically unhealthy, insulin-resistant abdominal fat to insulin-sensitive, subcutaneous adipose tissue associated with improved metabolic health46,47,48. Lanifibranor data are in alignment with these observations. About half of the patients had weight gain ≥2.5% during lanifibranor therapy, with mean increase of 2.4 and 2.7 kg for low and high dose, respectively. Steatosis, IS and the panel of CMH markers improved in patients on lanifibranor whether or not they had a change in weight, and independent of the degree of weight change. Patients on placebo who gained weight showed either no effect or worsening of CMH markers.
While PPARγ-associated weight gain is thus indicative of maturation of adipose tissue, some contributing effect on fluid retention is suggested by the treatment effect on NT-proBNP. Past pure PPARγ agonists such as the thiazolidinediones pioglitazone and rosiglitazone are effective for glycemic control and improving IR, but also have been associated with an increased risk of edema and heart failure49. There was no clinical evidence for congestion in patients on lanifibranor in NATIVE.
The efficacy of lanifibranor on CMH markers parallels a robust increase in adiponectin levels. Adiponectin is a pleiotropic adipokine and PPARγ downstream mediator, while PPARα activity may affect adiponectin signaling through receptor upregulation50. Adiponectin improves IR, lipid metabolism, inflammation and fibrosis; it induces maturation of insulin-sensitive, mostly subcutaneous adipose tissue resulting in less toxic lipid intermediaries51,52. Low adiponectin levels are indicative of adipose tissue dysfunction53, are associated with CVD and have also been reported in MASH44,54,55, which illustrates the role of adipose tissue dysfunction in both MASH and CVD biology. Baseline levels were indeed low in the patient population of NATIVE. Lanifibranor treatment significantly increased adiponectin levels in >90% of patients, which is expected to lead to maturation of insulin-sensitive adipose tissue, and related weight change53,56,57. The degree of adiponectin increase indeed correlated with weight change, as well as with improvement of CMH markers, including IR, lipids, hs-CRP and hepatic steatosis. No adiponectin increase was seen with placebo, rather a small decrease in patients who gained weight on placebo, further pointing to the beneficial role of adiponectin in the opposite metabolic effects correlated with weight change in lanifibranor versus placebo arms. This is supported by the observation that steatosis decreased most in patients with the highest, >4-fold increase of adiponectin levels. The data support a link between adiponectin increase with lanifibranor and a shift toward a metabolically healthier, insulin-sensitive profile.
MASLD and CVD are pathogenetically linked and not just comorbidities resulting from shared risk factors58. The association between MASLD and atherosclerosis is stronger than can be explained by common risk factors alone59. With CVD being the main cause of mortality, the risk for non-fatal CV events is even stronger in MASLD compared to controls, with a hazard ratio of 3.7160. Steatosis by itself increases the risk of atherogenic dyslipidemia and is correlated with the severity of coronary heart disease61. In one cohort study, an association between MASLD severity on ultrasound and carotid atherosclerosis as well as between MASLD regression during follow-up and reduced risk for subclinical carotid atherosclerosis was found62. Progression to steatohepatitis increases the risk for CVD further63. The pathogenetic link between MASLD and CVD results from production and secretion of toxic lipid intermediates and atherogenic lipids in e.g., very low-density lipoproteins by the liver, and from systemic inflammation that accompanies progressive MASH64.
The broad therapeutic effect of lanifibranor in patients with MASH can in the first instance be explained through its balanced pan-PPAR agonist activity. PPAR isoforms α, β/δ and γ have distinct and overlapping ligand binding, tissue expression pattern and biological effects2. Given their crucial biological roles in metabolic-immune diseases, PPARs have been targets of high interest for pharmacological drug development28. Among other effects, PPARα agonists reduce TG levels by increasing mitochondrial FA β-oxidation; PPARβ/δ ligands increase HDL-C levels, have anti-inflammatory effects and improve glucose utilization of skeletal muscle, while PPARγ activity exerts antifibrotic effects on activated hepatic stellate cells and improves IS in liver, adipose tissue and skeletal muscle. Together, the PPAR isoforms regulate pathways that encompasses the entire disease biology of MASLD/MASH. This provides the rationale for a PPAR agonist that, in contrast to selective PPAR agonists such as fibrates (PPARα) and thiazolidinediones (PPARγ), has balanced activity on all PPAR isoforms and is thus expected to have direct therapeutic effects on all major nodes of MASH disease biology, from upstream IR, dysregulated lipid and glucose metabolism, inflammation to hepatic fibrogenesis, and thereby to have therapeutic potential for both hepatic and cardiometabolic manifestations of MASH. The clinical metabolic-immune improvements with lanifibranor indeed substantiate the pan-PPAR activating mechanism across all three subtypes, exemplified by the effects on TG, HDL-C and IR reflecting mainly PPARα, β/δ and γ mediated mechanisms, respectively2.
Given the pathway interconnectedness of MASLD and CVD, improvement in hepatic health may have an effect on CMH and vice versa, in addition to direct pan-PPAR mediated pharmacological effects. Although this remains speculative and warrants further research, bidirectional interactions between course and severity of T2D and MASH are well documented65. The correlation analyses between improvement of CMH markers such as IR and hs-CRP and markers of hepatic health including steatosis, and histological MASH activity observed in this study point toward multidirectional interactions in disease biology that may add to the benefits of pan-PPAR agonist therapy.
The study has strengths and limitations. Strengths include the randomized double-blind design and the well-characterized, per protocol collected data with two active doses versus placebo in a study of sufficient sample size to show changes in biomarkers and clinical measurements across the different dimensions of CMH. The therapeutic effect sizes are similar for both doses, while the higher dose has a superior effect size on histological liver fibrosis; it will thus be of interest to evaluate the effects on liver histology of both doses after a longer treatment period. Limitations may include the fact that patients who meet study entry criteria may not represent all patients seen in varying practice environments; analyses were post-hoc of available data; other potential biomarkers such as NT-proBNP, proteomics, and hepatokines that affect the intricate network of interactions between the steatotic liver and other endocrine organs may be informative in future studies66. Lastly, a longer duration of therapy would be required to relate the effects on CMH markers to potential outcome effects; thus, this study represents a lead-in for combined investigations of hepatic and CV health in MASH.
In conclusion, MASH is part of a systemic metabolic-immune disorder with complex multidirectional interactions between affected tissues. Both progressive liver disease and CVD develop in this context and need to be addressed by pharmacological treatment claiming efficacy. The pan-PPAR agonist lanifibranor significantly improves CMH in correlation with improvements in liver health and indicators of improved adipose tissue function; the improvement in cardiometabolic and hepatic markers was independent of changes in weight, and was correlated with a response of adiponectin, a mediator of improved IS. The NATIVE data demonstrate that lanifibranor is a promising investigational therapy that addresses the broad disease biology of MASH and related CVD, corresponding to its pan-PPAR agonist mechanism of action. Future studies of longer duration are warranted to investigate the effects of lanifibranor on CV outcomes.
Methods
Trial oversight
This clinical trial has been registered at ClinicalTrials.gov, number NCT03008070 (first posted January 2, 2017). This study and all amendments have been approved by independent ethics committees and the appropriate authorities (Supplementary Table 1) in 16 countries (France, United States of America, Australia, Belgium, Bulgaria, Germany, Canada, Italy, Spain, Poland, the United Kingdom, Czech Republic, Switzerland, Slovenia, Austria and Mauritius), where at least one patient underwent randomization. The trial was conducted in accordance with the principles of the Declaration of Helsinki, the International Council for Harmonisation Good Clinical Practice guidelines, and all relevant regulations. Prior to the trial entry, written informed consent was obtained from all participants.
Study population
The NATIVE trial was conducted from 07-Feb-2017 (first patient first visit) to 16-Mar-2020 (last patient last visit), and enrolled 247 patients ≥18 years old with MASH confirmed by a centrally read biopsy performed at screening or in the preceding six months and a histological Steatosis Activity Fibrosis (SAF) score for disease activity (inflammation and ‘ballooning’) ≥367. Patients with cirrhosis, HbA1c > 8.5% (69 mmol/mol), recent change in anti-diabetic medication, type-1 diabetes or T2D on insulin therapy and other causes of chronic liver disease, including significant daily alcohol consumption, were excluded31. A total of 247 patients were randomized 1:1:1 to receive lanifibranor 1200 mg, 800 mg, or placebo, once daily for 24 weeks.
Cardiometabolic assessments
CMH markers assessed included: (a) IR (FIL, HOMA-IR), (b) lipid profile (TG, HDL-C, LDL-C, APO-A1, B and C3, and APO-B/APO-A1 ratio); (c) glycemic control (FG, HbA1c); (d) systemic inflammation (hs-CRP) and ferritin; (e) blood pressure; (f) body weight, and (g) adiponectin levels. NT-proBNP was also measured. All analyses were performed at the BARC Global Central Laboratory, in Ghent, Belgium. Histological grading of steatosis was evaluated according to the SAF and NASH CRN scoring systems. Steatosis was also assessed with ultrasound-based imaging (CAP™ on the FibroScan® device) using Youden cutoff values for S ≥ S1, S ≥ S2, and S ≥ S3 of 302 dB/m, 331 dB/m, and 337 dB/m, respectively43. All analyses were done according to the IRB-approved study documents.
Statistical analyses
This manuscript reports the results of several secondary objectives of the NATIVE trial, that were prespecified in the protocol and the Statistical Analysis Plan (SAP), including the effect of lanifibranor 1200 mg/day and 800 mg/day versus placebo on CMH markers, evaluated after 24 weeks of treatment (EOT) compared to baseline, and for some markers also at TW4. Further post-hoc analyses, i.e., not pre-specified in the SAP, included: the effects of therapy in the subgroups of patients with and without overt T2D; in patients with prediabetes at baseline, (defined as FG level between 5.6 and 6.9 mmol/L [100 to 125 mg/dL])68; the effects of therapy on hs-CRP categorized as high CV risk (>3 mg/L), intermediate (1−3 mg/L) or low risk (<1 mg/L)69; the effects of therapy on NT-proBNP, the correlation between weight changes (both continuous and by weight-change group, i.e., <2.5%, 2.5−5% and ≥5% increase from baseline) under lanifibranor and placebo, separately, and improvement in CMH markers (lipid and glucose metabolism, IR, inflammation, liver tests, DBP, hepatic steatosis grading and CAP™ imaging); the correlation between baseline levels of adiponectin (categorized as low, medium and high, defined as <5, 5−10 and >10 μg/mL, respectively, as previously described70) and disease severity; the correlation between changes in adiponectin levels both continuous or by category (unchanged, moderate or high defined as <1.5-fold, 1.5 to 4-fold and >4-fold change, respectively) during treatment and improvement in CMH markers; the correlation between HbA1c levels (continuous and by level of glycemic control: ≤6% [42 mmol/mol]; >6%- ≤ 7%; >7% [53 mmol/mol]) during treatment and histological MASH activity and fibrosis stage at baseline.
Descriptive statistics were presented using the mean and SD, median, interquartile ranges and minimum-maximum for continuous variables, and frequency counts and percentages for categorical variables. For statistical tests, the type-I error risk was set at 5% (2-sided) as per protocol. No multiplicity adjustments were performed for the analyses presented in this paper, that are considered exploratory. Point estimates, 95%CIs and p-values are provided. The CIs have not been adjusted for multiple comparisons. Comparisons of continuous parameters between treatment groups at EOT were done using Mixed Model for Repeated Measures (MMRM), using the change from baseline as endpoint, the time (Weeks 4, 14 and 24), treatment, the diabetic status, the interaction (treatment*time) and the baseline value as fixed effects, a time repeated measure within each subject and an unstructured variance covariance matrix, or using Student or Wilcoxon tests depending on tests of normality. Comparison of categorical parameters between groups was done using Cochran-Mantel-Haenszel test stratified on the diabetic status at baseline, or from Chi² or Fisher tests. The correlation between continuous parameters was estimated using Spearman correlation (Rs and p value). SAS® software version 9.4 was used to perform all analyses.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
All of the data necessary to reproduce the findings described here can be found in the manuscript, figures, supplementary information and the source data file, or from the corresponding author on request. Proposals should be directed to Michael.Cooreman@inventivapharma.com. All requests for data will be reviewed by the corresponding author who will make sure that they are available and consistent with participant privacy and informed consent. A response will be provided within three months. Data requestors will need to sign a data access agreement. The data will be available from six months after publication of the manuscript for a duration of a minimum of five years. Source data are provided with this paper and its supplementary information files. Source data are provided with this paper.
Code availability
The SAS® codes that support the findings of this study are available from the corresponding author upon request. The basic SAS® codes used to edit the statistical results are provided in the supplementary information file.
References
Godoy-Matos, A. F., Silva Junior, W. S. & Valerio, C. M. NAFLD as a continuum: from obesity to metabolic syndrome and diabetes. Diabetol. Metab. Syndr. 12, 60 (2020).
Francque, S. et al. Nonalcoholic steatohepatitis: the role of peroxisome proliferator-activated receptors. Nat. Rev. Gastroenterol. Hepatol. 18, 24–39 (2021).
Younossi, Z. M. et al. The global epidemiology of nonalcoholic fatty liver disease (NAFLD) and nonalcoholic steatohepatitis (NASH): a systematic review. Hepatology 77, 1335–1347 (2023).
Lazarus, J. V. et al. Advancing the global public health agenda for NAFLD: a consensus statement. Nat. Rev. Gastroenterol. Hepatol. 19, 60–78 (2022).
Allen, A. M., Lazarus, J. V. & Younossi, Z. M. Healthcare and socioeconomic costs of NAFLD: a global framework to navigate the uncertainties. J. Hepatol. 79, 209–217 (2023).
Haas, J. T., Francque, S. & Staels, B. Pathophysiology and mechanisms of nonalcoholic fatty liver disease. Annu. Rev. Physiol. 78, 181–205 (2016).
Koliaki, C. et al. Adaptation of hepatic mitochondrial function in humans with non-alcoholic fatty liver is lost in steatohepatitis. Cell Metab. 21, 739–746 (2015).
Schwabe, R. F., Tabas, I. & Pajvani, U. B. Mechanisms of fibrosis development in nonalcoholic steatohepatitis. Gastroenterology 158, 1913–1928 (2020).
Antar, S. A., Ashour, N. A., Marawan, M. E. & Al-Karmalawy, A. A. Fibrosis: types, effects, markers, mechanisms for disease progression, and its relation with oxidative stress, immunity, and inflammation. Int. J. Mol. Sci. 24, 4004 (2023).
Angulo, P., Machado, M. V. & Diehl, A. M. Fibrosis in nonalcoholic Fatty liver disease: mechanisms and clinical implications. Semin Liver Dis. 35, 132–145 (2015).
Kleiner, D. E. et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology 41, 1313–1321 (2005).
Ekstedt, M. et al. Fibrosis stage is the strongest predictor for disease-specific mortality in NAFLD after up to 33 years of follow-up. Hepatology 61, 1547–1554 (2015).
Hagstrom, H. et al. Fibrosis stage but not NASH predicts mortality and time to development of severe liver disease in biopsy-proven NAFLD. J. Hepatol. 67, 1265–1273 (2017).
Taylor, R. S. et al. Association between fibrosis stage and outcomes of patients with nonalcoholic fatty liver disease: a systematic review and meta-analysis. Gastroenterology 158, 1611–1625.e1612 (2020).
Anstee, Q. M., Targher, G. & Day, C. P. Progression of NAFLD to diabetes mellitus, cardiovascular disease or cirrhosis. Nat. Rev. Gastroenterol. Hepatol. 10, 330–344 (2013).
Mantovani, A. et al. Complications, morbidity and mortality of nonalcoholic fatty liver disease. Metabolism 111S, 154170 (2020).
Targher, G., Byrne, C. D., Lonardo, A., Zoppini, G. & Barbui, C. Non-alcoholic fatty liver disease and risk of incident cardiovascular disease: a meta-analysis. J. Hepatol. 65, 589–600 (2016).
Salah, H. M. et al. Meta-analysis of nonalcoholic fatty liver disease and incident heart failure. Am. J. Cardiol. 171, 180–181 (2022).
Jin, R. et al. Amount of hepatic fat predicts cardiovascular risk independent of insulin resistance among Hispanic-American adolescents. Lipids Health Dis. 14, 39 (2015).
Kasper, P. et al. NAFLD and cardiovascular diseases: a clinical review. Clin. Res. Cardiol. 110, 921–937 (2021).
Baratta, F. et al. Nonalcoholic fatty liver disease and fibrosis associated with increased risk of cardiovascular events in a prospective study. Clin. Gastroenterol. Hepatol. 18, 2324–2331.e2324 (2020).
Malladi, N., Alam, M. J., Maulik, S. K. & Banerjee, S. K. The role of platelets in non-alcoholic fatty liver disease: from pathophysiology to therapeutics. Prostaglandins Other Lipid Mediat. 169, 106766 (2023).
Mann, J. P. et al. Hospital admission with non-alcoholic fatty liver disease is associated with increased all-cause mortality independent of cardiovascular risk factors. PLoS One 15, e0241357 (2020).
Dulai, P. S. et al. Increased risk of mortality by fibrosis stage in nonalcoholic fatty liver disease: systematic review and meta-analysis. Hepatology 65, 1557–1565 (2017).
Chiriac, S. et al. Nonalcoholic fatty liver disease and cardiovascular diseases: the heart of the matter. Can. J. Gastroenterol. Hepatol. 2021, 6696857 (2021).
Golabi, P. et al. Causes of death in patients with Non-alcoholic Fatty Liver Disease (NAFLD), alcoholic liver disease and chronic viral Hepatitis B and C. Ann. Hepatol. 27, 100556 (2022).
Estes, C. et al. Modeling NAFLD disease burden in China, France, Germany, Italy, Japan, Spain, United Kingdom, and United States for the period 2016-2030. J. Hepatol. 69, 896–904 (2018).
Staels, B., Butruille, L. & Francque, S. Treating NASH by targeting peroxisome proliferator-activated receptors. J. Hepatol. 79, 1302–1316 (2023).
Wettstein, G. et al. The new-generation pan-peroxisome proliferator-activated receptor agonist IVA337 protects the liver from metabolic disorders and fibrosis. Hepatol. Commun. 1, 524–537 (2017).
Boubia, B. et al. Design, synthesis, and evaluation of a novel series of indole sulfonamide peroxisome proliferator activated receptor (PPAR) alpha/gamma/delta triple activators: discovery of lanifibranor, a new antifibrotic clinical candidate. J. Med. Chem. 61, 2246–2265 (2018).
Francque, S. M. et al. A randomized, controlled trial of the Pan-PPAR Agonist Lanifibranor in NASH. N. Engl. J. Med. 385, 1547–1558 (2021).
Marston, N. A. et al. Association between triglyceride lowering and reduction of cardiovascular risk across multiple lipid-lowering therapeutic classes: a systematic review and meta-regression analysis of randomized controlled trials. Circulation 140, 1308–1317 (2019).
Kandelouei, T. et al. Effect of Statins on Serum level of hs-CRP and CRP in patients with cardiovascular diseases: a systematic review and meta-analysis of randomized controlled trials. Mediators Inflamm. 2022, 8732360 (2022).
Jimenez, R. V. & Szalai, A. J. Therapeutic lowering of C-Reactive Protein. Front. Immunol. 11, 619564 (2020).
Pearson, T. A. et al. Markers of inflammation and cardiovascular disease: application to clinical and public health practice: a statement for healthcare professionals from the Centers for Disease Control and Prevention and the American Heart Association. Circulation 107, 499–511 (2003).
Ridker, P. M. et al. C-reactive protein levels and outcomes after statin therapy. N. Engl. J. Med. 352, 20–28 (2005).
Liu, J. R., Liu, Y., Yin, F. Z. & Liu, B. W. Serum ferritin, an early marker of cardiovascular risk: a study in Chinese men of first-degree relatives with family history of type 2 diabetes. BMC Cardiovasc. Disord. 19, 82 (2019).
Fu, A. Z., Qiu, Y., Radican, L., Yin, D. D. & Mavros, P. Pre-existing cardiovascular diseases and glycemic control in patients with type 2 diabetes mellitus in Europe: a matched cohort study. Cardiovasc. Diabetol. 9, 15 (2010).
Matheus, A. S. et al. Impact of diabetes on cardiovascular disease: an update. Int. J. Hypertens. 2013, 653789 (2013).
Alexopoulos, A. S. et al. Glycemic control predicts severity of hepatocyte ballooning and hepatic fibrosis in nonalcoholic fatty liver disease. Hepatology 74, 1220–1233 (2021).
Gujral, U. P. et al. Association between varying cut-points of intermediate hyperglycemia and risk of mortality, cardiovascular events and chronic kidney disease: a systematic review and meta-analysis. BMJ Open Diabetes Res. Care 9, e001776 (2021).
Neves, J. S. et al. Management of dyslipidemia and atherosclerotic cardiovascular risk in prediabetes. Diabetes Res. Clin. Pract. 190, 109980 (2022).
Eddowes, P. J. et al. Accuracy of FibroScan controlled attenuation parameter and liver stiffness measurement in assessing steatosis and fibrosis in patients with nonalcoholic fatty liver disease. Gastroenterology 156, 1717–1730 (2019).
Gastaldelli, A. et al. PPAR-gamma-induced changes in visceral fat and adiponectin levels are associated with improvement of steatohepatitis in patients with NASH. Liver Int. 41, 2659–2670 (2021).
Balas, B. et al. Pioglitazone treatment increases whole body fat but not total body water in patients with non-alcoholic steatohepatitis. J. Hepatol. 47, 565–570 (2007).
Shadid, S. & Jensen, M. D. Effect of pioglitazone on biochemical indices of non-alcoholic fatty liver disease in upper body obesity. Clin. Gastroenterol. Hepatol. 1, 384–387 (2003).
Basu, A. et al. Effects of pioglitazone versus glipizide on body fat distribution, body water content, and hemodynamics in type 2 diabetes. Diabetes Care 29, 510–514 (2006).
White, U., Fitch, M. D., Beyl, R. A., Hellerstein, M. K. & Ravussin, E. Adipose depot-specific effects of 16 weeks of pioglitazone on in vivo adipogenesis in women with obesity: a randomised controlled trial. Diabetologia 64, 159–167 (2021).
Rubenstrunk, A., Hanf, R., Hum, D. W., Fruchart, J. C. & Staels, B. Safety issues and prospects for future generations of PPAR modulators. Biochim. Biophys. Acta 1771, 1065–1081 (2007).
Tsuchida, A. et al. Peroxisome proliferator-activated receptor (PPAR)alpha activation increases adiponectin receptors and reduces obesity-related inflammation in adipose tissue: comparison of activation of PPARalpha, PPARgamma, and their combination. Diabetes 54, 3358–3370 (2005).
Hsiao, G. et al. Multi-tissue, selective PPARgamma modulation of insulin sensitivity and metabolic pathways in obese rats. Am. J. Physiol. Endocrinol. Metab. 300, E164–E174 (2011).
Rasouli, N., Kern, P. A., Elbein, S. C., Sharma, N. K. & Das, S. K. Improved insulin sensitivity after treatment with PPARgamma and PPARalpha ligands is mediated by genetically modulated transcripts. Pharmacogenet. Genom. 22, 484–497 (2012).
Gastaldelli, A. & Cusi, K. From NASH to diabetes and from diabetes to NASH: Mechanisms and treatment options. JHEP Rep. 1, 312–328 (2019).
Bajaj, M. et al. Decreased plasma adiponectin concentrations are closely related to hepatic fat content and hepatic insulin resistance in pioglitazone-treated type 2 diabetic patients. J. Clin. Endocrinol. Metab. 89, 200–206 (2004).
Belfort, R. et al. A placebo-controlled trial of pioglitazone in subjects with nonalcoholic steatohepatitis. N. Engl. J. Med. 355, 2297–2307 (2006).
Gastaldelli, A. et al. Importance of changes in adipose tissue insulin resistance to histological response during thiazolidinedione treatment of patients with nonalcoholic steatohepatitis. Hepatology 50, 1087–1093 (2009).
Gastaldelli, A. et al. Pioglitazone in the treatment of NASH: the role of adiponectin. Aliment Pharm. Ther. 32, 769–775 (2010).
Simon, T. G. et al. The nonalcoholic fatty liver disease (NAFLD) fibrosis score, cardiovascular risk stratification and a strategy for secondary prevention with ezetimibe. Int. J. Cardiol. 270, 245–252 (2018).
Sao, R. & Aronow, W. S. Association of non-alcoholic fatty liver disease with cardiovascular disease and subclinical atherosclerosis. Arch. Med. Sci. 14, 1233–1244 (2018).
Shang, Y., Nasr, P., Widman, L. & Hagstrom, H. Risk of cardiovascular disease and loss in life expectancy in NAFLD. Hepatology 76, 1495–1505 (2022).
Toh, J. Z. K. et al. A meta-analysis on the global prevalence, risk factors and screening of coronary heart disease in nonalcoholic fatty liver disease. Clin. Gastroenterol. Hepatol. 20, 2462–2473.e2410 (2022).
Sinn, D. H. et al. Nonalcoholic fatty liver disease for identification of preclinical carotid atherosclerosis. Medicine 95, e2578 (2016).
Targher, G., Byrne, C. D. & Tilg, H. NAFLD and increased risk of cardiovascular disease: clinical associations, pathophysiological mechanisms and pharmacological implications. Gut 69, 1691–1705 (2020).
Anstee, Q. M., Mantovani, A., Tilg, H. & Targher, G. Risk of cardiomyopathy and cardiac arrhythmias in patients with nonalcoholic fatty liver disease. Nat. Rev. Gastroenterol. Hepatol. 15, 425–439 (2018).
Targher, G., Corey, K. E., Byrne, C. D. & Roden, M. The complex link between NAFLD and type 2 diabetes mellitus - mechanisms and treatments. Nat. Rev. Gastroenterol. Hepatol. 18, 599–612 (2021).
Stefan, N., Schick, F., Birkenfeld, A. L., Haring, H. U. & White, M. F. The role of hepatokines in NAFLD. Cell Metab. 35, 236–252 (2023).
Bedossa, P. & Consortium, F. P. Utility and appropriateness of the fatty liver inhibition of progression (FLIP) algorithm and steatosis, activity, and fibrosis (SAF) score in the evaluation of biopsies of nonalcoholic fatty liver disease. Hepatology 60, 565–575 (2014).
American Diabetes, A. 2. Classification and diagnosis of diabetes: standards of medical care in diabetes-2018. Diabetes Care 41, S13–S27 (2018).
Pfutzner, A. & Forst, T. High-sensitivity C-reactive protein as cardiovascular risk marker in patients with diabetes mellitus. Diabetes Technol. Ther. 8, 28–36 (2006).
Zhao, S., Kusminski, C. M. & Scherer, P. E. Adiponectin, Leptin and Cardiovascular Disorders. Circ. Res. 128, 136–149 (2021).
Acknowledgements
The study was supported and funded by Inventiva. Inventiva clinical research staff was involved in the study design, and collection and analysis of data, prepared and reviewed the manuscript for medical and scientific accuracy. The authors retained responsibility for the final decision to submit the paper for publication. Medical writing support was provided by D.R.B. (Translational Medicine Academy, Basel, Switzerland) and funded by Inventiva. We thank the patients, study investigators and their staff who participated in the clinical study described here.
Author information
Authors and Affiliations
Contributions
Conceptualization of the analyses, interpretation of results, drafting of the manuscript (M.P.C.); statistical analyses and design of figures and tables (L.D. and P.H.M.), drafting of results section and quality control (D.R.B.), management and oversight of the trial (M.B., M.F.A., S.M.F.); contribution to interpretation of data (J.B., R.P.G., F.Z., J.L.J., P.B., M.F.A., S.M.F.); critical review of the manuscript (all authors).
Corresponding author
Ethics declarations
Competing interests
M.P.C., L.D., P.H.M., M.B. and P.B. are employees of Inventiva. J.L.J. is a consultant for Inventiva. D.R.B. has received honoraria from Inventiva via Translational Medicine Academy. J.B. has served as a consultant for Abbott, American Regent, Amgen, Applied Therapeutic, AskBio, Astellas, AstraZeneca, Bayer, Boehringer Ingelheim, Boston Scientific, Bristol Myers Squibb, Cardiac Dimension, Cardiocell, Cardior, Cardiorem, CSL Bearing, CVRx, Cytokinetics, Daxor, Edwards, Element Science, Faraday, Foundry, G3P, Innolife, Impulse Dynamics, Imbria, Inventiva, Ionis, Lexicon, Lilly, LivaNova, Janssen, Medtronics, Merck, Occlutech, Owkin, Novartis, Novo Nordisk, Pfizer, Pharmacosmos, Pharmain, Prolaio, Regeneron, Renibus, Roche, Salamandra, Sanofi, SC Pharma, Secretome, Sequana, SQ Innovation, Tenex, Tricog, Ultromics, Vifor, and Zoll. RPG received research support or honoraria form Amgen, Anthos Therapeutics, Daiichi Sankyo, Ionis, Dr. Reddy’s Laboratories, Medical Education Resources, Menarini, SAJA Pharmaceuticals, Servier, SUMMEET, and consults for Artivion, Beckman Coulter, Daiichi Sankyo, Gilead, Inari, Inventiva, PhaseBio Pharmaceuticals, Samsung and Aventis. FZ reports personal fees from 89Bio, Abbott, Acceleron, Applied Therapeutics, Bayer, Betagenon, Boehringer, BMS, CVRx, Cambrian, Cardior, Cereno pharmaceutical, Cellprothera, CEVA, Inventiva, KBP, Merck, NovoNordisk, Owkin, Otsuka, Roche Diagnostics, Northsea, USa2, having stock options at G3Pharmaceutical and equities at Cereno, Cardiorenal, Eshmoun Clinical research and being the founder of Cardiovascular Clinical Trialists. MFA received grants from Boehringer-Ingelheim, Gilead, Hanmi, Inventiva, Madrigal, Novo Nordisk; honoraria from Clinical Care Options, Fishawack, Medscape, Terra Firma, CLDF; royalties from Up-to-Date; consults for 89Bio, BMS, Hanmi, Inventiva, Intercept, Madrigal, Merck, Novo Nordisk. SMF received grants from Astellas, Falk Pharma, Genfit, Gilead Sciences, GlympsBio, Janssens Pharmaceutica, Inventiva, Merck Sharp & Dome, Pfizer, Roche; honoraria from Abbvie, Allergan, Bayer, Eisai, Genfit, Gilead Sciences, Janssens Cilag, Intercept, Inventiva, Merck Sharp & Dome, Novo Nordisk, Promethera, Siemens; serves as consultant for Abbvie, Actelion, Aelin Therapeutics, AgomAb, Aligos Therapeutics, Allergan, Alnylam, Astellas, Astra Zeneca, Bayer, Boehringer Ingelheim, Bristoll-Meyers Squibb, CSL Behring, Coherus, Echosens, Dr. Falk Pharma, Eisai, Enyo, Galapagos, Galmed, Genetech, Genfit, Genflow Biosciences, Gilead Sciences, Intercept, Inventiva, Janssens Pharmaceutica, PRO.MED.CS Praha, Julius Clinical, Madrigal, Medimmune, Merck Sharp & Dome, Mursla Bio, NGM Bio, Novartis, Novo Nordisk, Promethera, Roche, Siemens Healthineers.
Peer review
Peer review information
Nature Communications thanks the anonymous reviewer(s) for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Cooreman, M.P., Butler, J., Giugliano, R.P. et al. The pan-PPAR agonist lanifibranor improves cardiometabolic health in patients with metabolic dysfunction-associated steatohepatitis. Nat Commun 15, 3962 (2024). https://doi.org/10.1038/s41467-024-47919-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-024-47919-9
- Springer Nature Limited